Chronic health conditions are highly prevalent among Aboriginal and Torres Strait Islander peoples and this places significant strain on patients, their families, communities, and the healthcare system. Recent data demonstrated that 50% of all Aboriginal and Torres Strait Islander people have at least one chronic condition, and chronic disease contributes to 80% of the estimated 11.5-year life expectancy gap between Aboriginal and Torres Strait Islander peoples and other Australians1. Chronic conditions include diabetes, cardiovascular disease, heart failure (HF), renal disease, pulmonary disease and mental illness.
HF is the second leading cause of hospitalisation in Australia2,3. There is a 70% higher prevalence of HF among Aboriginal and Torres Strait Islander peoples than among non-Aboriginal Australians2. Their age-adjusted hospitalisation rates are three times higher and their HF mortality is twice as high as that of non-Aboriginal and Torres Strait Islander people with HF2,3. However, most Aboriginal and Torres Strait Islander people with HF have more than one chronic condition. These data highlight the need for holistic yet individualised approaches1,4,5 in accord with the values of Aboriginal and Torres Strait Islander community health care. HF patients who effectively manage their symptoms through lifestyle modification and adherence to medications have fewer hospitalisations. Nurse-led programs that teach and support self-care have also been shown to reduce hospitalisations[6}.
Although evidence indicates that self-care improves outcomes compared to usual care, 50% of patients experience minimal benefit from these interventions6. The variance in effect on reducing hospital admissions (0-45%)7,8 seems to indicate that 'one size does not fit all'. The variance is undoubtedly partly attributable to differences in patient characteristics. Little is known about factors that distinguish patients who successfully manage their HF self-care from those who do not or which elements of self-care lead to optimal outcomes. Even less is known about HF self-care strategies in Aboriginal and Torres Strait Islander peoples. Research has indicated that Aboriginal and Torres Strait Islander HF patients have significantly lower self-care behaviours (p<0.001)9. Continuous quality improvement programs, such as the Audit and Best Practice for Chronic Disease (ABCD) project, have shown positive results in improving outcomes for chronic disease and implementing evidence-based practice in urban and rural community clinics10.
Fluid management is a key component of symptom monitoring and management for HF patients. Telemonitoring data have shown that signs and symptoms of fluid overload begin around 8 days prior to an emergency hospital admission for acute decompensated HF11. These data suggest that there was sufficient warning time for action and prevention.
Current guidelines recommend patients weigh themselves daily and commence a prescribed fluid management plan if 2 kg over 2 days is gained with associated hand, ankle or abdominal swelling12. Monitoring and managing these simple signs of HF can prevent the deterioration that leads to acute decompensated HF and pulmonary oedema, and can prevent consequent readmission11,13,14.
Self-management programs assisted by information technology and telephone follow-up may assist in the effective management of HF patients. A systematic review and meta-analysis indicated that these programs are highly effective in reducing mortality and hospitalisation and in improving HF knowledge and medication adherence15. The use of tablet computers is one way of providing educational materials to help improve patient care16, and has the potential to be adapted for a range of different conditions and populations.
The educational intervention called Fluid Watchers developed in the USA by Caldwell and colleagues, educates patients about the signs, symptoms, causes and consequences of HF in their self-management and in particular, fluid monitoring by keeping a daily weight record14. The intervention is specifically aimed to reduce the anxiety that many HF patients (especially women) associate with weighing themselves due to adipose weight gain17. The program gives patients an action plan in the case of fluid gain and addresses perceived barriers that would prevent adherence to this action plan. Fluid Watchers has been shown to improve HF knowledge and self-care behaviour in rural patients, and participation in this program has been shown to lead to reduced rates of hospital readmission and mortality among these patients14,18.
Therefore, the purpose of this study was to create a tablet computer-based educational resource, adapted from the Fluid Watchers program to provide culturally safe HF education to Aboriginal and Torres Strait Islander peoples. The two phases of this project aimed to: (1) engage expert HF stakeholders and the local Aboriginal and Torres Strait Islander community healthcare workers and patients to participate in the redesign of existing Fluid Watchers-Pacific Rim HF educational materials to be culturally safe for the local Aboriginal and Torres Strait Islander community and; (2) conduct a feasibility study with a purposeful sample of Aboriginal and Torres Strait Islander HF patients to gather feedback regarding the tools developed to improve HF knowledge and self-care behaviours.
