Chronic conditions (such as arthritis, cancer, diabetes, depression, heart disease, asthma and chronic obstructive pulmonary disease) are a growing healthcare concern in Canada, as in many other developed countries. Approximately half of all Canadians are living with at least one chronic condition1 and it is estimated that chronic conditions amount to more than C$90 billion each year in lost productivity and health care costs2. In the USA, more than 60 million people have multiple chronic conditions3. Similarly, chronic conditions are a major health concern in Australia, with more than 7 million people having at least one chronic condition4. It is essential that effective ways to meet the health needs of this growing population are found.
In addition to healthcare services, people living with chronic conditions need support in learning and maintaining self-care behaviours that enable healthy living, often referred to as 'chronic condition self-management'5-7. Self-management within the context of chronic conditions refers to an individual's ability to manage the symptoms, treatment, and physical, psychosocial and lifestyle changes that accompany living with a chronic condition6,7. Receiving growing recognition as an effective and cost-efficient way of supporting people with chronic physical or mental health conditions to self-manage their health condition is the use of peer supports7,8. A poorly defined and inconsistently used9,10 term in the literature, peer support, for the purposes of this article, refers to support for a person with a chronic condition from someone with the same condition or similar circumstances5.
Peer support within a healthcare context involves '... the provision of emotional, appraisal and informational assistance by a created social network member who possesses experiential knowledge of a specific behaviour or stressor and similar characteristics as the target population'10. Peer supporters largely offer three types of support based on experiential knowledge: emotional, informational and appraisal10. Emotional support involves caring, empathy and encouragement; informational support involves advice, alternative actions suggestions, and factual input relevant to a specific issue; and appraisal support involves affirming feelings, thoughts and behaviors and thus is motivational in nature, encouraging the person to continue with problem-solving attempts despite frustrations10.
In chronic condition management, evidence showing the effectiveness of peer support for people living with chronic conditions to self-manage their conditions is strong6,7,11,12. Heisler provides a thorough overview of seven types of peer support models in chronic condition management5:
- professional-led groups that encourage peer interactions
- structured peer-led self-management training
- peer coaches
- community health workers
- support groups
- telephone-based peer support
- web- and email-based programs.
While Heisler's overview5 is useful in guiding the description, development and evaluation of peer supports for people living with chronic conditions, the unique challenges and strategies accompanying peer support in rural contexts have not been as thoroughly explored. This is particularly worthy of further exploration since many jurisdictions have noted the additional health disparities experienced by people living in rural regions, where economic disparity, aging populations, transportation issues and limited health services can further impact how people are able to manage their chronic conditions13, and that may also impact their ability to access and benefit from peer support programs. As populations in rural areas age, there is often a higher proportion of people with chronic conditions in locations where there may be less access to services. For example, people living with chronic conditions in rural areas face additional challenges as they try to manage their health conditions14. Some of these challenges include limited healthcare resources; few health professionals and consequently fewer support groups; longer distances; unpredictable road and weather conditions14; increased risk for chronic conditions because of tobacco use and exposure, obesity, dietary factors, insufficient physical activities, and socioeconomic factors15. There is a need to learn how best to support people in overcoming these challenges from service providers; providing access to peer supports may be one solution.
Within their local rural context of the south shore of Nova Scotia, which has the oldest population in the province, with high rates of obesity and chronic conditions16, the authors have worked with health and recreation sectors to discuss innovative ways to promote self-management17. Consultations with community partners have identified challenges similar to those identified in the literature faced by the aging populations in this rural area, including poverty, transportation, lack of communication, social isolation, lack of information on community resources and limited social supports. During consultations, strengthening social supports through formal and informal peer support was identified as a key strategy for supporting self-management in this rural region17. In order to inform the development of peer supports in this context, a scoping review was undertaken to discover community-based peer support initiatives for adults in rural settings living with chronic conditions.
Scoping reviews are exploratory in nature, with the aim of summarizing a range of research activities, mapping key concepts, identifying main sources of evidence and identifying gaps in the literature about a research topic18,19. They can be useful tools for knowledge exchange and transfer with community partners who can offer content expertise and perspectives on preliminary findings19. Scoping reviews are particularly appropriate for topics with emerging evidence that lack randomized control trials19 and where it is anticipated that literature may be limited or there would be diversity in types of studies20. As such, unlike systematic reviews, which strive 'to provide answers to questions from a relatively narrow range of quality assessed studies', scoping reviews are 'less likely to address very specific research questions or, consequently, to assess the quality of the included studies'18.
