South Africa is a middle-income country with serious socioeconomic risk factors for mental illness. Of its population of 52 million, 53% live below the poverty line, 24% are unemployed and 11% live with HIV/AIDS, all of which are factors associated with an increased burden of neuropsychiatric disease1,2. The negative social implications due to the mortality caused by AIDS are immense: thousands of children are being orphaned, increasing the risk of intergenerational mental illness3-5. Ensuring sufficient mental health human resources has been a challenge, with South Africa displaying lower workforce numbers than many low- and middle-income countries6. It is in South Africa's public rural primary healthcare (PRPHC) areas where difficulties with human resources for mental health are the greatest7,8.
An estimated 40% of South Africa's population live in rural areas9,10. In 1994, primary health care (PHC) was mainstreamed into South Africa's public healthcare system as a people-orientated healthcare system, endeavouring to achieve accessible health for all South Africans11. While South Africa has, in international terms, been at the forefront of developing services at a PHC level, much is left to be desired with regards to mental health services. Inclusive, accessible mental health for all has not been attained in the 37 years since the now-famous Alma Ata PHC conference11,12. Due to the lack of psychiatrists in South Africa13, especially in its rural areas8, the psychopharmacological treatment, at a PHC level, of mental illness falls onto the shoulders of already-stretched PHC physicians and PHC mental health nurses (MHNs)8. Efforts to decentralize mental health care to specialty PHC nurses has been falling short of the set benchmarks14-16.
Historically, South African studies indicate that the terrain of the MHN in PHC has been reorganized to focus primarily on violence, substance abuse and HIV/AIDS rather than on psychiatric care including psychotropic medication prescription17. Nurses are seen, and have traditionally been regarded, as the backbone of the public health sector, providing for the majority of the human resources for health in South Africa18. While the WHO estimates that South Africa has a passable ratio of 9.7 nurses trained in mental health per 100 000 population13, knowledge gaps remain about the progress that has been made to successfully integrate this mental health practitioner into the PHC setting, with very little data available on this category's human resources in rural areas. The primary goal of this situation analysis was to fill the knowledge gap with regard to human resources for MHNs practicing in PRPHC facilities. The secondary objectives were to analyse the gaps between resources provided and proposed standards of care, and then to consider approaches to improve the mental health treatment gap between mental health's available services and its burden of disease in South Africa's PRPHC areas.
The study was based on an analysis of both primary and secondary data.
Secondary data
The secondary data analysis included an extensive literature review of PRPHC mental healthcare and human resources for health in South Africa's PHC areas. Reports and policies published by government departments such as the National Department of Health and the South African Nursing Council (SANC), academic publications and dissertations (making use of online academic search engines such as PsychInfo, PubMed and Medline) as well as census data from Statistics South Africa, including findings from the 2011 general household survey, were utilized10,19. International secondary data were obtained from the WHO's recent reports on global mental health13,20,21. The examination of the secondary data revealed knowledge gaps in MHNs' human resource distribution in South Africa's PRPHC areas and necessitated a primary data collection and analysis.
Primary data
Primary data were obtained by communication with the National Department of Health's provincial and district managers with the goal of identifying health facilities in each province that are regarded as rural. Key informant interviews followed and included the medical managers, chief executive officers and/or the nursing service managers of the hospitals classified as rural by the National Department of Health22. The interviews followed a semi-structured interview schedule aimed at evaluating not only professional MHNs' human resources, but also whether they were actually practicing in mental health settings within the PHC setup. This was an important consideration as many professional nurses possess more than one area of specialization and a nurse trained in psychiatry may, for example, be working as a full-time midwife. Mental health nurses were defined as per SANC's definition as professional nurses with at least a 1-year, post-basic, SANC-accredited nursing qualification in Advanced Psychiatry Nursing Science18.
From the secondary data examination, it was established that eight out of the nine provinces in South Africa have health facilities classified as rural. The contributing provinces confirmed that the Department of Health's Human Resource Management Circular of 2004 was used to classify their hospitals as rural22. In collaboration with the participating provinces, an updated list of rural health facilities was constructed, with the 2004 circular serving as a foundation. A total of 163 PRPHC facilities were included in the audit.
