Introduction
A primary care physician's decision to refer has an enormous impact on the cost and quality of care that patients receive. Appropriate referrals can result in rapid diagnosis and treatment for a patient; whereas, inappropriate referrals may lead to unnecessary tests and procedures, increased healthcare costs, added risk for morbidity1, and decreased access for patients in need of subspecialty care.
Despite the large impact on health care, few studies have been performed on the referral patterns of general and family practitioners. Of the studies reported in the literature, some are outdated or performed outside the USA2-7,11, and many disagree on their conclusions1,3-5,8-12. Important factors identified by a 1992 British study included availability of qualified consultants and length of physician training1. A 1997 US study reports that a physician's sex influences their decision to refer2. In order to help clarify and identify influential factors pertinent to current health care in the US, a survey was designed, including selected items from previous studies1-21, and was mailed to 2400 family and general practitioners in the US.
Methods
A survey was designed to select the most consistently discriminating and influential factors from previous studies1-5,7,8,11-13,15-17 but to be concise enough for a clinician to complete within a few minutes. A scanable format was used for easy compilation of large amounts of data and to minimize data entry errors. Mailing lists of 1200 randomly selected physicians were purchased separately from the American College of Osteopathic Family Physicians (ACOFP) and the American Academy of Family Physicians (AAFP). In March 2002, surveys were mailed to the two groups. In order to increase the response rate, there were two follow-up mailings sent to non-responders at 2 and 4 weeks following the initial mailing. Main outcome measures included: physician gender, age, degree, training (residency vs internship), years in practice, type of practice, population, of the practice site, and perceived workload. The survey methodology was approved by the Institutional Review Board of the University of North Texas Health Science Center at Fort Worth.
Statistical Analysis
Demographic and professional characteristics of survey respondents were summarized using numbers (percentages) for each categorical variable. The referral rate to specialty physicians was self-reported as one of the following categories: 2% or less, 3-4%, 5-6%, 7-8%, 9-10%, 11-12%, 13-14%, and 15% or more. Logistic regression was then used to compute crude and adjusted odds ratios (OR) and 95% confidence intervals (CI) for factors associated with high levels of physician referral. For these analyses, high referral was determined to correspond to approximately the top quartile of responses (11% or greater). Potential confounders that were controlled in these analyses included age, gender, professional degree, residency completion status, type of practice, self-reported workload, years in practice, and practice site population. Analyses were performed with the SYSTAT statistical software package (Systat Software Inc, Richmond, CA, USA), using p = .05 as the criterion for statistical significance.
Results
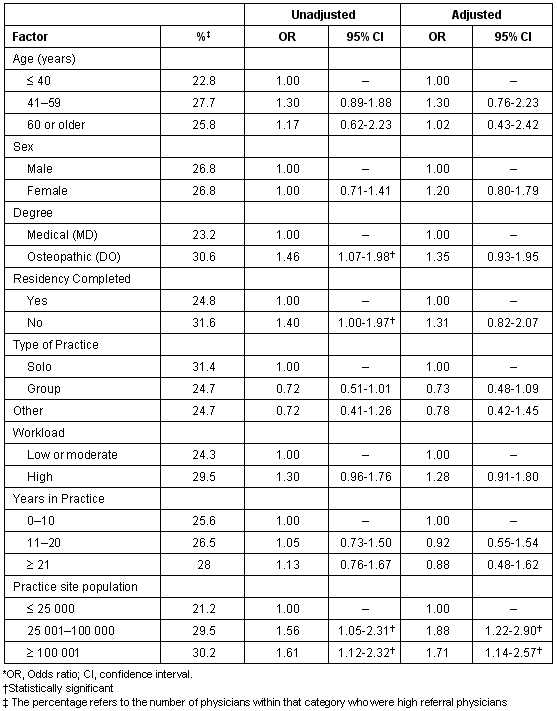
Eight hundred eighty-two (37%) surveys were returned. The demographic and professional characteristics of respondents are presented (Table 1). The distribution of reported physician referral is presented (Table 2). The unadjusted and adjusted factors associated with high referral are presented (Table 3). After adjustment for confounding variables, the only category significantly associated with high referral rates was the population of the practice site. A physician practising in a city with a population of 25 001-100 000 was 1.88 times (75% CI, 1.22 -2.90) more likely to be in the high referral rate category than a physician in a town of fewer than 25 000 people. Physicians in cities of more than 100 000 were 1.71 times (95%, CI, 1.14-2.57) more likely to be in the high referral category than their peers in towns of less than 25 000.
