Introduction
South Africa has undergone a major transformation of its health services over the last decade, moving from a highly fragmented inequitable system, to one based on the district health system, with a cornerstone of equity1,2. The district hospital can be described as the backbone of health care in the district health system. The effective management of local health facilities such as district hospitals is essential for the implementation of health policy.
The district health system is now the vehicle for the provision of public healthcare services in South Africa3, with clear referral pathways from primary care clinics to health centres and on to district hospitals within that. The National Department of Health sets the policy framework while Provincial Departments of Health are responsible for implementation of policies, largely through district health care services. District hospitals report to health district management structures, while still being accountable to provincial head offices in terms of issues such as budgets and service delivery. While district boundaries and sizes have undergone many changes during this process, with resulting uncertainty and confusion, the system has generally been implemented more quickly and fully in rural areas.
At the same time, leadership of the management team in district hospitals has moved away from medical superintendents to general managers or chief executive officers, who may or may not have a background in health care. A shortage of professional staff continues to be a problem, especially in terms of doctors and nurses who continue to leave at alarming rates, and the impact of HIV/AIDS on patient numbers and on staff morale and capacity is significant. Norms and standards for the provision and delivery of healthcare services by district hospitals have been developed4, which place greater responsibilities on these hospitals, and managers are under constant pressure to show that they can meet these demands.
Despite major achievements, the transformation has not been achieved smoothly; there has been and still is some disorder and disorganisation. There has been a lack of management capacity to implement the health policies and programmes required for an effective district health system5. It is thus easy to find examples of district hospitals not functioning well. It is not clear, however, what the ingredients are in the management of a well-functioning district hospital. Subjectively, however, there is a sense of what this means and some agreement that certain health services and hospitals are functioning better than others.
Our understanding is that every system is designed to achieve exactly the results that it does achieve6. We thus decided to study well-functioning district hospitals in two rural districts from a qualitative perspective, listening to those involved in their management, in order to understand the key factors in their success - why they were managing to achieve when others were failing.
Research on the management of (district) hospitals has largely focussed on technical, economic and infrastructural issues7-11; where process issues are discussed, these tend to be at a macro level, looking at how policy is implemented in the health sector, rather than the process at a hospital, or district level12.
We deliberately focused on the process of management, from the perspective of the managers themselves. For this reason, there was no attempt to measure success, but only to understand factors contributing to it. We made the assumption that similar sets of organisational, financial and transformational issues face rural hospitals in South Africa, and sought to understand how managers found a way to move forward effectively within the constraints they face. This is particularly important because factors that influence the motivation of health providers and managers are essential in effective healthcare reform13.
The aim of this project was to explore and document what assists a rural district hospital to function well, in order to produce material to assist and guide managers of district hospitals. This article is based on the resulting booklet14, which was intended for use in training of district hospital managers.
Methods
A cross-sectional exploratory study was carried out using in depth interviews with managers of five well-functioning district hospitals in South Africa.
Hospitals in two rural districts in South Africa, in North West and KwaZuluNatal Provinces, were sampled. Hospitals in these districts were described as functioning well by key informants involved in rural health care and health service development. In these districts we selected members of the broad hospital management teams, the district managers and two former medical superintendents who were available for interview during pre-arranged visits between July and October 2000.
Data collection was through free attitude in-depth interviews conducted in English by IC. Each interviewee was asked a single question, 'What are the things that you think make this hospital function relatively well?' The approach was to leave the question open to the respondents and to build all the information from what was presented by them. The discussion was facilitated through reflection and clarification techniques. The interviews lasted between 20 min and 2 hours. A total of 21 people were interviewed, with a spread of professional backgrounds (Table 1).
