Introduction
As we attempt to eliminate health disparities and increase the quality and years of healthy life for all persons in the US, it is critical that people have access to comprehensive and quality health care services1. For the socioeconomically disadvantaged, access to care can be challenging. For the Latino immigrant population in rural areas, barriers to health care are exacerbated due to conflicting cultural health practices.
The Accessible and Culturally Competent Health Care Project was formed in order to provide care for underserved populations in Oconee County, South Carolina and to provide educational opportunities for health services students. The project was funded because of its potential to benefit rural and underserved populations, particularly the largely immigrant Latino population. The project identified the health needs of the community and barriers to accessing healthcare for this population, and designed a program to target these needs and overcome these barriers. Through collaboration with various health professionals, agencies, and volunteers in the community, the program has succeeded in providing appropriate and competent care to people in Oconee County, and has served as a 'hands on' education tool for nursing and public health students while improving the health of this rural community.
Background: barriers to health care access among rural Latinos
Access to health care can be defined in terms of factors that influence the ease with which medical care can be obtained. Although many factors affect health status, the lack of health insurance and other barriers to obtaining health services effectively diminish racial and ethnic minorities' utilization of preventive services and medical treatments that could reduce their burdens of disease and contribute to improved health status2. For Latinos, common barriers to obtaining care include lack of health insurance, language barriers, and cultural differences. These access barriers are typical among rural Latinos, compounding the problem of rural Latinos obtaining competent and appropriate health care.
Insurance-status is the most significant determinant of healthcare utilization3. An uninsured person is twice as likely as an insured person to go without medical care. The issue of health care access as related to insurance status is compounded for rural Latinos considering that minorities, regardless of insurance status, are less likely than whites to use physician services, and use is even lower if the person is from a rural area. This is especially a problem since Latinos are less likely to be insured than other groups, and therefore have poorer access to healthcare2. When ethnicity and insurance status are combined, rural uninsured Latinos are among the least likely individuals to receive health care.
New immigrant groups from Latin America living in southern states have significantly low percentages of insured individuals. A recent needs assessment conducted in South Carolina found that Latinos average 30 years of age with an average residency in the USA of 3 years. Ninety-three percent were of Mexican origin, and a majority (75%) were employed but had limited English-proficiency. Eighty seven percent of this population was uninsured4. Latino immigrants are limited in their ability to secure health and insurance benefits through their employment. According to research, unregistered workers have a real or imagined political inability to gain occupationally related security5. Fear of job loss or of deportation prevents individuals from requesting employee benefits. The high percentage of Latinos living without insurance and their reduced likelihood of obtaining health care due to insurance status makes it imperative that any program seeking to improve health among this population addresses the issue of insurance.
Although lack of health insurance is extremely significant, it is not the sole factor limiting access to care for Latinos. Language barriers are cited as a common problem between healthcare providers and patients6. Nearly 27 million Latinos in the US speak Spanish, and 12.4 million report that they speak English less than 'very well'7. A survey released in December 2001, conducted by the Robert Wood Johnson Foundation, found that 19% of Latino patients did not seek medical treatment because of language barriers. These language barriers lead to difficulties in understanding symptoms, asking questions and decreased trust in the physician's ability to comprehend their medical needs. In the same survey, 94% of healthcare providers stated that communication is a top priority in delivering quality care; they agreed that language barriers were a major challenge6.
Cultural barriers also affect the pattern of healthcare utilization for rural Latinos. There are many different views about healthcare practices and medicine. Women often negotiate encounters between their family and the practitioners of traditional Western medicine due to cultural differences in perspectives on health. There tends to be large contrasts between traditional folk remedies and modern medicine. These differences, and the role of emotion and religion in the manifestation and treatment of disease, shape interactions with healthcare providers. As Latino immigrants arrive from a variety of ethnic subcultures with a mixture of religious and folk beliefs concerning health and illness, it is important to be aware of potential barriers posed by these beliefs to the practice of traditional Western medicine among Latino immigrants8-11.