The authors followed the five stages of a scoping review outlined by Arksey and O'Malley18 and advanced by Levac et al19, with a brief description of the research team's process at each stage.
Identify research question: This scoping review aimed to answer the question What is known from the existing literature about the key features and potential formats of community-based peer support initiatives for adults living with chronic conditions in rural settings? Structures of peer support in rural areas and the support/preparation provided to peer leaders in these rural settings developed into sub-questions.
Identify relevant studies: A research librarian was contracted to create and run searches in six databases (CINAHL, PubMed, Sociological Abstracts, Embase, Cochrane Library and PsycInfo) from the date of inception to July 2013. The searches combined the concept of chronic conditions (including both physical and mental health conditions) with the concept of rural, community-based peer support. These concepts were captured by identifying relevant index terms and their free-text synonyms. See Appendix I for the full PubMed search strategy. The search was adapted to the other databases, taking into account appropriate search syntax and corresponding index terms. The search produced a total of 1978 abstracts. The references of included studies and related reviews were checked for additional relevant citations, which were also reviewed in relation to the inclusion and exclusion criteria below.
Study selection: In light of a detailed protocol that provided descriptions of inclusion/exclusion criteria with examples, all abstracts were reviewed by two research team members. Inclusion criteria featured:
- interventions/programs (rather than opinion pieces)
- the years 2000-January 2014 (to ensure currency)
- English only (due to language limitations of the research group)
- adults (≥18 years)
- explicit involvement of peers who work with people who have a chronic condition the peer is familiar with
- community-based (rather than hospital-based) with an emphasis on community involvement (rather than medical management)
- explicit reference to being located in rural settings.
Inclusion/exclusion criteria were further refined and discussed by the research team to address any ambiguous articles encountered. Through these discussions, the following exclusion criteria were refined:
- professional-led initiatives with no focus on the development of peer supports
- initiatives that only focus on friendship development without reference to community involvement
- initiatives that focus on caregivers of people with chronic conditions
- involvement of lay leaders who do not have lived experience of chronic condition.
Following the review of all 1978 abstracts by two team members, 1907 articles were excluded, leaving 71 articles to be reviewed in full. Each of these 71 articles was read by two team members. The research team met regularly during this stage to discuss challenges in applying the inclusion/exclusion criteria and their modifications, including (a) excluding projects from developing countries (where differences in contextual factors limited applicability to the Canadian context) and urban-based telephone peer support, and (b) including projects that targeted people at risk of chronic conditions, in addition to those living with chronic conditions. A secondary review of bibliographies was also conducted, retrieving 74 possible articles, but all were excluded, primarily because they did not occur in rural settings. The selection process resulted in 13 articles meeting the inclusion criteria (representing 10 separate programs). See Figure 1 for an overview of the search process.

Figure 1: Overview of search process.
Charting the data: Key information about the included articles was charted (including information on context, recipients, intervention and ongoing support, and peer leader information) and reviewed to identify key themes across the programs using a qualitative content analysis approach.
Collating, summarizing and reporting results: Preliminary analysis of included articles occurred and was shared at a national conference21 and with community partners.
Consultation: The topic of peer support in rural communities was first identified by community partners in the context of a collaborative research project that aimed to support people living with chronic conditions to become actively engaged in their communities17. This collaborative research project took place in the south shore of Nova Scotia, which comprises many rural communities. The final consultation with community partners included review of the findings in light of their local context.
Ethics approval
According to Dalhousie University's Research Ethics Board, ethics approval is only required when there are human subjects involved, which is not the case in a scoping review.
Based on the 13 articles that met the inclusion criteria, the key features and formats of rural peer support programs for people with chronic conditions were identified. The study descriptions are briefly summarized in Table 1 to provide a general overview of the range of literature available in this field. This is followed by a synthesis of the programs' peer leader roles and support, content of programs and key elements, and issues related to program implementation and sustainability. Considerations in designing peer support in rural areas form the results of this scoping review.
