In the Australian population, the highest rate of suicide (38.3 per 100 000) is found in men aged 85 years and older1. Both suicide and intent to die by suicide are associated with depression and extreme stress in older people2-4. In men, suicide rates increase with age in Asian and English- speaking countries, particularly amongst the 'older old' (ie more than 80 years of age)4-6. Suicide in this group has been attributed to increased mental illness, family conflict and long-term or chronic illness4-6. Over the past 25 years, suicide in Australian rural communities has been widely researched; however, the focus has been predominantly on younger males7,8 and all aged farming populations9-13.
The rates of rural farmer suicide vary by age and state, with research in Queensland suggesting the highest rate of rural suicide is in male farmers aged 18-34 years12, with the National Rural Health Alliance stating that farmers aged 55 years and older accounted for two-thirds of all farmer suicides14. The reasons for an increased rate of suicide in rural males compared to urban males is unclear, but suggests that factors other than mental health disorders may influence suicidal behaviour13. A number of initiatives designed to reduce the risk of suicide in all age groups have been developed and implemented around Australia15-19. Although services are targeted for specific locations, including rural communities, the extent to which these initiatives modify the factors leading to suicidal behaviour, or improve access to services that may reduce suicidal intent, seems unclear18,19.
Reviews of research into rural male suicide by Alston20 and Handley et al21 investigate the differences in urban and rural suicide. Alston highlights the multiple factors that contribute to increased suicide rates in all aged rural men, including farming under stress, the reluctance of men to utilise health services, the stigma of mental illness, stoicism, threatened masculinity and changing rural practices20. Handley's review concluded that there are (1) inconsistencies in terminology used in urban, rural and remote suicide research, (2) a reliance on cross-sectional studies, rather than studies that established causality and (3) a focus on urban suicide. Handley's review identified areas for future research, highlighting the importance of rural research that uses a longitudinal approach and includes community samples21.
Given the differences between suicide rates in rural males aged 75 years or more, compared to urban males the same age, it is reasonable to assume there are unique factors in rural communities that contribute to suicidal behaviour. To explore this further, this article reviews the Australian literature to investigate the factors unique to rural males that may be associated with increased suicidal behaviour or suicidal intent.
Method
Literature search strategy
A literature search (Fig1) was conducted using electronic databases (MEDLINE (1950 - March 2015), PubMed (January 1976 - March 2015), and CINAHL (up to March 2015). Terms included in the initial search were 'aged', 'elderly' and 'older males'. Results were then combined with the terms 'rural', 'suicide*' and 'Australia'. Secondary searches were conducted of bibliographies of identified articles and previous systematic reviews.
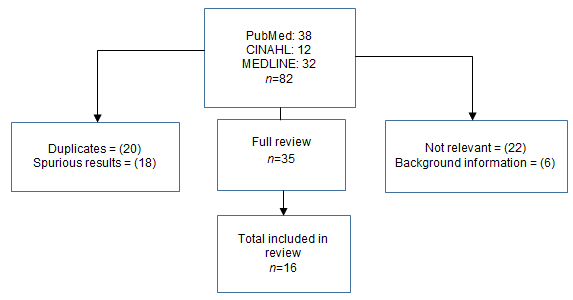
Figure 1: Literature search strategy.
Inclusion criteria
To be eligible for inclusion in the review, studies needed to be:
- published in English between 1950 and 2014
- peer-reviewed journal articles reporting factors that may contribute to suicide in rural men aged more than 65 years.
Results and analysis
A total of 82 articles were initially identified. After exclusion of duplicates (n=22) and articles that did not meet the inclusion criteria (n=44), 16 articles were selected for analysis and inclusion in the review (Table 1). Study findings were synthesised, using the Critical Appraisal Skills Program (CASP)22 appraisal tool. Key factors contributing to suicide in older males were identified from the articles and categorised by the authors (KCG and LW). Categories were organised conceptually, based on context, and included the role of age and gender, stigma of mental illness, availability of mental health services, socioeconomic status (financial adversity), isolation and changes to rural climate patterns. These categories are presented individually and in context, with other categories where they overlap and intersect.
