Introduction
The Irukandji syndrome is a constellation of diverse symptoms and signs, which follow a sting from small carybdeid jellyfish1,2. Although other carybdeids are suspected, only Carukia barnesi is currently definitively associated with the syndrome3-5. Irukandji syndrome has been described around the northern Australian coastline from Rockhampton, Queensland in the east, to Broome, Western Australia in the west (Fig 1). Most of this area is classified as remote in terms of the Australian Bureau of Statistics standard geographic classification of remoteness: the Accessibility/Remoteness Index of Australia (ARIA)6.
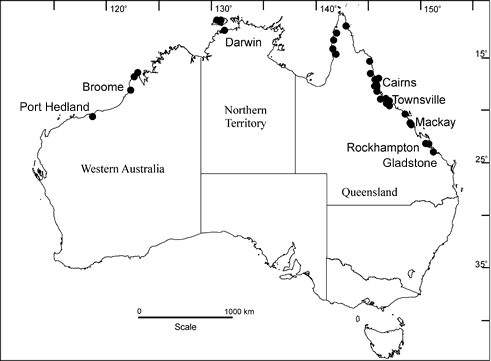
Figure 1: Location of 34 surveyed institutions in northern Australia
Common symptoms include severe pain, particularly in the chest, abdomen, lower back and limbs, and those suggestive of catecholamine excess, including sweating, anxiety, tachycardia and hypertension4,7. The recent death of two sting victims8 and documented pulmonary oedema in 11 other cases6 has highlighted the need for optimal first aid and hospital management in all cases of suspected Irukandji syndrome. However, there remains some disagreement over optimal approaches to care5,9-11, and there are currently no Australian national guidelines for medical management of Irukandji syndrome.
We conducted a telephone survey of coastal medical centres covering the geographical limit of the Australian Irukandji range to investigate current Irukandji patient management approaches and the existence of local guidelines.
Methods
Setting
During November and December 2003, a telephone survey was conducted of coastal hospitals and health centres responsible for the primary management of Irukandji syndrome patients from Gladstone in Queensland to Port Hedland in Western Australia. A total of 34 institutions were identified for contact following communication with the relevant District Health Managers. Some District Managers specified which institutions could be contacted, and one District Manager did not respond to requests for permission to contact institutions under his jurisdiction. Coastal health facilities were selected on the assumption that an Irukandji sting patient would seek help from the nearest health facility.
Interview participants were recruited by telephoning the identified institutions and asking to speak to the health professional who would be responsible for the primary management of a patient with suspected marine stinger envenoming on the survey day. Participation was voluntary, and respondents were assured of personal and institutional confidentiality.
All institutions contacted agreed to participate in the survey and provided answers to a structured questionnaire that was telephonically administered. To ensure optimal consistency, all interviews were performed by a single investigator (FB).
Interview
Participants were provided with a vignette relating to Irukandji syndrome and asked to describe their institution's approach to management:
A 24 year old male was swimming in the ocean when he became aware of a mild stinging sensation in his right arm, but continued swimming. Thirty minutes later he developed severe back, abdominal and chest pain, and became agitated. He has been brought to see you by his family. Please describe your assessment and management of this patient.
The participant's initial spontaneous description of clinical management was documented. This was followed with general prompts:
- Is there anything else which you would observe, assess or monitor?
- Is there any other management which you would undertake?
Thereafter, the respondent was asked to provide the institution's usual response to the following additional questions:
- What aspects of management would change if the patient was a 5 year-old child?
- What would be the frequency of observations?
- What first-aid measures are considered by your institution?
- What would be the usual approach to managing a blood pressure >180/110 mmHg in such a patient at your institution?
- What would be the approach to managing unresolved pain at your institution?
- What are the discharge criteria for a stinger patient at your institution?
- If the patient is admitted - to where?
Respondents were asked whether or not their institution had printed protocols or guidelines for marine envenoming. Where guidelines were not available, respondents were asked whether printed guidelines would be useful.
