There are two potential benefits to developing rural EM rotations. Emergency medicine (EM) workforce studies show low rates of board-certified/residency-trained emergency physicians practising in rural emergency departments (EDs) in the USA1. There is some evidence to suggest rural ED rotations for EM residents may lead to increased numbers of residency-trained EM providers in rural areas2. Additionally, because half of all US EDs see less than 19 000 patients annually and most residents do not practice in a tertiary care facility after completion of residency, there may be additional benefit to training in a low-resource environment such as a rural ED3. Despite these potential benefits, only 5% of all US EM residencies have a required rural EM rotation, and even amongst these programs it is often only a small part of the clinical curriculum4.
From a purely clinical standpoint, there are reasonable concerns that limit the expansion of rural EM rotations. Emergent and lifesaving procedures are an important aspect of EM practice, and becoming well trained at performing these procedures is a concern of many residents and faculty. The practice of emergency medicine is also focused on identifying and treating a wide variety of life-threatening conditions, often referred to as critical diagnoses. Perhaps the strongest argument against rural EM rotations centers on decreased procedural opportunities and lower rates of critical diagnoses. There is, therefore, a balance between providing adequate rural EM exposure during residency to realize the potential benefits and the concern of providing adequate exposure to procedures and critical diagnoses.
The current literature contains only one single-residency study that provides a procedural experience and patient acuity comparison between metropolitan and rural EDs; this study showed similar procedure frequency but overall lower patient acuity at rural sites5. The purpose of this study is to utilize the Agency for Healthcare Research and Quality (AHRQ) Nationwide Emergency Department Sample (NEDS)6 to compare the rates of selected procedures and critical diagnoses at rural and metropolitan EDs in the US. This information may also be useful for EM residency programs as they evaluate the potential procedural experiences available within rural EM rotations. The results of this analysis should provide a generalizable comparison of the clinical experiences within rural and metropolitan EDs.
This study utilized Nationwide Emergency Department Sample (NEDS) data for the year 2006. NEDS is a database managed by the Healthcare Cost and Utilization Project (HCUP) and sponsored by the Agency for Healthcare Research and Quality6. The AHRQ NEDS database contains ED visit records from 958 hospitals and approximates a 20% stratified sample of US hospital-based EDs6. Procedures and critical diagnoses were selected based on Accreditation Council for Graduate Medical Education procedural guidelines and the American College of Emergency Physicians' Model of the Clinical Practice of Emergency Medicine. Procedures and diagnoses were identified in the NEDS database by International Classification of Diseases (9th revision) code or Current Procedural Terminology code. The rates of these selected procedures and critical diagnoses are compared between two categories: the metropolitan category includes hospitals that are in counties defined as large metropolitan or small metropolitan; the rural category includes hospitals that are in counties defined as micropolitan or non-metropolitan. These designations were based on the population size of the county in which the hospital-based ED was located. Large metropolitan counties had a population of at least 1 million residents, small metropolitan counties had a population of less than 1 million residents, micropolitan counties were areas with an urban core of at least 10 000 people but less than 50 000 total population and rural counties had less than 10 000 residents6. It is assumed that a hospital in a micropolitan county would have resources more consistent with a rural ED than one in a metropolitan or urban center.
By using the discharge weights provided in this dataset, the authors computed nationally representative estimates of the percentage of procedures or critical diagnoses occurring in metropolitan and rural hospitals based on the total number visits in these locations. In order to assess the variability between the hospitals in this sample, unweighted rates for each hospital were also calculated. These rates of procedures and critical diagnoses were then compared between metropolitan and rural hospitals by using Wilcoxon rank sum tests. The medians and interquartile ranges (25th and 75th percentiles) for these rates are reported for the rural and metropolitan hospitals. All analyses were performed using Statistical Analysis Software v9.2 (SAS Institute; http://www.sas.com).
Ethics approval
This project was reviewed by the authors' Institutional Review Board and a non-human subject research determination was made for this work.
