Context
While research remains the foundation of academic medicine, medical school curricula provide few opportunities for students to develop research skills and to participate in research. A MEDLINE search combining the terms 'research' and 'students, medical' yielded 119 articles, of which only a few described elective research preceptorship programs for medical students. Of note, when 'rural' was added to the search, there were no matches. There are few reported student research initiatives that focus on rural medicine research1,2.
Outside academic centres, few physicians are actively involved in research. In rural areas, even physicians with research ideas and inclinations may be put off by barriers such as lack of skills, support and time to do research. Students may see rural practice as offering challenging and exciting clinical work, but little opportunity to be involved in research. The tremendous potential for rural practice and rural population community-based research has generally been unrecognized and underdeveloped. A search of the medical literature for programs involving medical students doing rural research found little. One article has been published describing medical student rural research electives with a group of physicians in one community2. Another paper describes medical student summer placements in clinical settings with underserved populations, both urban and rural, with a goal to solve a problem identified by the communities1. The current article describes a unique Rural Summer Studentship Program developed at the Schulich School of Medicine & Dentistry at The University of Western Ontario, that combines student research and clinical learning which has, to date, involved 44 students in 20 communities.
Program description
Goals:
- to develop student knowledge and interest in rural and regional medicine
- to encourage medical students to undertake rural healthcare research
- to develop rural preceptors' research and teaching roles.
Strategies:
- facilitate practical research for students (and preceptors) to learn basic research project design and ethics, conduct and analysis, and reporting
- facilitate practical rural clinical learning with a focus on students' areas of interest
- increase rural preceptors' research and teaching by providing a medical student/researcher
The University of Western Ontario (Western) medical school, now known as the Schulich School of Medicine & Dentistry, was established in 1878. It recently has increased from 100 to 133 undergraduate medical students per year, most of whom have completed a minimum of a 4-year university degree prior to entry to the undergraduate medicine program. Western is located in London, a city of 350 000 in the heart of Southwestern Ontario. This region of Ontario that stretches from Tobermory to Pelee Island, has a population of 1.4 million. Forty percent of the population lives in communities of less than 10 000 people, thus making these communities rural but not remote. In 1997, The University of Western Ontario integrated rural medicine into its medical school curriculum to better reflect the realities of this region. Exposure to rural education begins in first year and extends throughout a student's medical education, at both the undergraduate and postgraduate levels. The Southwestern Ontario Rural Medicine Education, Research, and Development Network (SWORM) began in 1997 as the rural medicine unit of the Faculty of Medicine and Dentistry at The University of Western Ontario. As part of the rural-oriented undergraduate medical curriculum at Western, SWORM developed an elective Rural Summer Studentship Program (RSSP). SWORM has now been integrated into SWOMEN (Southwestern Ontario Medical Education Network)3.
Coordinated and supported by SWORM, the Rural Summer Studentships were developed as a partnership between Western, medical students, physicians, and community hospitals in Southwestern Ontario. Rural Summer Studentships have been offered to 10-12 students each year since 1999 on a competitive basis (based on project proposal and relevance to student's educational goals). Studentships are eight-week summer jobs, held during summer vacation following first or second year. Students are placed in small and mid-sized communities where they have an opportunity to perform rural health research combined with clinical experience. They receive a stipend at the level of a summer research grant, a small travel stipend, and coverage of liability insurance (because the studentships were not considered part of the core curriculum). In 2004, this was changed to a non-credit summer elective course that included liability coverage, and the students paid a minimal administrative fee. A small stipend is allocated to the supervising physician. The majority of funding is provided by the Province of Ontario's Ministry of Health and Long Term Care. A generous donation in memory of Dr Charles Drake funds additional students each year. The Change Foundation provided funding for additional studentships in 2001 and 2002 for medical students to help rural doctors integrate palm-top evidence-based medicine information technology into their practices.
Students traditionally have either conceived their own projects under physician supervision or worked on a physician-initiated research project. Projects are now required to go through the Ethics Review Board process. Following completion of the studentship, students are required to submit a report in manuscript format, suitable for submission to a peer-reviewed journal, as well as to complete a questionnaire evaluating their experience and the program. Examples of RSSP projects are listed (Table 1). SWORM (now SWOMEN) provides coordination, support and supervision of the RSSP projects. This includes research assistance with project design, the Ethics Review Board process, statistical analysis, and manuscript and poster presentation.
