Rural areas face unique challenges ensuring availability and accessibility of healthcare services1-4. Delivery of quality end-of-life care is no exception5-8. Palliative care has been both more available and more heavily researched in urban than in rural areas9. In general, rural residents have been found to be less likely to use specialized palliative care than their urban counterparts5,6,10, and more likely to be hospitalized near end of life10-12. However, beyond dichotomous urban/rural comparisons, there remains a need for research exploring the influence of rural economic, social, and physical environments on palliative care, in order to support service planning9.
The World Health Organization defines palliative care as 'an approach that improves the quality of life of patients and their families facing the problems associated with life-threatening illness.' It seeks to provide relief from pain and other distressing symptoms, and integrates psychological and spiritual aspects of patient care13 . Palliative care typically requires an interdisciplinary team approach, with members each contributing specialized knowledge14. Although it is often the case that rural residents travel to urban centers for specialized care, quality palliative care can and should be available in rural communities where people who are at end of life can be close to the support of their families, friends, and healthcare providers who know them well. Models exist that provide assessment, consultation, support, and knowledge regarding the delivery of palliative care to family physicians and other non-specialized care providers, in order to enable access to a palliative approach in the absence of a large specialized workforce15. In this article formal palliative care programs (PCPs) enable the delivery of appropriate palliative services, even if most direct patient care is provided by generalists9,15.
This study examines factors associated with enrollment in a PCP, and place of death, across urban and rural districts of the Canadian province of Nova Scotia. PCP enrollment and place of death are accepted indicators of quality end-of-life care16,17 and are used in regional surveillance reporting18. Rather than simply comparing urban and rural areas, this research uses linked administrative data to closely examine how the effects of demographic, geographic, and socioeconomic factors differ across service delivery settings.
Approach
This retrospective, population-based study used linked administrative health and census data.
Study data
This study linked PCP patient enrollment files from three districts to Nova Scotia vital statistics death certificate data. Postal codes of the decedents were mapped to 2006 Canadian dissemination area census data. The included districts had electronic service databases suitable for linkage, and represent 60% of people who died in Nova Scotia over the study period19. Probabilistic linkage with multiple identifiers (provincial health card number, name, postal code, dates of birth and death, sex, and address) was used because health card number was missing for 10% of the vital statistics records and to varying degrees in other databases.
Analysis
Descriptive statistics are reported. Logistic regression was used to produce univariate and multivariate (adjusted) odds ratios (OR) and their 95% confidence intervals (CI). Analysis was performed first with all study subjects and then stratified by the three districts of residence. All analysis was completed using Statistical Analysis System v9.2 (SAS Institute; http://www.support.sas.com/software/92).
Setting/subjects
Nova Scotia provides a unique context in which to examine geographic variations in end-of-life care. Unlike most provinces in Canada that have a large percentage of urban residents, almost half (44.5%) of Nova Scotians live in rural areas20. There is a PCP in each of the nine district health authorities in the province, meaning that all Nova Scotians have some degree of PCP access within their district of residence. The PCPs are hospital-based services that can include community-based consultation in the home and in nursing homes. There are no free-standing hospice facilities. At the same time, the districts differ markedly in their geographic characteristics, socioeconomic composition, and availability of tertiary care and health human resources. The PCPs themselves also differ in their history, especially in the degree to which they were tied to cancer treatment as they developed and whether or not home-based services and rural populations were explicitly targeted.
