Introduction
The same technology that is commonly used for university educational applications has the potential for bridging the urban-rural divide for the benefit of new and continuing health professions education1,2. The use of interactive and Internet-streamed video provides opportunities for professionals' education when working in rural and remote areas anywhere in the world. As shown (Fig 1), based on a bibliographic search of the Telemedicine Information Exchange (TIE), the use of this technology has grown rapidly3. Only 53 articles on distance-delivered health professional education (using various search terms) were published between 1985 and 2004 with the majority of applications for new education4. A few discuss distance delivery for education and specifically continuing-education (CE) applications5-9. This is curious, because nearly every telehealth program listed at TIE reports that they provide CE and continuing medical education, while a simple internet search reveals the frequent use of distance-delivery methods for CE. Perhaps those doing distance education as part of their health education programs do not consider it worth documenting. However, this lack of literature may have negative, unintended consequences. Even as the practice appears to be common, at least some funders seem reluctant to support it.
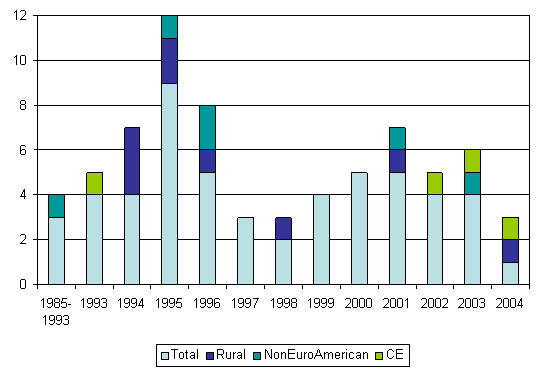
Figure 1: Distance education in telehealth articles, 1985-2004. CE, Continuing education.
This brief communication reports on one program's education applications through Telehealth Idaho of which the CE program called Virtual Grand Rounds (VGR) forms the cornerstone. The purpose of Telehealth Idaho is to improve healthcare access and quality and to serve as a telehealth resource center. To accomplish these goals, we needed to:
- increase the workforce size
- extend the reach of the existing workforce
- preserve the existing workforce.
Extending the workforce is accomplished with methods typically thought of as telemedicine, supervision, consultation, and home health. We worked to preserve the workforce through improving professional quality of life 10.
Increasing the workforce through new and CE was more perplexing. Ultimately, we developed a bifurcated but complementary educational program that included two types of education: (i) continuing; and (ii) new and 'upgraded' education. CE is that associated with ongoing training in a particular field, new training is training in a new field, upgraded training allows a person to increase their level of expertise within a field.
Methods
Historically, new education programs have been guided by general educational applications rather than telehealth applications. Many are affiliated with academic departments and use the university's distance-education center-which incorporates electronic classrooms equipped with two cameras, document cameras, large monitors and ISDN dial-up and Internet2 connections-for their broadcasts. Our CE programs, like VGR, have been run through our telehealth programs office, and range in their technology from utilizing the university distance-education system to point-to-point videoconferencing passing over private or public networks, to Internet-based videostreaming. On some occasions, ISDN dial-up connections are used. The typical number of locations for a live videoconference is six with a maximum of 42. In the case of the larger videoconferences, we utilize multiple bridges, each rebroadcasting to multiple sites. This prevents the entire conference from collapsing if problems occur, and allows us to redirect the video signal around the trouble site with minimum disruption.
Telehealth Idaho participants include Idahoans interested in new or CE. Between October 2001 and May 2004 approximately 2500 attendees accessed our educational opportunities. Most attendees live and work in rural areas, and just over half (57%) work in hospitals. Participants come from all types of professional backgrounds, primarily nurses (25%) and health administrators (23%). In all, participants represent over 25 health professions as well as school personnel, community administrators, public safety personnel, and interested consumers.
Discussion
Continuing education
VGRs, delivered by statewide interactive videoconference, are our primary CE vehicle. Because we do not require unique identifiers for participation, we can only estimate an unduplicated count of 1000 people based on Web registration and other identifiers such as CE sign-in sheets. Participants provide identifying information in proportion to the educational credit they seek: university course credit, certified CE such as APA-approved CE, or a certificate of attendance. Similarly, costs are associated with credit sought. There is no charge for participants' certificate of attendance while those seeking specific credit are charged rates commensurate with the certifying organization. All participants have the opportunity to provide anonymous course feedback and research information.
