More than one billion people in the world lack access to basic health care1. This lack of health care is more pronounced in rural communities and creates a gap between urban and rural indicators of health1-3. According to WHO, an insufficient number of adequately trained health workers is an obstacle to achieving Millennium Development Goals (2015)4; therefore, the focus of the United Nations Sustainable Developmental Goals is the development of human resources5. Some of the factors contributing to the reduced number of rural healthcare professionals are demanding working conditions, substandard medical equipment and facilities, inadequate financial remuneration, and inadequate opportunities for professional growth6.
Additionally, studies reveal that in some countries, valuable resources are expended by training a mix of specialists that does not adequately respond to community needs, especially in rural areas7. Evidence suggests that primary care physicians are uniquely trained to respond to the healthcare needs of underserved populations who live in rural and remote areas worldwide8-10. However, many countries lack the robust primary care infrastructure and workforce needed to meet the health needs of their rural population11. The response of many middle- and low-income countries to their rural workforce shortage has been to require their medical trainees to complete a period of social service in rural areas of the country, either in their last year of medical school or upon graduation6. However, since many do not stay after completing service, this provides only a temporary solution12.
The continental Central American region of the world lies between the isthmuses of Tehuantepec (in Mexico) and Panama13,14. Five of the eight countries in this region fall below the density of 25 physicians per 10 000 habitants recommended by WHO15,16 with a great disparity in the distribution between urban and rural areas17. Central America has 95 medical schools, a population of 145 million, and 229 407 physicians, with a physician density of 15.8 per 10 000 inhabitants18. It has been previously suggested that medical care in this geographical area must combine primary care and community interventions, using a team approach, in order to provide optimal care19. A major barrier in many of the countries in continental Central America is that most medical schools train their students to become specialists rather than primary care practitioners20,21. To respond to community needs, a few of the countries in this region have created teams composed of a variety of health professionals22. However, in order to improve the health of rural populations, interventions for prevention, and management of acute and chronic diseases are still needed23. Observations made by medical anthropologist Moira Wood document that the reality in most rural areas is that this healthcare team often lacks a physician24.
The medical literature4,25,26 suggests educational strategies to retain health professionals in rural areas, including: (a) enrolling students from rural backgrounds and with experience working with underserved communities; (b) locating medical schools and residencies in rural areas, decentralized from urban academic medical centers; (c) training future physicians in rural settings, with longitudinal rural preceptors; (d) modifying the medical curriculum to cover topics and skills pertinent to rural settings; and (e) creating medical literature specific to rural healthcare providers. Others have suggested that medical education should include early clinical exposure to rural areas27, as some students decide early in their careers the location of future practice12. These suggestions for enhancing the medical curriculum provide students with the skills and knowledge to practice in rural areas, thus enhancing their confidence to practice in rural communities in the future4,28. Specific skills needed for rural practice mentioned in the literature include healthcare management, leadership, cross-cultural communication, procedural skills and emergency care12,29 .
Currently, there are no studies that specifically address the question: How does the medical education system in continental Central America prepare physicians for the practice of rural medicine? The goal of this study was to (a) understand the current state of medical education preparing physicians for rural practice in this region of the world and (b) identify common needs, challenges and opportunities for improvements in rural health training in continental Central America.
A rigorous narrative literature review was conducted30. This involved a comprehensive literature search31, using a reproducible stepwise process, to identify all relevant literature. A narrative synthesis, using qualitative methods was then done to extract relevant information and themes from the identified articles.
Search methods
Multiple methods were used to search for articles, reports or conference proceedings that addressed the study objectives. First, PubMed, Web of Science/Web of Knowledge, ERIC and Google Scholar databases were searched from December 2013 to May 2014. Relevant English and Spanish language articles were identified using the medical subject heading (MeSH) terms 'medical education', 'rural health', 'primary care', 'community medicine', and 'social service' in conjunction with any of the following: 'Central America', 'Latin America', 'Mexico', 'Guatemala', 'Belize', 'El Salvador', 'Nicaragua', 'Costa Rica', 'Honduras' and 'Panama'. In order for the search to be as comprehensive as possible, the term 'social service' was included in the literature search because in many countries in this region of the world training regarding rural health is incorporated into required social service commitment time. This search yielded 36 articles. The titles and abstracts of these 36 articles were reviewed by one member of the research team. Literature met inclusion criteria if it was: (1) published after 1984; (2) concerned medical education for primary care, community health or rural health; and (3) pertained to one or more of the eight countries in continental Central America being studied. Sixteen journal articles were identified by this method.
Second, the search was expanded to include grey literature32 found through internet search engines (Google and Pan American Health Organization Regional Health Observatory resource page). The same MeSH terms used for the database search were used as key words to search the grey literature. Examples included non-governmental organizational reports, conference proceedings, and newspaper articles, which were directly related to the research question and would provide more in-depth knowledge of the topic. It has been suggested that grey literature can be the primary source of evidence for some topics and should be included in literature reviews31. Grey literature searching revealed five additional resources.