Table 1: Examples of rural summer studentship projects

From 1999 to 2003, inclusive, 44 students have participated in more than 20 communities with over 30 preceptors and 49 projects. Fifty-seven percent of the projects were supervised by family physicians. The other preceptors were mainly community specialists such as general surgeons, and general internists. A few preceptors were outreach specialists based in London, such as ophthalmologists who run rural clinics and perform operations, and nephrologists involved in clinical and research follow up of a major rural water-contaminated community.
Preliminary evaluation
At the end of medical school, students (Meds 2002 and 2003) were given an exit questionnaire to evaluate many different aspects of their medical education, including the rural/regional medicine components. Twenty of the medical students who graduated in 2002 and 2003 had perfomed RSSP (including three students who were funded to participate in the Change Foundation rural information technology project); 19 of those completed the questionnaire component about RSSP. They reported that their Rural Summer Studentships had increased their knowledge of rural/regional medicine, increased their interest in rural/regional practice as a career, and they found it a valuable learning experience (Fig 1).
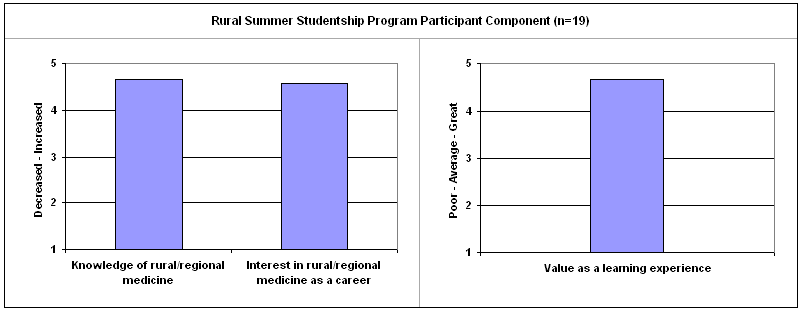
Figure 1: Medical school exit survey graduating class 2002 and 2003.
In the summer of 2002, Alexandra Zorzi (Meds 2005) completed an in-depth evaluation of the RSSP program as her RSSP project. This also included compiling all the RSSP projects as a resource for students and faculty.
In order to better assess the impact of the RSSP program on the participants' subsequent medical education at UWO, Ms Zorzi developed a new evaluation questionnaire. Its focus was to determine whether or not this program was a valuable education tool, and if it had any influence on students' attitudes toward rural medicine. Current participants and students who previously participated in the RSSP were emailed the evaluation questionnaire. Completed questionnaires were received from 22 students. Data were analyzed by calculating mean per question, where questions used the Likert Scale rankings. Open and closed ended questions were also used to qualitatively assess areas of improvement and student suggestions/impressions of the program.
Twenty-three percent of respondents spent their adolescent years in rural areas, that is a population of less than 10 000. Thirty-six percent of students who participated in the RSSP were from large urban cities (population > 500 000). By comparison, approximately 10% of the graduating class of 2002 were of rural background.
Table 2 shows the students evaluated the RSSP learning experience very positively. The data in Table 3 show a trend towards an increase in knowledge about, and interest in, rural medicine. This is consistent with the preliminary evaluation data in Figure 1.
Table 2: Rural Summer Studentship learning experience (n = 22)

Table 3: Retrospective student self assessment of knowledge and interest (n = 22)

Student responses to 'Comments and suggestions' were overwhelmingly positive.
The success of this program as indicated by its participants can only be viewed as a commendation to SWORM as it is its mission to advocate rural medicine through education, research and development. The fact that this goal is being achieved in the eyes of students is all the more important as it is through the education of future physicians that the greatest impact on healthcare reform will be felt. (Alexandra Zorzi, Meds 2005, RSSP student 2002).
Some examples of student comments are listed below3,4.
It's been a great experience. More and more it's confirming my desire to do rural family med/ER. I guess that's the point of the program, so I just want to let you know that it's working.
