Diarrhea remains one of the public health problems contributing to high morbidity and mortality among children under 5 years of age in most developing regions of the world1-5. In Sub-Saharan Africa, diarrhea is responsible for 25-75% childhood morbidity and 50% childhood mortality6.
Although death from childhood diarrhea (CDD) has declined significantly due to the improvement of case management, CDD morbidity has declined only slightly in the past three decades4,7. In many Sub-Saharan African countries, the incidence of CDD morbidity and mortality remains high8-10. Studies have shown that CDD is associated with sociodemographic, behavioral and environmental factors11-17.
According to the 2004 joint statement of UNICEF and WHO, appropriate healthcare-seeking practices for diarrhea include administering oral rehydration salts (ORSs) to the sick person, utilization of zinc supplements and seeking care at healthcare institutions (HCIs)18. Timely provision of ORS and zinc tablets has proven to be both cost-effective and efficacious as primary interventions for preventing diarrhea mortality19-23. However, many children with diarrhea are not treated appropriately using these interventions due to low utilization of HCIs for CDD24.
Ethiopia has made great progress in improving the accessibility and provision of primary healthcare services through health extension packages since 2003. Despite this fact, in 2011 only 39.7% of children aged less than 5 years with diarrhea received any form of ORS25. ORS utilization has been relatively stable for the past 10 years in the country25,26. Moreover, healthcare utilization of mothers who had children with diarrhea was low in Ethiopia27. There is a paucity of evidence that identifies factors associated with healthcare utilization for CDD. Credible evidence from such studies is important to identify the gaps of interventions to develop evidence-based interventions that help to increase healthcare service utilization. This study aimed to identify factors associated with mothers' healthcare services utilization for CDD treatment at a population level in Ethiopia.
Study design and setting
A secondary data analysis was conducted using data from the Ethiopian Demographic and Health Survey (DHS) of 2011. This survey is carried out at 5-year intervals to provide health and health-related indicators at the national and regional level in Ethiopia. The Ethiopian DHS samples were selected using a stratified, two-stage cluster sampling procedure. Enumeration areas (EAs) were the sampling units for the first stage, and the second-stage strata were urban and rural areas. The sample included 624 EAs (187 in urban areas and 437 in rural areas) that represented all areas of the nation. All households in all cluster EAs were included in the study, a total of 17 817 households. The detailed sample procedure has been presented in the DHS country report (EDHS)25.
Study population
Households that had children aged less than 5 years with diarrhea were extracted from the Ethiopian DHS dataset in 2011. The Ethiopian DHS data also have epidemiological variables such as age, sex, wealth index of parents, place of residence and healthcare service utilization.
Outcome measurement
The outcome variable of this study was healthcare service utilization among mothers who had children aged 5 years or less with CDD. In DHS data collection, mothers were interviewed to report the presence or absence of diarrhea by asking, 'Were any of your children aged five and below passed loose watery stool with or without blood continuously for more than three times in any particular day in the last two weeks?' Mothers were further probed about the type of care that was sought. Healthcare utilization was measured if mothers of a child with diarrhea sought care from a medical center, which included treatment received at any healthcare facility given by public, non-government or private entities. Mothers who did not seek treatment from those medical centers were considered as non-users of healthcare services.
Explanatory variables
Epidemiological variables of children, mothers and parents included age, sex, place of residence, educational status of mother and partner, presence of job for mother, wealth index of parents and health-service-related factors (antenatal care attendance, postnatal checkup and community conversation). The wealth index used in the survey is a measure that has been used in many DHS and other country-level surveys to indicate socioeconomic inequalities and was computed by principal component analysis from household assets (presence of own farmland, own toilet facility, bank account, mobile phone, electricity, roof of a house with corrugated iron sheets, number of cows/oxen, horses/mules/donkeys, goats/sheep and chickens). Once the index was computed, households were categorized into five wealth quintiles (from lowest to highest).
Statistical analysis
Data were analyzed using the Statistical Package for the Social Sciences v21 (SPSS; http://www.spss.com). Descriptive statistics were used to show the sociodemographic variables, treatment options used by mothers and exposure to mass media. Binary and multivariable logistic regressions were carried out to identify factors associated with healthcare utilization for CDD. Both crude and adjusted odds ratios were calculated with 95% confidence interval (CI). All tests were two-sided, and p<0.05 was considered statistically significant.