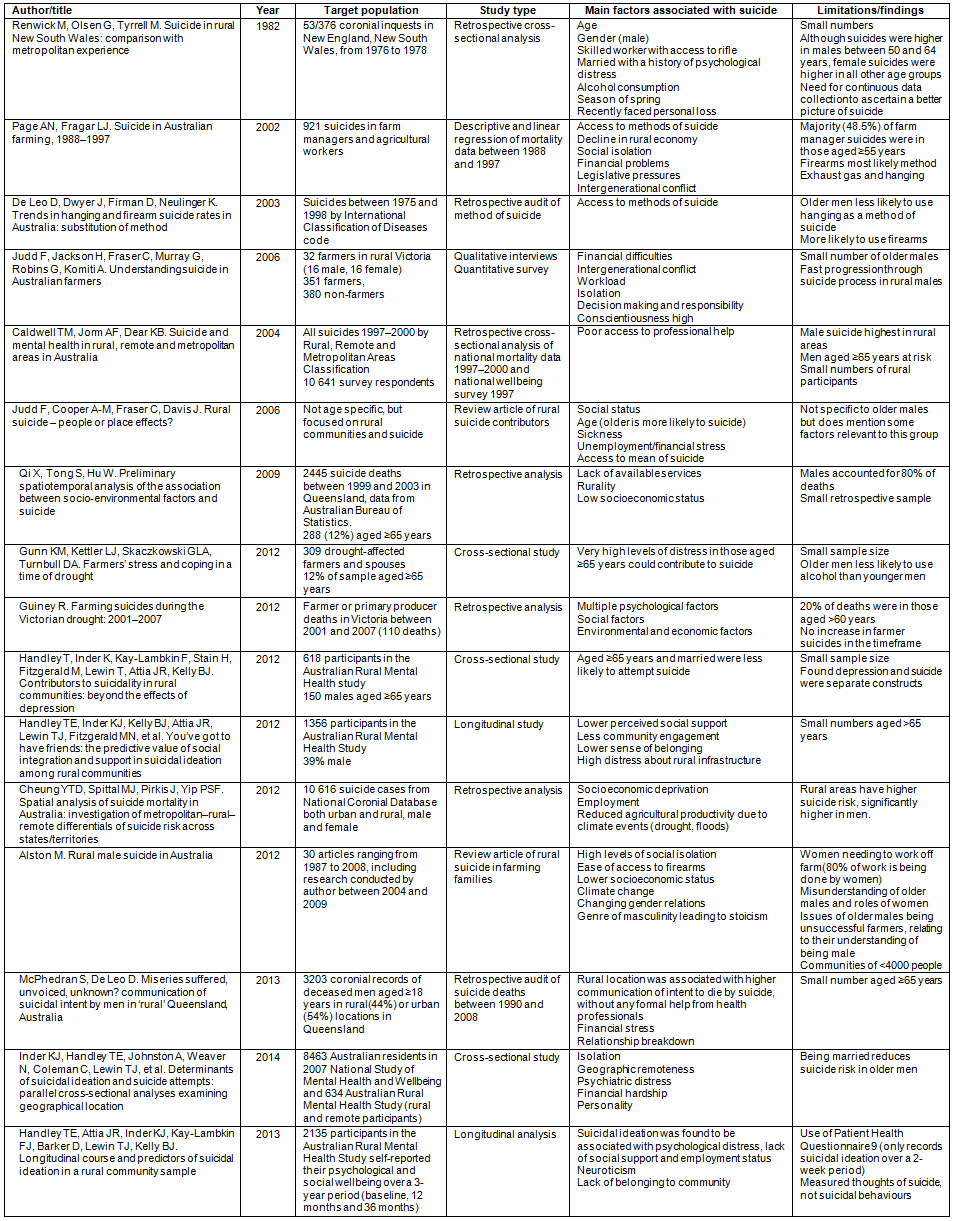
Literature review
Age and gender
Advancing age is a risk factor for suicide, because many older males cope less well with physical illness and loss of ability and social connections, as a result of the ageing process23, particularly those who are unmarried or have lost a partner24,25. Ageing migrant males are at higher risk of suicide, possibly as a result of limited education and employment opportunities, as they age in rural settings20. Page and Fragar's national review of suicides over a 10-year period showed that 48.5% of completed suicides in rural areas were by farm managers aged 55 years and older23. Guiney's study published in 2012, following the drought in the state of Victoria of 2001-2007, showed 20% of suicides were in men more than 60 years of age10. Guiney's study of males working in rural Australia highlights the gender imbalance in rates of suicide, the deteriorating health of older rural farmers, the high rate of male suicide generally, the changing dynamics in farming relationships, and the reduced sense of self-worth and feelings of 'entrapment' (p. 157)20, as a result of growing levels of debt and increased poverty for those older male farmers20. Highlighting similar stressors in rural Australia, Judd et al26 discuss the high rates of suicide for males, with a particular focus on the longitudinal research conducted by Page and Fragar23, who highlighted the issue of farm managers being placed in a high risk category for suicide. This is a result of a combination of geographical location; physical injury; psychological, emotional and financial stress; and the importance placed on feelings of place26.
Stigma of mental illness and availability of mental health services
The unwillingness of people to discuss mental illness is evident in the reviewed articles, with one paper by Judd et al. discussing the preference to talk to professionals about practical things, such as seeking financial assistance, rather than discussing mental health11. The stigma of mental illness was identified as a factor that prevented older rural males asking for assistance when they felt unable to cope with their daily life and responsibilities10,11,20,24-26. Similarly, other studies reported the reluctance of older rural men to report feelings of stress and anxiety to their local doctor/general practitioner (GP)9-11, with Rajkumar and Hoolahan's study on the experiences of isolation in rural Australia reporting the low use of mental health and GP services generally27. Guiney's study of rural farmer's highlights discussions pertaining to family pride and personal and family values, being reasons why people are not connecting with their local health services10. These factors reduce the likelihood of diagnosis and treatment for mental health issues.
