Overview
Climate change is widely acknowledged as one of the largest foreseeable threats to community health and wellbeing in the 21st century1. The extent to which health services are prepared for, or able to adequately respond to, climate change impact-related risks remains unclear2,3. The fifth assessment report (AR5) of the Intergovernmental Panel on Climate Change (IPCC) concluded that action to adapt health services is the key unknown in estimating the future health burden of climate change4. Additionally, the IPCC's special report on managing extreme events (SREX) concluded that adaptive actions will be necessarily 'framed by trade-offs between competing prioritized values and objectives'2. Building health decision-support mechanisms in order to involve and empower local stakeholders to help create the basis for agreement on these adaptive actions is an important first-step aid for informing health sector adaptation actions.
This article examines the development and pilot implementation of an approach to support local community decision-makers to plan health adaptation responses to climate change. The approach involves health and wellbeing risk assessment supported through the use of an electronic tool based on an IPCC style of assessment. First, the article examines the complexity of the climate change science to adaptation translational process - with reference to existing research literature on community development - in the context of addressing human health risks for rural and remote communities in Tasmania, Australia. Second, this process is further examined through the pilot implementation of an electronic tool designed to support the translation of physically based climate change impact information into community-level assessments of health risks and adaptation priorities. It is argued that, if managed carefully within a balanced portfolio of efforts2, such integrative tools are likely to provide valuable support for decision-making that will assist reducing human health vulnerability to climate change in rural communities.
The urgency of building risk management capital
More than 80 000 journal papers on climate change have been published. More than 7300 of these describe the health effects of climate change, and of those more than 6800 were published after 2000. The leading health journal The Lancet, summarising the findings of the IPCC fourth assessment report (AR4)5, described climate change as likely to be the biggest human health threat of the 21st century without appropriate health sector adaptation1. Estimates produced by the UN suggest an escalating human toll globally from climate change of >300 000 mortalities, >300 million seriously affected annually, half a billion at extreme risk, and several billion people being vulnerable6. Developing countries and rural communities are most at risk as climate change works to multiply health inequalities arising from socioeconomic disadvantage2,7,8. Australia, the country where this pilot tool was developed, is one of the world's most at-risk developed countries9-13 .
Climate vulnerability of rural communities is a function not simply of geographical location, socioeconomic disadvantage and more limited access to community infrastructure, but also of the lower levels of climate change risk management capital held by these communities and about them. 'Climate change risk management capital' for the health sector can be described as access to adaptive mechanisms for managing the health and wellbeing effects of climate change, from adaptation know-how and motivation to material assets for making those adaptations14. Climate adaptation is often defined as an 'adjustment in natural or human systems in response to actual or expected climatic stimuli or their effects, which moderates harm or exploits beneficial opportunities'5 - in contrast to 'mitigation' or reduction of carbon emissions. Adaptation activities are wide-ranging and can include preventative or avoidance actions, as well as sharing or bearing risk and loss15,16.
Yet communities are heterogeneous. As working group II of AR5 concluded, 'the precise causes of vulnerability, and therefore the most relevant adaptation capacities, vary greatly from one setting to another'4 such that 'choices and outcomes for adaptive actions to climate events must reflect divergent capacities and resources and multiple interacting processes'2. While adaptation more generally at the local community level can confer health benefits4 and health stakeholders are diverse, health adaptation requires specialised health sector knowledge and action. Health adaptation involves understandings of the culture and nature of the health professions, the biomedical dynamics of health, and the operational contexts of health services2. This heterogeneity of communities and specialist requirements of health adaptation presents particular obstacles to achieving community-level health adaptation, notwithstanding the extensive literature on adaptation documented in SREX2. As working group II of AR5 suggests, the focus of adaptation has been on public health surveillance, disaster planning and coordination measures, vulnerability mapping and early warning systems4. However, while the volume of quantitative studies relevant to adaptation is growing and the importance of epidemiological approaches has been asserted17, relatively little practical health sector adaptation at the local, whole-of-community governance level is occurring16,18-23.
It is important to observe that just because an event can be researched, is foreseeable and/or detected through early warning systems, it does not mean that communities have 'actionable knowledge'24. Scientific knowledge must be integrated into local contextual knowledge in meaningful ways for it to be actionable. As the policies of the global UN and WHO suggest, climate change adaptation must involve applied, decision-support approaches that build on, and learn from, local community knowledge, particularly for already disadvantaged groups25,26.
