A study on vision impairment in the Pacific region1 concluded that there is no single model of blindness prevention for all due to huge regional differences. Differences also exist within countries, where rural areas may be at a lower stage of development than urban areas1-3. The Campaign to Eliminate Avoidable Blindness4 outlined that disease control, human resource development, strengthening infrastructure and appropriate technological developments for eyecare delivery are the main actions needed to achieve its goal. In the Western Pacific areas, targeted diseases vary from country to country, with cataracts still a major cause of blindness in some nations and diabetic retinopathy, glaucoma and refractive errors of major importance in others5.
Taiwan is located between Japan and the Philippines, off the south-east coast of China. The eastern shoreline is relatively steep with the East Coast Mountain Range extending down the east coast of the island and the narrow Huatung Valley separating it from the high Central Mountain Range. Therefore, the terrain of eastern Taiwan is long, narrow and mountainous. This geographic characteristic means that indigenous tribes and rural villages are scattered throughout the area.
With the implementation of National Health Insurance since 1995, most inhabitants of Taiwan are entitled to comprehensive medical care (such as disease prevention, outpatient clinic, hospitalisation and prescription medication). Nevertheless, the availability of subspecialty care differs widely between rural and urban areas.
There are many more optometry and ophthalmology services in urban areas than in remote regions. Turner et al2 reported that the prevalence of poor vision is lower with the increasing availability of optometry services. Staffing limitations and poor accessibility to primary eyecare facilities are therefore the priority issues that need to be addressed when developing eyecare programs in geographically isolated regions1,2,6. To implement a comprehensive eyecare service for remote regions6-9, a Mobile Vision Van Unit (MVVU) equipped with ophthalmic instruments was established. This MVVU was operated in cooperation with public health nurses and the district infirmary to establish an effective referral system. The referral from a primary to a secondary and thereafter to a tertiary level is important to overcome the barrier of accessibility to advanced eye care1,10. This study presents the MVVU model for vision screening, primary eye care and community outreach services in remote and indigenous areas, as well as the educational and training programs that were conducted.
This study is a population-based public health project based on the experience and data obtained during operation of an MVVU.
Mobile Vision Van Unit
The MVVU was a modified 4.7 metre 2400 cc Mitsubishi Space Gear equipped with ophthalmic instruments (Fig1), including an autorefractometer, a non-contact tonometer, a slit-lamp biomicroscope, a retinoscope, a direct ophthalmoscope, and a mini optician workshop. The MVVU team members included one senior ophthalmologist, one driver, two well-trained technicians and/or opticians.

Figure 1: The Mobile Vision Van and the instruments the van carried.
Setting and participants
The MVVU was driven to the local infirmary or the community centre of a village. Immediately upon arrival, an ophthalmic screening workstation was set up. The instruments were unpacked and reassembled carefully on site. To facilitate the operation of the MVVU, ample spaces for data collection and preliminary examinations, spacious waiting areas for patients, a semi-dark room for retinoscopy and fundoscopy and a standardised screening procedures were set up (Fig2).
The team members cooperated extensively with the administrative institutes, Public Health Bureau of Hualien and Taitung Counties, and local infirmaries. The public health nurses of the local infirmary, volunteers from the community or non-governmental organisation (NGO), and translators who spoke the local dialects were all essential for the ophthalmic care project.

Figure 2: Flowchart and photographs showing the screening and examination process.
Ophthalmic examinations
A standardised chart was used to collect data on demographics (gender, age, ethnicity), general health (body weight, blood pressure, underlying disease such as diabetes, hypertension, dyslipidemia, and the disease duration) and eye condition. A standardised ophthalmic examination was conducted, including presenting visual acuity or uncorrected visual acuity (UCVA), best-corrected visual acuity (BCVA), automatic refractometry, non-contact tonometry, slit-lamp biomicroscopy, retinoscopy and fundus examinations. The ocular examination findings were recorded on the standardised chart with easily checked and marked categories. A project assistant later entered the data into a spreadsheet according to the data categories presented on the standardized sheet.
Visual acuity was measured using the WHO 'tumbling E' test chart at a distance of 6 metres. UCVA or visual acuity for each eye with the current distance spectacles was measured initially. Further subjective refraction with full refractive error correction was measured if the UCVA was less than 20/60. If appropriate refractive errors could not be obtained, visual acuity with pinhole correction was recorded. On-site dispensing of low-cost spectacles and the rapid delivery of more complex prescriptions were provided for those with a BCVA better than the presenting visual acuity. Dilatation of pupils was performed when the BCVA was less than 20/60 or the lens opacity interfered with the retinal examination. The definition of ocular diseases and the details of ocular examinations have been described in a previous study11,12.
