Introduction
The national shortage of healthcare providers in rural areas has been persistent despite the growing number of physicians. Rural areas are generally underserved with only 9% of physicians available to serve almost 20% of the US population1. The size of the future rural physician workforce may be further compromised, because medical students tend to develop less favorable views of primary care as they progress through medical school2 and increasingly choose non-generalist specialties3. Many educators and policymakers believe that major curricular reforms emphasizing primary care4,5 and community-based training will be efficacious in bolstering the number of physicians serving in rural areas6-8.
Some factors cited in the literature as being predictors of physician selection of rural practice include: having grown up in a rural/underserved area; having a strong interest in rural practice when beginning medical school; being male; and choosing a senior year rural family practice preceptorship9,10. A rural educational experience has been reported to increase students' favorable attitudes toward rural affiliations11. A tendency for student perception of increased social responsibility (not statistically significant) has been reported after a rural community clerkship12. While not predicting specifically for rural practice, a service orientation or perception of social responsibility of medical students predicts for the generalist careers13-18 that can lead to rural practice.
A variety of educational initiatives have been devised to address the chronic shortage of rural healthcare workers. These initiatives have primarily been rural training experiences for trainees, with some programs offering a special admissions process and/or a separate rural track19-21. The literature supports the presumption that long-term, intensive, multi-faceted curricula in primary care, rural and underserved settings will be found effective22, but most studies have had little accounting for pre-existing characteristics and interests, and little is known about educational factors affecting career choices4,7. A longitudinal tracking system has been reported that involves several medical schools and has the potential to track practice sites and to correlate this information with student and program characteristics23.
There is some evidence that community-based training with medically underserved populations and primary care role models living and practicing in underserved communities can reinforce and guide students' interests to serve rural communities5. In order to promote this attitude that practicing in a medically underserved area could be rewarding, Pathman and Riggins22 suggest that favorable attitudes toward underserved area practice may be enhanced when students spend more time in these areas.
The lack of physicians in rural areas is a critical concern for West Virginia (WV), and could have a negative impact on the health of its population. Approximately 23.6% of West Virginians live in primary care Health Professional Shortage Areas, compared with 17.3% nationally, and the physician/population ratio is lower (180 vs 198 per 100 000)24. WV has an increased prevalence of many diseases and a higher rate of patients who state that they have difficulty seeing a provider due to cost25. A community-based rural curriculum for healthcare discipline students was thought to be of value in orienting trainees to future rural practice and to increasing the availability of health care in rural WV. The West Virginia Rural Health Education Partnership (WVRHEP) was designed to address these concerns26. This article describes the statewide WVRHEP training program and its structure for collecting student feedback regarding rural clinical experiences; correlation of selected outcomes with other variables for healthcare discipline students; and pre-post testing of selected outcomes for medical students.
Project description
In 1991, the WV legislature addressed health professional shortages and rural health disparities by building a community-based rural health training system. Under the Rural Health Initiative Act, the state chose to expand the rural training initiated in the state through the Kellogg Community Partnerships Initiative and, in 1995, formally integrated this expansion with the Kellogg Initiative to form WVRHEP. Financial support from the WK Kellogg Foundation and the state legislature was used to build a statewide infrastructure of community-based training sites in rural communities, and to make changes within the academic institutions to emphasize rural primary care and inter-disciplinary clinical training at the community level. In 2001, when WV received its Area Health Education Center (AHEC) grant, it entered into a partnership with WVRHEP. WVRHEP shares AHEC's commitment to serve the healthcare needs of underserved populations, seeking to increase the numbers of health professionals in rural communities and linking health professions education to dynamic community-based recruitment and retention activities.