Ethics approval
The data were downloaded and used after the purpose of the analysis was communicated and approved by the MEASURE DHS. The original DHS data were collected in confirmation with international and national ethical guidelines. Ethical clearance for the survey was provided by the Ethiopian Public Health Institute (formerly the Ethiopian Health and Nutrition Research Institute Review Board), the National Research Ethics Review Committee at the Ministry of Science and Technology, the Institutional Review Board of ICF International, and the Centers for Disease Control.
A total of 11 654 mothers who had children aged less than 5 years were interviewed in the study. Of those, 1620 mothers had children with diarrhea for the 2 weeks preceding the survey. About 35% (95%CI: 32.7-37.3%) of mothers used HCIs for CDD treatment. Of those mothers who did not use HCIs for CDD treatment (65% (95%CI: 62.7-67.3%), 60.2% did not seek any treatment and nearly 3% sought treatment from pharmacy and drug vendors (Fig1).
Among those who sought healthcare services at HCIs for CDD, 51.9% were male, 78.3% were rural and 24.5% were from the poorest wealth quintile. Most mothers (87.3%) who sought healthcare services for CDD at HCIs had information about ORSs. More than 60% of mothers who sought healthcare services at HCIs for CDD were illiterate (Table 1).
Table 1: Frequency of health facility users for childhood diarrhea across different sociodemographic characteristics in Ethiopia, 2011
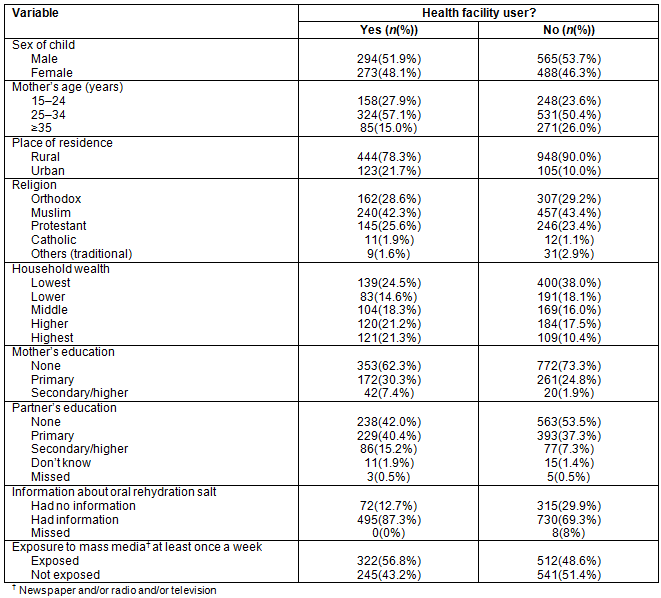
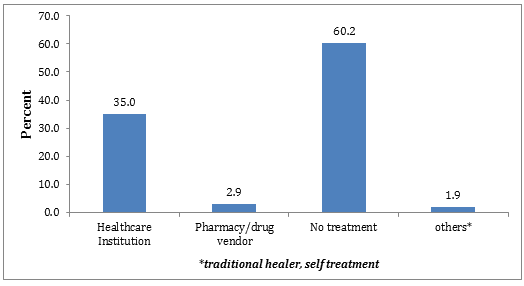
Figure 1: Diarrhea treatment options used by caregivers/mothers with children aged less than 5 years, based on Ethiopian Demographic and Health Survey 2011.
