An important objective of an education in health care is to improve clinical competence and, hence, the confidence of the students. '"Competence" is conceptualized in terms of knowledge, abilities, skills and attitudes displayed in the context of a set of realistic professional tasks while "confidence" in oneself denotes the belief that one has the ability to do things well or deal with situations successfully'1. For providing an efficient oral health care for patients 'confidence' is considered as an important educational outcome2.
Several studies have shown increased confidence is associated with increased clinical competence, although the relationship between the two is not very well understood3. Medical literature states 'outreach programs' can be an effective alternative to promote an increase in confidence as well as competence level of the students, in addition to improving the effectiveness in implementation of preventive services in a community; such arrangements or programs are thus called outreach, extramural, or community-based experiences4-6.
The traditional model of dental undergraduate education does not encourage the holistic management approach that dentists need to adopt in general dental practice/the dental office, but may lead some students to consider patients as 'items of treatment' to be ticked off a list7.
Keeping this in mind, the curricula in various dental schools is currently changing and increasingly incorporating clinical experiences in primary care settings outside the four walls of the traditional dental school environment by employing the concept of outreach programs in urban or rural settings, with the aim of best preparing dental school graduates for eventual careers as independent dental practitioners2,6,8.
Thus, the outreach placements, in which students undertake supervised practice on consenting patients away from the dental hospital in primary care settings, have been said to enhance undergraduates' performance, and help them to develop their confidence and competence for later dental practice9. Recently, the Dental Council of India has directed the Creation of Setup of the Satellite Clinics in Remote Areas for Internship compulsory requirement according to the recent revised Bachelor of Dental Surgery Course (3rd Amendment) Regulations, 201110.
While these community-based outreach programs seem to address some of the perceived difficulties in contemporary dental school programs, it is important that these new programs should be fit for purpose. As confidence cannot be directly measured, students' self-reporting of perceived confidence is the most commonly employed measurement method2.
Although the literature contains ample anecdotal evidence from various medical program evaluations that hands-on outreach experiences do increase students' confidence in coping with clinical situations, hard data on outreach educational outcomes pertaining to dental education are still limited2. Hence, the present study was undertaken to assess the effectiveness of outreach placement on students' confidence and communication skills in providing treatment for patients and also to assess the perception of dental students regarding such outreach programs.
A non-randomized trial was conducted amongst 89 dental students who were pursuing internship program in three randomly selected dental colleges of Bangalore city in Karnataka State, India: M.R. Ambedkar Dental College and Hospital, V.S Dental College and Hospital, and M.S. Ramaiah Dental College and Hospital. The sample size was estimated based on earlier study6 using the Statistical Package for the Social Sciences v21 (SPSS Inc; http://www.spss.com), where α-error was at 5% and β-error at 20% (80% power for a two-sided test).
Permission was obtained from the principals of the selected dental colleges prior to the commencement of the study. Lists of interns were obtained from the respective dental colleges, which served as a sampling frame. The nature of the posting schedule in various departments of dental colleges in India is decided by the institutional office sections at commencement of internship, which precluded dedicating the process of selection to a fully randomized allocation schedule. Based on their posting schedule, the students were recruited to the outreach group (study group, n=44) and dental school based group (control group, n= 45) until the required sample size was achieved.
Inclusion criteria of the study were:
- students undergoing their internship program at the time of the study
- students who had been exposed to any of the outreach programs for at least 1 month and had undergone at least 3 months of their clinical dental school based postings (outreach group)
- students who had not been exposed to any of the outreach programs but had undergone at least 3 months of their clinical dental school based postings (dental school based group only).
The students in the outreach group had attended an outreach program such as postings to peripheral satellite centres, rural health training centres, rural camps, semi-urban and underserved community camps and other allied postings organized by the Department of Public Health Dentistry by various colleges, where the students were given the independence to make their own clinical decisions, treat patients independently, conduct certain oral health surveys and render health education to improve their communication skills. Concurrently, the students of the dental school based group continued only with their normal dental school based postings in various clinical departments.