Study descriptions
Seven of the 10 included programs were located in the USA, two were from Australia and one from Canada; all were in self-identified rural areas as is shown in Table 1. Half of the programs (five) focused on diabetes education. Of the remaining programs, two targeted people with multiple chronic conditions, one focused on mental health and one addressed risk for cardiovascular disease. Three programs targeted women specifically15,22,23, and two targeted distinct cultural groups (African Americans and American Indians)24,25. A range of formats was used in the initiatives, with four programs using telecommunications only (including one or more of the following: websites, discussion boards, emails, telephone and/or telehealth), four using in-person meetings only and two combining telecommunication and in-person.
Peer leader roles and support
Peer leaders in the included programs had varied experiences with chronic conditions. Some peers had the shared experience of the same chronic condition as those targeted by their initiative23,25-31, while others shared the general experience of having a chronic condition22,26-28,32,33. Other peer leaders had family members/close friends with the condition25,29,31 or had a shared risk of the condition based on shared social characteristics or culture15,24,29. All studies except one provided training to peers but not to the program participants; the exception was the Women to Women project22,26-28.
Within programs offering peer training, peers were trained to use computer/telecommunications or a website22,23,26-28,32, provide educational information about conditions and/or management of conditions15,25,31-33, encourage physical activity training29, and provide information about local resources29,31. Some programs also provided training on how to engage with participants, in addition to the content of interactions: ways to motivate others31, teaching others to problem solve31,32, and providing non-directive support29. Peers were involved in research of the program in one project and thus provided training to peers on collecting data for the project and ethical treatment of research participants31.
Programs with ongoing support for peer leaders included mechanisms such as regular meetings for peer leaders29, remuneration25,31, rewards15,24,31 and/or recognition for leading24, flexible scheduling and breaks from leading31, and finding ways to streamline paperwork31. Some studies commented specifically that the long-term success of the program would depend on the continued action of peer leaders beyond the duration of the immediate project24,29. Peer leaders were noted to be susceptible to burnout31.
Table 1: Program descriptions and target groups
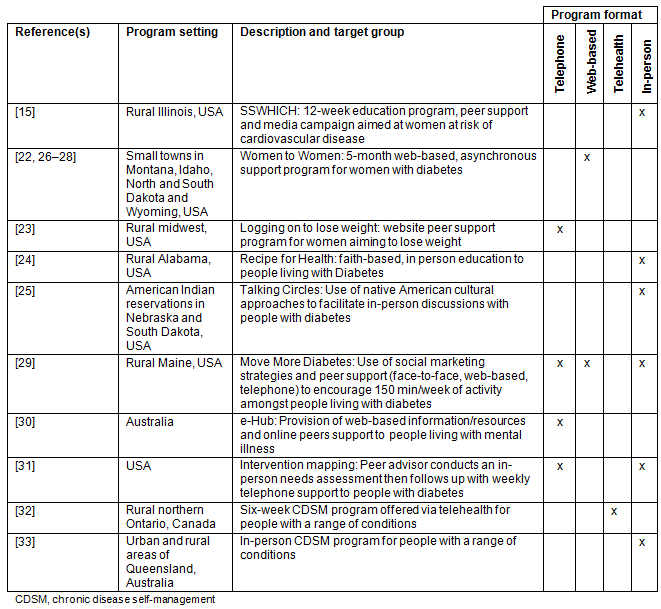
Content of programs and key elements
Information on the chronic condition was provided to program participants in all 10 programs. The majority of the programs explicitly provided general social support to participants8 and developed new skills8. Examples of skills that were taught/developed included using a computer to assess health information22,26-28, preparing meals24,25, improving self-management skills29,32,33, goal setting and problem solving31 and general skills to promote lifestyle changes15. Six programs tracked or promoted physical activity15,23,29,31-33 and three monitored diet/weight loss15,23,31.
Promoting social connectedness, reducing stigma, resonance and empowerment were also key features of these programs, in addition to skill development. As it relates to promoting social connections, several studies reported that participants valued the sense of feeling connected to others. In some cases, the social contact specifically motivated participants to complete or participate in program activities.