Without a doubt, the Rural Summer Studentship program gave me a new perspective in the various areas of medical care and how they are more challenging and exciting in a rural community.
Overall, I am having a great experience, gaining insight into the machinations of hospital bureaucracy, development and implementation of a research plan and exposure to a variety of areas in clinical medicine. Thank-you for your support in this area - it is a great help for those who participate in the Rural Summer Studentship program.
Limitations
Three factors, in particular, suggest some caution should be used in interpreting these findings: the small numbers of participants, the response rate, and the reliance on student self-reports.
This preliminary evaluation was done as a part of an 8-week rural summer studentship program. This was a narrow window of time for the survey to be developed, sent out, returned, and analyzed. This made it difficult to contact all of the previous RSSP participants, particularly as many were scattered geographically and at various stages of their training and/or summer holidays. Despite these constraints, the common trends observed in the preliminary evaluation and both the quantitative and qualitative data in this study give substantial support to the veracity of the positive trends observed.
Discussion
A similar medical school student summer research program successfully involving a group of physicians and one community has been described in Northern Ontario2. The model developed at The University of Western Ontario has involved more than 20 communities, over 30 physician preceptors and 44 students over a five-year time period. This shows that summer student electives combining research and rural clinical learning can be successfully developed on a larger regional scale.
Research assistant support in the early design phase of projects and the Ethics Review Board process was vital, because most of the students and rural preceptors had little experience in this regard. It is important that the projects be practical and do-able within the limit of an 8-week summer studentship time. Research assistant support was similarly helpful in statistical analysis and manuscript preparation of the projects. We found it useful to have both spring and summer workshops for the participants. The Assistant Dean for Rural and Regional Medicine/Director of the SWORM program was also involved at this critical stage, and throughout the process, as overall supervisor and principal investigator role.
The student comments provided in the qualitative section of the evaluation were overwhelmingly positive, but also included some constructive feedback which has been used to improve the program. The 8 weeks of the rural summer studentship is a serious time limitation for all RSSP. The application and acceptance process has been streamlined to avoid the students' exam times and provide greater preparation time in the spring for students to fully develop the projects prior to their eight-week summer studentship. This was also necessary so project designs could be completed in order to go through the ethics review process prior to the start of the eight-week summer studentship. Some students have completed their projects in the second summer, which reduces the time pressure effects dramatically.
The effectiveness of the program was reflected in the students' positive perception of their learning experience including knowledge of rural medicine and patient care, as well as project-specific knowledge. In their opinion, this program provided a valuable opportunity for learning in their medical education, both clinically and academically. Students also reported the program stimulated interest in rural medicine. Their practical learning about research, as well as clinical experience, will be of value in whatever field of medicine they choose. The opportunity for students to be involved in RSSP projects with rural specialists, as well as rural family doctors, gave students a broader choice of experience and potential career influence.
Already two students have had their research published in peer reviewed journals and six have presented at major conferences. Many more have presented at local or regional conferences. This is a major accomplishment, not only with respect to students, but for the program itself, which is able to facilitate the production of research publications and presentations carried out in a minimal time of a summer studentship by medical students partnered with rural preceptors.
Conclusion
The Rural Summer Studentship Program developed at Western is a successful model that combines student research and clinical learning. Medical students partnered with physicians in small and mid-sized communities develop research skills by developing and performing practical community-based rural health research with program support that makes it possible. This model addresses the need to increase research methods education for medical students, to provide positive rural learning experiences, and to engage and support rural physicians in community-based research.
References
1. Davidson RA. Community-based education and problem solving: the community health scholars program at the University of Florida. Teaching and Learning in Medicine 2002; 14: 178-181.
2. Kelly L Rourke J. Research electives in rural health care. Canadian Family Physician 2002; 48: 1476-1480.
3. Western Medicine and Dentistry. SWOMEN. (Online) 2004. Available: http://www.med.uwo.ca/education/SWOMEN/ (Accessed 20 July 2005).
4. Undergraduate rural studentship program. 7b Rural Summer Studentship Program. (Online) no date. Available: http://www.sworm.on.ca/5year/07b_undergraduate.pdf (Accessed 20 July, 2005).


