Myanmar, in South-East Asia, has a population of 51.4 million population. Malaria, which is a tropical disease, is prevalent in 284 of 330 townships, with a morbidity rate of 6.44/1000 population in 2013; early two-thirds (62%) of the population has a malaria risk. Malaria is a major public health problem in Myanmar and the National Malaria Control Programme (NMCP) has been promoting intense malaria control programs nationwide. Since 2006-2007, community-based malaria control activities have been implemented in 182 townships and a 3875 malaria volunteers have been trained. These volunteers reach out to rural areas and conduct community-based malaria control programs, which include early case detection and prompt treatment, provision of health education to the community and notification of the health authorities in case of a potential malaria epidemic. Although the NMCP's programs encourage community participation in malaria control, most of its approaches are set up and directed by health authorities, and communities are only passively involved. Thus, community members have no opportunity to participate in the program planning stage. Moreover, malaria volunteers for community-based malaria programs are directly selected by the health program authorities1.
It has been suggested that a community-based health program should be delivered using a community development approach that focuses on its members' perceptions and motivations to improve health care for every individual of that community. The community should be actively involved in the program from the start of its planning and should be mobilized to increase participation in the program2.
It is particularly important to improve knowledge and skills in community malaria control because community participation has been shown to be effective in enhancing malaria prevention and control practices3,4. It has also been reported as one strategy for promotion of community awareness and confidence in malaria control5.
However, there is limited evidence of community participation in malaria control in Myanmar. Therefore, this study aimed to examine the effectiveness of active community participation in malaria control by developing and using a suitable active community participation program (ACPP), which applies the participatory learning approach.
Study design and area
A community-based study which employed a mixed method approach, collecting data quantitatively and qualitatively on process and outcome indicators of the developed ACPP program, was conducted between May and October 2014 in Thabeikkyin township, in the Mandalay region. The Mandalay region, in the central part of Myanmar, had a population of 6.3 million and a malaria morbidity rate of 2.2/1000 population in 2013. Out of 31 townships in the Mandalay region, Thabeikkyin township, which had the highest malaria prevalence in 2013 (morbidity rate of 26.86/1000 population), was selected as the study township. Thabeikkyin township accounted for 25% of total malaria cases in the Mandalay region in 20136. Two study villages were purposively selected based on the malaria morbidity and similarity in malaria occurrence and socioeconomic conditions. Out of 92 villages of this township, the two villages that had the highest malaria burden and similar (but not identical) malaria morbidity in 2013-2014 were selected as study villages. Ohn-Paing village (population 844 and malaria morbidity rate 66.3/1000 population) was selected as the ACPP village and Kyauk-Kyi village (population 520 and malaria morbidity rate 75/1000 population) as the non-ACPP village7. These two villages were 9 km apart, separated by a forest, and had similar socioeconomic conditions.
Study population
The study population was selected based on household population, and almost all households within each village were systematically included in the study. This study included 142 of a total of 150 households from the ACPP village and 96 of a total of 100 households from the non-ACPP village. One representative from each household (ACPP: n=142; non-ACPP: n=96) participated in baseline and endline surveys. Fifteen community volunteers (one for every 10 households) from the ACPP village were recruited and trained for the development of ACPP.
A total of 20 villagers, 10 from each village, with the emphasis on, but not limited to, vulnerable persons such as pregnant mothers and those engaged in risky behaviors such as gold panning and wood or bamboo cutting, were intentionally selected to participate in in-depth interviews. The mentioned occupations of the villagers in this area put them at risk due to their residency and work activities in the indigenous malaria endemic zone.
Study procedures
Development of the ACPP: The ACPP was developed by applying six steps of the community action cycle (Fig1), which has a bottom-up approach and focuses on locally defined priorities and local perspectives. Participatory learning and action (PLA) methods were used in the ACPP village as community mobilization tools to promote participation in malaria control and community malaria knowledge. Participatory action was maintained in all steps of the ACPP.