Under-utilisation of health risk assessments
One response to these shared challenges globally has been to conduct climate change impact and risk management exercises at the local community level, including through local climate witnessing programs27. Climate change risk management exercises are often led by local government, building on their strong foundations in impact and risk assessments for local planning. A 2013 review of climate change adaptation tools by Australia's National Climate Change Adaptation Research Facility (NCCARF) estimated that about a third of local government associations in Australia have completed some kind of climate change risk assessment exercise, even if only of an awareness-raising kind3. However, most of these exercises are broadly focused paper-based questionnaires that do not target climate change-related risks to health specifically. While the NCCARF review identified more than 300 international products that could be variously described as supporting processes, data collection, or providing integrated knowledge portals, few online whole-of-community health risk assessment and adaptation tools were identified3.
This is not to deny the richness of potential adaptation options in the literature summarised by SREX2. Nor is it to deny the accumulating efforts of leading agencies to develop early warning systems28-37, as opposed to products for community health adaptation decision support.
In this context, this article argues that the lessons from climate change research and from the findings of government-funded state and national health impact and risk assessments38,39 have not been well translated into local community health impact and risk assessments. Furthermore, the health sector has not been well supported to translate the findings of localised climate change impact and risk assessment exercises into provincial or national health planning.
Community health sector adaptation tools
Many countries are developing fine-grained local-level climate change projections for local community use. However, the need remains for more integrated mechanisms with greater utility for stepping local communities through what is required to turn climate change projections into local health sector adaptation priorities leveraging local knowledge2.
Accordingly, the present study was informed by principles consistent with the experience of effective local-level disaster risk assessment summarised by IPCC2 and SREX2. The study is also consistent with the literature on community climate change risk perceptions that has recommended climate change adaptation tools should involve (1) use of local municipality-level climate change projections to target local contexts; (2) re-framing and re-examination of risk perceptions40-42 using a structured process of scrutiny of the evidence; (3) building a sense of self-efficacy43 in using climate change projections, together with other information, to make decisions; and (4) consensus-making among community stakeholders about the risks and adaptive actions needed, in the light of practical barriers, to create the impetus for collective action.
The Tasmanian context
Tasmania is an Australian island state with a population of approximately 500 000 people. More than half of this population lives in the greater city area of the capital Hobart, located in the south of the island. While the overall population density is low, the average age of the population is amongst the oldest in Australia, which is also contributing to increased pressure on health services.
Tasmania has a cool temperate climate, with current projections predicting average annual temperatures across the island will increase by between 1.6ºC and 2.9ºC by 2100. With eastern and north-eastern coast waters warming rapidly, it is increasingly recognised as a global warming hotspot13.
Significantly, it has been noted that in the area of climate change impact on health services a number of important gaps exist, including in relation to 'regionally-focussed vulnerability and risk assessment and monitoring; and techniques for improving the responsiveness and management of health impacts or events as they arise, as well as preparing communities for longer term adjustment to changing environmental and health conditions'13.
In responding to these challenges, the authors developed and piloted an electronic tool to help support the translation of physically based climate change impact information into community-level assessments of health risks and adaptation priorities. The development of this tool was intended for use primarily by local government or similar community governance agencies. The primary research question driving its development was 'What can be learned from pilot implementation of a community health and well-being risk assessment (CHWRA) IT-based tool designed to support understanding of, and decision-making on, local community challenges and opportunities associated with health risks posed by climate change?'
Approach
Stakeholder participants in the project attended three face-to-face workshops hosted by local government agencies in Tasmania (southern rural inland, rural north coast, and remote north-western highlands). Local government authorities administered invitations to local community members identified with particular expertise, or the need to develop expertise, in climate change and health risk management. Municipal authorities were advised to keep the workshops to a manageable size of about eight people. There were eight participants on the north coast and six at each of the southern and north-western highlands workshops. Some IT support and equipment were provided to participants, building on available local resources. Each workshop was about 5 hours in duration and involved the following steps.
Create understanding: A climate scientist presented local area climate projections using a PowerPoint presentation via Skype conference. The facilitator then described the evidence on climate-health dynamics, using both the international epidemiology literature as well as pre-workshop research into local general practitioners' conceptualisations of observed local climate-health dynamics.
Profiling: Data were collected from workshop participants about the length of time they had resided in the region, their community role and their opportunities to observe health or health-related effects of climate in their local government area.
Climate health effects: Working individually, participants provided broad observations identifying health impacts already felt in their local area, in ways useful to conceptualising a wide range of possible local climate-health dynamics, both positive and negative.
Climate health risks and opportunities: Working individually, participants provided detailed, structured estimates of health risks and opportunities, which involved identifying the nature, extent and likelihood of these risks and opportunities.
Supplementary questions: Working as a group, participants added and answered any additional questions about climate health issues not covered previously but that they considered important to their region.
Identify priorities: Working individually, participants developed priorities for adaptation under five domains for health service development (service governance and culture, service delivery, workforce development, material infrastructure and finance) described in the pre-pilot publication on these health adaptation domains, particularly for more climate-vulnerable groups.
