One of the most common cancers diagnosed globally is skin cancer, and the incidence and mortality has increased in the past decade1,2. Exposure to ultraviolet radiation (UVR) is the most significant risk factor for skin cancer2,3, specifically squamous cell carcinoma and basal cell carcinoma (collectively known as non-melanoma skin cancer (NMSC))4,5, and melanoma2,6. Worldwide, Australia has one of the highest skin cancer incidence and mortality rates1,7. Two out of three Australians will be diagnosed with skin cancer before 70 years of age7. This represents a significant monetary cost; for example, the treatment of 700 000 NMSCs cost Australia $511 million in 20108. Excessive UVR exposure also has a number of other detrimental health outcomes such as premature ageing and eye disease9,10.
Predominantly, outdoor workers are employed in the agricultural, transport, building and construction industries. Dosimetry methods, which measure UVR exposure, indicate outdoor workers are exposed to much higher than recommended levels of UVR11-14 due to the nature of their occupation13. There is a strong link between outdoor work and increased risk of NMSC4,5. There is also evidence to suggest outdoor workers, despite being exposed to high levels of UVR, do not adopt sun safety behaviours12,15.
In Australia, national workplace health and safety legislation does not specifically mandate sun safety in the workplace, and assessment and action against identified risks is a general responsibility of workplaces. However, some experts suggest there is enough evidence to consider skin cancer an 'occupational disease'16. Workplaces that do not provide sufficient sun safety strategies can be held responsible for skin cancer developed from occupational exposure17. Workplaces can and have implemented policies addressing sun safety strategies15 and mechanisms to raise awareness about skin cancer risks and promote sun safety18.
Currently, there is a lack of evidence about effective sun safety in workplaces. Most evidence is quantitative15 and most recommendations are based on avoiding UVR as a risk factor for NMSCs19, which is often not feasible for outdoor workers. Existing research has examined sun safety policy14,20, environmental changes21-23, education21,22 and workplace culture23,24. The evidence suggests best outcomes are achieved when workplaces adopt multi-strategy interventions for both employers and workers15.
A number of factors may impact the success of health promotion strategies in workplaces. Many Australian 'blue collar' (manual labour) workplaces are characterised by under-resourcing and unrealistic timeframes25, creating job strain, which may limit the capacity of workplaces and workers to prioritise health promotion26,27. The socioeconomic disadvantage in many Australian blue collar workplaces may also limit engagement in workplace health promotion interventions28; indeed, there is evidence to suggest that such workplaces often view workplace health promotion programs as an unnecessary or unaffordable expense27. Additionally, the organisational structure and environmental context of outdoor work contributes to workplace culture, which may have significant impact on the success and sustainability of health promotion strategies29,30. For example, many blue collar workplaces have covert structural frameworks that place an expectation on workers to perform long hours, weekend work and/or irregular work, impairing their ability to maintain a health work-life balance27. In many blue collar workplaces, a pervasive masculine culture and stoicism may lead to sigma associated with health and help-seeking behaviour27. The evidence suggests factors such as the attitude of those involved, the characteristics of the target group, and organisational factors may significantly influence the success of strategies31. This diversity suggests one size is unlikely to fit all, and environmental and cultural contexts need to be considered in customised sun safety strategies.
The Outdoor Worker Sun Protection Project
The Outdoor Worker Sun Protection Project (OWSPP) was conducted by the Queensland University of Technology in partnership with Queensland Health, the Cancer Council Queensland and Curtin University in Western Australia. The purpose of this project was to investigate the most effective combination of sun safety strategies for high risk outdoor workers in Queensland, Australia. Fourteen workplaces across Queensland, each predominantly employing outdoor workers, were recruited to the project. The project defined an outdoor worker as somebody who works outdoors at least 3 hours of the day for 5 days per week. The workplaces represented small and large business sizes across the agricultural, building and construction, public and local government sectors. Workplaces were located across four regions in Queensland: the Darling Downs, North West, Mackay and Far North. The two workplaces selected for this case study article were chosen because they demonstrate the diversity of the workplaces involved in the OWSPP (providing opportunities to make comparisons), the differences in workplace cultures and the need for customised sun safety interventions.
The OWSPP is unique because it is the first study to investigate sun safety strategies for high risk outdoor workers across outdoor industries. Findings from the OWSPP have been reported in various other publications, reports and conference articles32-35. The purpose of this article is to present two diverse case study examples from the OWSPP to demonstrate the influence of workplace culture on sun safety strategies. Each case study will explore the successes, challenges and contextual complexities associated with the effectiveness of sun safety strategies.