Community meetings were held in both villages where the study was introduced. Community health needs were explored and social group differences were perceived. Three social groups namely, upper, middle and lower, identified by the villagers were seen at both villages. The villagers usually identified their social groups based on their types of business and owned properties as follows: villagers who engaged in various kinds of earnings such as doing business, opening grocery shops at the village, own a motorcar, own farms (10-15 acres) and dig gold with machines were defined as the upper social group; villagers who earned their living by farming (own less than 10 acres) and dug gold manually using weaves were defined as the middle social group; and the daily wage workers and manual laborers who earned their living taking part in the jobs of upper and middle social groups were defined as the lower social group.
A second community meeting was held in the ACPP village on the following day. At this meeting, the ACPP steps that would be implemented in the village were explained, and a village malaria committee (VMC), including representatives of all three social groups, was formed with community consensus. The roles and responsibilities of the committee members were assigned by the consensus of villagers and facilitated by the researcher. The VMC was regarded as the ACPP steering committee and was integrated into the existing village health committee. The job description of a community volunteer involved in ACPP implementation was explained to the villagers and their agreement on the selection criteria for community volunteers was obtained. The villagers were then requested to select representative community volunteers from their village at the subsequent community meeting. At the third community meeting, community volunteers were recruited based on the consensus of the VMC members and also in line with the selection criteria, which were as follows: (1) aged 18 years or more, (2) ability to read and write, (3) residing in the ACPP village for at least 1 year and does not have any plan to move to another village during the study period and (4) willing to participate in the implementation of the ACPP. Here again, it was ensured that the community volunteers came from all three social groups. However, because of economic reasons, the majority were from the middle social group (8 of 15 volunteers). The volunteers were tested to assess their background knowledge and perception of malaria with the help of the same structured questionnaire used in the baseline survey.
The community volunteers at the ACPP village were provided training for a period of 3 days on three key activities that would need to be implemented. The training emphasized small group education sessions (SGES) involving group discussions, brainstorming, role-play (to demonstrate the impact of malaria in the village) and two-way discussions with the facilitator. A volunteer training module and field manual were developed based on the WHO publication A manual for community health workers8 and We control malaria9. Post-testing was performed immediately after the completion of training to evaluate the process. Thereafter, the community volunteers began to act as community development facilitators (change agents), thereby initiating and facilitating the community participation process.
An action plan, which focused on the implementation of the three key activities, was developed by the community volunteers together with the VMC. The resources required (such as money, materials and human resourced) were discussed and identified. The three key activities implemented were as follows.
Activity 1 The following six key malaria messages were shared and discussed with the villagers.
- Our malaria problem: Discussion of the impact, signs and symptoms of malaria.
- How do we get malaria? Discussion on the way malaria is contracted and the transmission pathway in humans.
- How do we prevent malaria? Discussion of various preventive measures for malaria and how these measures can block the transmission pathway.
- What prevention measures can we adopt? Discussion on the preventive measures that villagers can adopt on their own (without outside support) and how to adopt these measures and encourage villagers to practice them.
- Mosquito breeding sites in our community: Discussion about potential breeding sites in and around the village and identification of vulnerable individuals using social mapping.
- Choice of malaria treatment: Discussion on how to properly select a malaria treatment, seek rapid diagnostic testing and effective treatment and the importance of completing the treatment course.
The SGES included the presentation and discussion of drawings specifically designed to transmit key messages about malaria and other information in rural communities. Information, education and communication materials, such as large posters (vinyl), pamphlets and posters from the NMCP, were also used. SGESs were held monthly to share key information about malaria, and the number of villagers and households participating in them were recorded in a logbook by community volunteers.
Activity 2 This involved reduction of potential mosquito breeding sites in and around the village and encouraging villagers to control these sites as one of the preventive measures that could be completed without any support from the health department. This activity was conducted in the same SGES.
Activity 3 Patients with fever were encouraged to seek prompt testing and treatment for malaria at the health center. Each community volunteer monitored family members from 10 households and helped any individual presenting with malaria symptoms to get tested and treated at the health center. They also encouraged the individual to complete the entire treatment course, and all of these activities were recorded in the logbook.