Table 1: Demographic and professional characteristics of survey respondents
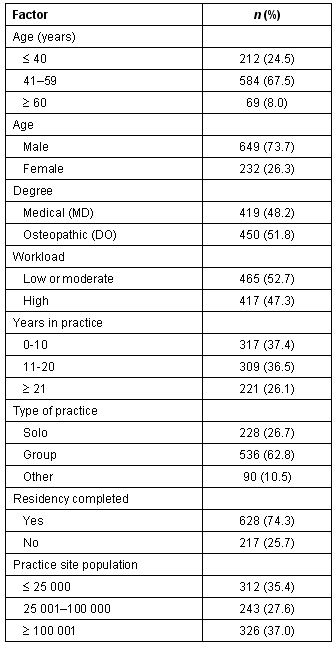
Table 2: Levels of physician referral
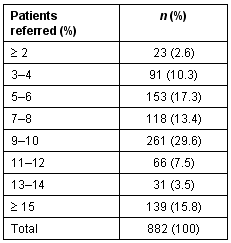
Table 3: Factors associated with high levels of physician referral*
Discussion
Physicians practising in less populated areas refer patients less frequently. Roland and Morris3, in a 1988 UK study, claim that availability of specialists is a major influence on referral rates of family physicians. Similarly, another study conducted in the UK demonstrated that the availability of qualified consultants is the most common factor influencing a physician's decision to refer1. Despite differences in healthcare systems between the UK and USA, these findings may help to explain why this study demonstrated less frequent high referral rates among physicians in smaller towns. Forrest et al14 noted that because of the differences in structure in the nations' healthcare systems, only 1 in 7 patients were referred per year in the UK, versus 1 in 3 patients per year in the USA. The researchers cited fewer specialists and decreased availability of specialists as factors in lower referral rates in the UK. Rural areas in the USA may face similar circumstances with fewer specialists, possibly resulting in decreased availability of specialists and lower referral rates. Of note, Forrest et al made no claim that one group refers too often or not enough based on outcomes, but reported that general practitioners in the UK believe the long waiting lists for appointments with specialists threaten their capacity to deliver high quality care. A 1996 Finnish study found that distance to a specialist was not a large factor influencing referrals, but did find that physicians in smaller municipalities had lower referral rates4. A 2003 Canadian study agrees with the finding that smaller town physicians refer less frequently, but contradicts the former findings by reporting that specialist supply was unrelated to referral rates22.
The current study found no statistically significant difference in referral rates by age of physician or sex of physician. Franks and Clancy8 found that the average age of physicians who referred versus those who did not was nearly identical and, therefore, dismissed age as a major factor in referral patterns. This is contrary to a study by Bachman and Freeborn13, which demonstrated that younger physicians have higher referral rates. Some authors10 have argued that older physicians generally have an older (and sicker) patient population, which can skew the referral rates, which has now been confirmed by a 2003 Canadian study22. Three studies demonstrate that female physicians are more likely to refer than their male counterparts8,12,22.
Another factor possibly related to high referral rates is the amount of training (ie, internship only vs residency). In support of the lack of influence of residency training, Franks and Clancy8 showed that referral rates between general and family practitioners (ie, non-residency vs residency trained) are nearly identical. This could be explained by the fact that physicians who are not residency trained are generally older and have more collective years of experience than residency trained physicians. This may equalize their comfort level in managing similar cases. In the interviews performed by Newton et al2, one physician stated, 'I refer fewer patients now than at the beginning of my career. I think it's an increase in experience, having seen something before, and having had a consultant opinion about it in the past.' Vehvilainen et al agree with the claim that less experience leads to more referrals. In contrast, two studies suggest the more experience and expertise a physician has, the more likely he or she is to refer a patient4,5. As a whole, the current evidence concerning residency training and referral rates is inconclusive.