Although initiatives have been implemented to assist the mental health of older rural men15-19, there are still areas where services are limited or not available. Judd and colleagues11,26 suggest this may relate to a reduction in rural health services generally, with rural communities facing increased levels of out-migration and decreased population mass (a result of younger residents leaving rural areas to attend tertiary educational facilities and improve their chances of employment). The study conducted by Qi et al28, looking at socio-environmental factors and suicide, found that areas with high suicide rates also had higher populations of Aboriginal and Torres Strait Islander people, who are known to have high suicide rates, poorer access to mental health services and lower socioeconomic status29.
Socioeconomic status, unemployment, and financial adversity
Research conducted into social integration and friendship by Handley et al. suggests that unemployment is also predictive of socioeconomic status30. A study conducted in 2012 by Inder et al, reviewing reasons for suicidal behaviour, suggests that the presence of a psychiatric disorder, marital status, use of mental health services and a person's perception of financial viability can contribute to suicidal behaviours31. Renwick et al compared suicide in both rural and metropolitan areas, in order to highlight the inequity between rural and urban income levels, with rural residents earning far less than urban dwellers32. Inder et al31 suggest that prolonged or unforced unemployment in a rural or remote location may impact negatively on an individual's social capital and this may impact upon already compromised levels of psychological distress, leading to an increase in suicide risk33,34. Other studies suggest that having to leave the family farm, either through forced or unforced means, results in an increased risk of suicide9-11,20. Major factors associated with an increase in psychological stress and subsequent risks of suicide in older rural men were issues with farm ownership, and about who will inherit the family farm9-11,20. Three studies found that when younger generations leave the farm, the burden of debt usually stays with the older generation, who are unable to leave the farm, and often unable to make a profit from it10,11,20. Some studies identified economic (global agricultural export) and government regulatory factors (such as workplace injury laws) that place farmers under increased pressure, resulting in anxiety, and sometimes post-traumatic stress disorder, following workplace injury20,26,35. Three studies11,20,33 highlight the stoic, hardworking persona of the Australian farmer, and the feelings of failure and disappointment when family farms fail or financial situations seem unresolvable.