Research implies that health programs should examine local variations in language, culture, social and economic factors in order to provide culturally sensitive interventions. A better understanding of culture and world view is important in patient education and disease detection, and it is essential to study local conditions when planning health policies or programs12,13. Rural Latinos in the south have some of the lowest insurance rates in the nation, and suffer from cultural and language barriers relating to health care. As such, any program that wishes to serve the rural Latino population must be designed to meet the needs of this group by addressing these barriers to health care.
Health needs of rural areas: the case of Walhalla, SC
South Carolina is largely a rural state, with 31 of its 46 counties classified as either rural or very rural. A rural county's largest town has less than 25,000 people, while a very rural county's largest town has less then 10,000 people. According to classification by the South Carolina Office of Research and Statistics, 29% of South Carolina's population is considered rural, and 18% is considered very rural.
There are disparities between rural and urban residents in several health categories. Rural areas are commonly known to have higher rates of uninsured citizens and significantly decreased access to health services. Rural residents are 26% more likely to be hospitalized for a possibly preventable hospitalization than urban residents. Residents of the very rural areas of South Carolina are 20% more likely than urban residents to die from cancer. People in very rural South Carolina are almost 50% more likely to die from prostate cancer than are urban residents. Overall, very rural residents are 37% more likely than urban residents to die from heart problems. These disparities highlight the need to provide competent, appropriate, and affordable healthcare to rural populations in order to lessen the gap between rural and urban residents.
Walhalla, a town in Oconee County, is located in the northwest corner of South Carolina. The county is classified by the state as very rural and has experienced many changes in its economic base and population since 1970. The textile industry, which once dominated the local job scene, suffered from international competition and began to decline. Family farms, which also played a vital role in the local economy, have begun to disappear. The Duke Power Project has created electrical generating facilities and new jobs, which has provided an increase in the tax base. Development of lakes, particularly Lake Keowee, has drawn thousands of people, including many retirees, into the area.
The composition of Oconee County's population has changed dramatically in the past few decades. While Oconee's population has increased 63% since 1970, the Hispanic population alone has increased 88% in just the past 10 years (http://www.oconeesc.com/planning/elements/November2002draft.pdf). Census 2000 data shows a population of 66 215 in Oconee County. According to that report, 2% (1562) are Latino7. This figure is significantly understated because approximately 60% of Latinos are undercounted in traditional census measures.
Most of the Latinos in Oconee County have made their homes in Walhalla, which had a population of 3801 in the year 2000. The majority (76%) of the Latinos in the region are of Mexican origin4. Latino men are typically employed in plant nurseries or construction work. Many of the women work at a small textile plant that manufactures quilts. The employing entities are very small and offer no health benefits. More than 85% lack insurance for health care coverage, and almost all have limited physical access to services. The immigrants from Mexico have brought with them ideas and traditions formerly unknown in the area. These differences, compounded by language barriers, have sometimes led to negative perceptions of the newcomers by established residents and increased cultural friction.
Designing a program to fit the community - the 'Walhalla experience'
It became increasingly apparent that Walhalla needed some health program that could help the Latinos in the area, as well as other rural, uninsured residents. Testimonials regarding the need for comprehensive health services had been numerous in Walhalla. The Accessible and Culturally Competent Health Care Project (ACCHCP) was begun to provide care for the underserved populations, particularly Hispanic groups in Oconee County, South Carolina. Funded by the Health Resources and Services Administration of DHHS, the program was designed to offer care in a mobile clinic setting. The main goals of the program were to increase access to affordable, culturally and linguistically competent, quality primary and preventive health services among the medically underserved population of Oconee County and to improve the health status among community residents with a particular focus on identifying and treating those with chronic health care problems as well as women's health problems. The initiative was led by the Joseph F. Sullivan Center, an academic nursing center at Clemson University, in collaboration with the departments of nursing, public health science, nutrition, counseling and languages.
