A visit to the emergency department (ED) can be a potentially harmful experience for the older person living with dementia1. Errors in care related to atypical signs and symptoms of disease make timely and accurate diagnosis difficult2 with underrecognition of illness in older adults at ED triage remaining a complex and poorly understood phenomenon3. Individuals with dementia are more sensitive to illness and changing circumstances associated with the hospital4, and cognitive impairment decreases the ability to remember, follow directions, solve problems, perform independent self-care and communicate5. Multinational data show 26% of older adults in EDs have cognitive impairment, and 46% are dependent in one or more activities of daily living before illness6. Older adults with cognitive impairment in the ED have been found to have pre-existing dependence in activities of daily living, nutrition concerns, bladder/bowel control problems, and vision and hearing impairment7, adding to the challenge of providing care. Most ED studies of older adults with dementia1,7 or vulnerable older adults including those with cognitive impairment8, have been undertaken in large urban EDs, with little known about this at-risk population in rural EDs.
Differences between rural and urban ED exist, with role and function varying by location9. Rural EDs face unique challenges in care of older people with dementia. There are limited healthcare services, lack of healthcare providers and challenges including distance and transportation10. Rural caregivers have been reported to have less access to in-home support services, in-home respite and respite day care, and may have to travel longer distances for diagnostic and extended care services11-13 than urban caregivers. Often, dementia services in rural hospitals are limited14, with family physicians providing most medical care in rural EDs9,15. Compared to their urban counterparts, rural ED patients have been found to be older, have lower educational and income levels and be less likely to have a family physician, with more seeking primary care services9. Smaller community-oriented EDs, which are often rural, may play a role in providing primary care16,17. Other contextual factors such as distance from medical clinics or regional EDs18 may influence the decision to come to the ED.
While it has been suggested that smaller rural EDs may provide better services for some older adults through community resource links16, rural transitional care is not well understood. Transitional care has been described as actions to uphold coordination and continuation of care when patients move between locations or levels of care in a setting19, with poor transitional care leading to poor clinical outcomes. Patient safety is linked to quality of care, and is focused on mitigating unsafe acts to optimize outcomes20. For older adults, identification of adverse events that produce harm must go beyond single-event issues such as medication errors or procedure-related complications and to also include unnecessary functional decline and new-onset geriatric syndromes21,22. It is not known if healthcare professionals (HCPs) in rural EDs embrace this broad conceptualization of safety and harm. The purpose of this study was to understand safety and harm in rural ED transitional care for community-dwelling older adults with dementia from the perspective of HCPs.
Design
An interpretive, descriptive exploratory design guided by the social ecological perspective23-25 with two underlying assumptions was used. The first assumption is that people cannot be understood apart from their environmental context. Second, physical as well as social and organizational environments must be studied together as one without the other significantly diminishes the likelihood of understanding relevant mediating factors contributing to positive (safe) or negative (harmful) outcomes. To achieve this understanding, the qualitative analytical approach described by Graneheim and Lundman26 was used.
Sample and setting
Two rural hospitals in two western Canadian provinces participated in the study. Both hospitals were nominated by their respective regional health service organization as they operated a 24-hour ED staffed with nurses and a physician, functioned as a regional facility for surrounding smaller rural communities without 24-hour ED service and the community served as a retirement location for local residents. Each hospital had other HCPs (nurse consultant/coordinator, occupational therapist, social worker and/or physical therapist) available weekdays for consultation in the ED. One hospital had 95 inpatient beds and was located 61 km from the nearest large urban setting. The other had 76 inpatient beds and was located 94 km from the nearest large urban setting.
Participants were recruited through staff and hospital meetings as well as posters in the participating EDs. At the meetings, a research team member gave a brief summary of the study, and the ethics-approved information letter for potential participants was made available. This letter and the posters included a contact number for the research team that interested staff could call individually if they wanted more information and to book an interview. Two research team members, one in each province, travelled to the communities to conduct the interviews in person. Using purposive and snowball sampling27, interdisciplinary HCPs with experience working or consulting in the two participating EDs were recruited. HCPs who worked in the ED, as well those who consulted on cases involving people with dementia, were invited to participate to ensure maximum variation in ED experience with the population of interest. Target sample size was guided by Creswell28.