A self-administered pre-tested, structured questionnaire in English was employed (Fig1). At baseline, students' clinical confidence and communication skills were assessed for matching both the groups using questions A and D, respectively: a global self-assessment with its five-point Likert-style scale ranging from 'not at all confident' to 'totally confident'. At follow-up after 3 months, students' clinical confidence and communication skills were measured using questions A and D for global self-assessment of clinical confidence and communication skills at that present time, questions B and E as a then-test for self-assessment of clinical confidence and communication skills before the posting, and questions C and F as transition judgements to assess the change from the past to the present level of clinical confidence and communication skills. Students' perceptions about the outreach program were also assessed, using question G, also on a five-point Likert-style scale. The outcome variables in each group were described using a simple descriptive measure of mean and standard deviation. Inferential statistics were then generated using statistical package SPSS v21 and outcome measures were compared between the groups using the t-test.
Ethics approval
Ethical clearance was obtained from M.R. Ambedkar Dental College and Hospital Ethical Committee Institutional Review Board (no. MRADCH/ECIRB/15/2/10) prior to the commencement of the study.
Mean age of the 89 eligible and consenting students was 24±0.5 years with male:female ratio of 1:1. The outreach group (study group) comprised 44 students, and 45 students were in the dental school based group (control group).
Table 1 shows the mean values of the students' clinical confidence and communication skills at baseline in order to match the study group and control group. The students in both outreach group and dental school based group were found to have similar levels of clinical confidence (4.02±0.21 vs 3.99±0.31) and communication skills (4.03±0.61 vs 3.98 ± 0.65) at baseline with no statistical difference between them.
Data were collected regarding the outreach program assessment with the help of the questionnaire (Fig1). The global assessment question for clinical confidence (question A) revealed that the outreach group's perceived confidence level in the present time was greater than that of the dental school based group (4.37±0.49 vs 4.04±0.21, p<0.001). When the outreach group retrospectively analysed their baseline clinical confidence with the help of the then-test (question B), their score was less than that of the dental school based group (3.42±0.75 vs 3.72±0.72, p<0.04) (Table 2). The outreach group's self-rating for increase in clinical confidence was significantly greater than that of the dental school based group for the transition judgement (question C; 4.24±0.91 vs 2.54±0.66, p<0.001) (Table 2).
The global assessment question for communication skills (question D) revealed that the outreach group's perceived level of communication skills in the present time was greater than that of the dental school based group (4.22±0.55 vs 4.02±0.51). When the outreach group retrospectively analysed their baseline confidence with the help of the then-test (question E), their baseline communication skills score was significantly less than that of the dental school based group (3.53±0.75 vs 3.81±0.62) (Table 3). The outreach group's self-rating for increase in communication skills was greater than that of the dental school based group for the transition judgement (question F) and was statistically significant (4.08±1.18 vs 2.56±0.62, p<0.001) (Table 3).
Both the outreach and dental school based group perceived that the outreach programs do help in improving the confidence level, communication skills and understanding ability of the students with insignificant statistical difference (4.35±0.77 vs 4.08±0.68, p=0.4972) (Table 4).