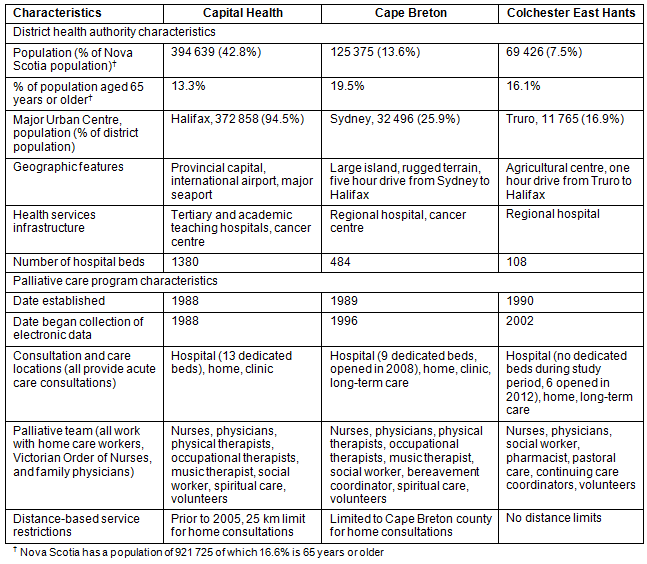
This study covers three districts that have differing contexts for health services provision (Table 1). Both the Capital Health (CH) and Cape Breton (CB) PCPs developed with strong ties to cancer treatment centres, while the more rural Colchester East Hants (CEH) was established slightly later, with support from Federal Health Transition Funds15. CB and CEH had the most developed volunteer societies. CEH was conceived with barriers to palliative care in rural communities considered from the outset, and a focus on supporting care at home, through coordination and service integration21. The CEH model uses an interprofessional palliative care consult team to support care providers in rural communities, enabling greater access to a palliative approach at home. The team provides advice and support to family physicians, enabling them to follow patients into hospital and maintain continuity of care. Consultation nurses also work in the community to support home care nurses, home support workers, and family caregivers. During the study time period, after-hours phone support to family physicians, Victorian Order of Nurses (VON) care providers, and patients and families was available from palliative care consult nurses who had access to a palliative care physician.
All residents of CH, CB, and CEH districts who were 20 years or older and died between 2003 and 2009 were included, with two exceptions. Nursing home residents were excluded because they have different demographics and patterns of end-of-life care use21, and their postal codes of residence may not reflect their community of longer-term residence. Those who died with accidental, mental health, or unclassifiable causes of death were excluded as they are not normally candidates for palliative care.
Table 1: District and palliative care program characteristics for three districts in Nova Scotia
Measurements
Dependent variables: PCP enrollment was a dichotomous variable (enrolled or not), as indicated by the existence of a PCP record. Place of death from vital statistics records was dichotomized as in or out of hospital.
Independent variables: Age and sex are known predictors of PCP registration22. Age was divided into five categories with ≥85 years used as the reference in multivariate analyses.
A classification system developed by Fassbender et al. was used to assign each underlying cause of death to a pattern of functional decline23. This divides decedents into those with terminal illness (eg cancer, amyotrophic lateral sclerosis, and human immunodeficiency virus), organ failure (eg congestive heart failure, chronic obstructive pulmonary disease), and frailty (eg dementia, Parkinson's disease, infections, weight loss, osteoporosis). Lunney et al. found that those dying of terminal illness show a rapid decline in functioning near death24,25. The decline for persons with organ failure is accompanied by acute life-threatening episodes. Those in the frailty category more typically experience a gradual decline over an extended time period. Trajectory of decline has implications for palliative care planning, and in the past, palliative care has focused on patients with the terminal illness trajectory, most commonly cancer26.
Year of death was included because PCP enrollment increased over time, as did the proportion of deaths occurring outside of hospital. The inclusion of year of death also controls for changes over time in health system policy, programs, practices, and funding.
Two geographic characteristics were examined that may have influenced PCP enrollment as well as place of death. Distance from each person's residence to their nearest PCP was examined because it has been an inverse predictor of PCP enrollment7,27. A dichotomous urban/rural variable was also included. Residents in a Census Metropolitan Area (urban area with a core population of >100 000: Halifax) or a Census Agglomeration (urban area with a core population between 10 000 and 100 000: Sydney and Truro) were compared to those in non-metropolitan (rural) areas. Urban residents typically have shorter travel time to PCP clinics and hospital beds based in the urban centres, so a correlation between distance to PCP and this urban/rural indicator was expected. However, attributes of rurality beyond distance may be relevant to end-of-life care, such as living in an area of sufficient population size and density to support the constellation of health and social services used at end of life7, as well as cultural aspects of urban and rural residence related to caregiving at end of life9,27,28.
Previous research has shown that those living in more economically deprived communities were less likely to access specialized palliative services6, and more likely to die in hospital11, though not all studies examining palliative care across urban and rural settings have captured economic deprivation10,12. Qualitative studies have found that the provision of palliative care in rural communities involves a complex network of care providers and that social resources are key to understanding care provision29-31, but socioeconomic measures have rarely been examined quantitatively6. To address this, two deprivation indices were constructed using dissemination area census data and methods from Pampalon et al32. These relate to economic and social resources available in people's communities that may influence access to services. Economic deprivation combines the proportion of individuals with a high school diploma, proportion employed, and average family income. Social deprivation is based on the proportion of individuals living alone and who are separated, divorced or widowed, as well as the proportion of single-parent families. All variables were logged if skewed, normalized as z-scores, summed, and then divided into quintiles. The least-deprived quintile was used as reference in multivariate analyses.