Strong letters of support for the development of a clinic were received from various regional agencies, including the Asociaciòn Hispana Humanitoria, the County Health Department, the local Catholic Church, the SC Statewide Hispanic Health Coalition, Partners for a Healthy Community and the SC Employment Security Commission. However, concerns were expressed when local officials were contacted regarding support for the project. Officials were concerned because they believed Hispanics would receive preferential treatment. Planning meetings revealed that officials were worried the location of the clinic might detract from local business. The project team had underestimated the potential conflict between the immigrants and the local population. In response, the development strategy was modified to address concerns. Meetings were held with the local officials to discuss the project and overcome objections. It was emphasized that the project would serve anyone who needed health services, not just the Latino population. The City Council was involved in the selection of a clinic site, and their input was sought in the preparation of a press release concerning the program. Representatives from the City Council, local churches, businesses, schools, social service agencies and community residents were also invited to serve on the program advisory board. A program design that was satisfactory to everyone involved ultimately was formed after much collaboration.
The Accessible and Culturally Competent Health Care Program was designed to fit Walhalla's unique community. A mobile clinic from the Sullivan Center traveled to Walhalla once a week to meet with patients for screenings, immunizations, and other basic health care needs. A key strategy in the success of the program was in scheduling of clinic services. To identify the optimal service times for the clinic, focus groups were held with patients. Through this process, it was determined that the clinic could best accommodate the work schedules of the Latino community by offering services on Friday evenings.
While the mobile clinic is central to the success of the program, the program design involves many more aspects. Various health professionals, including health educators, nurse practitioners, students from Clemson University, and medical residents are involved at the mobile clinic and local hospital. Language professors and bilingual interpreters are also vital to the program. Another aspect of the program that addresses the cultural uniqueness of the community is the involvement of Promotoras, lay advice-givers who are involved in the community. Each aspect of the program is necessary for its success.
The Promotora model
The Promotora model is a program that was used to help shape the program in Walhalla. It involves training informal advice-givers (Promotoras) that are already a part of the community to reach out to and help the underserved. Such advocacy roles appear to be an integral part of the Mexican and Mexican American experience14, and the Promotora model builds on this aspect.
There are three ways Promotoras differ from other types of volunteers. First, other members of the community view them as caring, respected individuals who are credible advice-givers. 'Outside' volunteers, such as agency staff, may not have the same relationship with the community as the Promotoras. Second, Promotoras offer spontaneous and informal advice within daily social interactions and can 'blend in' to community groups. Third, because of their extensive social networks, Promotoras are able to address the beliefs, attitudes, and behaviors of informal social groups15.
The Walhalla Clinic has effectively utilized lay helpers or 'promotoras' from the community. Promotoras were recruited during May and June, 2003. A list of 40 women was formulated through contacts at local churches, agencies, and the mobile clinic. Twenty-five of these women were invited to serve as Promotoras; ten accepted. Training materials were developed for the Promotoras and consisted of a manual in both English and Spanish, and a bilingual trainer for each topic. Promotoras received certificates of achievement, WalMart giftcards, and t-shirts when their training was completed.
The Promotoras were often approached throughout the week. They were recognized as important 'health connectors'-access points in the community, for which patients and community members can obtain information, referrals and assistance in a non-threatening environment. When Latinos interacted with the Promotoras, they were not concerned about documentation status or other issues that often arise when they seek services from social services agencies.
Inter-agency collaboration
One operational strategy that has been particularly effective for the Walhalla program is the development of collaborative partnerships with community agencies. Since the program is multi-faceted, it has required the cooperation of people with various health backgrounds and skills. Many different agencies throughout the community play a role in this program.
The local health department provides the use of its facility on clinic nights by allowing the mobile health unit to park adjacent to it. The additional waiting room, bathrooms and exam rooms available within the health department enable the clinic to see more patients than would be possible with the mobile unit alone.
Doctors in the area have collaborated with the Walhalla program. The Seneca Lakes Family Practice Residency Program, a rural residency program at Oconee Memorial Hospital, provides prenatal care, postpartum exams and initial exams for well childcare. The medical residents come to the Walhalla Mobile Clinic to provide care. Deliveries are done by the residents at Oconee Memorial Hospital.
