Achieving equity in access to health care is a top priority of healthcare systems worldwide. Equity in access to healthcare means all people should have equal opportunity to use health care regardless of their socioeconomic status, geographical location, and ethnicity1,2. To ensure equity, adequate allocation of healthcare resources, including human resources, is imperative3. Empirical evidence indicates that ensuring adequate distribution of skilled healthcare workforce could lead to the improvement of patient health outcomes4. Unbalanced distribution of health workforce, particularly physicians, between and within countries is a global longstanding problem contributing to great disparities in health outcomes between rural and urban populations5,6. The uneven distribution of physicians results in the 'law of inverse care': people who most need healthcare services consume the least care7.
The shortage of physicians in rural and remote areas is a commonplace problem in both developed and developing countries5. In countries such as Canada, Australia, and USA, which vary dramatically in size and population density, maldistribution of health workforce in rural and remote areas still remains a challenge8-10. Uneven geographic distribution of physicians is also a major healthcare issue in Iran, a middle-income country with a vast territory and uneven regional economic development. This has led to the aggregation of physicians in urban areas and their shortage in rural and underdeveloped areas11,12.
Numerous factors affect practice location decisions among physicians, such as physicians' personal attributes, community characteristics, socioeconomic factors, and professional issues7,13. There is general agreement that particular personal characteristics of physicians are associated with the recruitment and retention of physicians in rural areas14,15. Male physicians are more likely to practise in rural areas than their female counterparts16,17. Rural background has been shown in many different countries to be a significant factor associated with medical graduates' intentions to practise in rural settings14,18,19. Evidence indicates that students from local medical schools are more likely to enter rural practice in future20. Exposure to rural practice could influence physicians' decisions and attitudes to enter rural practice21,22. Related studies suggest that physicians entering rural field residency or medical students who have pre-vocational experiences in rural communities are more likely to pursue rural practice in their future careers23,24. It is widely perceived that selection of medical students based on pre-determined criteria may increase the likelihood of their retention in rural and remote areas once they are qualified7.
Overview of health system and distribution of physicians in Iran
Iran, a middle-income developing country with a population of 75 million, is one of the most populated countries in the Middle East. The Iranian healthcare system has experienced major reforms through the past three decades. In 1985, the integration of the two systems of healthcare delivery and medical education led to the establishment of the Ministry of Health and Medical Education (MOHME). The main purpose of the integration was to establish a more coordinated approach to healthcare provision and medical education25. MOHME has delegated some of its responsibilities to the medical universities, which all operate under the supervision of MOHME. Medical universities are responsible for training the required workforce for the health system, as well as providing public health services through a three-tiered healthcare system.
For more than a decade, MOHME has invested great efforts aimed at redressing the maldistribution of physicians through a wide array of policies and programs, including increasing the supply of physicians, obligatory community service, and providing financial and non-financial incentives. To increase the supply and improve the distribution of health workforce, particularly physicians, the number of medical universities had increased to 50 in 2014, of which 10 were established in the underdeveloped areas of the country. Training local workforce for underdeveloped areas is one of the main goals of these local medical universities26.
The community service program requires specialist physicians to serve in public facilities for a specified time period following their graduation. They will be allowed to practise in the public and/or private sectors following the completion of the community service. Specialist physicians are assigned across the country based on a number of factors, including the need for specialized care in different areas, physicians' choices, and their personal and educational characteristics (i.e. marital status and the score obtained in specialty certification examination)26.
Although the number of physicians has grown considerably in the past few years, the uneven rural-urban distribution of physicians remains a significant problem that may have implications for health. It means that equitable access to health care in underdeveloped areas and rural communities, where residents experience poorer health outcomes, still poses a serious challenge for the Iranian health system11,12.
To the authors' knowledge, there is no previous study that explores factors affecting physicians' choice of practice location using a large sample in Iran. Therefore, the aim of the present study was to investigate the relationship between personal characteristics of the recently graduated specialist physicians, who must perform community service, and their choice of practice location. This study aimed to investigate what personal characteristics of the newly graduates were associated with an increased likelihood to practise in an underdeveloped area for a community service program.
