Introduction
A number of medical school initiatives in recent years have been designed to make medical education more oriented to medical practice in rural environments. Their aim has been to produce more medical graduates willing and able to practice medicine in rural and remote areas and eventually lead towards long-term solutions to chronic problems of recruitment and retention of doctors in regions with widely dispersed populations.
This article documents a selected number of such initiatives in three countries: Canada, the United States and Australia. One important task has been to examine how the rural mandate fits within the overall mandate, the policies and practices and the curricula of the different schools. To this end, a typology of rural schools has been developed to capture such differences with an aim to understand their impact on their respective medical education programs. A second task was to reflect on the preoccupations of the academic leaders of innovative rural schools as a means of assessing where the weaknesses and strengths of these programs lie. The main focus of the article is on undergraduate medical education, although some reference is made to post-graduate residency training.
Method
Schools noted for the rural thrust to their programs were selected in each of the three countries. The intent was to choose representative examples of different approaches to rural medical education, rather than making some prior judgment as to their level of success. Interviews were conducted with officials designated as having responsibility for the rural component of each school's program. An open-ended interview process was used focusing on the respondents' perceptions of the strengths and weaknesses of their programs, and on their preoccupations with the challenges they face in meeting their rural mandate. This study is based on an analysis of 31 interviews carried out across the seven schools. The interview data were supplemented by published material on the schools and programs studied.
Results
Typology of schools
The schools break down into different types according to the extent to which their mandate may be defined as rural. Mixed Urban/Rural Schools are historically urban based schools which have expanded their mandate to address the needs of specific rural and remote jurisdictions with which they have developed relationships (Table 1). The examples chosen here are the University of Washington WWAMI program in the US, the expansion of the University of British Columbia program in Vancouver, Canada (UBC) and the Flinders University program in Adelaide, South Australia. DeFacto Rural Schools are schools with a mandate to serve geographic regions (province or state) with substantial rural populations, but they do not necessarily define their role as rural (Table 2). The examples used here are the University of New Mexico (UNM) in the US and Memorial University of Newfoundland in Newfoundland and Labrador, Canada. Stand Alone Rural Schools are new schools specifically created to meet the needs of defined rural and remote regions, the examples being James Cook University (JCU) in Queensland, Australia and the Northern Ontario School of Medicine (NOSM) in Canada (Table 3). The tables outline the basic structure, admissions policy and level of rural exposure of students for each of the different schools.
Table 1: Structure of mixed urban/rural schools
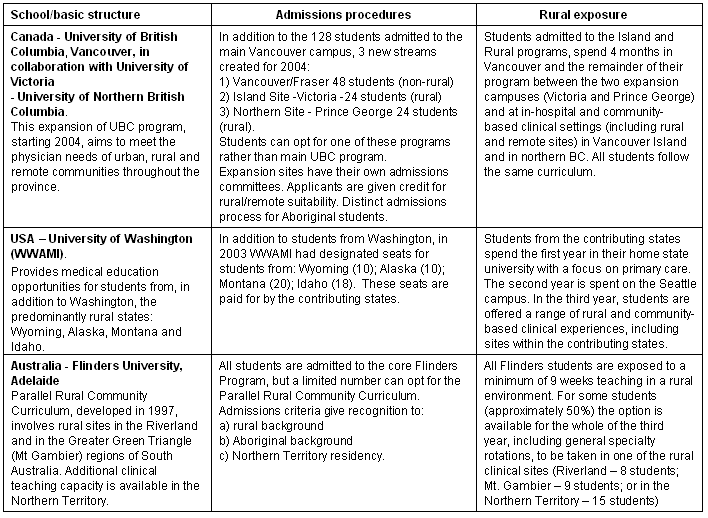
Table 2: Structure of defacto rural schools

Table 3: Structure of stand-alone rural schools
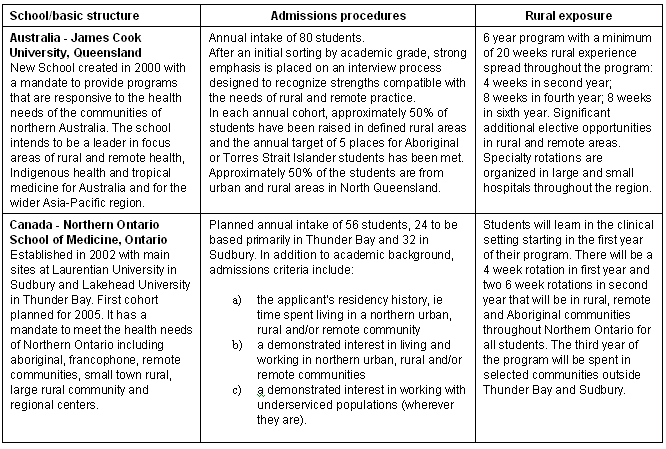
The rural pipeline
Typically, medical students are drawn disproportionately from urban professional family backgrounds1. Rural medical education programs have sought to admit students whose social composition more closely reflects that of the communities they serve. It has been well established that students from rural backgrounds are more likely than urban students to opt to practice in a rural community2-6, and that greater exposure of students to rural health issues during their medical training further enhances the likelihood of rural practice after graduation7,8. Selecting students with a more natural affinity for rural practice, and shaping their educational experience in a way that builds on this affinity, represents an appealing non-coercive strategy for attracting more doctors into areas that have historically been shunned by medical graduates.
