The origin of rural community postings for medical students in Nigeria's university system is the Ibarakpa Community and Primary Healthcare Programme of the University of Ibadan, in Ibadan in western Nigeria, which was initiated in 19631. This program, which was initially named the Ibarakpa project2, preceded the famous Alma-Ata declaration on Primary Health Care by 15 years3. It has been described as an interdisciplinary training program in community health, development and empowerment2. Based on the realization that community-based education has been useful in developing health personnel who are responsive to community needs4,5, this concept has in recent times been regarded as an innovative approach to medical education6-8.
Some specific objectives of the Ibarakpa Community and Primary Healthcare Programme were to teach medical students, through practical work, the principles and practice of community medicine and to build a body of knowledge on the several factors that influence health promotion and disease prevention in rural communities1. Studies from other regions of the world have revealed a significant relationship between exposure to a rural clinical school and willingness of medical students to practise in rural areas after graduation9,10. It has also been found that exposing medical students to community field works during the period of training motivates the students to work in rural areas after graduation11.
In Nigeria, no medical school is located in a rural area; however, every medical student undergoes a rural-based medical education by virtue of the rural community posting. The rural community posting is a mandatory and rotational 2-3-month rural community experience by medical students during the period of training. This rural community program is under the supervision of the departments of community medicine of the various institutions and at present is a prerequisite for the accreditation and re-accreditation of any medical school in Nigeria. The National Universities Commission, in adopting the rural community posting as part of the curriculum of medical schools in Nigeria, viewed it as a way of introducing the students to life in rural community settings with the aim of assisting them to develop the skills, attitudes and motivation to work and live in rural communities after graduation12. Some federal medical centers in Nigeria, which serve as tertiary health facilities, have also adopted this rural community healthcare program, especially if that institution hosts a department of community medicine.
Except for the accreditation programs of the various universities (once every 3-5 years) by the National Universities Commission, there has been no formal evaluation of the rural community program. However, it has been found that there is a significant relationship between satisfaction with rural community posting and willingness of medical students to practise in rural areas after graduation13. Medical practice in rural area is of relevance because a higher proportion of Nigerians reside in rural areas14, where access to doctors is lower than in urban areas15 and the health indices are poorer16. Perhaps all these necessitated the call for the rural community posting to be student oriented and the need to emphasize this rural community experience for doctors in training13. Similarly, WHO policy recommendations on how to increase access to health workers in rural areas acknowledged the need for clinical rotations in rural areas during training17. And from a study in Nepal, medical students were of the opinion that repeated rural exposures and postings in rural hospitals and health centers would adequately prepare them for medical practice in rural areas18.
The present study was conducted among final year medical students in medical schools of south-east Nigeria to determine their satisfaction with rural community posting.
Setting
The study was conducted in medical schools in south-east Nigeria, which is one of the six geo-political zones in Nigeria. It is made up of five states: Abia, Imo, Ebonyi, Anambra and Enugu. It has a population of 16 381 729 people19, within a total area of 28 987 km220. The inhabitants are mostly of Igbo ethnic nationality and are predominantly Christians.
The south-east zone of Nigeria has 17 universities, comprising six federal and five state universities, while the remaining six are privately owned. Medicine is accredited for study in six universities in the zone. Two of these universities belong to the Federal Government of Nigeria: Nnamdi Azikiwe University, Awka, and the University of Nigeria, Nsukka, which was established in 1960 and is Nigeria's second oldest university. The state-owned universities that offer the study of medicine are those of Abia, Imo, Ebonyi and Enugu states.
Study design and participants
The study employed a cross-sectional descriptive study design using self-administered questionnaires.
The study population consisted of all final year medical students in medical schools of south-east Nigeria who had completed their rural community posting and also gave consent to participate in the study. The students completed the questionnaire after they had completed the rural community posting.
