Francophones in Canada who reside outside of Quebec continue to experience several health inequalities when compared to the anglophone population1-3; these are particularly pronounced in underserviced areas such as Northeastern Ontario4. Recent research has found that the potential supply of Ontario physicians who can conduct their practice in French is quite promising, with a French-speaking family physician to French-speaking population ratio (3.4/1000) that is nearly four times greater than the general physician to population ratio (0.9/1000)5. However, a maldistribution of French-speaking physicians has also been reported, with most located in urban communities of Southern Ontario, where smaller proportions of francophones reside6. Given the relatively large number of French-speaking physicians in the province, it is clear that numbers alone cannot account for these health inequalities. The present study seeks to understand barriers experienced by physicians serving francophone populations in Northeastern Ontario.
Interpersonal communication has been described as the primary tool by which health information is exchanged7. According to the Société Santé en français, the quality of health services depends largely on the ability to communicate in one's own language8. Linguistically concordant patient-physician interactions can lead to an improved sense of wellbeing, higher medication adherence, greater patient satisfaction and higher patient return rates9. Conversely, linguistic discordance has been found to obstruct medical comprehension10, lead to inappropriate or unnecessary testing11, increase the risk of adverse medication reactions10, and increase the likelihood of misdiagnosis and negative outcomes11. In essence, communication can contribute to both improved health and increased illness, thus it is essential to providing a quality healthcare service.
Many studies have explored the barriers that may arise when linguistic and/or cultural differences are present between physicians and patients. For instance, language barriers affect communication during medical encounters12, cause difficulties in describing symptoms and understanding instructions13 and lead to longer visits14,15. The use of interpreters, despite being a common solution to overcoming language barriers, has proven to be problematic, particularly when interpreters are recruited ad hoc (eg family members)16. Additionally, certain physician characteristics can be a barrier to providing appropriate care to linguistic and cultural minorities. For instance, suboptimal interpersonal skills may result in part from inadequate training of communication skills during medical education17. Also, due to the natural human tendency to categorize, physicians may subconsciously stereotype patients belonging to minority groups, thus influencing their expectations and attitudes when interpreting behaviors and making recommendations18,19.
Cultural differences have been found to be a key barrier to providing health care. Conflicting cultural values can result in patients inaccurately perceiving and reporting symptoms20 or refusing to follow health recommendations13. An unfamiliarity or insensitivity to cultural differences may negatively affect physicians' treatment decisions, influencing health outcomes and patient satisfaction19. However, research in this field often focuses on ethnic minority groups or recent immigrants being treated by physicians from the ethnic and/or linguistic majority group. Few studies have explored language barriers experienced by francophone minorities when receiving health care in an officially bilingual country. Furthermore, most studies of this nature in Ontario focus primarily on issues of access to and utilization of French-language services6,21. Nevertheless, Franco-Ontarians are unique from other cultural and linguistic minority groups in Canada, thus the barriers described above may not apply to this group.
At least three characteristics of Ontario francophones make these people unique. First, French is one of Canada's two official languages and is protected in Ontario under the French Language Service Act, which recognizes the 'right' to receive government services in French22. Therefore, it is reasonable for francophones to expect French-language services23, which may not be realistic for other minority groups. Second, unlike most ethnic minority groups, Franco-Ontarian culture is not vastly different from that of 'Anglo-Ontarian' providers. Although Franco-Ontarians maintain a unique identity, mainly through artistic expressions24, their minority situation and their fragmented and dispersed population across the province has led to assimilation into the dominant anglophone culture25. Thus, it is likely that many francophone patients and anglophone physicians share a similar Ontarian identity. As a result, it is unlikely that the cultural barriers described above would manifest themselves in the same way with Franco-Ontarians. Finally, as a direct result of assimilation, a gradual shift in language from French to English has been observed in recent generations of francophones, evident in the high rates of bilingualism and the prevalence of linguistically mixed marriages26. Therefore, many francophones can both understand and speak English, a skill that may not be as prevalent in other minority groups.
As such, it can reasonably be expected that the barriers experienced by Ontario francophones when receiving care, and the barriers physicians experience when providing care, will differ from those experienced by other minority groups. To the authors' knowledge, no other study has examined language barriers in rural and Northern Ontario, particularly not from the physician's perspective, an essential point of view if one wishes to understand and improve healthcare delivery in this region. The present article identifies perceived barriers to serving francophone populations experienced by Ontario physicians and explores differences between physicians who can and who cannot offer services in French.