The clinic employs a health educator and nurse practitioner to interact with the patients. The nurse practitioner assesses patients and identifies health problems that they might have. The health educator is responsible for helping the patients learn how to treat their diagnoses, and educating the patients about prevention strategies, such as vaccinations, diet and exercise.
Students from various majors at Clemson University have become involved in the Walhalla program. Since its inception, 231 students have rotated through the clinic for 3010 practice hours. Nursing, public health science, language, counseling, and third year medical students have educational experiences through the clinic.
Public Health Science students (PHS), through their core curriculum, learn how to perform various clinical skills, such as taking blood pressure, hemoglobin, blood sugar, and cholesterol readings. PHS students also take courses that teach how to create culturally sensitive health campaigns, that identify certain health risks of different population groups, and that teach appropriate ways to modify health behaviors. Through involvement with the Walhalla Program, PHS students receive the chance to apply classroom knowledge to real life situations. PHS students help design behavior modification programs for the patients at the clinic; they assess blood pressure and cholesterol; they design culturally appropriate brochures and information packets; they interact with patients and make sure things run smoothly; they help plan health fairs for the community. The students also help eligible patients sign up for Medicaid, a state-funded health services program. Another responsibility of the PHS students is to watch children at the clinic. Many mothers who come to the clinic state that they do not have anyone to watch their children and might not come to receive care without knowing someone would be able to supervise children. Involvement in this program allows PHS students to expand upon their core skill set and the chance to learn through experience.
Nursing students also play a key role in the clinic. Nursing students are assigned clinical rotations and assist the nurse practitioner in patient care. The skills and knowledge they have learned in the nursing program are applied at the Walhalla clinic where they are able to see patients and get an understanding of how a clinic is run. Students also help plan appropriate nutrition programs for patients based on screening results. With the help of interpreters, the nutrition students are able to target problem areas and educate the patients about what they can do to improve eating habits and overall health.
Spanish students from Clemson University are able to help serve as bilingual interpreters at the clinic. This immersion into a Latino healthcare setting helps them build their speaking and interpretation skills while also becoming aware of the nearby Hispanic culture.
The Walhalla Clinic has six bilingual interpreters, four of whom are native Spanish speakers. Special care has been taken to train interpreters regarding the role and responsibility of medical interpreting. Because many of the interpreters come from the community served, a focus of the program is on ensuring that clients understand that interpreting staff value patient confidentiality. In order to ensure accurate medical interpretation and cultural sensitivity, interpreting staff receive ongoing training under the supervision of the lead interpreter who has completed a national train-the-trainer medical interpreting program. Priority is placed on medical terminology as well as verbal and non-verbal communication skills. A system is being developed which will provide ongoing training opportunities to Spanish language students and opportunities to observe interpreters to identify issues and areas that may need additional training in order to enhance consistency in interpreter services.
Training opportunities
The clinic promotes opportunities to enhance and build Spanish-language skills among staff and volunteers. Language and Public Health students are given opportunities to build language skills through patient intake and observation of interpreters. Students receive opportunities to build their core skill set, but also opportunities for building cultural competence through this rural 'immersion' experience in a predominantly Latino community. Additionally, faculty members from the language department provided a series of seminars focused on increasing cultural sensitivity among clinic staff and volunteers.
Recruitment of bilingual/bicultural health professionals continues to be a struggle in rural areas, and the Walhalla experience is no exception. Ideally, both the health educator and the nurse practitioner for the program were to be bilingual and bicultural. Unfortunately, due to the nature of the part-time positions and the rural location, bilingual applicants were difficult to recruit. The program turned to current staff to identify team members with interest in developing the necessary language skills. For example, the clinic's health educator was sent to Mexico for intensive Spanish language training. The experiences focused both on increasing language proficiency as well as improving understanding of cultural differences. The nurse practitioner understands basic Spanish but relies on interpreters to ensure quality of healthcare. Language training is an ongoing process and is being made available to anyone involved in providing clinic services.