Data collection
After individual written informed consent was obtained, demographic data were collected. Audio-recorded, in-depth interviews lasting 1-1.5 hours were conducted by one of two study co-leads using a semi-structured interview guide. HCPs were asked to describe their experiences of working with older adults with dementia and their caregivers in the ED, and to recall examples of what went right or wrong. Field notes were recorded post-interview to capture observations made during the interviews.
Data analysis
Transcripts were transcribed verbatim, with participants assigned a pseudonym. Qualitative data analysis was ongoing and iterative29, beginning with coding individual transcripts from the first provincial data set collected, followed by the second province, using constant comparative analysis30. Codes from individual transcripts were collapsed to categories initially representing manifest (visible) data, with categories further collapsed into themes representing the latent (interpretative) content26 that crossed both provincial data sets. Interpretation culminated in a conceptual model illustrating the interaction between the themes and their relationship to the balance between safety and harm. An ongoing detailed audit trail was kept to document research team discussions and decisions.
Ethics approval
Ethics approval was obtained from the University of Alberta Health Research Ethics Board (Panel B Study Pro00038003).
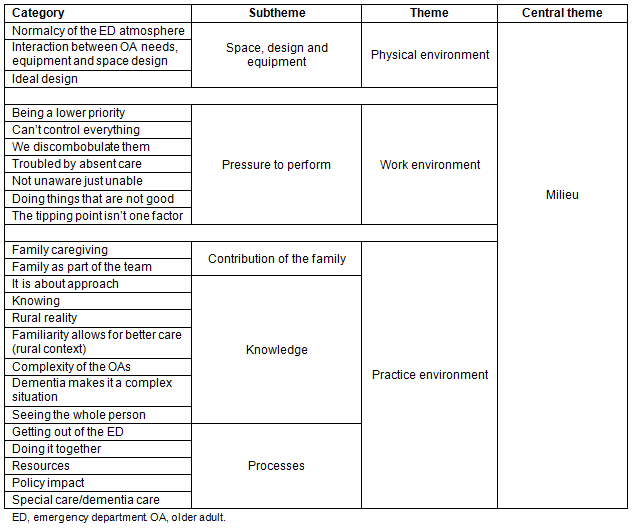
Twelve HCPs from two rural EDs participated, seven from one province and five from the other. Participants included seven HCPs whose clinical work responsibilities were in the ED, and five from hospital rehabilitation/social work or community liaison services who had consulting roles in the ED, with a mix of each from both sites. Participants were from nursing, social work, occupational therapy, physical therapy and medicine. Study findings reflect overlapping physical, social and organizational environments in which HCPs attempt to find a balance between safety and harm for older adults with dementia. Three themes were identified: physical environment, work environment and practice environment (Table 1).
Table 1: Final categories, subthemes and themes across participating emergency departments
Physical environment: space, design and equipment
The physical environment comprised interrelationships between treatment space purpose/expectations, design of the space and equipment. The interplay between these elements affected both the ability of the older person to function, and processes of care, producing consequences on the balance between safety and harm. The ED mission drove the physical design, creating a busy atmosphere, challenging for older adults with dementia. From the perspective of participants, the physical environment was not set up to meet the needs of older adults with dementia. Noise, overcrowding and lack of privacy created a sense of chaos and tension as part of the milieu. Traffic, commotion and noise made it difficult for patients with dementia to communicate their needs. One participant likened it to a crazy place, while another described the following.
When I go down there, it's like walking into a M*A*S*H unit or into a war zone. It's noise, noise, noise all the time. There's machines going off, there's people calling from one end to the other and there's ambulance crews out here. It would upset anybody in their normal mind, like what's goin' on here? ... I mean it's nothing to do with staff down there, it's to do with this is what an Emergency Room is used for. (Rosalie)
Tension arose from a desire to provide the right care for older adults with dementia within the chaotic atmosphere. HCPs were constantly weighing where to locate them in an environment built for acute patients requiring short-term medical intervention. Participants struggled about keeping the older person with dementia in the line of sight or locating them in a quiet out-of-the-way area.
If you put them in an isolated spot, they don't know what's happening. So really what we should be doing is trying to put them in an area where we can engage with them frequently, re-orientate them to time, give them information on what's happening ... But being right on the other side of the nurses' desk or doctors' desk where there's so much discussion that sounds like babble and people walking by them constantly isn't a good spot and yet they end up there a lot. (Valerie)
In critically thinking about the effect of the environment and using judgement to try to do the right thing, staff tried to create a balance between protecting their patients with dementia from the chaos (safety) while avoiding the psychological harm of isolation.