The contact details of these facilities' chief executive officers were obtained from the various provinces' district health managers and they were informed of their facilities being included in the audit, the nature and the context of the study and the voluntary nature of participation in the study. The medical managers and/or nursing service managers of the participating facilities were then contacted and their permission to participate in the audit was requested. The nature of the study, confidential participation and voluntary withdrawal/refusal to participate was discussed. Informed consent was obtained and the participants were subjected to a brief interview schedule concerning the mental health nursing human resources at their facilities. In cases where the chief executive officers, medical managers and/or the nursing service managers were unreachable via telephone, an electronic version of the telephonic questionnaire was forwarded to participants to complete via e-mail, with three reminders prompting them to complete the questionnaire. If no response was obtained after the reminders, it was assumed that the prospective participants chose not to participate in the study.
Data analysis and presentation
The telephonic interviews were digitally recorded and transcribed verbatim. Both the transcribed telephonic interviews and electronic interviews were collated and transferred to a spreadsheet where lists of MHNs' human resources in PRPHC settings per province were constructed. A quantitative descriptive analysis was performed and the results are presented as tables in subsequent sections.
Ethics approval
The primary data collection procedure was initiated by obtaining University of KwaZulu-Natal Biomedical Research Ethics Committee clearance (BE416/13), followed by provincial approval to conduct the research at their health facilities.
Of the 163 facilities representing the public rural health centres in South Africa, 98% (160) participated in the audit.
Human resources
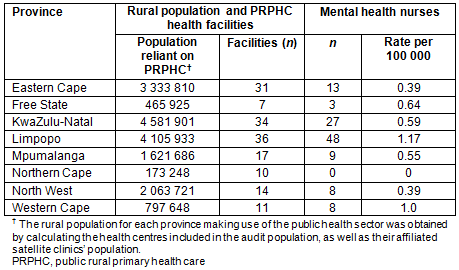
Of the 160 PRPHC facilities, 62 (38.7%) employed a total of 116 MHNs that were working in mental health settings. These rural health facilities, together with their affiliated satellite clinics and community health centers, serve an estimated combined population of 17 143 872 people9,10,19, suggesting that MHNs are employed there at a rate of 0.68 per 100 000 population (Table 1). The analysis of the secondary data indicates that MHNs are practicing in South Africa at a national rate of 9.7 per 100 000 population13.
Table 1: Mental health nurse human resources in public rural primary healthcare facilities per province and population rates per 100 000 population.
Human resource production
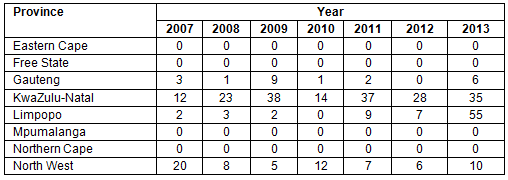
The output of MHNs qualifying per year has been 56 on average between 2007 and 2013 (Table 2).
Table 2: Mental health nurses qualifying per year, per province from 2007 to 201318.
Discussion
Lack of mental health nurse human resources in rural areas
When compared to other middle-income countries, the national ratio of MHNs per 100 000 population practicing in South Africa of 9.7 seems to be well on par with WHO recommendations13. The woeful representation (0.68 per 100 000 population) of this cadre of mental healthcare professional in the public sector's rural areas is then both a worrying and an unexpected finding. With approximately 40% of South Africa's population living in rural areas10, the setting where access to medical psychiatric prescribers (psychiatrists) is the direst6, one would expect to find more human resources for MHNs in these areas, owing to the task-shifting approach endorsed by the WHO20 and adopted by South Africa's National Department of Health23.
Due to mental health prescriber shortages, the task of prescribing psychotropic medication in rural PHC settings has been shifted from psychiatrists to MHNs and PHC medical officers. Task shifting is defined as the delegation or substitution of tasks from one cadre to another (new or existing) cadre with either less training or narrowly specialised training20,24. While this approach has been found to be an effective method to alleviate medical workforce shortages, especially in rural communities23-26, this study's findings suggest a worrying shortage of MHNs working in mental healthcare to whom the task of prescribing psychotropic medication can be shifted. Medical officers dedicated to mental health care are represented at a rate of 0.37 per 100 000 population at PRPHC level while psychiatrists are practicing in these settings at a rate of 0.03 per 100 00027. De Kock's findings that only 18.7% (30) of South African rural public hospitals employ medical officers dedicated to mental healthcare, and only 3.7% (6) employ psychiatrists, allude to a heavy burden on the limited number of MHNs.