Consensual summary statements: The facilitator shared the data provided by individual respondents with the group (ie showed group responses on a screen using the inbuilt tool capabilities for data integration and display); the group considered these data to reach consensus on the key impacts, risks and opportunities, and adaptations needed, taking into account practical implementation issues such as costs, and key strategies needed for particular vulnerable groups.
Details of the CHWRA decision-support tool
The CHWRA information technology-based climate change adaptation decision-support tool was designed to help support resource-poor rural communities through all aspects of the interactive face-to-face workshop. Primarily this involved the collection and collation of responses from workshop participants that the tool could then be used to easily display graphically to facilitate further discussion around emerging priorities and perspectives. The tool was designed to provide secure web-based data access, data integration and data discovery services designed to optimise data availability, useability, security and interoperability. Development of the tool involved investigating ways of integrating open-source features and functions suitable for the workshop. Detailed weather and climate data are available for Tasmania and may be obtained from the Australian Bureau of Meteorology databases. To make the tool usable in locations where these detailed data are not available, the authors adapted free open-source mapping tools to support interpolation of less granular data to support workshop activities. The tool offers a number of specific functions and features that include:
- a simple user interface supporting ease of data collection, collation, analysis and display of data generated by workshop participants
- localised geospatial mapping of key features and community services within any local community/region
- dynamic visualisation of climate time-series data (historic and projected) overlaid on maps of the local community region
- integration and visualisation of other locally available data - demographics, community service facilities and capacities - mapped at the local government region level.
It should be emphasised that the tool continually evolved through the life of the pilot and post-pilot period. Figure 1 is a screenshot of the initial form of the integrative tool used in the pilot, from a section used to obtain data for step 6: participant identification of priorities for adaptation under five domains for health service development.
Figure 2 is a screenshot showing one of the functions of the tool available post-pilot. It illustrates what could be described as the interactive 'tagging function' of the tool, which enables stakeholder perceptions and knowledge about services to be incorporated into existing maps (ie maps that were not developed by the researchers and do not presently include that local knowledge). The local knowledge could be some aspect of a health service or some other feature of the local area relevant to understanding a community's infrastructure and adaptive capacity. To the right of the figure can be seen a box including the local area climate change projections or profile. While technically this tagging feature is straightforward, the task of ensuring its ease of use and integration into the flow of the workshop in a manner that optimised data capture from stakeholders, with data discovery and visualisation relevant to health-climate risks, proved to be complex. Ultimately this function aims to capture such features of local services easily added by participants, to map and run time-series data based on climate model projections over the tagged maps, aiding visualisation of likely impacts and risks faced into the future. While data-poor communities present specific challenges, for regions where good-quality health services data are not available at a sufficiently fine detail or granularity, the tagging function can aid incorporation of local knowledge with climate change projections.
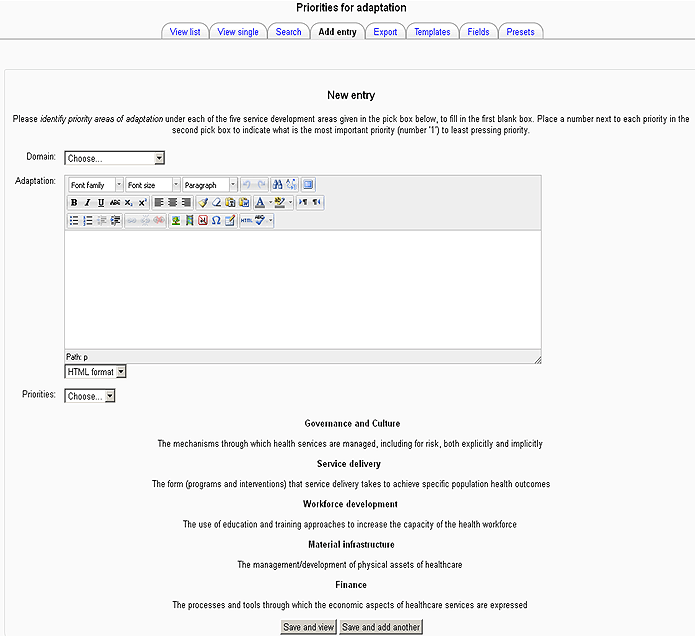
Figure 1: Screenshot of the community health and well-being risk assessment tool at pilot stage.