A third method to identify relevant sources was a careful review of the reference list from the sources identified through the first two methods. These sources were reviewed by one member of the research team and included or excluded on the basis of the same criteria as above. This search produced six additional references.
All sources identified through this stepwise process were independently reviewed in more detail for relevance to the study question by three members of the research team. Seven articles were excluded after this review since they did not meet relevance criteria: (1) medical education for practice in rural settings; and/or (2) medical education for primary care and/or community medicine.
Analysis methods
The 20 remaining articles were categorized into source type. Only four sources were research studies (three retrospective studies and one focus group study). Given the paucity of research studies on this subject, all 20 relevant resources were included in the analysis. A narrative analysis methodology, using qualitative research techniques to extract common content and themes, was chosen as the most appropriate analysis approach for this study33. This approach has been used by others to synthesize information from a wide variety of sources, when research studies are lacking34,35.
The specific analysis method employed was a thematic analysis using an inductive approach36. This entailed three members of the research team (all bilingual in Spanish and English) independently extracting meaningful content and themes from each article. The researchers then met as a group periodically to identify common themes and subthemes found in the literature sources. Rounds of meetings continued until there was agreement among all researchers regarding major themes and subthemes.
General findings
Twenty articles were analysed in depth37-56. There is a significant paucity of research related to medical education preparing physicians for rural practice in continental Central America. Additionally, few articles described in depth or evaluated specific rural medicine educational initiatives in this geographical territory. Therefore, data were extracted primarily from expert opinion articles. Table 1 summarizes these articles and sources of data37-56. The 20 articles included six historical reviews44,49-51,54,56, five descriptive reports from non-governmental organizations37,40,45,48,55, three retrospective studies41,46,47, two expert opinions extracted from conference proceedings38,53, one focus group study39, one thesis42, one observational narrative52 and one news report43. Articles ranged in publication date from 1987 to 2012.
Overview of themes and subthemes from qualitative analysis
Qualitative analysis of the content of the 20 articles revealed several themes and subthemes (Tables 2-4) related to the structure and content of medical education specific to rural health in continental Central America. Some successful educational programs were described. However, there appear to be many common challenges faced by countries in this region, prompting several authors to propose suggestions for improvements in rural medicine education for physicians and medical students.
Table 1: Summary of the systematic literature search results37-56
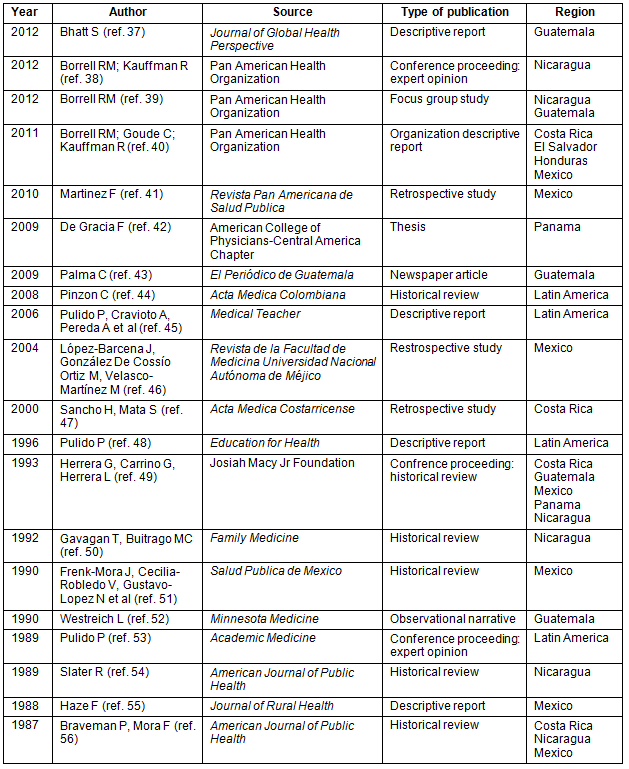 Table 2: Successes in rural medicine education in continental Central America
Table 2: Successes in rural medicine education in continental Central America
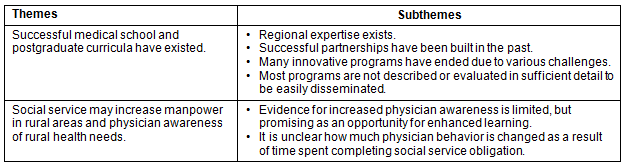 Table 3: Challenges related to medical education for rural practice in continental Central America
Table 3: Challenges related to medical education for rural practice in continental Central America
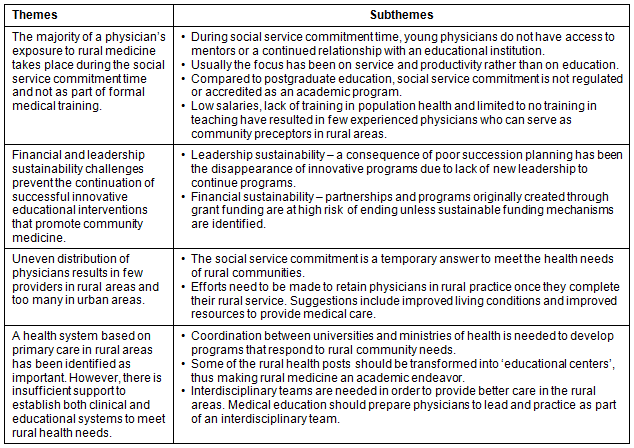 Table 4: Core content necessary to improve rural medicine education in continental Central America
Table 4: Core content necessary to improve rural medicine education in continental Central America

Successful rural medicine educational programs (Table 2)
Theme 1. Successful medical school and postgraduate curricula exist: Historically, there have been several successful educational programs in this region. One example is the pilot program Programa de Servicio a la Comunidad in rural Guatemala49. This unique program was an innovative collaboration between Universidad San Carlos, the Ministry of Public Health and international organizations. Students and faculty worked in multidisciplinary teams, in a learning and working program, for 6-12 months. Students collaborated with community leaders to perform research and develop health programs, were supervised individually once a week, and had both formal and informal teaching sessions. Another example is Programa San Ramon in partnership with Universidad Central de America in Costa Rica56, which provided both rural patient care and medical education. This program exposed students to rural hospital and community-based care; thus training students in the social determinants of health in both environments.