The passage of students, from the point where they first develop their aspiration for a career in medicine, through the shaping effects of the medical education process itself, has been compared with a pipeline in which the flow must be maintained at every point to sustain the supply of doctors to rural areas9,10. Key points along the pipeline are:
- the formation of career aspirations during the school years
- medical school admission procedures
- exposure during medical school and during residency training to rural clinical practice
- a curriculum oriented to rural health delivery
- a system of educational and professional support for practicing rural doctors.
The schools studied reported that rates of application by rural students were as low as half that of urban students and they all acknowledged the importance of increasing the profile of medicine as a career to rural school-aged children. Most of the schools had programs aimed at Aboriginal and minority populations and many had special units, such as the Hispanic and Native American Centre of Excellence at the University of New Mexico, encouraging the recruitment of these students to their programs, and providing them with support once admitted. There were, however, few initiatives directed at rural youth in general and clearly this is an area where most schools would like to do more if they could obtain the necessary funding support.
All of the schools studied had admissions policies designed to attract students from rural backgrounds, although in the Mixed Urban/Rural Schools, these policies only applied to the rural stream students. Typically, there is a grade threshold which students must meet in order to be considered for admission but, beyond this, other factors predictive of good practice in a rural setting play a role in the selection process. The University of British Columbia, for example, assesses all applicants with a Rural/Remote Suitability score. Most of the schools had rural community members on their admissions committees to ensure that the rural mandate was respected, and most also had specific admission processes and targets for Aboriginal students.
The level of exposure to rural clinical settings within each of the programs varied considerably among the schools studied. The Mixed Urban/Rural Schools (UBC, WWAMI and Flinders) have defined streams which are exposed to an enriched rural environment in designated regions. At Flinders, this exposure extends beyond family medicine to specialty clinical disciplines and the whole of the third year is spent in rural community settings11. A recent study has shown that when these rural stream students were compared with their urban counterparts based in acute care settings, the rural students showed a higher level of performance on common exams12. The DeFacto Rural Schools (UNM and Memorial) organize the rural exposure of their students largely within their family or community medicine programs. The Stand-Alone Schools (JCU and NOSM) have the most extended opportunities for rural exposure and, like Flinders, consider the challenges of the rural health context an enriched clinical learning environment compared with acute care hospitals.
All of the schools studied provided for substantial rural training opportunities within their post-graduate family medicine residency programs, thus ensuring the strong rural orientation at the undergraduate level is sustained during the critical period prior to entry to practice. The availability of rural training sites for other speciality residencies, such as general surgery or paediatrics, was more limited, with most schools providing only short periods of rural-based training. The Stand Alone Rural Schools had the most substantial plans for rural-based speciality training, but almost all respondents saw this as an important area for future development, particularly in forming specialists with general skill sets appropriate for rural contexts.