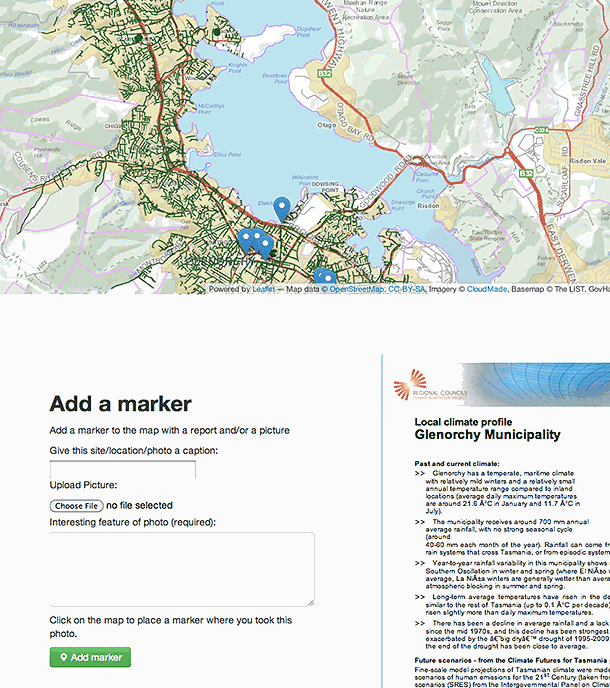
Figure 2: Screenshot of the tagging function of the community health and well-being risk assessment tool.
Local climate profiles
Workshop participants received a local climate profile for their municipality prepared by a climate scientist from the University of Tasmania's Antarctic Climate and Ecosystems Cooperative Research Centre, drawing on their technical reports series from the Climate Futures for Tasmania project44. This was a point of departure for the first step of the workshop where the climate scientist gave an oral presentation by Skype summarising the local climate change projections and the science behind these projections, and was available to answer questions. The local climate change profiles for each of the three municipalities included assessments and/or estimates of the past, current and future climate information. The future climate information was based on fine-scale (~10 km) dynamically downscaled regional climate model projections corresponding to two plausible scenarios of carbon emissions in the 21st century: high emissions continuing (the A2 scenario), as well as emissions plateauing and then falling (the B1 scenario)45. These two emissions scenarios were chosen from the suite of scenarios presented in the special report on emissions scenarios (SRES)46; future iterations of the tool could easily accommodate later emissions scenarios. For example, in the pilot tool workshop, under the higher emissions scenario (A2), the rise in average temperatures over the 21st century for the southern inland municipality was projected to be 2.6-3.3ºC compared with the lower emissions scenario (B1) projected change of 1.3-1.6ºC. Changes in the frequency, intensity and duration of extreme temperatures were included for the two different scenarios for each municipality in the study. Further changes in rainfall, runoff, river flows and flooding, as well as projections for extreme sea level events, were described for different areas of the municipality. This information was nuanced for the local context; for example, specific local municipality river flooding projections were based on climate model outputs as well as flood hydraulic models. This allowed estimates of high flood levels for catchments with a critical duration of less than a specific number of hours in a specific area given by the climate profile for a specific region. Some example agricultural impacts and opportunities were also given based on standard agricultural indices, such as specific decreases in chill hours relevant to vineyards, and increases in suitable agricultural land currently undeveloped due to temperature-linked altitude limitations. These climate profiles also noted where conditions would stay the same, for example the proportion of time in severe drought.
Climate and health information
Workshop participants were also informed by a 30-minute presentation on national and international research on climate and health, consistent with the summary paper of the field3, as well as available Tasmanian research from the published pre-pilot study. The Tasmanian-based research described a wide range of clinical and non-clinical effects of climate change on communities from a qualitative interview-based study of how general practitioners conceptualised observed health effects of climate change: mental health effects such as depression from drought and dispossession; insect-borne diseases such as Ross river virus in communities where this virus had not previously been observed; asthmatic conditions linked to shifts in the seasonality of pollens; water (quality and supply) issues linked to extreme weather; anxiety and stress linked to interactions between climate change, the global financial crisis and changes in global markets affecting farm viability and food costs. This juxtaposition between the international literature and pre-pilot work for the tool provided a point of departure for conceptualising (not establishing) possible climate health effects in the local community.
Ethics approval
Ethics approval for the study was obtained from the Human Research Ethics Committee at the University of Tasmania, REF #H0012002.
Respondent profiles
In all three municipalities, respondents indicated they had spent a range of time in their region, from 1-5 years through to 35-45 years. Their responses indicated they had diverse occupational roles: local government environment officers, emergency services staff, medical and allied health professionals, and representatives of health consumer organisations. A rural general practitioner from each region was in attendance at each workshop. Most respondents across the three regions indicated they had spent 25% or less of their time 'observing the health or health-related effects of climate change': four out of the six attending in the south, all eight in the north, and three in the north-west. As intended, the stakeholders were not primarily health practitioners, but community leaders with a wide range of roles important to whole-of-community responses to the health effects of climate change.