Table 1: Baseline measures of students' self-rated clinical confidence and communication skills
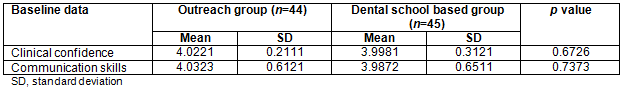
Table 2: Students' self-rating of change in clinical confidence: outreach group and dental school based group
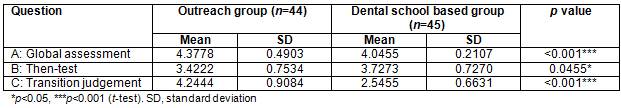
Table 3: Students' self-rating of change in communication skills: outreach group and dental school based group
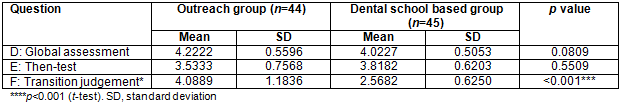
Table 4: Student perceptions of outreach program

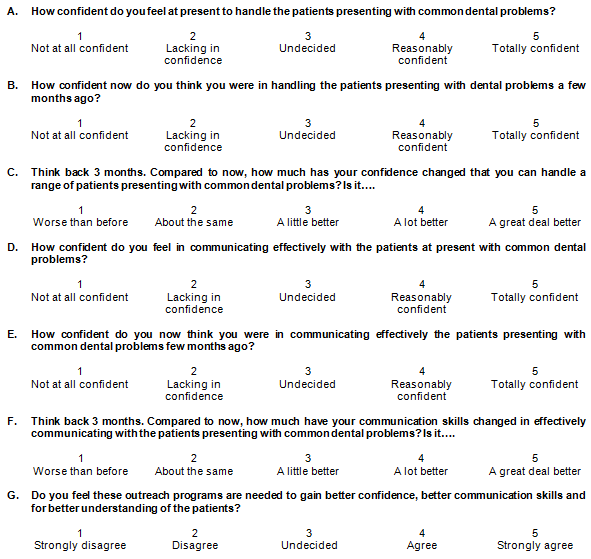
Figure 1: Outreach program assessment questionnaire.
Discussion
This trial was the first of its kind in the developing world for evaluating the effectiveness of ongoing dental outreach programs. As per the results, the present study emphasised the importance of the outreach experience in significantly helping dental students to increase their clinical confidence and communication skills.
The measurement of self-assessed change in clinical confidence and communication skills in the study was reflected by the alteration observed in their internal scales of clinical confidence and communication skills. Whilst this comparison revealed similar levels of scores between the groups, the then-test used to indicate past judgement revealed the outreach programs do encourage students to re-evaluate their internal confidence scales in relation to clinical confidence and communication skills.
Moreover, the then-test used indicated that the outreach group now believed they had been over-optimistic about their earlier confidence and level of communication skills. This newly gained insight is reflected by the difference in transition judgements between groups.
The probable reasons for such results for the outreach group are exposure to more patients (nearly a fourfold increase), fewer students per supervisor and a more intimate working environment with a small dental team.
Students in both the groups perceived that the outreach programs are a promising educational strategy to facilitate improvement in personal and professional development, which is in line with other studies as conducted in western countries by Mofidi et al9 and Hunter et al11.
Anecdotal reports from various countries state that such community outreach experiences aid in, for example, students' confidence level, competence, understanding of the patients' presenting problems, experience of new types of patients and their communities, access to alternative approaches and practicing in different settings, team working and a holistic and pragmatic view of health care4,8,11-16. But the literature pertaining to the effectiveness of dental outreach programs from developing countries like India is scant.
Outreach was equally or more important for students' confidence in clinical diagnosis, treatment planning, direct restorations, communicating with patients, and managing patients, time and resources, as reported by Eklind et al8.
Lennon et al12 revealed outreach programs had a large positive impact on developing clinical skills, better working in a busy practical environment and in developing interpersonal skills.
Smith et al6 conducted a randomized controlled trial and reported an increase in confidence level in students placed in an outreach group. A pilot version of the community outreach placements was conducted, and an increase in confidence level was attributed to repeated opportunities to reapply skills, appreciative comments from patients and, especially, support from both dental nurses and supervising dentists12,16.
Although the present study reinforces educational benefits, outreach programs are associated with increased costs to academic programs. Additional human and financial resources are required to carry out outreach programs. Further, despite core similarities, multi-faceted outreach facilitation interventions may vary in characteristics. Thus, these results should be viewed with care.