The final stage in the pipeline is a system of support for rural doctors. All the schools studied depended on a widespread network of rural doctors to act as preceptors and tutors to their students and this network needs to be sustained by a range of academic support, professional development and information services. These services not only support the teaching function, they also enrich the skills and experience of rural doctors and serve to reduce their sense of isolation.
Designing curriculum for rural practice
The feature which most distinguishes the Stand Alone Rural Schools from the other models is their curriculum content. The Mixed Urban/Rural Schools had developed their rural programs within the framework of existing urban, acute care-based programs. As a consequence, the rural component of the program is an add-on feature, characterized largely by the special clinical experience of the rural stream students. The main framework of the curriculum, which must serve both the urban and rural students, remains relatively unchanged. Stand Alone Rural Schools, however, have had the freedom, within the framework of their national accreditation processes, to create new curricula that are more reflective of the population health and medical care needs of rural and remote populations. Advocates for rural health have stressed the importance of integrating rural health issues into the core of the curriculum13,14, and the new schools have been able to do this and to capitalize on the challenges of rural environments as a rich source of clinical learning opportunities.
James Cook University exemplifies a curriculum which places a strong emphasis on rural and remote health issues15. In addition to specific content, such as a semester-long course titled 'Rural, Remote, Indigenous and Tropical Medicine', the case materials, on which learning modules are based, reflect regional and rural health realities. A substantial part of the students' clinical training takes place in community-based settings and learning groups are led by group tutors who are mostly rural physicians. The rural focus is not limited to the family medicine components of the program, but extends to all areas of study. Similarly, NOSM has a newly designed curriculum in which Northern and Rural Health and Social and Population Health are two of the five themes that are woven through the whole four years of the program. Both of these new schools maintain that their goal is not just to produce rural physicians, but rather to take advantage of the health challenges of rural and remote environments to train students with superior skills that would serve them in a wide variety of contexts, both rural and urban.
Discussion
Notwithstanding their differences, all three types of school have shown a clear recognition of the importance of rural health. This is expressed in a positive focus on students learning about rural health and rural practice, presentation of rural practice as a positive career option, and depiction of clinical placements in rural settings as positive for students (in that they see a wide range of clinical problems and develop a broad variety of clinical skills). This contrasts with common and longstanding stereotypes of rural health as irrelevant, rural practice as the ultimate 'failure' (as compared with specialty/sub-specialty practice in metropolitan tertiary care teaching hospital) and rural clinical attachments as 'doing time' away from where the 'real medicine' is in the teaching hospital/academic health science centre.
It is a reasonable conclusion from our study that the structure most suited to maintaining this positive view of rural practice is that of the dedicated Stand Alone Rural Schools. The centrality of their rural and remote mission, the fact that this mission does not have to compete with other more specialist oriented agendas, and the fact that their government funding is largely contingent on them being successful in this mission, ensures that the positive view of rural health translates into real commitments within their programs. Thus, they show evidence of practical commitments to real curriculum time with a focus on rural health and rural practice, dedicated academics/faculty members who teach and research rural health and rural practice, and sustained investments in rural based infrastructure and resources. But it should also be noted that the two schools studied, JCU and NOSM, are relatively new ventures and the long-term impact on their regions' physician resources has yet to be demonstrated.
It is also reasonable to conclude that the Mixed Urban Rural Schools and the DeFacto Rural Schools have shown impressive results, given that their mandates are more diverse. The rural streams in the Mixed Urban Rural Schools have admission processes favouring rural students, they make provision for substantial exposure to rural clinical practice, and they have developed widespread networks of rural clinical teachers. The fact that these programs are highly dependent on targeted government funding represents both a strength and a weakness. It is a strength because the external funding means that the rural streams do not have to compete for the core funding of the host school, but it is a weakness because the contingent nature of the funding makes it harder to attract and support tenured faculty and permanent staff. Also, the fact that these streams must coexist with more traditional programs with strong biomedical orientations does inhibit the development of an overarching rural health focus to the curriculum. These weaknesses aside, the lesson for others is that strong and successful rural programs can be developed within the framework of more traditional schools in areas where the development of a Stand Alone Rural School is not warranted.