The OWSPP collaborated with 14 workplaces across Queensland to develop and implement a customised sun protection program for high risk outdoor workers. The project used a mixed methods approach underpinned by participatory action research (PAR).
Participatory action research
The three fundamental components in PAR are collaboration, participation and reflection (Fig1). These three elements constitute cycles of observation, reflection, planning, action, evaluation and sharing36. The underpinning principle of PAR is about engaging those most affected by change, often the least powerful, as active participants in the change process37. In this project, PAR was considered the best way to work with a diversity of workplace cultures because it allowed workers to influence the identification and implementation of sun safety strategies relevant to their work tasks and environment. The PAR process was guided by the Ottawa Charter (1986) and the project was evaluated using the REAIM paradigm38.
The nature of PAR is compatible with a mixed methods approach because it is collaborative and participatory37. The OWSPP used a mixed methods approach with all workplaces throughout the intervention phase. A mixed methods approach is the amalgamation of a number of qualitative and quantitative methods and takes advantage of the interface, and arising insights, gained from combining these two methods. This approach provided flexibility and adaptability to customise, implement and respond to emerging sun safety strategies in each workplace. It ensured the active engagement of each workplace to guarantee sun safety strategies were relevant and achievable, and provided rich insights about the enablers and barriers to the adoption of sun safe behaviours and a comprehensive picture of sun safety in each workplace.
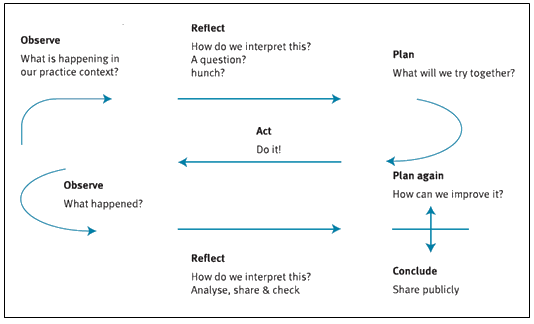
Figure 1: The process of participatory action research.
Recruitment and participants
Workplaces were recruited across four industries: agricultural, building and construction, and public sectors including local government. Workplaces were either small (30 or less workers), medium (between 30 and 99 workers) or large (100 or more workers). Those within 150 km of an airport were eligible for recruitment. The first stage of recruitment involved telephoning every 33rd workplace from the Queensland 2009-2010 business telephone directory. The second stage involved sending an invitation letter to interested workplaces.
The OWSPP established a close working relationship with the workplace champion. In most cases, this was the worker responsible for workplace health and safety identified by the researchers in the recruitment phase. The workplace champions were the primary point of contact at each workplace. Their roles included participating in and facilitating data collection, assisting in the development of the workplace's Sun Safety Action Plan (SSAP) and, with the support of researchers, implementing the workplace's sun safety interventions.
Data collection
Data collection commenced after recruitment phase was completed and was sequential and staggered across workplaces (Fig2). Data were collected before and after intervention using a number of data collection tools: interviews with workplace champions, discussion groups with workers, readings from dosimeter badges (not reported here) and worker surveys. A case study framework was used to both collect and analyse the data (see Data analysis below).
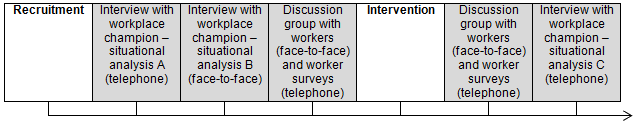
Figure 2: Overview of the data collection process.
Interviews with workplace champions: Before intervention, data was collected from interviews with the workplace champion using situational analysis A and situational analysis B. Each of these tools comprised a set of structured questions that aimed to identify the existing context of sun safety in each workplace. These tools were developed for this project.
Situational analysis A was conducted over the telephone with the workplace champion. This tool was designed for two purposes. First, it was used to initiate contact, develop rapport and seek formal approval for participation from each workplace. Second, this tool was used to establish a baseline context by collecting quantitative and qualitative data about workplace demographics, locations and structures, existing workplace policies and procedures related to sun safety and UVR and workers' compensation histories.
Situational analysis B was a more comprehensive tool and was conducted face-to-face with the workplace champion. The tool was designed to systematically collect qualitative data about workplace sun safety policies and procedures, sun safety risk assessments, personal protective equipment (PPE), structural and environmental sun safety strategies, sun safe education, skin examination and sun safety role modelling.