Factors associated with mothers' healthcare service utilization for childhood diarrhea
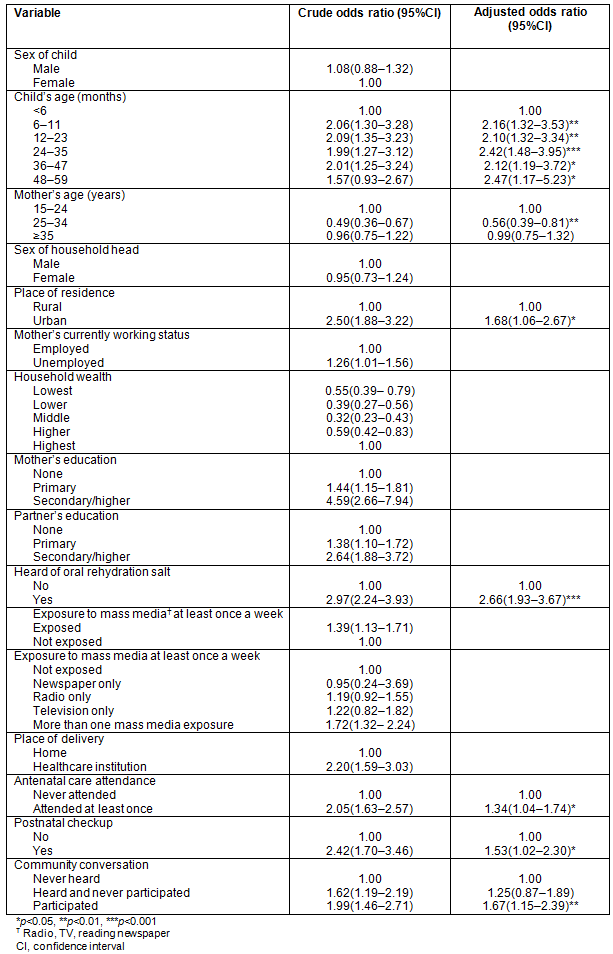
Healthcare utilization of mothers for CDD was associated with age of the child. Those mothers who had children aged 6-11 months were 2.16 times more likely to use HCIs for CDD treatment (adjusted odds ratio (AOR)=2.16, 95%CI: 1.32-3.53) compared to mothers who had children aged less than 6 months. Utilization of healthcare services at HCIs for CDD treatment was also significantly associated with mothers' age. Those mothers aged 25-34 years were 0.44 times less likely to seek healthcare services at HCIs for CDD treatment compared to mothers aged 15-24 years (AOR=0.56, 95%CI: 0.39-0.81). Mothers from urban areas were 1.68 times more likely to use HCIs for CDD treatment compared to mothers from rural areas (AOR=1.68, 95%CI: 1.06-2.67). Those mothers who had information about ORSs were 2.66 times more likely to use HCIs for CDD treatment (AOR=2.66, 95%CI: 1.93-3.67) than those mothers who had no information about ORSs. Mothers who attended antenatal care were 1.34 times more likely to use HCIs for CDD treatment compared to mothers who had never attended (AOR=1.34, 95%CI: 1.04-1.74). Mothers who had postnatal checkups were 1.53 times more likely to use HCIs for CDD treatment compared to mothers who had no postnatal checkups (AOR=1.53, 95%CI: 1.02-2.30). Those mothers who participated in community conversation were 1.67 times more likely to use HCIs for CDD treatment compared to those mothers who had no information about community conversation (AOR=1.67, 95%CI: 1.15-2.39) (Table 2).
Table 2: Logistic regression on factors associated with healthcare service utilization for childhood diarrhea, Ethiopia, 2011
Discussion
According to the recommendation of UNICEF and WHO, appropriate healthcare seeking practices for diarrhea include administering ORSs to the sick person, utilization of zinc supplements and seeking care at a healthcare facility18. Improving the healthcare practices of mothers would therefore play a key role in improving the health status of children. Almost two-third (65% with 95%CI of 62.7-67.3%) of mothers did not use HCIs for CDD treatment in this study.
This finding is comparable to a study finding of UNICEF and WHO conducted in developing countries, which found that nearly 60% of children did not get the recommended treatment28. This is higher than for other studies done in Ethiopia (44%)27, Mozambique (57%)29, rural Niger (30%)30 and rural China (33%)31. However, it is lower than a study done in rural Bangladesh (78%)32. The variation in healthcare-seeking behavior could be due to the sociodemographic variation, cultural differences and difference in access to HCIs between the countries. Qualitative findings have revealed that the use of health services in case of illness is a complex behavior influenced by norms, moral values, beliefs, preferences and socioeconomic potential, as well as the perceived needs of users33,34.