Management and evaluation of ACPP: Throughout its implementation, the ACPP was facilitated by community volunteers and monitored by the VMC. The first session of each volunteer and certain subsequent sessions were monitored by the researcher. Discussions were held among VMC members, community volunteers and the researcher at monthly monitoring meetings and, when possible, the ACPP was improved by adopting an alternative solution.
All training materials were supplied to community volunteers, and US$20 per person was paid for attendance. All materials and documents, including materials for drawing and logbooks required for participatory activities completed by the villagers, were freely supplied to the volunteers. They also received a stipend of US$10 per person per month as compensation at monthly monitoring meeting, whereas the VMC members received US$1 per person per month for attendance at the monthly evaluation meetings. A shirt, bag and hat specifically designed for the ACPP were provided to all volunteers and VMC members to enhance their motivation.
Insecticide tablets were freely supplied to the VMC and community volunteers, and these were used for impregnation of mosquito bed nets. Additional necessary support such as technical assistance for mosquito net treatment was provided by the township malaria team.
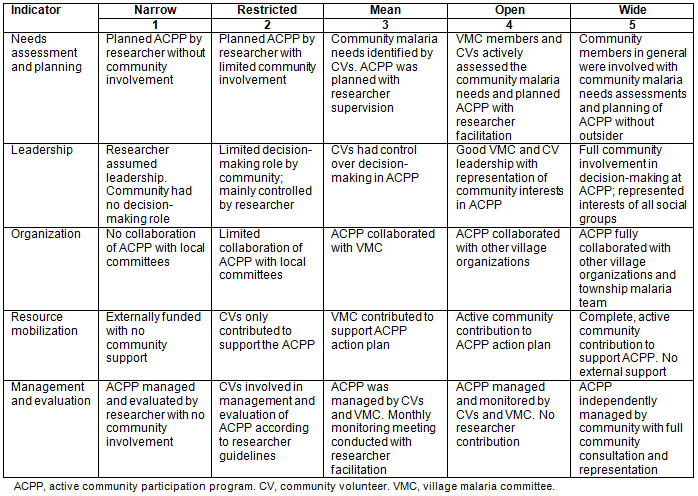
The ACPP was evaluated using process and outcome indicators. For evaluation of the process, spider gram analysis was performed using five process indicators, which measured, visualized and identified levels of community participation in the ACPP. These indicators and the scoring system have been described in Table 1, where each cell provides a definition of the indicator values at various points. Outcome evaluation involved reviewing records on community volunteer activities and community participation in malaria control activities. Moreover, the level of community malaria control knowledge and practice were identified as outcomes of the ACPP.
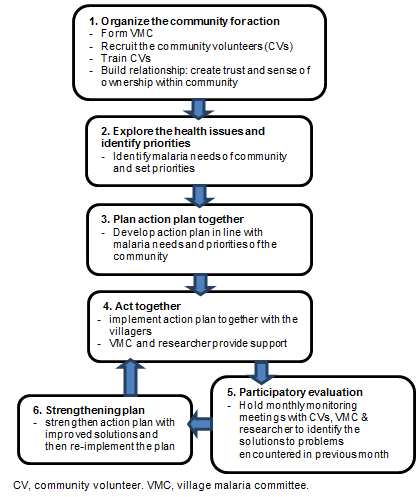
Figure 1: Six steps of the active community participation program.
Table 1: Process indicators and scoring of the active community participation program
Data collection and analysis
During implementation of the ACPP, the community volunteers recorded their daily activities of the ACPP in logbooks. Recorded were number of participatory activities to promote malaria knowledge and practice, number of activities directed towards individual household reduction of mosquito breeding grounds, number of fever patients encouraged to undergo early diagnosis and number of malaria patients encouraged to receive early diagnosis and supported of those patients in completing the entire course of malaria treatment.
This study used a pre-tested structured questionnaire to determine quantitatively the level of community malaria control knowledge and practice. The questionnaire explored five areas: general characteristics (seven questions), malaria knowledge (six questions), perception of malaria (eight statements), malaria preventive behaviors (three questions) and treatment-seeking behaviors (six questions). The questionnaire also contained one question to determine the active participation status of household representatives in malaria control. The questionnaire was developed after extensive literature review and the first draft was assessed by an academic expert for content and construct validity. The same structured questionnaire was used for quantitative data collection in two waves of survey of both villages.