Community participants' risk assessments and adaptation priorities
Table 1 describes the health risks identified by participants in the site working individually, as part of step 4 of the workshop asking them to identify 'what might happen in the near or distant future' for their local government region. The results in the table suggest that community members identified perceived catastrophic effects that are 'likely' to 'almost certain' to occur, as well as myriad other health effects with lesser expected impacts, likelihood and immediacy.
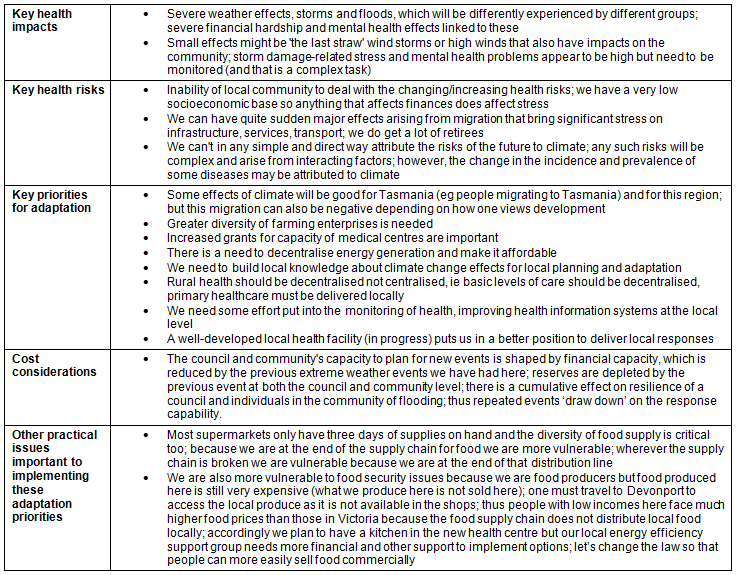
Table 2 provides an example community consensus statement from the integrative tool, suggesting the 'free form' of these statements of key impacts, risks, priorities for adaptation, cost considerations and other practical issues. As such, it offers a snapshot of the kind of observations captured from each of the three pilot sites. The themes that connected the three consensus statements collected were a concern with adaptation capacity and community resilience, and what they described as 'last straw' climate effects for stressed communities. There was an emphasis also on limited health infrastructure and its implications for adaptive capacity. Statements also focused on preventative action and community engagement, including for groups with lower health literacy.
A key theme was managing the socioeconomic multipliers of the effects of climate change. Food security was cited as important, with adaptive capacity shaped by a community's disadvantaged location in the food supply chain, even where that community is a food-producing community. Another theme was declining community volunteerism (leading, for example, to a lack of trained voluntary firefighters) and community participation generally. Statements also referred to declining localism of policy and planning, and its implications for managing nuanced and locally informed rural responses to climate change. They included a concern about the absence of evidence-based supports for decision-making about health adaptation. Above all, responses emphasised the importance of an applied, complexity-oriented understanding of how climate interacts with local services and communities to create health effects. In relation to the CHWRA tool, the northern group in particular stated the need for more modelling of the kinds of information the tool was designed to elicit from local climate witnesses.
Table 1: Community stakeholder-identified health risks during workshops at three rural Tasmanian local government sites
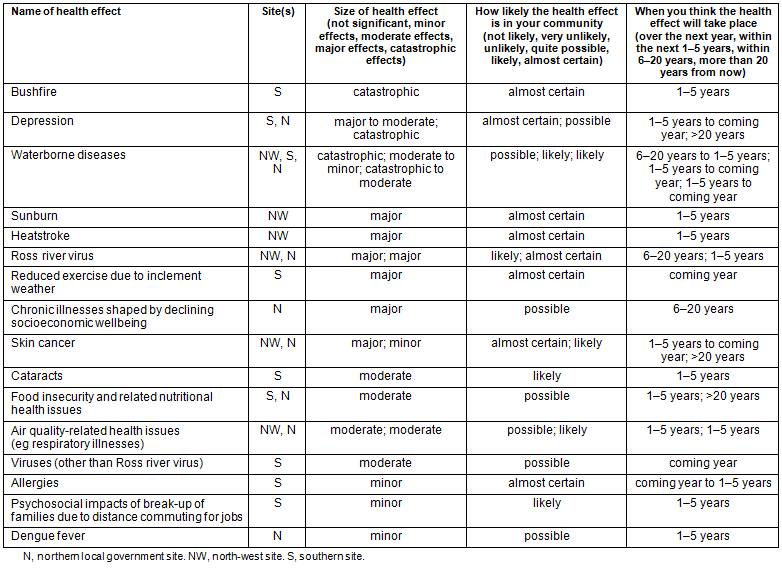
Table 2: Tasmanian north-west highlands consensus summary statement from the integrative tool
Discussion
This study presents a practical example of how complex community-level judgements about climate change, health risks and responses can be usefully captured electronically in ways that offer potentially actionable information about priorities for climate adaptation - a first step in planning. The authors found that community stakeholders were willing and able to provide information about their observations of health risks and offer suggestions for adaptive actions for their community. Such contextualised priority setting has the potential to shift debates away from contested beliefs about climate change towards much-needed action on the shared vulnerabilities facing a particular community.