Program results
The Accessible and Culturally Competent Health Care Program has been successful in meeting its program goals of increasing access to primary and preventive health services among the medically underserved population of Oconee County. The program also improved health status among community residents with focus on identifying and treating patients with chronic and women's health problems. Between January 31, 2003 and June 30, 2004, the Joseph F. Sullivan Center held 63 mobile clinic sessions and provided services to 1076 patients. During that same time, the Seneca Lakes Family Residency Program treated 92 prenatal patients who were referred through the Accessible and Culturally Competent Health Care Program. The demographic characteristics of the patients at the mobile clinic are detailed (Figs 1-3). The majority (65%) are Hispanic, female (67%), and 19-39 years old (51%). As shown in Figure 4, the majority (87%) of patient visits were for laboratory work and immunizations. Most of the patients seen could only pay the minimum payment because they lacked health insurance (Fig 5).

Figure 1: Accessible and Culturally Competent Health Care Project patients' race.
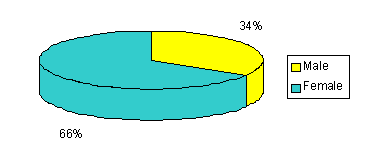
Figure 2: Accessible and Culturally Competent Health Care Project patients' sex.
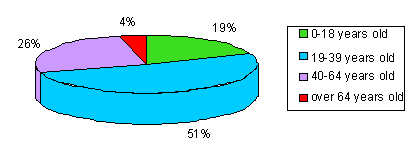
Figure 3: Accessible and Culturally Competent Health Care Project patients' age.
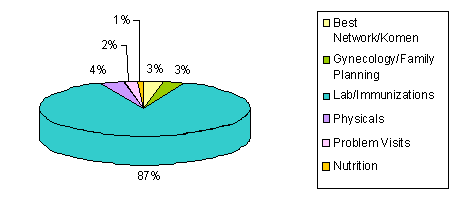
Figure 4: Accessible and Culturally Competent Health Care Project type of patient encounters.
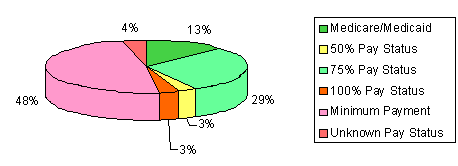
Figure 5: Accessible and Culturally Competent Health Care Project payment status of patients.
A patient satisfaction survey was distributed to a sample of clients using the clinic services. Of the patients surveyed, a majority (68%) use the clinic as their primary source of care. A significant portion of the patients reported that, without the clinic, their only option for health care would be the emergency room. Clients state that the friendliness and openness of the clinic staff enable them to feel comfortable seeking services. They also report that the regular presence of trained interpreters and Spanish speaking staff removes a barrier to care. Many clients have returned to the clinic seeking services for their entire family.
A particular success of the program was the integration between academic programs, the health services system and the community. The collaboration between these entities was important in the development and implementation of the clinic. The involvement of faculty and students complemented the full-time clinic staff and ensured that the clinic could service as many patients as possible. The training opportunities experienced by the students will be beneficial as they consider future careers in health services.
Conclusion
As rural communities struggle with maintaining healthcare services, supporting the rural health care safety net is critical. Access related factors are among the most significant barriers to equitable care and must be addressed in order to eliminate healthcare disparities, particularly among rural Latinos16. Through innovative strategies such as bringing health care to the community via a mobile medical clinic, inter-agency collaboration, involvement of students in the program, and utilization of Promotoras for information, referrals, support and lay education, the Accessible and Culturally Competent Latino Health Care Project is making a positive impact on rural Latinos in South Carolina.
References
1. HHS. Healthy People 2010. (Online) 2001. Available: http://www.healthypeople.gov/document/html/volume1/01access.htm#_Toc489432809 Accessed March 31, 2003.
2. Brown E, Ojeda VD, Wyn R, et al. Racial and ethnic variables in access to health insurance and health care. UCLA center for health policy research. (Online) 2000. Available: http://www.healthpolicy.ucla.edu/pubs/files/RacialandEthnicDisparitiesReport.pdf (Accessed 19 August 2005)
3. Mueller K, Patil K, Boilesen E. The role of uninsurance and race in healthcare utilization by rural minorities. Health Service Research 1998; 33: 597-611.