Interaction between older persons' needs (eg mobility, toileting, psychosocial, proximity of caregivers), equipment availability (eg bedrails, mobility aids, stretchers) and design of the space (eg layout, bathroom facilities, access to unmonitored exits) produced consequences for older adults. Participants identified only negative consequences within their current workspaces.
We probably only have 2 bathrooms for our facility. One of them ... there's a 4 bed ward and there's 1 bathroom to share with 4 patients, and then right across the hall there's another 2 bed, so that's basically 6 patients, they're sharing 1 bathroom. (Carol)
Participants identified positive consequences that might arise from a more dementia friendly ideal design. Environmental solutions and physical space changes could influence the ED experience, help staff monitor patients with dementia, provide adequate space and equipment for mobility and optimal function, and allow for family/caregiver involvement. Participants spoke of creating a safe space where the responsibility of keeping an eye on the person with dementia would be balanced with quiet and comfort.
What would be in it? Hmm. Well, a safe area where they could, if they were able to walk, they could walk. What would be in it? Honestly, nice mattresses ... Depending on the situation and the willingness of the caregivers or family, a phone so they could actually phone and get re-oriented if they were really feeling scared or upset ... (Emma)
For participants, dissonance existed between current reality and an idealized potential for the built environment.
Work environment: pressure to perform
The work environment was dominated by pressure to perform. Pressure emanated from conflicting priorities, lack of control and having to provide less-than-optimal care to the older adult with dementia. This pressure acted as a barrier to safe transitional care as staff were not unaware, but felt unable, to provide optimum care, which inadvertently contributed to the older adult with dementia being a lower priority. Staff saw themselves as too busy to care for such patients, and were compelled to choose who to see first on priority of needs. Processes such as triage played a role in setting priorities.
... this morning we had a person come to go in for an O.R. procedure and two ambulances arrive and the O.R. is calling. And you can only do so much at one time, hey. And so that, and that's the same with the dementia patient, like I mean even though you know that patient in the waiting room should get a bed. The O.R. is telling us triage, and triage, and triage ... (Sasha)
A consequence of such competing pressures was the perception that frail older persons did not do well in the ED. The pressure-filled work environment aggravated confusion, although staff recognized this and tried to find ways to mitigate harm.
When I'm prioritizing patients going up to beds that we've been given, frail elderly come first. So I get medical beds, frail elderly are first. I can keep the younger patients down here because they do much better in this environment than the frail elderly [who] just cannot manage it especially if there's a delirium or a dementia on board as well. We totally discombobulate them. It's awful. (Vanessa)
Another consequence was moral distress stemming from feeling troubled about absent care, not being able to control everything and being aware of care needs but being unable to meet them. Staff described doing things that were suboptimal care for short-term gain.
... and so we start to do terrible things like drugging or tying their wrists to the rail to make sure they can't undo their IV which makes you feel awful ... It still keeps them safe and where they're supposed to be, but it's not good nursing and of course then they don't get clean and they have no concept of, okay, it's morning, I'm gonna have my breakfast. They're not getting any activity because we're in a rush so they're not being walked to the bathroom. (Emma)
Survival mechanisms for staff included constantly juggling priorities and decision making, becoming task oriented and living with lesser quality care than what they wanted to provide. Multiple tipping points, including the older person staying too long in the ED when access internal hospital or limited external community resources and a health system demand for ED services, led to a crisis management orientation as the mode of operation.
I think, like most emergency rooms, we operate in crisis mode. So we respond to people going into crisis when they become confused or agitated. So we tend to respond after that's occurred which, I think, is the worst possible way to do that. It leads to a lot of delirium. (Tabitha)
Trying harder and working faster were not always enough as pressure and time constraints left HCPs unable to address the needs of patients with dementia. HCPs recognized that sometimes simple solutions were a way of preventing harm, and being strapped for time led to poor care and outcomes. They had little time to give and did the best they could in the circumstances.
Practice environment: family, knowledge and processes
This theme involves people and their roles, their knowledge, and how people use knowledge in the processes of care. The practice environment consists of three subthemes: contribution of family, knowledge and processes.
