Dear Editor
Many of the maternal deaths caused by postpartum hemorrhage (PPH) in rural settings may have been avoidable if effective hemostatic procedures had been available; intrauterine hemostatic balloon has recently been widely used1. The non-uterine-specific condom-balloon has become more popular in limited-resource countries1,2: a systematic review showed that, of all types of intrauterine balloon, the condom-balloon was used in 80% of cases in low-resource countries, with hemostasis achieved in 96% of cases1. For example, caregivers in Kenya, after training in condom-balloon use, became accustomed to using it and it achieved hemostasis in most patients3. The condom-balloon is especially useful as a temporary measure until higher-level care is reached3.
I have discussed use of the condom-balloon in a previous article published in Rural and Remote Health2. In that article I mentioned another hemostatic measure for PPH - 'holding the cervix' - available in rural settings: forceps are used to close the cervical ostium; blood is accumulated in the uterus, tamponading the uterine bleeding surface, achieving hemostasis2,4,5.
One drawback of the intrauterine balloon is balloon prolapse into the vagina: severe bleeding, once stopped by a balloon, may recur if the balloon prolapses. In a Kenyan study, approximately 10% of providers encountered balloon prolapse3. If this occurs during transport, it may be fatal. Our team recently developed a combination of the abovementioned two methods, which prevents balloon prolapse, achieving hemostasis6,7. Although we usually use uterine-specific intrauterine Bakri balloon (Cook Medical, Bloomington, Indiana, USA) in our tertiary center, our technique is similarly useful for preventing condom-balloon-prolapse in rural settings.
After placing the balloon, both cervical lips should be held by sponge forceps (Fig1), closing the cervical ostium2,4,5. Usually, at balloon insertion into the uterus, the anterior lip may be held by forceps; one extra effort makes the 'holding the cervix' method easy, even for less-experienced practitioners. Any other forceps with a weak grasping force, possibly available in many rural facilities, can be used. This prevents balloon prolapse. Usually, we use ultrasound to check that intrauterine or intraperitoneal hemorrhage is absent8. Without ultrasound monitoring, if massive intrauterine bleeding occurs after closing the cervix, blood usually exits through the cervix into the vagina, causing alarm for medical staff because the intrauterine bleeding is uncontrolled. We have had no instances of uterine rupture, even though uterine rupture is a potential adverse effect of this technique. Sponge forceps are usually released after 12-24 hours but can be released earlier or later after the patient's arrival at more adequately equipped centers. This is effective as a hemostatic method, especially while waiting for, and also during, transport to a center.
Japan is listed as and considered to be a high-resource country; however, it has many remote rural areas in which medical resources are insufficient. For example, Japan has more than 400 islands, which are completely isolated during bad weather: the situation may be fundamentally the same irrespective of whether the country is a low- or high-resource nation. I worked on several islands before becoming a university staff member. Condom-balloons may be a boon for these settings, and our method may increase hemostatic effect.
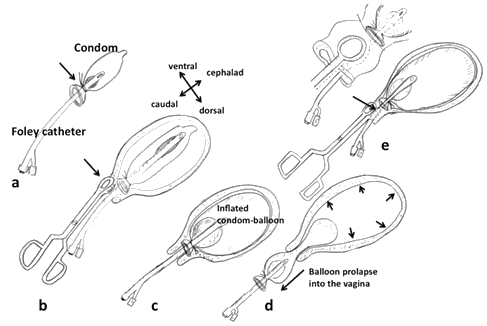
Figure 1: Schematic presentation of condom-balloon (a-d) and 'holding the cervix' method (e) to prevent condom-balloon-prolapse into the vagina. a. The tip of a Foley transurethral catheter is inserted into the condom. The open end of the condom is tightly tied with sterile thread (arrow). b. The condom is inserted into the uterus. For its easy insertion, the anterior cervical lips should be held by sponge forceps (arrow). c. The condom is inflated by saline or water either by syringe or an intravenous infusion set. The condom is usually filled with 250-500 mL1 - inflation volume depends on the situation. d. A balloon prolapse into the vagina (arrow). The tamponading effect is lost, and thus bleeding recurs from the uterine surface (arrows). e. Anterior and posterior cervical lips are held by sponge forceps (arrow), which prevents balloon prolapse. Upper inset indicates the schema at a higher magnification, illustrating both cervical lips being held by a sponge forceps.
Shigeki Matsubara
Department of Obstetrics and Gynecology, Jichi Medical University, Tochigi, Japan
References
1. Tindell K, Garfinkel R, Abu-Haydar E, Ahn R, Burke TF, Conn K, et al. Uterine balloon tamponade for the treatment of postpartum haemorrhage in resource-poor settings: a systematic review. BJOG 2013; 120(1): 5-14.
2. Matsubara S. Available hemostatic measures for postpartum hemorrhage in rural settings. Rural and Remote Health (Internet) 2012; 12: 2248. Available: www.rrh.org.au (Accessed 23 March 2016).
3. Natarajan A, Chavez J, Ahn R, Nelson BD, Eckardt M, Dulo L, et al. Provider experiences with uterine balloon tamponade for uncontrolled postpartum hemorrhage in health facilities in Kenya. International Journal of Gynecology and Obstetrics 2015; 131(2): 201-204.
4. Matsubara S, Kuwata T, Usui R. Forceps holding the cervix for postpartum haemorrhage. Journal of Obstetrics and Gynaecology 2011; 31(6): 509-509.
5. Matsubara S. A simpler alternative to the Sengstaken-Blakemore tube: cervix-holding by forceps to control hemorrhage after cesarean section for placenta previa. Journal of Obstetrics and Gynaecology Research 2012; 38(5): 903-904.
6. Matsubara S. Combination of an intrauterine balloon and the 'holding the cervix' technique for hemostasis of postpartum hemorrhage and for prophylaxis of acute recurrent uterine inversion. Acta Obstetricia et Gynecologica Scandinavica 2014; 93(3): 314-315.
7. Matsubara S, Baba Y, Takahashi H. Preventing a Bakri balloon from sliding out during 'holding the cervix': 'fishing for the balloon shaft' technique (Matsubara). Acta Obstetricia et Gynecologica Scandinavica 2015; 94(8): 910-911.
8. Matsubara S, Kuwata T, Usui R, Ohkuchi A. 'Holding the cervix' technique for post-partum hemorrhage for achieving hemostasis as well as preventing prolapse of an intrauterine balloon. Journal of Obstetrics and Gynaecology Research 2013; 39(5): 1116-1117.