The present study showed that those mothers who had children older than 6 months were more likely to seek healthcare services at HCIs for CDD treatment. This study contradicts some other studies, which showed the younger age of the child was significantly associated with seeking a higher level of care for diarrhea31,35-37. The possible justification why older children get treatment at HCIs for CDD could be due to the high prevalence of CDD after the age of 6 months. Some studies in Ethiopia38-40 found that the prevalence of CDD peaked between 6 and 11 months and declined slightly until 36-47 months due to unhygienic complementary feeding initiation after 6 months and crawling, which exposes children to contaminated objects and materials.
This study found that mothers aged 25-34 years were 44% less likely to use HCIs for CDD treatment as compared to mothers aged 15-24 years. This finding is consistent with a study done in Kenya in which older mothers were less likely to take their child for health care than younger mothers35. The reason could be due to the experience of older mothers in managing this illness compared to younger mothers. The other possible justification might be that those older mothers had more children and lacked time to visit HCIs, which prevented them from seeking appropriate treatment for CDD.
Urban residents were more likely to seek CDD treatment from HCIs compared to their rural counterparts. This could be because urban mothers had more access to information and HCIs and better education than the rural residents. This finding is consistent with a study done in Oromiya region, Ethiopia, which showed that the urban residents had more chances of utilizing HCIs for childhood illness27.
Antenatal care attendance improves utilization of HCIs for CDD. Those mothers who had attended antenatal care at least once were 34% more likely to seek care from HCIs for CDD. The purpose of providing antenatal care at HCIs is to improve maternal health and health of children, informing mothers about the advantages of visiting HCIs for childhood illness. During antenatal care attendance, mothers were also informed about the advantage of postnatal visits.
Having prior information on ORSs was also associated with healthcare utilization for CDD. Those mothers who were informed about ORSs were nearly three times more likely to seek care from a HCI than their counterparts. It is consistent with a study from eastern Ethiopia39. If mothers are aware of the advantage of ORSs, they are more likely aware about diarrhea and use ORSs as an appropriate treatment option for CDD.
Postnatal checkup was also associated with utilization of HCIs for CDD. Mothers who had postnatal checkups were 53% more likely to utilize HCIs for CDD than non-attending counterparts. When mothers visit HCIs for a postnatal checkup, they are informed about common childhood illnesses and the appropriate place to seek care, which helps them to bring their child to a HCI during any illness.
Community conversation is one of the programs implemented in rural communities of Ethiopia to communicate health information on different topics such as antenatal care, diarrhea, pregnancy and nutrition41. In this study, those mothers who participated in the community conversation program were more likely to use HCIs for CDD treatment. The community conversation might help mothers to be aware of the advantages of seeking care at HCIs for CDD treatment. Women who were aware of the community conversation program would have a positive understanding of the benefits of using HCIs.
This study has limitations; it shares the drawbacks of other similar studies conducted using cross-sectional study design. Since this is a secondary data analysis, it missed key variables like perception about diarrhea, knowledge on ORSs and other important key variables. The sample size was large, which is helpful to fit a regression model to identify factors associated with healthcare service utilization and can be considered the strength of the study.
Healthcare services utilization for CDD treatment has been found to be poor in Ethiopia. Urban residency, older age of the child, information about ORSs, community conversation, antenatal care attendance and postnatal check were the identified factors associated with healthcare services utilization for CDD treatment. Special attention should be given to rural mothers and younger children to improve healthcare services utilization for CDD through the existing health system. Promotion of appropriate CDD treatment during antenatal care, postnatal checkup and community conversation are the recommended interventions.
Acknowledgement
The authors are grateful to MEASURE DHS for the data used in this study.
References
1. Walker CF, Perin J, Aryee M, Boschi-Pinto C, Black R. Diarrhea incidence in low- and middle-income countries in 1990 and 2010: a systematic review. BMC Public Health 2012; 12: 220.
2. Boschi-Pinto C, Velebit L, Shibuya K. Estimating child mortality due to diarrhoea in developing countries. Bulletin of the World Health Organization 2008; 86(9): 710-717.
3. Kotloff K, Nataro J, Blackwelder W, Nasrin D, Farag T, Panchalingam S, et al. Burden and aetiology of diarrhoeal disease in infants and young children in developing countries (the Global Enteric Multicenter Study, GEMS): a prospective, case-control study. Lancet 2013; 382(9888): 209-222.