Contribution of family: This subtheme reflects HCP's sensitivity to the family's situation prior to coming to the ED and their ability to sustain care at home, helping or hindering the families' role in the ED environment. Within the subtheme are multiple co-existing facets that were constantly in motion, including the family role in provision of basic care, background factors and challenges faced by caregivers in the ED.
We had a situation where a woman was found wandering in the neighborhood and had had a fall. She had had dementia for a number of years, but it was progressive, progressing. She refused to let anybody in the home. She had a dear, dear lovely husband who was weary, very weary, and a son who had a life, he had a wife and young children. (Mabel)
Participants accepted that not all families contributed in the same way and the ability to contribute was fluid. Participants recognized the need to be aware of potential family burnout or lack of resources.
And so it's looking at the bigger picture and recognizing that sometimes people with dementia are in the Emergency Room because the family who are often looped [overwhelmed] and must be burnt out ... there's nothing physically wrong with them. ... [The person with dementia is] just here because their family can't do it anymore. (Rosalie)
Many participants saw the older person with dementia and the family as the unit of care, and that HCPs had an obligation to both the older person with dementia and their family caregivers to ensure a safe transition through the ED.
... we don't often think of them [caregivers] as being the primary recipient of our care but they go together, right. You have, they have to go together as a unit and so if we, if we fail the caregiver, we fail the client. (Jen)
Caregivers and older adults were viewed as a package deal, and caregivers were valued for their contribution in the ED environment such as bringing in information or attending to basic care needs. Having a family member present reduced potential harm to the older person with dementia.
A lot of times what I see is if there's a caregiver with the patient, that's the person giving the care. The nurse does the vitals and gives the meds, but ultimately we kind of rely on the person who's with that person. (Emma)
Now, if a caregiver comes in or a family member is willing to stay, they do far better. (Vanessa)
Caregivers were also viewed as part of the team and their actions key to either helping or hindering the situation. Absence of family could mean negative consequences for the older person with dementia.
I find that that happens a lot and it's, you know it's unfortunate because even, even new onset dementia patients, they still know the majority of their family and it's, you know not having them here makes them more agitated. (Lee)
I guess [in] my experience, those people usually end up being admitted if there's no, if there's absolutely no family support. (Kate)
Knowledge: There were different types and sources of knowledge. Some was speciality knowledge of dementia and older people, and some knowledge arising from being in a rural community. HCPs recognized the need for application of specialty gerontological knowledge when working with people with dementia. While not all participants had such training or experience, they recognized the value that specialized knowledge brought to caring for patients with dementia. Participants spoke of the importance of a knowledgeable approach and knowing to ask the right questions.
But it's knowing how to ask those questions, taking the time and having that lens ... I think the lens is social work or the lens is a nurse that's got specialties in geriatrics. Just that you have those skills, you have that psychosocial, that's your focus and you know the questions to ask and you ask them. (Mabel)
Specialty knowledge acquired through education or experience in working with older adults influenced how HCPs defined and carried out their role. One participant with such experience identified as being a patient advocate for those with dementia. For another, teaching others was important.
... it's a teaching process ... with the staff, emergency staff. You know that, you know someone with dementia needs to have, be in a safe environment, so you need to consider ... the living, the living options where they're gonna be turned home to, to ask, ask the questions and not just send them out the door in a taxi. (Kate)
Knowing came from moving beyond the superficial when working with patients with dementia. Dementia contributed to complexity, and it was important to see the whole person by understanding where that person had come from and understanding their baseline function in order to move to a deeper level of knowledge of the person. For HCPs, safety involved taking account of multiple potential scenarios, putting the pieces together and seeing the bigger picture in order to arrive at an action plan. The consequences of not going beyond the superficial could inadvertently contribute to potential harm.
And we weren't looking for other signs 'cause dementia patients can't always tell you how they're feeling, you have to be a detective and look for other physical signs to see what's going on ... And so we missed out on some of the clues and sent him home. And he was unsteady on his feet, but we didn't appreciate the fact he wasn't before. And so the unsteady on his feet probably was low blood pressure and they were just assuming he was unsteady on his feet. (Valerie)
Being in a rural community brought with it perceived advantages and disadvantages. Participants identified this meant that there were many older people accessing the hospital, and that encountering people living with dementia was common. Advantages of being in rural community came from knowing and recognizing people when they came to the ED, which created a safety net for those with dementia.
