Dear Editor
Physician undersupply in rural areas is prevalent worldwide1. Particularly among young physicians, reluctance to work in rural areas may be related to limited opportunities for education and participation in cutting-edge clinical practice1. We would like to introduce our experience in rural Fukushima following the 2011 triple disaster: the case of an unexpected increase in physicians.
Minamisoma Municipal General Hospital (MMGH) is a public hospital in Minamisoma City, Fukushima, Japan. The city's population density of 390/km2 in 2014 was much less than the Japanese national average of 1044/km22, with a physician proportion of 85.7 per 100 000 residents, significantly fewer than the Japanese average of 233.6/100 0003. In March 2011, MMGH, located 23 km from Fukushima Daiichi Nuclear Power Plant, experienced an earthquake, tsunami and nuclear disaster4. Yet, despite the hardship of a disaster on this rural and medically underserved area, we have observed a consistent increase in physicians in post-disaster years, from 12 in 2010 to 32 in 2016 (Fig1).
Two factors possibly related to this increase are the expansion of research and media coverage. There was a strong push to publish as many scientific papers as possible on local health issues post-disaster. Although MMGH is a small 200-bed hospital, the number of post-disaster publications indexed in PubMed was 39, as of 11 July 2016, compared to 0 in any year pre-disaster. In addition, physicians have made regular contact with newspaper reporters, and the nationwide newspaper coverage of MMGH in the post-disaster period as of 11 July 2016 was 5.6 times greater than the same period pre-disaster (167 vs 30 articles). The time trends of newspaper articles and disaster-related publications, as well as the number and demographics of full-time physicians employed at MMGH pre- and post-disaster, are summarized in Figure 1. The annual number of newspaper articles and publications were calculated, designating 11 March as the beginning of each year in order to align with the date of the disaster. For 2016, articles and publications as of 11 July were considered. The number and demographics of full-time physicians employed in each year is shown as of 1 April, the start of the Japanese fiscal year.
When interpreting these changes, some details deserve recognition. It is true that a support system was launched to partially cover salaries of newly employed full-time physicians in affected areas of Fukushima Prefecture post-disaster, using a public disaster-reconstruction budget. However, MMGH has utilized this scheme for only four full-time physicians as of 11 July 2016, leading us to suspect that disaster relief funds were not a main cause for the observed increases in physicians. It is notable that before the disaster, persistent shortages of physicians meant that the hospital budget for physicians was never completely used, and we therefore speculate that MMGH has, for the first time, obtained a necessary number of physicians after the unexpected increase post-disaster, related to media coverage and research. It is additionally to be noted that the number of physicians under 30 has remarkably increased, from none in 2010 to eight in 2016, and that all are currently from outside Fukushima.
The trends in Minamisoma suggest that countermeasures for physician undersupply in rural areas may benefit by including a rigorous research program and media activities. These opportunities can enhance the education of young physicians, potentially contributing to a more attractive working environment and chances for career growth.
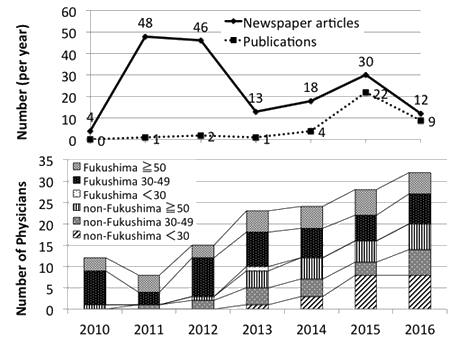
Figure 1: Newspaper articles and publications, and the number, age, and original working place of physicians, pre- and post-disaster, at Minamisoma Municipal General Hospital, Fukushima, Japan.
Acknowledgements
We express our gratitude to Ms Rina Tadano, Ms Echiko Baba, and the staff of MMGH for data provision.
Kana Yamamoto, Department of Obstetrics and Gynecology; Akihiko Ozaki, Department of Surgery; Claire Leppold, Department of Research; Yukio Kanazawa, Department of Gastroenterology
Minamisoma Municipal General Hospital, Minamisoma, Fukushima, Japan
Tetsuya Tanimoto, Department of Internal Medicine
Jyoban Hospital of Tokiwa Foundation, Iwaki, Fukushima, Japan
References
1. Staiger DO, Marshall SM, Goodman DC, Auerbach DI, Buerhaus PI. Association between having a highly educated spouse and physician practice in rural underserved areas. JAMA 2016; 315(9): 939-941. https://doi.org/10.1001/jama.2015.16972
2. Statistics Japan. Statistical observations of Shi, Ku, Machi, Mura (in Japanese). (Internet) 2016. Available: http://www.stat.go.jp/data/s-sugata/index.htm (Accessed 8 August 2016).
3. Fukushima Prefectural Office. Statistical observation of health care providers in Fukushima prefecture (in Japanese). (Internet) 2016. Fukushima: Fukushima Prefectural Office. Available: https://www.pref.fukushima.lg.jp/uploaded/attachment/155600.pdf (Accessed 8 August 2016).
4. Kodama Y, Oikawa T, Hayashi K, Takano M, Nagano M, Onoda K, et al. Impact of natural disaster combined with nuclear power plant accidents on local medical services: a case study of Minamisoma Municipal General Hospital after the Great East Japan Earthquake. Disaster Medicine Public Health Preparedness 2014; 8(6): 471-476. https://doi.org/10.1017/dmp.2014.112