Setting
Ontario is Canada's most populous province, constituting more than 38% of the Canadian population27. The northern part of the province, which has an area three times that of the south, is rather sparsely inhabited (constituting only 6% of Ontario's population) and home to numerous rural communities28. Ontario holds Canada's largest French population residing outside of Quebec29. Although francophones are a minority across the province, accounting for less than 5% of the population, they account for 23% of the population in the north-east30. Thus, the present study narrowed its focus to communities in Northeastern Ontario, as the need for French-language services is presumably greatest in these communities and physicians are likely to encounter barriers more frequently.
Participants
A series of key informant interviews were conducted with family physicians who had located their practice in rural and urban communities of Northeastern Ontario with large francophone populations6. Purposive sampling was used to identify physicians who had been in practice for 5-35 years and had been trained in Canada (to reduce differences arising from educational background). Both physicians who can and cannot practice in French (henceforth referred to as French and non-French-speaking physicians respectively) were interviewed, as it was estimated that each group would experience unique challenges as a result of differences in linguistic concordance10,11. Physicians who met the inclusion criteria were identified using the doctor search on the College of Physicians and Surgeons of Ontario website (http://www.cpso.on.ca/public-register/all-doctors-search). This sampling technique was supplemented with snowball sampling. At the end of each interview, physicians were asked to forward a recruitment email on behalf of the research team to colleagues who may be interested to participate in the study.
Data collection
Principles of grounded theory were applied throughout31. An open-ended semi-structured interview guide was initially developed and refined as interviews progressed and common barriers arose. Interview questions were generated with the assistance of expert consultants, two French-speaking physicians (authors NG and JP) with practices located in francophone communities. These physicians provided face validity and confirmed the appropriateness of the interview questions. Interviews lasted between 45 and 60 minutes and were conducted either in person or over the phone, depending on physician preferences and availability. Interviews were audio-recorded and an honorarium was provided to reimburse participants for their time.
Analysis
Interviews were analyzed using a thematic analysis process32. Recordings were transcribed verbatim and shared with interviewees, who were given the opportunity to review the content. A data collection-data analysis cycle was applied. Individual meaningful units of text were identified, coded, combined into themes and, using an iterative process of constant comparisons, further refined into categories. This process was repeated until saturation occurred. Although each interview produced unique examples of barriers, saturation was considered to have been achieved when no new types of barrier or theme arose33. The final themes and categories were contextually validated by the two physician authors. All quotes are presented in English; quotes stemming from a French interview have been translated and are denoted by an asterisk (*). Original French-language quotes are available upon request.
Identifier coding is as follows: RP, responding physician; E, English; F, female; Fr, French; M, male; R, rural; U, urban.
Researcher reflectivity
All researchers involved in the study consider themselves Franco-Ontarian and have experienced first-hand the inequalities surrounding access to linguistically appropriate health care, which undoubtedly influenced the way in which the interviews were conducted and results interpreted. However, this linguistic duality also offered a unique ability to conduct interviews in both official languages and to shift seamlessly from one language to another, giving interviewees the freedom to express themselves in their language of choice. Furthermore, the researchers' cultural heritage provided an understanding of both the colloquial expressions used and the historic meaning behind them, which would have been lost on a unilingual anglophone researcher. Because of the relatively small physician population in Northeastern Ontario, an interviewer occasionally had a prior acquaintance with an interviewee. When this occurred, the researcher in question would abstain from participating in the interview.
Ethics approval
Ethics approval was granted by the research ethics board of the lead authors' institution (Laurentian University - approval number 2012-05-02).
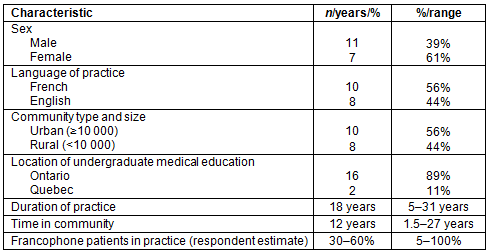
A total of 18 interviews were conducted, with physicians practicing in nine francophone communities across Northeastern Ontario (Table 1). Saturation was achieved after the 15th interview. Data collection was continued past saturation to ensure an adequate representation of rural and urban physicians as well as French-speaking and non-French-speaking physicians, which was achieved when saturation occurred within these subgroups.
