The fourth Millennium Development Goal of reducing child mortality cannot be met without substantial reduction in early neonatal deaths1. Perinatal mortality reflects the quality of health care during pregnancy and early neonatal period. Most of these deaths are potentially preventable with good quality health services, including antenatal and intranatal care2.
In India, perinatal mortality rate (PMR) stood at 32 per 1000 births in 2010. It is high in rural areas (35/1000) compared to urban areas (23/1000). The PMR significantly varied across the states, Kerala (13/1000) being the lowest and Madhya Pradesh and Chhattisgarh (45/1000) being the highest3.
Despite remarkable progress in health, there are people living in isolation far away from modern civilization with their traditional values, customs, beliefs and myths intact. About half the world's tribal people, comprising 635 tribal communities, live in India4. They form approximately 8% of the total population5. The health status of tribal populations is very poor because of marginalization, a lack of health facilities and roads, poor access to the developmental process and cultural beliefs6.
Jawadhi Hills is a part of the Eastern Ghats in the state of Tamil Nadu in southern India. With limited road access and poorly developed infrastructure for health care, the population faces many challenges in health. The Community Health Department of Christian Medical College, Vellore, has been involved in health-related activities in this region for a population of around 25 000. Since 2008, the program has been enhanced through special funding to make comprehensive health service and development opportunities available for this population. Over the past two years, a vital reporting system has been developed, bringing attention to a very high perinatal mortality rate of around 150 per 1000 births, which is five times higher than the state average7.
The objective of the current study was to identify the causes and risk factors for perinatal deaths in the tribal population of Jawadhi Hills. Identification of causes and risk factors for perinatal mortality will enable policy-makers and service providers to plan and implement targeted activities to reduce perinatal deaths in the region.
Study setting
The Jawadhi Hills are one of the largest range of hills in the Eastern Ghats, in the northern part of the state of Tamil Nadu in south-eastern India. About 80 km wide and 32 km long, they lie at an altitude of 720-1070 m above sea level. Their steep south-eastern flanks are forested with sandalwood. The hills are sparsely populated. Many of the residents of the Jawadhi Hills, including women, work as migratory laborers in tea estates of the neighboring state. People are organized in hamlets, each with 30-40 huts and placed between valley and plains. The time taken to travel between hamlets is very long because of the hilly terrain. The main thrust of the Community Health and Development Program, run by the Community Health Department of Christian Medical College in Jawadhi Hills, is in the area of maternal and child health. At the village level, there is a set of trained health and development workers. They are supervised by supervisors and auxiliaries, who in turn are supervised by public health nurses and doctors. Data about health-related events, including perinatal and neonatal deaths, are collected on a regular basis, by making home visits, and entered into a computerized health information system. These data are periodically subjected to validation and checks, and are reviewed every month.
Study design: community-based case control study
Definition of cases and controls: A case is defined as a perinatal death (either a stillbirth or a late fetal death (>28 weeks gestation) or a live birth with early neonatal death (<7 completed days since birth) in the study population who delivered during the study period. Controls were chosen by simple random sampling from a sampling frame of all children who were born alive in the study population, ±7 days from the day of birth of the case and the baby being alive and well on the seventh day of life. Controls were chosen from the health information system of the Community Health and Development Program described earlier. All the cases registered in the study period were included in this study.
Sample size: Sample size was calculated with an alpha error of 5% and a beta error of 20% and an anticipated odds ratio (OR) of 4. With an assumption of proportion of controls with 'preterm' as 10% and for three controls per case, the number of cases needed was calculated to be 32 and controls to be 96.
Study tools: Mothers of all cases and controls were interviewed at their home within two weeks of the event. The questionnaire included demographic information, and a detailed antenatal, intranatal and postnatal history. Accessibility was measured in terms of minimum time to reach the nearest health facility. The International Standard Verbal Autopsy Questionnaire developed by WHO was used to identify probable cause of deaths8. The purpose of the questionnaire was to distinguish between stillbirths and early neonatal deaths and to determine the causes of those perinatal events and deaths. The questionnaire contains extensive questions concerning the history of the pregnancy, the delivery, the condition of the baby soon after birth, and the mother's health and contextual factors.
Analysis: Data entry was done using the software Epi-Info2002 v3.5.1 (http://epi-info.software.informer.com/3.5). Statistical Analysis Software v12.0 (SAS Institute; www.sas.com) was used for the analysis. Descriptive statistics for causes of death were carried out. Univariate analysis for factors associated with perinatal deaths was carried out, generating OR and 95% confidence intervals (CI). Selected variables were then entered into a logistic regression model.
