Maintaining an adequate medical workforce in rural and remote northern Australian towns has been a challenge for many years1. To address this challenge, intern places and postgraduate training opportunities have slowly been expanded in northern Australia, although training is currently available locally in only a limited range of more generalist specialties. James Cook University (JCU) in regional north Queensland, the first new Australian medical school for a generation, enrolled its first intake in 2000 with a mission to select and educate medical graduates prepared to work as doctors in rural and remote locations2.
The JCU approach has been to combine a number of strategies shown to increase the likelihood of graduates working in rural and remote areas. Evidence shows a number of characteristics associated with increased likelihood of rural practice: rural origin at application3-5, providing early and repeated exposure to rural experiences during training4-7, and a preference for specialising in general practice7,8 and rural medicine9,10. Consequently, the JCU medical school draws students predominantly from northern Australian locations (70% of intake) and/or from outer regional, remote or very remote towns (66% of the total intake) classified using the Australian Standard Geographical Classification Remoteness Area (ASGC-RA) index11. Admission decisions are based on a combination of academic performance adjusted for rurality of prior education12, interview scores and scoring of a personal statement.
Successful applicants go on to experience significant rural exposure. Students undertake distributed rural clinical placements across the 6 years of the Bachelor of Medicine, Bachelor of Surgery (MBBS) degree in the second (4 weeks), fourth (8 weeks) and sixth year (8 weeks) of the course, with a significant proportion of these sites located in remote areas. In addition, approximately 60% of students move to clinical school sites in Cairns, Mackay and Darwin in years 4-6. This combination of rural medical education strategies has been shown to be associated with markedly different patterns of practice for JCU graduates compared to those from other Australian medical schools13,14. However, no study has yet investigated predictors of remote medical practice. This is a significant gap in the literature, as remote Australia has substantial deficits compared to metropolitan, regional and rural Australia in terms of health workforce and health indicators. Over three-quarters of Australia is classified as geographically remote. Smith et al (2008) note (p. 159): 'Remote areas are characterised by geographic isolation, cultural diversity, socioeconomic inequality, resource inequity, Indigenous health inequality and a full range of extreme climatic conditions.' These authors identified eight key features of remote medical practice: employment rather than private practice, isolation, use of telehealth, increased clinical acumen, extended practice, cross-cultural setting, multidisciplinary practice, and an emphasis on public health and personal security15. It seems clear that many remote communities have health needs that are not being met.
The comparative effect of the JCU program in promoting remote practice cannot be quantified without data from other Australian medical schools, which is limited. Therefore, this article explores the remote practice outcomes of JCU graduates through bivariate and multivariate analysis. These analyses identify specific subgroups and factors predicting JCU MBBS graduates (that is, graduates in the fourth to tenth year of post-degree training) working for at least 1 year in a remote practice location by collating data from their pre-medical school application, undergraduate experience, and postgraduate practice location and specialty training. Medical training at JCU involves a 6-year undergraduate degree which is then followed by a 1 year internship year and additional experience as a junior doctor or in postgraduate training for 3-6 years or longer.
This work is significant as a number of studies have evaluated the impact of rurally oriented programs at universities like JCU, the University of Queensland and the University of Western Australia13,14,16-18. While it is clear that some of these programs are meeting their aims of producing increasing numbers of graduates who are working in rural and remote locations, with concomitant growth in the rural workforce, it is important to consider whether all communities are benefiting from these initiatives. Specifically, the study investigates whether smaller, remote communities such as Cooktown (population 2339) and Mount Isa (population 22 013) - those with demonstrably the greatest need - benefit to the same extent as larger regional and rural locations on the east coast, such as Cairns (population 157 847) and Mackay (population 87 324) (estimated population at 30th June 2015, Australian Bureau of Statistics).
Design
In 2015, a cross-sectional analysis was undertaken of the JCU medical school's ongoing longitudinal tracking database to explore remote location of practice between PGY 4 and 10 for all JCU medical graduates (2005-2011 graduate cohorts). Only remote practice at PYG 4 and above was considered because graduates usually undertake their early vocational training in metropolitan or regional teaching hospitals, with fewer options to undertake this training in remote locations. Consent for graduate participation was obtained from an annual exit survey of final-year JCU medical students, which has been conducted for all graduating cohorts.