There may be limitations on generalizing these results to dental education programs operating in different ways across different places: the sample size was small so matching of various variables in both the groups might influence the study results. However, some features of this trial increase its validity: independent outreach locations and incorporation of the then-test and transition judgement to compare the actual shifts in students' internal scales of confidence level and communication skills of the students.
The present trial supports the concept of outreach program placements to be incorporated in the existing dental curricula in order to supplement the traditional school based dental education to achieve an overall professionally trained dentist.
Furthermore, the present study opens a new vista to explore which outreach program renders a maximum benefit in training the future dental graduates as well as providing an effective alternative method of healthcare delivery aimed at providing services to those who otherwise are not able to utilize the dental services.
References
1. Elzubeir MA, Rizka DE. Assessing confidence and competence of senior medical students in an obstetrics and gynaecology clerkship using an OSEC. Education Health 2001; 14(3): 373-382.
2. Lynch CD, Ash PJ, Chadwick BL, Hannigan A. Evaluation of a U.K. community-based clinical teaching/outreach program by former dental students two and five years after graduation. Journal of Dental Education 2010; 74(10): 1146-1152.
3. DeCastro JE, Mattheson PB, Panagakos FS, Stewart DC, Feldman CA. Alumni perspectives on community-based and traditional curricula. Journal of Dental Education 2003; 67(4): 418-426.
4. Hogg W, Lemelin J, Graham ID, Grimshaw J, Martin C, Moore L, et al. Improving prevention in primary care: evaluating the effectiveness of outreach facilitation. Family Practice 2008; 25: 40-48.
5. Morgan PF, Hogg DC. Comparison between medical students' experience, confidence and competence. Medical Education 2002; 36: 534-539.
6. Smith M, Lennon MA, Brook AL, Robinson PG. A randomized controlled trial of outreach placements' effect on dental students' clinical confidence. Journal of Dental Education 2006; 70(5): 566-570.
7. Lynch CD, Ash PJ, Chadwick BL, Hannigan A. Effect of community-based clinical teaching programs on student confidence: a view from the United Kingdom. Journal of Dental Education 2009; 74(5): 509-516.
8. Eklind A, Blinkhorn AS, Blinkhorn FA, Duxbury JT, Hull PS, Brunton PA. Developing dental education in primary care: the student perspective. British Dental Journal 2005; 198: 233-237.
9. Mofidi M, Strauss R, Pitner LL, Sandler ES. Dental students' reflections on their community-based experiences: the use of critical incidents. Journal Dental Education 2003; 67(5): 515-523.
10. Dental Council of India. Creation of setup of Satellite Clinics in Remote Areas for Internship compulsory requirement of the Dental Council of India revised Bachelor of Dental Surgery Course (3rd Amendment) regulations, 2011. No. DE-130-2012/B-6001. New Delhi: Dental Council of India, 2013.
11. Hunter LM, Oliver R, Lewis R. The effect of a community dental service outreach programme on the confidence of undergraduate students to treat children: a pilot study. European Journal of Dental Education 2007; 11(1): 10-13.
12. Lennon MA, Ireland RS, Tappin J, Ratcliffe PM, Taylor I, Turner R, et al. The personal dental service as a setting for an undergraduate clinical programme. British Dental Journal 2004; 196: 419-422.
13. Smith M, Lennon MA, Brook AH, Ritucci L, Robinson PG. Student perspective on their recent dental outreach placement experiences. European Journal of Dental Education 2006; 10: 80-86.
14. Harris RV, Dailey Y, Lennon MA. Recording and understanding social histories by dental post-graduates in a community based clinical programme. European Journal of Dental Education 2003; 7: 34-40.
15. Smith M, Lennon MA, Robinson PG. Students' clinical experience on outreach placements. European Journal of Dental Education 2010; 14(1): 7-11.
16. Smith M, Lennon MA, Brook AH, Blinkhorn FA, Blinkhorn AS, Robinson PG. A randomised controlled trial of the effect of outreach placement on treatment planning by dental students. British Dental Journal 2006 (Education Supplement 06): 27-31.