4. Kosek M, Bern C, Guerrant R. The global burden of diarrhoeal disease, as estimated from studies published between 1992 and 2000. Bulletin of the World Health Organization 2003; 81(3): 197-204.
5. Cynthia Boschi-Pinto C, Lanata CF, Mendoza W, Habte D. Diarrheal diseases. In D Jamison, R Feachem, M Makgoba, E Bos, F Baingana, K Hofman, et al. (Eds). Disease and mortality in Sub-Saharan Africa. Washington, DC: World Bank, 2006; ch. 9.
6. Walker CLF, Rudan I, Liu L, Nair H, Theodoratou E, Bhutta ZA, et al. Global burden of childhood pneumonia and diarrhoea. Lancet 2013; 381(9875): 1405-1416.
7. Aggarwal R, Sentz J, Miller M. Role of zinc administration in prevention of childhood diarrhea and respiratory illnesses: a meta-analysis. Pediatrics 2007; 119(6): 1120-1130.
8. Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380(9859): 2095.
9. Forsberg B, Petzold M, Tomson G, Allebeck P. Diarrhoea case management in low- and middle-income countries - an unfinished agenda. Bulletin of the World Health Organization 2007; 85(1): 42-48.
10. Shivoga W, Moturi W. Geophagia as a risk factor for diarrhoea. Journal of Infection in Developing Countries 2009; 3(2): 94-98.
11. Genser B, Strina A, Teles CA, Prado MS, Barreto ML. Risk factors for childhood diarrhea incidence: dynamic analysis of a longitudinal study. Epidemiology 2006; 17(6): 658-667.
12. Vafaee AM, Khabazkhoob M. Case-control study of acute diarrhea in children. Journal of Research in Health Sciences 2008; 8(1): 25-32.
13. Woldemicael G. Diarrhoeal morbidity among young children in Eritrea: environmental and socioeconomic determinants. Journal of Health, Population and Nutrition 2001; 19(2): 83-90.
14. Yassin K. Morbidity and risk factors of diarrheal diseases among under-five children in rural Upper Egypt. Journal of Tropical Pediatrics 2000; 46(5): 282-287.
15. Lamberti L, Walker CF, Noiman A, Victora C, Black R. Breastfeeding and the risk for diarrhea morbidity and mortality. BMC Public Health 2011; 11 (Suppl. 3): S15.
16. Awoke W, Much S. A cross sectional study: latrine coverage and associated factors among rural communities in the District of Bahir Dar Zuria, Ethiopia. BMC Public Health 2013; 13: 99.
17. Prüss-Üstün A. Preventing disease through health environments. Towards an estimate of the environmental burden of disease. Geneva: World Health Organization, 2006.
18. UNICEF/WHO. WHO/UNICEF Joint Statement on Clinical Management of Acute Diarrhoea. Geneva: UNICEF/WHO, 2004.
19. Bhatnagar S, Bahl R, Sharma PK, Kumar GT, Saxena SK, Bhan MK. Zinc with oral rehydration therapy reduces stool output and duration of diarrhea in hospitalized children: a randomized controlled trial. Journal of Pediatric and Gastroenterological Nutrition 2004; 38(1): 34-40.
20. Ali M, Dutta K, Chatterjee R, Ghosh S, Biswas R. Efficacy of oral rehydration therapy in dehydrating diarrhoea of children. Journal of the Indian Medical Association 2003; 101(6): 352-356.
21. Bhatnagar S, Bhandari N, Mouli U, Bhan M. Consensus Statement of IAP National Task Force: status report on management of acute diarrhea. Indian Pediatrics 2004; 41(4): 335-348.
22. Bhandari N, Mazumder S, Taneja S, Dube B, Agarwal R, Mahalanabis D, et al. Effectiveness of zinc supplementation plus oral rehydration salts compared with oral rehydration salts alone as a treatment for acute diarrhea in a primary care setting: a cluster randomized trial. Pediatrics 2008; 121(5): e1279-1285.
23. Gregorio G, Dans L, Cordero C, Panelo C. Zinc supplementation reduced cost and duration of acute diarrhea in children. Journal of Clinical Epidemiology 2007; 60(6): 560-566.