Participants and data sources
A total of 529 medical graduates were in the 2005-2011 graduating cohorts. A longitudinal profile of location for all postgraduate years was collated for each of these graduates. Medical school application and undergraduate data were retrieved from administrative databases held by JCU for the following variables: gender, ethnicity, home town at application, selection interview score, if awarded Honours (completed an Honours research project in last 2 years of course), if awarded a scholarship (includes 45 Medical Rural Bonded Scholarships, 26 Rural Australia Medical Undergraduate Scholarships and 46 Queensland Health Rural Scholarship Schemes (QHRSS); rural placement location (in ASGC-RA) in years 2, 4 and 6, and location of clinical school attended in years 5 and 6 (Townsville, Cairns, Mackay or Darwin).
Postgraduate location and specialist training data were accessed by contacting graduates directly through the personal email and mobile phone details provided as part of an exit survey of all final-year students, with additional practice location data sourced from a JCU Medicine Facebook page created specifically to maintain a current contact list for the longitudinal cohort study, and from the Australian Health Practitioner Regulation Authority website19. Combining these strategies, practice location data for the first seven graduating cohorts from PGY 4-10 was available for 529 of the total 530 (response rate of 99%). Postgraduate practice location data were then linked to individual student data.
Variables
The dependent variable was location of practice (Australian town) for each year of PGY 4-10, categorised into 'metropolitan'/'inner regional'/'outer regional' versus 'remote'/'very remote' based on the ASGC-RA classification11. The Australian Institute of Health and Welfare's ASGC-RA classification allocates locations to one of five categories ('major cities', 'inner regional', 'outer regional', 'remote' and 'very remote') to describe and represent remoteness from goods and services for any part of Australia based on road distance as a surrogate for remoteness, and on the population size of a service centre as a surrogate for the availability of services. Internship training location was similarly categorised using the ASGC-RA index. Postgraduate variables around specialty training were created by categorising graduates who had undertaken specific specialist training (eg rural generalist pathway, general practice, surgery including subspecialties, adult internal medicine including subspecialties) compared with graduates who had chosen other specialties or had not yet undertaken training.
Participant demographics recorded on the application forms were obtained from the student database held by the university, except for remoteness of home town at application, which was determined by categorising the location into either ASGC-RA 1-3 (non-remote) or ASGC-RA 4-5 (remote). Undergraduate variables regarding whether the student was awarded a scholarship or degree with Honours, and year graduated, were created directly from JCU medical school data sources. A complete list of the variables as they were considered for statistical analysis is in Table 1.
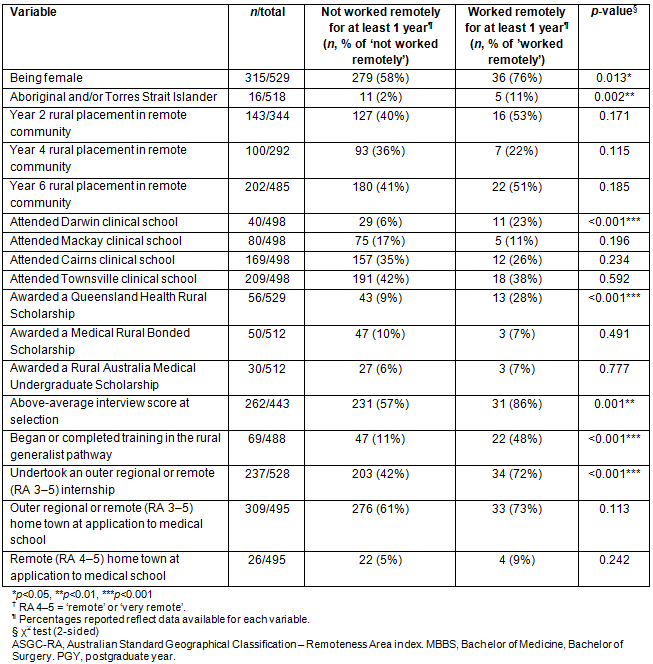
Table 1: Bivariate associations with 529 James Cook University MBBS graduates (PGY 4-10) undertaking at least 1 year of remote practice (ASGC-RA 4-5?)