Referral and case management
When a referral was indicated, the public nurses or the coordinators of the infirmary provided a referral sheet, set up the appointment at the secondary or tertiary hospital, reassured the patient about the referral procedure, and contacted the family of elderly patients regarding the scheduled referral. The referred patients, with the referral sheets upon visiting, were entitled to deduction of their co-payment, and the government provided subsidies for transportation costs for those living in remote areas.
Whenever glaucoma was either suspected or diagnosed, and optic neuropathy or disproportional decrease in visual acuity, the patients were referred to the medical centre for further examinations, including visual field test, optical coherence tomography, and further brain imaging whenever brain lesions were suspected. Patients with retinal diseases were also referred for further ophthalmic investigations including fluorescein angiogram, optical coherence tomography, and electroretinography.
Statistical analysis
Data were input into an electronic database and statistical analysis was performed using Excel (Office 2011, Microsoft Corp., Redmond, WA, USA). Data were checked for missing values, and where possible missing data were followed up.
As set out by WHO13, moderate and severe vision impairment were defined as visual acuity with best possible correction (VABC) worse than 6/18 but better than 6/60 in the better-seeing eye and VABC worse than 6/60 but better than 20/400 in the better-seeing eye. Blindness is therefore defined as VABC worse than 20/400.
Ethics approval
Ethical approval was obtained from the Institutional Review Board of Tzu-Chi General Hospital (No. IRB 100-86).
Eyecare services conducted using the Mobile Vision Van Unit model
Between 2002 and 2008, 600 primary eyecare services were delivered to 28 indigenous villages and remote townships in eastern Taiwan (Fig3). The MVVU screened a total of 35 275 participants, with ages ranging from preschool children to the elderly. Of these participants, 15 516 children were examined for strabismus and amblyopia, and 12 504 middle-aged and elderly inhabitants were provided with eyecare services. The MVVU also screened for diabetic retinopathy by thoroughly examining and educating 4801 patients with diabetic mellitus. In cooperation with the Tzu Chi International Medical Association (TIMA), the MVVU provided community eyecare services to 4102 patients through volunteer medical services. On-site dispensing of low-cost spectacles and the rapid delivery of more complex prescriptions were provided to 1816 low-income participants without charge. In addition, 118 eyecare educational programs for the public and training courses and workshops for paramedical personnel and volunteers were conducted (Table 1).
Table 1: Number of screened subjects and eyecare services provided using the Mobile Vision Van Unit model
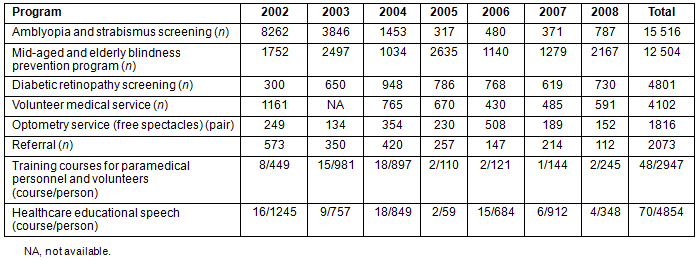
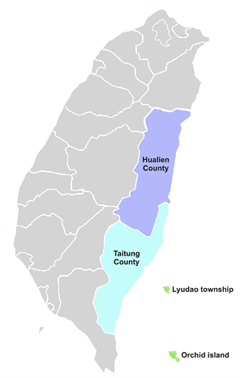
Figure 3: Map of Taiwan; coloured areas show where the Mobile Vision Van Unit served.
Demographic data and major causes of visual impairment in the Middle-aged and Elderly Blindness Prevention Program
Among the tasks that the MVVU fulfilled, the Middle-aged and Elderly Blindness Prevention Program (MEBPP) focused on the major causes of visual impairment in those aged ≥40 years. There were 12 504 participants in the MEBPP, and the ratio of women to men was 5:4 (6953:5551). The mean age of the participants was 67.06 years. In the age group of 40-64, there were more women participants (64.91%) than men. Numbers of women and men participants were more equal in the age group above 65 (Table 2).
