The unequal and inequitable distribution of the medical workforce between rural and urban parts of Australia1 has been well documented. Commonwealth and state governments have introduced several significant initiatives in an attempt to address this imbalance, including recruitment of many overseas trained doctors2. One longer-term initiative is the funding of university departments of rural health and rural clinical schools3 in medical schools. In essence the aim here is to develop a rural academic infrastructure through which medical students can receive significant parts of their clinical training. It is known that medical students that receive rural undergraduate training are more likely to become rural doctors4.
Because rural clinical schools have only been established in the last few years there are no published data on their impact on the rural medical workforce. Fundamentally, the key measure of success of the rural clinical schools will be an increase in the number of Australian rural doctors. Thus, long-term monitoring and evaluation will be necessary to test this. However, the first sign of success would probably be an increase in the number of interns seeking to work in rural and regional hospitals. We provide evidence from Queensland that this is indeed starting to happen.
Methods
Setting
The School of Medicine at The University of Queensland is among Australia's largest, and approximately 320 students enrolled in this graduate medical program in 2004. The first 2 years of the program are delivered using a problem-based approach and, in the second 2 years, students learn through core clinical rotations. Rotations are medicine, surgery, rural health, general practice and mental heath in 3rd year, and obstetrics, child health, surgical specialties, medical specialties and electives in 4th year.
All students spend 8 weeks on a rural health rotation and at least 25% of students spend all of 3rd or 4th year in the rural clinical division doing the same core rotations as the urban students. Some choose to spend both 3rd and 4th years in the rural clinical division.
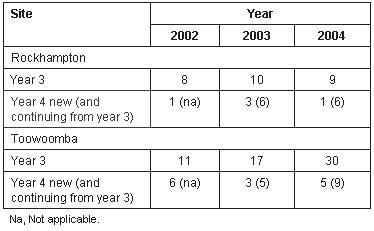
The rural clinical division has two schools, one in Rockhampton (central Queensland) and one in Toowooomba (south west Queensland), based in and around the regional hospitals in the two towns. For both sites the number of students spending 3rd year and 4th year there is shown (Table 1).
Table 1: Number of students spending 3rd and 4th year at Toowoomba and Rockhampton Hospitals
Intern allocation
In Queensland, interns are allocated to hospitals across the State according to a ballot run by the University of Queensland medical student society, with support from Queensland Health. A small number of students are exempted from the ballot due to specific social and family circumstances. Students who hold Queensland Health Rural Scholarships are allocated to specific hospitals (rural or urban) that will provide them with the experience that they need prior to subsequent bonded rural service. All students express a preference for which hospital they would like to work in and the first preference is provided wherever possible. Hospitals unable to fill their intern places from University of Queensland graduates seek doctors from interstate and overseas.
Data collection and analysis
We set out to answer the question: 'What has been the impact of the rural clinical division on the preference for and demand for intern placements in the associated regional hospitals?' To answer this question we sourced data on intern preferences from Queensland Health and also on the source of interns who worked at the hospitals from the hospitals themselves.
As student placements started in 2003 we collected data from 2001 onwards to allow a time series analysis before and after the development of the schools. We also collected similar data from Mackay Hospital (on the central Queensland coast) as an external control as the rural clinical division does not have a presence there. We did not collect data for Townsville and Cairns because of the confounding effect on these sites of the activity of the University of Queensland Northern Clinical School and subsequently the James Cook University Medical School.
Results
First preferences
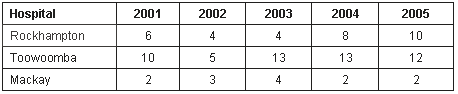
The number of medical students selecting Rockhampton Hospital as their first preference site for intern employment increased from six and four in 2001 and 2002, to eight and 10 in 2004 and 2005. For Toowoomba, first preferences increased from 10 and five in 2001 and 2002, to 13 and 12 in 2003 and 2004. For Mackay, first preferences were stable at two and three in 2001 and 2002 and two and two in 2004 (Table 2).
Table 2: Number of first preferences made for intern places from University of Queensland graduates at Rockhampton, Toowoomba and Mackay Hospitals in the intern ballots for 2001-2005.
