People with COPD living outside urban areas experience poorer health outcomes such as higher rates of hospitalisation and mortality2,5. Approximately 14% of New Zealanders live in non-urban settings6 and 33% of Australians live in rural or remote areas7. On average, Australians living outside urban areas have poorer health risk factor profiles, lower levels of education and lower incomes compared with those living in major cities8. They also experience lower levels of access to health and other services with almost all health professions being less prevalent9.
The progressive and complex nature of COPD suggests that a multifaceted approach to its management is required10. Kruis et al11 reviewed 26 studies from 11 different countries of integrated disease management (IDM) for people with COPD. Each study reported at least two interventions with two different healthcare providers and of at least 12 weeks duration. Participants in an IDM program had better quality of life, exercise tolerance, reduced respiratory-related hospital admissions and hospital days at 12 months review. Likewise, Peytremann-Bridevaux et al12 found similar results in their review of 13 studies of COPD disease management programs.
While these reviews demonstrate positive outcomes, the majority of studies were located in urban areas. The Australian Lung Foundation's database of Pulmonary Rehabilitation Locations in Australia and New Zealand shows approximately 50% of programs are run in rural or remote locations. The type and effectiveness of these interventions is largely unknown. Some authors suggest that service models used in these communities must take account of the specific geographical, social, economic and cultural contexts of rural and remote communities13. The purpose of this review is to explore the type and cost effectiveness of COPD management interventions located in rural or remote settings of Australia or New Zealand in order to inform and influence planning for ongoing service development in the authors' local health district.
This review considered COPD interventions set in rural or remote locations in Australia or New Zealand, defined using the Rural, Remote and Metropolitan Areas (RRMA) Classification14. Included studies were set in locations classified as rural zones 1-3 or remote zones 1 or 2. Studies were considered if they provide a non-pharmaceutical, disease management intervention for people with COPD, for example home-based nursing interventions (post-acute, long-term support), community-based support programs, telehealth interventions, pulmonary rehabilitation programs, education or self-management interventions. Interventions were required to be disease specific or, if part of a generic chronic disease program, specifically target people with COPD, and report outcome measures of health resource utilisation such as emergency department (ED) presentations, inpatient admissions or length of stay.
Using four key search domains derived from the research question (COPD, models of care, rurality and Australia and New Zealand), search terms were developed to search Medline, Premedline, Scopus, Proquest, Cinahl and Informit databases as well as Google Scholar to find literature relevant to the topic of interest. The reference lists of identified literature were also searched for further relevant studies.
Study selection
Figure 1 shows the selection process for inclusion in the review. Of the 107 records identified, 76 were excluded based on title, 24 excluded based on abstract and 5 excluded after full paper review. The two remaining studies were included in the review.
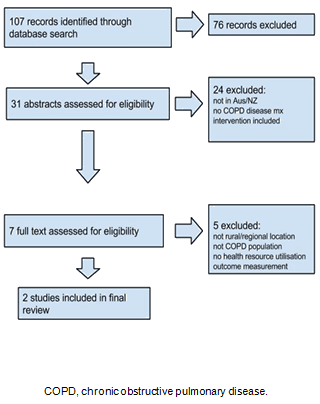
Figure 1: Flow diagram15 showing the process of study selection in a systematic review of the availability and cost effectiveness of chronic obstructive pulmonary disease management interventions in rural Australia and New Zealand.
Study characteristics
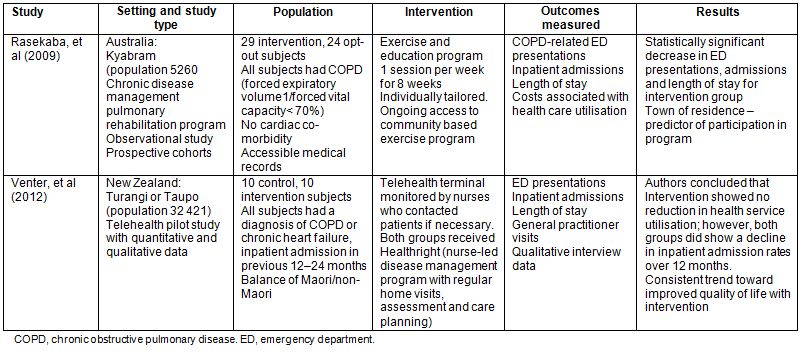
Study characteristics are summarised in Table 1. While both studies were set in a rural location and provided a program for the management of COPD, there were no similarities in the interventions provided; one focused on exercise training while the other provided a telehealth monitoring intervention.
Study quality
Both studies had a small sample size, and randomisation of subjects to control or intervention groups was poor.
Factors limiting the methodological quality of the Venter study16 included that the study included patients with a diagnosis of COPD or chronic heart failure; however, the number of subjects with each diagnosis or severity of disease was not specified. Forty percent (4/10) of the control group did not survive at 6 months and these subjects were replaced with matched subjects to complete the 12-month study period. Large differences existed in the baseline values of control and intervention groups for ED attendances, inpatient admissions and inpatient bed days. Outcomes were measured based on percentage change from baseline, with no statistical analysis performed, and it was not possible to determine level of significance.