Study design
This study was conducted in two stages utilising a mixed-methods design to create the educational resource and test its feasibility, including action research and pre-intervention/post-intervention knowledge and self-care questionnaires. The first stage was the development of a culturally safe version of Fluid Watchers-Pacific Rim HF educational materials for use on a tablet computer.
Community consent was sought through initial discussions with local elders before initiating the study or contacting participants. Aboriginal and Torres Strait Islander HF patients were sent letters inviting them to participate in the study. The letters stated study objectives and intended outcomes, participant inclusion criteria, a prompt to participate, incentives, notification to receive a call in the next few days and contact details for further information and explanation.
Development of educational resource
Action research methods were used to develop the new resource using materials provided by Fluid Watchers19. Two working groups were established to accomplish this. An expert HF panel, consisting of a cardiologist, an HF nurse practitioner, HF research academics, and a cardiac nurse, Aboriginal researchers and community nurses as well as an IT team provided advice on appropriate modification of the resources. The development of the education resource was conducted using the principles of action research cycles, ie plan, act, observe and reflect.
During the planning phase, the expert panel took the Fluid Watchers resource and proposed modifications to ensure that (1) the curriculum was delivered according to evidence-based guidelines provided by the Australian National Heart Foundation and American Heart Association Self-management Guidelines for patients12,20; (2) the applicability of psychometric tools were appropriate; (3) the language and format was accommodating to Aboriginal and Torres Strait Islander patients' culture and literacy; (4) images and interactivity reflected Aboriginal and Torres Strait Islander culture and gender.
The IT team then actioned ('Act') the proposed modifications into a new Aboriginal and Torres Strait Islander specific resource. The expert panel then reviewed the modifications ('Observe') and proposed further modifications. Case notes were kept during the development stage for subsequent analysis. This was repeated through two cycles.
The resource was then taken to a broader group of stakeholders consisting of representatives including university and medical researchers, staff from the Aboriginal and Torres Strait Islander medical service, technology developers and two Aboriginal and Torres Strait Islander HF patients. This was a key component of the reflection stage of action research. Bringing in Aboriginal and Torres Strait Islander medical staff and HF patients allowed for questions relating to cultural appropriateness and shared understanding to be addressed. The outcomes of these discussions were also fed back into the resource development to reach the final product.
The Fluid Watchers program included an illustrated PowerPoint presentation featuring a HF patient (male or female, whichever the patient chose) and patient diary for adaptation. The larger stakeholder group alongside the expert panel prepared the adaptations and gave feedback verbally, in written or electronic form. Information collected was integrated to produce the next version of the teaching tool. Specific feedback regarding illustrations of Aboriginal body shape, facial features, choice of clothing, colours, skin tone and environment were communicated to the graphic designer.
Feasibility and acceptability testing
The second stage involved pilot-testing the feasibility and acceptability of the newly designed resource with a group of HF patients based at an Aboriginal and Torres Strait Islander medical service in central Ipswich, Queensland, Australia. To be included in the feasibility study participants had to be of Aboriginal or Torres Strait Islander descent, aged over 18 years and have a clinical diagnosis with NYHA function class II-IV symptoms. Potential participants were excluded if they were a resident of a nursing home or institution as these patients generally do not perform self-care.
Eligible participants identified by the Aboriginal healthcare worker were introduced to the researcher. An Aboriginal researcher explained to the HF patients the purpose of the study; an Aboriginal themed diary for recording daily observations and a Heart Foundation 'Living each day with my heart failure' booklet was given to each patient in appreciation for their time and contribution.
Intervention
Prior to viewing the resource, participants completed questionnaires on their knowledge of heart failure and self-management behaviours. Participants then spent approximately one hour trialling and reviewing the resource. After this, they had one attempt to complete the knowledge and self-management questionnaires again as well as a satisfaction survey related to their experience with the resource.
