The New Cooperative Medical Scheme (NCMS) is a voluntary health insurance program established in 2003 to reduce the risk of catastrophic health spending for rural residents in China. It is guided, organized and conducted by the government and financed in part from household contributions and in part from government subsidies1. From the 1950s to 2002, the old Cooperative Medical Scheme was an integrated part of the overall collective system for agriculture production and social services in China. The NCMS had been taken up by 850 million rural residents by the end of 2008 and throughout rural areas in China by 2010, and has been a main component of the Chinese new rural medical insurance system since then. It has been hailed by WHO and the World Bank as the only example of developing countries addressing health funding.
The NCMS is a scheme of voluntary mutual assistance among participating farmers against catastrophic illnesses. The emphasis on covering catastrophic illnesses came from the desire to prevent rural residents from being impoverished by such illnesses. The NCMS has played a positive role in farmers' basic medical protection and improved the quality of farmers' health. The aim of NCMS is to alleviate the financial burden of farmers, to raise the level of farmers' health, and to promote rural economic and social stability. As a mutual scheme, the more farmers that participate, the higher the new cooperative medical participation rate and the greater benefit for farmers. With the expanded scale of NCMS, there has been a basic protection in the health care needs of the farmers, and NCMS can play an active role in more affluent areas of Chinese society2,3.
The aim of the present study is to evaluate the hospitalization cost of rural patients with nephrotic syndrome and to provide useful data for improving the NCMS.
In China at present, rural people have agricultural household registration and urban people have non-agricultural household registration. Only people with agricultural household registration are able to be part of the NCMS. In China, the vast majority of the population has agricultural household registration; in hospitals, most patients come from rural areas. Thus only rural patients were enrolled in the present study.
Three hundred and ninety patients with nephrotic syndrome were enrolled from Department of Nephrology, Qilu Hospital of Shandong University, Jinan, China. All patients came from the countryside. All patients were divided into two groups: group A, 201 patients who joined NCMS between January 2011 and December 2012; and group B, 189 patients who were not part of the NCMS between February 2010 and September 2011. Gender and percentage of patients in the two groups are shown in Table 1. Total hospitalization cost, check cost (such as laboratory testing and ultrasound) and drug cost, length of stay in hospital, amount and proportion of renal biopsy and actual personal expenses were all collected and analyzed.
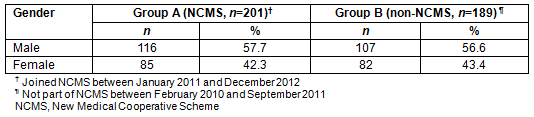
Table 1: Gender and percentages of patients in Group A (NCMS) and Group B (non-NCMS)
Ethics approval
The present study protocol was approved by the ethics committee of Qilu Hospital. Because it was a retrospective investigation, no ethics approval number was required. Written informed consent was obtained from all patients after they had carefully read and understood a written summary of the study plan.
There was no significant difference between the two groups on length of stay in hospital (14.5±2.7 days vs 13.6±1.9 days), but significant difference (p<0.01) was seen in ratio of accepting renal biopsy between different groups (71.6% vs 42.9%) (Table 2). There was no significant difference in total hospitalization cost, drugs cost or check cost between the two groups. Because of reimbursement from NCMS, patients in group A only pay part of cost, so these patients' personal expenses was less than those of group B (p<0.001) (Table 3).
Table 2: Days of hospitalization and ratio of renal biopsy for Group A (NCMS) and Group B (non-NCMS)
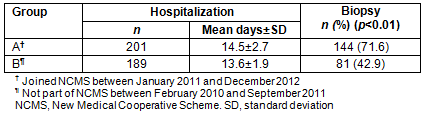
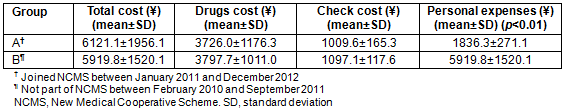
Table 3: Hospitalization costs and personal expenses for Group A (NCMS) and Group B (non-NCMS)
Discussion
The NCMS, first introduced by the Chinese government in 2003, had been taken up by 850 million rural residents by the end of 2008 and throughout rural areas in China by the end of 2010 and the start of 2011. So before the end of 2010, there was a lower proportion of the population that had joined NCMS, but after 2011 the proportion increased significantly. Patients were selected over various time periods to better illustrate the problem in the present study.
People joining the NCMS can obtain reimbursement of hospitalization costs from relevant local departments, and thus actual personal expenses are lower than before. In the present study, there was a significant difference in the actual personal expenses between the two groups (p<0.001) (Table 3). Renal biopsy is an important means to guide treatment of nephrotic syndrome. Patients with nephrotic syndrome should accept renal biopsy4. In the present study, although there was no significant difference between two groups in each cost and the hospitalization time, a significant difference was seen in ratio of renal biopsy (144 vs 81; 71.6% vs 42.9%, p<0.01). Reduced actual personal expenses for patients in group A explains this result.
There was no significant difference in the total cost between the two groups. The patients undertaking renal biopsy get an accurate pathological diagnosis, which helps to set up more targeted therapies for the disease, and can shorten the time of stay hospital, so the cost decreased, and the cost of renal biopsy was added, but the total cost was the same to another group. But for the patients without renal biopsy, there was no pathological diagnosis, the treatment completely depended on the laboratory tests and doctors' experience, the time was longer than patients undertaking renal biopsy, and the cost increased. So there was no significant difference in the total cost between the two groups.
Different groups in rural areas show quite different attitudes to participation in NCMS. Elderly and infirm farmers show great enthusiasm, but young and strong farmers have less positive attitudes. Lack of willingness to participate in the NCMS for high-income farmers resulted in low participation rates and less funds in the NCMS account, which inevitably affects the farmers' medical loss ratio standard. NCMS has a funds accumulation mechanism, which comes from government, the collective and individuals, makes the NCMS a 'low-level, wide coverage' scheme. It is the essential means to ensure the healthy development of the cooperative medical care system5. Although hospitalization expenses decreased because of NCMS and the costs of examination and treatment were reimbursed, not all tests and treatments were covered by NCMS. Nevertheless, hospital costs of patients were lower than before NCMS application.
The actual personal cost of patients who were part of NCMS were lower than for those without NCMS, and more adequate treatment was observed. Patients with renal disease in rural China potentially have benefitted from the scheme.
References
1. Wang Y, Wang J, Maitland E, Zhao Y, Nicholas S, Lu M. Growing old before growing rich: inequality in health service utilization among the mid-aged and elderly in Gansu and Zhejiang Provinces, China. BMC Health Services Research 2012; 12: 302.
2. Huang L, Yang D, Yao L, Liu Z, Wu W. Guangxi's rural health insurance scheme: evidence from an ethnic minority region in China. Rural and Remote Health (Internet) 2013. 13(2): 2454. Available: www.rrh.org.au (Accessed 14 January 2016).
3. Haghdoost A, Momtazmanesh N, Shoghi F, Mohagheghi M, Mehrolhassani M. Accreditation the education development centers of medical-sciences universities: another step toward quality improvement in education. Iranian Journal of Public Health. 2013; 42(Suppl 1): 134-140.
4. Peng T, Guo L, Xia Q, Yang X. Clinical significance of serum CA125 in nephrotic syndrome. Clinical Laboratory 2012; 58(1-2): 113-115.
5. Zhang M, Wu X, Li L, Huang Y, Wang G, Lam J, et al. Understanding barriers to cataract surgery among older persons in rural China through focus groups. Ophthalmic Epidemiology 2011; 18(4): 179-186.
