Introduction
Despite issues brought to attention over the last couple of decades1-3, early postgraduate, or junior doctors, are still required to practise in rural and remote communities, and continue to face numerous issues and difficulties. Posts in Queensland, Australia, where junior doctors have been required to practice include numerous small towns and remote communities. The time spent in these locations can vary from a couple of days undertaking country relieving duties, to rural terms up to ten weeks, or extended placements, which may be a year or longer. The nature of practice may be a solo doctor practice (relieving is based at the hospital or where the doctor is the acting medical superintendent at the hospital and also required to undertake private general practice within the community), or within a multi-doctor practice (which provides public and/or private services). Practice in rural and remote communities is different from that in urban areas due to isolation and independence, limited staff and resources available, remoteness from specialists and speciality facilities, differences in patterns of health in rural communities and the unique socio-cultural environment of rural communities4.
Medical schools have undertaken the challenge of providing more rural exposure throughout the undergraduate years5 and the establishment of the Australian College of Rural and Remote Medicine (ACRRM) has facilitated the development of a vocational training pathway and ongoing professional development for rural practitioners6. A rural training program established in South Australia in 1997 provided interns with a well-supervised rural rotation. Through this program numerous benefits were identified and positive experiences were reported by those involved, including the early postgraduate doctors7.
The introduction of the Rural and Remote Area Placement Program (RRAPP) in 2002, administered through ACRRM, has made significant progress toward providing opportunities for early postgraduate doctors to experience rural general practice in a supportive environment8. The program, which provides up to 70 places nationally, has contributed to filling the rural training gap, expanded knowledge about rural community practice, and assisted junior doctors in their decision-making about future training and careers8.
Although initiatives have been introduced at the undergraduate and vocational levels, during the early postgraduate years spent primarily within the hospital setting, exposure to rural practice appears to be very limited. This is a major issue, particularly for Queensland Health Rural Scholarship Holders who are bonded to rural and remote practice for several years after internship9. With limited RRAPP positions available in Queensland, there is a need for hospitals where junior doctors are based to be contributing to their preparation for rural practice. This research investigated the current issues and difficulties faced by junior doctors required to undertake rural and remote practice in Queensland.
Methods
An exploratory study was undertaken. Primary data were collected through semi-structured interviews held with key stakeholders. A series of open-ended questions were asked, however prompts were used to investigate some specific issues. Purposive sampling methods were used to identify stakeholders or potential interviewees. The potential participants were selected according to the positions they held and/or the location of their employment. Stakeholders included: Directors of Clinical Training (DCTs); Medical Educators (MEs); Junior Doctors (JDs); Rural Practitioners (RPs); Academic Rural Practitioners (ARPs); and Medical Administrators (MAs). A variety of perspectives strengthened the quality of data. Of the 23 people approached, a total of 19 agreed to be interviewed. Of those who did not participate, one was not contactable, one had resigned, one was too busy and one was new to the position and did not feel a valuable contribution could be made to the project. The response rate was 82.6%. Interviews were conducted either in person or via telephone. With the respondents consent, the interviews were tape-recorded. Data were transcribed and analysed using Nvivo software (QSR International; Durham, UK). A systematic coding process facilitated the identification of core themes emerging from the data. Respondents were provided with a draft report and given the opportunity to validate results and provide feedback.
Results
The broad range of perspectives collected in the interviews included those of JDs who were being sent out into rural practice, practitioners being relieved (RPs), staff supporting junior doctors within the hospital setting on the ground level (DCTs and MEs), administrators overseeing programs for junior doctors (MAs) and recognised experts in the field (ARPs). The positions held by respondents are outlined (Table 1).
Table 1: Positions held by respondents
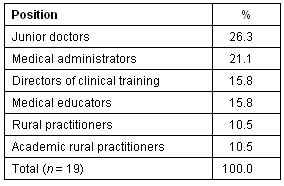
Of the 19 respondents, over half were male (63.2%, n = 12) and nearly three-quarters were medically trained (73.6%, n = 14). The remaining respondents held positions as educators or administrators. Over half of the medically trained respondents had practised in a rural or remote community. These respondents reported having both positive and negative experiences. Overall the more experienced medical practitioners were positive about the time they had spent in the outback. These practitioners expressed the value of taking extra responsibility in smaller hospitals which had forced them to become resourceful, learn more and be involved in many more cases than they would have in a larger hospital. Positive comments from respondents included:
...you can learn a lot from the country, you have that extra step where you take responsibility and you do things and you sort of become a real doctor [DCT04].