Source of interns
Rockhampton Hospital offered 10 intern places each year between 2001 and 2005 (Table 3). University of Queensland graduates filled six or seven of these places between 2001 and 2003, while two interns were recruited from overseas in 2001 and three from interstate in 2002. University of Queensland graduates filled all intern places for 2004 and 2005. Excluding scholarship holders as a special (bonded) category, while in 2001 and 2002, zero and one intern chose to work at Rockhampton, in 2004 and 2005, seven and six chose to work at this hospital. In contrast to all previous years, in 2005 no interns were allocated to Rockhampton.
Table 3: Changes in source of interns at Rockhampton, Toowoomba and Mackay Hospitals 2001-2005
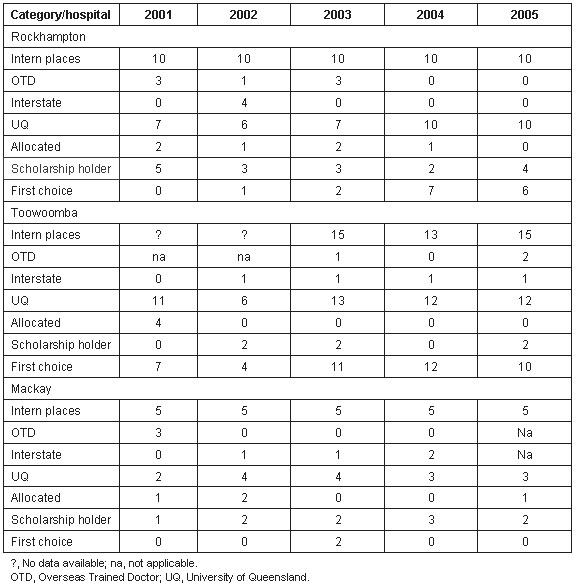
Toowoomba Hospital has offered approximately 15 intern places each year. Toowoomba has continued to recruit one to two interns from overseas or interstate each year with UQ providing 12/13 interns in 2004 and 13/14 in 2005, an increase from 11 and six in 2001 and 2002 respectively (Table 3).
Mackay continues to need to source interns from interstate and overseas with UQ graduates providing only 3/5 interns (60%) in 2004 and 2005.
At Rockhampton in 2004, all interns had spent 3rd year in the rural clinical division, while only five of the 10 interns in 2005 had done this. For Toowoomba, in 2004, seven of 12 interns had spent all 3rd year there, and in 2005, three had.
Discussion
These data provide evidence that since the rural clinical schools were established in Rockhampton and Toowoomba in 2003, interns are more likely to seek to work in the hospitals in these towns. There has been an increase in the number of medical students choosing these two hospitals as their first preference for internship, while there has been no change in preferences at Mackay. All interns at Rockhampton and almost all at Toowoomba are now supplied by the UQ, while Mackay still relies on overseas and interstate applicants. Interestingly, not all interns choosing to work in the regional hospitals had spent their whole 3rd year in the rural clinical school, and the number doing so was lower for the 2005 intern intake than for 2004.
Some caution needs to be applied in interpreting these data. First, the numbers are relatively small and, second, we are studying trends over a fairly short period of time. Nevertheless, the same positive trend is observed in both Rockhampton and Toowoomba, while the situation in Mackay, an external control, has remained stable. The increases in first preferences, reductions in overseas trained and interstate doctors, and increases in the number of interns choosing to work in the two study sites are consistent with each other and with the hypothesis that exposing students to rural medicine during their undergraduate study increases the chance of them choosing rural practice as a career4. Choice of rural internship is a positive first step. It seems unlikely that changes in policy relating to Queensland Health scholarship holders account for these changes because there has been no increase in their numbers (Table 3) and any changes would not explain changes in first preferences. In short, we provide early evidence that the rural clinical division of the School of Medicine at UQ is already having a positive impact on the rural medical workforce.
It will be important to continue to monitor these trends, and to conduct similar evaluations in other jurisdictions. With many millions of dollars being spent on the rural clinical school initiatives it is vital that rigorous evaluation occur. A number of issues arise from this study.