A total of 113 blind participants were identified and 489 with moderate or severe vision impairment; overall, 602 (4.80%) subjects were visually impaired. A referral platform coordinated by the local infirmary and case manager was used to refer 2073 patients in MEBPP to secondary or tertiary centres for further management. The actual referral rate from the MEBPP was 16.58% (2073/12 504). Analysis of the causes of vision impairment showed that cataracts (29.40%) were the leading cause, followed by age-related macular disease (21.10 %), optic neuropathy (10.63%), diabetic retinopathy (9.30%), corneal opacity (7.14%), myopic degeneration (4.98%) and glaucoma (4.98%) (Fig4).
Table 2: Gender and age distribution in the Middle-aged and Elderly Blindness Prevention Program (≥40 years)
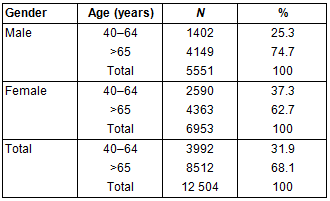
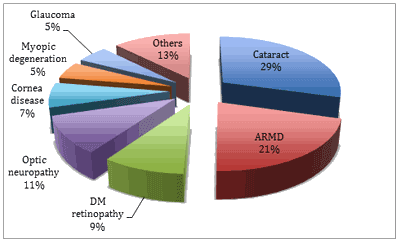
Figure 4: Causes of visual impairment (best-corrected visual acuitydle <20/60) in the Middle-aged and Elderly Blindness Prevention Program (≥40 years).
Budget for the Mobile Vision Van Unit
The MVVU project was carried out in districts across 300 km of eastern Taiwan. With the integration with the local infirmary and tertiary hospital, the cost of the MVVU operation was around US$20,000 per year. Therefore, the cost for screening each participant over the seven years was merely US$4.09, which is very cost-effective (US$20,621Ž7/35 275=US$4.09).
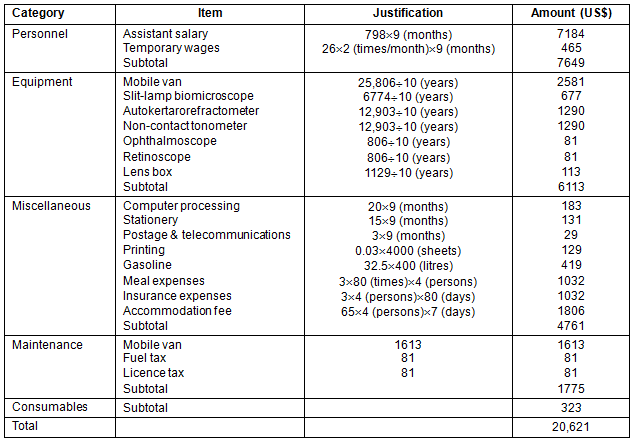
The budget for the MVVU included the initial set-up cost for the Mobile Vision Van (the vehicle, ophthalmic instruments and office equipment, which were separated into 10 year annual depreciation of assets), the salary and insurance of the full-time and part-time medical and administrative assistants, consumable supplies (battery, alcohol wipes, cotton swabs, eye drops and office supplies), operating costs (electronics, postage, phone service, office supplies, printing, gasoline, accommodation and meal expenses) and maintenance (equipment repair and replacement, insurance and maintenance of the vehicle) (Table 3). The personnel expenses included the employment of one administrative assistant (full time), one medical technician (full time) and one optician (temporary, paid hourly). The physician fee was paid by the hospital and the local infirmary paid the public nurses' salary. Volunteers also helped.
Table 3: Annual budget of the Mobile Vision Van Unit
Discussion
Despite decades of effort, the inverse care law3,14, which describes the imbalance of medical care and needs, still exists worldwide15,16. This is also true in the scope of different socio-professional categories within any individual country3. The MVVU model, in cooperation with the local infirmary, is a highly facile and efficient screening and referral framework to overcome obstacles while operating in remote districts. The MVVU was able to approach most, if not all, of the remote areas in eastern Taiwan not only to provide primary eyecare services, but also to bridge the gap between community-based eyecare services and the more advanced management in a hospital2,10.