After intervention, interviews with the workplace champion were conducted using situational analysis C. This tool was designed to identify changes in sun safety strategies that occurred during the intervention phase for each workplace.
Discussion groups with workers: Before the intervention phase commenced, a discussion group with workers from each workplace was pre-organised through the workplace champion. The workplace champion invited available workers to attend a semi-structured discussion group on-site to obtain their views about how sun safety in the workplace could be improved. One further discussion group was conducted at each workplace after intervention to gather information from workers about their perceptions of changes in sun safety strategies that occurred during the intervention phase. The discussion groups facilitated the expression of ideas, valued the workers' existing skills and knowledge and stimulated group thinking.
Worker surveys: Telephone surveys were conducted with workers pre- and post-intervention. The survey was designed to collect quantitative data about workers' behaviours, attitudes and beliefs about sun exposure and protection in the workplace, including knowledge about skin cancer and sun protection measures, perceived skin cancer risk, attitudes towards tanning, perceived workplace support and policy, and training and equipment provision.
Sun Safety Action Plans
After data collection, the OWSPP worked in partnership with each workplace to develop an SSAP. The SSAPs were customised for each workplace and included sun safety strategies related to policy, environment, education and awareness, PPE, skin screening and role modelling. Initially, the OWSPP compiled a draft plan based on the data collected from each workplace; ongoing revisions were invited and discussed until the workplace considered the SSAPs were relevant and achievable.
Data analysis
A case study approach was used to analyse the data for each workplace. A case study provides a framework for exploring and explaining research in real-life settings, and is widely accepted as a rigorous form of enquiry in qualitative research39. Case studies involve in-depth data on multiple variables being collected systematically over time, building to create a comprehensive picture of a situation39. The OWSPP considered the perspective of management and workers (through a discussion group and survey), informed but not constrained by evidence-based strategy information. The case study framework enabled researchers to identify the barriers and enablers to the implementation of the SSAP unique to each workplace.
Ethics approval
Ethical approval for this project was received from the Queensland University of Technology's ethics committee (approval number QUT 1000000968).
This article presents the results of two workplaces recruited to the OWSPP as case studies.
Workplace 1
Workplace 1 is a small family-owned and run agricultural business situated on the Darling Downs in south-western Queensland, Australia. Before recruitment to the OWSPP, workplace 1 had a number of existing sun safety strategies (Table 1).
The baseline discussion group for workplace 1 was held in July 2012. The discussion group included 12 workers and was approximately 40 minutes in length (Table 2).
Eleven workers completed the workers' survey prior to the intervention phase and, of these, eight completed the post-intervention survey.
A number of sun safe strategies were successfully adopted in this workplace (Table 3).
One of the key sun safety interventions in this workplace was the development of a 'working in the sun and heat' policy. Based on extensive discussions with the workplace champions, the OWSPP researchers drafted a policy document for the workplace. The policy was based on the workplace's provision of PPE to reduce workers' sun exposure, including long-sleeved shirts made of lightweight material, a broad-brimmed hat, long pants and sunglasses. The policy was reviewed, discussed and agreed upon by the workplace champions. It was then presented to all workers at a workplace meeting, and workers were given the opportunity to engage in a process of choosing the type of PPE they wished to wear. The sun safety policy and other sun safety information is now given to all new workers during their induction. The 'working in the sun and heat' policy was generally well received; however, workers expressed some concerns about the PPE. Specifically, workers felt the long-sleeved shirts and pants might get and stay wet, and they perceived the uniform changes were primarily to protect the company from litigation.
Education was another key sun safety intervention at this workplace. The workplace conducted a number of toolbox talks on sun safety and skin cancer. A speaker from the Cancer Council Queensland presented at one of these toolbox talks. Workplace champions reported providing sun safety education to workers in a range of other ways, including through verbal reminders and informal discussions with workers, staff meetings, a monthly staff memo and messages on staff pay slips. Brochures and posters from the Cancer Council Queensland were also distributed and displayed in the workplace. The research team also delivered a range of educational materials to the workplace, including weekly emails on sun safety, skin examinations and the UVR Index; website links to factsheets; packages of Cancer Council Queensland educational resources; and workplace sun safety tips and recommendations. Because this workplace had a significant proportion of workers whose first language was one other than English, the effectiveness of the written resources was somewhat limited.