Isolation
Rajkumar and Hoolahan identified geographic isolation, loss of social capital and increased psychological distress were factors, working together or separately, in not accessing local medical services27, and in higher recorded rates of suicide in rural areas32-36. Research conducted by Taylor et al highlighted isolation in some rural and remote communities as a reason why rural residents are not easily rescued or saved from a suicide attempt34. Qi et al discussed that the greater the distance from a GP trained in recognising mental illness, the greater the risk of suicidal behaviours in older rural males28.
Changes to the rural environment
In the years between 2001 and 2007, Victoria experienced one of its worst weather events, a drought lasting 6 years, which caused high levels of stress for the local drought-affected areas. Both Guiney and Alston discussed the relationship between changing climate patterns (particularly drought) and increased risk of suicide, in older rural men, with particular regard to recovery from extreme weather events10,20. Five other articles highlighted that the changing rural environment was considered a major factor contributing to suicide risk, with changes to agricultural practices, reduced services, increased debt, reduced land values, decreased ability to find work and changing social support networks all playing a part in increased levels of psychological distress20,24,26,33,35.
Discussion
The key finding of this review is that, for an older male in a rapidly changing rural environment, where financial adversity is increasing and social cohesion diminishing, likelihood of psychological distress and subsequent risk of suicide increases.
The literature reviewed clearly shows that older males are hesitant to access mental health programs, due to the stigma of mental illness, a lack of awareness of the benefits of mental health services, or an inability to access these services due to geographic isolation. Farmers in particular are less likely to access mental health services due to the stigma of mental illness, high workloads and lack of access, either perceived or real. In addition, farmers in live-work situations have an increased level of stress, with weekends viewed as another work day, and increased psychological pressure of ongoing work and family commitments. Increasing levels of environmental change are major contributors to an increased risk of suicide in this group. Factors outside the control of the rural male resident (such as global economics, climate events, societal change and financial adversity) may compound, leading to high levels of psychological distress and an increased risk of suicide33.
Much of the literature review commented on the connection of the farmer to the land, and the sense of place and connection to the rural way of life11,20,26. These findings reflect other rural Australian studies that highlight the strong connection of rural residents to their land and community20,37,38. Hence, changes to the rural economy, a decrease in productive farms by 25% in the last 25 years and globalisation of agricultural product export have placed pressure on farmers to expand and carry large debts. When younger generations leave the farm, the burden of debt usually stays with the older generation, who feel trapped and unable to sell, but are also facing low profits and yields. Farmers who are forced to sell stock at extremely low prices or kill animals because they are unable to afford to feed them, as a result of climatic events, are at high risk of psychological illness and suicide.
It is clear that, in spite of programs targeting the mental health of rural men, there is still a stigma attached to being diagnosed with a mental illness, or displaying an inability to cope. Research suggests that rural males personalise their own experience (such as feeling a sense of responsibility for failed crops), limiting their ability to understand the broader impact of changing weather patterns, and the way this affects others similarly. The perception that the persona of Australian rural men is hardworking, stoic and indestructible may lead this group to feel that the success of the farm is attached to their masculinity20. In addition, the increasing requirement for women to work in other paid positions away from the farm has been identified as causing feelings of inadequacy, and therefore psychological distress, in older males. In addition, the increasing unpredictability of climate patterns leading to long periods of drought and/or unseasonal flooding have had an impact on the psychological state of rural communities10,11,39.