Procedure rates were identified and calculated based upon the total number of visits to rural EDs (22 766 219) and metropolitan EDs (97 267 531) (Table 1). The percentage of procedures occurring per total visits was lower in the rural ED group for every procedure that was measured. There was a greater difference for some procedures than for others. The rate of procedures was about twice as great in metropolitan EDs as compared to rural EDs for the following procedures: fracture reduction, chest tube thoracostomy and intubations. Other procedures had a greater difference in rate of occurrence, such as cricothyrotomy, lumbar puncture, pericardiocentesis and thoracotomy. As a percentage of total visits, performance of procedures in rural EDs occurred about half as frequently as in metropolitan EDs.
The Wilcoxon rank sum tests showed a greater disparity of procedures in rural as compared to metropolitan hospitals throughout all procedures measured when looking at the median percentage of procedures per total number of visits. For some of the procedures, such as cricothyrotomy, pericardiocentesis and thoracotomy, there was a 0.000% occurrence for the median. The median of any procedure being performed at a rural hospital was 0.370% as compared to 1.166% in a metropolitan hospital.
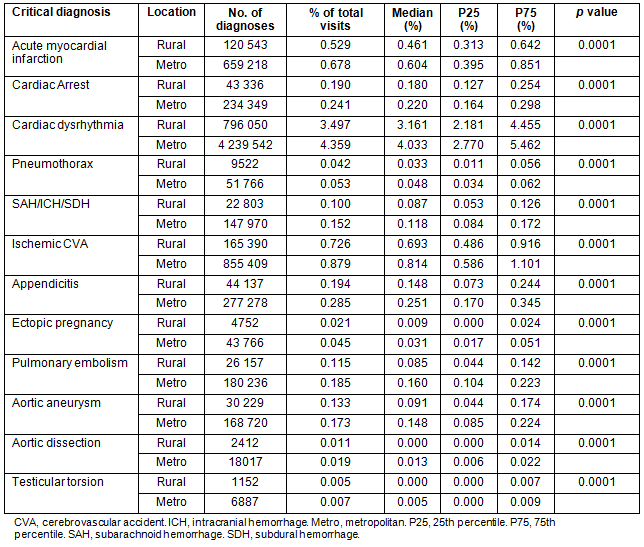
The rates of critical diagnoses in rural versus metropolitan EDs can be seen in Table 2. As with procedures, the rate of critical diagnoses was less in the rural ED group than in the metropolitan ED group; however, the difference was not as great. Diagnoses that had more similar rates included acute myocardial infarction; cardiac arrest; pneumothorax; subarachnoid, intracranial or subdural hemorrhage; acute ischemic cerebrovascular accident; pulmonary embolism; aortic aneurysm; aortic dissection and testicular torsion. Select diagnoses such as cardiac dysrhythmia, ectopic pregnancy and appendicitis appeared to be found less frequently in the rural environment compared to the metropolitan.
The Wilcoxon rank sum tests showed that the rates of diagnoses were significantly lower in the rural environment as compared to the metropolitan; however, the magnitude of the differences in the medians was not necessarily as great for diagnoses such as acute myocardial infarction, cardiac arrest, pneumothorax, subarachnoid, intracranial or subdural hemorrhage and ischemic cerebrovascular accident. When the median was examined the diagnoses of pulmonary embolism, aortic aneurysm, aortic dissection and testicular torsion were found to occur less frequently in the rural setting. Cardiac dysrhythmia, appendicitis and ectopic pregnancy occurred much less frequently in the rural environment than in the metropolitan setting.