Statistical analysis
Data were coded numerically and entered in the Statistical Package for Social Sciences v20 for Windows (SPSS; http://www.spss.com). Bivariate relationships between the dependent variable ('practised in remote ASGC-RA location for one year or more from PGY 4-10' - yes/no) and pre-medical, undergraduate training and postgraduate factors were assessed using two-tailed χ2 tests. Throughout the study, a statistical test was considered significant with p<0.05.
Data were analysed in two further ways: with multivariate (binary outcomes) logistic regression analysis and with explorative Classification and Regression Tree (CART) analysis (Fig1). The multivariate logistic regression analysis identified independent predictors of undertaking at least 1 year of remote practice location from PGY 4 to 10 and estimated their strength of association (Table 2). All variables in Table 1 were considered in the multivariate logistic regression analysis, but only independent significant predictors were accepted into the final model. Goodness of fit of the final logistic regression model was evaluated using the Hosmer-Lemeshow test and found to be p=0.881, indicating the model is a good fit for the data. Results of the multivariate logistic regression analysis are presented as prevalence odds-ratios (PORs) together with 95% confidence intervals (95%CI). PORs give an estimation of relative risk with fewer assumptions than are required for prevalence ratio analyses, and are the generally accepted measure of association used in cross-sectional studies to assess the strength of the relationship between study factor and outcome20.
CART analysis can statistically demonstrate those factors that are particularly important in a model, while visually presenting the data in a way that is easily interpreted by those not well versed in statistical analysis. A detailed explanation of CART analysis is described in the seminal paper by Breiman et al (1984)21. In this study, the CART analysis defined all statistically significant subgroups associated with remote practice. First the entire sample, and thereafter all newly defined subgroups, were investigated at every step of the analysis to determine which variable yielded the most significant subdivision into the group most strongly associated with practising remotely (Fig1). The CART procedure stopped when no further significant predictors were identified.
Table 2: Results of multivariate logistic regression analysis identifying predictors of James Cook University MBBS graduates (n=405?; PGY 4-10) practising for at least 1 year (n=35) in a remote town (ASGC-RA 4-5¶)
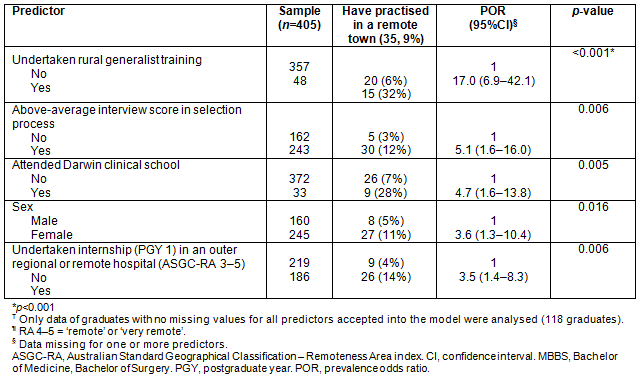
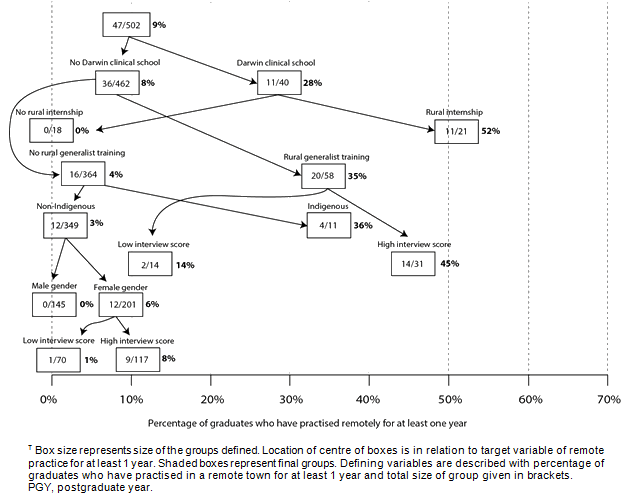
Figure 1: Result of Classification and Regression Tree analysis identifying 'risk' groups for 47 James Cook University graduates (PGY 4-10) who have practised in a remote town for at least 1 year (n=529).?
Ethics approval
Ethics approval for the tracking study was obtained in 2004 from the JCU Human Research Ethics Committee (# H1804).