In recognition of the possibility that stigma may play a role in program participation, programs provided strategies to mitigate stigma, including use of telecommunications with de-identification processes in place, such as passwords and pseudonym usernames23,30; holding face-to-face meetings in places available to a variety of populations (eg community centres, churches)15; and not labelling interventions as specifically just for people living with chronic disease29.
Studies note the important role of the peers in translating information to participants in ways that make sense to them, and/or to match the culture, world view and/or value system of participants24,25. Again, this is noted as a crucial strategy for marginalized populations or populations sharing a particular culture24,25. The importance of participant empowerment in study design or in effecting change was noted in a number of studies15,22,24-28,31,33. The significance placed by participants33 and/or peer leaders25 on making a meaningful contribution to the process and/or to be able to reciprocate by helping others33 was noted in some studies.
Program implementation and sustainability
In addition to peer leaders' support, a number of approaches were taken to enhance recruitment, implementation and sustainability of the programs. Several programs used mass media campaigns as a way to recruit participants15,22,23. Zimmermann et al15 note that mass media campaigns are especially good for rural areas as costs are lower in these areas than in urban areas, and are effective at reaching a dispersed population. Meaningful goal setting contributed to motivation for physical activity; however, being able to set own goals was reported as more relevant23. In one study, goals set in person with peer support were followed up via weekly and then monthly telephone calls31, illustrating how telecommunications can allow for longer term support. Studies that utilized telecommunications as part of the intervention often provided technical support services to ensure effective use throughout the program22,23,26-28,30,32.
During design and implementation, several studies commented specifically that consulting with local leaders/members of the community during the design phase was crucial to the success of the program15,24,25,31. Building on extant resources in the community further achieved involvement of the local community. Specific resources may include existing organizations or networks15,24,29, physical infrastructure such as walking paths and gyms29, or telehealth equipment at local hospitals32. This is especially true of communities comprising mainly vulnerable or marginalized populations24,25,31. One study noted the need for timelines long enough for the program to be effective15.
Outcomes
Of the nine studies that reported on program outcomes, eight reported positive outcomes with one study reporting mixed results. Overall program success, participants valuing the social aspects of the programs, improved activity or weight loss, and participants feeling increased feelings of efficacy were the related positive outcomes reported.
Discussion
There is a need for low-cost and sustainable interventions that meet the unique needs of people living with chronic conditions in rural regions; peer support interventions seem to be a potentially viable option. The authors sought to understand the characteristics of peer support interventions intentionally designed for delivery in rural contexts through a scoping review. Consistent with the extant literature, all the initiatives identified unique issues faced by people with chronic conditions in rural areas that their program identified as important to recognize and address, including lack of access to basic health services22,26-28,31, lack of appropriate places to exercise29, lack of access to fresh food15, and/or increased levels of social isolation22,26-28,31.
The programs were also designed to consider the cultural context (wherein people may want to access local networks instead of formal programs), rural people's capacity to travel distances to meet or to absorb other costs that could inhibit participation22,26-28,31, and the time commitment required by participants to be involved in the study22,26-28. Use of telecommunications appeared to be especially useful to alleviate problems associated with distance and isolation in rural areas22,26-28,30,31. In particular, the flexibility in scheduling allowed by asynchronous chat/email was considered very valuable to rural users with limited time22,23,26-28. A final issue noted as a unique challenge in rural contexts was the difficulty of achieving anonymity in small communities and its possible negative effect on program participation25.
Limitations
An examination of the research and evaluation methods of the programs included within the review is not a focus for a scoping review; thus the studies included were primarily supported by descriptive results and satisfaction surveys, which limits transferability of findings. Further research and/or evaluation of peer support interventions is required to move beyond program satisfaction surveys to identifying factors that consistently contribute to the successful implementation of programs that effect meaningful change in the daily lives of participants living in rural contexts.
Based on the populations served by the included studies, the findings of this scoping review are not applicable in lower income, developing countries as these were excluded because of significant differences in health and contextual factors compared to the context of interest, rural Canada. Finally, ambiguity pertaining to some of the key search terms, such as 'peer', and limited details provided regarding the rural nature of program contexts (eg some telephone peer support programs did not indicate if they were in rural or urban areas) may have excluded relevant studies.