Table 1: Procedure rates described as a percentage of total visits to rural (n=22 766 219) and metropolitan (n=97 267 531) emergency departments
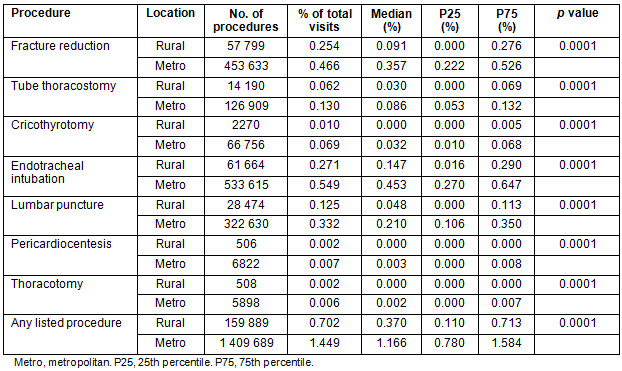
Table 2: Critical diagnosis rates described as a percentage of total visits to rural (n=22 766 219) and metropolitan (n=97 267 531) emergency departments
Discussion
One previous single-site study showed that procedure frequencies were similar in metropolitan and rural EDs, whereas the results of the present study, based on a national representative sample, demonstrate a lower rate of procedures in rural EDs when compared to metropolitan EDs5. This was true for each individual procedure and for the likelihood of any procedure being performed. While each procedure was less likely to occur in the rural setting there were some that occurred hardly at all, including thoracotomy, pericardiocentesis and cricothyrotomy. The rates of diagnoses are more similar, but are still lower in rural EDs, as a recent study has shown3.
Even though procedure rates are lower in the rural ED there is still utility in training residents in a rural environment. The rates may be higher for some procedures in the metropolitan ED but this does not imply that every procedure being done in the ED is performed by an ED physician. For example, if one were to consider fracture reductions the study data showed they occur less frequently in the rural ED; however, in the rural environment the EM resident would have the opportunity to perform this procedure, as opposed to the orthopedic attending or resident who may be consulted to perform the reduction in a metropolitan tertiary care hospital. The same assumption could be extrapolated to chest tube thoracostomy, cricothyrotomy and chest thoracotomy if a surgery or trauma service is present in the metropolitan ED. The assumption that there is a greater reliance on consultant services to perform procedures in larger EDs where their services are more readily available is difficult to quantify. However, a resident training in the rural ED would likely be the sole proceduralist which would provide the opportunity to perform procedures they may not otherwise have in a larger metropolitan ED.
Increasing the academic presence, such as incorporation of a rural EM rotation for residents, in a rural ED may also increase the number and variety of procedures performed at that institution. According to the present study's data, certain procedures such as thoracotomy, pericardiocentesis and cricothyrotomy were never performed in rural EDs. This may have been because there is limited subspecialist availability to manage the disease process once the procedure has been performed. However, it could also be a reflection of a lack of operator confidence or desire to perform these relatively rare procedures. Thoracotomy should arguably not be performed if a cardiothoracic surgeon is not closely available; however, pericardiocentesis and cricothyrotomy are lifesaving procedures. These procedures could be performed if the operator was skilled and the ED had ready access to safe transport to a higher level of care.
The rates of diagnoses were more similar but still lower in rural EDs when compared to a recent study3. Nevertheless, one could assume that encountering one of these critical diagnoses in a rural ED and determining the appropriate management and disposition or transfer would provide a unique learning opportunity for an EM physician in training. The management of an acute myocardial infarction in the rural ED may give the resident a unique opportunity to administer thrombolytics and receive a high-yield educational experience. This has potential benefits for trainees when compared to a typical metropolitan center experience where such encounters usually result in catheterization lab activations and ED physician involvement consists mostly of electrocardiogram interpretation. Resident physicians may choose to practise at a facility that may not be rural by definition but does not have select specialty services such as a catheterization lab or trauma service. Training in a rural ED would prepare future EM physicians for situations when they may not have certain resources available.
Limitations
Even though the NEDS database has a very large sample size it is limited to 24 US states and may not represent the particular location of an individual location if the state was not included in the data collection. However, because of this large sample size and the sampling approach used the results can most likely be generalized to any rural location throughout the USA. Additionally, the use of the sampling weights allows one to produce national estimates that represent ED usage nationwide7. The applicability this database may also not be reflective of or generalizable to EDs outside the USA.