Ethics approval
Ethical approval for this research was provided by all participating districts (file numbers CDHA-RS/2011-243, CB-2011-004, and CEHHA1101).
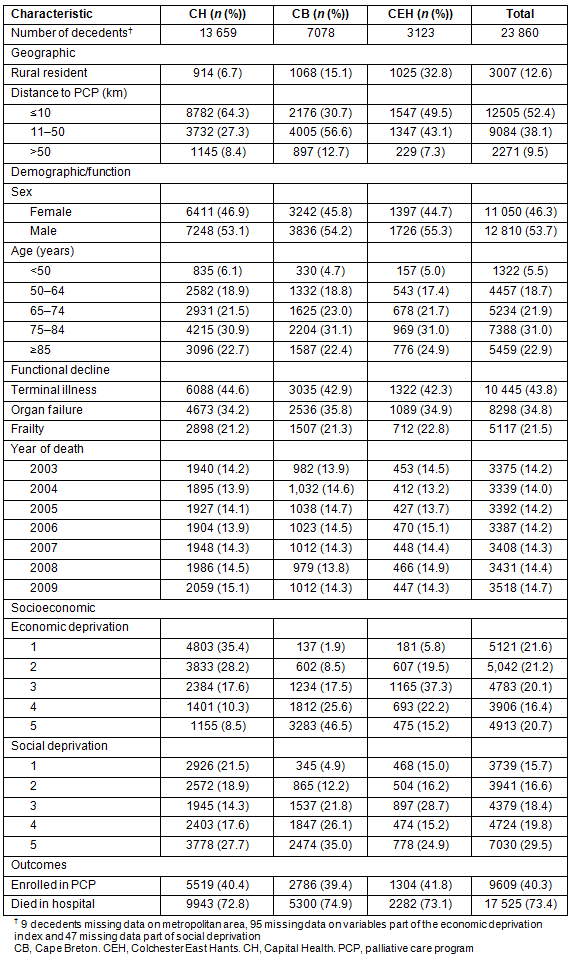
There were 33 181 adult (aged ≥20 years) Nova Scotians who died in the study areas between 1 January 2003 and 31 December 2009. Of these, 7472 were nursing home residents, and 1849 were non-nursing home residents who died suddenly or of 'other' causes of death, and were excluded, leaving 23 860 study subjects (71.9% of all decedents). CEH had a higher proportion of rural residents (32.8%) than CB (15.1%) and CH (6.7%). People in CB lived at greater distance from the PCP with only 30.7% living within 10 km, compared to 49.5% for CEH and 64.3% for CH (Table 2).
Approximately 54% of the study subjects were male. Patterns of trajectory of decline were similar across districts with 42-45% terminal illness, 34-36% organ failure, and 21-23% frailty. The small differences by district were consistent with the variation by age in that those dying of terminal illness were younger than those dying of organ failure or frailty. The number of deaths per year increased slightly over time for all three districts. The count of deaths in 2009 (3518) was 4.2% higher than 6 years earlier (3375).
The study population differed markedly by socioeconomic status across the districts. Residents of CB were both more economically and socially deprived; 46.5% were in the lowest income quintile compared to 15.2% for CEH and 8.5% for CH. CB only had 4.9% in the most socially advantaged quintile compared to 15.0% for CEH and 21.5% for CH.
Overall, 40.3% of the study subjects were enrolled in a PCP, and 73.4% died in hospital. CEH had the highest PCP enrollment rate (41.8%) and CB the lowest (39.4%). CB had the highest in-hospital death rate (74.9%) and CH the lowest (72.8%).
Table 2: Characteristics of district health authority populations and total study population, 2003-2009
PCP enrollment
No significant differences were observed in univariate odds of PCP enrollment across districts (Table 3). However, after adjusting for demographic, geographic, and socioeconomic characteristics, the residents of the more predominantly rural CEH and CB districts had higher odds of PCP enrollment than CH residents (CEH OR: 1.42; 95%CI: 1.27, 1.60; CB OR: 1.21; 95%CI: 1.11, 1.34).