Instruments
Three validated questionnaires were used in this study to evaluate Aboriginal HF patients' knowledge, self-management behaviour and satisfaction levels with receiving education via the adapted Fluid Watchers program. All questionnaires were embedded in the program and appropriate permission to use the questionnaires was obtained from each of the original authors. Patients answered the questionnaires by touching their answers on the tablet computer. An HF knowledge questionnaire14 and Self-Care Heart Failure Index (SCHFI) V6.2 questionnaire21 were used as pre- and post-intervention measures. Aboriginal HF patients' satisfaction level with the program and its contents was measured by a satisfaction survey22 adapted for heart failure. All questionnaires were converted into plain, conversational language as advised by the Aboriginal and Torres Strait Islander members of the expert panel. A consistent layout with large text and images was used wherever feasible.
Examples of content adaptation of the questionnaires included 'Symptoms are vague or come on gradually' being changed to 'I feel this (symptom) all the time or don't notice a change', 'Overall how do you feel about keeping yourself free of heart failure symptoms?' being changed to 'Do you feel you can look after you, so that your heart failure doesn't give you trouble?' and 'How quickly did you recognise it as a symptom of heart failure?' changed to 'When did you know it (the symptom) was because of your heart failure?'.
Heart failure knowledge
The questions for assessing HF knowledge were initially developed based on the Rapid Early Action for Coronary Treatment (REACT) study in the acute myocardial infarction population23. The questionnaire was modified for an HF population14,19 and content validity of the modified questionnaire was established by HF experts. Internal consistency and reliability for the modified questionnaire was 0.8314. The modified HF knowledge questionnaire covered basic HF physiology, recognition of HF signs and symptoms and barriers to seeking care14. The 20-item questionnaire allowed patients to choose what they perceive as the correct answer from multiple choice, yes/no or true/false options. In this survey, the correct answer for each question accrued one point (the wrong answer has zero points). Therefore, the questionnaire had a minimum score of 0 and a maximum score of 20 points14.
Self-Care Heart Failure Index (SCHFI)
Self-management behaviours were measured using the Self-Care Heart Failure Index (SCHFI) v6.2 questionnaire21. The SCHFI evaluates patient self-management behaviour by assessing the following skills: frequency of self-care behaviours such as daily weighing, physical activity, medication concordance (maintenance), ability to confidently manage HF (confidence) and ability to evaluate the importance of symptoms, recognise changes in health status, take required actions to relieve symptoms and evaluate the effectiveness of self-management and treatment (management). Each of these components has been tested for reliability (Maintenance: coefficient alpha=0.553, Confidence: coefficient alpha=0.827 and Management: coefficient alpha=0.597)21. Scores for maintenance, confidence and management were calculated in accordance with the authors' instructions21. Patients with higher scores are considered to have a greater ability to self-manage.
Satisfaction survey
To examine the level of satisfaction with receiving education via the adapted Fluid Watchers program, a satisfaction survey was administered following exposure. This survey evaluated the ease of navigation and useability of the resource. A previously validated satisfaction survey22 that determined participant satisfaction for receiving health care via telephone interaction was modified to be appropriate for the tablet computer-based program. The finalised questionnaire included 29 items with a 5-point Likert scale (1=strongly disagree, to 5=strongly agree). Open-ended questions were also asked to collect qualitative data on acceptance, comprehension and impact of the program.
Data analysis
Microsoft Excel 2010 was used to collate and analyse data. To describe the process of resource development, summaries of field notes were used and data were reported according to the method proposed by Huberman and colleagues (1994) to identify emerging patterns and themes24.
Quantitative data are reported using descriptive statistics, including means (standard deviations). Due to the small sample size, statistical comparisons for the pre- and post- knowledge and SCHFI questionnaires were not performed.
Ethics approval
The Queensland University of Technology University Human Research Ethics Committee approved the study (No. 1300000079), and written, informed consent was provided by all participants.
