Introduction
The organisation and delivery of out of hours care by general practitioners varies enormously between among European countries1. Reacting to similar demand and supply pressures, European healthcare systems are undergoing significant structural changes to the provision of out of hours care. These changes have been fuelled both by increasing demands for out of hours care and by increasing reluctance among general practitioners to provide such out of hours care2.
Chief among the structural changes are the development of general practice out of hours co-operatives. In the United Kingdom, the first general practitioner co-operatives were set up in the early 1980s, but it was not until the late 1990s that social, cultural and health service changes produced a climate which favoured their development3. By then, the number of co-operatives had increased from approximately fifteen at the end of 1994, to an estimated figure of 250 by 19974. In Denmark in 1992, major national structural reform resulted in the development of a network of local co-operatives5. In the Republic of Ireland, the first co-operative was established in 1999, and by 2002 co-operatives had been initiated in all health board areas in the state.
Rural general practitioners, in comparison to their urban colleagues, are on call more frequently and expected to provide a wider range of medical services, including emergency care6. Such expectations are proving increasingly onerous and unsustainable7-9. It would be expected, therefore, that the development of co-operatives would be especially welcomed by rural practitioners. Rural patients are often used to a small numbers of doctors, sometimes personally known to them, providing out of hours care. They are also used to accessing care close to their own homes. Co-operatives can significantly change both these attributes10, potentially causing patient dissatisfaction. The objective of this study was to investigate whether rurality has an influence on patient satisfaction with out of hours care provided by an Irish general practice co-operative.
Methods
Definitions used in the study
Out of hours contact: An 'Out of hours contact' is defined as any request for medical care between 18.00 hours and 08.00 hours on weekdays, from 08.00 hours on Saturdays to 08.00 hours on Monday morning, and includes all public holidays until 08.00 hours the following morning.
General Medical Services: Free primary care and medications are available to 30% of the population of the Republic of Ireland on a means tested basis; they are described as General Medical Services (GMS) eligible. The other two-thirds, whose income is above a certain level (in 2002: 138 euro per week for a single person aged up to 65 years who is living alone), are responsible for their own primary health care costs. GMS eligible patients are, therefore, the most economically deprived in the community.
Rurality: Rousseau highlighted how widely differing definitions of rurality are utilised, ranging from population density, indices of rurality, and remoteness to subjective assessment11. With such a wide range, it is clear that none captures fully the essence of rurality and that emphasis must, therefore, be placed on 'fitness for purpose'. Within Ireland, there are no standard indices of rurality and in a population-based survey, a pragmatic subjective respondent assessment of rurality was considered to be both feasible and reliable. Patients were, therefore, asked to indicate whether they felt they lived in a town, in a village or in the countryside. To consider remoteness, they were also asked how far from the nearest treatment centre they lived.
Service under study
The family doctor co-operative under study ('Shannondoc') covered a mixed urban and rural population of 85 000 people in the West of Ireland and was funded by the Department of Health and Children. The service began on 25 June 2002, involved 38 family doctors, and responded to approximately 350-450 out of hours calls per week. The Shannondoc receptionist, having received the patient's call, logged the patient's registration details and reason given for calling directly into the 'Adastra' computer system. The details then appeared in a prioritised log that is used by the nurse to identify callers waiting to be assessed and triaged. The triage nurse took the call at the earliest opportunity, using the pre-set protocols to guide and document the process of assessment. The triage nurse either offered advice or organised for the patient to be seen by the doctor on duty. Calls were categorised as either 'emergency', 'urgent' or 'routine', according to agreed guidelines. Call details were then forwarded via mobile telephone and fax to the relevant on-duty general practitioner. The whole process took approximately 5 min. The doctor on duty responded to a patient call by providing telephone advice, undertaking a home visit, or inviting the patient to the designated primary care centre. Every morning general practitioners were faxed a print-out of the calls and associated management received for their own patients during the previous out of hours session.
Shannondoc had fully equipped primary care centres in the general hospital in the geographical centre of Clare and in four surrounding towns. Each primary care centre had a driver and car available at all times and maintained communication via mobile telephone and fax with the Shannondoc call centre.
Design
The study design was comprehensively described in an accompanying paper12. In brief, all patients contacting Shannondoc during a designated 24-day period from 20 September to 14 October 2002 were included in the study. This period was chosen to avoid winter epidemics or holiday periods and to allow a sufficient lag period between the inception of the service and the beginning of the study. The questionnaire had been piloted on two occasions with a sample of 12 patients on each occasion. These patients were living in the area under study and the questionnaire was adjusted in response to the pilot participants' feedback. Patients were sent a postal questionnaire with a covering letter and stamped addressed envelope within 7 days of their contact with the out of hours service (Appendix I). Patients received a telephone reminder between 2 and 4 weeks after the initial sending of the questionnaire.