I think there can be really wonderful things about working in a rural area. We know and often individually care about these patients. They sometimes recognize us which rarely happens in an urban environment and that is an advantage. We also recognize when they're not normal which is an advantage. (Tabitha)
Close relationships and networking between hospital and community staff were perceived to contribute to pre-existing or easy access to knowledge about patients, a part of the community-oriented attitude in a rural ED. Small-town knowing, including knowing how to find contacts in the community that could have important information and tapping into the older persons' network of contacts, often created safety.
Also, what's really good about a rural little setting here is that easy connections with home care, there's one person to call or, not just one 'cause it's the liaison nurse, we know exactly who the social workers are. (Claire)
However, the rural advantage did not always work, and familiarity had the potential to be a double-edged sword.
So the small town ... Well, it can be helpful or it can be detrimental. It could be helpful in that you don't have to do quite as much diggin' around 'cause you may know all the pieces, but the picture might be different and you might make assumptions. (Mabel)
Processes: Processes, the final subtheme, contributes to the practice environment by explaining how people with dementia receive or do not receive care for their presenting problem. Policy-driven processes such as triage involve activities that focus on getting the patient treated and out of the ED. Recognizing the influence of dementia on processes was key to facilitating safety and avoiding harm. Getting out of the ED involved formulating a plan for either admission to the hospital or community discharge, and executing processes to enact the plan.
... the client is either admitted to the hospital until we can make a safe and successful discharge plan. Or they can go home you know with a family member to, to supervise until you know other arrangements can be made in the assessment ... by homecare. (Kate)
Getting the older person with dementia home involved doing it together through teamwork. The inside part of the team (those whose work was ED based) functioned on an efficiency model, dealing with those that fit the ED service mandate (acute illness) and moved along when biomedical needs were addressed. The outside team members were hospital staff brought in as consultants to organize resources for a community discharge or advocate for an admission if the resources in the community were insufficient.
... [the] discharge planner is the best one to talk to, she will tell you all about that side of the world ... they are the ones that really are, are exceptional at doing those linkages and really knowing what's available. (Jen)
Infrastructure resources and administrative policies drove system and care processes, which resulted in positive or negative outcomes for older people and affected HCP performance of roles and responsibilities. Some policies, an example being a delirium protocol, were perceived as improving safety. However, limited availability of resources within the ED (personal and consulting HCPs, time and access to beds and food) and community resources (primary care services and home care) affected the balance between safety and harm.
Quite often we will say to our liaison staff, 'Can we not get this person home with 'round the clock care?' So it used to be, just a few weeks back, that they could do that for short periods of time. Now there's a delay 'cause they have to ask permission of their bosses to be able to do that. (Vanessa)
ED staff perceived weekends as a particularly challenging time for caring for patients with dementia and meeting the need to move people out of ED. Many hospital and community services were available only during weekdays or office hours.
And homecare doesn't go 24 hours ... So if they're coming in at night, and there's ... nobody there for them to head home, yes they need to be admitted at the hospital or at least stay in emergency 'til morning ... (Carol)
Participants were sensitive to the special care needs of those with dementia and the ways in which processes may or may not meet their needs. HCPs recognized that staying long periods in the ED was detrimental, but also identified numerous potential solutions to address challenges with the ED practice environment for those with dementia. Solutions ranged from increased staff resources to help meet basic care needs, distracting activities, changing the physical environment, putting in place a plan of care and even exploring changes to key processes such as triage.
I think it's helpful to have a care plan particularly for frequent presenters with dementia. I think that triage is a very useful thing, but doesn't always determine the best placement of the patient or the best timing for that placement, that there are some other things that can weigh very heavily on the patient's eventual outcome and that the triage system can be more flexible. (Tabitha)
Creating milieu
The themes of physical environment, work environment and practice environment overlapped and worked synergistically to converge and create the milieu of the rural ED. Safe transitional care for older adults with dementia within the ED was positively or negatively influenced by these interacting environments. The ED existed at the interface of the hospital inpatient and community services, and this milieu was one in which HCPs constantly attempted to balance safety and risk of harm for older adults with dementia. The conceptual model developed illustrates how the overlapping environments and resulting milieu in the rural ED, which existed between the community and hospital, rested on a balance between safety and harm for people living with dementia (Fig1).
