Following the delivery of a child, women are vulnerable to a number of serious health risks (eg infections, depression)1. Because of these risks, new mothers in Asia, Africa, and some European countries remain in hospitals at least 1 week2. American mothers, on average, remain in hospital for only 2.6 days following delivery. This short stay following delivery has raised concerns that it may contribute to conditions such as postpartum complications and mental disorders that subsequently lead to rehospitalizations or even deaths3-5.
Research indicates that post-partum problems resulting in hospitalization (ie rehospitalizations) result in considerable, potentially avoidable, spending by payers (insurance companies)6. Olsen et al. reported that the attributable total hospital cost of a surgical site infection after a cesarean section (C-section) was approximately $35297. Qasim and Andrews also found that average cost per stay involving a C-section procedure was $5400 for a low-income patient but the readmission costs were $66008.
The Patient Protection and Affordable Care Act (PPACA), a federal health reform law, stresses that reducing hospital readmissions is an important strategy both for improving quality of care and to lowering the cost of care9. Several studies have examined rural-urban differences in hospital readmissions. Some of this work has shown that treatment in a rural hospital lowered the likelihood of hospital readmission10,11. However, older rural veterans seem more likely to have higher 30-day readmission rates than urban veterans, although a Congressional report suggests that rural-urban differences in readmissions do not exist12,13. Previous research has focused largely on readmissions in general. Only veterans' care has been subjected to closer scrutiny. None of this work investigated potential rural-urban differences in maternal readmissions. To begin to fill this knowledge gap, this study investigates the effects of rurality on the likelihood of maternal rehospitalizations, using the 2011 California Healthcare Cost and Utilization Project (HCUP).
This research has four objectives. These are to:
- describe the respective outcomes (ie rehospitalizations/readmissions) and individual characteristics of women with a normal delivery or a C-section
- compare the differences of individual characteristics between patients who were and who were not readmitted
- estimate the cumulative readmission rates within 7 days, 14 days, and 30 days for urban and rural hospitals
- identify how rural-urban factors may affect the likelihood of readmission, while controlling for covariates such as age and insurance plan. Proper assessment of geographic differences in readmissions and by two different delivery modes may be important for designing cost-effective interventions to reduce unnecessary readmissions.
Data source
The data of this cross-sectional study were drawn from the 2011 California HCUP. The HCUP, a national pool of all-payer hospital discharge data, is expected to provide empirical evidence of hospital readmission problems at the national level14. Unfortunately, only 15 out of the 50 states have continuously collected readmissions information. This research focuses on data from the state with the largest number of total discharges in the USA: California15. Therefore, this study focuses on maternal care in urban and rural hospitals in California.
When a patient is admitted to a hospital for one or more conditions, a patient medical record is created with his/her demographic data. When this patient is discharged, a bill will be generated. This patient information becomes the basis of the HCUP databases16. State-level data organizations, hospital associations, private data organizations, and the federal government collect discharge data from community hospitals and send these data to the Agency for Healthcare Research and Quality (AHRQ) for inclusion in the HCUP. Three components of the HCUP data set were used in this study: inpatient care data in the State Inpatient Database (SID), outpatient care data in the State Emergency Department Database (SEDD), and information in the State Ambulatory Surgery Database (SASD)17.
This study used both single-level Clinical Classifications Software (CCS) codes for procedure and Medicare Severity Diagnosis Related Groups (MS-DRG) systems to identify the research sample. The single-level CCS was developed by AHRQ for aggregating cases into 285 mutually exclusive illnesses and 231 mutually exclusive procedures18. The DRGs developed by Yale University and the MS-DRGs, which were consolidated into 746 categories, were adopted for use of Medicare's Inpatient Prospective Payment System19,20. Both CCS and MS-DRG are diagnosis systems officially used by HCUP.
The research sample for this study included women admitted to inpatient departments, emergency departments, or ambulatory surgery units in 2011. Female patients without geographic information and primary procedure diagnoses were excluded. The remaining sample was divided into three groups:
- normal delivery (CCS-133, CCS-136, CCS-137; DRG-767, DRG-768, DRG-774, DRG-775)
- assisted delivery (CCS-135)
- C-section (CCS-134; DRG-765, DRG-766)21,22.