Ethics approval
The study was approved by the Institutional Review Board and Ethics Committee at the Christian Medical College, Vellore (No. 7371/2011). Community consent was taken from leaders and written informed consent was obtained from all study participants.
During the study period from 1 February to 30 July 2012, 288 births and 43 perinatal deaths were reported with a perinatal mortality rate of 149.3/1000 births (95% CI for perinatal mortality rate is 107-190/1000 births). Data were collected from 40 cases and 110 controls. Information was not obtained from three cases and ten controls as they had migrated or were not available at their home during the time of interview.
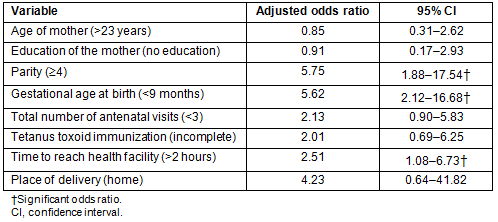
There were 22 early neonatal deaths and 18 stillbirths. Of the early neonatal deaths, 63.6% happened within 24 hours of birth. The probable causes of perinatal deaths based on verbal autopsy are shown in Table 1.
Out of the 40 perinatal deaths, 16 (40%) were probable preterm births as reported by the mothers. Among the 40 cases, the cause of death for 17.5% were probable sepsis, 12.5% were birth asphyxias and another 10% were due to abnormal presentations leading to prolonged labor and birth asphyxia. Three (7.5%) women had reported loss of fetal movements after a significant fall. Infanticide was suspected in eight (20%) instances. No conclusions could be arrived at after verbal autopsy for four cases.
The age of the mother was dichotomized with the median age of mothers of controls (23 years); the age of mothers was less than 23 in 35% of the cases and 50.9% of the control group (p=0.061). Around 90% of mothers who had perinatal deaths did not receive any formal education in comparison to the 78.2% in the control group (p=0.12). Among the study participants, 60% of cases and 63.3% of controls lived in huts (p=0.843). Univariate analysis of factors associated with perinatal deaths is shown in Table 2.
Of the cases, 25% had at least two living children other than this pregnancy, while 11.8% of the controls had the same (p=0.009). The odds of high parity (order of pregnancy more than or equal to four) was 5.25 (95% CI 1.60-17.17) times higher among the cases than among the controls. The OR for those who were para 2, 3 and 4, with para 1 as the reference category, were 5.46, 6.87 and 12.6 respectively.
Among the study participants, 37.5% of the cases had at least three antenatal check-ups, while 78.2% of the controls had the same (OR 2.79, 95% CI 1.28-6.08). Mothers who had registered in an antenatal clinic four months or later (including those who had not registered) had an OR of 1.06 (95% CI 0.49-2.26) for perinatal death as compared to mothers who registered early before four months. Incomplete immunization with tetanus toxoid had OR 2.6 (95% CI 1.05-6.34) for perinatal deaths as compared to mothers who had complete immunization.
About 30% of mothers in the case group said delivery happened before nine lunar months of gestation, while the figure was 2.7% among the control group (OR 6. 95%, CI 2.47-14.58). Among the cases, 92.5% had home deliveries while this happened in 89.1% of the controls (p=0.091). In 82.5% of cases and 82.7% of controls, delivery was conducted by relatives. Delivery being conducted by an untrained person had OR 1.76 (95% CI 0.56-5.56) as compared to deliveries conducted by trained persons. There were four abnormal presentations and all resulted in perinatal deaths. No association was found between sex of the baby and perinatal deaths (p=0.12). In 44.5% of controls and 15% of cases, a new blade was used to cut the umbilical cord. Those who had to travel more than two hours to reach a health facility had OR 2.67 (95% CI 1.22-5.85) for perinatal death as compared to those living in places from where the healthcare facility could be reached within two hours.
A logistic regression model was generated by including age of mother, education of mother, preterm/term, time to reach nearest health facility >2 hours, total number of antenatal visits (<3), immunization with tetanus toxoid (incomplete) and place of delivery (home) as the independent variables (Table 3). In the final model, parity ≥4 (OR 5.75 [95% CI 1.88-17.54]), preterm births (OR 5.62 [95% CI 2.12-16.68]) and time to reach the nearest health facility more than 2 hours (OR 2.51 [95% CI 1.08-6.73]) were significantly associated with the perinatal deaths.