Responses were determined by scoring based on WHO's manual for a community health worker8 to calculate the respondents' malaria control knowledge, perceptions, preventive behaviors and treatment-seeking behaviors. Emphasis was put on 'must know' and 'must do' items and thus the number of questions covered for calculating knowledge, perception and behaviour scores were considered sufficient.
It should be noted that two cross-sectional surveys were conducted at each study site at the same time period. With such multiple cross-sectional surveys, the data might be collected from different persons in the two waves at each study location, and there could also be variations in sample sizes at different surveying times. Considering the limitations and potential biases in the study design, the analyses were purposively performed as changes in program indicators within each group employing either independent t-test or χ2 test, rather than paired t-test or McNemar χ2 test. No sampling weight was applied in the analysis because information was collected from almost all household representatives in each village.
In addition, the focus of the study was on how the ACPP influenced changes within implemented village while the changes in another village with normal practice would serve as a negative control; thus the changes in both villages were performed separately. The comparisons of the changes between groups were not possible as the information gathered in two waves in each group came from different persons. The primary purposes of the analyses were thus not planned for comparing between the two villages but rather to descriptively explore any changes happening in the two locations with different malaria prevention and control approaches.
The pre-tested in-depth interview guide was used for qualitative data collection and the guide focused on five themes: knowledge of malaria prevention, perception of malaria prevention, malaria preventive behaviors, treatment-seeking behaviors and community-based malaria prevention and control activities. The required questions were asked for each theme and went in-depth to determine the respondents' knowledge, perception, opinion, feeling, barriers, peer pressure, family experiences and influences on malaria prevention and control. The collected data were transcribed and thematically analyzed.
Ethics approval
Participation of respondents in this study was voluntary and written informed consent was obtained from all respondents. Respondents had the full right to deny participation in this study and to ask any question about the study in any time. They had the right to withdraw from this study at any phase of the study. Confidentiality of respondents' answers to the questionnaire was strictly maintained. This study was approved by the Ethics Committee of the Faculty of Tropical Medicine, Mahidol University (reference no. MUTM 2014-036-01) and the Department of Medical Research (Upper Myanmar) (reference no. 1/Ethics/DMRUM/2014). The study was also approved by the Myanmar National Malaria Control Program (reference no. 10 Ngapha (Ngga) 2014).
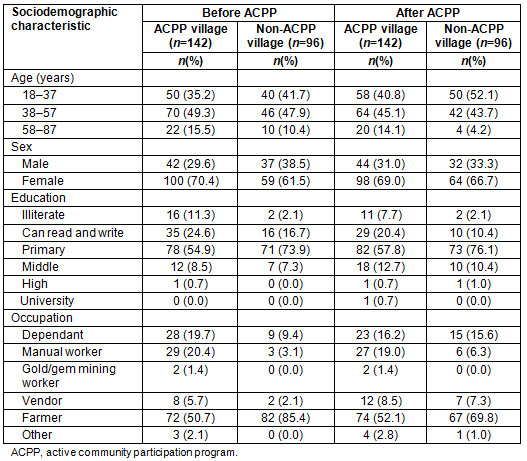
Through the community meetings, three perceived social groups were identified in both villages, namely upper, middle and lower. The middle group was the largest (about 60% of the population) in both villages, whereas the upper group had the fewest people (about 10-15%). People from the lower social groups of both villages constituted about 25-30% of population. Although they had other community health needs as well, both villages identified malaria as a priority health need because it hampered their economic lives to a great extent. The sociodemographic characteristics of household representatives of both villages participating in two waves of the survey are described in Table 2.