Overall, women and those younger than 85 years were more likely to be enrolled, as were people with terminal illness (as opposed to organ failure or frailty). Urban residents had higher adjusted odds of enrollment (OR: 1.51; 95%CI: 1.29, 1.77), while those at greater distance from a PCP had lower odds (OR: 0.33; 95%CI: 0.27, 0.40) for those >50 km vs those ≤10 km). Gradients in PCP enrollment were observed by economic and social deprivation in univariate analysis, but not for economic deprivation in the multivariate analyses. The multivariate social deprivation findings were significant for two quintiles.
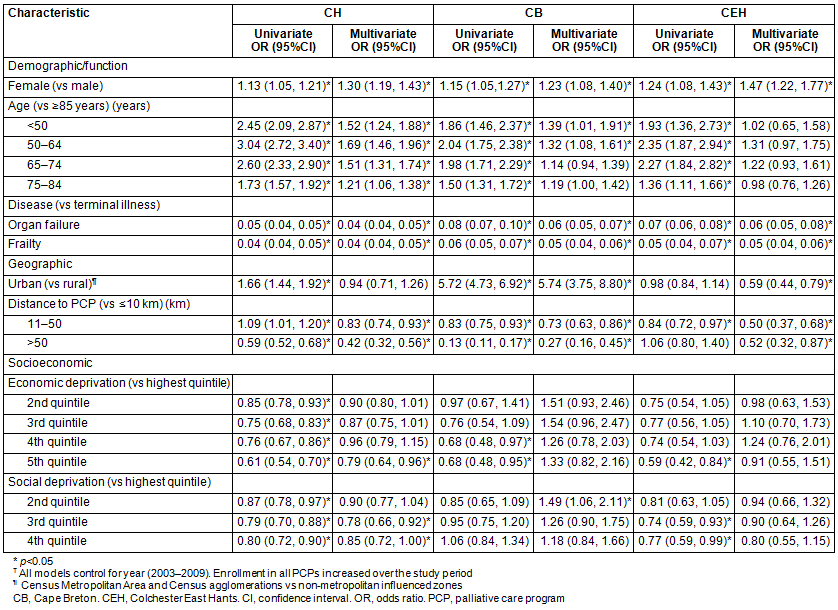
When stratified by district (Table 4), being female and terminal disease remained significant predictors of PCP enrollment in all districts. In general, a U-curve pattern of PCP enrollment was observed for age, with a peak for those aged 50-64 years. While a significant effect was not observed in multivariate results for CEH population, this may be due to the smaller sample size because the magnitude of the CEH OR was similar to those for CB.
While an inverse relationship between distance to PCP and PCP enrollment was evident in all districts, the magnitude was greatest in CB. The effect of urban residence differed across districts. After distance and other variables were controlled, there was no urban/rural effect in CH. In CB and CEH, urban/rural status and distance were both independent and significant factors associated with PCP enrollment, but they operated in different directions. Not surprisingly, CB residents were less likely to be PCP enrollees if they lived at a distance and if they lived in rural areas. CEH shows surprising multivariate findings: being an urban resident (OR: 0.59; 95%CI: 0.44, 0.79) and living at a distance (11-50 km OR: 0.50; 95%CI: 0.37, 0.68); ≥50 km OR: 0.52; 95%CI: 0.32, 0.87) are both predictors of decreased probability of PCP enrollment.
In multivariate analyses, beyond the most economically deprived in CH having lower odds of PCP enrollment, there is no evidence that living in an area of economic deprivation is a predictor of PCP enrollment (Table 3). A more marked social deprivation gradient effect was observed in CH. Similar magnitudes of social deprivation odds were observed for CEH but they are not statistically significant. Significant interpretable patterns were not observed between social deprivation and PCP enrollment in CB.