Analysis
Data were captured and analysed using SPSS v.11.0 for Windows (SPPS Inc; Chicago, IL, USA). After the usual data cleaning processes, standard statistics were used for univariate descriptives. Bivariate comparisons of proportions were tested by means of exact versions of c2 tests. Confidence intervals were calculated using exact binomial distributions. For analysis, the health institutions were classified according to their proximity to larger towns because this has relevance to patient referral using the following categories: location within a town with a population greater than 50 000; sited within 50 km of these larger towns; more distant than 50 km from these larger towns; or location on an island.
Ethics
Approval for the study was obtained from the human research ethics committee of James Cook University (Ethics Approval no. H1577), and each District Manager responsible for institutions contacted.
Results
All 34 institutions (25 hospitals and 9 health centres) identified and contacted participated. Of these, 24 were located in Queensland, 4 in Northern Territory and 6 in Western Australia (Fig 1). Five were located in towns with a population greater than 50 000 (Cairns, Townsville, Mackay, Rockhampton and Darwin). Four were within 50 km of these towns, while 20 were more distant and five were on islands. Twenty-five doctors and nine nurses were primarily responsible for management of a suspected Irukandji patient on the day of contact, with doctors responsible at 23 of the hospitals and 2 of the health centres. All nine nurses were located in facilities greater than 50 km from a large town or on an island. All health centres were more than 50 km from a large town or on an island.
Twenty-two of the facilities contacted (65%) reported having guidelines for Irukandji syndrome management. Of facilities with guidelines, eight (36%) used the Primary Clinical Care Manual (PCCM); six (27%) the Central Australian Rural Practitioners Association Standard Treatment Manual (CARPA STM), and the remainder independently produced protocols. All major centres, three centres <50 km away (75%), 11 centres >50 km away (55%), and three island centres (60%) had guidelines. All Northern Territory respondents had guidelines.
All respondents reported that pulse and blood pressure would be routinely measured for every patient with suspected Irukandji syndrome, 32 (94%) routinely recorded respiratory rate and 30 (88%) oxygen saturations. Ten (29%) facilities would perform continuous cardiac monitoring, while 30 (88%) recorded routine observations at least every 15 min. There was no significant difference in frequency of observations with increasing rurality.
Vinegar as a first aid measure was not mentioned by all respondents (Table 1). The spontaneous mention of vinegar was significantly associated with increasing remoteness, p = 0.023 (Table 2). Two respondents (6%) reported that their centre would apply a pressure bandage, three (9%) indicated that this would not occur at their centre, four (12%) would use heat and six (18%) would apply ice to the sting site. One respondent reported not knowing what first aid should be administered. A summary of common management measures reported is presented (Table 3).
Table 1: Use of vinegar as a first aid measure for suspected Irukandji syndrome
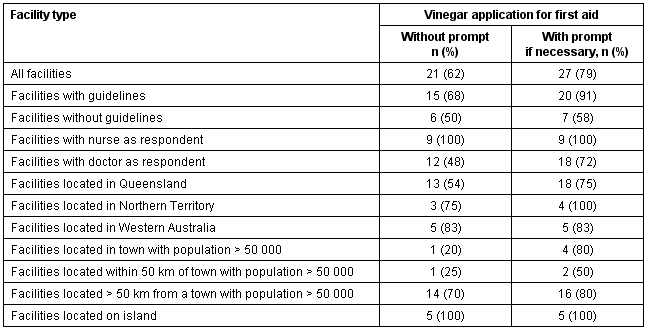
Table 2: Association of spontaneous mention of vinegar as a first aid measure with increasing remoteness
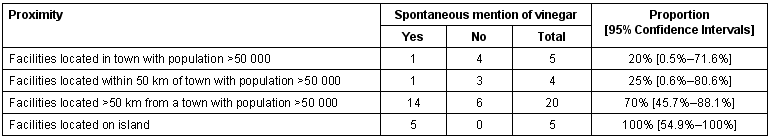
Table 3: Standard management measures in Irukandji syndrome by facility type and profession of respondent
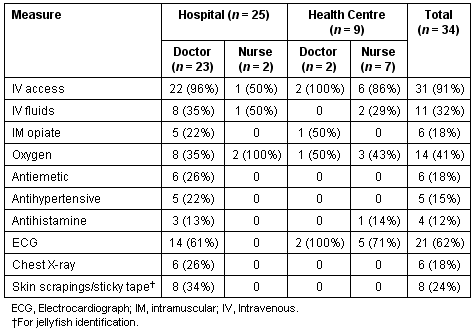
Blood tests were infrequently used, with full blood counts being most commonly performed (n = 14, 41%) and 13 respondents (38%) indicating that they did not have access to blood testing facilities. All respondents who did not have access to these services were located outside the larger urban centres.