The study was a cross-sectional study conducted in 2013. The study population consisted of 6673 physicians who graduated from all public medical schools across the country between 2009 and 2012. It should be noted that 2848 of them were not mandated to perform compulsory community service for different reasons, hence they were excluded from the study. Most of the excluded cases were military physicians, for whom working for military organizations was the only choice. Others were physicians who were obliged to perform military service once they graduated. Iran has a mandatory military service for men, which starts at the age of 18. The rest, who accounted for a small number of participants, were overseas specialists with no Iranian citizenship who were to leave the country after their graduation. As a whole, the study participants were those physicians who were free to choose their practice location (n=3825).
In Iran, only public medical schools train specialist physicians; no private medical school has a residency program. The study participants graduated in a range of specialties: orthopedics, urology, pathology, anesthesiology, dermatology, obstetrics and gynecology, neurosurgery, internal medicine, ophthalmology, radiology, neurology, otolaryngology, cardiology, and general surgery.
Physicians' personal data were collected from the MOHME directorate general for personnel. Physicians' personal information included age, sex, specialty, birthplace, the rank of the university attended, place of residence, previous exposure to rural practice, board examination certification, and year of graduation. Further, to categorize the graduates' birthplace and place of residence into two zones (developed and underdeveloped areas), the socioeconomic development index of provinces and regions established by the government was used. The universities where the study participants graduated were categorized as I, II or II - according to the system used by MOHME. Classification of the medical universities has been made on the basis of different criteria (ie number of beds of affiliated hospitals, financial and scientific capacity, number of faculty members, research activities, and efficiency of use of research capacities). Medical schools categorized as type III are not allowed to hold residency and fellowship programs.
The graduates' selected locations were classified as developed, semi-developed, or underdeveloped areas. MOHME has classified the areas according to the level of socioeconomic development of the provinces, geographical location, and infrastructure and health facilities. Due to Iran's geographical vastness, the areas in need of specialists are not necessarily deprived areas. Specialist physicians are allowed to select from among 40 areas to perform their compulsory service. Each area is the catchment area of one of the medical universities. They are not allowed to perform their compulsory service in a number of province capitals and large cities. During the assignment process, physicians did not know if there was any open vacancy in their selected areas. If there was not any open vacancy in their first selected location, the next choice would be considered in the assignment process. Because the current study aimed to assess the relation between physician choice and their personal characteristics, only their first choice was considered as their preferred choice, regardless of the result of the assignment.
To explore the relationship between physicians' attributes and their choice of practice location, data were analyzed using χ2 test and multivariate logistic regression analysis with the assistance of Statistical Package for the Social Sciences software v18 (SPSS; http://www.spss.com). A p-value≤0.05 was considered statistically significant.
Ethics approval
This study received ethics approval from the Ethics Committee of Iran University of Medical Sciences; ethics approval number 92-04-136-24339.
Normality of the distribution was checked using the Kolmogorov-Smirnov (K-S) test (p≥ 0.05, normal distribution). All 3825 graduated physicians who were mandated to perform compulsory community service were included in the study. As Table 1 shows, 60.4% of the physicians were male. The majority of the physicians were married (79.6%) and 80.7% of them graduated from type I medical schools. Most physicians were born and lived in developed areas (92.5% and 91.3%, respectively). Sixty-four percent of physicians had passed the specialty certification examination successfully. The mean age of the study population was 34 years (range, 27-50 years).
Table 2 shows the number of graduates within different specialties. The physicians graduated in 2011 comprised 34% of the study sample. Within the sample, obstetricians and gynecologists made the highest number (14%) and neurosurgeons the lowest (2%).
Table 3 summarizes the results of the χ2 test. The results of the test indicated that the choice of practice location was associated with birthplace, sex, year of graduation, rank of the university attended, place of residence, exposure to rural practice before residency program, and age (p<0.05). Graduates' marital status and holding of board certification were not found to be significantly related to the dependent variable.