Description
Forty-seven (9%) JCU MBBS graduates in the first seven cohorts had practised for at least 1 year in a remote location between PGY 4 and 10. Sixty percent of the 47 had spent more than 1 year in remote practice, with 17% spending 2 years, 21% spending 3 years, 10% spending 4 years, and the other 12% spending 5-8 years in remote practice. Remote practice sites in Queensland included Cooktown (4), Collinsville (1), Hughenden (2), Thursday Island (4), Palm Island (5), Kowanyama (1), Mount Isa (6), Weipa (2), Longreach (6) and Charleville (1); sites in Western Australia included Broome (4); and in the Northern Territory Katherine (1), Elcho Island (1), Alice Springs (5), Jabiru (1), Gove/Nhulunbuy (1) and Tiwi Islands (3). Five others were elsewhere in the country and in Antarctica.
Characteristics of the 529 JCU MBBS graduates in the analysis included median age at graduation 23 years (interquartile range 23-24 years), 315 (60%) female, 26 (5%) reporting an ASGC-RA 4-5 hometown at application, 56 (11%) awarded a QHRSS scholarship, and 16 (3%) of Aboriginal and/or Torres Strait Islander origin.
The number of students undertaking a placement in a remote town during years 2, 4 and 6 were 143 (42%), 100 (34%) and 202 (42%), respectively. The locations of clinical school attended in years 5 and 6 were Townsville (209; 42%), Cairns (169; 34%), Mackay (80; 16%), Darwin (40; 8%). Of the 529 graduates with remote practice location available for PGY 4-10, the most common specialty training undertaken was general practice (76; 16%) and the rural generalist subspecialty (69; 14%), with 237 (45%) having undertaken their internship in rural or remote hospitals (ASGC-RA 3-5).
Bivariate analysis
JCU MBBS graduates who had practised in a 'remote' location (ASGC-RA 4-5) from PGY 4 to 10 were significantly more likely than other graduates to: be female (p=0.013), receive an above-average score during the selection interview (p=0.001), be Aboriginal and/or Torres Strait Islander (p=0.002), be awarded a QHRSS (p<0.001), attend the Darwin clinical school in years 5 and 6 (p<0.001), complete their internship in a rural or remote hospital (p<0.001) and undertake training in rural generalist medicine (p<0.001) (Table 1).
Multivariate analysis
Multivariate logistic regression identified that the likelihood of JCU MBBS graduates practising in a 'remote' location from PGY 4 to 10 was predicted by undertaking rural generalist training (p<0.001; POR=17.0), being awarded an 'above average' interview score at medical school selection (p=0.006; POR=5.1), attending the Darwin clinical school in years 5-6 (p=0.005; POR=4.7), being female (p=0.016; POR=3.6) and undertaking an outer-regional or remotely based internship (p=0.006; POR=3.5) (Table 2).
CART analysis
Attending the Darwin clinical school (dichotomous yes/no) showed the strongest significant bivariate relationship with JCU graduates PGY 4-10 practising in a remote town for at least 1 year, in the first step of the CART analysis based on the entire sample of 529 graduates (Fig1). Following the CART procedure, the sample was then further split into subsets based on the strongest significant bivariate relationship with graduates who practised in a remote location. One subset of graduates who attended the Darwin clinical school was further identified as having the highest likelihood of practising remotely: graduates who also went on to undertake a rurally based (ASGC-RA 3-5) internship (11/21; 52%).
For the subset of graduates who did not attend the Darwin clinical school, several further groups were identified as high likelihood for remote practice: graduates who had undertaken rural generalist training after graduation (20/58; 35%), in particular, if they had an above average interview score (14/31; 45%); Aboriginal and/or Torres Strait Islander graduates (4/11; 36%); and female graduates (12/201; 6%), in particular, if they were awarded a 'better than average' interview score during the medical school selection process (9/117; 8%).