The erection of shade structures was another important sun safety intervention in this workplace. Shade structures were fitted to a number of tractors, and the workplace made a commitment that all new tractors purchased would have a roof. Shade structures were also fitted to the 'bed' machine workers ride on when planting, over the portable 'smoko unit' (providing workers with a shaded place in which to take breaks), and over the diesel pump (located in the middle of a paddock). The workplace manufactured all of these shade structures. Portable shade structures were purchased for workers to use when laying irrigation pipes.
A range of other sun safety interventions were implemented in this workplace. The workplace changed its procurement policy to ensure all new vehicles purchased would have tinted windows and air conditioning (thereby reducing the likelihood that workers would roll down their windows). Workplace managers also demonstrated a commitment to encouraging workers to drive with their vehicle windows up between the hours of 9 am and 3 pm. Dispensers for SPF30+ sunscreen were provided at three locations in the workplace - the workshop, the tearoom and the office - along with posters to encourage use. Sunscreen was also taken by site managers to distribute to workers offsite. Workplace champions regularly checked the sunscreen dispensers to ensure they are available, full and in-date. The workplace provided workers with 1 hour of paid leave annually to receive a clinical skin examination. Additionally, workplace champions demonstrated a commitment to role-modelling sun safe behaviours.
Table 1: Workplace 1 existing sun safety strategies
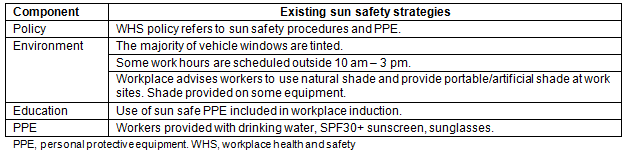
Table 2: Workplace 1 'before and after' themes from discussion groups with workers
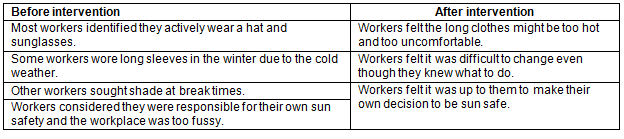
Table 3: Workplace 1 action plan overview - what worked?

Workplace 2
Workplace 2 is a large public sector organisation (government department) situated on the Darling Downs in south-western Queensland, Australia. Before recruitment to the OWSPP, Workplace 2 had a number of existing sun safety strategies (Table 4).
The baseline discussion group for workplace 2 was held in July 2012. The discussion group was comparatively large and ran for approximately 30 minutes (Table 5).
Eighteen workers completed the workers' survey prior to the intervention phase. Twenty-four workers completed the workers' survey after the intervention phase.
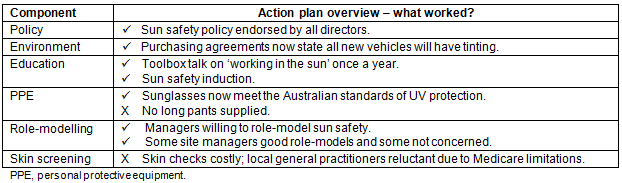
A number of sun safe strategies were successfully adopted in this workplace (Table 6).
The workplace drafted a 'sun protection and outdoor work' policy, which included specific information relating to vehicle window tinting, portable shade and the use of PPE (including long pants and sunglasses). The policy was presented to a workplace health and safety committee for approval, before being endorsed by workplace directors. It was communicated to workers via toolbox talks and on the workplace's intranet. This policy underpinned many of the other sun safety interventions implemented by this workplace, including the adoption of sun safety practice during all work-related social events and the inclusion of a 'sun safe' clause in all work method statements.
As per its new 'sun protection and outdoor work' policy, the workplace updated its purchasing agreement so that all new vehicles purchased would have tinted windows. Workplace managers encouraged workers to drive with their vehicle windows up between the hours of 9 am and 3 pm, using strategies such as reminders in toolbox talks and on the intranet. In addition to window tinting in vehicles, the provision of portable shade was another key strategy outlined in the workplace's new 'sun protection and outdoor work' policy. However, budgetary constraints were a significant barrier to the implementation of portable shade interventions at this workplace, and as a result this intervention did not progress.
A third important sun safety strategy identified under the workplace's new policy was the use of sun safe PPE. The workplace agreed to trial long pants with a UV protective factor, with a longer-term plan of making such PPE mandatory. However, this strategy was strongly opposed by workers (who preferred to wear shorts) and, subsequently, management, and no long pants have been supplied. The workplace did supply workers with wrap-around tinted sun and safety glasses, which comply with minimum Australian sun safe specifications. This strategy was not included in the workplace's original SSAP, but was developed as an additional intervention after the workplace recognised its importance. Despite the difficulties associated with the use of sun safe PPE in this workplace, workplace champions demonstrated a level of commitment to role-modelling the wearing of this PPE.