There have also been successful postgraduate training programs. One example is the 'medicina integral' postgraduate training program during the mid-1980s in Nicaragua54. This three-year program prepared graduates for primary care and was created because of the government's concern that the country had too many specialists concentrated in urban areas. Another example is the postgraduate program in Family Medicine at Universidad Nacional Autonoma de Mejico55. In this program, trainees spent four months in agricultural villages in Tlaxcala working in clinical care and community projects, with weekly supervision from the academic institution and local preceptors.
These examples demonstrate both the benefits of rural medicine education and the presence of local expertise in rural medical education in continental Central America. Unfortunately, some of these programs no longer exist due to numerous challenges, including sustainability of funding and leadership. Additionally, most successful curricula have not been described or evaluated in sufficient detail to be readily disseminated.
Theme 2. Social service may increase manpower in rural areas and physician awareness of rural health needs: A retrospective study from Mexico46 revealed that the collaboration between the Ministry of Health and the Ministry of Education has been successful at assigning young physicians to serve in rural areas during their social service commitment time. In some countries, such as Mexico49 and Costa Rica49, there is some evidence suggesting that social service time may result in indirect education and sensitization of the physicians to the impact of the psychosocial factors on health and disease49. Physicians completing their rural social service commitment are exposed to the same psychosocial and ecological environmental conditions as their patients, helping them learn about non-biological factors that affect illness49. However, more robust research is needed to better understand the degree of impact of this exposure and whether this changes physician behavior.
Challenges to rural medicine education in continental Central America (Table 3)
Theme 1. The majority of physicians' exposure to rural medicine takes place during the social service commitment time and not as part of formal medical training: Medical students in continental Central America appear to have little formal training in rural medicine. In most of these countries41, young physicians are required to engage in social service commitment time, either just before or after receiving their medical degree. Social service commitment in this region started in Mexico in response to healthcare provider shortages in rural areas49. This often represents students' only experience caring for people in rural areas45. In most cases, young physicians are not adequately supervised during this period of social service rural practice41. This lack of supervision and formal rural health curriculum has created a gap in the knowledge and mastery of skills needed to practice in rural areas. A study done in Mexico41 between 2006 and 2008 revealed that young graduates doing social services did not have the knowledge to provide high-quality medical care in rural communities. An example of required knowledge differences can be seen in Panama, where in urban communities the top causes of death are chronic diseases, whereas in the rural areas mortality is due to infectious disease, malnutrition and violence42. Another example is the high maternal mortality rate in rural Guatemala compared to in urban areas, creating a greater need for skilled birth attendants in rural communities37.
The lack of supervision and adequate payment during their social service time has been associated with a negative experience for many medical graduates49. As a consequence, few physicians stay in rural areas after completing their service and the cyclical problem of physician shortage in rural continental Central America has persisted. Thus, it has been argued that social service commitment is not the answer to the needs of the population in rural areas, as it has not facilitated the recruitment of permanent healthcare providers49. Some have argued49 that social service should be transformed into an academic program. This transformation could provide graduates with mentors and continued medical education while in isolated practice. One of the countries that supervises their young social service physicians is Panama49. Learner outcomes, through monthly evaluations, are taken into consideration when the graduates apply for postgraduate training programs, which is motivation for better performance49.
Another significant challenge is the lack of faculty to sustain educational programs in rural areas. For example, in one medical school in Mexico56 students spent their fifth year in a rural setting in preparation for their social service commitment. This innovative program was not sustainable, as rural professors needed multiple jobs in order to earn an adequate income. It has been argued that purposeful incentives, beyond salaries, are needed for physicians to continue to practice and teach in these underserved areas48, such as better training and working conditions56.