Discussion
This is the first longitudinal study to identify contextual and professional factors that are associated with choice of early- to mid-career remote practice location for medical graduates from a rurally oriented Australian medical school. The significant factors identified in this study for practising in a remote location postgraduation included being awarded an 'above average' interview score at medical school selection, attending the Darwin clinical school, undertaking an outer-regional or remotely based internship, undertaking rural generalist training, being female, and identifying as Aboriginal and/or Torres Strait Islander. While perhaps lower than expected, the percentage of JCU graduates working remotely each year (3%) is several times more than the percentage of all Australian medical graduates working remotely each year, as described by the National Health Workforce Dataset for 201422, and very similar to the overall percentage of the Queensland population who live remotely (3%)23.
Most of these factors could be considered components of a 'pipeline to remote medical practice' for medical graduates from JCU (and elsewhere): selecting students with motivation, experience and attributes for remote practice, and then providing them with remotely based undergraduate experiences and later regionally based internships and/or rural generalist training. The association between remote practice and the JCU selection process for medical applicants, attending the geographically remote Darwin clinical school and undertaking rural generalist training in Queensland indicates the importance of providing motivated graduates with access to medical career pathways and experiences that align with the needs and practice requirements of remote Australia. Indeed, with the JCU medical school having only produced 11 cohorts so far, and the Queensland rural generalist pathway only established a decade, it could be argued that the full impact of this successful partnership on remote practice in northern Australia is yet to be felt24.
While the regionally located Mackay, Cairns and Townsville clinical schools were not shown to be significantly associated with remote practice, these sites are valuable in allowing students to rotate through satellite rural and remote clinical sites. Previous analysis has demonstrated that students based in these clinical school sites have greater recruitment and retention back to these regions after graduation25.
The JCU medical school has more recently built upon this regional and remote training pipeline by establishing the Northern Clinical Training Network (NCTN) and 'Generalist Medical Training' (GMT) programs. The NCTN aims to develop career and training pathways to postgraduate practice in a range of specialties across the region. GMT, which commenced operations in January 2016, provides postgraduate education and training for doctors in general practice and rural medicine as part of the Australian general practice training program for all of Queensland except the south-east. With a footprint covering the majority of rural and remote Queensland, GMT aims to better connect the training pipeline from medical school to a career in general practice, with a special emphasis on remote and underserved communities.
It also appears that other characteristics may predict remote practice in JCU graduates. Being awarded a 'better than average' interview score during the selection process into medical school was the second highest predictor of JCU graduates later practising remotely. The JCU medical program selection process scores an applicant's interest in rural, remote and Indigenous health, and their pre-medical skills in self-reliance, communication and teamwork - all attributes appropriate for rural and remote practice. Temperament characteristics have previously been associated with rural practice, with Eley et al (2009)26 using the Temperament and Character Inventory27 to show rural GPs had greater enthusiasm for 'testing the unknown' (high novelty seeking) and higher self-reliance and confidence in the face of uncertainty (low harm avoidance) than urban GPs. These emerging findings suggest other Australian medical schools could increase the proportion of graduates interested in rural and remote practice by implementing selection processes that place weight on attributes such as high novelty seeking, low harm avoidance and good communication and teamwork skills, as well as motivation for remote practice.
This study also identified an association between cultural background and remote practice. While Aboriginal and/or Torres Strait Islander students are selected in similar proportions into the JCU medical course from rural and urban areas (p=0.725), it is possible that the exposure to remote communities across the 20 weeks of mandatory placements and the curriculum emphasis on rural, remote, Indigenous and tropical health motivates Aboriginal and/or Torres Strait Islander graduates to take up opportunities to work to address Indigenous health disadvantage in remote Australian communities. The University of Western Australia's medical school, which has a significant Aboriginal health undergraduate curriculum, also found many students intended to work in rural areas to help improve Aboriginal peoples' health28.
The finding that female JCU medical graduates are more likely to practise remotely is also quite interesting, as several studies show males are more likely to enter rural practice29,30, and five studies found rural GPs were more likely to be male31. Future studies will explore this area further, but the CART analysis findings (Fig1) suggest this may be related to the JCU medical selection process leading to a higher proportion of female applicants being chosen with a strong interest in remote Australian practice, as the overwhelming majority of female graduates who have gone on to practise remotely received an 'above average' score for their selection interview. Other factors could include more supportive work environments in remote Queensland, such as equipment and systems in the practice facility, and the strength and experience of the local medical and allied health team.