The DeFacto Rural Schools, UNM and Memorial, have adopted rural medical education strategies as a means of meeting their regional mandates largely as a result of strong leadership that has taken them in that direction. They have been helped in this by governments keen to encourage them to focus on the business of meeting the physician needs in their region. Other schools serving geographically similar populations have not necessarily adopted explicit rural orientations, preferring rather to emulate the metropolitan model. There is no doubt that leadership is an issue, particularly in fostering a positive view of rural medicine and a culture of service to otherwise neglected populations rather than one of high technology and multiple specialities and sub-specialities.
Conclusion
Academic leadership appeared an important factor in all the schools studied, but it is also clear that without the targeted government funding that supports these programs, many would not exist. The rural components of the Mixed Urban/Rural Schools are funded outside of the normal allocation model for the metropolitan university based program and both the DeFacto Rural and the Stand Alone Rural Schools are specially funded by governments with strong expectations that they meet the demand for rural doctors. Enlightened government policy toward the support of rural health has gone a long way to redressing significant imbalances in the distribution of health care that market forces alone have seemed incapable of correcting.
Acknowledgements
This study was part of a larger project: 'Strengthening the Medical Workforce in Rural Canada: The Roles of Rural/Northern Medical Education' funded by the Canadian Institutes of Health Research. Support has also been given from the Centre for Rural and Northern Health Research at Laurentian University and the Newfoundland and Labrador Centre for Applied Health Research at Memorial University.
References
1. Dhalla IA, Kwong JC, Streiner DL, Baddour RE, Waddell AE, Johnson IL. Characteristics of first-year students in Canadian medical schools. Canada Medical Association Journal 2002, 166: 1029-1035.
2. Rabinowitz HK. Relationship between US medical school admission policy and graduates entering family practice. Family Practice 1988; 5: 142-144.
3. Roberts A, Davis L, Wells J. Where physicians practicing in Appalachia in 1978 to 1990 were trained and how they were distributed in urban and rural Appalachia. Academic Medicine 1991; 66: 682-686.
4. Stratton TD, Geller JM, Ludtke RL, Fickenscher KM. Effects of an expanded medical curriculum on the number of graduates practicing in a rural state. Academic Medicine 1991; 66: 101-105.
5. Strasser RP. How can we attract more doctors to the country. Australian Journal of Rural Health 1992; 1: 39-42.
6. Tepper JD, Rourke JTB. Recruiting rural doctors: ending a Sisyphean task. Canadian Medical Association Journal 1999: 160: 1173-1174.
7. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. Which medical schools produce rural physicians? JAMA 1992; 268: 1559-1565.
8. Rourke JTB. Building the new Northern Ontario Rural Medical School. Australian Journal of Rural Health 2002; 10: 112-116.
9. Council on Graduate Medical Education. Tenth report, physician distribution and health care challenges in rural and inner-city areas. Rockville, MD: CGME, 1998.
10. Hart LG, Salsberg E, Phillips D, Lishner DM. Rural health care providers in the United States. The Journal of Rural Health 2002; 18(Suppl): 211-232.
11. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: An integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 503-504.
21. Worley P, Esterman A Prideaux D. Cohort study of examination performance of undergraduate medical students learning in community settings. BMJ 2004; 328: 207-209.
13. Kaufman A. Rurally based education: Confronting social forces underlying ill health. Academic Medicine 1990; 65: S18-S21.
14. Rourke JTB, Strasser RP. Education for rural practice in Canada and Australia. Academic Medicine 1996; 71: 464-469
15. Hays R. Rural initiatives at the James Cook University School of Medicine: A vertically integrated regional/rural/remote medical education provider. Australian Journal of Rural Health 2001; 9(Suppl.11): S2-S5.