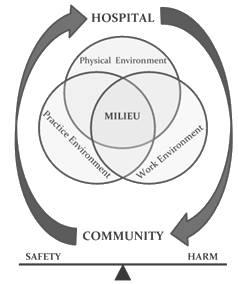
Figure 1: Balancing safety and harm for older adults with dementia in rural emergency departments.
Discussion
The unique contribution of this study is the focus on care of older adults with dementia in rural EDs, and perceived rural advantages and disadvantages in the provision of safe transitional care to these individuals and their caregivers while coming to, being in and leaving the ED. While others studies have included HCP perspectives1,8,31 on care of older people with dementia in EDs, the findings of this study illuminate what McCusker et al16 suggested might exist in rural EDs with regards to links to community. Participants in this study identified a rural advantage by knowing the person from repeat visits to the ED in a small regional hospital and knowledge of who to connect with in local community services, and how to do this, within this context. Participants were aware that this advantage could also be a disadvantage, a double-edged sword, if familiarity leads to assumptions about the individual and complacency in looking for changes in function and health status.
Many participants expressed a broad conceptualization of safety and appreciated the influence of physical, work and practice environments on the physical, cognitive and emotional wellbeing of older adults with dementia. Other participants, as illustrated by the HCP describing keeping patients 'safe' through use of restraints, wrestled with reconciling concepts of safe care with quality care. HCPs working at the interface of hospital and community services constantly balance promoting patient safety and minimizing harm. Strategies to prevent harm included locating the older person in the ED environment to prevent worsening of cognition or isolation, viewing family as part of the unit of care and valuing their contribution, as well as moving the person with dementia out of ED as quickly as possible to an inpatient bed or to the community with support. This is in contrast to Moyle et al's32 study of inpatient care of people with dementia, where staff narrowly defined safety as risk management and emphasised this over wellbeing and dignity. Both of the participating EDs in this study had access to consulting staff from hospital inpatient services (social work and rehabilitation) and hospital-based community liaison workers, services that may not be available in all rural jurisdictions. This, along with rural community connections, may have contributed to the perception of safety and harm involving more than single incidents and procedural complications.
Specialty knowledge of dementia care may play a role in perceptions of safety and harm, but education alone is unlikely to be effective in achieving positive consequences for people with dementia in the ED as the physical environment, pressure to perform and care processes stemming from administrative policies would remain. Organizational change is complex. Creating successful knowledge translation to achieve organizational change involves individual understanding of new knowledge, autonomy in decision making, resources to sustain change and system facilitators to alter contextual factors33. Further research is needed to more fully understand how potential harm for those with dementia transitioning through ED can be mitigated through a combination of strategies addressing the interacting environments and resulting milieu.
The double-edged sword of familiarity, varying perceptions of safety and harm for older persons with dementia and the need to address specialty knowledge along with organizational change has implications for staff as well as at administrative and policy levels. Rural ED HCPs need to be aware of potential risk of overlooking change in status when assuming prior knowledge of the person. Establishing care processes that include a review of current functional status and health status through actively engaging and seeking input from family and other community caregivers regarding changes and usual approaches to care has potential to mitigate risk. HCPs from both inside and outside EDs need opportunities to discuss perceptions of safety and harm and come to a common understanding within their local context. Such discourse could lead to development of strategies to minimize harm including involving families as partners in care. Organizational policy is needed to change the approach to triage of older adults with dementia to one that incorporates specialized gerontological knowledge, and creates elder-friendly physical environments that support practice. The findings of this study support the value of access to the outside team, those with knowledge of community services, as part of facilitating a broader understanding of safety and harm that extends beyond the ED walls. Administrators and policy makers should seek opportunities to make this type of support available in rural EDs seven days a week.
A limitation of the study is that only two rural EDs and a small number of HCPs were included. Perceptions of safety and harm in the ED for older adults with dementia in other jurisdictions needs to be explored. While moral distress among staff was present in the data, it was not explored in depth. This should be examined in future research. As well, there was a suggestion of system ageism and dementiaism in the data, but it was insufficient to include as it did not cross both data sets. Further research on belief systems will be important for understanding and transforming ED care environments.