A VMC, which is a community-based organization, was successfully organized in the ACPP village and it supervised and provided necessary support to the community volunteers with regard to ACPP implementation. It also organized village malaria control activities and provided support to villagers who had contracted malaria. The VMC included village leaders, a middle school principal, a midwife from the health center, representatives from the three social groups of the village and an assistant from the township malaria control team. The middle school principal was the committee chair, and the midwife was the secretary. With the consensus of the villagers, 15 community volunteers from different social groups including both sexes and various ages (young, middle and older) were successfully recruited.
The 3-day training provided to community volunteers was an input to the ACPP, and these volunteers gained strength and competency in executing the PLA with the villagers. Moreover, their willingness to participate in ACPP was enhanced. The study helped in capacity development of the community volunteers, and the cost of training the community volunteers was US$1000.
Table 2: Sociodemographic characteristics of household representatives in two waves of the survey
Process evaluation
Three indicators (needs assessment and planning, leadership and resource mobilization) were given a score of 4, the organization indicator had a score of 5 and the management and evaluation indicator had a score of 3. The spider gram is shown in Figure 2.
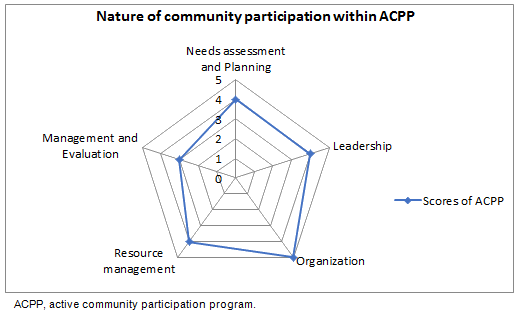
Figure 2: A spider gram of the active community participation program.
Outcome evaluation
The volunteers engaged in SGES with the villagers 103 times to promote malaria-related knowledge and practice, while activities directed towards individual household reduction of mosquito breeding grounds were conducted 78 times. The VMC and community volunteers organized an activity where the entire village strove to reduce mosquito breeding sites in and around the village. With support from the VMC, community volunteers impregnated all existing mosquito bed nets with insecticide. Volunteers encouraged 82.4% (98/119) of fever patients to undergo early diagnosis and 80.6% (25/31) of malaria patients to receive early treatment and supported 96.8% (30/31) of those patients in completing the entire course of malaria treatment. In the ACPP village, community participation in malaria control activities by household representatives increased significantly from 6.9% to 49.3% (p<0.001) (Table 3).
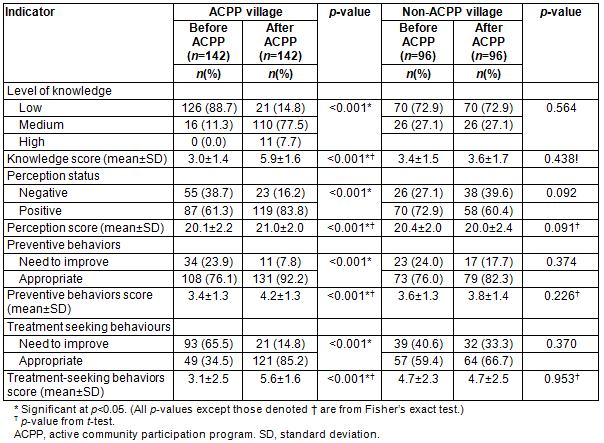
After participating in the ACPP, changes in community malaria knowledge, perception, preventive behaviors and treatment-seeking behaviors were observed (Table 4). Before the ACPP, only 11.3% of household representatives had a medium level of knowledge but this increased to 77.5% with a medium level of knowledge and 7.7% with a high level of knowledge after the ACPP (p<0.001). The mean knowledge score increased from 3.0 to 5.9 (p<0.001). The positive perception significantly increased from 61.3% to 83.8% after the ACPP (p<0.001), and the mean perception score significantly increased from 20.1 to 21.0 (p<0.001).
After the ACPP, the community became more skilled in malaria control. Only 76.1% had appropriate preventive behaviors before the intervention, and this significantly increased to 92.2% after the ACPP (p<0.001). The mean preventive behaviour score increased from 3.4 to 4.2 after the ACPP (p<0.001). Appropriate treatment-seeking behavior increased from 34.5% to 85.2% (p<0.001) and the mean treatment-seeking behavior score significantly increased from 3.1 to 5.6 (p<0.001).