Deliveries with complicating diagnoses were not included as those have a higher risk of readmissions and might bias the observed effects of rural-urban location in this study23. The sample size of the assisted delivery group with readmission records was too small (n=220) to produce convergence in the multivariate analysis. In addition, only three female patients having assisted delivery procedure were readmitted. This group was dropped from the database. The final study sample (n=481 902) included two groups: the normal delivery group and the C-section group.
Dependent variables: maternal rehospitalizations
In response to the increasing attention to the issue of readmissions, AHRQ compiled HCUP supplemental files to provide additional information for the analyses of 'revisits' readmissions16. Since each record in the HCUP represents one discharge abstract, the term 'revisit' implies two or more visits for health services for a particular patient. Any patient's first admission related to delivery and occurred between 1 January and 30 November was treated as the index admission. Any patient's admission to the same or different hospital that occurred within 30 days after the index admission was treated as a 30-day readmission.
If a patient passed away, was transferred to another facility on the same day, or was readmitted more than 30 days after the index admission, this patient was not considered as a 30-day readmitted case17. In short, the 30-day readmission rate is the number of readmissions that occurred within 30 days of the index admission divided by the number of total index admissions.
The second outcome variable of interest is to compare 7-day, 14-day, and 30-day readmission rates. The denominator for these rates was the total number of readmitted patients. In other words, the patients with only one admission record (ie their index/first admission) were excluded. The numerators were the numbers of patients readmitted within 7, 14, or 30 days after their previous discharge of delivery.
The third outcome variable in this study was a binary measure indicating whether this patient had been readmitted between 1 January and 30 November. One of the advantages using the HCUP is that the encrypted person identifier allows researchers to track all of each patient's admission records. A patient who was discharged alive and had only one admission record was defined as no readmission group (=0). If a patient was discharged alive and had any record of reasons for/causes of readmission, this patient was defined as a readmitted case (=1).
Independent variables: hospital location and patient residence
The HCUP collects the ZIP codes of both hospitals and patients. Using the 2003 version of the Urban Influence Codes (UIC), every hospital was identified as a hospital in a rural (micropolitan areas or non-core) area, small metro (metropolitan with fewer than 1 million resident) area, or large metro (metropolitan with at least 1 million residents) area18,24. Likewise, individual patient ZIP codes were also classified into these three unique groups.
Covariates: patient characteristics
This study investigated readmissions, while adjusting for eight covariates that have been shown to have a significant association with obstetric outcomes25-28. A patient's age at admission was a continuous variable. Race/ethnicity is categorized as 'non-Hispanic White', 'non-Hispanic African American', 'Hispanic', and 'others'. Expected primary payer was coded as 'Medicare' (ie both fee-for-service and managed care Medicare plans for disabled women), 'Medicaid' (ie both fee-for-service and managed care Medicaid patients), 'private insurance' (eg Blue Cross), 'self-pay' (ie uninsured), and 'others' (eg those with worker's compensation). One category of this measure, 'no charge', had was not observed based on inclusion criteria. A quartile classification of patient's estimated median household income from lowest (poorest) to highest (richest) quartile was also collected by HCUP.
The HCUP used chronic condition indicators to identify patients' chronic conditions (eg diabetes and mental illness) listed on their medical records29. Length of stay (LOS) is equal to the number of days between the admission date and the discharge date for each admission record. That means same-day stays are coded as 0. Both the number of chronic conditions and LOS were continuous variables. The former illustrates patients' health status and the latter illustrates how long they stayed in hospital immediately after giving birth (ie the index event).
Analyses
Descriptive analysis was conducted to determine the patient-level characteristics of patients with a normal delivery or a C-section in 2011. The binary analysis provided the individual differences between patients readmitted or not readmitted for each of these two groups. The accumulative readmission rates were also calculated based on the hospital location to demonstrate rural-urban differences.