A total of 457 final year medical students in the six medical schools in south-east Nigeria participated in the study, representing a response rate of 86.7%. The participating medical schools included University of Nigeria, Nsukka (132 medical students, response rate 95%), Nnamdi Azikiwe University, Awka (79 students, response rate 82.3%), Abia State University, Uturu (67 students, response rate 80.7%), Ebonyi State University, Abakaliki (79 students, response rate 90.8%), Enugu State University of Science and Technology, Enugu (37 students, response rate 74%) and Imo State University, Owerri (63 students, response rate 87.5%).
Study instrument
The study instrument was a pretested, semi-structured questionnaire designed by the researchers. The aim of the pretesting was to detect and correct deficiencies or ambiguities of the study instrument. Information was obtained on the socio-demographic characteristics of the students, on whether or not they were satisfied, and why, with the rural community posting, the measures that could be adopted to improve the rural community posting and whether or not a good rural community posting could influence the willingness of the students to practise in a rural area after graduation.
Data analysis
The analysis was performed using STATA statistical software v13 (StataCorp; http://www.stata.com). Frequency tables and cross-tabulations were generated and level of significance was based on p<0.05. Multivariate analysis using binary logistic regression was used to determine the factors predictive of satisfaction of students with rural community posting. Variables with p<0.2 in bivariate analysis were entered into the logistic regression model to determine the predictors of students' satisfaction with their rural community posting. The results were reported using adjusted odds ratio (AOR) and 95% confidence interval (CI).
Ethics approval
Ethical approval for the study was obtained from the Health Research and Ethics Committee of the University of Nigeria Teaching Hospital Ituku-Ozalla, Enugu, with approval number NHREC/05/01/2008B-FWA0002458-IRB00002323. The students were required to sign a written informed consent form before participating in the study. The nature of the study, its relevance and the level of their participation were well explained to them. They were assured that all information that they provided in the questionnaire would be treated confidentially and anonymously. Participation in the study was voluntary and participants were assured that there would be no victimization of anyone who refused to participate or who decided to withdraw from the study after providing consent.
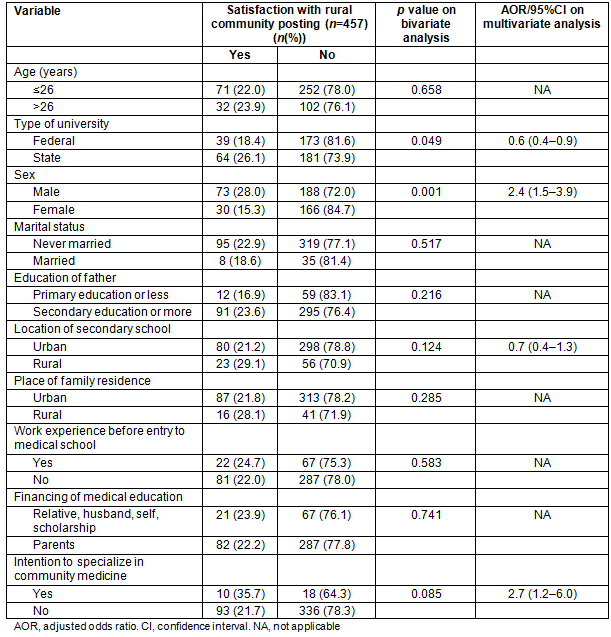
Table 1 shows the socio-demographic characteristics of the students. The mean age of the students was 25.5±2.9 years with the majority (51.6%) within the age group of 25-29 years. A higher proportion of the students (57.1%) were male and the majority of the parents of the students had a tertiary education. Most students had an urban background and had attended secondary schools in urban areas.
Table 2 shows the satisfaction of the students with their rural community posting. A minor proportion of the students (22.5%) were satisfied with their rural community posting. The most common reasons for dissatisfaction among the students included lack of interest in rural communities (30.5%), poor supervision (24.3%) and inadequate community exposure/experience (21.2%). Suggestions by the students on how to improve the posting were improved interaction with lecturers during the posting period (66.9%), proper rural community posting orientation (38.9%), provision of transport (31.7%) and availability of residential quarters for the students (30.4%). Most of the students (68.7%) were of the opinion that a good rural community posting could influence students to practise in rural area after graduation.