Table 3: Participation status of household representatives in malaria control activities before and after the active community participation program
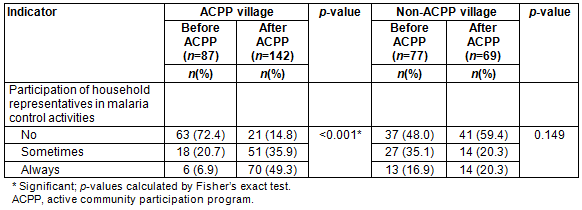
Table 4: Community malaria control knowledge, perception, preventive behaviors and treatment-seeking behaviors of villages before and after the active community participation program
Program sustainability
The VMC was integrated into the village health committee and effectively collaborated with other village organizations and the township malaria team. Furthermore, under the supervision of VMC, a community micro-financing scheme for health was developed to support malaria patients with urgent need for referral. The qualitative survey showed that the villagers exhibited the willingness to engage in the ACPP. One villager who was male, 37 years old, completed his middle level of schooling and was a farmer from the middle social group expressed his willingness as follows.
I am willing to be a volunteer in the village malaria prevention services if I am selected. It is very good for the village. I request to give training to our youth for malaria prevention and control.
Discussion
This study employed mixed methods and assessing the process and outcomes of the ACPP. Several lessons learned from the process of the ACPP development included key features of ACPP that were different from other community-based malaria programs in Myanmar, which are generally directed by health professionals without a basis in local perspectives and rarely involving the local people at the beginning of the planning phase of the program. The results of this study indicating several significant changes in the ACPP village while not much change in the non-ACPP village suggest the importance of having active community involvement at the planning phase as well as managing their own activities in malaria prevention and control for their village. For the ACPP, the inclusion of village representatives from three social groups including powerless people from the lower social group, their willingness and community consensus were keys factors that aided in organizing the VMC and recruiting community volunteers. Community approval and the willingness of the villagers to be volunteers motivated them to remain until the completion of the study. Additional motivational factors included incentives in terms of money, materials and technical support. Similar factors enabling the retention of community health workers in community-based health programs have been reported in other studies10-12.
The participatory learning approach was followed in the training sessions, and the contents for volunteer training were easy to understand, practical, comprehensive and focused on malaria prevention rather than cure. Discussion, active learning and sharing of learning experiences were performed at monthly monitoring meetings. These activities strengthened the performance of the community volunteers, leading to capacity development and motivation to serve as volunteers throughout the study. Comprehensive training with frequent supervision and continuous education improved the performance of the community health workers and increased their motivation to serve the local community13,14.
ACPP was developed and implemented by following the steps of the community action cycle integrated with PLA approaches. This allowed the program to build the community's capacity and skills in assessing the malaria problems faced by the community. These concepts and steps of the community action cycle have been previously used for mobilizing and empowering a community in Kenya for post-abortion care15 and for building a community's capacity to address tobacco-related health disparities16.
In this study, five process indicators were used to measure, illustrate and identify levels of community participation within the ACPP. The utility of these indicators in determining the status of community participation in community-based health programs has been demonstrated in other studies17-21. After the ACPP, approximately 85% of the residents in the ACPP village participated in malaria control, suggesting that the intervention was effective in mobilizing community participation.
Regarding the outcome indicators, this study focused on knowledge, perceptions and behaviors of villagers in malaria prevention and control. It was found that overall knowledge, perceptions, preventive behaviors and treatment-seeking behaviors of household representatives were significantly improved after the ACPP because the villagers gained malaria control knowledge and practice by participating in the ACPP. As reported in other settings, a community-based intervention utilizing participatory tools was effective in improving community knowledge and perceptions regarding malaria control22, and a health education intervention was suitable for improving community knowledge in home-based management of malaria23. Moreover, community participation was effective in improving a woman's ability to provide malaria control and also improved the malaria preventive behaviors of family health leaders and family members3,4. High community participation in an intermittent preventive treatment of childhood malaria prevention program has previously led to a decreasing trend in hospital admission due to malaria in Ghana24. Therefore, community participation is important for the success of malaria control, and effective malaria elimination programs require substantial interaction between the community and its leaders, malaria workers and health workers to ensure successful early diagnosis and prompt treatment25,26.