4. Lopez-de Fede A. South Carolina Statewide Hispanic needs assessment. Columbia, SC: Institute for Families in Society, 2000.
5. Moore E. Issues in access to health care: The undocumented Mexican resident in Richmond, California. Medical Anthropology Quarterly 1986; 17: 65-70.
6. American Public Health Association. The Nation's Health Web exclusive March 2002. Spanish-English language barrier dissuades Hispanics from pursuing medical care. (Online) 2002. Available: http://www.apha.org/journal/nation/langbarriersexclus302.htm.(Accessed 19 August 2005).
7. US Census Bureau,
8. Bearison D, Minian N, Granowetter L. Medical management of asthma and folk medicine in a Hispanic community. Journal of Pediatric Psychology 2002; 27: 385-392.
9. Murguia A, Peterson R, Zea M. Use and implications of ethnomedical health care approaches among Central American immigrants. Health Social Work 2003; 28: 43-51.
10. Robledo L, Wilson A, Gray P. Hispanic mothers' knowledge and care of their children with respiratory illnesses: a pilot study. Journal of Pediatric Nursing 1999; 14: 239-247.
11. Tedlock, R. An interpretive solution to the problem of humoral medicine in Latin America. Social Science Medicine 1987; 24: 1069-1083.
12. Chavez L, Hubbell FA, Mishra S, Valdez RB. Undocumented immigrants in Orange County, California: A comparative analysis. International Migration Review 1997; 31: 88-107.
13. Hubbell FA, Waitzkin H, Mishra SI, Dombrink J, Chavez LR. Access to medical care for documented and undocumented Latinos in a Southern California county. Western Journal of Medicine 1991; 154: 414-417.
14. Patterson S, Marsiglia F. 'Mi casa es su casa': beginning exploration of Mexican Americans' natural helping. Families in society: The Journal of Contemporary Human Services 2000; 81: 22-31.
15. Brownstein JN, Cheal N, Ackermann SP et al. Breast and cervical cancer screening in minority populations: a model for using lay health educators. Journal of Cancer Education 1992; 7: 321-326.
16. National Heart, Lung and Blood Institute. Women's Heart Health: Developing a National Health Education Action Plan. Strategy Development Workshop Report, March 26-27, 2001, Bethesda, MD National Institutes of Health; (Online) 2001. Available at http://www.nhlbi.nih.gov/health/prof/heart/ (Accessed 19 August 2005).
Abstract
Background:
Access to comprehensive and quality healthcare services is difficult for socioeonomically disadvantaged groups in rural regions. Barriers to health care for rural Latinos include lack of insurance, language barriers and cultural differences. For the Latino immigrant population in rural areas, barriers to access are compounded.Health Needs of Rural Areas: The Case of Walhalla, SC: The town of Walhalla, South Carolina, USA, is a rural community located in Oconee County, the northwest corner of the state. Disparities exist between rural and urban residents in several health categories, and these disparities illustrate the need to provide competent, appropriate and affordable healthcare to rural populations. The Hispanic population of Oconee has dramatically increased in the past decade, and the majority of these immigrants have no health insurance and have limited access to health services.
Designing a Program to fit the Community - the "Walhalla Experience": The purpose of the Accessible and Culturally Competent Health Care Project (ACCHCP) is to provide care for underserved populations, in Oconee County, South Carolina while providing rural educational opportunities for health services students. Funded by the Health Resources and Services Administration of DHHS, the program is designed to offer culturally appropriate, sensitive, accessible, affordable and compassionate care in a mobile clinic setting. In this interdisplinary program, nurse practitioners, health educators, bilingual interpreters, medical residents and Clemson University students and professors all played key roles. Women in the community also serve as promotoras or lay health advisors. The program is unique in using educational initiatives and innovative strategies for bringing health care to this underserved community and offers important information for rural healthcare initiatives targeting minority groups. This article reports on the challenges and successes in the development and implementation of the ACCHCP program in Walhalla, South Carolina.
Key words: Hispanic, Latino, insurance, access, rural.