Theme 2. Financial and leadership sustainability challenges prevent the continuation of successful innovative educational interventions that promote community medicine: In Guatemala56, successful community medicine educational programs disappeared due to lack of adequate collaboration between the government and medical institutions. In the past, organizations such as Pan American Health Organization (PAHO)56, Rockefeller Foundation, Kellogg Foundation56 and the Josiah Macy Jr Foundation49 have provided financial support to promote community-orientated primary care and to evaluate the social service commitment programs. Grants provided temporary funding to establish programs to serve communities. However, due to lack of plans for long-term financing, these programs were not sustainable56. Another identified challenge is the lack of trained leaders to continue established programs as older physicians and faculty retire56. Thus, both financial and leadership sustainability are essential for any new rural medicine educational program.
Theme 3. Uneven distribution of physicians results in few providers in rural areas and too many in urban areas: After the social service commitment time, most physicians assigned to rural and remote communities do not continue to practice in these areas. While most countries in this region have an adequate number of total physicians for the population, there is a much higher concentration of human resources in urban areas45,54. In Costa Rica, there are insufficient social service positions in rural areas for young medical graduates, so the majority are assigned to urban centers47. In rural Panama, there is a population density of 2852 inhabitants per physician, compared to 510 inhabitants per physician in urban areas42. To address this uneven distribution, Panama requires their graduates to serve one year in rural areas42 as part of their two years social service commitment. It has been argued that these short-term assignments do not provide the community with long-term physician-patient relationships that are essential for trust building and long-term health outcomes37. One possible solution for the shortage of rural physicians as teachers is to place equal value and recognition on community preceptors as on academic instructors38.
Theme 4. A health system based on primary care in rural areas has been identified as important. However, there is insufficient collaboration to establish and sustain clinical and educational systems to meet rural health needs: Although governmental, non-governmental and educational institutions have all worked independently to improve health for rural communities, there appears to be a need for improved communication between these various sectors. In Mexico, for example, the graduates from a community-based training program were unable to obtain jobs after completion56, since the health system was not oriented towards community primary care. In other countries, such as Nicaragua and Costa Rica56, similarly trained graduates have been employed in administrative positions. As a result, the needs of rural communities are still not met48. Consequently, some authors have argued that medical education goals should be redefined to respond to the health needs of the community and align with national health policies44,48. They suggest that governmental institutions and community stakeholders should have input into curriculum redesign efforts38. One possible solution is the transformation of the infrastructure of existing health posts into community educational centers48, creating a partnership between government and educational institutions45.
Another identified need in continental Central America is the creation of primary care teams that include physicians and other healthcare providers. In some countries, doctors are considered too expensive; therefore, health posts are staffed by nurses, community health workers and traditional healers56. For example, in rural Guatemala, health posts may be staffed only by a nurse or medical student37. In Costa Rica, very few medical graduates going into the social service program are exposed to rural EBAIS (primary care teams composed of physician, nurse and technician)47. This lack of exposure to physician role models in rural practice results in one of the critical challenges identified in this region - that social service programs actually promote specialization rather than primary care rural practice48.
Common suggestions for core curricular content needed to improve rural medicine education (Table 4)
Theme 1. Primary care should be an essential component of medical education: In many of the countries in this region, clinical medical education takes place in tertiary care centers that do not provide sufficient exposure to primary care, primary prevention and community medicine. This work environment also does not provide learners with a rich exposure to the social determinants of health44,52. In the era of 'beyond Flexner' it has been suggested that a shift to the 'critical paradigm' will bring about curricular reform with a greater focus on health prevention and primary care with teaching centers located in the community44,51.
Some of the countries in continental Central America have started to redesign their medical curriculum. For example, in Nicaragua, Universidad de Leon uses problem-based learning to expose students to the difficulties in the community38. These students are also exposed to primary care in rural communities through medical brigades38 and 12 weeks of community medicine, coordinated with the Ministry of Health and community health posts39. Another example is Guatemala's Rafael Landivar Medical School39,where students are exposed to primary and community medicine early in their education.
The ability to perform community health assessments is another skill identified as critically necessary for work in this region. Medical graduates need to be able to help solve community health problems while simultaneously involving community members as key stakeholders and integral members of the team. Many have called this the integration of primary care and public health38. This integration requires the teaching of core topics related to poverty and the health consequences of marginality49, which will enable medical graduates to be more successful in their leadership roles during their social service commitment time. It has also been argued that governmental health facilities, where physicians fulfill their social service commitment, such as Caja Costarriquense de Seguro Social in Costa Rica and the Ministry of Health (MINSA) in Nicaragua, could contribute to the social mission and knowledge of medical schools by sharing this knowledge49, creating a relationship of mutual benefit.
Theme 2. The medical school curriculum needs to prepare students to practice in cross-cultural contexts and address socioeconomic issues affecting health: Language is a major obstacle to providing high-quality care in some rural communities. Native populations sometimes speak dialects requiring translation. In countries such as Panama42 and Guatemala37, the indigenous population often do not seek health care, as providers do not speak their language and professional translation is not available. It has also been observed that this creates a disparity in the level of health literacy between the patient and physician. To increase health-seeking behaviors, barriers in language and health literacy have been identified as still needing attention by the health system in Guatemala37.