Previous research demonstrates an association between workload (patients/hour) and fewer referrals13. The current study, however, found no statistically significant difference in referral rates between those with a perceived high workload and those with a perceived low or moderate workload. Additionally, the current study found no difference in referral rates among different types of practice (solo, group, or other). No prior studies compared referral rates between physicians trained in different types of medical schools (DO vs MD).
This research has focused solely on physician characteristics associated with a high referral rate. Previous research does not distinctly delineate whether physician or patient characteristics are more influential on physician referral rates9,17. One weakness of this study is that the physicians' referral rates were self-reported. The accuracy of these estimates is difficult to determine and a more objective method of measuring consult may very likely yield significantly different results even if gathered from the same physicians. Personal biases such as a desire to appear qualified to manage difficult patients may have influenced the reported values. Additionally, as with any cross-sectional study, a cause and effect relationship cannot be demonstrated.
With the increasing amount of research that has surfaced recently on factors influencing referral rates, future research should focus on how to define appropriate referrals. With this information, we may be able to more accurately determine weaknesses in our healthcare system and training, and make appropriate adjustments. Some suggestions for changes have been proposed, such as changing our current 'gatekeeper' system into one where there is more free access to specialists18. It is important to note that an increased referral rate has not been associated with a decreased quality of referrals1,5,6,10
Conclusions
As hypothesized, family practice physicians in larger towns and cities were more likely to have a high referral rate than physicians in smaller towns. After controlling for possible confounders, practice site population was the only variable significantly associated with high referral rate. Non-residency trained physicians referred more than residency-trained physicians, but this relationship did not persist after controlling for confounders. Additionally, osteopathic physicians (DOs) had a significantly higher referral rate than MDs before controlling for confounding variables. High levels of physician referrals were not associated with age, sex, type of practice (solo, group, other), perceived workload, or years in practice.
Acknowledgement
Funded by a grant from the American Osteopathic Association (AOA).
References
1. Nutting PA, Franks P, Clancy CM. Referral and consultation in primary care: Do we understand what we are doing? Journal of Family Practice 1992; 35: 21-23.
2. Newton J, Hayes V, Hutchinson A. Factors influencing general practitioners' referral decisions. Family Practice 1991; 8: 308-313.
3. Roland M, Morris R. Are referrals by general practitioners influenced by the availability of consultants? BMJ 1988; 297: 599-600.
4. Vehvilainen AT, Kumpusalo EA, Voutilainen SO, Takala JK. Does the doctor's professional experience reduce referral rates? Evidence from the Finnish referral study. Scandinavian Journal of Primary Health Care 1996; 14: 13-20.
5. Reynolds GA, Chitnis JO, Roland MO. General practitioners outpatient referrals: Do good doctors refer more patients to hospitals? BMJ 1991; 302: 1250-1252.
6. Knotterus JA, Joosten J, Daams J. Comparing the quality of referrals of general practitioners with high and average referral rates: an independent panel review. British Journal of General Practice 1990; 40: 178-181.
7. Vehilainen AT, Kumpusalo EA, Takala JK. Reasons for referrals from general practice in Finland. Scandinavian Journal of Primary Health Care 1997; 15: 43-47.
8. Franks P, Clancy CM. Referrals of adult patients from primary care: demographic disparities and their relationships to HMO insurance. Journal of Family Practice 1997; 45: 47-53.
9. Franks P, Zwanziger J, Mooney C, Sorbero M. Variations in primary care physicians' referral rates. Health Sciences Research 1999; 34: 323-329.
10. Roland MO, Bartholomew J, Morrell DC, McDermott A, Paul E. Understanding hospital referral rates: a user's guide. BMJ 1990; 301: 98-102.
11. Stoverinck MJM, Lagro-Janssen ALM, Van Weel S. Sex differences in health problems, diagnosis, testing, and referrals in primary care. Journal of Family Practice 1996; 43: 567-576.