Students from seven state institutions of higher education (public and private) and 10 health profession disciplines (clinical psychology, dentistry, dental hygiene, medicine, nursing, pharmacy, occupational therapy, physical therapy, physician assistant and social work) participate in the WVRHEP and AHEC programs through partnerships with rural organizations and community leaders. These rural organizations provide faculty/preceptors, learning resources and technical support for the students. Today, WVRHEP's infrastructure serves rural areas in 50 of WV's counties through 12 regional partnerships, each with its own board. The joint effort of the WVRHEP and AHEC programs will soon enable WV to offer training opportunities in medically underserved communities in all 55 counties. Within these 12 consortia, 332 training sites serve as partners, 215 of which are located in communities with a federal designation as an underserved area or serve primarily underserved populations. In addition to private physician offices, these training sites include 28 community health centers, 32 federally qualified health centers, 29 rural health clinics, 30 small rural hospitals, 25 dental offices, 37 pharmacies, 12 county health departments, 20 physical therapy agencies or rehabilitation centers in underserved areas, and 17 county boards of education or school systems.
Since 1996, most of WV's state-supported health professions students have been required to spend at least 12 weeks in a rural setting. The exceptions include dental and dental hygiene students who spend 6 weeks in a rural setting and students in medical technology and occupational therapy programs that are still in the process of identifying appropriate rural sites and preceptors. As part of their rural training, students spend 20% of their time in community service and interdisciplinary activities. Community service includes participation in activities such as tobacco cessation, diabetes support groups, nutrition and life style education, and health fairs. Interdisciplinary activities primarily consist of an interdisciplinary seminar held 2-4 times per month at the rural site.
An evaluation of the multi-faceted WVRHEP effort is complex. The effects of WVRHEP on provider recruitment and retention in rural WV are the ultimate outcome for program evaluation, and data collection allows measurement of recruitment and retention. State databases regarding practice location of graduates indicate that since 1991, 142 physicians who have graduated from the program have entered rural WV practice27. However, additional data are needed to help us to understand the extent to which specific individual characteristics or programmatic factors influence choice of practice location, and to evaluate the predictive validity28 of individual characteristics and reported experiences in forecasting intent for rural practice. Since 2001, we have used an accumulating online database to assess intermediate outcomes of students' reported attitudes, service orientation, and career intents in a longitudinal fashion, and to study correlates of these intermediate outcomes.
Methods
The data analyzed for this report covered the period from initiation of online questionnaires in January 2001 to February 2004. Baseline data questionnaires (BDQ) were completed by 907 medical students, usually during their second year, from the state's three medical schools (two allopathic and one osteopathic). At the time of initiation of the evaluation in 2001, third- and fourth-year medical students also had an opportunity to complete the BDQ, regardless of their WVRHEP experience. A post-rotation questionnaire, the student evaluation of rural field experience (SERFE), was completed by 1360 students in 10 disciplines from seven institutions of higher learning. Of the 907 medical students who completed a BDQ, 620 had also completed a SERFE.
The questionnaires queried student attitudes on curricular components, overall rotation quality, clinical experiences, career intents, community activities and social obligation. In addition, the medical student BDQ queried perceived "rural hometown". Selected entries were regarded as intermediate outcomes: interest in rural health, confidence in becoming an active part of the community, importance of meeting the unique needs of the poor, and anticipated population category of practice town. Attitudinal responses were quantified on ordinal scales with three to six possible choices. Response to each questionnaire item was voluntary and not all students answered all queries. The questionnaire responses were accumulated in an electronic database and combined with additional demographic information available for the students.
With the accumulated database, it was possible to study correlations of outcomes with selected demographic and attitudinal factors. Correlation analyses were performed by use of ordinal logistic regression and significant predictors of an outcome response were arranged in summary tables. Fewer than ten responses were present for four disciplines; due to the low number of responses, these were eliminated for correlation analyses where discipline was entered as a possible predictor of a response. Due to the longitudinal nature of the database, it was also possible to study trends in student attitudes and intents over time, for example medical student pre-post testing as is presented in this article. Of the 620 medical students who had completed both a BDQ and SERFE, 279 had no previous record of WVRHEP rotation experience and had completed the BDQ at least 28 days prior to completion of the SERFE. Pre-post analyses were performed on these data by use of the Wilcoxon signed rank test. The level of significance for statistical testing was 0.05. The JMP statistical software package (SAS Institute Inc., Cary, NC, USA) was used for data analyses.