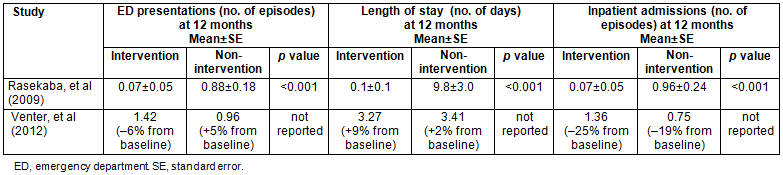
Table 2 summarises outcomes related to health resource utilisation of the two studies.
Effect of intervention on outcome
Table 2 summarises the findings of the two studies reviewed. Both interventions appear to positively influence a reduction in both ED presentation and inpatient admissions over a 12 month period. Interestingly, Rasekaba et al17 found that town of residence was a predictor of participation in the intervention they offered; participants living in outlying areas were less likely to participate.
While both studies have provided some evidence of their interventions resulting in a reduction in health resource utilisation, the lack of homogeneity between the two interventions does not allow any further comparisons or conclusions to be drawn.
Discussion
This review aimed to explore the type and cost effectiveness of COPD management interventions for people living with COPD in rural or remote areas of Australia or New Zealand. The limited literature, as well as a lack of homogeneity within the literature, has resulted in no definitive findings being drawn from this review. It has highlighted a need to review the key success factors for COPD management interventions internationally and in urban Australia and New Zealand and determine the transferability of intervention design to rural areas.
The authors included studies that reported on interventions specifically targeting people with COPD living in rural or remote locations in Australia or New Zealand. These countries share a common guideline for the management of COPD, specified by the Thoracic Society of Australia and New Zealand15, which means interventions in the review were more likely to fall within the COPDX guidelines and be relevant to the investigators' practice. While reviewing only literature based in rural or remote areas substantially limited the scope of the review, it was recognised that the context of rural health is geographically, sociologically and demographically different to metropolitan settings18. People with COPD in rural settings have different experiences relating to the management of their health in comparison to those in urban settings19. These experiences include poorly coordinated care, difficulty accessing specialist care and inadequate information sources and support services19.
Limiting the scope of this review to include only studies that had outcomes related to health resource usage further reduced the number of studies available for review. Including studies measuring outcomes related to patient experiences and quality of life may have given a wider range of interventions available for review and a greater understanding of patient-related issues. Evaluation of these factors are particularly relevant in a rural and remote setting, where more complex issues relating to accessibility and coordination of services are known to exist. However, planning for new health services in rural and remote communities must consider financial efficiency as well as clinical effectiveness, particularly as hospital services in rural and remote areas face higher fixed costs of operation. The present review did not specifically address issues related to indigenous health as these were not raised in the studies that met inclusion criteria. Other factors having the potential to impact on care received by those with COPD in rural and remote areas, such as the knowledge and skills of health practitioners20, were not considered.
Other components of care reported in the reviewed studies, but not directly examined as part of the intervention, were identified as having potentially significant influences on outcomes. For example, Rasekaba et al17 proposed that ongoing support received by the intervention group via linkage with a community-based exercise program may have played an important role in reducing health resource utilisation over the intervention period. Venter et al16 suggest that the ongoing support provided to intervention and control groups via a nurse-led disease management program (regular home visiting, systematic assessment and care planning) may have masked any effect of the telehealth intervention.
Multidisciplinary, multi-treatment disease management programs for COPD have been shown to be an effective way of reducing health resource utilisation in COPD populations internationally11,12. Adams et al's21 systematic review of the use of Wagner's chronic care model in COPD management identified that interventions combining an extensive self-management program, with individualised action plan, advanced access to care from a knowledgeable healthcare provider, guideline-based therapy, and a clinical registry system resulted in reduced healthcare use. Based on the findings of this review, this model may provide an appropriate structure from which rural and remote services could be developed. The current review revealed insufficient evaluation exists regarding the cost effectiveness of either single or multifaceted approaches to the management of COPD in rural and remote settings of Australia or New Zealand.
The present review was limited by the availability of literature specific to this area and small sample sizes within each of the studies reviewed, a common limitation of healthcare research in rural populations. Unpublished data (Casemix, NSW Ministry of Health) from a facility within a rural health setting currently using an integrated approach to the management of chronic respiratory disease have shown positive outcomes in reducing COPD hospital admissions, readmissions and length of stay. The service offers home visits by nurses and allied health, access to COPD clinics with specialist care, smoking cessation, medication reviews and pulmonary rehabilitation. Further evaluation of this service is warranted to determine its effectiveness in a rural setting.