Mental health nurse human resource production
With regard to the human resource output, future prospects of alleviating this cadre's human resource crisis appears gloomy: the relatively small number of MHNs trained18 as described in Table 2 is worrying. Some provinces (Mpumulanga, Eastern Cape, Northern Cape and Free State) have trained no MHNs over the last 7 years and so it is not surprising then that these provinces are most affected with regard to a lack of human resources for MHNs in rural PHC areas (see Table 2). Recent efforts to up-scale the training of MHNs in KwaZulu-Natal, Limpopo, North West and Western Cape have seen an increase of MHNs in these provinces. This increase stems directly from the National Department of Health's renewed commitment to mental health and the SANC's focus on specialist nurse production18. The distribution, however, of these newly qualified nurses remains uneven and the increases are less than what is required to meet national norms in PRPHC areas. If the average output of MHNs remains at 55 per year (as was recorded between 2007 and 2013), and all of these newly trained nurses are employed in the public sector's rural settings, it would take in excess of 35 years to reach the WHO13 middle-income country standard of 9.7 MHNs per 100 000 population in PRPHC areas.
Unbalanced distribution of mental health nurses
Even though the substantial treatment gap between human resources for mental health in rural areas (0.68 per 100 000 population) and its burden of disease suggested by this study is in keeping with WHO21 estimates and South African studies15,28, one cannot help but wonder where the rest of this cadre of professionals (nationally MHNs are represented at 9.7 per 100 000 population) are practicing. The seemingly obvious explanation may be that MHNs are practicing in the private sector and/or the urban/peri-urban public sector. Another explanation may be that they are employed at traditional psychiatric hospitals or in public rural areas but practicing within other health areas29. The degree of need relating to the burden of disease of other health conditions such as HIV/AIDS may also have taken priority in the distribution of nursing tasks at a PHC level, with mental health being traditionally regarded as 'the Cinderella of health care' in South Africa30. This, together with the introduction of occupation-specific dispensation in 200731, may have led to a task-reshuffling of nurses (including MHNs that are qualified in more than one specialty) taking up positions in other PHC areas. To substantiate these hypotheses, it is recommended that SANC update their databases with regard to human resources for MHNs, with a specific focus on this cadre's distribution in public, private, rural and urban populations.
Recommendations
With the human resources for mental health in South Africa's rural areas being in a state of crisis, recommendations are firstly made to increase the numbers of MHNs in these areas. The SANC is urged to re-evaluate their mental health nursing training program outcomes and output and then, together with the Department of Health, further address the shortfall in MHNs trained that has been witnessed over the past couple of years18. Where MHNs have been allocated to practice in other PHC/health areas within rural public health facilities, it is imperative that they are transferred back to practice within mental health areas. Nursing service managers at the rural facilities are urged to reflect on the PHC system's heavy reliance on this cadre of mental health professional with regard to diagnosing mental illness and prescribing psychotropic medications, especially when taking into account that medical prescribers are almost non-existent in these areas6.
Over the past 5 years the SANC has started to prioritise mental health as a part of their National Strategic Plan for Nurse Education, Training and Practice for 2012/13-2016/17, most noticeably by considering a rural preparation element to their mental health training program18. Unfortunately, at the time of writing, no sources of the commitment of this ideal was available to the authors. The upscaling of human resources for MHNs in rural areas will necessarily be a lengthy process: based on the current training output at least a generation of rural South Africans will continue to have poor access to prescribing mental health professionals. For this reason, by relying exclusively on MHN numbers to increase in order to improve care we will be a doing a disservice to South Africa's rural communities. Policy makers, during the South African National Mental Health Summit of April 2012, re-affirmed that the overhauling of the PHC system should first and foremost be based on inclusive health care, including mental health care, for all South Africans30. The integration of mental health into the PHC system, as a part of its re-engineering, would consist of creative problem-solving approaches to a system in dire need of human resources. Recently, South African clinical associates, a mid-level health cadre of health practitioner32, were granted the authority to prescribe medications, including limited psychotropics, in rural PHC areas33. In a similar fashion, it is recommended that consideration is given to other appropriately trained mental health professionals who are practicing in the public sector's rural areas, by extending their scopes of practice to include psychotropic prescriptive authority in an effort to further alleviate mental health workforce shortages and to improve access to care. Shifting this task of prescribing to a variety of appropriately trained non-medical prescribers has had positive outcomes internationally25.