12. Franks P, Williams GC, Zwanziger J, Mooney C, Sorbero M. Why do physicians vary so widely in their referral rates? Journal of General Internal Medicine 2000; 15: 163-168.
13. Bachman KH, Freeborn DK. HMO physicians' use of referrals. Social Science & Medicine 1999; 48: 547-557.
14. Forrest CB, Majeed A, Weiner JP, Carroll K, Bindman AB. Comparison of specialty referral rates in the United Kingdom and the United States: retrospective cohort analysis. BMJ 2002; 325(7360): 370-371.
15. Wright J, Wilkinson J. General practitioners' attitudes to variations in referral rates and how these could be managed. Family Practice 1996; 13: 259-263.
16. Donohoe MT, Kravitz RL, Wheeler DB, Chandra R, Chen A, Humphries N. Reasons for outpatient referrals from generalists to specialists. Journal of General Internal Medicine 1999; 14: 281-286.
17. Shea D, Stuart B, Vasey J, Nag S. Medicare physician referral patterns. Health Service Research 1999; 34: 331-348.
18. Bodenheimer T, Lo B, Casalino L. Primary care physicians should be coordinators, not gatekeepers. Journal of the American Medical Association 1999; 281: 2045-2049.
19. Forrest C B, Nutting PA, Starfield B, Von Schrader S. Family physician's referral decisions: results from ASPN referral study. Journal of Family Practice 2002; 51: 215-222.
20. Gruen R L, Knox S, Britt H. Where there is no surgeon: the effect of specialist proximity on general practitioners' referral rates. Medical Journal of Australia 2002; 177: 111-115.
21. Tabenkin H, Oren B, Sterinmetz D, Tamir A, Kitai E. Referrals of patients by Family physicians to consultants: A survey of the Israeli Family practice research. Family Practice 1998; 15: 158-164.
22. Chan BT, Austin PC. Patient, physician, and community factors affecting referrals to specialists in Ontario, Canada: a population-based, multi-level modeling approach. Medical Care 2003; 41: 500-511
Abstract
Introduction:
Variability in the referral patterns of primary care physicians is well established. The objective of this study was to determine which factors have the most impact on a family physician's decision to refer a patient.Methods: In March 2002, surveys were mailed to 1200 randomly selected members of the American College of Osteopathic Family Physicians (ACOFP) and 1200 randomly selected members of the American Academy of Family Physicians (AAFP). To increase the response rate, there were two follow-up mailings to non-responders at 2 and 4 weeks following the initial mailing. Main outcome measures included: physician and practice characteristics (ie, age, sex, degree, training, practice type, population) and perceived workload. 'High' referral rate was defined as 11% or more of patients seen (the top quartile in the survey). Logistic regression models were used to determine which factors influence physician referral rate. Variables of interest for predicting high referral rates were age group, gender, DO versus. MD, residency training, perceived workload, years in practice, type of practice, and practice site population.
Results: Four hundred and fifty surveys sent to ACOFP members and 419 of those sent to AAFP members were returned (37% overall response rate). The significant differences in referral rates were for DO versus MD (OR = 1.46; 95% CI, 1.07-1.98); residency trained versus not residency trained (OR = 1.40; 95% CI, 1.00-1.97); and population of the practice site: 25 001-100 000 (OR = 1.56; 95% CI, 1.05-2.31) and more than 100 000 (OR = 1.61; 95% CI, 1.12-2.32). After adjustment for potential confounding variables, the only significant finding was population of the practice site, 25 001-100 000 (OR = 1.88; 95% CI 1.22-2.90) and more than 100 000 (OR = 1.71; 95% CI, 1.14-2.57).
Conclusions: The only factor that showed a significant association with having a high referral rate was the population of the practice site. Physicians in larger towns and cities have higher referral rates than physicians in small towns.
Key words: consultations, family practice style, patient population, primary care, referrals.
You might also be interested in:
2007 - An innovation in Australian dental education: rural, remote and Indigenous pre-graduation placements
2006 - Medical students' assessments of skill development in rural primary care clinics