Implications
The following summary consists of four key implications for research and practice yielded from this scoping review regarding peer support in rural areas for people living with chronic conditions:
- A combination of telecommunications - telephone and online supports - with some face-to-face meetings can support the accessibility of peer support programs in rural areas. Diversity of formats can assist in meeting diverse learning styles as well as challenges with transportation in these contexts.
- A core element of peer support programs for people with chronic conditions in rural areas is the provision of social support and skill development, in daily activities, health information and self-management strategies. How this material is presented is important in promoting its relevance, acceptability and usefulness to participants. Strategies to mitigate perceived stigma associated with having a chronic illness need to be considered, as do strategies for promoting participant involvement in effecting change and being valued contributors to the process.
- The training of peer supporters in skills including using telecommunications, sharing chronic condition management strategies and providing information about local resources is important as is training in how to engage participants with the material (eg ways to motivate others, teaching problem solving). Central to peer supporters being able to do their work is the provision of ongoing support (eg meetings, recognition) to them. This is consistent with peer support leader training (not specific to rural areas), which emphasizes the importance of systematic training of leaders34.
- Sustainability of such programs is complex and requires broad mass media campaigns, meaningful goal setting, consultation with local leaders, building on existing resources, ongoing technical support and reasonable timelines that allow for these connections to be fostered. The development of peer support initiatives must take into account local cultural values and beliefs. This pertains to different ethnic groups, but also to particular cultures and ways of interacting that may be unique to rural communities. For example, rural communities may have more informal ways of providing general support to community members in ways that are considered acceptable (eg informal networks for checking on those who may need help with snow clearing or during particularly poor weather), and it is possible that better understanding of these informal networks could inform ways to strengthen formal peer support in these communities.
The scoping review findings can also be used to inform ongoing discussions with community partners as the authors collaboratively explore the potential role of peer support in their local Nova Scotian context.
Potential areas for further research
Beyond the findings about program structure and content, this scoping review also highlights a number of areas that require further exploration. One notable challenge encountered by the research team when conducting this review was variability in definitions of 'peers'. Even in the included studies, variations in experience with chronic conditions (eg lived experience with a chronic condition versus being a family member of someone with a chronic condition) are evident. Further clarity on these definitions coupled with research on the implications of different peers is called for. What are the benefits or potential drawbacks of training peers with chronic conditions themselves, versus peers who primarily have experience in supporting a family member? In rural contexts where populations are sparse, might greater flexibility in this definition be necessary to meet the needs of peer support? More research on how peers are defined and what is realistic in rural settings is required.
The impact of age and gender on the development, implementation and evaluation of peer support programs in rural areas has not been thoroughly explored. We know that gender impacts health behaviors, access to services, social participation and activity choices, among other considerations. These are all relevant to peer support programs in rural areas that aim to increase social participation and health, thus a gender analysis of program participation would be helpful in identifying effective supports distinguished by gender. Similarly, factors such as age and ethnicity also affect participation and should be specifically examined.
While the programs in this scoping review illustrate a range of combinations of teleconference and face-to-face interactions, factors to consider in determining a reasonable array of communication strategies within a particular rural community have not been explored. What has to be accounted for when determining the type and frequency of peer interactions in a rural setting and what is the most appropriate balance of these?
The issue of sustainability was discussed in most of the included programs. Cherrington et al31 point specifically to the lack of studies investigating how to sustain programs beyond the life of the study, particularly with regard to peer leadership. Communities will have to consider whether peer leaders will have the continued interest and/or stamina to sustain the program through time. A potential solution is to build the capacity of peer leaders to teach others to become peer leaders24. Further exploration of this 'training of trainers' model and ways to best support it may be particularly relevant to rural communities with lower population densities.
As researchers with clinical backgrounds in occupational therapy (HL) and recreational therapy (SLH), the authors were intrigued that some of the programs particularly noted the importance of meaningful activities, some of which were recreational in nature. Building on the notion of sustainability, the authors proposed that theories from occupational science35 and leisure studies36, as well as the practical involvement of occupational therapists and recreational therapists in such peer support programs, may make a positive contribution to the sustainability of peer support programs by emphasizing linkages with local recreational programs and other opportunities for community participation (eg volunteering).