24. Walker CF, Fontaine O, Young MW, Black RE. Zinc and low osmolarity oral rehydration salts for diarrhoea: a renewed call to action. Bulletin of the World Health Organization 2009; 87(10): 780-786.
25. Central Statistical Agency (CSA) of Ethiopia. Demographic and Health Survey 2011. Addis Ababa: CSA and ORC Macro, 2011.
26. Central Statistical Agency (CSA) of Ethiopia. Demographic and Health Survey 2005. Addis Ababa: CSA and ORC Macro, 2005.
27. Assefa T, Belachew T, Tegegn A, Deribew A. Mothers' health care seeking behavior for childhood illnesses in Derra District, Northshoa Zone, Oromia Regional State, Ethiopia. Ethiopian Journal of Health Sciences 2008; 18(3): 87-94.
28. UNICEF/WHO. Diarrhea: why children are still dying and what can be done. (Internet) 2009. Available: http://apps.who.int/iris/bitstream/10665/44174/1/9789241598415_eng.pdf (Accessed 22 October 2013).
29. Nhampossa T, Mandomando I, Acacio S, Nhalungo D, Sacoor C, Nhacolo A, et al. Health care utilization and attitudes survey in cases of moderate-to-severe diarrhea among children ages 0-59 months in the District of Manhica, southern Mozambique. American Journal of Tropical Medicine and Hygiene 2013; 89(1 Suppl): 41-48.
30. Page AL, Hustache S, Luquero FJ, Djibo A, Manzo ML, Grais RF. Health care seeking behavior for diarrhea in children under 5 in rural Niger: results of a cross-sectional survey. BMC Public Health 2011; 11: 389.
31. Gao W, Dang S, Yan H, Wang D. Care-seeking pattern for diarrhea among children under 36 months old in rural western China. PLoS ONE 2012; 7(8): e43103.
32. Das SK, Nasrin D, Ahmed S, Wu Y, Ferdous F, Farzana FD, et al. Health care-seeking behavior for childhood diarrhea in Mirzapur, rural Bangladesh. American Journal of Tropical Medicine and Hygiene 2013; 89(1 Suppl): 62-68.
33. Colvin CJ, Smith HJ, Swartz A, Ahs JW, de Heer J, Opiyo N, et al. Understanding careseeking for child illness in sub-Saharan Africa: a systematic review and conceptual framework based on qualitative research of household recognition and response to child diarrhoea, pneumonia and malaria. Social Science and Medicine (1982) 2013; 86: 66-78.
34. Yalew E. A qualitative study of community perceptions about childhood diarrhea and its management in Assosa District, West Ethiopia. BMC Public Health 2014; 14: 975.
35. Taffa N, Chepngeno G. Determinants of health care seeking for childhood illnesses in Nairobi slums. Tropical Medicine and International Health 2005; 10(3): 240-245.
36. Ndugwa R, Zulu E. Child morbidity and care-seeking in Nairobi slum settlements: the role of environmental and socio-economic factors. Journal of Child Health Care 2008; 12(4): 314.
37. Tee GH, Kaur G, Ramanathan P, Amal NM, Chinna K. Health seeking behavior among Malaysians with acute diarrheal disease. Southeast Asian Journal of Tropical Medicine and Public Health 2011; 42(2): 424-435.
38. Getaneh T, Assefa A, Tadesse Z. Diarrhoea morbidity in an urban area of southwest Ethiopia. East African Medical Journal 1997; 74(8): 491-494.
39. Mengistie B, Berhane Y, Worku A. Predictors of oral rehydration therapy use among under-five children with diarrhea in Eastern Ethiopia: a community based case control study. BMC Public Health 2012; 12: 1029.
40. Dessalegn M, Kumie A, Tefera W. Predictors of under five childhood diarrrhea: Mecha district, West Gojjam, Ethiopia. Ethiopian Journal Of Health Development 2010; 25(3): 192-200.
41. Federal Ministry of Health Ethiopia. Program implementation manual of National Nutrition Programme, July 2008 - June 2013. Addis Ababa: Federal Ministry of Health Ethiopia, 2008.