However, the literature and the example in the present study also highlight the challenges associated with translating climate change projections into community-level assessments about health adaptation priorities. A translational tool will most likely not be used by local communities unless resources and commitment exist for that translation. The CHWRA tool needs to be facilitated by a local governance mechanism and supported by at least one climate scientist and climate and health researcher. Further, as the facilitator emphasised to the workshop participants, such judgements must be regarded as only one indicative source of information for health planning in a region, designed to supplement other information that a community has about itself. What is important about these community judgements is not their precision or reliability - as if it is this that should or does limit action - but the creation of shared values and commitments.
This pilot study encountered other key decision-support challenges that would benefit from further exploration. While community participants identified a wide range of broad adaptive priorities, they found it difficult to provide advice about more specific adaptation actions. Accordingly, while the integrative tool delivered a wide range of broad, potentially useful information for each region and was feasible given local community resources and time, its technical features (data visualisation, integration and analysis) are in ongoing development in light of these findings. The tool will eventually be fully web-based and adaptable to any geospatial location, regardless of the diversity in the granularity of data sources available for that location. A future inclusion will be the introduction of an expert-system module to support best-practice adaptation scenarios, providing participants with opportunities to develop their know-how about health adaptation. This adaptation modelling work is especially important as knowledge about adaptation strategies increases. Currently, it involves examining known adaptation activities and strategies covering 'share loss or share risk; bear loss or bear risk; prevent effects or reduce effects; avoid risk or exploit changes in risk'15, under each of the service adaptation domains in the tool (Fig1) in relation to specific known climate-vulnerable groups.
In the context of the wider community development literature, the present study supports theoretical frameworks emphasising the importance of accessing local creativity and innovation including through competence-building44,45. However, it also indicates the limitations of such frameworks. The consensus statements obtained reinforce that local government and community resources and capabilities are indeed finite. Consistent with the IPCC's conclusions2, local adaptive processes need support from higher levels of government and often also from other local areas to be effective47. Future development of the tool should help achieve this integration through data sharing and presentation in different policy-relevant forums and formats. The data from the tool will need to be presented in a way that helps community participants explain the findings to other members of their community not at the workshop. There is a potential gulf between those who participate in such risk assessment exercises and the wider community: other residents may not necessarily agree with participant-held or even community-wide notions of, for example, bushfire risk48. Much more needs to be understood about whether and how identifying adaptation priorities in such risk assessment exercises leads to real action.
Notwithstanding the complexity of the challenges in providing communities with decision-support tools of this kind, interest in and demand for such support tools is high. The project has been widely disseminated across Australian local government industry forums as well as other national and international climate change research forums. Information about the project has been selected by the Southern Tasmanian Councils Authority for inclusion in their wider adaptation guidelines for local government authorities, an encouraging sign of horizontal or intermunicipal integration. The CEOs of environmental protection agencies or their equivalents in 11 African and central Asian countries have collaborated with the authors of this study to develop a funding application platform for trialling and adapting the tool in their countries, particularly in rural communities. Additional partnerships for trialling and adapting the tool for use in the South Pacific and mainland Australia are still under discussion. Such dissemination is proceeding with an awareness that, managed poorly, community health risk assessment could work as a liability, adding to the risks such communities already face from climate change. Yet, if managed carefully, such tools could work within a balanced portfolio of measures2 to help reduce the rising health burden from climate change.
Acknowledgements
This article is dedicated to the memory of our dear colleague and friend Erica Bell - the primary author of this manuscript - who sadly passed away in late July 2014. Erica was the inspiration for this project and was an important figure in moving forward the area of public health issues and climate change in the state of Tasmania.
The content of this article was submitted as part of a consultant's report to the funder and has been presented at a wide range of national and international conferences. Prior to the project being conducted, the intentions of this study were described in a paper published in the 2011 conference proceedings of the Australian Centre for Excellence in Local Government Researchers Forum. This project has also had the support of key national and Tasmanian stakeholders: the Australian Centre for Excellence in Local Government, the Local Government Association of Tasmania and the Southern Tasmanian Councils Authority, as well as the three local government authorities who participated in the pilot. The authors thank the local community organisations that provided participants. Special thanks are also owed to the University of Tasmania's Antarctic Climate and Ecosystems Cooperative Research Centre for providing the climate scientist for workshops and for allowing workshops to draw on their technical reports series from their Climate Futures for Tasmania project. The authors gratefully acknowledge OpenStreet Map as the provider of the open-source mapping tool used. Notwithstanding, all content in this article is the sole responsibility of the authors and this article does not purport to express the views of any of the individuals or organisations so acknowledged. This project was supported by the Tasmanian Government's Office of Climate Change, Department of Premier and Cabinet 'ClimateConnect' community grants program and a University of Tasmania Research Enhancement Grant.