I think the diversity of the role and that lots of interesting, exciting urgent things happened. I think quite enjoyed being responsible for more than what's possible in a bigger town and I enjoyed the team work and the people working together and making health work [ARP16].
There were fewer negative experiences and most comments were made by the less experienced medical officers. The new doctors were still making the transition into being independent practitioners and had not yet come to terms with the independence and expectations that were required in rural and remote practice. Comments included:
Well certainly it was very frightening especially before I got there for the first time [JD05].
I've had to deal with all sorts of horrendous situations... I'm glad I've done it in a way but I think it would have been nice to have got that experience without being sent to the middle of nowhere by myself [JD10].
Environment of rural and remote practice
A few respondents were critical of the fact that junior doctors were sent out into rural and remote practice in their second postgraduate year, particularly to solo doctor towns. It was recognised that this is not ideal because junior doctors have limited knowledge, skills and experience, and in going to these places, little or no on-site supervision and support. Comments from respondents included:
I think, my initial answer is that junior doctors shouldn't go without support full stop... You should not send a junior doctor by themselves to [Remote Aboriginal Community 1, Remote Aboriginal Community 2 or Remote Centre 1]. That is insane and does a lot more harm than anything else [RP18].
I don't think that anybody should be going to a remote or rural area, relieving or as a scholarship holder, if they haven't done 2 years... I still deplore the idea that scholarship holders should have to go out to [Remote Centre 2] and they should certainly not be going into solo unsupervised places [DCT09].
I don't think we should be sending people to rural hospitals until they've done two years, in a hospital, which gives them time indeed to do most of those things [ARP16].
Issues and difficulties
How well a medical officer copes in rural and remote practice may depend on the amount of experience they have had in the field and how comfortable they feel with independence and responsibility. Respondents identified a range of issues or difficulties that were faced by junior doctors who undertake rural practice. These were grouped into six themes.
Preparedness: Respondents made several comments relating to the lack of preparation that junior doctors receive for rural practice and this was a general umbrella for the other issues raised. This involved not knowing what to expect in clinical practice, the degree of responsibility that they have in practice and managing staff, greater workloads including the requirement to undertake private general practice, living in small town and Indigenous communities, and just not knowing in what sort of situations they might find themselves. One respondent reported:
Junior doctors without a doubt feel an overwhelming sense of awe and fear... it tends to be a fearful experience and they wonder about their preparation and competence to handle what's going to present to them [MA03].
Clinical issues: Limited clinical experience was identified by a few respondents as causing difficulties for junior doctors. It was reported that often they do not possess an appropriate level of emergency and procedural skills. It was also identified that having to deal with major trauma and obstetrics were issues. Advice and input by more senior medical staff was still sought regularly. One rural practitioner reported:
They're not really ready to go in the first place, with their level of knowledge and experience [RP18].
Inadequate support and supervision: Lack of support and supervision was raised by every respondent. When junior doctors were sent to relieve doctors in rural towns there were generally few, or sometime no other, medical officers based in the same town. Isolation from consultants and experienced senior medical officers required junior doctors to take on much more responsibility and decision-making than they were usually comfortable with. No on-site supervision made junior doctors become more reliant on telephone support. Support was accessed from two main sources, primarily from consultants at the junior doctor's 'home' hospital or from the Royal Flying Doctors Service. Several respondents identified that they had used the telephone to access clinical support; however, it was suggested that this does not assist them adequately. One respondent commented:
All the telemedicine and audio-medicine and what have you in the world doesn't make up for having somebody else on the ground who can put their hands on the patient [DCT06].
Another issue raised was confusion as to whom the junior doctor should call for advice, particularly after hours. There was a reported feeling of anxiety in anticipating whether the person called would be responsive. A comment was made that frequently senior staff were overworked and not able to provide support and put in as much effort as was required by junior staff.