The results for the outcome indicators suggested potential benefit for the ACPP village such that the villagers, or at least household representatives, had gained knowledge and better perception about malaria prevention and control at village level. With such improvement in proper practices and perceived benefit, they realized that they could actually and actively take part in malaria prevention and control corresponding to their own community's needs.
For the program sustainability, the cost for the ACPP was minimal and the program had been set up by having the willing villagers contribute small amounts of money in a community micro-financing scheme, and not relying on government support, to run the community volunteer operation under the supervision of the VMC.
Study limitations
The main limitation of this study was its short duration (only 6 months for ACPP implementation), and this allowed us to assess the outcomes over a short period only. Besides this limitation, the study did not have an equal sample size in both arms because the study villages were purposively selected based on the key criteria of similarity in malaria morbidity, socioeconomic and geographical conditions. Also, the study results were based on partially different people in the two waves of survey.
The ACPP was satisfactorily developed by following the steps of the community action cycle integrated with PLA approaches. Moreover, the use of community volunteers under VMC supervision was effective in boosting community participation in malaria control and improving the community's malaria control knowledge and practice. The ACPP developed in this study is the adapted version of a standard community-based program and the method proposed in this study provides evidence of its potential benefit in designing a health promotion program. Particularly, the study's results suggested that the involvement of the villagers at the beginning of the planning phase and basing on their need and locally oriented issues could be the effective approach for a future malaria prevention and control program in Myanmar in moving towards malaria elimination in 2030.
Several features used in the ACPP model in this study may be adopted as useful strategies for the current NMCP's programs implemented in similar settings, and this recommendation has been made in time for the new democratic government in Myanmar. Community engagement is one of the nine strategic directions identified for universal health coverage in Myanmar, and the ACPP model is a cycle that emphasizes it27. Although the model described in this study required a longer period of evaluation to fully ascertain the impact of community participation, it is innovative because it has not been tried in Myanmar before.
Acknowledgements
This research was funded by DAAD Germany for the research team at the Faculty of Tropical Medicine, Mahidol University. We thank the program manager, Myanmar National Malaria Control Programme, for his kind permission to conduct this study. We also thank the township medical officer, local malaria control team, local village leaders, our community volunteers and community members who participated in this study.
References
1. Ministry of Health. Health in Myanmar. Nay Pyi Taw: Ministry of Health, 2014.
2. Rifkin SB. Lessons from community participation in health programmes. Health Policy and Planning 1986; 1(3): 240-249.
3. Geounuppakul M, Butraporn P, Kunstadter P, Leemingsawat S, Pacheun O. An empowerment program to enhance women's ability to prevent and control malaria in the community, Chiang Mai province, Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2007; 38(3): 547-559.
4. Duanchai J. The empowerment program on malaria prevention among family health leaders in Aranyapathet district of Sakaeo province (MSc Thesis). Salaya, Thailand: Mahidol University, 2002.
5. Bamidele JO, Ntaji MI, Oladele EA, Bamimore OK. Community participation in malaria control in Olorunda local government area, Osun state, southwestern Nigeria. African Journal of Infectious Disease 2012; 6(2): 24-28.
6. National Malaria Control Programme. Malaria annual report. Myanmar: National Malaria Control Programme, 2013.
7. Township Health Department. Malaria morbidity and mortality of Tha-beik-kyin, Myanmar: Township Health Department, 2013.
8. World Health Organization. A manual for community health workers. (Internet) 1996. Available: http://apps.who.int/iris/bitstream/10665/41875/1/9241544910_eng.pdf (Accessed 24 January 2014).
9. Simpson-Hebert M. We control malaria: participatory learning and action planning for Ethiopia. (Internet) 2008. Available: http://www.crsprogramquality.org/storage/pubs/.../ We_Control_ Malaria.pdf (Accessed 12 March 2014).