References
1. Costello A, Abbas M, Allen A, Ball S, Bell S, Bellamy R, et al. Managing the health effects of climate change. The Lancet 2009; 373, 1693-1733.
2. Intergovernmental Panel on Climate Change. Managing the risks of extreme events and disasters to advance climate change adaptation: special report of working groups I and II of the Intergovernmental Panel on Climate Change. Cambridge: Cambridge University Press, 2012.
3. Webb B, Beh J. Leading adaptation practices and support strategies for Australia: an international and Australian review of products and tools. Brisbane, Qld: National Climate Change Adaptation Research Facility, 2013.
4. Intergovernmental Panel on Climate Change assessment report 5, working group II. Climate change 2014: impacts, adaptation, and vulnerability. IPCC fifth assessment report. Cambridge and New York: IPCC, 2014.
5. Pachauri RK, Reisinger A, Eds. Climate change 2007: synthesis report. Contribution of working groups I, II and III to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change. Geneva: IPCC, 2007.
6. Global Humanitarian Forum. Human impact report: climate change - the anatomy of a silent crisis. Geneva: Global Humanitarian Forum, 2009.
7. Marmot M, Friel F, Bell R, Houweling T, Taylor S. Closing the gap in a generation: health equity through action on the social determinants of health. Geneva: World Health Organization, 2008.
8. Department of Environmental Affairs. South Africa's second national communication under the United Nations Framework Convention on Climate Change. Pretoria: Department of Environmental Affairs, Republic of South Africa, 2011.
9. McMicheal A, Weaver HJ, Berry H, Beggs PJ, Currie B, Higgins J, et al. National adaptation research plan: Human health. Gold Coast, Qld: National Climate Change Adaptation Research Facility, 2008; 1-59.
10. Climate Commission. The critical decade: climate science, risks and responses. Canberra, ACT: Climate Commission, 2011.
11. Holmes C. Queensland Floods Commission of Enquiry: final report. Brisbane, Qld: Queensland Government, 2012.
12. Teague B, McLeod R, Pascoe S. 2009 Victorian Bushfires Royal Commission. Summary report; volumes I-IV. Melbourne, Vic: Parliament of Victoria, 2009.
13. McDonald J, Harkin J, Harwood A, Hobday A, Lyth A, Meinke H. Supporting evidence-based adaptation decision-making in Tasmania - the state of adaptation research. (Online) 2013. Available: http://www.nccarf.edu.au/publications/adaptation-synthesis-tasmania (Accessed 10 January 2014).
14. Adger WN, Agrawala S, Mirza MMQ, Conde C, O'Brien K, Pulhin J, et al. Assessment of adaptation practices, options, constraints and capacity. In ML Parry, OF Canziani, JP Palutikof, PJ van der Linden, CE Hanson, Eds. Fourth assessment report of the Intergovernmental Panel on Climate Change. Contribution of working group II. Cambridge: Cambridge University Press, 2007; 717-743.
15. West C, Gawith M. Measuring progress: preparing for climate change through the UK Climate Impacts Programme. Technical report. Oxford: UK Climate Impacts Programme, 2005.
16. Burton I, Diringer E, Smith J. Adaptation to climate change: international policy options. Arlington: Pew Centre for Global Climate Change, 2006.
17. Hosking J, Campbell-Lendrum D. How well does climate change and human health research match the demands of policymakers? A scoping review. Environmental Health Perspectives 2012; 120: 1076-1082.
18. European Environment Agency. Adapting to climate change - SOER 2010 thematic assessment. Copenhagen: EEA, 2010.
19. Massey E, Bergsma E. Assessing adaptation in 29 European countries. Amsterdam: IVM Insititute of Environmental Studies, 2008.
20. Swart R, Biesbroek R, Binnerup S, Carter TR, Cowan C, Henrichs T, et al. Europe adapts to climate change comparing national adaptation strategies. PEER report no 1. Helsinki: Partnership for European Environmental Research, 2009.
21. Balbus J, Ebi K, Finzer L, Malina C, Chadwick A, McBride D, et al. Are we ready? Preparing for the public health challenges of climate change. Washington, DC: Environmental Defense Fund, 2008.
22. Ford J, Berrang-Ford L, Paterson J. A systematic review of observed climate change adaptation in developed nations. Climatic Change 2011; 106(2): 327-336.