Stakeholder feedback
Two main themes emerged from stakeholder feedback while adapting materials for Aboriginal patients: identity and comprehension. Identity was an important concept to portray in the new teaching tools. Stakeholders felt that illustrations should accurately reflect Aboriginal people of the same gender as the patient and from the local community. Feedback was given to alter the skin tone, choice of clothing, facial features and body shape of original illustrations and the program was voiced by members of the local Aboriginal community. The environment in which the Aboriginal people appeared was also important and was changed to reflect one to which the community could relate. Finally, symbolism was added to reflect the Aboriginal cultures. Reviewers saw symbolism as necessary to reflect identity, and Aboriginal flags were featured where possible, and text and background colours changed to represent those of the flags (Fig1).
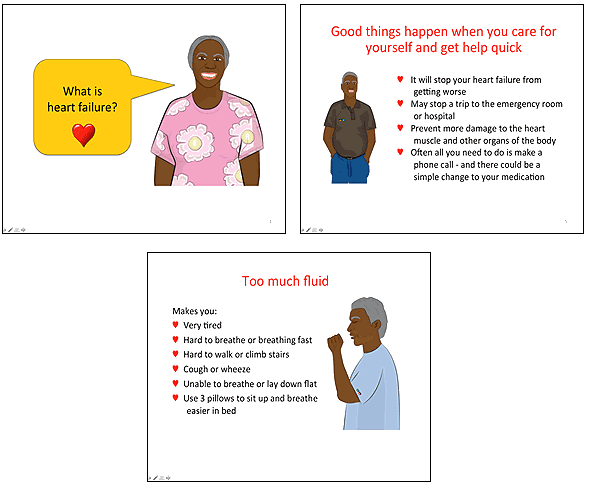
Figure 1: Examples of slides from the patient education material for the tablet computer.
Comprehension was also a theme that emerged to be of importance to stakeholders. Reviewers considered it important that illustrations be created to portray an action; for example, additional fluid accumulation in the abdominal region was illustrated by a man having difficulty doing up his belt. Images complemented text and provided another aid to dependence upon reading ability, and text was converted into plain language. Researchers also changed the tense of language; in most instances first person was used so as to closely identify with the person reading it. For example, in a questionnaire, the original wording 'A primary cause for symptoms of heart failure is too much fluid' was changed to 'Too much fluid in my body causes heart failure'. Acronyms were removed and complex nouns and verbs were replaced with simple descriptive language. Simplifying language therefore occurred in this manner within the PowerPoint slides and questionnaires, and illustrations were developed to aid comprehension.
IT experts constructed the technology interface with the following additional features: simple animated anatomy and physiology to teach concepts of the normal heart and HF; voice-over presented by members of the local Aboriginal community; user-friendly interface; simultaneous login; secure method of data retrieval and analysis to retrieve patient responses with a shortcut key to provide ease of searching and data categorisation; and secure settings for patient confidentiality with data unable to be accessed in the public domain.
Patient feedback
Participants: The Aboriginal medical clinic patient database produced a list of 11 potential participants. Five of these patients agreed to participate in the program and the other six declined to participate due to an inability to commit the time to the project. All five participants who trialled the program were Aboriginal people, born in Australia and spoke English as their primary language. The mean age of participants was 61.6±10.0 years. Three participants had an NYHA classification of Class III and two participants had a classification of Class IV.
Acceptance: Two participants (female) expressed having enjoyed their experience, stating 'I liked it all' that the teaching tool was 'good' and they 'enjoyed it'. One patient (male, NYHA Class IV) became tired during the program and at the end stated that overall 'it was all right'. Another (male) appreciated the concept of providing information via this teaching method stating, 'That is a good idea, instead of just talking or asking about it, the iPad just tells you.'
All five participants had never used a tablet computer before. One person (female) described the experience as having initially made her nervous - 'At first I was scared' but then reflected that she found the experience 'enjoyable'. Another participant (male) reflected upon the teaching tool as 'simply moving with technological advancements', stating that 'We need to keep up'. Most participants used the tablet computer touch screen with ease; however, one participant (male) had repeated difficulty utilising a gentle touch and stated that it was not easy to use the touch screen. Another participant (female) stated that the general organisation of the teaching materials was easy to navigate from the home screen and that the video was 'very helpful'.