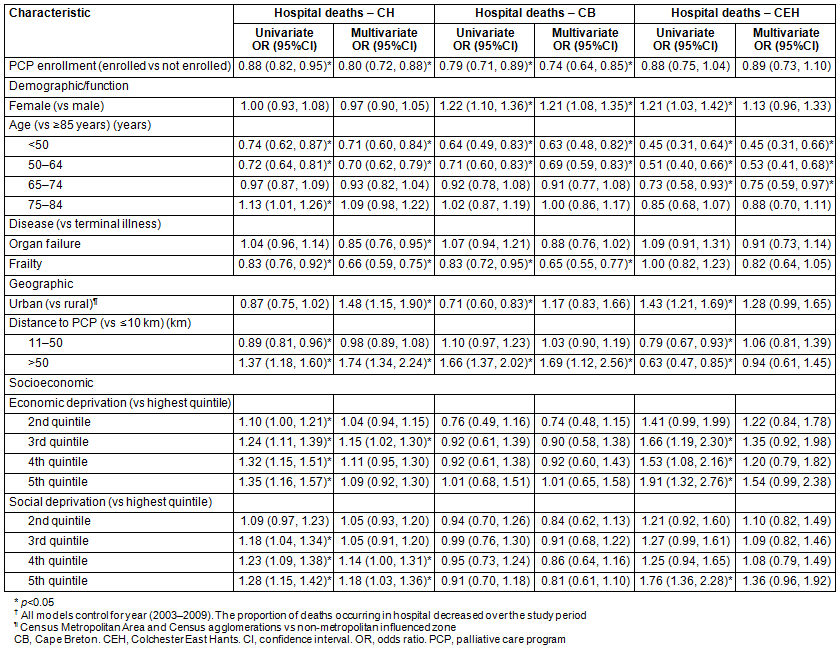
Table 3: Odds of palliative care program enrollment and place of death?
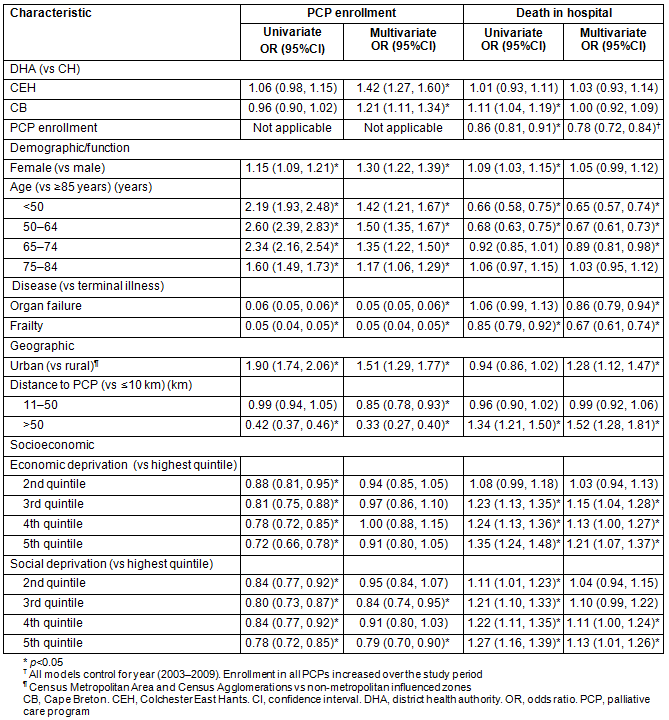
Table 4: Univariate and multivariate odds of palliative care program enrollment by district health authority?
Place of death
No significant differences among districts were observed in multivariate odds of death in hospital (Table 2). Overall, PCP enrollment was a predictor of decreased likelihood of dying in hospital (OR: 0.78; 95%CI: 0.72, 0.84) (Table 3), but this effect was smaller and non-significant for CEH (OR: 0.89; 95%CI: 0.73, 1.10) (Table 5).
There was no overall difference between males and females in the likelihood of dying in hospital (OR: 1.05; 95%CI: 0.99, 1.12). However, CB showed higher odds of hospitalization among females (OR: 1.21; 95%CI: 1.08, 1.35)). Younger adults were less likely to die in hospital across all areas. Those with frailty trajectories were less likely to die in hospital in CH (OR: 0.66; 95%CI: 0.59, 0.75)) and CB (OR: 0.65; 95%CI: 0.55, 0.77), but a significant association was not observed in CEH (OR: 0.82; 95%CI: 0.64, 1.05).