Table 1: Causes of perinatal deaths as identified by verbal autopsy
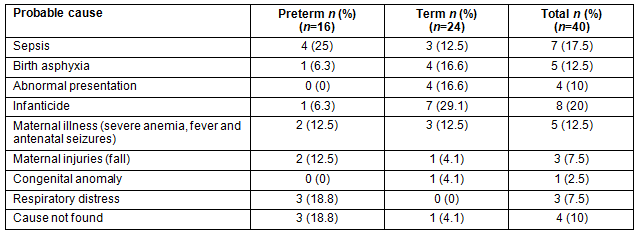
Table 2: Univariate analysis of factors associated with perinatal deaths
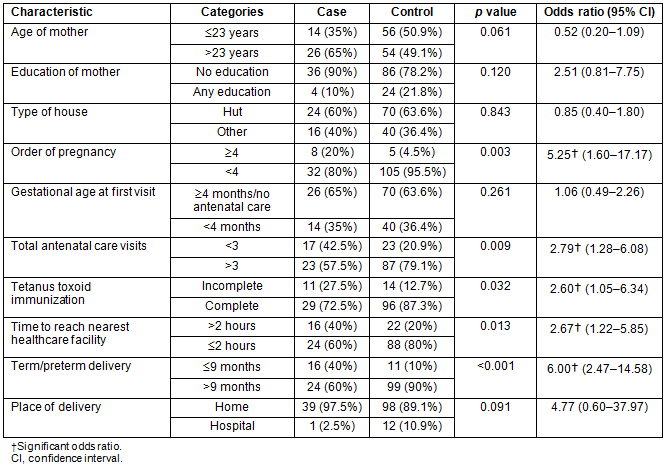
Table 3: Logistic regression model showing factors associated with perinatal deaths
Discussion
In spite of the tremendous advancement in the field of medicine, the healthcare delivery in the tribal people is poor and needs to be strengthened in order to achieve the goal of health for all in the country. The current study aimed to identify causes and risk factors for high perinatal deaths in a tribal population. The major findings of the study were as follows. Among the perinatal deaths, 40% were preterm births. Sepsis (17.5%) and birth asphyxias (12.5%) were the major causes of deaths. In the final logistic regression model, parity ≥4 (OR 5.72 [95% CI 1.18-17.52]), preterm births (OR 5.89 [95% CI 2.1916.24]) and time to reach the nearest health facility more than two hours (OR 2.54 [95% CI 1.09-6.79]) were significantly associated with the perinatal deaths. There were four abnormal presentations and all resulted in perinatal deaths. Among the cases, 92.5% had a home birth compared to 89.1% among the controls.
High parity of mother was associated with perinatal death in the study. A dose-response relationship was observed with increasing parity. This finding was consistent with a study done in Kenya to determine risk factors for perinatal mortality9. Whether increasing parity is a risk factor for perinatal death or whether it was a result of high perinatal mortality in the region needs to be elucidated further. It is possible that high mortality rate would have led to the practice of not restricting the number of children. Pregnancies would not have been adequately spaced and this would have led to high perinatal mortality. It is possible that lack of awareness regarding contraception and termination of pregnancy were the reason for increasing fertility, and if parents did not really want that child, it would have resulted in an infanticide in early neonatal period.
All abnormal presentations could have been picked up if the women had an antenatal check-up near term or if they had delivered in a health center. These deaths were potentially preventable provided there was a system for antenatal care that was accessible and affordable. Three women reported falls during pregnancy followed by loss of fetal movements. This could be because of the difficult terrain. Probable infanticide was identified as the cause of death in 20% of all deaths, which was disturbing. Previous reports of infanticides have been reported from these areas during the monthly cluster meetings and reports by health workers. This study has not addressed the factors leading to infanticide adequately. Well-planned qualitative studies are needed to further explore infanticide and the factors leading to it.
Prematurity was a significant risk factor for perinatal deaths. Preterm babies are prone to neonatal deaths due to the immature respiratory system or low birth weight. They are also at high risk of developing sepsis. Bed rest has been traditionally the most accepted way of preventing preterm labour, as well as in arresting the progression of threatened preterm labour, but adequate rest would not have happened for mothers living in a difficult terrain, most of whom work to earn a living, and the majority of whom migrate to other states seeking jobs.