Five categories of barrier were identified: (1) language discordance, (2) characteristics of francophone patients, (3) dominance of English in medicine, (4) lack of French-speaking medical personnel, and (5) physicians' linguistic (in)sensitivity. As expected, some barriers were unique to non-French-speaking physicians, some were unique to French-speaking physicians, and some were common to all physicians.
Table 1: Interviewee characteristics (n=18)
Language discordance
Language discordance, defined here as the inability to provide care in the patient's language of preference, was particularly problematic. Language barriers challenged physicians' confidence and led to increased time commitments, difficulties supplying written material, and a need for translators or interpreters. For many non-French-speaking physicians, patient visits take longer with francophones due to the need to continually translate and interpret the conversation and the use of time-consuming strategies such as speaking slowly and repeating information:
You just kind of say the same instruction several times through the visit, make sure, say ok 'what did I tell you to do now?' and then have him repeat it back to me so I knew he understood ...(RP18_E_F_U)
Though French-speaking physicians may not suffer from this language barrier, they did experience unique time commitments with French patients. For instance, referrals to a Non-French-speaking specialist often resulted in lengthy follow-up visits:
They will often go see Anglophone specialists, and it falls on me to reinterpret the letter for them, to re-explain what the specialist has told them and I'm happy to do that, there's no problem, but it slows down the flow of my office. (RP9_Fr_M_U*)
A lack of French written material was experienced by French and non-French-speaking physicians alike and ultimately became a barrier for their francophone patients, who may not receive linguistically appropriate literature. Some French-speaking physicians reported that much of their French literature was translated 'in-house' by their own staff. Despite efforts to offer French material, many non-French-speaking physicians added that 'there's no uptake' (RP8_E_M_U) on the French handouts they do have. One physician explained why so little French literature is handed out:
If I'm explaining something on the pamphlet, I usually grab the English one, I won't grab the French one because I don't understand what it says and how can I explain a pamphlet that's not in my language, so I usually will grab the English one and explain everything in English to the francophone person. (RP17_E_M_R)
As a result, these French patients are unlikely to ever request or receive French literature.
One barrier experienced exclusively by non-French-speaking physicians was the need for an interpreter or a translator during patient visits and how this may negatively impact the communication process. This concern became particularly problematic with ad hoc or inappropriate interpreters, such as family members:
It was just kind of awkward, especially for the woman, she had some female things she wanted to tell me about and it's hard for her to explain it to her husband and her husband has to tell me. (RP1_E_M_U)
Furthermore, the likelihood of misunderstandings occurring during translation was apparent in Northern Ontario where colloquial expressions or slang are used, and language is interspersed with both French and English words:
There's a lot of 'Frenglish', I guess if you want to call it that ..., mostly French and then throw in English words. There's a lot more slang living and working here, I noticed, compared to 20 years ago when I was at school in Ottawa and working in the hospital there as a medical student. People that lived down in that area, for example, speak much more; I hate to say it but, a proper French. As an English kid learning French in an English school system, I could understand them a lot easier than a lot of the people up here (in Northern Ontario) because they speak a lot of slangy kind of mixed up French, like words that you would never hear on Radio Canada or French CBC. (RP18_E_F_U)
Such language barriers left some physicians feeling intimidated and less confident in their abilities to serve French patients:
I don't feel my language skills are strong enough to pick up on little nuances so that's where I worry ... There are times where I think ['sigh'] I feel extremely inadequate. (RP5_E_F_U)
This lack of confidence was particularly pronounced in relation to psychological issues. Communicating with people who were elderly, who had dementia or who were very ill was particularly challenging:
... their ability to communicate in English is now being compromised because of health issues. (RP8_E_M_U)
When you're sick, you communicate with your mother tongue and you'll regress a little. (RP6_Fr_F_U*)
In essence, language, age and health status become a double or even a triple barrier. These language challenges formed a fear that vital information would be missed, and the quality of care impacted.