It was identified that sometimes support was available from other doctors in the town. However a confounding issue emerged, where one respondent reported that a significant proportion of the rural and remote workforce were overseas trained doctors, some of whom were inadequately trained and were positioned as the direct supervisor of relieving junior doctors. It was noted that rural hospitals had constant troubles recruiting, including for senior staff positions. Some respondents mentioned that other clinical staff including nurses were supportive. However this was confounded by reports that, again, there were difficulties in recruiting, and junior doctors did not necessarily have the full complement of staff for back-up.
Other professional issues: A range of other professional issues were identified by respondents. The most common issues were workload and numbers of doctors, and the requirement for junior doctors to undertake private general practice and provide on-call services without relief. Other difficulties included access to reliable communication in the bush, lack of pathology and radiology services, limited access to clinical information (books, journals and online resources), and not understanding referral and evacuation processes.
Education and training: A third of the respondents, representing all stakeholder groups, identified issues relating to education and training. These could be divided into two levels. The first related to preparation and support for rural practice. It was identified that currently there was limited education and training provided to prepare for and support junior doctors in rural practice. The second pertained to the pursuit of vocational training and specialist pathways. There were reported difficulties in accessing accredited positions for vocational training in rural areas. Comments included:
They have no planned ongoing educational development programmes for second year's that I have seen [ARP01].
At the moment we're seeing a bigger issue regarding their achievement of postgraduate qualifications or college qualifications. So they have difficulty sometimes in being able to be in accredited positions for vocational training [MA17].
Personal and other issues: The majority of respondents highlighted personal issues that were faced by junior doctors undertaking rural and remote practice. The most predominant issue raised was isolation and distance from partners, family and friends. The lack of social support while relieving was a problem. Factors that contributed to this problem included partners following their own careers and the perceived quality of schooling available in remote towns for children. Some respondents identified that for those on longer placements whose family accompanied them, difficulties were experienced in keeping the family happy.
Adjusting to living in small communities was another common issue. Those accustomed to living in big cities found it quite peculiar in towns where everybody knew everybody, and everyone knew everyone else's business. It was reported to be quite confronting socially. A few respondents identified personal safety and loneliness as being a concern, particularly for females. This was an issue generally in the smaller, more remote communities. For example, some respondents reported that it was not advisable for a single female to go walking around the streets on her own. Another comment was:
... in [Remote Aboriginal Community 1 and Remote Aboriginal Community 2] the violence and attitudes of the community are very, very draining indeed [JD10].
A number of other issues were highlighted by some respondents. These included coping with reality shock. There was a lack of awareness regarding transport and accommodation, safe driving on country roads and community issues. Other issues were recruitment and retention problems and objection to allocated or relieving terms.
Current programs
With the focus on addressing rural issues at an undergraduate level, including through integrated curricula and placements10it was explored as to whether current hospital-based programs for junior doctors had followed this trend. Of those interviewed, just over half were directly involved in coordinating or participating in education and training programs for junior doctors. Generally, formal education activities were scheduled for one to two hours per week and held around lunchtime. Attendance rates were variable. Generally, a specific curricula had not been developed. Only a couple of respondents reported having undertaken a 'needs assessment' involving junior doctors on their return from rural practice, local consultants and their education committee. However, some topics were based only on the interests of the particular consultant presenting the session. It was reported that the sessions were usually didactic and focussed on knowledge.
Representatives from one of the five hospitals involved in the study reported providing regular workshops aimed to facilitate junior doctors attaining practical skills, which would assist them in preparation for rural practice. These were held five times per year on a weekend. It was reported that attendance at these was good. However, overall the majority of respondents did not think that the current education programs were adequately preparing junior doctors for rural and remote practice. When asked, the majority of respondents supported the identification of core skills and knowledge, and integration of these and other issues affecting rural practice into hospital-based programs. It was commented that orientation and education, with a rural emphasis, could assist junior doctors in their preparation for country relieving, rural terms and longer placements.