Some subgroups within the older male rural cohort have particularly high levels of suicide. These are older migrants and Indigenous and Torres Strait Islander populations. High levels of suicide in rural migrants could be due to a lack of access to education and poor English, coupled with the hardworking, stoic nature of many migrant families, who are determined and accustomed to living with adversity40. Indigenous and Torres Strait Islander communities have a 20% lower life expectancy than non-Indigenous communities, with higher unemployment rates and lower socioeconomic status. These disparities are exacerbated in rural and particularly remote areas and can impact on later suicide risk41.
The unique vulnerability relating to factors for older age cohorts in rural areas, relating to socioeconomic factors such as isolation, physical comorbidity, health service access and lack of resources, can be interpreted in the context of the Vulnerable Persons Conceptual Framework, developed by Flaskerud and Winslow42. This framework was used to try to interpret the themes that emerged from the literature. The Vulnerable Persons Framework has three dimensions relating to relative risk, health status and resource availability. Commonly, in epidemiological research, relative risk relates to the risk of association between strength of exposure to a disease and the outcome of disease. In this instance, relative risk applies to a population in regards to the relationship between increased risks of illness, due to lack of resources and decreased health status. Ideally speaking, the greater the access to resources, the better the health status will be, leading to a general decrease in risk of comorbidities in vulnerable people43. Health status indicators, using a vulnerable persons framework, can be defined as levels of morbidity and mortality44, while resource availability relates to the amount of community resources available to the community, in order to improve their overall health.
The research included in the present article makes recommendations for increasing current strategies, with a view to the development of future strategies in order to assist rural people who may be experiencing suicidal behaviours. These include increased identification of people at risk through screening30, increased clinical and telepsychiatry services to assist rural GPs caring for rural people at risk27 and further research into suicide risk factors, comparisons with other male-dominated occupations. Along with further examination of the incidence of farming suicides, these may provide a more complete picture of the complexities of older male suicide in rural Australia10,41. Kennedy et al13 suggest there needs to be more discussion and research into the impact of suicide on communities, and an understanding of the specific needs of farming communities, both in the local and regional sense. In view of the high suicide rate in older rural males, compared to urban males, Shah and Bhat suggest there is a need for further research into the risks and protective factors for older men40. There is a suggestion that the experience of adversity can protect some people from suicidal behaviours40. This is supported by other research in rural communities that highlights the role of protective factors in preventing high levels of stress, building resilience and successful adaptations10. Coping mechanisms such as the collective resource of social capital, the camaraderie found in rural communities and the shared experience, may be an area of research to investigate further. Such research can then drive changes to existing policies and suicide prevention programs.
There were two obvious gaps discovered in the existing research on suicide in older rural men. The first is the reluctance of researchers to explore the possible misclassification of suicide deaths (ie deaths classified as accidents, which may, in fact, be suicide), with only one article, by De Leo, discussing the importance of recording appropriate suicide mortality data45. With this at the forefront, it is likely that stigma around suicide, and issues relating to insurance claims, following the death of an older male, may be associated with underreporting of suicide deaths13. The second finding is that of the paucity of research, giving particular regard to the impact of retirement, overall mental wellbeing and suicidal behaviour on older rural males.
This article reviewed the literature outlining the potential contributing factors to suicide in elderly Australian rural dwelling males. The literature highlights the impact of the changing rural economy and the differing dynamics of contemporary rural families. In this setting, ageing rural men are exposed to a number of issues that compound the risk of suicide, compared to older men living in urban Australia. Those who are farmers are burdened with the rising financial cost of maintaining increasingly large farms to ensure financial return, whilst dealing with unpredictable climatic conditions. The burden of financial adversity and the stress of losing farms that have been in families for generations are key factors impacting on the mental health of farmers. Similarly, rural men who have a long history working in service industries (such as farm fencing, shearing, and agricultural supplies) are also affected by the downturn in the rural economy. Future research should focus on improved suicide prevention strategies, improved understanding of suicidal behaviours, identification of possible misclassification of suicide death, further investigation into retirement pathways, and the effect that retirement may have on mental wellbeing and suicidal behaviours in older rural dwelling males.