HCPs in rural EDs are at the interface of hospital and community and attempt to balance promoting safety and avoiding harm for older adults with dementia. Participants perceived safety broadly, grasping consequences of the milieu created through physical, work, and practice environments on the physical, cognitive and emotional wellbeing of older adults with dementia. The practice environment, in which HCPs identified a 'rural advantage', was tied to knowledge of community and the people with dementia and caregivers who sought care in the participating EDs.
Acknowledgements
Funding for the research came from a Canadian Institute of Health Research Catalyst Grant: Health Services and Systems for an Aging Population.
The authors would like thank Cheryl Beach for her efforts to facilitate recruitment to the study.
References
1. Parke B, Hunter KF, Strain LA, Marck P, Waugh EH, McClelland A. Facilitators and barriers to safe emergency department transitions for community dwelling older people with dementia and their caregivers: a social ecological study. International Journal of Nursing Studies 2013; 50(9): 1206-1218. https://doi.org/10.1016/j.ijnurstu.2012.11.005
2. Thomas EJ, Brennan TA. Incidence and types of preventable adverse events in elderly patients: population based review of medical records. BMJ 2000; 320(7237): 741-744. https://doi.org/10.1136/bmj.320.7237.741
3. Grossmann FF, Zumbrunn T, Ciprian S, Stephan F-P, Woy N, Bingisser R, et al. Undertriage in older emergency department patients - tilting against windmills? PLoS ONE 2014; 9(8): e106203. https://doi.org/10.1371/journal.pone.0106203
4. Parke B, Chappell NL. Transactions between older people and the hospital environment: a social ecological analysis. Journal of Aging Studies 2010; 24(2): 115-124. https://doi.org/10.1016/j.jaging.2008.09.003
5. McKhann GM, Knopman DS, Chertkow H, Hyman BT, Jack CR, Kawas CH, et al. The diagnosis of dementia due to Alzheimer's disease: recommendations from the National Institute on Aging-Alzheimer's Association workgroups on diagnostic guidelines for Alzheimer's disease. Alzheimer's & Dementia 2011; 7(3): 263-269. https://doi.org/10.1016/j.jalz.2011.03.005
6. Gray LC, Peel NM, Costa AP, Burkett E, Dey AB, Jonsson PV, et al. Profiles of older patients in the emergency department: findings from the interRAI multinational emergency department study. Annals of Emergency Medicine 2013; 62(5): 467-474. https://doi.org/10.1016/j.annemergmed.2013.05.008
7. Schnitker LM, Beattie ERA, Martin-Khan M, Burkett E, Gray LC. Characteristics of older people with cognitive impairment attending emergency departments: a descriptive study. Australasian Emergency Nursing Journal 2016; 19(2): 118-126. https://doi.org/10.1016/j.aenj.2016.04.002
8. Cadogan MP, Phillips LR, Ziminski CE. A perfect storm: care transitions for vulnerable older adults discharged home from the emergency department without a hospital admission. The Gerontologist 2016; 56(2): 326-334. https://doi.org/10.1093/geront/gnu017
9. Hodgins MJ, Wuest J. Uncovering factors affecting use of the emergency department for less urgent health problems in urban and rural areas. Canadian Journal of Nursing Research 2007; 39(3): 78-102.
10. Forbes DA, Hawranik P. Looming dementia care crisis: are Canadian rural and remote settings ready? In: J Kulig, AM Williams (Eds). Health in rural Canada. Vancouver, BC: UBC Press, 2012; 447-461.
11. Forbes DA, Markle-Reid M, Hawranik P, Peacock S, Kingston D, Morgan D, et al. Availability and acceptability of Canadian home and community-based services: perspectives of family caregivers of persons with dementia. Home Health Care Services Quarterly 2008; 27(2): 75-99. https://doi.org/10.1080/01621420802022548
12. Forbes DA, Morgan D, Janzen BL. Rural and urban Canadians with dementia: use of health care services. Canadian Journal on Aging 2006; 25(3): 321-330. https://doi.org/10.1353/cja.2007.0003
13. Bowd AD, Loos CH. Needs, morale and coping strategies of caregivers for persons with Alzheimer's disease in isolated communities in Canada. American Journal of Alzheimer's Disease and Other Dementias 1996; 11(3): 32-39. https://doi.org/10.1177/153331759601100305
14. Bail K, Hudson C, Grealish L, Shannon K, Ehsen S, Peaut A, et al. Characteristics of rural hospital services for people with dementia: findings from the Hospital Dementia Services Project. Australian Journal of Rural Health 2013; 21(4): 208-215. https://doi.org/10.1111/ajr.12041
15. De Freitas TL, Spooner GR, Szafran O. Admissions and transfers from a rural emergency department. Canadian Family Physician 1998; 44: 789-795.