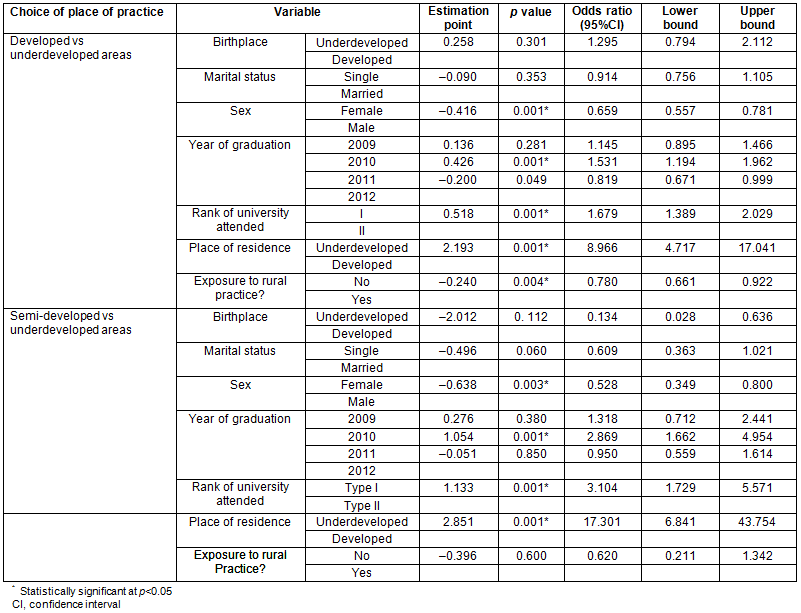
The results of regression analysis are shown in Table 4. The independent variables included birthplace, marital status, sex, year of graduation, rank of the university attended, place of residence, and exposure to rural practice before residency training program. To compare the two groups of graduates (those who chose to practise in the underdeveloped areas and those who chose to practise in the developed areas) logistic regression analysis was used. The results of the analysis revealed that the independent variables (sex, year of graduation, the rank of the university attended, place of residence, and exposure to rural practice before residency training program) were significantly associated with the decision to practise in an underdeveloped area (p≤0.05). The analysis suggested that female physicians were less likely to choose underdeveloped areas to practise as compared with their male counterparts (OR=0.659, 95%CI, 0.557-0.781, p≤0.001). The likelihood of choosing an underdeveloped area to practise increased for those who studied in type I medical schools as compared with those who attended type II medical schools (OR=1.679, 95%CI, 1.389-2.029, p≤0.001). Physicians who lived in the underdeveloped areas were nine times more likely to choose to practise in the underdeveloped areas than those lived in the developed areas (OR=8.966, 95%CI, 4.717-17.041, p≤0.001). Physicians who had no previous exposure to rural practice were less likely to practise in the underdeveloped areas as compared to those who were exposed to rural practice before entering a residency training program (OR=0.780, 95%CI, 0.661-0.922, p=0.004).
According to the regression logistic analysis, variables such as sex, year of graduation, rank of the university attended, and place of residence were significantly different in graduates whose first choice was a developed area as compared to those who selected to practise in a semi-developed area. Female physicians were more likely to select a developed area to practise as compared with male physicians (OR=0.528, 95%CI, 0.349-0.800, p=0.003). Physicians who lived in the underdeveloped areas were 17 times more likely to choose to practise in the underdeveloped areas as compared with those who lived in other parts of country (OR=17.301, 95%CI, 6.841-43.754, p≤0.001).
Table 1: Demographic characteristics of study population
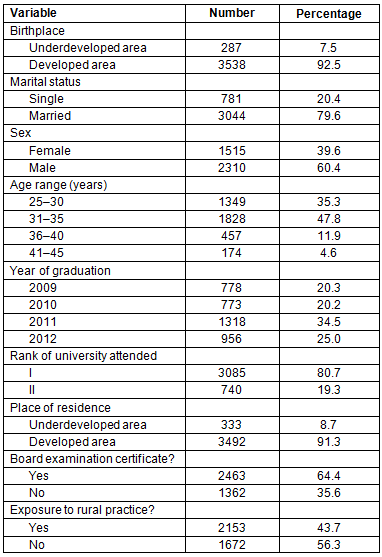
Table 2: Number of graduated physicians by specialty and year of graduation
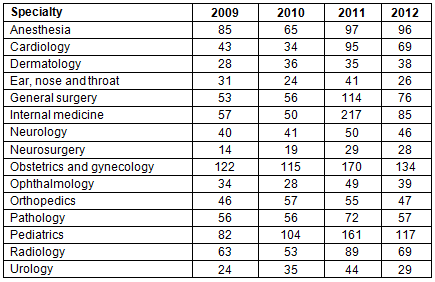
Table 3: Choice of practice location among participants based on personal characteristics: results of χ2 test
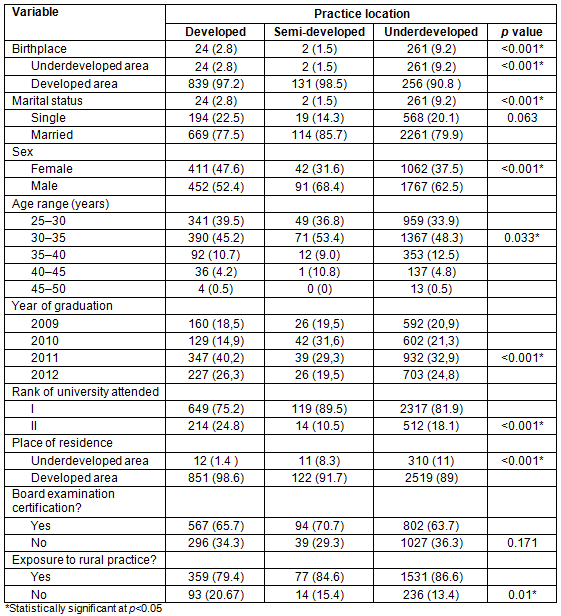
Table 4: Factors predicting practice in underdeveloped areas: results of regression analysis
Discussion
The shortage and uneven distribution of the health workforce represents a longstanding problem in rural and remote areas of Iran, with serious implications for access to healthcare services in such areas. As noted earlier, a number of government national policies have sought to increase the number of rural physicians. There is increasing evidence that the recruitment and retention of physicians in particular areas is affected by multiple factors, including physicians' personal attributes, community characteristics, economic, and professional education factors18. There is a general agreement that personal characteristics of physicians such as growing up in a rural community, exposure to a rural practice during training, marriage to a person from a rural area, and training in family medicine rather than other specialties are associated with the recruitment and retention of physicians in rural areas13. According to the findings of the study, key personal attributes determining initial practice location after graduation among the young Iranian physicians included sex, birthplace, place of residence, and exposure to rural practice before residency program.