Time taken to reach a health facility has been described as a risk factor for neonatal and perinatal mortality in developing countries10,11. A large proportion of women in the Jawadhi Hills need to travel more than two hours to reach a health facility. Most of the roads are difficult to navigate. They had to climb steep areas or cross mountain streams to reach a health center. Time taken to reach a health facility and lack of appropriate means of transport might have de-motivated people living in difficult terrains to approach a health center either for antenatal care or for delivery. Poor accessibility also prevents healthcare workers from reaching those places and delivering services.
The number of antenatal visits and incomplete immunization with tetanus toxoid were significantly associated with perinatal deaths in the univariate analysis. This study showed that the quality of antenatal care in terms of early identification of pregnancy, number of antenatal visits, immunization, identifying high risk factors and referring appropriately was grossly inadequate and needs improvement. Most of the deliveries were at home and conducted by relatives or friends. The unhealthy practices of cutting the cord with unsterile instruments and applying oil to the umbilical stump still prevails in these communities.
Although verbal autopsies are generally accepted as tools for measuring mortality in many countries without vital registration, their validity and sensitivity vary widely between locations12. But they are the only available tool to identify cause of death in an area where most of the deliveries happen at home and the healthcare sector has not been well established. Some questions such as gestation at birth would have been affected by recall and reporting bias by the mothers. Including a qualitative design such as a focus group discussion or key informant interview in addition to the current design would have helped to explore the unknown risk factors for perinatal mortality and helped to deal with sensitive issues such as infanticide. The study is powered to detect an OR≥4, which is a very high value. The power of the study was not enough to assess some variables and the outcomes that reflect the complexity of the interrelations present among these variables. Owing to the small sample size, bias due to multiple testing while doing regression might be present.
Perinatal mortality is high in the Jawadhi Hills and factors such as prematurity, poor accessibility and high parity were significantly associated with perinatal deaths. The issue not only has medical dimensions; it also has social dimensions. High prevalence of home deliveries is a problem and professionally designed behaviour change communication is needed for promoting institutional deliveries. Considering the fact that most deliveries in these areas will continue to be at home, birth attendants should be appropriately trained in safe delivery and cord care. Socioculturally appropriate, evidence-based strategies are needed, focusing on improving coverage of antenatal and family welfare services, promoting institutional deliveries, strengthening health systems and ensuring community participation.
References
1. Lawn JE, Cousens S, Bhutta ZA. Why are 4 million newborn babies dying each year? Lancet 2004; 364: 399-401.
2. World Health Organization. Neonatal and perinatal mortality. Geneva: WHO, 2006.
3. Ministry of Health and Family Welfare. Family Welfare Statistics in India. (Online) 2011. Available: http://mohfw.nic.in/data/1892/972971120 (Accessed 3 April 2014).
4. Central Intelligence Agency (CIA). Field Listing: Ethnic groups, CIA World Factbook 2009. Available: https://www.cia.gov. (Accessed 17 June 2014).
5. Ministry of Home Affairs. Census of India. (Online) 2011. Available: http://www.censusindia.net (Accessed 4 April 2014).
6. Souderssanne MB, Thiruselvakumar D. Overcoming problems in the practice of public health among tribals of India. Indian Journal of Community Medicine 2009; 34: 283-287.
7. International Institute for Population Sciences and Macro International. National Family Health Survey (NFHS-3), India, 2005-06: Tamil Nadu. (Online) 2008. Available: http://rchiips.org/NFHS/NFHS-3%20Data/TamilNadu_report.pdf (Accessed 3 November 2014).
8. World Health Organization. International standard verbal autopsy questionnaire 1. Geneva: WHO, 2007.
9. Anne AK, Patrick MN. Factors associated with perinatal deaths in Kenya. Proceedings of the Fifth African Population Conference, Tanzania, 10-14 December 2007.
10. Beatrice A. Risk factors for perinatal mortality in Arua regional referral hospital. Uganda. East African Journal of Public Health 2000; 5(3): 34-37.
11. Emmanuel T, Notion G, Gerald S, Chadambuka, Tshimamga M, Simukai Z. Determinants of perinatal mortality in Marondera district, Mashonaland East Province of Zimbabwe. Pan African Medicine Journal 2011; 8: 7.
12. Aggarwal AK, Jain V, Rajesh Kumar. Validity of verbal autopsy for ascertaining the causes of stillbirth. Bulletin of the World Health Organization 2011; 89: 31-40.