16. McCusker J, Roberge D, Ciampi A, Silva RB, Vadeboncoeur A, Larouche D, et al. Outcomes of community-dwelling seniors vary by type of emergency department. Academic Emergency Medicine 2012; 19(3): 304-312. https://doi.org/10.1111/j.1553-2712.2012.01295.x
17. Harris L, Bombin M, Chi F, deBortoli T, Long J. Use of the emergency room in Elliot Lake, a rural community of Northern Ontario, Canada. Rural Remote Health (Internet) 2004; 4(1): 1-12. Available: www.rrh.org.au (Accessed 26 June 2012).
18. Zubieta L, Bequet S. Factors of primary care demand: a case study. Rural Remote Health (Internet) 2010; 10(4): 1-12. Available: www.rrh.org.au (Accessed 26 June 2012).
19. Coleman EA, Boult C. American Geriatrics Society Health Care Systems Committee. Improving the quality of transitional care for persons with complex care needs. Journal of the American Geriatrics Society 2003; 51(4): 556-557. https://doi.org/10.1046/j.1532-5415.2003.51186.x
20. Davies JM, Hébert P, Hoffman C. The Canadian patient safety dictionary. Ottawa, ON: The Royal College of Physicians and Surgeons of Canada, 2003.
21. Long SJ, Brown KF, Ames D, Vincent C. What is known about adverse events in older medical hospital inpatients? A systematic review of the literature. International Journal for Quality in Health Care 2013; 25(5): 542-554. https://doi.org/10.1093/intqhc/mzt056
22. Ackroyd-Stolarz D, Read Guernsey J, MacKinnon NJ, Kovacs G. The association between a prolonged stay in the emergency department and adverse events in older patients admitted to hospital: a retrospective cohort study. BMJ Quality & Safety 2011; 20(7): 564-569. https://doi.org/10.1136/bmjqs.2009.034926
23. Moos RH. Social-ecological perspectives on health. In: GC Stone, F Cohen, NE Alder (Eds). Health psychology. San Francisco, CA: Jossey-Bass; 1979; 523-547.
24. Stokols D. Establishing and maintaining healthy environments: toward a social ecology of health promotion. American Psychologist 1992; 47(1): 6-22. https://doi.org/10.1037/0003-066X.47.1.6
25. Rubinstein RL, De Medeiros K. Ecology and the aging self. In: H Wahl, RJ Scheidt, PG Windley (Eds). Focus on aging in context: socio-physical environments. Philadelphia, PA: Springer, 2004; 59-83.
26. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Education Today 2004; 24(2): 105-112. https://doi.org/10.1016/j.nedt.2003.10.001
27. Field PA, Morse JM. Nursing research: the application of qualitative approaches. Rockville, MD: Aspen, 1985.
28. Creswell JW. Qualitative inquiry & research design: choosing among five approaches, 2nd edn. Thousand Oaks, CA: Sage, 2007.
29. Morse, JM. Determining sample size. Qualitative Health Research 2000; 10(1): 3-5. https://doi.org/10.1177/104973200129118183
30. Goertz JP, LeCompte MD. Ethnography and qualitative design in educational research. Orlando, FL: Academic Press, 1984.
31. Boltz M, Parke B, Shuluk J, Capezuti E, Galvin JE. Care of the older adult in the emergency department: nurses' views of the pressing issues. The Gerontologist 2013; 53(3): 441-453. https://doi.org/10.1093/geront/gnt004
32. Moyle W, Borbasi S, Wallis M, Olorenshaw R, Gracia N. Acute care management of older people with dementia: a qualitative perspective. Journal of Clinical Nursing 2011; 20(3-4): 420-428. https://doi.org/10.1111/j.1365-2702.2010.03521.x
33. Kitson AL. The need for systems change: reflections on knowledge translation and organizational change. Journal of Advanced Nursing 2008; 65(1): 217-228. https://doi.org/10.1111/j.1365-2648.2008.04864.x