Education was another key sun safety intervention at this workplace. The workplace updated and presented a toolbox talk about working safely in the sun, presented to workers once annually. The information in the toolbox talk is supported by sun safety messages on the workplace's intranet and in the rolling screen in the lunch room. Posters on sun protection and skin cancer prevention, developed by the Cancer Council Queensland, were displayed throughout the workplace and information about access to other Cancer Council Queensland resources (website, brochures, etc.) was provided to staff. The research team delivered a range of educational materials to the workplace (very similar to the materials provided to workplace 1). Additionally, the workplace improved the amount and type of information about sun safety it provides in its induction sessions.
The final key sun safety intervention implemented at this workplace was the investigation of clinical skin screening options for outdoor workers. However, local general practitioners were hesitant to become involved in this initiative due to Medicare limitations, and the costs associated with the workplace funding skin screens were prohibitive. Instead, the workplace delivered a program of education and awareness about the importance of skin screening early detection of skin cancer, supported by speakers from the Cancer Council Queensland.
Table 4: Workplace 2 existing sun safety strategies
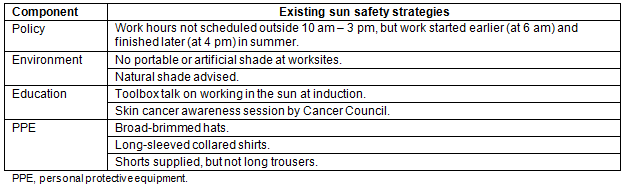
Table 5: Workplace 2 'before and after' themes from discussion groups with workers

Table 6: Workplace 2 action plan overview - what worked?
Limitations
There are limitations to this project:
- The sample of workers was convenient. Some outdoor workers were not able to participate in the discussion group and results may be limited in terms of generalisability.
- The sample of outdoor workers within the two workplaces was small, and the results may not generalise to other workplaces.
- As a population, outdoor workers have low levels of literacy. Workers with lower levels of literacy may have been reluctant to participate in the OWSPP.
- Only one large and one small workplace were included in this article; therefore, the results presented are only indicative.
Discussion
From these two case studies, there are a number of significant themes worthy of discussion. These themes are related to (1) the structure of workplace, (2) policy, (3) workplaces' responses to researchers, (4) the workplace champion and (5) reciprocity.
Workplace structure
The size and structure of each workplace influenced its ability to make decision and progress action, as seen in other similar studies40. Workplace 1 is a small (n=22 workers) family-owned business. There were two workplace champions: one of two brothers who owned the business and the daughter-in-law of one of the brothers who managed the office. This workplace had a relatively flat structure - it was non-hierarchical in nature and responsibilities related to decision-making were shared. This meant decisions were made easily and action was progressed quickly. This process was usually face-to-face, there was little or no paperwork involved and it was often completed within days. Workplace 2 is a comparatively large government organisation (n=190 workers at the research site). The workplace champion was required to seek approval to progress the SSAP through appropriate channels. This took a number of weeks because the workplace champion found it difficult to meet with the line manager, who identified the SSAP could not be given priority because of pending workplace changes. The SSAP was ratified by management some months after it was first initiated by the workplace champion. That the smaller workplace progressed many interventions more successfully than the larger workplace is a novel finding, as similar research suggests smaller workplaces may be more encumbered than larger ones by barriers such as a lack of formal practices and resource shortages41.
Workplace policy
At the beginning of the intervention, neither of the workplaces had a sun protection policy in place. By the end of intervention, both workplaces had implemented a sun protection policy. Workplace 1 adopted a number of policy directives, including the provision of two long-sleeved shirts and a bucket hat to workers each year. Workplace 2 struggled to endorse policy related to long trousers but was successful in securing policy to purchase tinted windows in all new vehicles. There is some evidence to suggest policy alone will not ensure all workers adopt sun safety behaviours14. However, there is also evidence to suggest workers at workplaces with mandatory sun safety polices have lower rates of skin cancer precursors and NMSCs14, indicating mandatory sun safety policy might impact workers' sun exposure, sunburn and skin cancers. In both workplace 1 and workplace 2, policy was considered fundamental to the implementation of an effective sun safety strategy.