Discussion
Despite the identification of recommendations in previous studies1-3 there still appears to be significant gaps in the preparation and support of junior doctors going into rural and remote practice. Some medical schools are now recruiting rural candidates and decentralising training11. In addition, posts are available for resident medical officers in suburban or provincial hospitals. While the RRAPP has been useful to clarify expectations and assist junior doctors prepare for future rural practice8, the current capacity of the program does not equate with the number of junior doctors in Queensland, who will be required to undertake country relieving or be bonded to rural practice to fulfil scholarship requirements.
In general, there also appears to be little personal development and preparation provided for junior doctors in the hospital setting towards preparation for rural practice. There was no evidence of any hospital-based general practice oriented teaching, which was suggested by Harvey and Linn et al1. There was also no evidence that the prior recommendation of pre-arranged formal supervision had been implemented.
Data collected in this study have confirmed that junior doctors are still being sent to undertake rural relieving in their second postgraduate year. Similar to the issues identified in the literature, there are a number of barriers influencing the ability of junior doctors to practise competently and confidently when working in rural and remote communities. Minimal clinical experience, lack of supervision and on-site support, inadequate orientation and uninformed expectations, limited access to relevant education, and the influence of isolation results in an overall lack of preparation both professionally and personally. Current hospital-based education and training programs were not adequately preparing junior doctors for rural and remote practice.
Limitations
There were limitations in this study. Some biases may have been encountered from only utilising a small sample, which were chosen using purposive sampling methods. Additionally, conducting the study in one particular geographic area may have limited the accuracy of results. With a restricted cohort and geographic boundary, the findings may not be generalisable to a broader audience.
Conclusions
There are a range of issues that still remain for junior doctors when undertaking practice in rural and remote communities. Results from this study suggest that prior recommendations have not been fully implemented. A recommendation from this research is that initiatives at the undergraduate level, including increasing rural exposure and integration of rural context into training, be further developed at the early postgraduate level. Core rural competencies should be identified, and realistic preparation and support strategies put in place in the hospital setting. This will further the effort to prepare junior doctors for rural practice and minimise some of the barriers currently being experienced.
Acknowledgements
The author would like to acknowledge Professor David Prideaux, Professor Paul Worley, Professor Craig Veitch and Associate Professor Dennis Pashen, the supervisors of this project, for their input and guidance.
References
1. Harvey BC, Linn JT, Saville GG. A training programme for rural general practitioners in Australia. Medical Journal of Australia 1980; 2: 597-600.
2. Hickner JM. Training for rural practice in Australia 1990. Medical Journal of Australia 1991; 154: 111-118.
3. Iredell J. Relieving medical officers in Queensland country hospitals. Medical Journal of Australia 1992; 157: 523-527.
4. Australian College of Rural and Remote Medicine. Primary Curriculum. 2nd edn. Brisbane, QLD: Australian College of Rural and Remote Medicine; 2002.
5. Rural Undergraduate Steering Committee. Rural doctors: reforming undergraduate medical education for rural practice: final report of the Rural Undergraduate Steering Committee for the Department of Human Services and Health. Canberra: Commonwealth Department of Human Services & Health, 1994.
6. Australian College of Rural and Remote Medicine. Professional Development Program Handbook 2003. Brisbane, QLD: Australian College of Rural and Remote Medicine, 2002.
7. Mugford B, Worley P, Braund W, Martin A. Rural Intern Training. Rural and Remote Health 1: 86. (Online) 2001. Available: http://rrh.org.au (Accessed 10 October 2005).
8. Nichols A, Worley P, Toms L, Johnston-Smith P. Change of place, change of pace, change of status: rural community training for junior doctors, does it influence choices of training and career?: Rural and Remote Health 4: 259. (Online) 2004. Available: http://rrh.org.au (Accessed 10 October 2005).
9. Queensland Health. Queensland Health Rural Scholarship Scheme Information Kit. Roma, QLD: Queensland Health, 2000.
10. Rural Undergraduate Steering Committee. Rural doctors: Reforming undergraduate medical education for rural practice: Final report of the Rural Undergraduate Steering Committee for the Department of Human Services and Health. Canberra: Commonwealth Department of Human Services & Health; 1994.
11. Hays RB. A new medical school for regional Australia. Medical Journal of Australia 2000; 172: 362-363.
