Introduction
There are differences around the world in terms of health systems and needs, but inadequate access to health care is common to rural areas globally. Internationally, countries face shortages of health professionals and resources as well as difficulties with transportation, and communication in rural areas1,2. Many rural people worldwide experience the associated factors of poverty, poor health and low productivity which may create a downward spiral into more of the same1.
In the USA, New Mexico is no exception. It is large and sparsely populated, and the need for health professionals is acute in rural counties3,4. Rural New Mexicans experience extensive rural poverty and lack health insurance5,6.
Interdisciplinary educational programs have been identified as a strategy to help students prepare for rural healthcare practice in many countries7-10, and reported results include greater confidence to work in rural settings, increased expectation to actively collaborate with other health professionals, and development of skills needed for rural health practice11-12. In addition, interdisciplinary training has been associated with improved communication with other health professionals, improved health outcomes for patients, and more satisfaction with work13,14.
In order to encourage and train health professional students for rural practice, the University of New Mexico Rural Health Interdisciplinary Program (RHIP) was established in 199115. The RHIP employs interdisciplinary problem-based learning (PBL) coupled with rural training. Rural educational experiences have been associated with choosing rural practice4,16. Interdisciplinary PBL has been used in a number of rural interdisciplinary training programs12,17 and identified as a potential method to teach respect and understanding of health professional roles, and facilitate development of team skills11,14,18,19.
RHIP program description
In RHIP, students from 12 health professional programs (nursing/nurse practitioners, dental hygiene, masters in public health, medicine, medical laboratory sciences, occupational therapy, pharmacy, physical therapy, physicians assistant, respiratory therapy, social work, and speech language pathology) work in interdisciplinary PBL groups on the University of New Mexico campus for 2 months. Teams are typically made up of 8-12 students, and they are formed around the seven community sites where the students will work later in the year. Teams typically consist of 1-2 students from 5-7 different professional programs (for example, a team might consist of one medical student, two pharmacy students, one nursing student, two physical therapy students, one medical laboratory science student, and one dental hygiene student). Medical students are in their first year of study. All other students are in their second or third year of study. Faculty members from different health professional programs work with each group.
Tutorial groups meet once a week for three hours at a time, and each case lasts for two sessions. The initial PBL case is developed and facilitated by faculty members so that students can become familiar with each other and the process. After receiving training in case development and facilitation, small interdisciplinary groups of 2-3 students within each team assume responsibility for writing and tutoring all of the following cases. Students report that actually writing the cases helps them to understand interprofessional rural practice more deeply, and that it facilitates development of teamwork competencies more strongly than if faculty members wrote and facilitated the cases. Cases are used once and then archived. Next, the students move to the rural sites for 2 months where they complete discipline-specific clinical rotations and also continue to meet once a week in half-day PBL tutorial sessions, using cases that they write based on their actual experiences.
Post-test RHIP evaluation results indicate that participants consistently demonstrate greater confidence and desire to work in rural settings as well as increased expectation to consult with other health professionals after completing the program11. Additionally, close to half of participants choose healthcare practice with rural and underserved communities on graduation20,21.
Student-developed PBL cases are a central educational method used in RHIP. Students may spend approximately 50-55 hours in interdisciplinary PBL sessions during the program. However, because each team develops its own cases, we have never described the content of the cases. This study was designed to analyze the actual content of the student-developed cases.
Methods
Cases and supporting documentation
This study was based on data from 222 PBL cases that were developed by RHIP students between 1991 and 2002. Cases had been stored in files from the inception of the program. Each case has a title page that includes the names, disciplines and rural site of the case writing team and an attendance list. Some cases included old handwritten notes from faculty and old case analysis forms that had been developed in the mid 1990s to start describing cases.
Case coding
The authors developed a research case analysis form to systematically record and code information designed to answer the research questions. This form was modified from old case analysis forms that had originally been developed but used inconsistently by the RHIP faculty over the years. The new form collected the following data for all cases: rural group identification by site; the professions of case authors and tutorial participants; client (case) demographics; health conditions; written case questions; and evidence of incorporation of case guidelines. The current new form was used to recode all cases, even if they had been coded previously using an old form.
Demographic information for the client in each case included age, gender, marital status, and ethnicity. In cases where some demographic information was not described, the category was left blank.