An adaptation of the McKinley questionnaire13 was used to measure patient satisfaction. As an alternative to the five-point Likert scale used by McKinley, a more simple 'Yes or No' scoring system was utilised. This was the format used in other studies evaluating family doctor co-operatives in the Republic of Ireland14. The questionnaire consisted of a total number of 16 questions grouped into four themes, each requiring a 'Yes or No' answer, as well as an overall rating of the service received. No validation of this adaptation, to our knowledge, has been preformed. The themes used in the questionnaire were: access to care, interpersonal aspects of care, quality of care and overall rating of the service. The final section recorded demographic details of the patients using the service. Respondents were also asked to state their preference for the new Shannondoc provision of out of hours care in comparison to previous arrangements. Patients' previous rota cover (eg 1:1) was determined by LG from the name of the respondents' general practitioner.
Patients were excluded if they had died or were seriously ill, had been admitted to hospital under the Mental Health Act, were a nursing home resident, were non-competent in the English language, did not have a permanent address in the area or had an invalid address, or where confidentiality was a concern. Ethical approval was obtained from the research ethics committee of the Irish College of General Practitioners.
Statistical methods
The data were entered into SPSS for Windows (vers. 11.0) (SPSS Inc; Chicago, IL, USA) for analysis, and appropriately double-checked. For respondents and non-respondents, comparisons of mean age were made using independent-samples t-test while comparisons of gender and GMS status were made using c2 analysis. Comparisons of patient satisfaction were made using c2 analysis. Not all questions were answered by all respondents.
Results
Study population
There were 1203 contacts for the designated study period. A total of 966 questionnaires were forwarded to patients following application of the exclusion criteria. The exclusion rate was 19.7% (237/1203). The largest exclusion category (43.0%) was for those who did not have a permanent address in the area under study. This group was significant because the study area is a popular tourist destination. Other important reasons for exclusion were an invalid address (eg a sports ground) (20.3%), or nursing home resident (17.3%). The overall response rate was 55% (531/966). There was no significant difference between respondents and non-respondents in terms of gender and GMS status. Respondents were older than non-respondents (t (964) = 2.986, p = 0.003).
Respondents
Patients over 65 years of age made up 13.4% (71/531) of the respondents, while 56.5% (300/531) were aged 15 to 64 years with the remainder (29.9% [159/531]) aged less than 15 years. Of the respondents, 39.2% (208/531) were male; 43.3% (229/531) were GMS eligible. Of those who responded, 17.7% (94/531) had received a house call, 67.4% (358/531) were seen at the treatment centre, and the remaining 14.9% (79/531) were managed with telephone advice.
Overall satisfaction with out of hours service
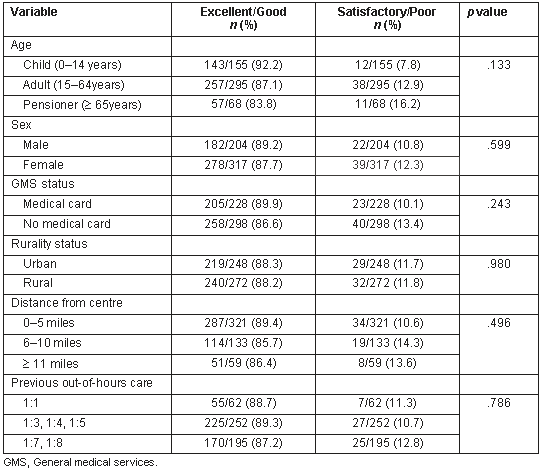
Among the respondents to the questionnaire, 62.0% (328/531) rated the service as excellent; 26.1% (138/531) rated the service as good, and 8.1% (43/531) rated the service as satisfactory. The out of hours service was rated poor by 3.8% (20/531) of patients. Differences of gender and GMS status did not significantly affect overall satisfaction (Table 1). In regard to age grouping, patients 65 years or more had the lowest levels of overall satisfaction followed by adults, with children and their parents or guardians expressing the highest levels of overall satisfaction, but these differences were not statistically significant (p = 0.09).