By no means is the claim made that prescribing psychotropic medication is the only need in the South African rural mental health crisis. Careful consideration to context-specific approaches to mental health care should be given in settings where the understanding of mental illness is not based on the biomedical Western model34. Mental health in rural South Africa can and should be seen as a multifactorial, reciprocal biopsychosocial-spiritual construct and not merely as the freedom from disease. Community engagement and psychosocial interventions in PHC settings have been found to play a crucial role in mental health promotion and the demarginalization of patients15,17. South Africa has started the process of task shifting on various psychosocial levels of care, with pilot studies showing positive outcomes5,15,28. While the medicalization (to apply a biomedical model to mental health care) of mental health has understandably been critiqued over the last decade, most notably for advancing medical solutions to mental health problems at the expense of social, political and community action35-37 , the availability of appropriate medical treatment remains paramount to mental health in PHC settings5. The WHO's task-shifting approach, for example, actively encourages community engagement in mental health care; it also clearly states that the availability and correct usage of psychotropic medication is integral to mental health in a PHC system38-40. South African studies further advocate MHNs' ability to work as holistic (biopsychosocial) practitioners as central in their provision of mental health care in PHC settings41. This article's findings suggest a critical shortage of prescribers in PRPHC areas to whom prescribing tasks can be shifted. This article, rather than promoting a medicalization model of mental health, advocates the responsible use of psychotropic medication by making it available to underserved communities that are in dire need of competent prescribers. If the task-shifting initiative could provide prescribers that are attuned to their patients' needs, they could not only provide a greater choice to patients at PRPHC level, but also choose not to prescribe medications if psychosocial interventions are more appropriate42.
Limitations
This study attempted to give the first published overview of MHNs' human resources in South Africa's PRPHC settings. Even though this study's findings could be interpreted as representative because 98% of the sample's facilities participated in the audit, the results should be regarded as a guide for further, comprehensive enquiries by SANC and the Department of Health, especially with regard to MHN distribution. At the time of initiating this situation analysis in 2013, a paucity of resources was available about this cadre's distribution in the private, public and rural public settings. At the time of the situation analysis completion, distribution statistics were still not available from SANC, the national nursing governing body, or from the Department of Health. Some efforts have been made to update the nursing database as proposed and accepted as a part of the Strategic Plan for Nurse Education, Training and Practice 2012/13-2016/1718. This updated database was not available at the time of writing, making it difficult to formulate evidence-based hypotheses regarding the discrepancy between the rate of 0.68 per 100 000 population at which MHNs are practicing in the public sector's rural areas and the supposed healthy distribution of this cadre in the rest of South Africa (9.7 per 100 000). With the time elapsed since the start of the audit, the authors, while making every effort to maximise the inclusivity of facilities, cannot claim that an exhaustive list of health facilities was included because some facilities may have been added or removed by provincial departments. This limiting factor, together with the rural population's calculation that was based on primary and secondary data collection9,19 , suggests a tentative interpretation of findings.
As a result of serious socioeconomic risk factors, South Africa's burden of disease for mental illness is likely to continue to rise in the foreseeable future6. Due to the lack of medical mental health prescribers in rural PHC settings, the task of prescribing psychotropics has been shifted to MHNs. This situation analysis suggests that there is a distressing shortage of MHNs to whom this task could be shifted, indicating that the rural parts of South Africa are in a crisis with regard to prescribing mental health professionals. It also suggests that South Africa is falling short of its target to integrate mental health successfully into the PHC system, which is the system that the majority of rural South Africans rely on for healthcare services19. Recommendations are made in line with the Department of Health's approach to re-engineer and integrate mental health into PHC services30, by scaling up the human resources for MHNs, but also by including more cadres of health professionals in the WHO-endorsed campaign of task shifting with regard to the delivery of mental health services, including the prescription of psychotropic medications20.