Generalized estimating equation (GEE) models were then used to estimate the likelihood of being readmitted over time. Since patients might repeatedly go to the same hospital, GEE models are particularly useful by estimating the average response over the population (ie population-averaged effects) compared to a traditional logistic regression model. To meet the research purpose, the covariance structure was set as unstructured, the link function as logit, and family as binary. Data was imported into Statistical Analysis Software v9.3 (SAS; http://www.sas.com) based on the original format provided by the HCUP distributor. Then the data was transported into Stata v12.0 (http://www.stata.com). All analyses were conducted using Stata v12.0 and a p value of less than 0.05 was considered statistically significant.
Ethics approval
The use of data was approved by the Office of Research Compliance and Biosafety (Protocol # IRB-2013-0117) at Texas A&M University.
The 323 051 women who delivered with minor assistance (normal delivery) and 158 851 women who delivered by C-section were included in this study. Of those, only 7 patients died after vaginal deliveries and 14 patients after C-section procedures. Next, 70.64% of women (228 198 cases) had only one admission after vaginal delivery and 67.49% of women (107 206) after a C-section.
Less than 1% (0.98%) of women (3171 cases) with normal deliveries were readmitted within 30 days after the index admission and the corresponding number is 1.41% of women (2243 cases) with C-section deliveries. The majority of residents living in large-metro or small-metro areas gave birth in their local hospitals. Of rural women, 77.19% of rural women (6418 cases) were admitted to rural hospitals to deliver, 15.20% (1264 cases) to small-metro hospitals, and 7.61% (633 cases) to large-metro hospitals.
Table 1 presents the distribution of each individual characteristic for those women in either the normal delivery or C-section group. Chi-square tests were not conducted here since the large sample size results in significant p values throughout the analysis. The effect size was measured for the number of chronic conditions (effect size=0.30) and for the length of first stay (effect size=0.64). On average, women with C-section procedures were slightly older, non-Hispanic Black, more from large-metro areas, more admitted to large-metro hospitals, more covered by private insurance, having lower income, and had more chronic conditions and longer stays during the index admissions than women with normal delivery.
Within either the normal delivery or C-section delivery group, women were further divided into two subgroups: 'discharged alive but not readmitted', and 'discharged alive and then readmitted'. The χ2 tests were conducted in each group of delivery comparing the distributions of readmitted and not readmitted patients. The effect size was calculated for the number of chronic conditions and the length of first stay. For women with a normal delivery, the effect sizes were 0.33 and 0.19, respectively. For women with a C-section procedure, the effect sizes were 0.45 and 0.23, respectively. For women with normal delivery (Table 2), those who were readmitted were much more likely to
- be African American (14.25>5.10%)
- have lived in rural areas (5.27%>1.81%)
- have gone to hospitals in small metro areas (28.96%≥23.54%)
- have public insurance plans (Medicare or Medicaid: 71.74%≥48.55%)
- have lower household income (37.20%≥29.57%).
Likewise, higher proportions of women readmitted to hospitals after the C-section delivery were non-Hispanic Blacks (16.32%≥6.19%), lived in small-metro areas (25.06%≥22.49%), received care in small-metro hospitals (23.53%≥21.91%), had public insurance plans (70.31%≥47.26%), had lower household income (38.69%≥29.75%), had more chronic conditions (1.24>0.62) and had longer lengths of first stay (4.53>3.57).
The cumulative readmission rates in patients with C-section delivery were higher than their normal delivery counterparts except in small-metro hospitals (Table 3). For example, the 30-day readmission rate in C-section patients from a large-metro hospital was 33.87% while it was 31.55% in patients with normal delivery. Regardless of delivery mode, patients giving birth in a rural hospital were more likely to be readmitted than in hospitals in metropolitan areas. The 7-day readmission rate of women with normal delivery in rural hospitals was 20.06% but it was only 12.20% of women in urban hospitals.