Table 3 shows the factors affecting the satisfaction of the students with their rural community posting. The medical students in federal universities were half as likely to be satisfied with rural community posting as those from state universities (AOR=0.6, 95%CI=0.4-0.9). The male medical students were 2.4 times more likely to be satisfied with rural community posting than were female medical students (AOR=2.4, 95%CI=1.5-3.9). The students whose intention was to specialize in community medicine after graduation were about three times more likely to be satisfied with their rural community posting than those who did not have such an intention (AOR=2.7, 95%CI=1.2-6.0).
Table 1: Socio-demographic characteristics of respondents
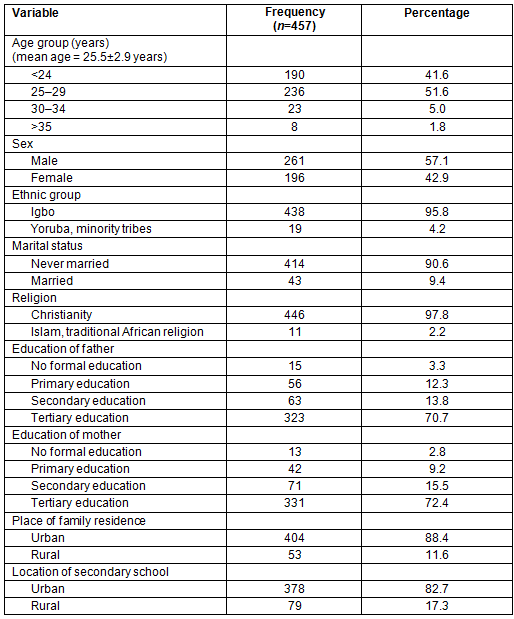
Table 2: Satisfaction of students with rural community posting
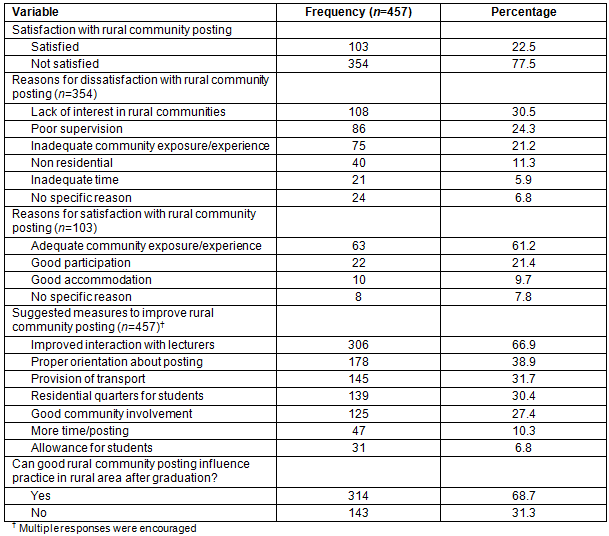
Table 3: Factors affecting satisfaction of students with rural community posting
Discussion
A minor proportion of the students (22.5%) were satisfied with their rural community posting. This is not encouraging, bearing in mind the long history of the program and also the recent call that this posting should be student oriented13. It may be an indication that the institutions may have lost touch with the values that informed the initiation of the rural community program. This is further supported by the fact that there has been no formal evaluation of this program since its commencement, either at the institutional or national level. This result is at variance with that from a similar study from South Africa where 81% of the students who participated in the study rated their experiences with rural medical education as above average21.
The major reason for dissatisfaction with rural community posting among the students was lack of interest in rural areas. This same reason was found to be the major reason why medical students were unwilling to practise in rural areas after graduation13. These responses by the students are not surprising since the majority of them live with their families in urban settings and they also had their secondary education in urban areas. This, however, should renew the focus on the relevance of rural community postings. This is because the posting has been viewed as an intervention at the medical curriculum level to reverse the negative attitude of medical students to life in rural communities and practise in rural area after graduation13,22 , hence the conclusion that community-based medical education produces health workers that are better prepared for community service delivery6-8. The emphasis on rural medical practice is justified as the majority of Nigerians reside in rural areas14, and the health indices are poorer than those of urban areas16. The National Universities Commission also had this concept in mind while including rural community postings in the curriculum of medical students in Nigeria12.