Some characteristics of francophone patients
Besides language, French patients were seen as possessing certain characteristics that were considered challenging. For instance, they tended to be older and less educated then average, many with lower levels of literacy. They were less likely to independently research their illnesses or take preventative measures and had more difficulty understanding and following instructions. They were more likely to exhibit unhealthy behaviors, such as smoking, consuming alcohol, eating a fatty diet and having a sedentary lifestyle. Additionally, physicians recognized that their French patients had more health problems, such as chronic illnesses, cardiovascular concerns, lung problems and cancers of various types. Their high-fat diet was associated with obesity and high cholesterol. As a whole, francophones were seen as possessing many characteristics that lead to complex comorbidities. Rural physicians added that distance to services was an issue and that many of their patients would refuse a consultation with a specialist if they had to travel.
Certain aspects of the Franco-Ontarian culture were also considered to be problematic. Francophones were seen as less likely to complain about their health and less willing to go in for checkups, particularly older men, who were seen as being too proud to admit that they do not understand their physician's instructions:
My (francophone) men they're just going (to say) 'yes, yes, I understand, go on ...'; they really don't want to look foolish and they will push you away. (RP14_Fr_F_U*)
Likewise, many physicians recognized that their French patients, men and women alike, would withhold information when speaking in English:
If ever I have a resident who is more anglophone, they will go in to take the history. When I will go in to confirm the history, then it will often grow quite a bit and they'll [the patients] tell me 'well I didn't know how to explain it in English so I didn't explain it'. (RP12_Fr_F_R*)
Such instances suggest that francophone patients may be more comfortable or may prefer to receive health services in French:
Often the people who have the option to speak both languages will speak more in French. (RP12_Fr_F_R*)
As a result, Non-French-speaking physicians may have more difficulty building a rapport with their French patients.
Interestingly, the notion that French-language services are always preferred was not supported. Some physicians explained that patients will spontaneously speak to them in English. This was particularly true when the physician had an English accent:
There are many people who could maybe offer a quasi-francophone/quasi-bilingual service... [However] if you're [the physician's] not able to speak [French] well, they're [the patients] going to switch to English pretty quickly... even if the doctor is ready to try to get by. So it prevents the doctor from having the opportunity to practice to eventually improve themselves. (RP4_Fr_M_U*)
This attitude becomes a barrier for both the non-French-speaking physicians, who are not given the opportunity to practice their French-language skills, as well as for the francophone patients, who are refusing a French-language service when one is available.
Various explanations for this English preference were suggested. Some believed that francophones have become accustomed to receiving health services in English and are thus more comfortable with English terminology, while others attribute the tendency to a lack of confidence. The perceived lack of physicians in Northern Ontario, particularly in rural communities, has instilled in patients a reluctance to insist for French service, fearing they may lose their physician if they are too demanding. Other physicians attribute this preference to an attitude that English medicine is of better quality:
Most people think that the language of medicine is English, and I've even heard that some francophone people would prefer to operate in English or see the English doctor because the presumption was that their education was better. (RP8_E_M_U)
Although the opinion that an English education is of greater quality is unfounded, the idea that English is the language of medicine can be argued.
English dominance in medicine
Most French-speaking physicians agreed that, in Ontario, the dominant medical language is English. Even those committed to offering French-language services have had to conform in part to this Anglo-dominant profession. For instance, all French-speaking physicians take their clinical notes in English, a necessity when making claims to insurance companies and to ensure proper continuity of care when patients are seen by anglophone colleagues. Furthermore, many physicians have developed a habit of switching to English for certain terms:
At the end of the day, the majority of my readings and the medical information I receive is in English. So when cases become more complex or something more complicated, often, if it's somebody bilingual, I'll change to English, just to make sure that I'm explaining myself appropriately, especially if the patient is looking for more technical information. (RP4_Fr_M_U*)
This tendency to use English terminology perpetuates the Anglo-dominance from both the physician and the patient's perspective. According to one physician, it is the provider's responsibility to not only offer services in French but also become an advocate for them and to build a French-language culture with their patients. However, most physicians agreed that, in Ontario, undergraduate medical training in French is scarce and there is limited availability for continuing education and professional development in French. Thus, advocating for French-language services is seldom at the forefront of their thoughts.