Because VGR faculty can originate from their home institutions, we are able to offer rural providers expert, up-to-date information from around the world. Between October 2001 and May 2004, we delivered 3910 person hours of CE in 42 VGR sessions at up to 21 locations8. Topics included aging, traumatic brain injury, older-adult and children's mental health, and nursing home care.
Evaluation data are at the core of the program's ongoing success; we have collected 1726 post-session evaluations (70% response rate) in which presenters and participants consistently respond positively. The overall satisfaction rating averaged 4 on a 5-point scale and participants estimate the likelihood of the information changing their practice at 3.8 on a 5-point scale. Participants also believe that the educational methods will assist them in understanding technology changes in their field. As one participant said, 'I think that we are getting ready for this technology and I, personally, am ready!'.
New and upgraded education
Another aspect of Telehealth Idaho's education programs involves courses taught with a combination of face-to-face and videoconference technology methods to high school, undergraduate, and graduate students. Between 2002 and 2004, 59 high school students enrolled in the certified nursing aid program and completed the university's 'Introduction to Telehealth Equipment Management' course. In addition to being an early infusion model for telehealth, the course allows students to develop a relationship with local health professions training institutions, encouraging them to train locally rather than potentially losing them to urban centers.
Two additional telehealth university courses were created in which 19 undergraduate and 15 graduate students enrolled. Other courses are delivered directly from rural communities. At Bear Lake Memorial Hospital (Bear Lake, population 574) 42 students participated in an online Certified Nursing Aid program. In this example of 'upgraded education', licensed practical nurses were pursuing their Associate Degree Registered Nurse.
Conclusion
Distance-delivered health professions education links rural communities with universities from which training and research originates. This bi-directional dialogue improves opportunities for health professionals to access knowledge and universities' ability to produce knowledge that is appropriate and useful for rural health professionals. This educational methodology appears to be quite common, yet documentation of educational activities associated with telehealth programs is at best scarce, which may inhibit field growth and even funding. However, based on the number of participants in Telehealth Idaho, and on the number of telehealth programs that offer distance-education opportunities, participants are likely to continue seeking educational opportunities through telehealth programs and would benefit from ever-evolving quality of technology and content.
Acknowledgements
This project was supported by grant # 1 D1B TM 00042-01 from the Department of Health and Human Services (DHHS) Health Resources and Services Administration, Office for the Advancement of Telehealth. The contents are the sole responsibility of the authors and do not necessarily represent the official views of DHHS.
References
1. President's New Freedom Commission on Mental Health. Achieving the Promise: Transforming Mental Health Care in America. A final report. DHHS Pub. No. SMA-03-3832. Rockville, MD: DHHS, 2004.
2. Stamm BH. Bridging the rural-urban divide with telehealth and telemedicine. In: BH Stamm (Ed.). Rural Behavioral Health Care. Washington, DC: American Psychological Association Press, 2003.
3. Telemedicine Information Exchange. (Online) 2005. Available: http://tie.telemed.org/ (Accessed 26 July 2005).
4. Kearns RC, Thompson NA. The reality of virtual learning for nurses in the largest integrated health care system in the nation. Nursing Administration Quarterly 2003; 27: 41-57.
5. Ellis DG, Mayrose J. Emergency telemedicine at the State University of New York at Buffalo. Telemedicine Journal and e-Health Spring 2003; 9: 73-79.
6. Laochamroonvorapongse D, Johnson E, Foong HB, Elpern DJ. A brave new world: Virtual grand rounds in dermatology. Seminars in Cutaneous Medicine and Surgery 2002; 21: 232-236.
7. Ruskin KJ, Palmer TE, Hagenouw RR, Lack A, Dunnill R. Internet teleconferencing as a clinical tool for anesthesiologists. Journal of Clinical Monitoring and Computing 1998; 14: 183-189.
8. Weeg SC, Stamm BH, Cutler K, Cunningham BJ. What can we do for continuing education for rural health professionals? Virtual grand rounds. Telehealth Practice Report 2004; 9(3): 3,8.
9. Witherspoon JP, Johnstone SM, Wasem CJ. Rural telehealth: Telemedicine, distance education and informatics for rural health care. Boulder, CO: WICHE Publications, 1993.
10. Stamm BH. Measuring compassion satisfaction as well as fatigue: developmental history of the compassion fatigue and satisfaction test. In: CR Figley (Ed.). Treating Compassion Fatigue. New York: Brunner/Routledge, 2002; 107-119.