When asked, all participants agreed they would use this teaching tool on the occasion they visit the AMS. Three participants (two female, one male) stated they would like to use the teaching tool to refresh their knowledge in the future, stating 'I would use that again', 'I would like to watch it again' and 'I would use something like that again'.
Comprehension: Participants commented that the teaching tool was very easy to understand with 'no big words' (female), and another (male) noting that the message was 'not complicated with jargon'. Another (female) stated that before they did not know much about their HF, but 'seeing that really did make me realise'. From this, it appears that participants were able to comprehend the information presented.
Impact: When referring to the overall message, one participant stated 'This is something I will never forget'. One patient stated that exposure to the messages of the teaching tool 'came at a good time' and described having begun a health overhaul in the new year by participating in a local walking group, and eating more fresh fruit and vegetables.
One participant was particularly motivated after participating, stating 'It's now up to me to do this'. This participant returned to the clinic later in the day to show the research team alternative low-salt items they had purchased.
HF knowledge and SCHFI
There was a 20.8% increase in HF knowledge (Table 1) with the percentage of correct responses increasing from 48.0±6.7% to 58.0±9.7%.
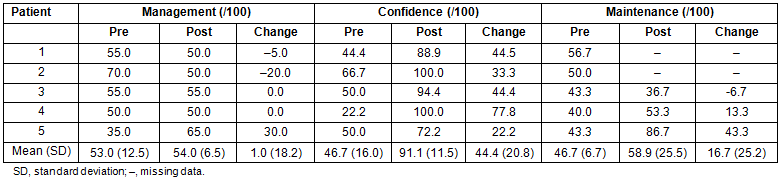
The results of the SCHFI questionnaire are described in Table 2. Despite the intervention and survey completion only taking 60 minutes two participants did not complete the follow-up questions on this survey related to maintenance as they became too fatigued to finish the questionnaire. Of the three participants that did complete this section there was a 26.1% increase in maintenance score (from 46.7±6.7 to 58.9±25.5 possible range 0-100). All five respondents completed the management and confidence questions and there was a 1.9% increase in management (from 53.0±12.5 to 54.0±6.5 possible range 0-100) and a 95.1% increase in confidence (from 46.7±16.0 to 91.1±11.5 possible range 0-100).
Table 1: Changes in heart failure knowledge score (out of a possible 20) for each participant
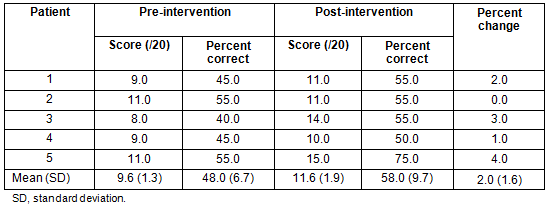
Table 2: Changes in Self-Care Heart Failure Index (SCHFI) questionnaire; possible range for scores was 0-100
Satisfaction
Participant satisfaction was 83.0% (Fig2). Greatest satisfaction was with the inbuilt video demonstration and in having questions answered. All participants indicated a willingness to adopt lifestyle changes (daily weighing) and endorse its use to educate others with HF.
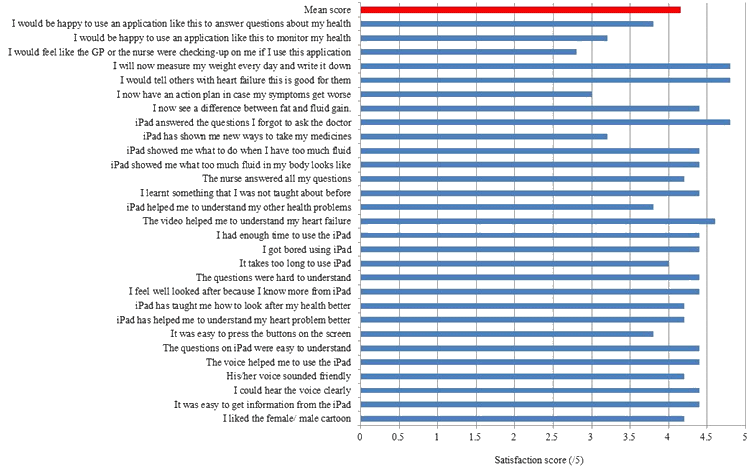
Figure 2: Results of patient satisfaction with the resource. Participants were asked to rate each statement out of 5:
1=strongly disagree, 2=disagree, 3=do not agree or disagree, 4=agree and 5=strongly agree. Where questions were negative, scores were reversed.