Lack of French-speaking medical personnel
Ontario's Anglo-dominant medical culture may contribute to another common barrier: the lack of French-speaking medical personnel. This need for French human resources was first experienced within the medical office, where the supply of qualified French-speaking staff (eg secretaries, nurses) is low. In the more rural communities, physicians have had to employ less experienced staff members with limited French skills:
So we've had to hire people you know that are new out of school and we've had to hire people that maybe weren't as strong in French as the previous ones we had, let's say, and so it takes a little time for them to catch up ... but that's because we can't find anybody. (RP2_E_F_R)
The need for French-speaking support staff is particularly acute for non-French-speaking physicians who rely on these individuals to help offer French-language services. Unfortunately, not all physicians have been able to recruit francophone staff. A similar gap was experienced in the supply of French-speaking specialists, particularly in rural and Northern Ontario, where fewer specialists are located:
We don't have the resources, or I feel like that's a luxury (sending a French patient to a French-speaking specialist), you know. There are not many, I can think of specialties where I'd be like 'Oh, I'll choose this one because they are French-speaking', and particularly because often your choice is around who can see them the quickest, so accessibility, urgency; who's on call that day. (RP13_E_F_U)
One of the biggest perceived barriers to serving francophones in Northern Ontario was the absolute lack of physicians. If hiring a physician is difficult in the north, recruiting one who can speak French has proven to be even more so:
We've been looking for a francophone physician for [community X] since I've been there. Never found one yet. (RP2_E_F_R)
The high demand for bilingual providers makes it difficult for smaller communities to compete with the bigger hospitals and urban centers:
It's very difficult to keep staff where we are [a rural community] ... and [medical personnel] get better benefits and better pay in the hospital system than they do in the [rural] community, so we've had a lot of trouble keeping them ... they don't want to work for less than the hospital's offering and the hospital's often looking for bilingual staff as well, so they steal them from us 'cause it's better pay. (RP2_E_F_R)
Adding to the shortage of French-speaking personnel is a lack of awareness of those French-language services that do exist. Many physicians expressed a need and a desire for a directory of such services:
I don't have anything that came to me that said these are the services for francophone people in the community. (RP5_E_F_U)
I've been pushing for a long time to have a good resource that tells us who are the francophone doctors...there's still a lack of identification of the francophone resources. (RP14_Fr_F_U*)
Linguistic (in)sensitivity
Despite good intentions, physicians exhibited some gaps in service. Although many agreed that linguistic sensitivity is important, certain non-French-speaking physicians assumed that French services were often unnecessary:
Most people are so bilingual anyway. I don't find language being a major problem. For me I don't speak any French practicing here, I don't really feel language being a major problem at all just because everyone is so bilingual. (RP17_E_M_R)
In fact, most non-French-speaking providers believe that less than 10% of their French patients require a French service. These physicians were less likely to report making extra efforts to refer francophone patients to French-speaking specialists.
Although French-speaking physicians reported making efforts to offer French-language services, they nevertheless held certain unfavorable beliefs. For instance, some thought that it was unnecessary to advertise themselves as French providers. One physician attributed this reluctance to the potential for a patient overload:
Family doctors of underserved areas quickly maximise their quantitative capacities. If you announce yourself as francophone ... you can have more people approaching you saying 'listen, my mother only speaks French, can you take her?'. (RP3_Fr_M_U*)
Furthermore, certain physicians believe they know their patients well enough to know their language of preference, thus impeding their continued active offer behaviors.
Discussion
The present study explored barriers to providing health care to rural and Northern Ontario's francophone population from the perspective of family physicians who can and who cannot speak French. Findings suggest that certain barriers outlined in previous studies of linguistic and cultural minority groups are also experienced with Ontario's francophones, the most common of which are likely the challenges surrounding the use of interpreters. Both the existing literature and present results suggest that untrained interpreters, although commonly used16,34, often lack the medical understanding and technical vocabulary to properly translate13, which can impede the disclosure of sensitive information35 and obstruct patient confidentiality13,36. In these instances, there is the potential that patients will withhold sensitive information from the interpreter (eg family member) and in turn from the physician12,35. Conversely, the interpreter may consciously withhold information or modify messages to 'protect' the patient37.
While other common barriers arose, these were often perceived and experienced differently by physicians in this study. For instance, language barriers are often associated with misdiagnoses, unnecessary procedures, and negative health outcomes10,11. Although physicians interviewed did not allude to such issues, language barriers nevertheless threatened their confidence as practitioners - they often feared that vital information would be lost in translation, particularly in relation to psychological disorders or ambiguous and idiosyncratic symptoms. Given that the challenges surrounding the use of interpreters and the insecurities caused by language discordance were predominantly experienced by non-French-speaking physicians, this study also supports the importance of language concordance7-9.