Table 1: Relationship between patient satisfaction and age, sex, GMS status, distance from nearest Shannondoc centre, rurality status, and previous out of hours care
Rurality and remoteness
47.8% (249/521) of respondents, perceived themselves as living in a town, 14.6% (76/521) perceived themselves as living in a village, and 37.6% (196/521) perceived themselves as living in the countryside. For the purposes of analysis, respondents were divided into urban (those who perceived themselves as living in a town) and rural (those who perceived themselves as living in a village or the countryside). Rurality did not affect overall patient satisfaction (Table 1).
Respondents lived between one and 25 miles from their nearest treatment centre. 62.6% (321/514) lived 5 miles or less from their nearest treatment centre, 25.9% (133/514) lived between 6 and 10 miles from their nearest treatment centre, and 11.5% (59/514) lived greater than 10 miles from their nearest treatment centre. As outlined, distance from the nearest Shannondoc treatment centre did not appear to affect overall patient satisfaction levels (Table 1). Additionally, distance from the nearest Shannondoc treatment centre did not appear to affect the likelihood of receiving a house call. For patients who lived within 5 miles of a treatment centre, 18.3% (59/322) received a house call. For those who lived between 6 and 10 miles of a treatment centre, 19.5% (26/133) received a house call; of those who lived more than 10 miles from the treatment centre, 10.2% (6/59) received a house call.
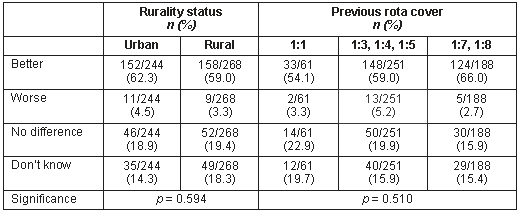
60.7% (315/518) of respondents considered Shannondoc service to be an improvement on their previous out of hours care, 3.9% (20/518) a disimprovement, 18.9% (98/518) no difference, and 16.4% (85/518) did not have an opinion. The perception of quality of care of Shannondoc, in comparison with previous arrangements is illustrated, according to rurality status and previous rota cover (Table 2). There were no differences in preferences according to rurality status or previous rota cover.
Table 2: Perception of quality of care of Shannondoc, in comparison with previous arrangements, according to rurality status and previous rota cover
Discussion
The findings provide reassurance to rural general practitioners concerned about the impact on patient satisfaction of out of hours care provided by a co-operative. In the present study, patient satisfaction was consistent for patients categorised by perceived rurality, distance from treatment centre or type of previous rota. Such concerns may be felt acutely by rural practitioners because they often live in the communities within which they practice. The negative impact on rural practitioner recruitment and retention of the demands in the provision of out of hours care is well recognised. For example, in Ireland less than 10% of a national sample of general practice registrars wished to work in rural practice with the demands of out of hours care perceived as the single biggest barrier15. In Australia, in a qualitative study of medical practitioners who had left rural practice, the most common 'pushing' factor was excessive on-call coverage16. Opposition to the extension of co-operatives to rural areas has sometimes centred around the perceived negative effects on patient satisfaction. The present study suggests that such concerns are unfounded.
An important effect of co-operative care is the increase in the numbers of patients managed by advice alone, and the decrease in those visited at home. It was of interest, therefore, that distance from the nearest treatment centre did not appear to affect the likelihood of receiving a house call. Regular review of such data could act as quality assurance to ensure that rural patients receive an equitable service. It is also noteworthy that the proportion of patients who received advice alone, while higher than that reported when care is reported by 'own general practitioner'17, is still less than that reported by co-operatives in the UK. In reports from Irish co-operatives14,18 generally the proportion of patients seen in treatment centres is much higher than that reported in the UK. Explanation of such process differences is beyond the scope of this paper.
The generalisability of rural research may be problematical. Many European countries do have similar health policy, organisation of general practice and geographical features to that of Ireland19. Extrapolation to countries with more remote rural communities such as Australia should be performed cautiously20. In any event, further confirmation of these findings in different settings would be welcome.
Study limitations
The patient satisfaction measurement instrument used in this study is adapted from McKinley's questionnaire13 on measuring patient satisfaction with out of hours care. Although, this will facilitate comparison with studies carried out in the Republic of Ireland where there is a dearth of published data in relation to out of hours care, it may limit comparison with results from studies that use the Likert scoring system.
Non-response bias is an important potential source of bias which we sought to minimise through careful planning of questionnaire design, sample selection, data collection and a reminder strategy21. The overall response rate for the study was 55% which is comparable with other similar studies.
Defining rurality in terms of perception alone presents some problems. Such an approach is clearly subjective. People's views are coloured by their past and current experiences. Someone who lives or has previously lived in an inner city may have a very different perception of what is rural from someone who has lived in a small farming community their entire life. Thus, two people from the same community may define that community in very different ways. Nonetheless, subjective assessment in the context of the geographical area being studied was pragmatically considered to hold a high degree of validity and reliability, and so this form of assessment was adopted for the current study.