Discussion
The results of the present study demonstrate that by working in collaboration with HF experts, Aboriginal researchers and patients, a culturally safe HF resource has been developed for Aboriginal and Torres Strait Islander patients. Engaging Aboriginal researchers, capacity-building, and being responsive to local systems and structures enabled this research to be successfully completed with the Aboriginal community, and the positive participant feedback shows that the methodology used in this study was appropriate and acceptable; participants were able to engage with willingness and confidence.
Currently, limited information is available on health promotion using a tablet or computer that has been developed specifically for Aboriginal and Torres Strait Islander people with HF. Participants rated their satisfaction with the program at 83%. They commented that the information was easy to comprehend and all endorsed its use to educate others with HF. Previous researchers have expressed that existing teaching resources for Aboriginal and Torres Strait Islander peoples' HF self-management are unsuitable, and practical self-care teaching resources are needed with key messages communicated simply and visually25. The stakeholder group emphasised that health promotion pictures and messages shouldbe contemporary and reflective of Aboriginal and Torres Strait Islander communities in the modern setting26.
Community organisations are viewed as vehicles for enhancing social connection and cultural expression among Aboriginal and Torres Strait Islander peoples27. The waiting room of an Aboriginal medical clinic has previously been described as creating opportunity for valued and important aspects of daily life to take place - sharing health information and spending time with friends and family28. During feedback time, all participants agreed they would be happy to use the tool upon subsequent visits to the clinic. Although all participants had never used a tablet computer, most became familiar and confident in using it during the trial and only one participant displayed limited dexterity while using the touch screen. Utilisation rates of internet-based programs are low among some Aboriginal and Torres Strait Islander communities with a notable 'digital divide'29. One participant stated that few persons of his generation used this type of technology on a daily basis; however, all agreed that they would be happy to refresh their knowledge using the technology upon visits to the clinic.
Use of touch-screen technology can therefore be regarded as an alternative (or substitute) way of presenting health information to more conventional mechanisms such as verbal advice, posters, leaflets and books in the appropriate healthcare provider setting29. The education tool has the potential to assist health professionals to provide a more positive experience for Aboriginal and Torres Strait Islander patients with HF through cultural recognition and consideration. After receiving the education, participants verbally expressed motivation to implement lifestyle changes and expressed gratitude; one participant positively stated 'This is something I will never forget'. Most notably, participants had greater self-efficacy, showing a measurable improvement of 95.1% in confidence to ably manage their symptoms.
Other studies that have measured changes in knowledge and self-care in Australian HF patients have shown similar results to the present study. Boyde and colleagues (2013) demonstrated improvements in HF knowledge (14% increase) as measured by the Dutch Heart Failure Knowledge Scale and increases in SCHFI maintenance (7% increase), management (28% increase) and confidence (11% increase)30. In addition, Caldwell and colleagues (2005) demonstrated a similar (3-point) improvement in HF knowledge over 3 months along with significant improvements in self-care behaviour14.
Limitations and future directions
As this was a pilot program, the number of participants was not sufficient to allow for the determination of statistically significant differences. The small number of participants was due to the use of one clinic for recruitment. Instead, the results support the need for further research, with participant numbers that allow for greater analysis of effect. Future studies will seek to recruit a greater number of participants.
Notwithstanding this limitation, it has been reported that changes in the SCHFI of ≥0.5 of a standard deviation maybe considered clinically relevant21 and thus scores on maintenance and confidence show improvements over and above 0.5 of the standard deviation and could be considered as clinically relevant, but this needs to be explored further in a larger population.