The present study reflects prior findings that suggest that patients with limited English abilities require longer visits14,15. Non-French-speaking physicians spent more time with francophone patients during appointments, due to the use of interpreters, and having to speak slowly and repeat themselves. Although French-speaking physicians may also spend added time during appointments, for instance explaining results following a visit with a non-French-speaking specialist, time commitments were more often experienced between appointments. French-speaking physicians were more likely to search for and translate written material, and to seek out French-speaking specialists when making referrals.
Many studies have described the dangers of cultural barriers, which arise when a physician is insensitive to the cultural particularities of their minority patients13 and/or relies on stereotypes and racial biases when making medical decisions18,19. Although physicians in the present study were culturally similar to their francophone clients, potentially harmful differences in physician and patient beliefs were nevertheless observed - for instance, the belief held by many non-French-speaking physicians that speaking French is unnecessary when serving Ontario francophones. In assuming that their patients are 'bilingual enough', these physicians fail to take the patients' linguistic abilities and preferences into consideration. As a result, both the patient and the physician may disregard important information due to an inability to properly express themselves38.
Some barriers appear to be unique to Ontario francophones. Shortages in the supply of French-speaking medical personnel, as well as a lack of French-language resources and educational opportunities, are examples of barriers that have not been previously observed. A possible explanation for such an absence in the literature may lie in the unique status that the French language holds as an official language in Canada. It is thus reasonable for francophones to expect to receive services in French23, an expectation that may not be realistic for linguistic minority groups whose mother tongue does not hold official language status, both in Canada and internationally. As a result, physicians in Ontario may feel an expectation to offer French services, thus any difficulty in accessing resources to do so would be perceived as a barrier that is unique to this group.
Additionally, francophone patients were perceived as possessing two competing preferences when receiving health care. While many physicians recognized a preference for French services in practice, describing how their patients are more expressive and seem to better understand instructions when given in French, francophone patients often indicated that they would rather receive their services in English. This tendency was also observed in a recent literature review that found that, when given the choice, francophones in Canada (excluding Quebec) chose to receive various services in English, even when the services are available in French39. According to this report, francophones are rather submissive, and choose to speak in English rather than demand French services39, a tendency also observed in the interviews of the present study and that has been attributed to a fear of losing their healthcare provider.
The present study outlines the importance of linguistic concordant communication in healthcare delivery, and describes some of the challenges faced when providing French-language services in rural and Northern Ontario. This qualitative study suggests that both French-speaking and non-French-speaking physicians experience barriers when serving francophone patients in rural and Northern Ontario, some of which are unique to the physicians' language of practice while others are common to all. Identifying such barriers is an important first step to providing support for providers who serve francophone clients, particularly in the rural north where the supply of French-speaking physicians is lowest6.
Healthcare providers serving this linguistic minority group and decision- and policy-makers may take interest in these results. Although physicians were the focus of the present article, the barriers expressed are likely experienced by other healthcare providers, and thus the lessons learned here extend beyond the physician workforce. For instance, the present findings can help build confidence, assuring novice and/or isolated providers of various types that such barriers are common in healthcare delivery, and providing a foundation to reflect on strategies for overcoming these barriers. The results have also identified areas where decision- and policy-makers could implement changes. For instance, although little can be done to improve the supply of French-speaking providers, a directory listing French-language services and providers could be created, regularly updated and shared. Many physicians expressed a desire for such a resource. Likewise, the need for linguistically appropriate written material was often expressed. Francophone health organizations and health planning entities could support physicians by providing such resources.
Efforts must also be made to offer educational opportunities for physicians who wish to improve their French-language skills and to ensure these opportunities are accessible to rural and northern providers. Medical education for learners and practicing physicians needs to include linguistic and cultural sensitivity training, in addition to strategies for the practice of 'active offer' of French-language services.
Acknowledgements
This work was funded by Health Canada (Consortium national de formation en santé-Secrétariat national and Laurentian University) and the Ontario Ministry of Health and Long-Term Care (Health System Research Fund). The views expressed in this manuscript do not necessarily reflect the position of the funding agencies. The authors thank Julie Sabourin, former research assistant at the Centre for Rural and Northern Health Research, for her contribution during the early stages of this project.
References
1. Batal M, Makvandi E, Imbeault P, Gagnon-Arpin I, Grenier J, Chomienne MH, et al. Comparison of dietary intake between Francophones and Anglophones in Canada: data from CCHS 2.2. Canadian Journal of Public Health 2013; 104(6): S31-S38.