Previous studies of outreach services8, mobile health vehicles7,9, and telemedicine17 have shown they enable sexual equality8 and accessibility7,9 to medical care. However, eyecare services are very different from services provided by other general health practitioners for disease screening. In internal medicine-oriented health vehicle screening services, health condition parameters such as blood pressure, glucose level and other biochemistry data can be obtained efficiently by paramedical personnel. However, in a MVVU, an ophthalmologist and an optometrist must be included to perform ocular examinations to make the correct diagnosis. For example, a presenting visual acuity of 20/60 may be due to refractive errors, which can be immediately corrected by spectacles, whereas a 20/20 vision or an intraocular pressure under 21 mmHg does not exclude the possibility of normal tension glaucoma. Therefore, a multidisciplinary team with ophthalmologists and optometrists is essential for thorough examinations and timely explanations and communication. During this seven-year MVVU project, it was found that the major causes of visual impairment were similar to the main ocular diseases in South Asia and the western Pacific area1,5, although the manpower and infrastructure issues5 were different. Besides the high prevalence of cataracts, the frequency rates of age-related macular disease and optic neuropathy in the visually impaired middle-aged and elderly population in the current study were comparable to those in other industrialised countries. The prevalence of corneal diseases was relatively high in the current study, and monocular blindness in the middle-aged was mainly caused by trauma (unpublished data). Therefore, with regards to eyecare staging1, these remote and indigenous districts were categorised as stage I to II, meaning that primary eye care was insufficient. In addition, secondary and tertiary services (stage III) were lacking and there were only a few programs regarding disease control and health promotion for eye care at the beginning of the project.
The MVVU dramatically improved eyecare practice in the rural districts, and the patients received timely advanced management via a well-established referral system. The MVVU also provided training courses and educational programs to the local paramedics and population, thereby aiding in the goal of preventing disease and promoting health. For example, the prevalence of diabetic retinopathy was high initially, but the rate reduced after the initiation of the project (unpublished data).
In our MVVU, many patients with an UCVA less than 20/60 were able to gain useful vision with spectacles. Refractive errors were estimated to account for 25% of the cases with an UCVA less than 20/60 (unpublished data). Optician stores were commonly unavailable within 100 km of the villages, and therefore an optometry service is an essential component of the MVVU2,18.
There are many indigenous peoples in eastern Taiwan, including the Amis, Atayal, Bunun, Kavalan, Paiwan, Puyuma, Tao and Truku tribes. Language barriers, especially when communicating with the elderly, can result in insufficient understanding of disease and unnecessary fear. This subsequently causes difficulties in referral. The regional eye health coordinator, who came from the same ethnic culture and spoke the local dialect, optimised the efficient access to eye care2.
The public health nurses and paramedics from the infirmary and teachers from kindergartens and elementary schools were trained through the MVVU workshops, and they were subsequently able to perform examinations accurately to assist the ophthalmologist. The prevalence of amblyopia in another article19 by the corresponding author of the current study was 2.20%. The causes of amblyopia were strabismus 2.6%, refractive errors 62.6%, anisometropia 24.3% and organic 10.4%. Most of these were correctable and were corrected when found early in the childhood. Certified school nurses did the first-line vision screening for the preschool and elementary students, and teachers also had adequate surveillance for ocular problems in class.
The prevention of avoidable blindness requires long-term provision to take effect1. The budget for such programs allocated by the government is usually limited, temporary and irregular, and therefore the operating expense of an MVVU project is frequently unsustainable. Furthermore, the support of the village chief, funding from an NGO (such as the Tzu Chi Foundation and Mennonite Foundation), and the policy of the administrative bureau are important supporting factors for operating an MVVU. The continued support of NGOs in funding and manpower, increased efforts in cataract surgery referral, and the inclusion of a low-vision aid professional as an eyecare team member are crucial for the success of an MVVU project.
An MVVU model with a multidisciplinary team of ophthalmologists, optometrists, public health nurses and technicians is highly facile and efficient in helping to prevent avoidable blindness in remote areas and in those with insufficient medical resources. The most valuable aspect of this MVVU model is to bring the screening tools to the community. That conquered the obstacles of transportation for the inhabitants.
Educational activities of disease prevention in the remote and indigenous district could not draw much attention, therefore had little effect, mostly due to the barrier of different local dialects of various ethnic groups in the region.
The communication with and mutual understanding of the village chiefs and the public health nurses played an enormous part in achieving screening success. Case-management was another key factor in blindness prevention. The visually impaired inhabitants, after referral, had to be followed up appropriately. Public health nurses in the infirmaries who were familiar with the inhabitants were one of the most important personnel on the task.