23. Bell E. Climate change and health research: has it served rural communities? Rural and Remote Health 13: 2343. (Online) 2013. Available: www.rrh.org.au (Accessed 10 January 2014).
24. Meinke H, Nelson R. Agriculture, food security and climate change - why science alone can't fix the problems. Keynote presentation at the Agricultural Research and Development Assistant conference, Agriculture under the climate changing world, 8-9 September 2010, Bangkok.
25. Conference of the Parties, United Nations. The Cancun agreements: outcome of the Ad Hoc Working Group on Long-term Cooperative Action under the Convention. Bonn: United Nations, 2011; 1-31.
26. World Health Organization. Climate change and health resolution WHA61.19. Geneva: WHO, 2008; 1-3.
27. World Wildlife Fund South Pacific Climate Change Team. Climate witness community toolkit. Suva: WWF-South Pacific Programme, undated.
28. Del Corral J, Blumenthal MB, Mantilla G, Ceccato P, Connor SJ, Thomson MC. Climate information for public health: the role of the IRI climate data library in an integrated knowledge system. Geospatial Health 2012; 6: 15-24.
29. Australian Greenhouse Office Department of Environment and Heritage. Climate change impacts and risk management: a guide for business and government. Canberra, ACT: Australian Greenhouse Office Department of Environment and Heritage, 2006.
30. Local Government Association of Queensland. Adapting to climate change: a Queensland local government guide. Brisbane, Qld: Local Government Association of Queensland, 2007.
31. International Council for Local Environmental Initiatives-Australia/New Zealand. Local government climate change adaptation toolkit. Melbourne, Vic: International Council for Local Environmental Initiatives-Australia/New Zealand Limited, 2008.
32. UK Climate Impacts Programme. The UKCIP adaptation wizard v 3.0. Oxford: UK Climate Impacts Programme, 2012.
33. European Commission. CLIMATE-ADAPT European climate adaptation platform. Brussels: European Commission, 2012.
34. Willows R, Connell, R. Climate adaptation: risk, uncertainty and decision making. Oxford: UK Climate Impacts Programme, 2003.
35. International Council for Local Environmental Initiatives-Canada. Changing climate changing communities: guide and workbook for municipal climate adaptation. Toronto: Local Governments for Sustainability, ICLEI Canada, 2012.
36. Programme of Research on Climate Change Vulnerability Impacts and Adaptation. Guidance on assessing vulnerability, impacts and adaptation (VIA) (Draft). Nairobi: United Nations Environmental Programme, 2012.
37. Swart R, Springer N. Methodology for effective decision making on impacts and adaptation (MEDIATION) project. Brussels: European Commission Seventh Framework Programme, 2012.
38. Spickett J, Brown H, Katscherian D. Health impacts of climate change: adaptation strategies for Western Australia. Perth, WA: Environmental Health Directorate, Department of Health, Government of Western Australia, 2008.
39. Turk R, Battle C, Hanna E, Spickett J, Raso B. The scoping of climate change impacts on population health and vulnerabilities - benchmarking. Melbourne, Vic: Department of Health, 2010.
40. Patchen M. What shapes public reactions to climate change? Overview of research and policy implications. Analyses of Social Issues and Public Policy 2010; 10: 47-68.
41. Etkin D, Ho E. Climate change: perceptions and discourses of risk. Journal of Risk Research 2007; 10: 623-641.
42. de Boer J. Framing climate change and spatial planning: how risk communication can be improved. Water Science & Technology 2007; 56(4): 71-78.
43. Brody SD, Zahran S, Vedlitz A, Grover H. Examining the relationship between physical vulnerability and public perceptions of global climate change in the United States. Environment and Behavior 2008; 40: 72-95.
44. Shaw K. The rise of the resilient local authority? Local Government Studies 2012; 38: 281-300.
45. Von Meding JK, Oyedele L, Cleland D, Spillane J, Konanahalli A. Mapping NGO competency to reduce human vulnerability in post-disaster communities: comparing strategies in Sri Lanka and Bangladesh. International Journal of the Humanities 2011; 8: 119-138.
46. Intergovernmental Panel on Climate Change. IPCC special report: emissions scenarios. Summary for policymakers. (Online) 2000. Available: http://www.grida.no/publications/other/ipcc_sr/?src=/climate/ipcc (Accessed 10 January 2014).
47. Hardoy J, Pandiella G, Barrero LSV. Local disaster risk reduction in latin American urban areas. Environment and Urbanization 2011; 23: 401-413.
48. Gordon JS, Matarrita-Cascante D, Stedman RC, Luloff AE. Wildfire perception and community change. Rural Sociology 2010; 75: 455-477.