Results
The response rate for the SERFE was 73% (1360 of 1872). Seventy-two percent of respondents from various disciplines rated the overall quality of the rotation as 'very good' or 'excellent'.
After their rotations, respondent students replied to, 'Did your rural rotation increase, decrease, or leave unchanged your interest in rural health?'. Table 1 shows a summary of results of significant correlation, found by ordinal logistic regression procedures, with this item for 568 medical students. Rating for increased interest in rural health was positively associated with higher rating for each of the ordinal variables: overall quality of the rural rotation, planning to live in WV, planning to practice in a smaller town, and planning to have a practice accessible to the indigent. The student's medical school was also a predictor of this interest, with a variation from 30-49% for a response of increased interest among the three medical schools. An indication of increased interest in rural health also positively correlated with the indication on the BDQ that the student had a 'rural' hometown.
Table 1: Summary table of analyses for significant factors found to be predictive of reported medical student 'increased interest in rural health' after the first rotation
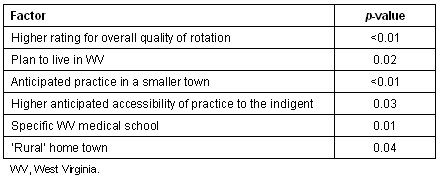
Table 2 shows the correlates for 549 medical students for 'anticipated practice in a smaller town'. Among the three medical schools, students showed a variation from 2-4% in choosing the lowest population category, 'less than 2500' and a variation from 11-23% choosing the highest, 'greater than 100 000'. Students who rated smaller town practice highly were more likely to say they had a rural hometown and to anticipate primary care practice. There were positive correlations of numerical ratings between intent for smaller town practice and ratings for each of the listed ordinal factors (Table 2).
Table 2: Summary table of analyses for significant factors found to be predictive of reported medical student ratings on 'anticipated practice in a smaller town' after the first rotation

Table 3 shows correlates for the outcome of 'confidence in becoming an active part of the community' for 1314 students of various disciplines after the first rotation. Confidence ratings correlated positively with ratings for the overall quality of the rotation and with plans to practice in a smaller town. The 'confidence' rating varied significantly by discipline, with nurse practitioner students most likely (66%) to give the highest rating of 'very confident'.
Table 3: Summary table of analyses for significant factors found to be predictive of reported healthcare discipline student 'confidence in becoming an active part of the community' after the first rotation

Table 4 shows correlates for 'importance in meeting the unique needs of the poor' given by various disciplines after the first rural rotation. Females tended to give a higher rating to this importance. There was a difference among disciplines in rating of this importance, with nurse practitioners most likely (98%) to give the highest rating. There was a positive association of rating of this importance and the indication of increased interest in rural health after the rotation.
Table 4: Summary table of analyses for significant factors found to be predictive of healthcare discipline student rating on 'importance of meeting unique needs of the poor' after the first rotation

Longitudinal testing (BDQ vs. SERFE) was done for the intermediate outcomes. One outcome, the perceived importance of meeting the unique needs of the poor, was statistically significantly changed for the group of 279 medical students who met the criteria for pre-post testing (p < 0.05). There was an overall trend toward an increase in the rating of this variable after a rural rotation, in comparison with the rating given on the BDQ.
Discussion and Conclusions
The WVRHEP program substantially changed health professions education in WV and developed an infrastructure for community-based education of physicians and other healthcare providers, with the ultimate goal of enhancing recruitment and retention in rural WV. At present, it is possible to identify some individual or program characteristics correlating with selected intermediate outcomes that may predict for rural practice. This report adds to the body of literature on rural health professions training by describing a required statewide program and evaluation project for longitudinally tracking multi-disciplinary attitudes, career intents, and career paths.