10. Alam K, Oliveras E. Retention of female volunteer community health workers in Dhaka urban slums: a prospective cohort study. Human Resources for Health 2014; 12: 29.
11. Alam K, Tasneem S, Oliveras E. Retention of female volunteer community health workers in Dhaka urban slums: a case-control study. Health Policy and Planning 2012; 27(6): 477-486.
12. Abbey M, Bartholomew LK, Nonvignon J, Chinbuah MA, Pappoe M, Gyapong M, et al. Factors related to retention of community health workers in a trial on community-based management of fever in children under 5 years in the Dangme West District of Ghana. International Health 2014; 6(2): 99-105.
13. Javanparast S, Baum F, Labonte R, Sanders D, Rajabi Z, Heidari G. The experience of community health workers training in Iran: a qualitative study. BMC Health Services Research 2012; 12: 291.
14. Kok MC, Dieleman M, Taegtmeyer M, Broerse JE, Kane SS, Ormel H, et al. Which intervention design factors influence performance of community health workers in low- and middle-income countries? A systematic review. Health Policy and Planning 2014: 1-21.
15. Community Mobilization for Postabortion Care (COMMPAC). A guide to action for community mobilization and empowerment focused on postabortion complications: Facilitator's manual. (Internet) 2010. Available: http://www.respond-project.org/pages/files/6_pubs/curricula-manuals/COMMPAC-Facilitator-Manual-May2010.pdf (Accessed 28 January 2014).
16. Hennessey-Lavery S, Smith ML, Esparza AA, Hrushow A, Moore M, Reed DF. The community action model: a community-driven model designed to address disparities in health. American Journal of Public Health 2005; 95(4): 611-616.
17. Bichmann W, Rifkin SB, Shrestha M (Eds). Towards the measurement of community participation. World Health Forum 1989; 10: 467-472.
18. Rifkin SB, Kangere M. What is participation? In Hartley S. (Ed.). CBR: a participatory strategy in Africa. London: University College London, 2002; 37-49.
19. Rifkin SB, Muller F, Bichmann W. Primary health care: on measuring participation. Social Science & Medicine 1988; 26(9): 931-940.
20. Baatiema L, Skovdal M, Rifkin S, Campbell C. Assessing participation in a community-based health planning and services programme in Ghana. BMC Health Services Research 2013; 13: 233.
21. Draper AK, Hewitt G, Rifkin S. Chasing the dragon: developing indicators for the assessment of community participation in health programmes. Social Science & Medicine 2010; 71(6): 1102-1109.
22. Opiyo P, Mukabana WR, Kiche I, Mathenge E, Killeen GF, Fillinger U. An exploratory study of community factors relevant for participatory malaria control on Rusinga Island, Western Kenya. Malaria Journal 2007; 6(1): 48.
23. Fatungase KO, Amoran OE, Alausa KO. The effect of health education intervention on the home management of malaria among the caregivers of children aged under 5 years in Ogun State, Nigeria. European Journal of Medical Research 2012; 17: 11.
24. Kpormegbe SK, Ahorlu CK. The role of community participation in intermittent preventive treatment of childhood malaria in southeastern Ghana. Ghana Medical Journal 2014; 48(2): 58-65.
25. Atkinson J-AM, Fitzgerald L, Toaliu H, Taleo G, Tynan A, Whittaker M, et al. Community participation for malaria elimination in Tafea province, Vanuatu: Part I. Maintaining motivation for prevention practices in the context of disappearing disease. Malaria Journal 2010; 9: 93.
26. Tynan A, Atkinson JA, Toaliu H, Taleo G, Fitzgerald L, Whittaker M, et al. Community participation for malaria elimination in Tafea Province, Vanuatu: Part II. Social and cultural aspects of treatment-seeking behaviour. Malaria Journal 2011; 10: 204.
27. Ministry of Health. Nine strategic directions for universal health coverage in Myanmar. Nay Pyi Taw: Ministry of Health, 2015.