Health condition referred to the specific diagnosis and/or general conditions of the client in cases such as: heart disease, diabetes mellitus, accidents, psychological conditions etc. The coding form allowed for multiple health conditions for each client.
Case questions are actual questions written in the paper cases to generate group discussion and were categorized as: assessment (eg, 'what diagnostic test would you use?'); basic science (eg, 'what structures in the arm might have been damaged?'); professional role (eg, 'what role would your particular profession play in assessing this person?'); therapeutic process; psychological; public health; legal/ethical; financial; or cultural. Coders identified which types of written case questions were included in the cases.
Case guidelines
In 1996, faculty members developed a set of guidelines for students to adhere to in developing cases17. Students received instruction in using the guidelines to write effective cases. These guidelines reflected program objectives and all cases were expected to include the following dimensions:
- three or more health professions represented
- community issues/social aspects of health care discussed
- family and psychosocial issues identified
- cases include different stages of care
- prevention/health promotion topics addressed
Coders were asked to identify which guidelines were reflected in each case.
Coding reliability
Using the research case analysis form, the two researchers independently coded 10 randomly chosen cases. Areas of disagreement were discussed. Next, a different set of 50 randomly chosen cases were analyzed separately by the two researchers, and this time coding agreement was 95%. Again, areas of disagreement were discussed and clarified. Thereafter, every 10th case coded by the student researcher was reviewed by the faculty researcher to check coding reliability on an ongoing basis, and reliability during this phase was 98%. All data from the cases were entered into Microsoft Access. Descriptive statistics were used to analyze the cases and c2 analysis was used to determine significant differences.
Results
In order to determine how well the RHIP student-developed cases reflected New Mexican demographics and health conditions, we compared the individuals in the cases to health statistics for the state as described by the New Mexico Department of Health3.
Case demographics
Forty-eight percent of the individuals described in the cases were female and 52% were male. The age distribution in the PBL cases matched the age distribution of the New Mexico population, and there was case representation from early childhood to old age. Of the 108 cases in which marital status was identified, 50 were married, 15 were widowed, 10 were divorced, 3 lived with a partner and 30 were single. Ethnicity was described in 102 cases (46%). Table 1 describes ethnicity in the PBL cases compared with New Mexico statistics.
Table 1: Ethnicity distribution in 102 RHIP cases developed between 1991-2002 compared with New Mexico demographics for 2000*
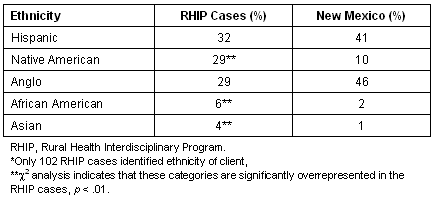
Case problems/conditions
We compared the top health problems of the PBL cases with the leading causes of death according to the NMDOH report for the year 2000. Causes of death are not synonymous with common causes of illness, but there was not a state list available identifying common causes of illness. Table 2 describes the percentage of cases with the most commonly described health conditions and also the leading causes of death in New Mexico. Most cases involved more than one health condition: 36 % of the clients in the cases had two conditions, 29% had three conditions, and 26% involved more than three health conditions.
Table 2: Comparison of the most common RHIP case conditions with the leading causes of death in New Mexico (in descending order of frequency)

Case questions
Case questions (written directly into the case) reflected the direction that case writers attempted to guide group discussion and development of learning issues. Table 3 lists the frequency of types of questions asked in the cases.
Table 3: Frequency of types of questions in cases (n = 222 cases)
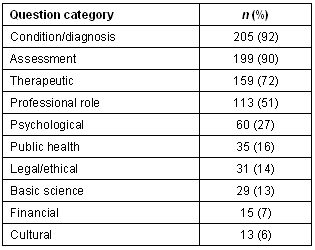
Case guidelines
As described earlier case development training for students included an emphasis on adherence to case guidelines. Table 4 describes the percentage of cases that reflected the different guidelines.