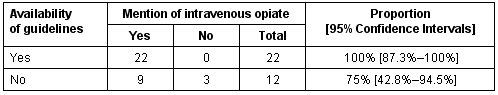
Intravenous opiate analgesia use was mentioned by all respondents in Western Australia and Northern Territory, and 21 (87.5%) in Queensland. All facilities with guidelines would administer intravenous opiate analgesia, compared with nine facilities (75%) without guidelines, p = 0.037 (Table 4). With unresolved pain, 19 respondents (56%) would administer more of the initial opiate, six would use an opiate infusion (18%), four would try a different opiate (12%) and two would attempt a different drug (6%). All nurses and five doctors indicated that they would consult an experienced medical officer. Administration of intravenous magnesium was mentioned by four respondents (12%). There was no significant difference in pain management with increasing rurality.
Table 4: Association of guideline availability with intravenous opiate analgesia use
When asked to describe their health facility's usual response to managing a blood pressure >180/110 mmHg in an Irukandji patient, 18 respondents (53%) indicated that further analgesia would be administered, while five would observe the patient (15%) and 12 (nine nurses and three doctors) would seek advice from an experienced medical officer. Other treatments mentioned included magnesium (n = 7, 21%), glyceryl trinitrate (GTN) (n = 4, 12%), hydralazine (n = 4, 12%), beta blockers (n = 2, 6%), labetalol (n = 2, 6%) and nifedipine (n = 3, 9%). Frusemide, diazoxide, nitroprusside, phentolamine and atenolol, midazolam, oxygen and reassurance were each mentioned by a single respondent.
Twelve respondents (35%) indicated that their facility would not alter management for a child, while six would transfer the child sooner (18%) and eight (24%) would adjust medication dosages.
If a patient required admission, 13 respondents (38%) would transfer the patient to another facility, including three Northern Territory (75%), three Western Australian (50%) and seven Queensland (29%) facilities.
Prior to discharge, 16 institutions (47%) required that the patient be pain free, 5 (15%) that pain be controlled, 17 (50%) that symptoms have abated, 15 (44%) that observations be stable, 4 (12%) that clinical examination be normal, 5 (15%) that blood results be normal, and 3 (9%) that the electrocardiograph be normal. The period of patient observation (in hours, where stated) varied: 2 (n = 1, 3%), 3 (n = 1, 3%), 4 (n = 3, 9%), 6 (n = 8, 24%), 12 (n = 2, 6%) or 24 (n = 2, 6%).
Discussion
Telephone surveys using vignettes are valuable tools for obtaining information from doctors and other health workers in a non-threatening manner12 and have been used in a variety of situations13-15. The current survey was well received by respondents, with 100% participation and 91% of respondents indicated that they would like to receive a copy of the study report.
There were few statistically significant differences in the management of suspected Irukandji syndrome patients between urban and remote facilities, despite the staffing and equipment constraints at many rural facilities. Despite this reassuring finding, remote facilities were less likely then larger facilities to have guidelines. This is important because many of these facilities are very isolated and have only telephone contact with large facilities, and the support of the Royal Flying Doctor Service to evacuate patients where necessary. All respondents were aware of the point of contact and assistance appropriate for their location and situation. Availability of guidelines may be of increased importance in a remote setting, particularly if telephone advice is not available or is delayed.