In CH, multivariate analyses found that urban residents (OR: 1.48; 95%CI: 1.15, 1.90), those residing more than 50 km from the PCP (OR: 1.74; 95%CI: 1.34, 2.24), in the middle economic quintile (OR: 1.15; 95%CI: 1.02, 1.30), and in the lowest two social deprivation quintiles (OR: 1.14; 95%CI: 1.00, 1.31; OR: 1.18; 95%CI: 1.03, 1.36) were more likely to die in hospital. The elevated odds of death in hospital among urban residents of CH emerge only in adjusted analysis, after controlling for the significant role of PCP enrollment, patient demographics, distance to PCP and socioeconomic status. In CB, only living more than 50 km from the PCP (OR: 1.69; 95%CI: 1.12, 2.56) was a predictor. For CEH, there were no significant predictors, although urban residence (OR: 1.28; 95%CI: 0.99, 1.65), lowest economic quintile (OR: 1.54; 95%CI: 0.99, 2.38), and lowest social deprivation quintile (OR: 1.36; 95%CI: 0.96, 1.92) approached significance.
Table 5: Univariate and multivariate odds of dying in hospital by district health authority?
Discussion
The high percentage of males among study subjects was expected, because nursing home residents were excluded and they have a higher proportion of women. Different proportions across districts were expected given the slight differences in age profiles.
Unlike expectations from other studies5,6,10, the adjusted odds of PCP enrollment were higher for the PCPs outside of the metropolitan centre, and the magnitude of the effect of distance to PCP differed across districts. For CEH, this might relate to the development of the PCP as an integrated palliative home care demonstration project that considered barriers to palliative care in rural communities from the outset15. The fact that odds of dying in hospital did not differ significantly for urban and rural residents, or by distance in this district, may also speak to the success of this model at integrating care in the home setting15. This is promising, as there is an established need for innovative models of service provision to address the unique challenges of palliative care in rural and remote settings9.
The development of the PCP in CEH as an integrated palliative home care model has as an underlying assumption the availability of comprehensive essential services. For example, as noted, 24/7 palliative consultation was available in CEH during the study time period. However, due to recent budget cuts, this has been discontinued. So it cannot be assumed that the success of the CEH as reported herein can be continued to the same extent into the future.
Also, while nursing home residents were excluded from this study, findings may have been affected by a lack of nursing home beds in both CH and CEH during the study period. Because hospice beds are not available in Nova Scotia, when nursing home beds are in short supply, and social and economic resources to support care at home are lacking, a family physician may admit to hospital rather than contact the PCP. This may explain the CEH findings that lower odds of PCP enrollment emerge among persons in both urban and more remote (>50 km) areas in multivariate analysis, since residents within the urban centre were less economically deprived on average, while those at greater distance from PCP were less socially deprived. This may also help explain the higher adjusted odds of hospitalization at end of life for urban persons in CH. Both CH and CEH have now seen the opening of new nursing home facilities to meet this need.
The higher magnitude of the effect of distance in CB and CH on both PCP enrollment and place of death may be related in part to the fact that home consultations were limited by distance to these PCPs. Both time and costs associated with traveling to receive care are strong concerns among patients and informal caregivers8,33. The dispersed population and hilly terrain in CB may exacerbate the role of distance as a barrier to services.
Others have noted a lack of attention to the positive aspects of rural and remote contexts with respect to the provision of palliative care9. The fact that social and economic gradients in PCP use and hospitalization were less apparent or non-significant in CB and CEH may speak to success enabling services for the economically and socially disadvantaged in these areas. However, relatively blunt measures of social and economic resources, and a lack of statistical power, complicate this interpretation. The authors' indices of social and economic deprivation, while representing improvements over more simplistic measures of socioeconomic status, are limited. They are based on area- rather than individual-level data, which may be especially problematic in lower-density rural settings where the aggregated areas are larger, and populations within may be more heterogeneous. The chosen measure of social deprivation focuses largely on family resources for care provision. Further research that assesses aspects of social capital that extend into the broader community is needed29.
An additional weakness of this analysis is that it could not differentiate palliative hospital beds from non-palliative beds in examining place of death. Place of death must also be distinguished from location of care in the last weeks of life. The latter may better reflect the total experience of care, but could not be measured in available data. Moreover, place of death must be aligned with individual preference to truly reflect quality of care. Patient preference was not captured in the study datasets, but a recent survey of caregivers following the death of a loved one in Nova Scotia found that of the 47.5% of decedents who had voiced a preference on where they would prefer to die, 73.4% preferred the home34.
Finally, the studied districts may differ from other districts. CEH is similar to the other non-metropolitan districts in Nova Scotia in size, geography, and health services infrastructure. However, strong clinical champions and targeted government funding were instrumental in developing the CEH program; these catalysts were not present in all other non-metropolitan districts in the province, or across Canada35.