This study supports previous findings that female physicians are less likely than their male counterparts to choose rural areas to practise17,18. This may be explained by the fact that the location choice of female physicians is often modified by a number of factors including family responsibilities and commitments, access to good schools for children, spouse's career concerns, and inadequate accommodation facilities in underdeveloped areas7. The literature from other countries has also reported that increase in the number of female physicians would not result in more physicians working in rural areas16-18. A study conducted in the USA concluded that growth in the number of female physicians would not resolve the shortage of physicians in rural and remote areas16. Being a female physician was reported as a negative predictor for rural practice in Japan27. In Australia, both female GPs and female specialists are much less likely to practise in rural locations compared with male physicians18. In Turkey, 86.5% of male physicians and only 13.5% of female physicians tend to work in rural areas17. A study conducted in Iran found that male physicians are more willing to practise in rural areas as compared with female physicians28. According to a previous study, the most common reasons for the unwillingness of Iranian female physicians to practise in rural areas are family issues and lifestyle considerations26.
It should be noted that to address gender imbalance and provide female patients with female physicians, MOHME has increased the number of female physicians in residency programs within most specialties up to 40% since 2000. While the number of women entering medicine has increased in recent years in Iran, there is concern that this could exacerbate the rural physician shortage26. It seems that this policy itself is unlikely to resolve the shortage of female physicians in remote and rural areas of Iran. Thus, it is time to revise the policy. It should be added that, due to the policy implementation, shortage of female physicians has been mostly resolved in large cities and urban areas. Consequently, it could be suggested that increasing the number of male physician admissions to residency programs, particularly in certain specialties that are more in demand in underdeveloped areas, could alleviate the problem of uneven distribution of physicians in underserved areas in the short term. Evidence suggests that rural medical school programs can substantially increase the likelihood of women serving in rural areas19,29. Therefore, to redress the shortage of female physicians in rural and remote areas in the long run, raising the enrollment of female students with rural backgrounds in local medical universities along with providing incentives to encourage them to work in rural settings after graduation may be some other possible strategies.
Unmarried physicians are more prepared to move or migrate because they have less family responsibilities5. However, the findings of the current study suggest that there is not a significant relationship between marital status of physicians and their choice to work in underdeveloped areas. Expectations such as higher income and working in better facilities, as well as the disparity between physicians' income in rural areas and urban areas, could be considered as some reasons for their desire to practice in urban areas.
Numerous studies have elucidated the association between rural background and rural practice18,19. In Turkey, for example, physicians who have particular socioeconomic backgrounds such as rural origin or come from low-income families are more likely to be motivated to work in underdeveloped areas17. The present study also identified rural background as a predictor of choosing underdeveloped areas to practise. However, according to the results, only 7% of the recently graduated physicians were born in underdeveloped areas. Students living in rural communities and underdeveloped regions have less opportunity to enter medical schools due to their socioeconomic background, and lack of access to good schools in such areas. To accelerate progress in achieving social justice, the Iranian parliament passed a law in 2014 that mandated MOHME to increase the number of students with rural background entering public medical schools by 30% across all specialty programs.