Another barrier to healthcare-seeking behavior is the lack of provider cultural awareness. In Guatemala, poverty in rural areas creates cultural disparities52 that affect the level of trust that patients feel towards physicians37. Additionally, some indigenous populations avoid medical care because physicians lack knowledge of their culture and beliefs. One example is that Mayan communities expect to accompany their family members during labor and delivery37. When this does not happen, families lose their faith in the quality of the health care provided. Since many of the young medical graduates assigned to rural posts come from significantly different socioeconomic backgrounds than their rural patients, they often lack knowledge of the variety and complexity of their patients' social challenges and of their cultural and healing beliefs. Without adequate preparation during medical training, these interactions can often result in the perpetuation of lack of trust between rural populations and the physicians assigned to serve them.
Discussion
The comprehensive literature search undertaken in this study revealed few research reports that addressed the goals of the study. However, it did reveal several robust articles and reports that shed light on the current state of rural medicine training in continental Central America. Qualitative analysis of the content of these articles revealed several themes related to successes, challenges and opportunities for improving rural health and rural medicine education in these countries. Limitations to this study are that resources analysed were restricted to articles readily identified via research and/or internet search engines. Since few research studies were available on this subject, results of this study reflect finding primarily from expert opinion. However, given the notable paucity of research on this subject, this review may be a valuable starting place for researches and educators interested in this subject.
The challenges to medical education for rural health practice identified in this study are similar to those faced by rural communities throughout the world57,58. They include a shortage of rural health workforce and resources, insufficient dedicated training in rural health topics during medical school, and lack of adequate supervision of young physicians during their social services commitment time in rural and remote communities. Expert opinion from a variety of sources suggests that improving the quality of training needed to meet the needs of rural, underserved communities in continental Central America will require a multidimensional approach, including teamwork between educational institutions, governmental and non-governmental organizations, and community stakeholders. Results of this literature review and reports from other regions of the world suggest several possible approaches for improving rural medicine education in continental Central America.
First, medical schools could develop curricula designed to recruit and retain physicians to serve in rural areas, emphasizing primary care and early exposure to the rural health system. Some suggest that extended and early exposure to rural experience has a strong association to long-term rural service59. An example of a successful program, close to continental Central America is Programa de Internado Rural Interdisciplinario in Chile60. This program, created by Universidad de La Frontera and the local government, responds to the unique health needs of this zone by blending primary care, public health and traditional medicine60. In Australia61, South Africa62 and the USA63, medical schools have developed immersion curricula in rural and community medicine that provide students with knowledge and skills comparable to that of students trained at urban and tertiary medical centers, thus enhancing their confidence in their skills and decision-making capacity. Additionally, faculty development has been identified as a priority, as this will foster development of leaders for the next generation of healthcare providers. Several authors suggest that through organizations such as World Organization of Family Doctors (WONCA) and Society of Teachers of Family Medicine (STFM), successful rural health curricula can be shared and then adapted to continental Central America64. Additionally, PAHO has developed El Observatorio Regional de Recursos Humanos, a web space to share human development resources in the Americas65. PAHO has also created unique virtual training programs, which specifically improves skills of healthcare providers working with indigenous populations66.
Second, partnerships between governmental authorities, educational institutions and rural communities could strengthen the health system in rural areas and tailor educational programs for rural health practice, consequently decreasing the healthcare gap between rural and urban communities. Creating partnerships of satellite clinics, which allow for rural postgraduate training in primary care, might be a solution for some countries. There is strong evidence suggesting that programs in postgraduate training, focusing on primary care and community health67,68, with local preceptors as supervisors, can reduce the mismatch between healthcare providers choosing to practice in rural areas versus urban areas, when compared to compulsory social service69,70. Involving the community in strategic remodelling of the health system and medical education may empower rural community members, as they become stakeholders in improving the local health system71. Satellite community clinics might also take a load off tertiary medical centers, and allow students to work with other health professionals, such as community health workers72.
Finally, topics related to professionalism and cultural and language competency could be strengthened in the medical curriculum. A focus group study that included rural communities from Honduras, Costa Rica and Panama found that the most fundamental need for the people is to have a physician in the community who they can trust73. An anthropological study done with the indigenous population in Guatemala revealed that health professionals need to develop creative skills to communicate more effectively with their patients and to overcome health literacy disparities74. The patient-physician relationship is particularly important for the indigenous population in continental Central America since their health problems are substantially affected by their sociocultural context75.
There is a long history of efforts in continental Central America to address the health needs of rural communities through healthcare programs and medical educational interventions, with a clear wealth of regional expertise in these subjects. However, there still remain substantial challenges to creating and sustaining medical educational programs that prepare physicians for rural practice and encourage physicians to choose careers in rural communities. Solutions require innovative partnerships between educational, governmental and non-governmental organizations and the rural communities being served. Additionally, there is a great need for further research on this topic, including evaluation and dissemination of successful educational programs76. This sharing of best practices is essential for improvement in health outcomes in rural communities and for the training of physicians to serve these communities.
Acknowledgements
The authors would like to thank Nicolla Palloti, Medical Librarian at Memorial Hospital of Rhode Island for her help in conducting the literature search.