The findings of this review suggest areas to be discussed if a rural community is considering how to plan, implement and evaluate peer support. Diversity of formats (eg combinations of telephone and online supports), strategies to ensure material is presented in relevant ways and the training of peer supports are key elements of any program. However, further research is required to explore the quality of programs and the effectiveness of their outcomes. Although further research is required, the results of this scoping review do provide a basis for potential conversations with community partners. Based on the findings of this scoping review, potential questions to guide community discussions regarding peer support may include:
- What are key context considerations in our local community, like culture, transportation and available resources?
- How will we define 'peers' based on the needs of the community and the resources/experiences available?
- In our local context, what are the advantages and disadvantages when considering different formats for peer support (eg prevalence of internet access in homes, general comfort with technology within the community, size of the community and people's desire for anonymity regarding their health concerns)?
- What relevant community resources and community leaders should we build upon and consult with?
- What types of training and support will be provided to peers and participants?
- What are locally relevant ways to ensure resonance, empowerment, sense of connection and reciprocity within peer support?
Acknowledgements
The authors would like to acknowledge the following contributions of their team: Robin Parker, W.K. Kellogg Health Sciences' Librarian, generated and applied the search strategy; Nadine Geddes, Research Associate, organized the research team during the review stage, contributed to article reviews, and charted article data; Beth Hargarty, Research Assistant and Masters student, assisted with article reviews; and Sue Haydt, Research Assistant, assisted with data analysis. Thank you to Dalhousie University's Faculty of Health Professions' Research Development grant, which supported this research. Preliminary findings of this project were reported at the Canadian Association of Occupational Therapists' Annual Conference in 2014.
References
1. Health Council of Canada. How do sicker Canadians with chronic diseases rate the health care system? Results from the 2011 Commonwealth Fund International Health Policy survey of sicker adults. Canadian Health Care Matters, Bulletin 6. Toronto, ON: Health Council of Canada, 2011.
2. Mirolla M, for Chronic Disease Prevention Alliance of Canada. The cost of chronic disease in Canada. Ottawa, ONT: Chronic Disease Prevention Alliance of Canada, 2004.
3. Wu S, Green A. Projection of chronic illness and prevalence and cost inflation. RAND Corporation, 2000.
4. Australian Institute of Health and Welfare. Authoritative information and statistics to promote better health and wellbeing: chronic diseases. (Internet) 2015. Available: http://www.aihw.gov.au/chronic-diseases/ (Accessed 11 May 2015).
5. Heisler M. Overview of peer support models to improve diabetes self-management and clinical outcomes. Diabetes Spectrum 2007; 20: 214-223.
6. Health Council of Canada. Self-management support for Canadians with chronic health conditions: a focus for primary health care. (Internet) 2012. Available: http://www.healthcouncilcanada.ca/rpt_det.php?id=372 (Accessed 11 May 2015).
7. de Silva D. Helping people help themselves: a review of the evidence considering whether it is worthwhile to support self-management. London: The Health Foundation, 2011.
8. Boothroyd RI, Fisher EB. Peers for progress: promoting peer support for health around the world. Family Practice 2010; 27: 162-168.
9. Doull M, O'Connor AM, Welch V, Tugwell P, Wells GA. Peer support strategies for improving the health and well-being of individuals with chronic disease (Protocol). Cochrane Database of Systematic Reviews 2005(3). Art. no. CD005352.
10. Dennis C. Peer support within a health care context: a concept analysis. International Journal of Nursing Studies 2003; 40: 321-332.
11. Chronic Illness Alliance. Peer support for chronic and complex conditions: a literature review. (Internet) 2011. Available: http://www.chronicillness.org.au/images/linked_documents/PeerSupportforChronicandComplexConditionsLitRevMay2011Final.pdf (Accessed 2 May 2015).
12. Cook JA, Copeland ME, Corey L, Buffington E, Jonikas JA, Curtis LC, et al. Developing the evidence base for peer-led services: changes among participants following Wellness Recovery Action Planning (WRAP) Education in two statewide initiatives. Psychiatric Rehabilitation Journal 2010; 34(2): 113-120.
13. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. (Internet) 2006. Available: https://secure.cihi.ca/free_products/rural_canadians_2006_report_e.pdf (Accessed 2 May 2015).
14. Sullivan T, Weiner C, Cudney S. Management of chronic illness: voices of rural women. Journal of Advanced Nursing 2003; 44(6): 566-574.