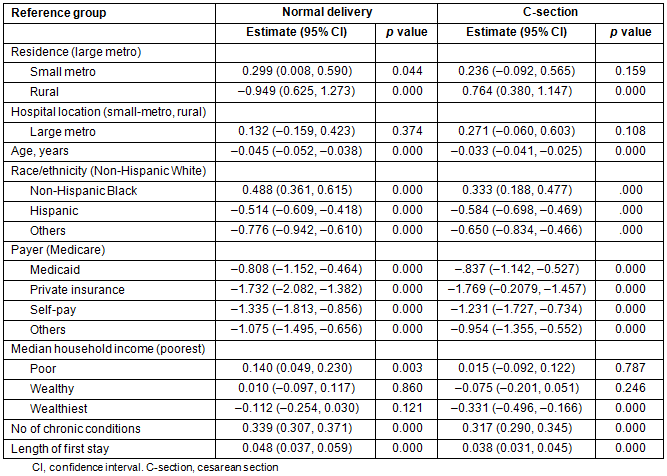
The GEE models for both delivery groups were employed to estimate the relationships between readmission likelihood and individual characteristics (Table 4). Since very few large-metro residents went to small-metro or rural hospitals for delivery, the variable of 'hospital location' was reclassified into two categories: 'large-metro area' and 'non-large-metro area'. When the response changes from 0 (not readmitted) to 1 (readmitted), the odds ratio was 1.35 (95% confidence interval 0.008-0.590) for women living in small-metro areas to be readmitted after their normal deliveries. Controversially, living in rural areas had protective effects for mothers with normal deliveries but adverse effects for mothers with C-section. The hospital location did not have a statistically significant impact on the likelihood of readmission.
Table 1: Characteristics of patients with maternal diagnoses, 2011 California Healthcare Cost and Utilization Project
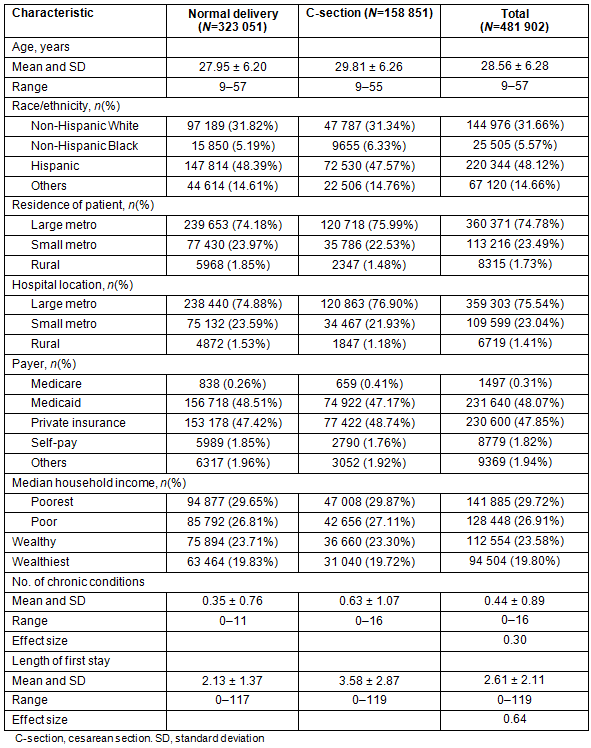
Table 2: Comparisons of characteristics between patients with and without maternal readmission, 2011 California Healthcare Cost and Utilization Project
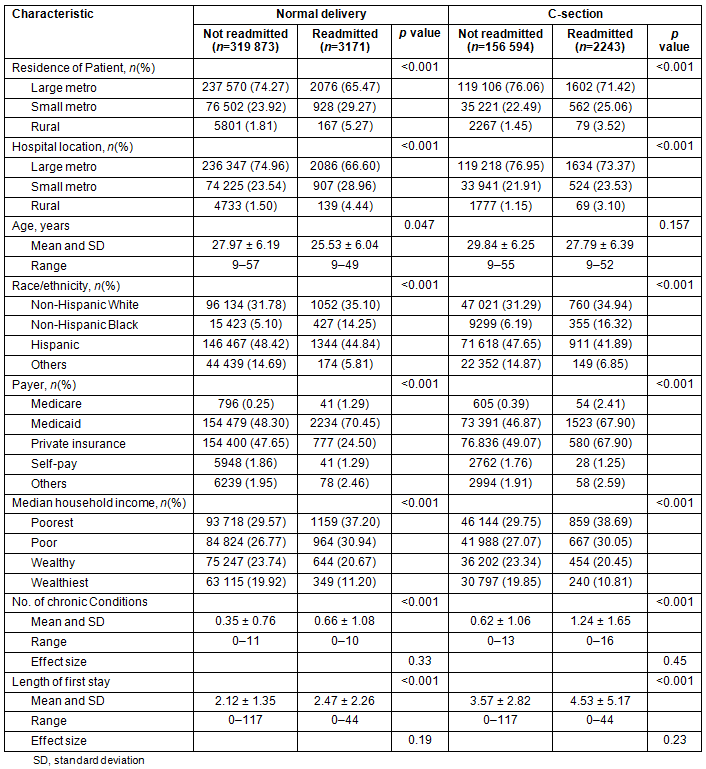
Table 3: Cumulative readmission rates among patients with readmissions, 2011 California Healthcare Cost and Utilization Project
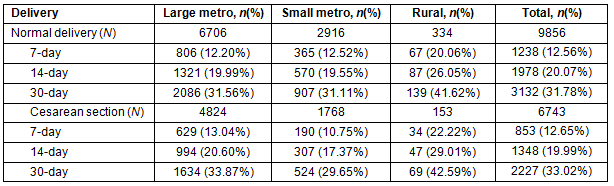
Table 4: Generalized estimating equation estimates about associations of readmission likelihood with individual characteristics, 2011 California Healthcare Cost and Utilization Project
Discussion
This study used the 2011 California HCUP data with its very large number of hospital discharges to compare readmission rates of women with a normal delivery or with C-section delivery procedures, while considering the geographic areas of hospitals and patients. The research findings suggested that childbirth in these areas is a relatively safe event with only a 0.98% readmission rate for the normal delivery group and 1.41% for the C-section group.