References
1. Wollard RF. From the villages to the globe: the social accountability of rural health practitioners. In: AB Chater, J Rourke, ID Couper, RP Strasser, S Reid (Eds). WONCA rural medical education guidebook. Bangrak: WONCA Working Group on Rural Practice, 1-13. (Online) 2014. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice/ruralguidebook.aspx (Accessed 4 July 2014).
2. Kidd M (Ed). Delivery trends affecting health service delivery. In: The contribution of family medicine to improving health systems. 2nd edn. London: Radcliffe Publishing, 2013; 25-28.
3. World Bank. World development report 1993: investing in health, Vol 1. New York, NY: Oxford University Press. (Online) 1993. Available: http://elibrary.worldbank.org/doi/abs/10.1596/0-1952-0890-0 (Accessed 7 Dec 2013).
4. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. France: WHO, 2010.
5. United Nations. Realizing the future we want for all: key recommendations from the report of the UN System Task Team on the post-2015 UN development agenda. New York, NY: UN 2012.
6. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 8: 19. (Online) 2008. Available: http://www.biomedcentral.com/1472-6369/8/19 (Accessed 15 July 2014).
7. Kidd M (Ed). Challenges to optimal health services delivery. In: The contribution of family medicine to improving health systems. 2nd edn. London: Radcliffe Publishing; 2013. 29-30.
8. Starfield B. Is primary care essential? Lancet 1994; 344: 1129-1133.
9. World Health Organization. Primary health care. (Online) 2014. Available: http://www.who.int/topics/primary_health_care/en/ (Accessed 22 August 2014).
10. Rosenblatt RA. Commentary: do medical schools have a responsibility to train physicians to meet the needs of the public? The case of persistent rural physician shortages. Academic Medicine 2010; 85(4): 572-574.
11. Inem V. The challenges of health systems in developing countries. In: AB Chater, J Rourke, ID Couper, RP Strasser, S Reid (Eds). WONCA rural medical education guidebook. Bangrak: WONCA Working Group on Rural Practice; 1-6. (Online) 2014. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice/ruralguidebook.aspx (Accessed 23 August 2014).
12. Robinson M, Slaney GM. Choice or chance! The influence of decentralised training on GP retention in the Bogong region of Victoria and New South Wales. Rural and Remote Health 13(2): 2231. (Online) 2013. Available: www.rrh.org.au (Accessed 15 July 2014).
13. Schleusener D. Where and what is Mesoamerica? The complete Mesoamerica ... and more. Weblog. (Online) 2011. Available: http://tcmam.wordpress.com/2011/07/30/where-and-what-is-mesoamerica (Accessed 23 August 2014).
14. Definition and More from the Free Merriam-Webster Dictionary [Internet]. Central America. Available: http://www.merriam-webster.com/dictionary/central america (Accessed 23 August 2014).
15. Fraser B. Human resources for health in the Americas. Lancet 2007; 369: 179-180.
16. Pan American Health Organization. Density map health manpower per 10 thousand inhabitants. (Online). Available: http://dev.observatoriorh.org/?q=node/242 (Accessed 27 Jul 2014).
17. Pan American Health Organization. Most countries in the Americas have sufficient health personnel but face challenges in distribution, migration and training. (Online) 2013. Available: http://www.paho.org/hq/index.php?option=com_content&view=article&id=9146:most-countries-in-the-americas-have-sufficient-health-personnel-but-face-challenges-in-distribution-migration-and-training&Itemid=1926&lang=en (Accessed 28 July 2014).
18. Boulet J, Bede C, Mckinley D, Norcini J. An overview of the world's medical schools. Medical Teacher 2007; 29: 20-26.
19. Ventres WB. The emergence of primary care in Latin America: reflections from the field. Journal of the American Boardof Family Medicine 2013; 26(2): 183-186.
20. Ramirez B, Berry DE. Introduction to Special Issue Rural Primary Health Care in Latin America. Journal of Rural Health 1988; 4(1): 5-11.
21. Puschel K, Rojas P, Erazo A, Thompson B, Lopez J, Barros J. Social accountability of medical schools and academic primary care training in Latin America: principles but not practice. Family Practice 2014; 31(4): 399-408.
22. Fernández-Ortega MA, Arias-Castillo L, Brandt-Toro C, Irigoyen-Coria A, Roo-Prato JB. Hacia el fortalecimiento de la Medicina Familiar y la Atención Primaria en los sistemas de salud: IV Cumbre Iberoamericana de Medicina Familiar. Asunción Paraguay. ArchivosenMedicina Familiar 2012; 14(4): 93-112.
23. Nisly JL. Re: The emergence of primary care in Latin America: reflections from the field. Journal of the American Board of Family Medicine 2013; 26(5): 612.
24. Wood M. 'El ano del humo': Nicaragua health care in context. Project report. St. Ollaf College; 2013.
25. Norris TE. Establishing a rural curriculum from an urban academic medical center. First. In: AB Chater, J Rourke, ID Couper, RP Strasser, S Reid (Eds). WONCA rural medical education guidebook. Bangrak: WONCA Working Group on Rural Practice; 1-9. (Online) 2014. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice/ruralguidebook.aspx (Accessed 4 July 2014).