In addition, it is not known whether the results of this study will be transferable to the wider community, which may have different levels of literacy.
Results may not necessarily equate to longer-term behaviour change or reduced hospital admissions. Prolonged effects were not measured as post-test questionnaires were distributed immediately after the education session19,30.
Further adaptations may be required for different Aboriginal and Torres Strait Islander communities. In this case, it should utilise an Aboriginal and Torres Strait Islander Reference Group from the community for which they are developing the resource. The findings support the need for future studies with longer follow-up time14 in a larger cohort with administrative blinding to measure longer-term behaviour change and the effect on clinical outcomes, including quality of life, hospitalisations and healthcare utilisation.
This project utilised a mixed-methods design to adapt and evaluate educational tools for Aboriginal and Torres Strait Islander HF patients that incorporated interactive voice-over and visual aids into a tablet computer-based resource. Consistent with previous studies in non-Aboriginal populations, favourable trends were observed in knowledge and self-care and participants expressed a high level of satisfaction with the resources. Further research is required to measure long-term behavioural change and effects on hospital admissions. Additional adaptation may be required for it to be transferable to other Aboriginal and Torres Strait Islander communities.
Acknowledgements
The research team would like to thank the following individuals: Vikki Blacka, Noel Hicks and Kay Mundraby for their input and fabulous voices for the app; Dr Johannes Moolman, Chris Horton and Nazli Bashi for their clinical heart failure expertise and research support.
References
1. Australian Institute of Health and Welfare. Life expectancy and mortality of Aboriginal and Torres Strait Islander people. Canberra: Australian Institute of Health and Welfare, 2011.
2. Australian Institute of Health and Welfare. Cardiovascular disease: Australian facts. Canberra: Australian Institute of Health and Welfare, 2011.
3. Woods JA, Katzenellenbogen JM, Davidson PM, Thompson SC. Heart failure among Indigenous Australians: a systematic review. BMC Cardiovascular Disorders 2012; 12(1): 99.
4. Australian Health Ministers' Advisory Council. Aboriginal and Torres Strait Islander Health Performance framework report. Canberra: Australian Health Ministers' Advisory Council, 2010.
5. Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander People: an overview. Canberra: Australian Institute of Health and Welfare, 2011.
6. Riegel B, Moser DK, Anker SD, Appel LJ, Dunbar SB, Grady KL, et al. State of the science promoting self-care in persons with heart failure: a scientific statement from the American Heart Association. Circulation 2009; 120(12): 1141-1163.
7. Riegel B, Carlson B, Glaser D, Romero T. Randomized controlled trial of telephone case management in Hispanics of Mexican origin with heart failure. Journal of Cardiac Failure 2006; 12(3): 211-219.
8. Stewart S, Marley JE, Horowitz JD. Effects of a multidisciplinary, home-based intervention on planned readmissions and survival among patients with chronic congestive heart failure: a randomised controlled study. The Lancet 1999; 354(9184): 1077-1083.
9. Schnell-Hoehn KN, Naimark BJ, Tate RB. Determinants of self-care behaviors in community-dwelling patients with heart failure. Journal of Cardiovascular Nursing 2009; 24(1): 40-47.
10. Si D, Bailie R, Cunningham J, Robinson G, Dowden M, Stewart A, et al. Describing and analysing primary health care system support for chronic illness care in Indigenous communities in Australia's Northern Territory - use of the Chronic Care Model. BMC Health Services Research 2008; 8(1): 112.
11. Spaeder J, Najjar SS, Gerstenblith G, Hefter G, Kern L, Palmer JG, et al. Rapid titration of carvedilol in patients with congestive heart failure: a randomized trial of automated telemedicine versus frequent outpatient clinic visits. American Heart Journal 2006; 151(4): 844, e841-844, e810.
12. National Heart Foundation of Australia. Living well with chronic heart failure: a guide for patients and their families (Online) 2008. Available: http://www.heartfoundation.org.au/SiteCollectionDocuments/Living-well-with-chronic-heart-failure.pdf (Accessed 8 May 2014).