The other reasons given by the students for their dissatisfaction with their rural community posting present a poor assessment scorecard for the program by the students. Reasons such as poor supervision, inadequate community experience and lack of residential quarters for the students are indications that the conduct of the rural community program in the various medical schools is not in line with the objectives guiding its establishment. The reasons are interrelated: a rural community posting that is non-residential and one in which supervision is adjudged to be poor cannot provide students with the expected community exposures during the period of posting. Also, the absence of residential quarters for the students during rural community posting runs counter to the good plans of the National Universities Commission for the posting.
The suggestions by the students on how to improve rural community postings are very interesting and should be adopted by the managers of the program in all the medical schools in Nigeria. Apart from the suggestion that monetary allowances be paid to the students for their participation in the posting, the suggestions indicate that the students may be aware of the need and relevance of the rural community posting in today's medical curriculum. Suggestions such as provision of residential quarters for the students, provision of transport and improved student lecturer interactions are a strong basis for improved funding and staffing by the management of the various medical schools. Likewise, on the part of the medical tutors it is a call on the insistence on minimum standards, especially as stipulated by the National Universities Commission, better supervision of the students as well as a proper orientation of the students on the relevance and expectations from the rural community posting. The posting period could also serve as an opportunity for innovative community learning processes like field trips, community outreach and involvement in community assessments.
Most students were of the opinion that a good rural community posting could positively influence students to practise in a rural area after graduation. Perhaps the students focused on their various suggestions in coming to this conclusion. A study in Malaysia also revealed that exposing medical students to field works in rural areas during public health postings is capable of influencing the willingness of the students to work in rural areas after graduation22. From a study in Nepal came the suggestion about the need for repeated rural exposures and postings in rural hospitals for medical students18. This was based on the observation by the students that their existing medical curriculum does not adequately prepare them for rural medical practice.
Based on the logistic regression results, the students in federal universities were about half as likely to be satisfied with rural community posting than were students in the various state universities. This may be a reflection of the different approaches the various medical schools have adopted in pursuit of the rural community posting. The male students were twice as likely to be satisfied with their rural community posting than were female students. This could be expected based on the fact that the rural community posting may require certain adjustments by the students since most of them have urban backgrounds. It could be that the male medical students adjusted better and faster than their female counterparts hence were more satisfied with their rural community posting.
The students who intended to specialize in community medicine/public health after graduation were about three times more likely to be satisfied with their rural community posting than were other students who did not have that intention. It has been found that students who had in mind to specialize in community medicine were more willing to practise in rural areas after graduation13. In the postgraduate medical training for community medicine/public health in Nigeria, the rural community posting has a very strong placement. It could be that the students were aware of this and were already becoming prepared for the task ahead. Satisfaction with rural community postings could be seen as promoting interest in community medicine and also the willingness of medical students to practise in rural areas after graduation13 , hence the need to strengthen the program. This could be done by looking into the suggestions by the students on how to improve the posting.
Most of the students in this study were dissatisfied with their rural community posting, and the major reason for dissatisfaction was lack of interest in rural communities. A properly organized rural community posting is capable of changing the negative attitudes of students towards life and medical practice in the rural area. Adequate orientation of the students on the relevance of the posting, good community exposure and enhanced student lecturer interactions during the posting period could ensure satisfaction of the students. There should be a targeted evaluation of the rural community posting at the various medical schools in the country with the aim of strengthening and modifying the posting where necessary so as to ensure its purpose is realized.