Workplaces' responses to researchers
Workplaces that agreed to participate in the OWSPP can be considered to represent sample bias, as they may have had an existing interest in sun safety in the workplace. This may explain an effect - similar to the Hawthorne effect - seen at workplace 1. The Hawthorne effect is seen when the presence of researchers alone evokes action42. For example, after the first site visit, the workplace champion at workplace 1 explored a number of sun safety strategies even before a sun safety action plan was developed for this workplace. This effect related to researchers' presence was not evident at workplace 2.
Workplace champions
Research suggests that there are significant gender differences in skin cancer prevention knowledge, attitudes and behaviours, and the presence of a workplace champion is important in male-dominated workplaces in particular30. The workplace champions in both workplaces were enthusiastic to progress the SSAP and were fundamental to its execution. In workplace 1, one of the workplace champions was able to progress sun safety strategies quickly and easily, and her efficiency was significant in processing the agenda. At the end of the intervention phase, this workplace champion had achieved implementation of multiple sun safety strategies and two additional strategies were in progress. The workplace champion in workplace 2 remained very enthusiastic throughout the intervention phase of the OWSPP despite finding his cause was not shared by line management, senior executives or the workers. Workplace 2 achieved implementation of some sun safety strategies in the SSAP and this was largely due to the determination and perseverance of the workplace champion. Whilst other research indicates the importance of workplace champions modelling sun-protective behaviour43, the workplace champions at workplace 2 demonstrated varying commitment to role-modelling such behaviours, particularly with regards to the wearing of the unpopular UV-protective long pants (as per the workplace's SSAP).
Reciprocity
Overt reciprocity between the workers and workplaces has been found in other similar studies40. This was most obvious in workplace 1. The workplace champions displayed a sense of 'doing the right thing' for their workers but understood the importance of engaging workers in directly impactful decisions. Workers identified an individual responsibility to adopt sun protection strategies; they did not feel it was the workplace's responsibility to implement sun safety strategies on their behalf. However, workers reflected a sense of caring for the owners of their workplace because implementing sun safety strategies would be costly to the workplace. The workers at workplace 2 also identified an individual responsibility to adopt sun protection strategies. However, they felt it was the workplace's responsibility to provide mechanisms for those who chose to adopt sun safety strategies. The workers at workplace 2 intonated respect for the workplace champion but did not display a sense of altruism to the workplace. The workers reflected that sun safety strategies would have to be legislated within occupational health and safety law if sun safety is to be taken seriously. The importance of reciprocity to effective workplace health promotion intervention is becoming widely recognised; indeed, research suggests this promotes a 'collectivist value' of health in the workplace culture, and may contribute to more positive health outcomes44.
The findings reported in this article are important because there is limited evidence about the impact of workplace culture on sun safety strategies for high risk outdoor workers41. The findings offer guidance to health promotion practitioners and policy-makers about effective strategies for workplaces to promote a culture of sun safety.
There are several recommendations from this article:
- Workplaces designate and remunerate workplace champions.
- Workplaces develop and implement mandatory policies on sun safety and related interventions.
- These policies should be reflexive, engaging staff with significant need of sun protection in the policy development process to maximise both worker engagement and 'fit for context' provisions.
- Workplaces seek funding opportunities to implement sun safe strategies (for example, through Queensland Government WorkSafe and WorkCover initiatives).
- Workplaces access sun safety resources from peak Australian government and non-government health promotion organisations.
These two case study examples demonstrate the contextual nature of workplaces when implementing sun safety strategies. This is supported by the findings from other workplaces involved in the OWSPP. Workplaces are complex and those in workplaces are best placed to know what might work in their workplace. Sun safety strategies should be intrinsically driven by the workplace so they are contextually bound and take advantage of existing social capital and connectedness.
Acknowledgements
This work was funded by the State Government of Queensland acting through Health Promotion (QCHO/002068), tender offer no. 00.01/026. The authors thank Jeff Allen and Heather Perina from Queensland Health for their support during the project. The authors also thank the project staff (Emily Mann, Louise Baldwin, Sheree Rye, Kristin Miller, Sarah Mair and Caitlin Horsham) for their contributions to the OWSPP and Laura McCosker for her assistance with reporting.
References
1. Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics. CA: A Cancer Journal for Clinicians 2002; 55: 74-108.
2. World Health Organization. World cancer report 2008. (Internet) 2008. Available: http://www.iarc.fr/en/publications/pdfs-online/wcr/2008/ (Accessed 4 October 2014)
3. Gandini S, Sera F, Cattaruzza MS, Pasquini P, Picconi O, Boyle P, et al. Meta-analysis of risk factors for cutaneous melanoma: II. Sun exposure. European Journal of Cancer 2005; 41: 45-60.