One of the preliminary program findings, a statistically significant increase in students' reported perceptions of a social responsibility parameter after a rural rotation, also makes a contribution in adding to the small body of literature on this subject. The programmatic value of this statistical finding is not yet known. Consistent with prior reports18,29, female gender was a predictor for increased perceptions of social responsibility. The increased interest in service to the indigent population seen between the BDQ and SERFE data may indicate that rural experiences can have an impact on students' understanding of the importance of serving this segment of the population. It may be speculated that increased awareness of social responsibility, correlated with primary-care career selection, can help to counter the trend away from primary-care specialization found during medical student matriculation. The finding of an association between perceived quality of the rural experience and increased interest in rural health supports the importance of providing an educationally rewarding experience.
The finding of an association between a "rural" hometown and interest in rural health supports earlier research. WVRHEP data indicate an association of perceived quality of the rural experience with increased interest in rural health and rural practice. One selected indicator for perceived social responsibility, anticipated accessibility of the practice to the indigent, was also associated with increased interest in rural health, and with intent for practice in smaller towns.
The current study is limited to self-reported attitudes and values. Program evaluations have contributed toward changes in the rural curriculum. The WVRHEP program will continue to track student reported attitudes and career intents as they progress through their various curricula, allowing longitudinal analyses of these data. Later, tracking of practice location of program graduates will be possible and these combined data will allow an assessment of WVRHEP effects on recruitment and retention, the correlation of stated intents and attitudes with ultimate outcomes and the efficacy of using intermediate outcomes in prediction of rural recruitment and retention.
References
1. Jolly P, Hudley DM (Eds). AAMC data book: statistical information related to medical education. Washington, DC: Association of American Medical Colleges, 1998.
2. Zinn WM. The effect of medical education on primary care orientation: results of two national surveys of students' and residents' perspectives. Academic Medicine 2001; 76: 355-365.
3. American Academy of Family Physicians. 2004 match information sheet. Kansas City, Mo: American Academy of Family Physicians. (Online) 2004. Available www.aafp.org/match/graph05.html (Accessed 30 September 2004).
4. Campos-Outcalt D, Senf J, Watkins AJ, Bastacky S. The effects of medical school curricula, faculty role models, and biomedical research support on choice of generalist physician careers: a review and quality assessment of the literature. Academic Medicine 1995; 70: 611-618.
5. Tippets E, Westpheling K. The health promotion-disease prevention project: effect on medical students' attitudes toward practice in medically underserved areas. Family Medicine 1996; 28: 467- 471.
6. Richards RW, Henry RC. Community partnerships: educational linkages to increase the number of primary care practitioners. Academic Medicine 1993; 68: 594-596.
7. Pathman DE. Medical education and physicians' career choices: are we taking credit beyond our due? Academic Medicine 1996; 71: 963-967.
8. Richards RW. Best practices in community-oriented health professions education: international exemplars. Education for Health 2001; 14: 357-365.
9. Xu G, Veloski JJ, Hojat M, Politzer RM, Rabinowitz HK, Rattner S. Factors influencing physicians' choices to practice in inner-city or rural areas. Academic Medicine 1997; 72: 1026.
10. Rabinowitz HK, Diamond JJ, Markham FW, Paynter N.P. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. JAMA 2001; 286: 1041-1048.
11. Woloschuk W. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-247.
12. Potts M. Rural community health agencies as primary care clerkship sites for medical students. Family Medicine 1994; 26: 632-637.
13. Kassebaum D, Szenas P. Factors influencing the specialty choice of 1993 medical school graduates. Academic Medicine 1994; 69: 164-170.
14. Madison DL. Medical school admission and generalist physicians: a study of the class of 1985. Academic Medicine 1994; 69: 825-831.
15. Martini CJ, Voloski JJ, Baransky B, Xu G, Fields SK. Medical school and student characteristics that influence choosing a generalist career. JAMA 1994; 272: 661-668.