Table 4: Percentage of cases addressing each case guideline (n = 222 cases)
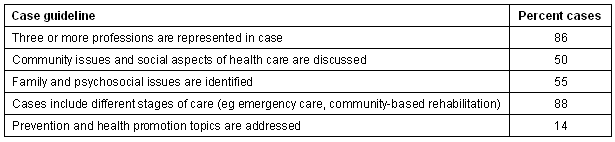
Discussion
Case demographics
Regional analysis of cases indicated that student-developed cases were strongly influenced by specific rural sites. For instance, the many Native American cases were developed by the groups that completed their rural rotations in the counties that border the Navajo reservation. Generally, site specific ethnicity analysis suggested that students created cases reflective of their actual experiences in actual geographic locations in rural New Mexico.
Health conditions
The students did not typically develop cases about people who died, so the conditions they described only partially matched the identified causes of death in New Mexico. It was clear that students wrote cases describing conditions typically treated by their professions (eg, the fact that 14% of all of the cases included dental concerns probably reflects the involvement of dental hygiene students in the RHIP). In addition, because of time limitations, students only completed four or five cases during the summer, so they were not able to develop cases to reflect all of the health conditions they encountered while working in the rural communities.
Co-morbidity has been described as common in rural communities6. However, no state statistics were available to actually describe the incidence of co-occurring conditions, making it impossible to compare student cases to the reality in rural New Mexico. The student emphasis on complex cases may reflect student experiences with rural health care, as well as the fact that RHIP was designed to emphasize multidimensional, interprofessional care. The fact that 14% of the clients in the cases had psychological concerns, 15% had substance abuse and 6% had physical abuse suggested that students were interested in exploring the complexity of health care concerns.
Case questions
The most frequently asked questions addressed knowledge of health problems and conditions, patient assessment, and professional roles in treating conditions. This suggested that the case writers actively encouraged discussion of a range of clinical concerns.
Case questions addressing broader healthcare topics including public health, ethical/legal, basic science, financial and cultural issues were less frequently asked in written form. This may reflect the student professions involved in RHIP. Student groups with masters in public health and social work students typically did ask questions that extended beyond narrowly defined medical concerns, and their cases tended to reflect a broader view of health issues, lending support to the suggestion that diverse student teams facilitate multidimensional healthcare discussion. However, since the health conditions described in Table 2 also include psychological and social conditions (eg, abuse), it is possible that group discussion did address a broader range of issues than the case questions might indicate.
Case guidelines
Student cases usually reflected guidelines concerning multiple stages of care and inclusion of three or more professions. Psychosocial concerns and community dimensions of care were addressed about half the time. Health promotion and prevention aspects of healthcare were rarely addressed. RHIP coordinates interprofessional learning, but does not dictate what students learn in their own professional programs. It is possible that health education/promotion and prevention are not well addressed in many of their discipline-specific curricula, or that students did not observe health promotion activities in their rural settings. It is also possible that the actual case discussion in the groups addressed more guidelines than could be determined from analyzing the paper cases retrospectively.
Conclusion
Challenges of the study
As a retrospective study that relied on the paper cases and supporting documentation, the analysis does not reflect actual tutorial discussions that typically lasted three to four hours per session. Groups may have verbally explored many related topics in great detail that could not be discerned from the paper cases alone. The complexity and nuances of group discussion were missing from our records.
Implications for health education
The current analysis suggests that the student-developed cases reflect rural New Mexico in terms of population demographics, and health condition complexity. To some extent they also reflect common health problems that they encounter in rural New Mexico. These findings lend moderate support to the theory that students can learn about relevant health conditions reflective of rural communities where they live and work by developing and discussing PBL cases.
In addition, the student-developed cases appear to offer opportunities to learn about multidimensional healthcare that requires interprofessional collaboration. However, it is not clear that the cases consistently facilitated discussion of non-clinical dimensions of healthcare (economics, legal issues etc), suggesting that students may have been conditioned to focus more on biomedical aspects of healthcare. Attention needs to be paid to strategies that encourage students to broaden their awareness of health issues. To some extent, the cases probably reflect the particular professions involved in the program. We need to actively recruit health professional students from programs such as public health, social work and law to raise non-medical issues in cases. In addition, faculty facilitators, case development training, and faculty modeling of cases are also factors that may have influenced case development and could be addressed directly.
The RHIP is popular with faculty and students alike, and this case analysis suggests that students can use PBL cases to explore certain aspects of rural healthcare. Student-centered PBL is adaptable, and interdisciplinary tutorials emphasizing rural practice could probably be creatively modified for application in a range of educational settings.