The development and reporting of empirical data on palliative care is critically important. In this case, it provides new information highlighting success in addressing socioeconomic and geographic barriers to care. However, caution is advised in the interpretation of population-level indicators that are not well grounded in an understanding of the geographic areas examined. This study used existing administrative data sources to examine PCP enrollment in both urban and rural settings, and uncovered complexities in interpreting comparisons between geographic areas. Further research is needed which makes use of alternative data sources and research designs to provide richer information about resources that equip communities to manage end-of-life care, and interventions that may support their development.
There remains a clear need for innovative service delivery models to address the unique conditions of palliative care provision in rural and remote settings. Though more research is needed, these findings show promise that disparities in access between urban and rural settings are not unavoidable, and positive aspects of rural and remote communities may be leveraged to improve care at end of life.
Acknowledgements
This study was supported by the Canadian Institutes of Health Research (grant number HOA-80067) on Reducing Health Disparities.
References
1. Sibley LM, Weiner JP. An evaluation of access to health care services along the rural-urban continuum in Canada. BMC Health Services Research 2011; 11: 20.
2. Wilson K, Rosenberg MW. The geographies of crisis: exploring accessibility to health care in Canada. Canadian Geographer 2002; 46(3): 223-234.
3. Pong RWR, Pitblado JRR. Beyond counting heads: some methodological issues in measuring geographic distribution of physicians. Canadian Journal of Rural Medicine 2002; 7(1): 12-20.
4. Pong RW, DesMeules M, Heng D, Lagace C, Guernsey JR, Kazanjian A, et al. Patterns of health services utilization in rural Canada. Chronic diseases and injuries in Canada. Sudbury, Ontario: Centre for Rural and Northern Health Research, Laurentian University, 2011; 1-36.
5. Cinnamon J. Examining the spatial accessibility of palliative care services in British Columbia: recommendations for providing care in BC's rural and remote regions. Vancouver, BC: University of British Columbia, 2009.
6. Lavergne MR, Johnston GM, Gao J, Dummer TJ, Rheaume DE. Variation in the use of palliative radiotherapy at end of life: examining demographic, clinical, health service, and geographic factors in a population-based study. Palliative Medicine 2011; 25(2): 101-110.
7. Wilson DM, Thomas R, Kovacs Burns K, Hewitt JA, Osei-waree J, Robertson S. Canadian rural-urban differences in end-of-life care setting transitions. Global Journal of Health Science and Education 2012; 4(5): 1-13.
8. Wilson DM, Justice C, Sheps S, Thomas R, Reid P, Leibovici K. Planning and providing end-of-life care in rural areas. Journal of Rural Health 2006; 22(2): 174-181.
9. Robinson C, Pesut B, Bottorff J, Mowry A, Broughton S, Fyles G. Rural palliative care: a comprehensive review. Journal of Palliative Medicine 2009; 12(3): 253-258.
10. Goodridge D, Lawson J, Rennie D, Marciniuk D. Rural/urban differences in health care utilization and place of death for persons with respiratory illness in the last year of life. Rural and Remote Health. 10(2): 1349. (Online) 2010. Available: www.rrh.org.au. (Accessed 10 March 2011).
11. Burge F, Lawson B, Johnston G. Where a cancer patient dies: the effect of rural residency. Journal of Rural Health 2005; 21(3): 233-238.
12. Menec VH, Nowicki S, Kalischuk A. Transfers to acute care hospitals at the end of life: do rural/remote regions differ from urban regions? Rural and Remote Health 10(1): 1281. (Online) 2010. Available: www.rrh.org.au. (Accessed 10 March 2011).
13. World Health Organization. WHO definition of palliative care. (Online). Available: http://www.who.int/cancer/palliative/definition/en. (Accessed 9 October 2014).
14. Burge F, Canning K, Cummings I, Dukeshire S, McKim A, Rowswell C, et al. A rural palliative home care model: the development and evaluation of an integrated palliative care program in Nova Scotia and Prince Edward Island. Truro, Nova Scotia: Province of Nova Scotia, 2001.
15. Canadian Hospice Palliative Care Association. Innovative models of integrated hospice palliative care, The Way Forward Initiative: an integrated palliative approach to care. Ottawa, Ontario: Canadian Hospice Palliative Care Association, 2013.