2. Gagnon-Arpin I, Makvandi E, Imbeault P, Batal M, Bouchard L. Le surplus de poids chez les Francophones et les Anglophones. [The surplus weight among the Francophones and Anglophones] Canadian Journal of Public Health 2013; 104(6): S21-S25.
3. Imbeault P, Makvandi E, Batal M, Gagnon-Arpin I, Grenier J, Chomienne MH, et al. Physical inactivity among Francophones and Anglophones in Canada. Canadian Journal of Public Health 2013; 104(6): S26-S30.
4. Bouchard L, Batal M, Imbeault P, Gagnon-Arpin I, Makandi E, Sedigh G. La santé des Francophones de l'Ontario: un portrait régional tiré des Enquêtes sur la santé dans les collectivités canadiennes (ESCC). (Internet) 2012. Available: http://www.rrasfo.ca/images/docs/publications/2012/rapport_escc_ontario-final.pdf (Accessed 17 August 2014).
5. Gauthier AP, Timony PE, Wenghofer E. Examining the prevalence and distribution of French-speaking physicians in Ontario. Canadian Family Physician 2012; 58: 717-724.
6. Timony PE, Gauthier AP, Hogenbirk JC, Wenghofer E. Promising quantities, disappointing distribution. Investigating the presence of French-speaking physicians in Ontario's rural Francophone communities. Rural and Remote Health (Internet) 2013; 13: 2543. Available: www.rrh.org.au (Accessed 10 July 2014).
7. Ong LM, De Haes JC, Hoos AM, Lammes FB. Doctor-patient communication: a review of the literature. Social Science & Medicine 1995; 40(7): 903-918.
8. Société Santé en français. Santé en français, communautés en santé: Résumé des Plans directeurs 2008-2013. [Health in French, healthy communities: Summary of the 2008-2013 Master plans] (Internet) 2007. Available: http://franco.ca/ssf/documents/ResumePlan2008-2013.pdf (Accessed 10 July 2014).
9. Jacobs E, Chen AH, Karliner LS, Agger-Gupta N, Mutha S. The need for more research on language barriers in health care: a proposed research agenda. Milbank Quarterly 2006; 84(1): 111-133.
10. Wilson E, Chen AH, Grumbach K, Wang F, Fernandez A. Effects of limited English proficiency and physician language on health care comprehension. Journal of General Internal Medicine 2005; 20(9): 800-806.
11. Fortier JP, Strobel C, Aguilera E. Language barriers to health care: federal and state initiatives, 1990-1995. Journal of Health Care for the Poor and Underserved 1998; 9(5): S81-S100.
12. Woloshin S, Bickell NA, Schwartz LM, Gany F, Welch HG. Language barriers in medicine in the United States. Journal of the American Medical Association 1995; 273(9): 724-728.
13. Brach C, Fraserirector I. Can cultural competency reduce racial and ethnic health disparities? A review and conceptual model. Medical Care Research and Review 2000; 57(4 suppl): 181-217.
14. David RA, Rhee M. The impact of language as a barrier to effective health care in an underserved urban Hispanic community. Mount Sinai Journal of Medicine 1998; 65: 393-397.
15. Hampers LC, Cha S, Gutglass DJ, Binns HJ, Krug SE. Language barriers and resource utilization in a pediatric emergency department. Pediatrics 1999; 103(6): 1253-1256.
16. Papic O, Malak Z, Rosenberg E. Survey of family physicians' perspectives on management of immigrant patients: attitudes, barriers, strategies, and training needs. Patient Education and Counseling 2012; 86(2): 205-209.
17. Simpson M, Buckman R, Stewart M, Maguire P, Lipkin M, Novack D, et al. Doctor-patient communication: the Toronto consensus statement. British Medical Journal 1991; 303(6814): 1385-1387.
18. Cooper-Patrick L, Gallo JJ, Gonzales JJ, Vu HT, Powe NR, Nelson C, et al. Race, gender, and partnership in the patient-physician relationship. Journal of the American Medical Association 1999; 282(6): 583-589.
19. Perloff RM, Bonder B, Ray GB, Ray EB, Siminoff LA. Doctor-patient communication, cultural competence, and minority health: theoretical and empirical perspectives. American Behavioral Scientist 2006; 49(6): 835-852.