The JCU medical school has a social accountability mandate. One aspect of this mandate is to ensure the student body reflects the population profile of the northern Australian region the school serves. Together with the workforce evidence supporting the outcomes of such strategies, this enables the school to preferentially select Aboriginal or Torres Strait Islander applicants, applicants from rural or remote northern Australia, and applicants who score highly for motivation for rural, remote and Indigenous health practice, self-reliance, communication and teamwork skills. Thus, the findings of this study suggest the school's preferential selection process has increased the percentage of JCU medical graduates who have gone on to practise in remote settings.
Limitations
The study has several limitations. Postgraduation factors known to influence remote practice, such as access to professional development, peer support, partner with a rural background or openness to remote living and adoption of lifestyle/integration into a remote community6,29, could not be obtained for inclusion in the analysis. The multivariate analysis also calculated predictors of practice location only for PGY 4-10 - a graduate's early to mid-career. Practice location from PGY 11 onwards may be more appropriate for showing factors associated with a long-term remote medicine career, and this will be investigated in time.
The new JCU medical school has produced 47 graduates who have practised in remote areas during their early career. While perhaps lower than expected, the percentage of JCU graduates working remotely each year (3%) is several times more than the percentage of the Australian medical graduates working remotely (1%), and similar to the overall percentage of the Queensland population living remotely (3%). This study provides the first Australian evidence that likelihood of early-career remote medical practice is enhanced by investment in a 'remote pipeline' - remotely based medical education via 'remote' clinical schools and the rural generalist pathway.
In addition, the JCU medical school's social accountability mandate to ensure the student body reflects the population profile of northern Australia has increased selection of Aboriginal and Torres Strait Islander applicants and also applicants who score highly for motivation for rural, remote and Indigenous health practice, self-reliance, communication and teamwork skills. This preferential selection process may have increased the percentage of JCU medical graduates who have later practised remotely. However, while there are some encouraging results in terms of rural training and outputs from the JCU medical school, not all remote communities in northern Australia are yet benefiting; thus, a more nuanced approach tailored to those communities most in need may be required.
Acknowledgements
The authors would like to gratefully acknowledge the efforts of all JCU medical graduates who consented to be contacted for this longitudinal study, and Dr Louise Young for contributing to the scholarship of the manuscript.
References
1. Ricketts TC. The changing nature of rural health care. Annual Review of Public Health 2000; 21: 639-657. https://doi.org/10.1146/annurev.publhealth.21.1.639
2. Hays RB, Stokes J, Veitch J. A new socially responsible Medical School for regional Australia. Education for Health 2003; 16(1): 14-21. https://doi.org/10.1080/1357628031000066613
3. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health (Internet) 2003; 3(1): 212. Available: www.rrh.org.au (Accessed 18 April 2016).
4. Orzanco MG, Lovato C, Bates J, Slade S, Grand'Maison P, Vanasse A. Nature and nurture in the family physician's choice of practice location. Rural and Remote Health (Internet) 2011; 11: 1849. Available: www.rrh.org.au (Accessed 18 April 2016).
5. Brooks RG, Walsh M, Mardon RE, Russel E, Lewis M, Clawson A. The roles of Nature and Nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798. https://doi.org/10.1097/00001888-200208000-00008
6. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health (Internet) 2009; 9(1): 1083. Available: www.rrh.org.au (Accessed 18 April 2016).
7. Stagg P, Greenhill J, Worley PS. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health. (Internet) 2009; 9: 1245. Available: www.rrh.org.au (Accessed 18 April 2016).
8. Horner RD, Samsa GP, Ricketts TC. Preliminary evidence on retention rates of primary care physicians in rural and urban areas. Medical Care 1993; 31(7): 640-648. https://doi.org/10.1097/00005650-199307000-00006
9. Pathman DE, Steiner BD, Jones BD, Konrad TR. Preparing and retaining rural physicians through medical education. Academic Medicine 1999; 74(7): 810-820. https://doi.org/10.1097/00001888-199907000-00016
10. Rosenthal TC, McGuigan MH, Anderson G. Rural residency tracks in family practice: graduate outcomes. Family Medicine 2000; 32(3): 174-177.
11. Australian Bureau of Statistics. ASGC Remoteness Classification: purpose and use. Census paper # 03/01. Canberra: Commonwealth of Australia, 2003.