4. Bauer A, Diepgen TL, Schmitt I. Is occupational solar ultraviolet irradiation a relevant risk factor for basal cell carcinoma? A systematic review and meta-analysis of the epidemiological literature. British Journal of Dermatology 2011; 165: 612-625.
5. Schmitt J, Diepgen T, Bauer A. Occupational exposure to non-artificial UV light and non-melanocytic skin cancer - a systematic review concerning new occupational disease. Journal of the German Society of Dermatology 2010; 8: 250-264.
6. McCool JP, Reeder AI, Robinson EM, Petrie KJ, Gorman DF. Outdoor workers' perceptions of the risks of excess sun exposure. Journal of Occupational Health 2009; 51: 404-411.
7. Australian Institute of Health and Welfare. Cancer in Australia: an overview. (Internet) 2008. Available: http://wwwcancer.org.au/preventing-cancer/sun-protection/about-skin-cancer.html (Accessed 4 October 2014).
8. Fransen M, Karahalios A, Sharma N, English DR, Giles GG, Sinclair RD. Non-melanoma skin cancer in Australia. The Medical Journal of Australia 2012; 197: 565-568.
9. Gallagher RP, Lee TK. Adverse effects of ultraviolet radiation: a brief review. Progress in Biophysics and Molecular Biology 2006; 92: 119-131.
10. World Health Organization. Solar ultraviolet radiation: global burden of disease from solar ultraviolet radiation. (Internet) 2006. Available: http://www.who.int/uv/health/solaruvradfull_180706.pdf (Accessed 4 October 2014).
11. Hammond V, Reeder AI, Gray A. Patterns of real-time occupational ultraviolet radiation exposure among a sample of outdoor workers in New Zealand. Public Health 2009; 123: 182-187.
12. Gies P, Wright J. Measured solar ultraviolet radiation exposure of outdoor workers in Queensland in the building and construction industry. Journal of Photochemistry and Photobiology 2003; 78: 342-348.
13. Thieden E, Philipsen PA, Heydenreich J, Wulf HC. UV radiation exposure related to age, sex, occupation, and sun behaviour based on time-stamped personal dosimeter readings. Archives of Dermatological Research 2004; 140: 197-203.
14. Woolley T, Lowe J, Raasch B, Glasby M, Buettner PG. Workplace sun protection policies and employees' sun-related skin damage. American Journal of Health Behaviour 2008; 32: 201-208.
15. Glanz H, Buller D, Saraiya M. Reducing ultraviolet radiation exposure among outdoor workers: state of the evidence and recommendations. Environmental Health 2007; 6: 22.
16. Diepgen TL, Fartasch M, Drexler H, Schmitt J. Occupational skin cancer induced by ultraviolet radiation and its prevention. British Journal of Dermatology 2012; 167(S2): 76-84.
17. Australian Radiation Protection and Nuclear Safety Agency. Regulatory impact statement: radiation protection standard - occupational exposure to ultraviolet radiation. (Internet) 2012. Available: http://www.arpansa.gov.au/pubs/rps/rps12_risfinal.pdf (Accessed 4 October 2014).
18. Soler RE, Leeks KD, Razi S, Hopkins DP, Griffith M, Aten A, et al. A systematic review of selected interventions for worksite health promotion: The assessment of health risks with feedback. American Journal of Preventive Medicine 2010; 38: S237-262.
19. Kuttin B, Drexler H. UV-induced skin cancer at workplace and evidence-based prevention. International Archives of Occupational and Environmental Health 2010; 83: 843-854.
20. Hammond V, Reeder AI, Gray AR, Bell ML. Are workers or their workplaces the key to occupational sun protection? Health Promotion Journal of Australia 2008; 19: 97-101.
21. Borland RM, Hocking B, Godkin GA, Gibbs AF, Hill DJ. The impact of a skin cancer control education package for outdoor workers. The Medical Journal of Australia 1991; 154: 686-688.
22. Mullan PB, Gardiner JC, Rosenman K, Zhu Z, Swanson GM. Skin cancer prevention and detection practices in a Michigan farm population following an educational intervention. The Journal of Rural Health 1996; 12: 311-320.
23. Azizi E, Flint P, Sadetzki S, Solomon A, Lerman Y, Harari G, et al. A graded work site intervention program to improve sun protection and skin cancer awareness in outdoor workers in Israel. Cancer Causes and Control 2000; 11: 513-521.