20. Poureslami I, Rootman I, Doyle-Waters M, Nimmon L, Fitzgerald JM. Health literacy, language, and ethnicity-related factors in newcomer asthma patients to Canada: a qualitative study. Journal of Immigrant and Minority Health 2011; 13(2): 315-322.
21. Bowen S. Language barriers in access to health care. (Internet) 2001. Available: http://www.hc-sc.gc.ca/hcs-sss/alt_formats/hpb-dgps/pdf/pubs/2001-lang-acces/2001-lang-acces-eng.pdf (Accessed 17 August 2014).
22. Government of Ontario. French Language Services Act. R.S.O. 1990, c. F. 32. (Internet) 2015. Available: http://www.ontario.ca/laws/statute/90f32 (Accessed 25 March 2014).
23. North East Local Health Integration Network. French language health services policy. (Internet) 2010. Available: http://www.nelhin.on.ca/Search.aspx?search=french%20language%20health%20services%20policy (Accessed 25 March 2014).
24. Thériault JY. Entre la nation et l'ethnie: sociologie, société et communautés minoritaires francophones. [Between nation and ethnic group: sociology, society and minority Francophone communities] Sociologie et sociétés 1994; 26(1): 15-32.
25. Cardinal L. Ruptures et fragmentations de l'identité francophone en milieu minoritaire; un bilan critique. [Breakdown and fragmentation of Francophone identity in a minority context; a critical appraisal] Sociologie et sociétés 1994; 26(1): 71-86.
26. Mougeon R, Beniak E. Bilingualism, language shift, and institutional support for French: the case of the Franco-Ontarians. International Journal of the Sociology of Language 1994; 105(1): 99-126.
27. Statistics Canada. Quarterly demographic estimates - January to March 2014. (Internet) 2014. Available: http://www.statcan.gc.ca/pub/91-002-x/91-002-x2014001-eng.pdf (Accessed 16 July 2014).
28. Ontario Ministry of Northern Development and Mines. Northern Ontario: a profile. (Internet) 2010. Available: http://s3.amazonaws.com/zanran_storage/www.mndm.gov.on.ca/ContentPages/2446172434.pdf (Accessed 16 July 2014).
29. Statistics Canada. Population by mother tongue and age groups (total), 2011 counts, for Canada, provinces and territories. (Internet) 2015. Available: http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/hlt-fst/lang/Pages/highlight.cfm?TabID=2&Lang=E&Asc=1&PRCode=01&OrderBy=999&View=1&tableID=401&queryID=1&Age=1 (Accessed 10 July 2014).
30. Office of Francophone Affairs. Profile of Ontario's Francophone community. (Internet) 2009. Available: http://www.ontario.ca/document/profile-ontarios-francophone-community-2009 (Accessed 16 July 2014).
31. Strauss A, Corbin J. Basics of qualitative research: techniques and procedures for developing grounded theory. 2nd edn. Thousand Oaks, CA: Sage, 1998.
32. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3(2): 77-101.
33. Guest G, Bunce A, Johnson L. How many interviews are enough? An experiment with data saturation and variability. Field Methods 2006; 18(1): 59-82.
34. Kale E, Syed HR. Language barriers and the use of interpreters in the public health services. A questionnaire-based survey. Patient Education and Counseling 2010; 81(2): 187-191.
35. Bauer A, Alegría M. Impact of patient language proficiency and interpreter service use on the quality of psychiatric care: a systematic review. Psychiatric Services 2010; 61(8): 765-773.
36. Timmins CL. The impact of language barriers on the health care of Latinos in the United States: a review of the literature and guidelines for practice. Journal of Midwifery & Women's Health 2002; 47(2): 80-96.
37. Brisset C, Leanza Y, Laforest K. Working with interpreters in health care: a systematic review and meta-ethnography of qualitative studies. Patient Education and Counseling 2013; 91(2): 131-140.
38. Ferguson WJ, Candib LM. Culture, language, and the doctor-patient relationship. Family Medicine and Community Health Publications and Presentations 2002; 34(5): 352-361.
39. Charbonneau F. Dans la langue officielle de son choix: la loi canadienne sur les langues officielles et la notion de 'choix' en matière de services publics. [In the official language of choice: The Canadian law on official languages and the notion of 'choice' in the realm of public services] Lien social et Politiques 2011; (66): 39-63.