16. Ellsbury KE, Burack J H, Irby D M, Stritter FT, Ambrozy D, Carline JD, Guo J, Schaad DC. The shift to primary care: emerging influences on specialty choice. Academic Medicine 1996; 71(Suppl.): S16-S18.
17. Kassebaum DG, Szenas PL, Schuchert MK. Determinants of the generalist career intentions of 1995 graduating medical students. Academic Medicine 1996; 71: 197-209.
18. Schubot DB, Cayley W, Eliason BC. Personal values related to primary care specialty aspirations. Family Medicine 1996; 28; 726-731.
19. Bland CJ, Meurer LN, Maldonaldo G. Determinants of primary care specialty choice: a non-statistical meta-analysis of the literature. Academic Medicine 1995; 70: 620-641.
20. Rosenthal TC, McGuigan MH, Osborne J, Holden DM, Parsons MA. One-two rural residency tracks in family practice: are they getting the job done? Family Medicine 1998; 30: 90-93.
21. Blackman JR. Predoctoral education for rural practice. In: JP Geyman, TE Norris, LG Hart (Eds). Textbook of rural medicine. New York: McGraw-Hill, 2001; 359-367.
22. Pathman DE, Riggins TA. Promoting medical careers in underserved areas through training. Family Medicine 1996; 28: 508-510.
23. Rabinowitz HK, Veloski JJ, Aber RC et al. A statewide system to track medical students' careers: the Pennsylvania model. Academic Medicine 1999; 74: S112-S118.
24. National Center for Health Workforce Information and Analysis. The Health Care Workforce in Ten States: Education, Practice and Policy - West Virginia. Washington: US DHHS, HRSA, Bureau of Health Professions, 2001.
25. West Virginia County Health Profiles. West Virginia - Overview (Online) 2000. Available: http://www.wvdhhr.org/bph/oehp/hsc/prof2000/cp00a.htm (Accessed 19 October 2004).
26. Carlton B, Weston WD. Changing health professions education in West Virginia. Academic Medicine 1997; 72: 110-115.
27. West Virginia Higher Education Policy Commission. West Virginia Rural Health Education Partnerships: Annual Report, 2003. Charleston, VA: West Virginia Higher Education Policy Commission, 2003.
28. Renger R, Meadows LM. Testing for predictive validity in health care education research: a critical review. Academic Medicine 1994; 69: 685-687.
29. Tippets EA Westpheling KM. Practice in medically underserved areas: medical students' attitudes and intents. Academic Medicine 1993; 68: S67-S69.
Abstract
Introduction:
A shortage of healthcare providers in West Virginia led to creation of a statewide, community-based program with a required three-month rural experience for most state-sponsored health professions students. Project Description: Initiated using funding from the W. K. Kellogg Foundation and expanded using both state funds and Area Health Education Center support, the West Virginia Rural Health Education Partnerships (WVRHEP) program impacts institutions of higher learning, 50 counties, and 332 training sites, and all students in state-funded health professions schools. A longitudinal database has been constructed to study program effects on students' reported attitudes, service orientation, and career intents.Methods: Baseline data are collected from medical students, and students in all disciplines provide feedback on rotations and information about career intents, social responsibility, and attitudes towards rural practice.
Results: Data indicate an association between perceived quality of the rural experience and increased interest in rural health, social responsibility and confidence in becoming part of the community. Medical students may tend to rate social responsibility higher after completion of the first rural rotation. Students who anticipate practice in smaller towns also tend to rate the quality of the rotation higher, to anticipate careers in primary care, and to acknowledge social responsibility.
Conclusion: As WVRHEP program graduates who have completed these surveys enter practice, both personal and community-specific program characteristics may be identified which strengthen interest in rural practice. The predictive validity of intermediate outcomes of attitudes and career intents in forecasting the ultimate outcomes of recruitment and retention may be studied.
Key words: program evaluation, rural curriculum, rural health education, rural recruitment, social responsibility, student careers intentions.