Previous exposure to rural practice during undergraduate or postgraduate medical training could influence the subsequent decision to practise in a rural community among physicians21,22,30. Consistent with the findings of prior studies21,23, the present study revealed that physicians who do not have experiences working in rural and remote areas before entering residency training programs are less willing to practise in the underdeveloped areas of the country after their graduation as compared to those who had such exposure. Previous studies also confirmed that working in rural and underdeveloped areas could prepare young physicians to cope with living in rural and remote areas and change their attitudes toward rural practice19,21. It should be noted that the current medical curriculum of the Iranian medical schools, which is primarily a tertiary hospital-based model of medical education, exposes medical students to curative and specialized care. This mainly could reduce the likelihood of entering a rural practice. Providing community-based education, where most of the clinical teaching is centered in the community (eg primary health clinics, small health centers, and rural hospitals), could be an appropriate way to prepare young Iranian physicians for rural practice and to equip them with adequate knowledge and skills to practise in rural settings.
More recently graduated students may have different career expectations than their older counterparts31, which was also observed in the present study. These findings indicate that recently graduated physicians are less likely to practise in underdeveloped areas as compared with those who graduated earlier. There could be several reasons for this. Due to the current economic issues in Iran, it seems that financial factors play a key role in physicians' early career decisions, which motivate them to work in urban areas and large cities to maximize their income. In addition to financial factors, newly graduated physicians may also take into account family and lifestyle factors such as leisure activities, access to good schools for their children, and spouse's employment opportunities in choosing their practice location.
Limitations
Certain limitations need to be acknowledged in the present study. First, as this study is a cross-sectional survey, the results are just a static picture which could not include changes or trends in physicians' job preferences or factors influencing workplace selection among them. Second, this study included a limited number of physicians' personal characteristics; other important factors such as spouse's background and preferences, family background, and salary expectations were not included. Third, due to the nature of the data, birth in a rural community was regarded as having a rural origin. However, in similar studies rural origin was defined as having completed primary or secondary school education in rural communities.
In this study, a number of factors have been found to be significantly associated with the recruitment and retention of physicians in underdeveloped areas of Iran. These findings have several implications that may assist policy-makers in making physician distribution more equitable. More than 90% of specialist physicians in Iran were born and lived in developed areas. Considering the relationship between being born in an underdeveloped area and selecting such areas to perform community service, it seems that the increase in the enrollment of physicians with a rural background in residency programs may solve the problem of uneven distribution of specialist physicians in Iran. Further, experiences in non-urban areas could influence their decisions as to where to practise. Also, because female physicians have less desire to live in the underdeveloped areas as compared to their male counterparts, increasing the number of male physicians entering residency programs, particularly within certain specialties that are more in demand in the underdeveloped areas, could alleviate the problem of uneven distribution of physicians in such areas. To increase the number of female physicians in rural and remote areas, programs that support raising the admissions of female students with a rural background into local medical universities along with providing incentives to encourage them to live and work in rural areas should be put on the policy agenda.
References
1. Gwatkin DR, Bhuiya A, Victora CG. Making health systems more equitable. Lancet 2004; 364(9441): 1273-1280.
2. Braveman P. Health disparities and health equity: concepts and measurement. Annual Review of Public Health 2006; 27: 167-194.
3. Braveman P, Gruskin S. Defining equity in health. Journal of Epidemiology and Community Health 2003; 57(4): 254-258.
4. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle-and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8(1): 19.
5. Dussault G, Franceschini MC. Not enough there, too many here: understanding geographical imbalances in the distribution of the health workforce. Human Resources for Health 2006; 4(1): 12.
6. Tanihara S, Kobayashi Y, Une H, Kawachi I. Urbanization and physician maldistribution: a longitudinal study in Japan. BMC Health Services Research 2011; 11(1): 260.
7. Wilson N, Couper I, De Vries E, Reid S, Fish T, Marais B. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9(2): 1060. Available: www.rrh.org.au (Accessed 5 June 2014).
8. Matsumoto M, Inoue K, Bowman R, Noguchi S, Toyokawa S, Kajii E. Geographical distributions of physicians in Japan and US: impact of healthcare system on physician dispersal pattern. Health Policy 2010; 96(3): 255-261.