Consistent with other studies4,30,31, the authors found that the readmission rate after the C-section procedure was slightly higher than that observed for the normal delivery group. Policy-makers may wish to consider efforts to target hospitals with higher readmission rates after C-section by a means of payment or incentive policy32. Prior studies have suggested that administration of perioperative antibiotics is helpful to reduce the rate of delivery infectious complications, the key reason for readmission33,34.
This study indicated that, in general, women discharged from rural hospitals had higher readmission rates than metropolitan hospitals. Several factors may contribute to this finding such as inadequate family support after delivery, poor quality of hospital care, and disease burden of mothers in rural areas35,36. In addition, fewer newborns and more elders in rural areas than in urban areas make the recruitment of obstetrics and gynecology doctors and related professionals difficult37. The ratio of obstetricians to residents is 35 per 1000 in urban counties but only 2 per 1000 in rural counties38. Rural hospitals may provide unstable prenatal and postpartum services because of their small numbers of patients39-41. Prior research noted that rural hospitals heavily depend on nurse practitioners and other mid-level health professionals42. Therefore, strengthening the knowledge and skills of this group of rural providers is important. Public health interventions such as strengthening the capacity of the obstetric workforce, the safety of delivery procedures, and education about self-care before and after delivery in rural areas are also imperative.
This study adds new findings to the literature that women with a normal delivery in small metro hospitals may be at significantly higher risk of maternal rehospitalizations controlling other individual characteristics. However, the location of a hospital is not related to the readmission likelihood for women with C-section procedures. Corresponding to the literature regarding patients' choices of hospital43, the present study found that 15.20% of rural populations went to hospitals in small-metro areas and 7.61% to large-metro hospitals for delivery. Rural patients' traveling to small-metro or large-metro hospitals for delivery indicates inadequate access to quality care in their local facilities44. More studies to address rural health disparities in obstetric services are necessary.