Acknowledgements
This work was supported in part by a grant from the Department of Health and Human Services, Health Resources and Services Administration, Bureau of Health Professions (USDHHS #5D35HP16001-12) to the University of New Mexico, School of Medicine in consortium with New Mexico Health Resources Inc. I would like to warmly thank Clark Hansbarger, MD for suggesting and initiating the analysis of RHIP cases many years ago.
References
1. Strasser R. Rural health around the world: Challenges and solutions. Family Practice 2003; 20: 457-463.
2. Strassser R. From Shanghai to Durban: International rural health conferences. Australian Journal of Rural Health 1997; 5: 165-168.
3. New Mexico Department of Health (NMDOH). New Mexico Selected Health Statistics. Santa Fe, NM: New Mexico Department of Health, 2000.
4. Hart LG, Lishner DM, Rosenblatt RA. Rural health workforce: Context trends and issues. State of the Health Workforce in Rural America: Profiles and Comparisons. Seattle, WA: WWAMI Rural Health Research Center, 2003.
5. Urbina C, Solan B, Counsellor A, Mines J, Serna L, Kalishman S. Where have all the students gone?: Retaining medical school graduates through educational innovations. Education for Health 2003; 16: 279-285.
6. Larson EH, Norris TE. Rural demography and the health workforce: Interstate comparisons. State of the Health Workforce in Rural America: Profiles and Comparisons. Seattle, WA: WWAMI Rural Health Research Center, 2003.
7. Revel T, Yussuf H. Taking primary care continuing professional education to rural areas: Lessons from the United Arab Emirates. Australian Journal of Rural Health 2003; 11: 271-276.
8. Dalton L, Spencer J, Dunn M, Albert E, Walker J, Farrell G. Re-thinking approaches to undergraduate health professions education: Interdisciplinary rural placement program. Collegian 2003; 10: 17-21.
9. McNair R, Brown R, Stone N, Sims J. Rural interprofessional education: Promoting teamwork in primary health care education and practice. Australian Journal of Rural Health 2001; 9: S19-S26.
10. Moorhouse C, Wilson C. Practical practice pointers: Learning together for remote area health care. Australian Journal of Rural Health 2004; 12: 223-236.
11. Geller ZD, Rhyne RL, Hansbarger LC, Borrego ME, VanLeit BJ, Scaletti JV. Interdisciplinary health professional education in rural New Mexico: A 10 year experience. Learning in Health and Social Care 2002; 1: 33-46.
12. Slack MK, Cummings DM, Borrego ME, Fuller K, Cook S. Strategies used by interdisciplinary rural health training programs to assure community responsiveness and recruit practitioners. Journal of Interprofessional Care 2002; 16: 129-138.
13. Institute of Medicine (IOM). Health professions education: A bridge to quality. Washington DC: The National Academies Press, 2003.
14. Hall P, Weaver L. Interdisciplinary education and teamwork: A long and winding road. Medical Education 2001; 35: 867-875.
15. VanLeit B. Interdisciplinary health professional education in the rural United States. World Federation Occupational Therapy Bulletin 2003; 47: 17-21.
16. McAllister L, McEwen E, Williams V, Frost N. Rural attachments for students in the health professions: Are they worthwhile? Australian Journal of Rural Health 1998; 6: 194-201.
17. Urbina C, Hess D, Andrews R, Hammond R, Hansbarger C. Problem-based learning in an interdisciplinary setting. Family and Community Health 1997; 20: 16-28.
18. Hughes L, Lucas J. An evaluation of problem based learning in the multiprofessional education curriculum for the health professions. Journal of Interprofessional Care 1997; 16: 77-88.
19. D'Eon MA. Blueprint for interprofessional learning. Journal of Interprofessional Care 2005; Suppl 1: 49-59.
20. University of New Mexico Health Sciences Center (UHMHSC). The Rural Health Interdisciplinary Program Executive Summary. Albuquerque, NM: University of New Mexico Health Sciences Center, 2004
21. Hansbarger C, Scaletti JV. Building interdisciplinary rural health education networks in New Mexico depends upon rural hospitals. Health Care Perspectives 2002: Winter: 12-15.