The classification system used in the NEDS database to delineate metropolitan, micropolitan and rural is a standard also used by the US Census Bureau. This system classifies its categories at the county level based on population, not by particular hospital size. It is most likely that hospitals in the micropolitan and rural categories have resources consistent with a rural ED based upon county population size; however, there is probably a small degree of uncertainty to this assumption.
In the NEDS data used in this study, the data is sorted based on hospital size and not hospital characteristic, such as a level I or II trauma center. Trauma centers would almost always be categorized as metropolitan in the population-based categories and would significantly influence the rates of particular procedures measured in this study. However, a residency training program may be located at a hospital that would be classified as metropolitan but may not have a trauma center designation. These locations may not have as great a contrast in their procedural exposure as suggested by the classifications of rural versus metropolitan used in this study.
Statistically significant differences were noted between the rural and metropolitan EDs in the rates of the various procedures and diagnoses. To a certain extent this reflects the rather large number of hospitals in each group. It is probably of greater importance to focus on the magnitude and distribution of the rates within these ED environments.
Based upon analysis of the NEDS database, the rates of procedures and critical diagnoses appear to be lower in rural versus metropolitan medical centers. The reduced number of procedures and critical diagnoses supports the concern that residents receiving a substantial portion of training in rural EDs may not have sufficient experience with certain procedures or clinical scenarios. However, training EM residents in rural EDs may still provide a high-yield educational experience through increased autonomy, potential for limited practice resources and the need to determine disposition to a higher level of care. Incorporating rural EM training into residency curriculum may lead to an increase in EM trained physicians practicing in the rural environment which may lead to an increased incidence of procedures that are currently infrequent.
This information may be useful for EM residency programs as they evaluate the potential procedural experiences available within rural EM rotations. The impact of a longer rotation in a rural ED on overall procedural competency and clinical experience cannot, however, be extrapolated. Further study is required to quantify this effect. Prospective collection of data from actual rural ED rotations through EM resident logbooks could better quantify the rates of these selected procedures and critical diagnoses.
References
1. Ginde AA, Sullivan AF, Camargo CA, Jr. National study of the emergency physician workforce, 2008. Annals of Emergency Medicine 2009; 54(3): 349-359.
2. Tavernier LA, Connor PD, Gates D, Wan JY. Does exposure to medically underserved areas during training influence eventual choice of practice location? Medical Education 2003; 37(4): 299-304.
3. Muelleman RL, Sullivan AF, Espinola JA, Ginde AA, Wadman MC, Camargo CA, Jr. Distribution of emergency departments according to annual visit volume and urban-rural status: implications for access and staffing. Academic Emergency Medicine 2010; 17(12): 1390-1397.
4. Talley BE, Ann Moore S, Camargo CA, Jr., Rogers J, Ginde AA. Availability and potential effect of rural rotations in emergency medicine residency programs. Academic Emergency Medicine 2011; 18(3): 297-300.
5. Wadman MC, Fago B, Hoffman LH, Tran TP, Muelleman RL. A comparison of emergency medicine resident clinical experience in a rural versus urban emergency department. Rural Remote Health 10(2): 1442. (Online) 2010. Available: www.rrh.org.au (Accessed 20 June 2011).
6. Agency for Healthcare Quality and Research. Overview of the National Emergency Department Sample (NEDS). (Online) 2006. Available: http://www.hcup-us.ahrq.gov/nedsoverview.jsp (Accessed 20 June 2011).
7. Agency for Healthcare Quality and Research. Introduction to the HCUP Nationwide Emergency Department Sample (NEDS), 2006. (Online) 2010. Available: http://www.hcup-us.ahrq.gov/db/nation/neds/NEDS_Introduction_2006v2.jsp (Accessed 20 June 2011).