16. Grunfeld E, Urquhart R, Mykhalovskiy E, Folkes A, Johnston G, Burge FI, et al. Toward population-based indicators of quality end-of-life care: testing stakeholder agreement. Cancer 2008; 112(10): 2301-2308.
17. Grunfeld E, Lethbridge L, Dewar R, Lawson B, Paszat LF, Johnston G, et al. Towards using administrative databases to measure population-based indicators of quality of end-of-life care: testing the methodology. Palliative Medicine 2006; 20(8): 769-777.
18. Canadian Institute for Health Information. Health care use at the end of life in Atlantic Canada. Ottawa, Ontario: Canadian Institute for Health Information, 2011.
19. Province of Nova Scotia. Nova Scotia Community Counts. Data modeled from Statistics Canada, Census of Population 2006. (Online) 2011. Available: www.gov.ns.ca/finance/communitycounts/profiles/health/profilec.asp (Accessed 6 September 2013).
20. Statistics Canada. Farm population and total population by rural and urban population, by province. 2001 and 2006 Census of Agriculture and Census of Population. (Online) 2008. Available: http://www.statcan.gc.ca/tables-tableaux/sum-som/l01/cst01/agrc42d-eng.htm (Accessed 23 September 2013).
21. O'Brien MB, Johnston GM, Gao J, Dewar R. End-of-life care for nursing home residents dying from cancer in Nova Scotia, Canada, 2000-2003. Supportive Care in Cancer 2007; 15(9): 1015-1021.
22. Burge FI, Lawson BJ, Johnston GM, Grunfeld E. A population-based study of age inequalities in access to palliative care among cancer patients. Medical Care 2008; 46(12): 1203-1211.
23. Fassbender K, Fainsinger RL, Carson M, Finegan B. Cost trajectories at the end of life: the Canadian experience. Journal of Pain and Symptom Management 2009; 38(1): 75-80.
24. Lunney J, Lynn J, Foley D. Patterns of functional decline at the end of life. Journal of the American Medical Association 2003; 289(18): 2387-2392.
25. Lunney JR, Lynn J, Hogan C. Profiles of older medicare decedents. Journal of the Americal Geriatrics Society 2002; 50(6): 1108-1112.
26. Murray S, Sheikh A. Care for all at the end of life. British Medical Journal 2008; 336: 958.
27. Castleden H, Crooks V, Schuurman N, Hanlon N. "It's not necessarily the distance on the map...": using place as an analytic tool to elucidate geographic issues central to rural palliative care. Health and Place 2010; 16(2): 284-290.
28. Waldrop D, Kirkendall AM. Rural-urban differences in end-of-life care: implications for practice. Social Work in Health Care 2010; 49(3): 263-289.
29. Pesut B, Robinson C, Bottorff J. Among neighbors: an ethnographic account of responsibilities in rural palliative care. Palliative and Supportive Care 2013; 12(02): 127-138.
30. Lewis JM, DiGiacomo M, Luckett T, Davidson PM, Currow DC. A social capital framework for palliative care: supporting health and well-being for people with life-limiting illness and their carers through social relations and networks. Journal of Pain and Symptom Management 2013; 45(1): 92-103.
31. Pesut B, Bottorff J, Robinson C. Be known, be available, be mutual: a qualitative ethical analysis of social values in rural palliative care. BMC Medical Ethics 2011; 12: 19.
32. Pampalon R, Hamel D, Gamache P, Raymond G. A deprivation index for health planning in Canada. Chronic Diseases in Canada 2009; 29(4): 178-191.
33. Lockie SJ, Bottorff JL, Robinson CA, Pesut B. Experiences of rural family caregivers who assist with commuting for palliative care. Canadian Journal of Nursing Research. 2010; 42(1): 74-91.
34. Burge F, Lawson B, Johnston G, Asada Y, Flowerdew G, McIntyre P, Grunfeld G. Experience of care during the end of life: early results from the Nova Scotia mortality follow-back study. (Online) 2012. Available: http://www.medicine.dal.ca/content/dam/dalhousie/images/faculty/medicine/departments/department-sites/family/DFM_research_nsmortalitystudy.pdf (Accessed 19 March 2013).
35. Kelley ML. Developing rural communities' capacity for palliative care: a conceptual model. Journal of Palliative Care 2007; 23(3): 143-153.