There are several limitations in this secondary data analysis. First, the data drawn from medical charts might be biased due to recording or transcription errors. For instance, some patients' procedure CCS were coded as 'C-section' while their diagnosis CCS was coded as 'normal delivery'. Researchers are not able to access the original report and had to adopt the valid procedure CCS codes only. Second, this data only contains community hospital discharges in California in 2011. As defined by the American Hospital Association, community hospitals include non-federal, short-term, general and other specialty hospitals but exclude veteran, Department of Defense, Native American, long-term, psychiatric, tuberculosis, and alcohol/chemical dependency treatment hospitals17. Critical access hospitals, which serve in rural areas, are not required to report the discharge data to the HCUP. However, there is no direct evidence about how many critical access hospitals in California did not provide the report. Another study pointed out that rural patients may be referred to urban hospitals since critical access hospitals are required to have an average LOS of less than 96 hours45. Twenty-two percent of the rural patients in this study received care in urban hospitals which means critical access hospitals were not their providers. Third, this study took into account of all-cause, all-area, and all-payer readmissions. The benefit of this approach is to prevent providers from changing the diagnosis code on purpose, since a hospital could pay high penalties due to readmissions32. Future studies to compare different causes of readmissions in rural and urban hospitals are recommended. Finally, the multivariate analyses of this study have been adjusted for personal characteristics. Nevertheless, characteristics of healthcare providers such as hospital bed size, hospital ownership, and the experience of obstetrics and gynecology doctors are not collected into this data. Future research should include more organizational characteristics.
The research findings show the real performance of hospitals in one state. California has above-average performance in terms of six maternal health indicators46. Thus the rate of maternal readmission might be higher for other states. It is imperative to address geographic differences in maternal rehospitalizations as well as to improve data collection. Studies about vulnerable mothers in rural areas are recommended to identify their access and utilization of obstetric services.
Acknowledgements
The authors thank Stata Corp for technical support.
References
1. Taylor RB. Family medicine: principles and practice, 6th edn. New York, NY: Springer Science & Business Media, 2013.
2. Podulka J, Stranges E, Steiner C. Hospitalizations related to child birth, 2008. (Online) 2011. Available: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb110.jsp (Accessed 9 June 2013).
3. Center for Disease Control and Prevention. Pregnancy mortality surveillance system. (Online) 2013. Available: http://www.cdc.gov/reproductivehealth/MaternalInfantHealth/PMSS.html (Accessed 9 June 2013).
4. Declercq E, Barger M, Cabral HJ, Evans SR, Kotelchuck M, Simon C, et al. Maternal outcomes associated with planned primary cesarean births compared with planned vaginal births. Obstetrics & Gynecology 2007; 109(3): 669-677.
5. Kendall-Tackett K. How other cultures prevent postpartum depression social structures that protect new mothers' mental health. (Online). Available: http://www.uppitysciencechick.com/how_other_cultures.pdf (Accessed 11 February 2015).
6. Sommers A, Cunningham PJ. Physician visits after hospital discharge: implications for reducing readmissions. Research Brief 2011; (6): 1-9.
7. Olsen MA, Butler AM, Willers DM, Gross GA, Hamilton BH, Fraser VJ. Attributable costs of surgical site infection and endometritis after low transverse cesarean section. Infection Control and Hospital Epidemiology 2010; 31(3): 276-282.
8. Qasim M, Andrews RM. Post-surgical readmissions among patients living in the poorest communities, 2009. (Online) 2009. Available: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb142.jsp (Accessed 19 June 2013).
9. Stone J, Hoffman GJ. Medicare hospital readmissions: issues, policy options, and PPACA. (Online) 2010. Available: http://www.ncsl.org/documents/health/Medicare_Hospital_Readmissions_and_PPACA.pdf (Accessed 19 June 2013).
10. Philbin EF, Dec GW, Jenkins PL, DiSalvo TG. Socioeconomic status as an independent risk factor for hospital readmission for heart failure. American Journal of Cardiology 2011; 87(12): 1367-1371.
11. Welch HG, Larson EH, Hart LG, Rosenblatt RA. Readmission after surgery in Washington State rural hospitals. American Journal of Public Health 1992; 82(3): 407-411.
12. Weeks WB, Lee RE, Wallace AE, West AN, Bagian JP. Do older rural and urban veterans experience different rates of unplanned readmission to VA and non-VA hospitals? Journal of Rural Health 2009; 25(1): 62-69.