This review demonstrates a lack of information regarding both care models available for rural and remotely located people with COPD and their cost effectiveness in relation to health resource utilisation. While the included studies reported on only a single intervention, both authors noted that concurrent, uninvestigated interventions may have played a significant role in the outcomes achieved. Approximately 50% of pulmonary rehabilitation programs in Australia and New Zealand are situated in rural and remote settings; however, only two have reported outcomes related to cost effectiveness. There is a need for existing programs to report outcomes in a consistent and coordinated manner so that health resource utilisation can be measured.
Acknowledgements
The authors acknowledge the assistance of Kerith Duncanson and David Schmidt from the Health Education and Training Institute (HETI), New South Wales for their assistance with the preparation of this manuscript. This review has been produced as a result of participation in a research development program provided by HETI. The authors acknowledge the librarians from Shoalhaven District Memorial Hospital and Wollongong Hospital, in particular, Christine Monie, for assistance with databases searches and access to journal articles.
References
1 Chronic respiratory diseases - chronic obstructive pulmonary disease. 2016. Available: http://www.who.int/respiratory/copd/en/ (Accessed 5 July 2016).
2 COPD - chronic obstructive pulmonary disease. 2016. Available: http://www.aihw.gov.au/copd/ (Accessed 5 July 2016).
3 COPD costs NZ $192m a year. 2015. Available: http://www.healthnavigator.org.nz/news/2015/04/07/copd-costs-nz-192m-a-year/ (Accessed 5 July 2016).
4 Characterisation of COPD heterogeneity in the ECLIPSE cohort.. Respiratory Research 2011; 11: 122. https://doi.org/10.1186/1465-9921-11-122
5 Rural-urban disparities in quality of life among patients with COPD. Journal of Rural Health 2013; 29(1): s62-s69.
6 A changing New Zealand . 2002. Available: http://www.stats.govt.nz/browse_for_stats/people_and_communities/households/changing-nz.aspx#the (Accessed 5 July 2016).
7 3218.0 - regional population growth, Australia, 2012-13. 2015. Available: http://www.abs.gov.au/ausstats/abs@.nsf/products/AC53A071B4B231A6CA257CAE000ECCE5?OpenDocument (Accessed 5 July 2016).
8 Rural health. 2016. Available: http://www.aihw.gov.au/rural-health (Accessed 5 July 2016).
9 Fact sheet 9: the state of rural health. 2009. Available: http://ruralhealth.org.au/sites/default/files/fact-sheets/fact-sheet-09-thestateofruralhealth_0.pdf (Accessed 5 July 2016).
10 Cochrane overview: comprehensive approaches to chronic obstructive pulmonary disease management. A23 Not a second time: solutions to COPD readmissions and care management. In: American Thoracic Society International Conference Abstracts, May 17-20 Denver, Colorado. New York: ATS Journals, 2015; A1113-A.
11 Cochrane corner: is integrated disease management for patients with COPD effective?. Thorax 2014; 69(11): 1053-1055. https://doi.org/10.1136/thoraxjnl-2013-204974
12 Effectiveness of chronic obstructive pulmonary disease-management programs: systematic review and meta-analysis. American Journal of Medicine 2008; 121(5): 433-443.e4. https://doi.org/10.1016/j.amjmed.2008.02.009
13 Rural health: why it matters. Medical Journal of Australia 2002; 176(10): 457-458.
14 Rural, Remote and Metropolitan Areas (RRMA) classification. 2016. Available: http://www.aihw.gov.au/rural-health-rrma-classification (Accessed 5 July 2016).
15 The COPD-X Plan: Australian and New Zealand Guidelines for the management of chronic obstructive pulmonary disease. Version 2.50. 2017. Available: http://copdx.org.au/copd-x-plan/ (Accessed 27 September 2017).
16 Results of a telehealth-enabled chronic care management service to support people with long-term conditions at home. Journal of Telemedicine and Telecare 2012; 18(3): 172-175. https://doi.org/10.1258/jtt.2012.SFT112
17 Can a chronic disease management pulmonary rehabilitation program for COPD reduce acute rural hospital utilization?. Chronic Respiratory Disease 2009; 6(3): 157-163. https://doi.org/10.1177/1479972309104419
18 The challenges confronting clinicians in rural acute care settings: a participatory research project. Rural Remote Health 2012; 12: 2017. Available: www.rrh.org.au (Accessed 5 July 2016).
19 Barriers to accessing specialist care for older people with chronic obstructive pulmonary disease in rural New Zealand. Journal of Primary Health Care 2009; 1(3): 207-214.
20 How prepared are rural and remote health care practitioners to provide evidence-based management for people with chronic lung disease?. Australian Journal of Rural Health 2012; 20(4): 200-207. https://doi.org/10.1111/j.1440-1584.2012.01288.x
21 Systematic review of the chronic care model in chronic obstructive pulmonary disease prevention and management. Archives of Internal Medicine 2007; 167(6): 551-561. https://doi.org/10.1001/archinte.167.6.551