First, it is interesting to note that although the popularity of Rockhampton and Toowoomba as internship locations seems to have increased, not all interns working there had spent all their 3rd (or 4th) year there. Hence, while we have good evidence that duration of exposure to rural life and rural practice increases the likelihood of a rural career5, it seems that not all students that spend all 3rd (or 4th) year in the rural clinical division will subsequently do a rural internship, at least in the same sites. Informal discussion with some students suggests that while they very much enjoy a rural 3rd year (and some do a rural 4th year too) they then wish to change location for internship, seeking a broader medical exposure and change of scene. Only a long-term cohort study will definitively determine whether these students are subsequently more likely to be rural doctors for a significant part of their working life. It would not be surprising if other factors influenced students' choice of internship location, and factors such as personal relationships have been mentioned in discussions we have had with students.
Second, and related to this first issue, it seems that news of the positive experience that students on long-term placements typically have in the rural clinical division may spread rapidly to their peers, some of whom are then motivated to do an internship in a regional setting. This may, of course, be positively influenced by their own 8 week rural rotation too.
There has been a significant investment in the establishment and ongoing operations of the rural clinical schools across Australia. Our data suggest that further funding may be warranted as a way of extending coverage to all regional and rural hospitals that take interns. The UQ is currently expanding its activity to include Hervey Bay and other central Queensland sites. Nationally, the rural clinical school program should ensure that all regional hospitals employing interns have the opportunity to accept undergraduate student placements. Increasing the number of rural interns is important because there is evidence that they are more likely subsequently to become rural general practitioners6.
Acknowledgements
The authors acknowledge Janelle Coe and Donna Georgeson who coordinated data collection from the hospitals, and the Queensland Health staff who provided preference data.
References
1. Johnstone G, Wilkinson D. Increasingly inequitable distribution of general practitioners in Australia, 1986-1996. Australian and New Zealand Journal of Public Health 2001; 25: 66-70.
2. Couper I, Worley PS. The ethics of international recruitment. Rural and Remote Health 2: 196. (Online) 2002. Available http://rrh.org.au (Accessed 11 November 2004).
3. Humphreys JS, Lyle D, Wakerman J, Chalmers E et al. Roles and activities of the Commonwealth Government Departments of Rural Health. Australian Journal of Rural Health 2000; 8: 120-133.
4. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
5. Laven GA, Beilby J, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
6. Peach HG, Trembath M, Fensling B. A case for more year long internships outside metropolitan areas? Medical Journal of Australia 2004; 180: 106-108.
Abstract
Introduction: The unequal and inequitable distribution of the medical workforce between rural and urban parts of Australia has been well documented. Commonwealth and state governments have introduced several significant initiatives in an attempt to address this imbalance, including recruitment of many overseas trained doctors. One longer-term initiative is the funding of university departments of rural health and rural clinical schools in medical schools. Objective: To determine the impact of the rural clinical division of the School of Medicine at the University of Queensland (UQ), Australia, on the intern workforce in central and southern Queensland, Australia.
Methods: Time series analysis of first preferences for intern allocation among UQ graduates and source of interns (UQ, interstate and overseas) from 2001-2005, and comparison of trends between Rockhampton and Toowoomba (UQ student placements since 2003) with Mackay (no placements).
Results: First preferences for Rockhampton increased from six in 2001 to 10 in 2005, and for Toowoomba from five in 2002 to 12 in 2005, while for Mackay preferences were stable at two. At Rockhampton while two interns came from overseas in 2001 and three were from interstate in 2002, UQ provided all interns in 2004 or 2005. UQ has provided 12/13 interns in 2004 and 13/14 in 2005 for Toowoomba. Mackay continues to source interns from interstate and overseas with UQ providing only 3/5 interns in 2004 and 2005. At Rockhampton, among non-bonded UQ graduates the number of interns choosing to work there increased from zero in 2001 to six in 2005. For Toowoomba, numbers were seven and 10 respectively, while for Mackay it was zero.
Conclusion: UQ's rural clinical division is having a positive impact on the intern workforce in the regional hospitals most closely allied with it.
Key words: interns, Queensland, rural, workforce.
You might also be interested in:
2020 - ‘It’s mostly about the job’ – putting the lens on specialist rural retention