15. Zimmermann K, Khare MM, Huber R, Moehring PA, Koch A, Geller SE. Southern Seven Women's initiative for cardiovascular health: lessons learned in community health outreach with rural women. American Journal of Health Education 2012; 43(6): 349-355.
16. Government of Nova Scotia. Nova Scotia Community Counts survey data. Halifax, NS: Government of Nova Scotia, 2004.
17. Barnes M, Lauckner H, Hutchinson S. Linking recreation and health with people living with chronic conditions. (Poster). Halifax, NS: Canadian Congress of Leisure Research, 21-24 May 2014.
18. Arksey H, O'Malley L. Scoping studies: towards a methodological framework. International Journal of Social Research Methodology 2005; 8(1): 19-32.
19. Levac D, Colquhoun H, O'Brien KK. Scoping studies: advancing the methodology. Implementation Science 2010; (5): 69.
20. Canadian Institute of Health Research. More about knowledge translation at CIHR. (Internet) 2014. Available: http://www.cihr-irsc.gc.ca/e/29418.html#7 (Accessed 2 May 2015).
21. Lauckner H, Hutchinson S, Geddes N, Hagarty B. Peer supports in rural areas: integrating literature and community perspectives. Fredericton, NB: Canadian Association of Occupational Therapists' Conference; 7-10 May 2014.
22. Smith L, Weinert C. Telecommunication support for rural women with diabetes. The Diabetes Educator 2008; 26(4): 645-655.
23. Pullen CH, Hageman PA, Boeckner L, Walker S, Oberdorfer M. Feasibility of Internet-delivered weight loss interventions among rural women ages 50-69. Journal of Geriatric Physical Therapy 2008; 31(3): 105-112.
24. Gore TN, Williams A, Sanderson B. Recipe for health: impacting diabetes in African Americans through faith-based education. Journal of Christian Nursing 2012; 29(1): 49-53.
25. Struthers R, Hodge F, De Cora L, Geishirt-Cantrell B. The experience of native peer facilitators in the campaign against Type 2 diabetes. Journal of Rural Health 2003; 19(2): 174-180.
26. Hill W, Weinert C. An evaluation of an online intervention to provide social support and health education. Computers, Informatics, Nursing 2004; 22(5): 282-288.
27. Hill W, Schillo L, Weinert C. Effect of a computer-based intervention on social support for chronically ill rural women. Rehabilitation Nursing 2004; 29(5): 169-173.
28. Hill W, Weinert C, Cudney S. Influence of a computer intervention on the psychological status of chronically ill rural women: preliminary results. Nursing Research 2006; 55(1): 34-42.
29. Richert ML, Webb AJ, Morse NA, O'Toole ML, Brownson CA. The Diabetes Educator 2007; 33(6): 179s-184s.
30. Bennett K, Reynolds J, Christensen H, Griffiths KM. E-hub: An online self-help mental health service in the community. Medical Journal of Australia 2012; 192(Suppl. 11): S48, S52.
31. Cherrington A, Martin MY, Hayes M, Halanych JH, Wright MA, Appel SJ, et al. Intervention mapping as a guide for the development of a diabetes peer support intervention in rural Alabama. Preventing Chronic Disease 2012; 9: e36.
32. Jaglal SB, Haroun VA, Salbach NM, Hawker G, Voth J, Lou W, et al. Increasing access to chronic disease self-management programs in rural and remote communities using telehealth. Telemedicine and e-Health. 2013; 19(6): 467-473.
33. Kendall E, Foster MM, Ehrlich C, Chaboyer W. Social processes that can facilitate and sustain individual self-management for people with chronic conditions. Nursing Research and Practice. 2012; 2826-2871.
34. Tang TS, Funnell, MM, Gillard M, Nwankwo R, Heisler M. The development of a pilot training program for peer leaders in diabetes: process and content. The Diabetes Educator 2011; 37: 67-77.
35. Wilcock AA. Occupational science: bridging occupation and health. Canadian Journal of Occupational Therapy 2005; 72(1): 5-12.
36. Nimrod G, Hutchinson SL. Innovation among older adults with chronic health conditions. Journal of Leisure Research 2010; 42(1): 1-24.
_____________________________
Appendix I: Example search strategy.