12. Hays RB, Bower AJ. Modifying academic ranking of rural and remote medical school applicants. Medical Journal of Australia 2001; 174(7): 371-372.
13. (Accessed 18 April 2016) Sen Gupta T, Murray R, Hays R, Woolley T. Rural medical education promotes rural medical career intentions and internship choices: a comparative outcome survey of a regional Australian medical school. Rural and Remote Health (Internet) 2013; 13: 2313. Available: www.rrh.org.au.
14. (Accessed 18 April 2016)Sen Gupta T, Woolley T, Murray R, Hays R, McCloskey T. Positive impacts on rural and regional workforce from the first seven cohorts of James Cook University medical graduates. Rural and Remote Health (Internet) 2014; 14: 2657. Available:www.rrh.org.au (Accessed 18 April 2016).
15. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P, et al. Defining remote medical practice. A consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 159-161.
16. Kondalsamy-Chennakesavan S, Eley DS, Ranmuthugala G, Chater AB, Toombs MR, Darshan D, et al. Determinants of rural practice: positive interaction between rural background and rural undergraduate training. Medical Journal of Australia 2015; 202: 41-45. https://doi.org/10.5694/mja14.00236
17. Rabinowitz HK. Relationship between US medical school admission policy and graduates entering family practice. Family Practice 1988; 5(2): 142-144. https://doi.org/10.1093/fampra/5.2.142
18. Playford DE, Nicholson A, Riley GR, Puddey IB. Longitudinal rural clerkships: increased likelihood of more remote rural medical practice following graduation. BMC Medical Education 2015; 15: 55. https://doi.org/10.1186/s12909-015-0332-3
19. Australian Health Practitioner Regulation Authority (AHPRA). Registration. (Internet). Available: http://www.ahpra.gov.au/Registration.aspx (Accessed November 2012).
20. Pearce N. Effect measures in prevalence studies. Environmental Health Perspectives 2004; 112(10): 1047-1050. https://doi.org/10.1289/ehp.6927
21. Breiman L, Friedman JH, Olshen RA, Stone CJ. Classification and regression trees. Belmont, California: Wadsworth International, 1984.
22. Australian Institute of Health and Welfare. National Health Workforce Dataset. Dynamic data display: Australia's registered health workforce by location (2014 medical practitioner data). (Internet). http://www.health.gov.au/internet/main/publishing.nsf/Content/health_workforce_data) (Accessed 18 April 2016).
23. Australian Bureau of Statistics. Australian Social Trends, 2008. Catalogue no. 4102.0. (Internet) 2008. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4102.0Chapter3002008 (Accessed 25 August 2016).
24. Sen Gupta T, Manahan D, Lennox D, Taylor N. The Queensland Health Rural Generalist Pathway: providing a medical workforce for the bush. Rural and Remote Health. (Internet) 2013; 13: 2319. Available: www.rrh.org.au (Accessed 25 August 2016).
25. Woolley T, Sen Gupta T, Murray R. James Cook University's decentralised medical training model: an important part of the rural workforce pipeline in northern Australia. Rural and Remote Health (Internet) 2016; 16: 3611. Available: www.rrh.org.au (Accessed 25 August 2016).
26. Eley D, Young L, Przybeck TR. Exploring the temperament and character traits of rural and urban doctors. Journal of Rural Health 2009; 25(10): 43-49. https://doi.org/10.1111/j.1748-0361.2009.00197.x
27. Cloninger CR, Przybeck TR, Svrakic DM, Witzel RD. The temperament and character inventory: a guide to its development and use. St Louis, MO: Center for Psychobiology of Personality, Washington University, 1994.
28. Paul D, Carr S, Milroy H. Making a difference: the early impact of an Aboriginal health undergraduate medical curriculum. Medical Journal of Australia 2006; 184(10): 522-525.
29. Lindsay S. Gender differences in rural and urban practice location among mid-level health care providers. Journal of Rural Health 2007; 23(1): 72-76. https://doi.org/10.1111/j.1748-0361.2006.00070.x
30. Shannon CK. A gender-based study of attitudes and practice characteristics of rural physicians in West Virginia. WV Medical Journal 2006; 102(6): 22-25.
31. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284. https://doi.org/10.1111/j.1440-1584.2003.00534.x