Limitations
There was the possibility of a recall bias on the part of the students; this is often the case in any study that involves memory recall on the part of respondents. Also, institutional variability could affect the perception of the students of the rural community posting. The different medical schools conduct their rural community posting at similar stages of the training but under different conditions and arrangements that may affect the judgement of the students. Finally, use of cross-sectional design for the study and the nature of the research question may be limited in exploring the underlying complexities of a concept like satisfaction. The inclusion of a qualitative research method could have complemented the results of this study.
References
1. Ogunlesi TO. The basic philosophy and founding objectives. In: ABO Oyediran, Brieger WR (Eds). 25 years of The Ibarakpa Community Health Programme. Ibadan: African Press Limited, 1989.
2. Asojo OA, Asuzu MC, Adebiyi AO. Ibarakpa programme: half a century of rural health service, training and international co-operation in Nigeria. PLoS Neglected Tropical Disease 2014; 8(10): e3201.
3. World Health Organization. Declaration of Alma-Ata. International Conference on Primary Health Care, Alma-Ata, USSR, 6-12 September 1978.
4. World Health Organization. Community based education of health personnel. Report of a WHO study group. World Health Organization Technical report series746. Geneva: WHO, 1987.
5. Ezzat E. Role of the community in contemporary health professions education. Medical Education 1995; 29: 44-52.
6. Magzoub ME, Schmidt HG. A taxonomy of community based medical education. Academic Medicine 2000; 75: 699-707.
7. Habbick BF, Leeder SR. Orientating medical education to community need: a review. Medical Education 1996; 30: 163-171.
8. Murray E, Modell M. Community based teaching: the challenges. Journal of General Practice 1999; 49: 395-398.
9. Isaac V, Watts L, Forster L, McLachlan CS. The influence of rural clinical school experiences on medical students' levels of interest in rural careers. Human Resources for Health 2014; 12: 48.
10. Longombe AO. Medical schools in rural areas -necessity or aberration? Rural and Remote Health (Internet) 2009; 9: 11-31. Available: www.rrh.org.au (Accessed 19 September 2015).
11. Khan AR. Public health posting as a motivating factor for medical students to work in rural areas upon graduation. Journal of Education and Practice 2012; 3(8): 233-238.
12. National Universities Commission. Benchmark minimum academic standards for undergraduate programmes in Nigerian Universities: Medicine and Dentistry. Abuja: National Universities Commission, 2007.
13. Ossai EN, Anyanwagu UC, Azuogu BN, Uwakwe KA, Ekeke N Ibiok NC. Perception about working in rural area after graduation and associated factors: a study among final year medical students in medical schools in Southeast Nigeria. British Journal of Medicine and Medical Research 2015; 8(2): 192-205.
14. World Bank. Rural population (% of total population) data. (Internet). Available: http://data.worldbank.org/indicator/SP.RUR.TOTL.ZS (Accessed 9 February 2016).
15. Ebuehi OM, Campbell PC. Attraction and retention of qualified health workers to rural areas in Nigeria: a case study of four LGAs in Ogun state, Nigeria. Rural and Remote Health (Internet) 2011; 11: 1515. Available: www.rrh.org.au (Accessed 7 October 2015).
16. National Population Commission (Nigeria) and ORC Macro. National Demographic and Health Survey 2013. Maryland: National Population Commission and ORC Macro, 2014.
17. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention. Global policy recommendations. Geneva: WHO, 2010.
18. Shankar PR, Thapa TP. Student perception about working in rural Nepal after graduation: a study among first and second year medical students. Human Resources for Health 2012; 10: 27-35.
19. Federal Republic of Nigeria. 2007. Official gazette. Lagos: Federal Republic of Nigeria, 2007.
20. Federal Republic of Nigeria. National Bureau of Statistics. Annual abstract of statistics. Abuja: Federal Republic of Nigeria, 2010.
21. Mateen FJ. Future practice location and satisfaction with rural medical education: Survey of medical students. Canadian Family Physician 2006; 52: 1106-1107.
22. Khan AR. Public health posting as a motivating factor for medical students to work in rural areas after graduation. Journal of Education and Practice 2012; 3(8): 233-239.