13. Akamigbo A, Stensland J. Mandated report: quality of care in rural areas. (Online) 2011. Available: http://www.medpac.gov/documents/october-2011-meeting-presentation-mandated-report-quality-of-care-in-rural-areas.pdf?sfvrsn=0 (Accessed 12 August 2015).
14. Jiang HJ, Wier LM. All-cause hospital readmissions among non-elderly Medicaid patients, 2007. Statistical Brief #89. Rockville, MD: Agency for Healthcare Research and Quality, 2010.
15. American Hospital Directory. Hospital statistics by state. (Online) 2012. Available: http://www.ahd.com/state_statistics.html (Accessed 19 June 2013).
16. Allen Communication Learning Services. The HCUP Overview Course designed for AHRQ. 2013. Available: http://www.hcup-us.ahrq.gov/tech_assist/trends/interactive/508_compliance/508course.htm# (Accessed 12 August 2015).
17. Healthcare Cost and Utilization Project. HCUP databases. (Online) 2013. Available: http://www.hcup-us.ahrq.gov/databases.jsp (Accessed 9 June 2013).
18. Elixhauser A, Steiner C, Palmer L. Clinical Classifications Software (CCS), 2013. Rockville, MD: Agency for Healthcare Research and Quality, 2013.
19. American Health Information Management Association. The evolution of DRGs (updated). (Online) 2010. Available: http://library.ahima.org/xpedio/groups/public/documents/ahima/bok1_047260.hcsp?dDocName=bok1_047260 (Accessed 11 February 2015).
20. Sun Y, Friedman B. Tools for more accurate inpatient cost estimates with HCUP databases. HCUP Methods Series Report # 2011-04. (Online) 2009. Available at: http://www.hcup-us.ahrq.gov/reports/methods/methods.jsp (Accessed 09 June 2013).
21. Healthcare Cost and Utilization Project. Sources and methods. (Online) 2009. Available: http://www.hcup-us.ahrq.gov/reports/factsandfigures/2009/sources_methods.jsp (Accessed 11 February 2015).
22. Healthcare Cost and Utilization Project. Hospitalizations related to childbirth, 2008. (Online) 2011. Available: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb110.jsp (Accessed 11 February 2015).
23. Liu S, Heaman M, Joseph KS, Liston RM, Huang L, Sauve R, et al. Risk of maternal postpartum readmission associated with mode of delivery. Obstetrics and Gynecology 2005; 105(4): 836-842.
24. United States Department of Agriculture. Urban influence codes. (Online) 2013. Available: http://www.ers.usda.gov/data-products/urban-influence-codes.aspx#.UkLp9BCMfrQ (Accessed 19 June 2013).
25. Bailit JL, Grobman WA, Rice MM, Spong CY, Wapner RJ, Varner MW, et al. Risk-adjusted models for adverse obstetric outcomes and variation in risk-adjusted outcomes across hospitals. American Journal of Obstetrics & Gynecology 2013; 209(446): e1-30.
26. Bryant AS, Worjoloh A, Caughey AB, Washington EA. Racial/ethnic disparities in obstetrical outcomes and care: prevalence and determinants. American Journal of Obstetrics & Gynecology 2010; 202(4): 335-343.
27. Werder E, Mendola P, Männistö T, O'Loughlin J, Laughon SK. Effect of maternal chronic disease on obstetric complications in twin pregnancies in a United States cohort. Fertility and Sterility 2013; 100(1): 142-149.
28. Halfon P, Eggli Y, Pretre-Rohrbach I, Meylan D, Marazzi A, Burnand B. Validation of the potentially avoidable hospital readmission rate as a routine indicator of the quality of hospital care. Medical Care 2006; 44(11): 972-981.
29. Healthcare Cost and Utilization Project. Chronic conditions indicators. (Online) 2015. Available: http://www.hcup-us.ahrq.gov/toolssoftware/chronic/chronic.jsp (Accessed 1 March 2015).