24. Lombard D, Neubauer TE, Canfield D, Winnett RA. Behavioural community intervention to reduce the risk of skin cancer. Journal of Applied Behaviour Analysis 1991; 24: 677-686.
25. MacKenzie S. A close look at work and life balance/wellbeing in the Victorian commercial building and construction sector. (Internet) 2008. Available: http://services.thomson.com.au/cpdnews/docs/OccHealthNews/DraftWellbeingResearchReport.pdf (Accessed 25 August 2014).
26. LaMontagne, AD, Sanderson, K. Estimating the economic benefits fo eliminating job strain as a risk factor for depression. (Inernet) 2010. Available: https://www.vichealth.vic.gov.au/media-and-resources/publications/economic-cost-of-job-strain (Accessed 25 August 2014).
27. Du Plessis K, Crokin D, Corney T, Green E. Australian blue-collar men's health and wellbeing: contextual issues for workplace health promotion interventions. Health Promotion Practice 2013; 14: 715-720.
28. Kolmet M, Marino R, Plummer D. Anglo-Australian male blue-collar workers discuss gender and health issues. International Journal of Men's Health 2006; 5: 81-91.
29. Cancer Council Western Australia. Occupational exposure to ultraviolet (UV) radiation. (Internet) 2011 Available: https://www.cancerwa.asn.au/resources/2011-12-05-ccupational-exposure-to-ultraviolet-radiation.pdf (Accessed 18 December 2014).
30. Woolley T, Buettner PG, Lowe J. Comparing the sun-related beliefs and behaviours of men and women across age groups: a qualitative study in a tropical region. Journal of Rural and Tropical Health 2010; 9: 101-108.
31. Mitchell PF, Pattinson PE. Organisational culture, intersectoral collaboration and mental health care. Journal of Health and Organisation Management 2012; 26(1): 32-59.
32. Janda M, Stoneham M, Youl P, Crane P, Sendall MC, Tenkate T, et al. What encourages sun protection among outdoor workers from four industries? Journal of Occupational Health 2014; 56: 62-72.
33. Horsham C, Auster J, Sendall MC, Stoneham M, Youl P, Crane P, et al. Interventions to decrease skin cancer risk in outdoor workers: update to a 2007 systematic review. BMC Research Notes 2014; 7: 10.
34. Rye S, Janda M, Stoneham M, Crane P, Sendall M, Youl P, et al. Changes in outdoor workers sun-related attitudes, beliefs and behaviours: a pre-post workplace intervention. Journal of Occupational and Environmental Medicine 2014; 56(9): e62-72.
35. Stoneham M, Sendall M, Crane P, Janda M, Kimlin M. Promoting sun safety in the workplace - what works? Journal of Health, Safety and Environment 2016; 31(2): 141-153.
36. Reason P, Bradbury H. Handbook of action research. London: Sage, 2001.
37. Crane P, O'Regan M. On PAR: using participatory action research to improve early intervention. (Internet) 2010. Available: https://www.dss.gov.au/sites/default/files/documents/05_2012/reconnect_0.pdf (Accessed 18 December 2014).
38. Glasgow RE, Klesges LM, Dzewaltowski DA, Estabrooks PA, Vogt TM. Evaluating the impact of health promotion programs: using the RE-AIM framework to form summary measures for decision making involving complex issues. Health Education and Research 2006; 21(5): 688-694.
39. Snyder C. A case study of a case study: analysis of a robust qualitative research methodology. The Qualitative Report 2012; 17(13): 1-21.
40. Yorio PL, Wachter JK. The impact of human performance focused safety and health management practices on injury and illness rates: do size and industry matter? Safety Science 2014; 62(1): 157-167.
41. Mittelmark MB, Perry MW, Wise M, Lamarre MC, Jones CM. Enhancing the effectiveness of the International Union for Health Promotion and Education to move health promotion forward. Journal of Education and Health Promotion 2007; S2: 33-35.
42. McCambridge J, Witton J, Elbourne DR. Systematic review of the Hawthorne effect: new concepts are needed to study research participation effects. Journal of Clinical Epidemiology 2014; 67: 267-277.
43. Woolley T, Buettner PG. Similarity of sun protection attitudes and behaviours within north Queensland peer groups. The Health Promotion Journal of Australia 2009; 20(2): 107-111.
44. Kawabata M. Is collectivism good for health promotion? Experiences of day labourers in Japan. Global Health Promotion 2013; 20(4): 44-51.