26. Grobler L, Marais BJ, Mabunda SA,Marindi PA, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Review 1; Art No.CD005314. doi: 10.1002/14651858.CD005314.pub2. (Online) 2009. Available: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD005314.pub2/abstract (Accessed 8 July 2014).
27. Williamson MI, Wilson R, McKechnie R, Ross J. Does the positive influence of an undergraduate rural placement persist into postgraduate years? Rural and Remote Health 12: 2011. (Online) 2012. Available: www.rrh.org.au (Accessed 30 August 2014).
28. Bollinger M. Rural residency programs: my case for a community-based curriculum. Canadian Family Physician 2014; 60: 187-188.
29. Smith J, Hays R. Is rural medicine a separate discipline? Australian Journal of Rural Health 2004; 12(2): 67-72.
30. Green BN, Johnson CD, Adams A. Writing narrative literature reviews for peer-reviewed journals: secrets of the trade. Journal of Chiropractic Medicine 2001; 15: 5-19.
31. Haig A, Dozier M. BEME Guide No 3: systematic searching for evidence in medical education - Part 1: Sources of information. Medical Teacher 2003; 25(4): 352-363.
32. Grey Literature Database. What is grey literature? (Online). Available: http://www.greylit.org/about (Accessed 8 July 2014).
33. Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, et al. Guidance on the conduct of narrative synthesis in systematic reviews. National Center for Research Methods: Lancaster, UK, 2006.
34. Islam MM, Topp L, Day CA, Dawson A, Conigrave KM. The accessibility, acceptability, health impact and cost implications of primary healthcare outlets that target injecting drug users: a narrative synthesis of literature. International Journal on Drug Policy 2012; 23(2): 94-102.
35. Jeon YH, Glasgow NJ, Merlyn T, Sansoni E. Policy options to improve leadership of middle managers in the Australian residential aged care setting: a narrative synthesis. BMC Health Services Research 10: 190. (Online) 2010. Available: http://www.biomedcentral.com/1472-6963/10/190 (Accessed 8 September 2014).
36. Thomas RD. A general inductive approach for analyzing qualitative evaluation data. American Journal of Evaluation 2006; 27(2): 237-246.
37. Bhatt S. Health care issues facing the Maya people of the Guatemalan Highlands: the current state of care and recommendations for improvement. Journal of Global Health Perspective 1 August. (Online) 2012. Available: http://jglobalhealth.org/article/health-care-issues-facing-the-maya-people-of-the-guatemalan-highlands-the-current-state-of-care-and-recommendations-for-improvement-2 (Accessed 13 March 2014).
38. Borrell RM. Educacion medica hacia la APS renovada y libros de texto, Conference proceedings, 3-15 December 2012, Buenos Aires, Argentina: Pan American Health Organization. 2012.
39. Borrell RM. Educación médica?: ¿Hacia dónde ir?? Pan American Health Organization. (Online) 2012. Available: http://observatoriorh.org (Accessed 15 December 2013).
40. Borrell RM, Goude C, Kauffman R. Residencias médicas en América Latina. Washington DC: Pan American Health Organization, 2011.
41. Vazquez-Martinez FD. Competencias profesionales de los pasantes de enfermería, medicina y odontología en servicio social en México. Revista Panamericana de Salud Pública 2010; 28(3): 298-304.
42. Gracia F. Medical education in Panama. Panama City, Panama: American College of Physicians, Central America Chapter, 2009.
43. Palma C. Dos escuelas de medicina abrirán sus puertas en enero. El Periódico de Guatemala 30 October. (Online). Available: https://elperiodico.com.gt/es/ Accessed 8 June 2014).
44. Eduardo C, Flórez P. Los grandes paradigmas de la educación médica en Latinoamérica. Acta Medica Colombiana 2008; 33: 33-41.
45. Pulido P, Cravioto A, Pereda A, Rondon R, Pereira G. Changes, trends and challenges of medical education in Latin America. Medical Teacher 2006; 28(1): 24-29.
46. Lopez-Bárcena JJ, González-de Cossio Ortiz M, Velasco-Martínez M. Servicio Social de Medicina en México. Factibilidad del cumplimiento académico en el área rural. Revista Facultad Medica Universidad Nacional Autonoma de Mejico. 2004; 47(5): 181-186.
47. Sancho-Ugalde H. Mata-Roldan S. Perspectivas del servicio médico social en Costa Rica. Acta Medica Costarricense 2000; 42(2): 71-75.
48. Pulido P. Medical practice and medical education in Latin America. Education for Health 1996; 9(3): 289-306.
49. Herrera G, Carrino, Herrera L (Eds). Social and Community Service in Medical Training and Professional Practice. Conference proceedings, 24-27 March 1993, Washington DC. New York, NY. Josiah Macy Jr Foundation; 1995.