References
1. Central Intelligence Agency. South Africa. In: CIA world fact book. Washington, D.C.: Central Intelligence Agency, 2014.
2. Hanass-Hancock J. Disability and HIV/AIDS-a systematic review of literature on Africa. Journal of the International AIDS Society 2009; 12: 34. http://dx.doi.org/10.1186/1758-2652-12-34
3. Vlassova N, Angelino AF, Treisman GJ. Update on mental health issues in patients with HIV infection. Current Infectious Disease Reports 2009; 11: 163-169. http://dx.doi.org/10.1007/s11908-009-0024-4
4. Karim SA, Karim QA. HIV/Aids in South Africa. Cape Town: Cambridge University Press, 2010. http://dx.doi.org/10.1017/CBO9781139062404
5. Patel V, Kleinman A. Poverty and common mental disorders in developing countries. Bulletin of the World Health Organization 2003; 81: 609-615.
6. Burns JK. The mental health gap in South Africa - a human rights issue. Equal Rights Review 2011; 6: 99-113.
7. Lund C, Petersen I, Kleintjes S, Bhana A. Mental health services in South Africa: taking stock. African Journal of Psychiatry 2012; 15: 402-405. http://dx.doi.org/10.4314/ajpsy.v15i6.48
8. Petersen I, Lund C, Bhana A, Flisher AJ. A task shifting approach to primary mental health care for adults in South Africa: human resource requirements and costs for rural settings. Health Policy and Planning 2012; 27: 42-51. http://dx.doi.org/10.1093/heapol/czr012
9. Kok P, Collinson M. Migration and urbanisation in South Africa. Pretoria: Statistics South Africa, 2006.
10. Lehohla P. Census 2011 Census in brief. Report no. 03-01-41. Pretoria: Statistics South Africa, 2013.
11. Kautzky K, Tollman S. A perspective on primary health care in South Africa. In: J Roma-Reardon (Ed). South African Health Review. Durban: Health Systems Trust, 2008; chapter 2.
12. World Health Organization. Alma Ata Declaration. Geneva: World Health Organization, 1978.
13. World Health Organization. Mental health atlas 2011. Geneva: World Health Organization, 2011.
14. Seedat S. Epidemiology of mental disorders in South Africa. Gauteng: Ministry of Health, Republic of South Africa, 2012.
15. Petersen I, Lund C. Mental health service delivery in South Africa from 2000 to 2010: one step forward, one step back. South African Medical Journal 2011; 101: 751-757.
16. Department of Health. Human resource needs in mental health. Pretoria: Ministry of Health, Republic of South Africa, 2012.
17. Swartz L, MacGregor H. Integrating services, marginalizing patients: psychiatric patients and primary health care in South Africa. Transcultural Psychiatry 2002; 39: 155-172. http://dx.doi.org/10.1177/136346150203900202
18. South African Nursing Council. The National Strategic Plan for Nurse Education, Training and Practice 2012/13-2016/17. Pretoria: South African Nursing Council, 2013.
19. Lehohla P. Use of health facilities and levels of selected health conditions in South Africa: findings from the General Household Survey, 2011. Report no. 03-00-05 (2011). Pretoria: Statistics South Africa, 2013.
20. World Health Organization. Task shifting: rational redistribution of tasks among health workforce teams: global recommendations and guidelines. Report no. 92-4-159631-7. Geneva: World Health Organization, 2008.
21. World Health Organization. WHO launches the World Health Statistics 2012. European Communicable Disease Bulletin 2012; 17.