Most respondents described appropriate assessment and pain management of a patient with Irukandji syndrome, but marked variation in management of sting site and hypertension was found. These differences were not related to remoteness, other than the increased spontaneous mention of vinegar noted with increasing remoteness. It is of concern that health staff who may encounter patients with Irukandji syndrome are not aware of the use of vinegar as first aid management (21%), and do not have guidelines to assist them in patient management (35%). This may be compounded by the documented rapid turnover of staff in rural Australian health facilities16,17. Although not specifically investigated in this survey, seven respondents spontaneously volunteered that they had been in their current location for less than 1 year. As some respondents, particularly doctors, were not of Australian origin, their knowledge of Australian tropical health conditions cannot be assumed. It is important that the management of marine stingers, including those causing Irukandji syndrome, be brought to the attention of all new staff arriving in areas where exposures may occur. Ten of the eleven respondents who indicated no prior experience of managing Irukandji syndrome were located in centres >50 km away from the major towns or on an island. Five of the six doctors who had no experience of treating a patient with Irukandji syndrome either did not have guidelines or were uncertain whether or not guidelines were available.
Vinegar application to the Irukandji sting site is considered good practice but was not universally practiced by participating institutions. It was mentioned spontaneously in a significantly higher number of remote than urban facilities, and by all nurses. Pressure bandaging was still used at two institutions although its use is controversial and recent evidence suggests that it may be dangerous11,18-20.
Generally, assessment of Irukandji patients was good, both in urban and remote settings, with most respondents describing an adequate physical examination and routine observations. The frequency of observations was appropriate in most cases, particularly when remote practice constraints are considered. One participant indicated that it was not possible to perform observations more frequently than every 15 min, because every aspect of patient assessment and management had to be manually performed by the only health professional in the particular facility.
Management of the severe pain associated with Irukandji syndrome was appropriate, with the majority of respondents in both urban and rural locations identifying the need for intravenous opiate analgesia, and often for repeated doses or an infusion. Management of elevated blood pressure associated with Irukandji syndrome was less uniform. Over half of the respondents correctly indicated that further analgesia might be required, but a number of additional pharmacological approaches were suggested to lower blood pressure. Magnesium was suggested by 21% of respondents, probably reflecting recent reported utility of intravenous magnesium sulphate in the management of pain and hypertension associated with Irukandji syndrome21. A variety of other pharmacological treatments were mentioned. The isolated use of beta blockers is of concern given a previous association between beta blocker use and circulatory collapse with acute renal failure22. Phentolamine has been used traditionally, in view of its alpha blocking effect9, but intravenous GTN has been suggested due to greater familiarity, availability, and ease of titration5. Sublingual GTN has been used in the pre-hospital management of hypertension associated with Irukandji syndrome but the appropriateness of this approach has not yet been proven23. A standardised approach to hypertension management in Irukandji syndrome is lacking, and studies to identify the most appropriate antihypertensive agent are clearly indicated.
The usefulness of guidelines is evident from the increased use of intravenous opiate analgesia by facilities with guidelines. All respondents without guidelines at their facility indicated that having guidelines would be useful. Improving knowledge of and access to manuals such as the PCCM or CARPA STM may improve the management of Irukandji syndrome. Use of appropriate antihypertensive agents, magnesium's role in Irukandji syndrome management and the use of pressure immobilisation bandaging should also be addressed in updated guidelines.
Conclusion
Irukandji syndrome belongs to the category of potentially life-threatening envenomings that occur predominantly in tropical environments24,25. All envenomings in this group demand optimal clinical management without delay in all affected patients. Unfortunately, many of these envenomings occur in remote locations where immediate access to specialised health facilities and care may be limited. Thus, it is essential that patient management at the first point of care is standardised and adheres to best available evidence. Our survey has highlighted first-aid and patient management deficiencies among health professionals responsible for treating patients with Irukandji syndrome in northern Australia. Consistent guidelines and education of new staff are essential if optimal management of Irukandji syndrome is to be assured.
Acknowledgement
This survey was funded by a grant from the School of Public Health and Tropical Medicine, James Cook University, Townsville.
References
1. Flecker H. Irukandji sting to North Queensland bathers without production of weals but with severe general symptoms. Medical Journal of Australia 1952; 2: 89-91.
2. Barnes JH. Cause and effect in Irukandji stingings. Medical Journal of Australia 1964; 1: 897 904.
3. Southcott RV. Revision of some Carybdeidae (Scyphozoa: Cubomedusae), including a description of the jellyfish responsible for the "Irukandji syndrome". Australian Journal of Zoology 1967; 15: 651-671.