50. Gavagan TF, Buitrago MC. Report on Family Medicine in the Nicaraguan Revolution: Advances and Obstacles 1985-1991. Family Medicine 1992; 24: 66-70.
51. Frenk-Mora J, Robledo-Vera C, Nigenda-Lopez G, Ramirez-Cuadra C, Galvan-Martinez O, Ramirez-Avila J. Políticas de formación y empleo de médicos en Mexico 1917-1988. Salud Publica de Mexico 1990; 32(4): 440-448.
52. Westreich L. Modern , medical training confronts Guatemalan poverty. Minnesota Medicine 1990; 73: 19-22.
53. Pulido P. Strategies for developing innovative programs in international medical education: a viewpoint from Latin America. Academic Medicine 1989: 64(1): S17-S22.
54. Slater RG. Reflections on curative health care in Nicaragua. American Journal of Public Health 1989; 79(5): 646-651.
55. Haze FA. The Need to Train Physicians for Rural Primary Health Care in Latin America?: Some Family Medicine. Journal of Rural Health 1988; 4(1): 13-21.
56. Braveman P, Mora F. Training physicians for Community-Orientated Primary Care in Latin America: model programs in Mexico, Nicaragua and Costa Rica. American Journal of Public Health 1, 987; 77, , (4): 485-490.57. Leonardia JA, Prytherch H, Ronquillo K, Nodora RG, Ruppel A. Assessment of factors influencing retention in the Philippine National Rural Physician Deployment Program. BMC Health Services Research 12(1): 411. (Online) 2012. Available: http://www.biomedcentral.com/1472-6963/12/411 (Accessed 31 August 2014).
58. Rourke J. How can medical schools contribute to the education, recruitment and retention of rural physicians in their region? Bulletin of World Health Organization 2010; 88(5): 395-396.
59. Clark TR, Freedman SB. Medical graduates becoming rural doctors: rural background versus extended rural placement. Medical Journal of Australia 2013; 199: 779-782.
60. Territorio Chile: Subsecretaria de Desarrollo Regional y Administrativo Gobierno de Chile. Programa Internado Rural Interdisciplinario PIRI. (Online). Available: http://www.territoriochile.cl/1516/article-76513.html (Accessed 3 August 2014).
61. Sturmberg JP, Reid AL, Thacker JL, et al. A community based, patient-center, longitudinal medical curriculum. Rural and Remote Health 3(2): 210. (Online) 2003. Available: www.rrh.org.au (Accessed 13 January 2014)
62. Van Schalkwyk SC, Bezuidenhout J, Conradie HH, Fish T, Kok NJ, Van Heerden BH, et al. 'Going rural': driving change through a rural medical education innovation. Rural and Remote Health 14: 2493. (Online) 2014. Available: www.rrh.org.au (Accessed 30 August 2014).
63. Zink T, Halaas GW, Finstad D, Brooks KD. The rural physician associate program: for third-year medical students. Journal for Rural Health 2008; 4(4): 353-359.
64. Knox L, Ceitlin J, Hahn RG. Slow progress: predoctoral education in family medicine in four Latin American countries. Family Medicine 2003; 35(8): 591-595.
65. Pan American Health Organization. Regional Observatory of Human Resources in Health. (Online) 2012. Available: http://www.observatoriorh.org (Accessed 6 August 2014).
66. Pan American Health Organization Center of Spanish Cooperation. Clínica virtual docente busca fortalecer competencias clínicas en áreas indígenas y de difícil acceso. (Online). 2013. Available: http://www.paho.org/blogs/esp/?p=3808 (Accessed 24 August 2014).
67. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
68. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26(3): 265-272.
69. Frehywot S, Mullan F, Payne PW, Ross H. Compulsory service programmes for recruiting health workers in remote and rural areas: do they work? Bulletin of World Health Organization 2010; 88(5): 364-370.
70. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 9(2): 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 8 August 2014).
71. Strasser R, Worley P, Hays R, Togno J. Developing social capital: community participation in rural health services. In: Leaping the Boundary Fence: Using Evidence and Collaboration to Build Healthier Rural Communities The 5th National Rural Health Conference; 14-17 March 1999; Adelaide, South Australia, 406-412.
72. Talib ZM, Baingana RK, Sagay AS, Van Schalkwyk SC, Mehtsun S, Kiguli-Malwadde E. Investing in community-based education to improve the quality, quantity, and retention of physicians in three African countries. Education for Health 2014; 26(2): 109-114.
73. Leon M. Perceptions of health care quality in Central America. International Journal for Quality in Health Care 2010; 15(1): 67-71.
74. Berry NS. Who's judging the quality of care? Indigenous Maya and the problem of 'not being attended'. Medical Anthropology 2008; 27(2): 164-189.
75. Montenegro RA, Stephens C. Indigenous health in Latin America and the Caribbean. Lancet 2006; 367(9525): 1859-1869.
76. Van Schalkwyk S, Bezuidenhout J, Burch VC, Clarke M, Conradie H, van Heerden B, et al. Developing an educational research framework for evaluating rural training of health professionals: a case for innovation. Medical Teacher 2012; 34(12): 1064-1069.