Conclusion
Based on the results of this study, we conclude that patients from rural areas are as equally satisfied with the provision of out of hours care by co-operatives, as urban patients. Extension of co-operatives to rural areas need not be constrained by concerns regarding decreased patient satisfaction.
Acknowledgements
The authors acknowledge Dr R McKinley for allowing them to adapt his patient satisfaction questionnaire; Mr Robert Scully for his data entry and proof reading; Mr Larry Maher, Drs John O'Dea, Billy O'Connell and Brendan Mullins as well as all the Shannondoc staff who contributed to this study. The authors also wish to acknowledge the kindness and generosity of the patients who participated, without whom, the study could never have taken place. The paper was completed whilst AWM was on sabbatical at the Department of General Practice at the University of Adelaide, Australia. This study was funded by a grant from the Research and Education Foundation of the Irish College of General Practitioners.
References
1. NIVEL. Proceedings of the international conference on emergency out of hours care in Europe (EMOCA). Utrecht: NIVEL, 1996.
2. Hallam L. Primary medical care outside normal working hours: review of published work. BMJ 1994; 308(6923): 249-253.
3. Hallam L, Reynolds M. General practice out of hours cooperatives. 24-hour primary care. Oxfordshire: Radcliffe Medical Press, 1999.
4. Dale J, Crouch R, Lloyd D. Primary care: nurse-led telephone triage and advice out of hours. Nursing Standard 1998; 12(47): 41-45.
5. Christensen MB, Olesen F. Out of hours service in Denmark: evaluation five years after reform. BMJ 1998; 316(7143): 1502-1505.
6. Nic Gabhainn S, Murphy A, Kelleher C. A national general practice census: characteristics of rural general practices. Family Practice 2001; 18: 622-626.
7. Cuddy N, Keane A, Murphy A. Married to the job: but at what cost to family life? Forum Journal of the Irish College of General Practitioners) 2002; 19: 14-16.
8. Cuddy NJ, Keane AM, Murphy AW. Rural general practitioners' experience of the provision of out-of-hours care: a qualitative study. British Journal of General Practice 2001; 51(465): 286-290.
9. Hegney P, Fahey P, Nanka A. General practitioners perceptions of after hours primary medical care. Rural and Remote Health 4: 287. (Online) 2004. Available: http://rrh.org.au/journal/article/287 (Accessed 6 September 2004).
10. Salisbury C. Observational study of a general practice out of hours cooperative: measures of activity. BMJ 1997; 314(7075): 182-186.
11. Rousseau N. Rural general practice in the United Kingdom: what is rurality? Report no: 71. London: Royal College of General Practitioners, 1995.
12. Glynn L, Byrne M, Murphy AW. The impact of health status on patient satisfaction with out of hours care provided by a family doctor co-operative. Family Practice 2004 (In press).
13. McKinley R, Manku-Scott T, Hastings A. Reliability and validity of a new measure of patient satisfaction with out of hours primary medical care in the United Kingdom: development of a patient questionnaire. BMJ 1997; 314: 193-198.
14. Lanigan A. Evaluation of the provision of a quality out of hours family doctor service - 'Caredoc' [MBA]. Dublin: University College Dublin; 2000.
15. Nugent A, Black N, Parsons B, Smith S, Murphy AW. A national census of Irish general practice training programme graduates 1990-96. Irish Medical Journal 2003; 96: 10-12.
16. Hays R, Veitch C, Crossland P. Why doctors leave rural practice. Australian Journal of Rural Health 1997; 5: 198-203.
17. Cragg DK, McKinley RK, Roland MO et al. Comparison of out of hours care provided by patients' own general practitioners and commercial deputising services: a randomised controlled trial. I: The process of care. BMJ 1997; 314(7075): 187-189.
18. Devine C. NE Doc Patient Tracking Study: the evaluation of pilot initiatives undertaken in the North Eastern and South Eastern Health Boards on the provision of general practitioner out of hours services in those areas. Dundalk: North Eastern Health Board; 2002.
19. Starfield B. Primary care: balancing health needs, services and technology. Oxford: Oxford University Press; 1998.
20. Wakerman J, Humphreys JS. Rural health: why it matters. Medical Journal of Australia 2002; 176: 457-458.
21. Boynton PM. Administering, analysing, and reporting your questionnaire. BMJ 2004; 328: 1372-1375.

Return to citation