30. Hebert PR, Reed G, Entman SS, Mitchel EF, Berg C, Griffin MR. Serious maternal morbidity after childbirth: prolonged hospital stays and readmissions. Obstetrics and Gynecology 1999; 94(6): 942-947.
31. Lydon-Rochelle M, Holt VL, Martin DP, Easterling TR. Association between method of delivery and maternal rehospitalizations JAMA 2000; 283(18): 2411-2416.
32. Center for Medicare and Medicaid Services. Readmission reduction program. (Online) 2013. Available: http://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/Readmissions-Reduction-Program.html (Accessed 19 June 2013).
33. Belfort MA, Clark SL, Saade GR, Kleja K, Dildy GA 3rd, Van Veen TR, et al. Hospital readmission after delivery: evidence for an increased incidence of nonurogenital infection in the immediate postpartum period. American Journal of Obstetrics and Gynecology 2010; 202(35): e1-7.
34. Smail F, Hofmeyr GJ. Antibiotic prophylaxis for cesarean sections. American Journal of Obstetrics and Gynecology 2007; 196: 526-527.
35. Kitzmiller JL, Dang-Kilduff L, Taslimi MM. Gestational diabetes after delivery: short-term management and long-term risks. Diabetes Care 2007; 30(supp. 2): S225-235.
36. Ray KN, Lorch SA. Hospitalization of rural and urban infants during the first year of life. Pediatrics 2012; 130(6): 1084-1093.
37. Vogel J. Doctor shortage raises rural C-section rate. (Online) 2012. Available: http://blogs.mprnews.org/ground-level/2012/06/conference-focuses-on-consequences-of-rural-doctor-shortage/ (Accessed 29 July 2013).
38. Health Resources and Services Administration. Area resource file (ARF) 2011-2012. Rockville, MD: US Department of Health and Human Services, 2012.
39. Lorch SA, Baiocchi M, Sillber JH, Even-Shoshan O, Escobar GJ, Small DS. The role of outpatient facilities in explaining variations in risk-adjusted readmission rates between hospitals. Health Services Research 2010; 45(1): 24-41.
40. National Rural Health Association. Rural women's health. (Online) 2013. Available: http://www.ruralhealthweb.org/index.cfm?objectid=F5A503E1-3048-651A-FE066957562D3AC7 (Accessed 29 July 2013).
41. Office of Rural Health and Primary Care. Rural Health Advisory Committee report on obstetric services in rural Minnesota. (Online) 2013. Available: http://www.health.state.mn.us/divs/orhpc/rhac/obrpt.pdf (Accessed 29 July 2013).
42. American Hospital Association. The opportunities and challenges for rural hospitals in an era of health reform. (Online) 2011. Available: http://www.aha.org/research/reports/tw/11apr-tw-rural.pdf (Accessed 8 March 2015).
43. Laditka SB, Laditka JN, Bennett KJ, Probst JC. Delivery complications associated with prenatal care access for Medicaid-insured mothers in rural and urban hospitals. Journal of Rural Health 2005; 21(2): 158-166.
44. Peck J, Alexander K. Maternal, infant, and child health in rural areas: a literature review. In: LD Gamm, LL Hutchison, BJ Dabney, AM Dorsey (Eds). Rural healthy people 2010: a companion document to Healthy People 2010. Volume 2. College Station, TX: The Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Health Research Center, 2003.
45. Toth M, Holmes M, Freeman VA, Pink GH. Rural/urban differences in inpatient related costs and use among Medicare beneficiaries. Findings brief of NC Rural Health Research Program. (Online) 2014. Available: http://www.shepscenter.unc.edu/wp-content/uploads/2014/03/Rural-urban-Differences-in-Inpatient-cost-and-Use-amoung-Medicare-beneficiaries.pdf (Accessed 5 June 2014).
46. US Department of Health and Human Services, Agency for Healthcare Research and Quality. Compare state health care quality ratings. (Online) 2014. Available: http://nhqrnet.ahrq.gov/snaps11/meter_metrics.jsp?menuId=4&state=CA&level=17®ion=0&compGroup=N (Accessed 12 August 2015).