4. Huynh TT, Seymour J, Pereira P et al. Severity of Irukandji syndrome and nematocyst identification from skin scrapings. Medical Journal of Australia 2003; 78: 38-41.
5. Little M, Pereira P, Mulcahy R, Cullen P, Carrette T, Seymour J. Severe cardiac failure associated with presumed jellyfish sting. Irukandji Syndrome? Anaesthesia and Intensive Care 2003; 31: 642-647.
6. Commonwealth Department of Health and Aged Care. Measuring remoteness: accessibility/remoteness index of Australia (ARIA) (Revised edition). Occasional papers: New Series Number 14. Canberra, ACT: CDHAC, 2001.
7. Burnett JW, Weinrich D, Williamson JA, Fenner PJ, Lutz LL, Bloom DA. Autonomic neurotoxicity of jellyfish and marine animal venoms. Clinical Autonomic Research 1998; 8: 125-130.
8. Fenner PJ, Hadok JC. Fatal envenomation by jellyfish causing Irukandji syndrome. Medical Journal of Australia 2002; 77: 362-363.
9. Fenner PJ, Williamson J, Callanan VI, Audley I. Further understanding of, and a new treatment for, "Irukandji" (Carukia Barnesi)stings. Medical Journal of Australia 1986; 45: 569-574.
10. Martin JC, Audley I. Cardiac failure following Irukandji envenomation. Medical Journal of Australia 1990; 53: 164-166.
11. Bailey PM, Little M, Jelinek GA, Wilce JA. Jellyfish envenoming syndromes: unknown toxic mechanisms and unproven therapies. Medical Journal of Australia 2003; 78: 34-37.
12. Finch J. The Vignette technique in survey research. Sociology 1987; 21: 105-114.
13. Durrheim DN, Thomas J. General practice awareness of notifiable infectious diseases. Public Health 1994; 10: 273-278.
14. Durrheim DN, Duse A, Kloeck PE. Managing dog bite in Mpumalanga Province, South Africa - the Vignette approach, a useful tool for assessing knowledge and practice. Southern African Journal of Epidemiology and Infection 1998; 13: 86-89.
15. Durrheim DN, Speare R, Petzer M. Rabies post-exposure management in South Africa: a telephonic survey used as a rapid tool for operational research. Tropical Medicine and International Health 2002; 7: 459-461.
16. Kamien M. Staying in or leaving rural practice: 1996 outcomes of rural doctors' 1986 intentions. Medical Journal of Australia 1998; 69: 318-321.
17. Queensland Health Ministerial Taskforce. Nursing Recruitment and Retention. Summary of final report. Brisbane, QLD: Queensland Health, 1999.
18. Pereira PL, Carrette T, Cullen P, Mulcahy RF, Little M, Seymour J. Pressure immobilisation bandages in first-aid treatment of jellyfish envenomation: current recommendations reconsidered. Medical Journal of Australia 2000; 73: 650-652.
19. Fenner PJ, Williamson JA, Burnett J. Pressure immobilization bandages in first-aid treatment of jellyfish envenomation: current recommendations reconsidered. Medical Journal of Australia 2001; 74: 665-666.
20. Little M. Is there a role for the use of pressure immobilization bandages in the treatment of jellyfish envenomation in Australia? Emergency Medicine 2002; 14: 171-174.
21. Corkeron MA. Magnesium infusion to treat Irukandji syndrome. Medical Journal of Australia 2003; 78: 411.
22. Fenner PJ, Williamson JA, Burnett JW. Clinical aspects of envenoming by marine animals. Envenomings and their treatments. Proceedings, First International Congress, Institut Pasteur, Paris 7-9 June 1995. Lyon: Fondation Marcel Merieux, 1995.
23. Fenner PJ, Lewin M. Sublingual glyceryl trinitrate as prehospital treatment for hypertension in Irukandji syndrome. Medical Journal of Australia 2003; 79: 655.
24. Cheng AC, Currie BJ. Venomous snakebites worldwide with a focus on the Australia-Pacific region: current management and controversies. Journal of Intensive Care Medicine 2004; 19: 259-269.
25. Fenner PJ, Williamson JA. World-wide deaths and severe envenomation from jellyfish stings. Medical Journal of Australia 1996; 165: 658-661.