22. Department of Health. Human Resource Management Circular 87 of 2004. Pretoria: Department of Health, 2004.
23. Petersen I, Lund C, Stein DJ. Optimizing mental health services in low-income and middle-income countries. Current Opinion in Psychiatry 2011; 24: 318. http://dx.doi.org/10.1097/YCO.0b013e3283477afb
24. Fulton BD, Scheffler RM, Sparkes SP, Auh EY, Vujicic M, Soucat A. Health workforce skill mix and task shifting in low income countries: a review of recent evidence. Human Resources for Health 2011; 9: 1-11. http://dx.doi.org/10.1186/1478-4491-9-1
25. Callaghan M, Ford N, Schneider H. Review: a systematic review of task-shifting for HIV treatment and care in Africa. Human Resources for Health 2010; 8: 8-16. http://dx.doi.org/10.1186/1478-4491-8-8
26. Nelson R. Combating global health worker shortages: task shifting and sharing may provide one solution. American Journal of Nursing 2012; 112(12): 17-18. http://dx.doi.org/10.1097/01.NAJ.0000423494.77404.42
27. De Kock JH. Alleviating the mental health crisis in South Africa's rural primary care areas through task shifting: non-medical prescribers and the case of clinical psychology. PhD dissertation. Durban: University of KwaZulu-Natal, 2016.
28. Lund C, Alem A, Schneider M, Hanlon C, Ahrens J, Bandawe C, et al. Generating evidence to narrow the treatment gap for mental disorders in sub-Saharan Africa: rationale, overview and methods of AFFIRM. Epidemiology and Psychiatric Sciences 2015; 24: 233-240. http://dx.doi.org/10.1017/S2045796015000281
29. Wildschut A, Mqolozana T. Shortage of nurses in South Africa: relative or absolute? Case study report, forming part of the HSRC study: a multiple source identification and verification of scarce and critical skills in the South African labour market. Pretoria: Department of Labour South Africa, 2008.
30. Motsoaledi AP. Speaking notes for the Minister of Health: Dr AP Motsoaledi at the national mental health summit. Gauteng: Ministry of Health, Republic of South Africa, 2012; 1-10.
31. Naledi T, Barron P, Schneider H. Primary health care in SA since 1994 and implications of the new vision for PHC re-engineering. South African Health Review 2011; 17-28.
32. Doherty J, Couper I, Fonn S. Will clinical associates be effective for South Africa? South African Medical Journal 2012; 102: 833-835.
33. Motsoaledi AP. Regulations defining the scope of practice of clinical associates. Pretoria: Department of Health, Republic of South Africa, 2014.
34. Shaw I, Middleton H. Approaches to 'mental health' in low-income countries: a case study of Uganda. Mental Health Review Journal 2013; 18: 204-213. http://dx.doi.org/10.1108/MHRJ-07-2013-0025
35. Petersen I. Comprehensive integrated primary mental health care for South Africa. Pipedream or possibility? Social Science & Medicine 2000; 51: 321-334. http://dx.doi.org/10.1016/S0277-9536(99)00456-6
36. Clark J. Medicalization of global health 2: the medicalization of global mental health. Global Health Action 2014; 7. http://dx.doi.org/10.3402/gha.v7.24000
37. Summerfield D. Afterword: against global mental health. Transcultural Psychiatry 2012; 49: 519. http://dx.doi.org/10.1177/1363461512454701
38. Clark J. Medicalization of global health 3: the medicalization of the non-communicable diseases agenda. Global Health Action 2014; 7. http://dx.doi.org/10.3402/gha.v7.24002
39. Kakuma R, Minas H, van Ginneken N, Dal Poz MR, Desiraju K, Morris JE, et al. Human resources for mental health care: current situation and strategies for action. Lancet 2011; 378: 1654-1663. http://dx.doi.org/10.1016/S0140-6736(11)61093-3
40. Saxena S, Thornicroft G, Knapp M, Whiteford H. Global mental health 2 - resources for mental health: scarcity, inequity, and inefficiency. Lancet 2007; 370: 878-889. http://dx.doi.org/10.1016/S0140-6736(07)61239-2
41. Petersen I. Training for transformation: reorientating primary health care nurses for the provision of mental health care in South Africa. Journal of Advanced Nursing 1999; 30: 907-915. http://dx.doi.org/10.1046/j.1365-2648.1999.01166.x
42. LeVine E, Foster EO. Integration of psychotherapy and pharmacotherapy by prescribing-medical psychologists: a psychobiosocial model of care. In: RE McGrath, BA Moore (Eds). Pharmacotherapy for psychologists: prescribing and collaborative roles. Washington, DC: American Psychological Association, 2010; 105-31. http://dx.doi.org/10.1037/12167-006