Health promotion lectures did not gain much popularity among the inhabitants; on the other hand, workshops for teachers and school nurses were very successful. Certified school nurses did the first-line vision screening for the preschool and elementary students, and teachers also had adequate surveillance for ocular problems in class. Therefore, in the consecutive years of the project, ophthalmologists merely had to see the students who were picked out by the preliminary screenings.
The annual budget to run the MVVU project was estimated at US$20,621 per year. The outreach project screened 35 275 participants in the seven-year period, at an average cost of US$4.09 per person, which is very cost-effective.
References
1. Keeffe JE, Konyama K, Taylor HR. Vision impairment in the Pacific region. British Journal of Ophthalmology 2002; 86(6): 605-610.
2. Turner AW, Xie J, Arnold AL, Dunn RA, Taylor HR. Eye health service access and utilization in the National Indigenous Eye Health Survey. Clinical and Experimental Ophthalmology 2011; 39(7): 598-603.
3. Bastawrous A, Hennig BD. The global inverse care law: a distorted map of blindness. British Journal of Ophthalmology 2012; 96(10): 1357-1358.
4. Pararajasegaram R. The Global Initiative for the Elimination of Avoidable Blindness. Community Eye Health Journal 1998; 11(26): 29.
5. Pizzarello L, Abiose A, Ffytche T, Duerksen R, Thulasiraj R, Taylor H, et al. VISION 2020: The Right to Sight: a global initiative to eliminate avoidable blindness. Archives of Ophthalmology 2004; 122(4): 615-620.
6. Khan MD. The Duke Elder Lecture: the challenge of equitable eye care in Pakistan. Eye (London) 2011; 25(4): 415-424.
7. Gardner T, Gavaza P, Meade P, Adkins DM. Delivering free healthcare to rural Central Appalachia population: the case of the Health Wagon. Rural and Remote Health 12: 2035. (Online) 2012. Available: www.rrh.org.au (Accessed 4 April 2013).
8. Pereira SM, Blignault I, du Toit R, Ramke J. Improving access to eye health services in rural Timor-Leste. Rural and Remote Health 12(3): 2095. (Online) 2012. Available: www.rrh.org.au (Accessed 4 April 2013).
9. Murthy KR, Murthy PR, Rao S, Murthy GJ, Kapur A, Lefebvre P. A novel model to deliver advanced eye care for people with diabetes living in resource-poor settings: results of care provided to date. Diabetes Care 2012; 35(4): e31.
10. Boudville AI, Anjou MD, Taylor HR. Indigenous access to cataract surgery: an assessment of the barriers and solutions within the Australian health system. Clinical and Experimental Ophthalmology 2013; 41(2): 148-154.
11. Huang TL, Hsu SY, Tsai RK, Sheu MM. Etiology of ocular diseases in elderly Amis aborigines in Eastern Taiwan (the Amis Eye Study). Japanese Journal of Ophthalmology 2010; 54(4): 266-271.
12. Chen N, Huang TL, Tsai RK, Sheu MM. Prevalence and causes of visual impairment in elderly Amis aborigines in Eastern Taiwan (the Amis Eye Study). Japanese Journal of Ophthalmology 2012; 56(6): 624-630.
13. WHO. International statistical classification of dieseases and related health problems (10th revision). (Online) 2006. Available: apps.who.int/classifications/apps/icd/icd10online2006 (Accessed 17 April 2015).
14. Hart JT. The inverse care law. Lancet 1971; 1(7696): 405-412.
15. Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. British Journal of Ophthalmology 2012; 96(5): 614-618.
16. Resnikoff S, Felch W, Gauthier TM, Spivey B. The number of ophthalmologists in practice and training worldwide: a growing gap despite more than 200,000 practitioners. British Journal of Ophthalmology 2012; 96(6): 783-787.
17. Xu L, Jonas JB, Cui TT, You QS, Wang YX, Yang H, et al. Beijing Eye Public Health Care Project. Ophthalmology 2012; 119(6): 1167-1174.
18. Anjou MD, Boudville AI, Taylor HR. Correcting Indigenous Australians' refractive error and presbyopia. Clinical and Experimental Ophthalmology 2013; 41(4): 320-328.
19. Chang CH, Tsai RK, Sheu MM. Screening amblyopia of preschool children with uncorrected vision and stereopsis tests in Eastern Taiwan. Eye (London) 2007; 21(12): 1482-1488.