References
1 Causes of death online. 2013. Available: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/bySubject/3303.0~2013~MainFeatures~KeyCharacteristics~10009 (Accessed 13 May 2016).
2 Suicide among the elderly: issues facing public health. American Journal of Public Health 1991; 81(9): 1109-1110.
3 At risk in America: the health and health care needs of vulnerable populations in the United States. San Francisco: John Wiley & Sons, 2002.
4 Suicide in centenarians: the international landscape. International Psychogeriatrics 2014; 26(10): 1703-1708. https://doi.org/10.1017/S1041610214001112
5 Differences in suicide between the old and the oldest old. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 2003; 58(5): S314-S322. https://doi.org/10.1093/geronb/58.5.S314
6 Acta Psychiatrica Scandinavica 2002; 105(4): 271-275. https://doi.org/10.1034/j.1600-0447.2002.1014.x
7 Toward understanding youth suicide in an Australian rural community. Social Science & Medicine 2003; 57(12): 2355-2365.
8 Further increases in rural suicide in young Australian adults: secular trends, 1979-2003. Social Science & Medicine 2007; 65(3): 442-453. https://doi.org/10.1016/j.socscimed.2007.03.029
9 Suicide and mental health in rural, remote and metropolitan areas in Australia. Medical Journal of Australia 2004; 181(7): S10.
10 Farming suicides during the Victorian drought: 2001-2007. Australian Journal of Rural Health 2012; 20(1): 11-15. https://doi.org/10.1111/j.1440-1584.2011.01244.x
11 Understanding suicide in Australian farmers. Social Psychiatry and Psychiatric Epidemiology 2006; 41(1): 1-10. https://doi.org/10.1007/s00127-005-0007-1
12 A regional approach to understanding farmer suicide rates in Queensland. Social Psychiatry and Psychiatric Epidemiology 2014; 49(4): 593-599. https://doi.org/10.1007/s00127-013-0777-9
13 Suicide and accidental death in Australia's rural farming communities: a review of the literature. Rural and Remote Health 2014; (1): 2517. Available: www.rrh.org.au (Accessed 21 April 2015).
14 Good health and well being in rural and remote Australia. Fact sheet 14. Available: http://ruralhealth.org.au/sites/default/files/fact-sheets/fact-sheet-14-suicideinruralaustralia_0.pdf (Accessed 21 April 2015).
15 Let's get serious: the infrastructure to effectively address suicide in Australia. A submission to the Senate Community Affairs Committee Inquiry on Suicide in Australia The Suicide Prevention Taskforce & Suicide Prevention Australia Inc. 2009. Sydney: Suicide Prevention Australia.
16 LIFE - livingisforeveryone.com.au A framework for prevention of suicide in Australia. Report No. P3 -2060. Canberra: Commonwealth of Australia, 2008.
17 Living is For Everyone. 2016. Available: http://www.livingisforeveryone.com.au/Projects.html?cat=124#23 (Accessed 1 March 2016).
18 LIFE: Living is for everyone, Farm Link Online: Life Communications. 2016. Available: http://www.livingisforeveryone.com.au/Projects.html?cat=127#31 (Accessed 1 March 2016).
19 Living is for Everyone - Men Online: Life Communications. 2016. Available: http://www.livingisforeveryone.com.au/Projects.html?cat=124 (Accessed 1 March 2016).
20 Rural male suicide in Australia. Social Science & Medicine 2012; 74(4): 515-522. https://doi.org/10.1016/j.socscimed.2010.04.036
21 Urban-rural influences on suicidality: gaps in the existing literature and recommendations for future research. Australian Journal of Rural Health 2011; 19(6): 279-283. https://doi.org/10.1111/j.1440-1584.2011.01235.x