13. Jaarsma T, Halfens R, Abu-Saad HH, Dracup K, Gorgels T, Van Ree J, et al. Effects of education and support on self-care and resource utilization in patients with heart failure. European Heart Journal 1999; 20(9): 673-682.
14. Caldwell MA, Peters KJ, Dracup KA. A simplified education program improves knowledge, self-care behavior, and disease severity in heart failure patients in rural settings. American Heart Journal 2005; 150(5): 983, e987-983, e912.
15. Inglis S. Structured telephone support or telemonitoring programmes for patients with chronic heart failure. Journal of Evidence-Based Medicine 2010; 3(4): 228-228.
16. Suhling H, Rademacher J, Zinowsky I, Fuge J, Greer M, Warnecke G, et al. Conventional vs. tablet computer-based patient education following lung transplantation-a randomized controlled trial. PloS One. 2014; 9(3): e90828.
17. Riegel B, Carlson B. Facilitators and barriers to heart failure self-care. Patient Education and Counseling. 2002; 46(4): 287-295.
18. Dracup K, Moser DK, Pelter MM, Nesbitt T, Southard J, Paul SM, et al. A randomized controlled trial to improve self-care in patients with heart failure living in rural areas. Circulation 2014; 130(3): 256-264.
19. Howie J, Banks A, Caldwell MA, Dracup K. A pilot educational intervention improves knowledge of symptoms of heart failure. American Journal of Critical Care 2003; 12(3): 278.
20. Adams K, Lindenfeld J, Arnold JMO, Baker D, Barnard D, Baughman K, et al. HFSA 2006 comprehensive heart failure practice guideline. Journal of Cardiac Failure 2006; 12(1): e86-e103.
21. Riegel B, Lee CS, Dickson VV, Carlson B. An update on the self-care of heart failure index. The Journal of Cardiovascular Nursing 2009; 24(6): 485.
22. Clark RA, Yallop JJ, Piterman L, Croucher J, Tonkin A, Stewart S, et al. Adherence, adaptation and acceptance of elderly chronic heart failure patients to receiving healthcare via telephone?monitoring. European Journal of Heart Failure 2007; 9(11): 1104-1111.
23. Simons-Morton DG, Goff DC, Osganian S, Goldberg RJ, Raczynski JM, Finnegan JR, et al. Rapid early action for coronary treatment: rationale, design, and baseline characteristics. Academic Emergency Medicine 1998; 5(7): 726-738.
24. Miles MB, Huberman AM. Data management and analysis methods. In: NK Denzin, YS Lincoln (Eds) Handbook of qualitative research. Thousand Oaks: Sage Publications, 1994; 428-444.
25. Kowanko I, Helps Y, Harvey P, Battersby M, McCurry B, Carbine R, et al. Chronic condition management strategies in Aboriginal communities. Flinders University and the Aboriginal Health Council of South Australia, Adelaide: 2012.
26. Baunach E, Lines D, Pedwell B, Lange F, Cooney R, Taylor HR. The development of culturally safe and relevant health promotion resources for effective trachoma elimination in remote Aboriginal communities. Aboriginal & Islander Health Worker Journal 2012; 36(2): 9-11, 16, 19.
27. Reilly RE, Doyle J, Bretherton D, Rowley KG, Harvey JL, Briggs P, et al. Identifying psychosocial mediators of health amongst Indigenous Australians for the Heart Health Project. Ethnicity & Health 2008; 13(4): 351-373.
28. Jowsey T, Yen L, Ward N, McNab J, Aspin C, Usherwood T, et al. It hinges on the door: time, spaces and identity in Australian Aboriginal health services. Health Sociology Review 2012; 21(2): 196-207.
29. Doessel DP, Travers H, Hunter E. The use of touch-screen technology for health?related information in Indigenous communities: some economic issues 1. Prometheus 2007; 25(4): 373-392.
30. Boyde M, Song S, Peters R, Turner C, Thompson DR, Stewart S. Pilot testing of a self-care education intervention for patients with heart failure. European Journal of Cardiovascular Nursing 2013; 12(1): 39-46.