9. Pitblado JR, Pong RW. Geographic distribution of physicians in Canada. Sudbury, ON: Centre for Rural and Northern Health Research, Laurentian University, 1999.
10. Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra: Commonwealth of Australia, 2008.
11. Mobaraki H, Hassani A, Kashkalani T, Khalilnejad R, Chimeh EE. Equality in distribution of human resources: the case of Iran's Ministry of Health and Medical Education. Iranian Journal of Public Health 2013; 42(Suppl1): 161.
12. Amini N, Yadollahi H, Inanlo S. Health ranking in Iran's provinces. Social Welfare Quarterly 2007; 5(20): 40-48.
13. Ballance D, Kornegay D, Evans P. Factors that influence physicians to practice in rural locations: a review and commentary. Journal of Rural Health 2009; 25(3): 276-281.
14. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. JAMA 2001; 286(9): 1041-1048.
15. Ricketts TC. Workforce issues in rural areas: a focus on policy equity. American Journal of Public Health 2005; 95(1): 42.
16. Doescher MP, Ellsbury KE, Hart LG. The distribution of rural female generalist physicians in the United States. Journal of Rural Health 2000; 16(2): 111-118.
17. Mollahaliloglu S, Aydogan Ü, Kosdak M, Öncül H, Dilmen U, Kosdak SMÜAM, et al. Physician scarcity in underdeveloped areas of Turkey: what do new graduate physicians think? Rural and Remote Health (Internet) 2012; 12: 2067. Available: www.rrh.org.au (Accessed 5 June 2014).
18. McGrail MR, Humphreys JS, Joyce CM. Nature of association between rural background and practice location: a comparison of general practitioners and specialists. BMC Health Services Research 2011; 11(1): 63.
19. Laven GA, Beilby JJ, Wilkinson D, Mc Elroy HJ. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179(2): 75-79.
20. Matsumoto M, Inoue K, Kajii E, Takeuchi K, Inoue MMK. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 2010; 10(2): 1432.
21. Kirby BA. The rural rotation in a medical technology program: a ten-year retrospective study. Clinical Laboratory Science 2006; 20(4): 202-209.
22. Wibulpolprasert S, Pengpaibon P. Integrated strategies to tackle the inequitable distribution of doctors in Thailand: four decades of experience. Human Resources for Health 2003; 1(1): 12.
23. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36(3): 241-247.
24. Jones AR, Oster RA, Pederson LI, Davis MK, Blumenthal DS. Influence of a rural primary care clerkship on medical students' intentions to practice in a rural community. Journal of Rural Health 2000; 16(2): 155-161.
25. Mehrdad R. Health system in Iran. Japan Medical Association Journal 2009; 52(1): 69-73.
26. Ravaghi H, Taati E, Abdi Z, Meshkini A, Sarvarizadeh S. Factors influencing the geographic distribution of specialist physicians in Iran: a qualitative study. Rural and Remote Health 2015; 15: 2967. Available: www.rrh.org.au (Accessed 10 March 2016).
27. Inoue K, Matsumoto M, Toyokawa S, Kobayashi Y. Transition of physician distribution (1980-2002) in Japan and factors predicting future rural practice. Rural and Remote Health (Internet) 2009; 9(2): 1070. Available: www.rrh.org.au (Accessed 20 June 2014).
28. Alla-Eddini F, Fatemi R, Ranjbaran Jahromi H, Asghari E, Eskandari S, Ardalan A, et al. Iranian physicians' willingness to work in underserved areas and related factors in 2001. Razi Journal of Medical Sciences 2004; 11(40): 247-255.
29. Rabinowitz HK, Diamond JJ, Markham FW, Santana AJ. Increasing the supply of women physicians in rural areas: outcomes of a medical school rural program. Journal of the American Board of Family Medicine 2011; 24(6): 740-744.
30. Tate RB, Aoki FY. Rural practice and the personal and educational characteristics of medical students. Survey of 1269 graduates of the University of Manitoba. Canadian Family Physician 2012; 58(11): e641-e648.
31. Mathews M, Seguin M, Chowdhury N, Card R, Chowdhury MMMSN, Card R. Generational differences in factors influencing physicians to choose a work location. Rural and Remote Health (Internet) 2012; 12: 1864. Available: www.rrh.org.au (Accessed 10 July 2014).