22 Checklist for qualitative studies. Available: http://www.casp-uk.net/#!checklists/cb36 (Accessed 3 November 2015).
23 Suicide in Australian farming, 1988-1997. Australian and New Zealand Journal of Psychiatry 2002; 36(1): 81-85. https://doi.org/10.1046/j.1440-1614.2002.00975.x
24 Miseries suffered, unvoiced, unknown? Communication of suicidal intent by men in 'rural' Queensland, Australia. Suicide and Life-Threatening Behavior 2013; 43(6): 589-597. https://doi.org/10.1111/sltb.12041
25 Longitudinal course and predictors of suicidal ideation in a rural community sample. Australian and New Zealand Journal of Psychiatry 2013; 47(11): 1032-1040. https://doi.org/10.1177/0004867413495318
26 Rural suicide - people or place effects?. Australian and New Zealand Journal of Psychiatry 2006; 40(3): 208-216.
27 Remoteness and issues in mental health care: experience from rural Australia. Epidemiologia e Psichiatria Sociale 2004; 13(2): 78-82. https://doi.org/10.1017/S1121189X00003298
28 Preliminary spatiotemporal analysis of the association between socio-environmental factors and suicide. Environmental Health 2009; 8(1): 46.
29 Archives of Suicide Research 2006; 10(2): 141-157. https://doi.org/10.1080/13811110600556889
30 You've got to have friends: the predictive value of social integration and support in suicidal ideation among rural communities. Social Psychiatry and Psychiatric Epidemiology 2012; 47(8): 1281-1290.
31 Determinants of suicidal ideation and suicide attempts: parallel cross-sectional analyses examining geographical location. BMC Psychiatry 2014; 14(1): 208-227. https://doi.org/10.1186/1471-244X-14-208
32 Suicide in rural New South Wales: comparison with metropolitan experience. Medical Journal of Australia 1982; 1(9): 377-380.
33 Farmers' stress and coping in a time of drought. Rural and Remote Health 2012; 12: 2071. Available: www.rrh.org.au (Accessed 21 April 2015).
34 Social and psychiatric influences on urban-rural differentials in Australian suicide. Suicide and Life-Threatening Behavior 2005; 35(3): 277-290. https://doi.org/10.1521/suli.2005.35.3.277
35 Contributors to suicidality in rural communities: beyond the effects of depression. BMC Psychiatry 2012; 12(1): 1. https://doi.org/10.1186/1471-244X-12-105
36 Spatial analysis of suicide mortality in Australia: investigation of metropolitan-rural-remote differentials of suicide risk across states/territories. Social Science & Medicine 2012; 75(8): 1460-1468. https://doi.org/10.1016/j.socscimed.2012.04.008
37 Climate adversity and resilience: the voice of rural Australia. Rural and Remote Health 2015; 15: 3071. Available: www.rrh.org.au (Accessed 21 April 2015).
38 Farming and mental health problems and mental illness. International Journal of Social Psychiatry 2005; 51(4): 340-349. https://doi.org/10.1177/0020764005060844
39 Suicide and drought in New South Wales, Australia, 1970-2007. Proceedings of the National Academy of Sciences 2012; 109(35): 13950-13955. https://doi.org/10.1073/pnas.1112965109
40 Does adversity earlier in life affect elderly suicide rates? A cross-national study. International Journal of Psychiatry in Clinical Practice 2009; 13(4): 273-277. https://doi.org/10.3109/13651500902912702
41 The influence of deprivation on suicide mortality in urban and rural Queensland: an ecological analysis. Social Psychiatry and Psychiatric Epidemiology 2014; 49(12): 1919-1928. https://doi.org/10.1007/s00127-014-0905-1
42 Conceptualizing vulnerable populations health-related research. Nursing Research 1998; 47(2): 69-78. https://doi.org/10.1097/00006199-199803000-00005
43 Vulnerable populations and ultimate responsibility. Issues in Mental Health Nursing 2010; 31(4): 298-299. https://doi.org/10.3109/01612840903308556
44 The application of a vulnerable populations conceptual model to rural health. Public Health Nursing 2003; 20(6): 440-448. https://doi.org/10.1046/j.1525-1446.2003.20604.x
45 Suicide mortality data need revision. Medical Journal of Australia 2007; 186(3): 157-158.