Table 1: Characteristics of respondents
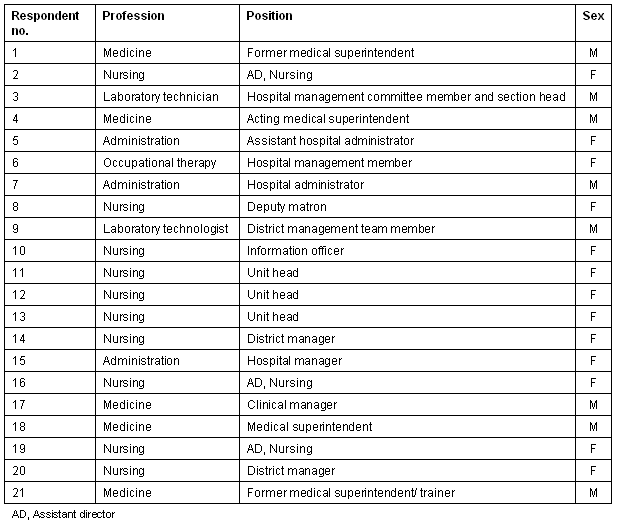
Each interview was recorded on audio and/or videotape and field notes were made at the time. All interviews were transcribed and analysed separately. Content analysis was performed individually by the researchers through theme identification and categorisation, using cut and paste methods. The analysis of each interview was then compared and combined. Differences were resolved by joint reflection on the original transcriptions. On the basis of these analyses a composite framework was developed. Finally the results from all the interviews were integrated into this framework. There was a remarkable degree of agreement among the interviewees.
A draft of the report was sent to all the respondents in order to validate the findings, and feedback was incorporated into the results.
The relevant district and hospital managers gave permission for us to conduct the research and individual respondents provided informed consent.
Results
Thirteen major themes were identified (Table 2), which were clustered in three groups. The themes are conceptualised and described diagrammatically, using direct quotes from the interviews. The diagrams present more detail of each theme, with actual phrases of respondents being used in most cases. The text highlights salient features. The direct quotes describe the theme concepts eloquently and using these allows the results to stay close to the original data.
Table 2: List of themes and theme clusters
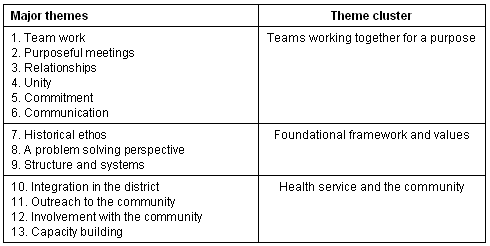
To protect confidentiality individual quotes are not identified, nor are they ascribed to professional cadres, because the team perspective was considered to be critical.
Teams Working Together for a Purpose
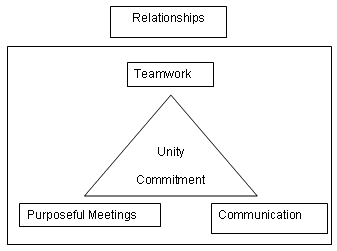
Figure 1: Teams working together for a purpose.
A first group of 6 themes can be summarised as TEAMS WORKING TOGETHER FOR A PURPOSE (Fig 1). Unity and commitment are the core which allow staff at all levels of the service to work together in teams, facilitated by regular meetings and enhanced by good communication. The solid cement of good relationships holds all this together.
Teamwork

Figure 2: Teamwork.
Almost every respondent mentioned the word 'team' (Fig 2). Perhaps the best definition of teamwork given was 'working together to maintain standards.' This was expressed in various similar ways, such as 'everybody is concerned and is involved in the decision making', and 'people are working together... in bringing positive outcomes'.
Teamwork is seen to occur at a number of levels. The management committee functions as a team, setting an example to the rest of the hospital. They work together with all staff members, seeing them not as subordinates but as fellow members of a team.
The team is multidisciplinary with different sections and units working together. 'There is a team spirit between the doctors, between the nurses, between the paramedics and all the hospital staff members.'
The community and community health services are part of the team.
Purposeful meetings
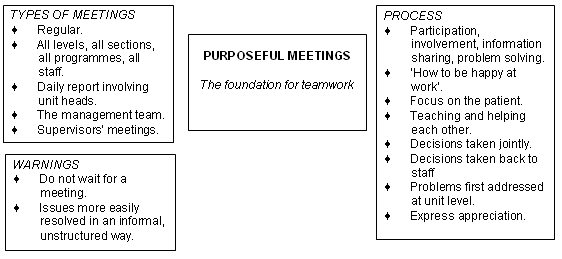
Figure 3: Purposeful meetings.
Many cynical words have been written about meetings and nearly every administrator's office has some quote on its walls about the lack of value in meetings. Yet it was very clear in all interviews that regular purposeful meetings are the foundation on which teamwork is built (Fig 3). Again and again regular meetings, at all levels, between all sections and all staff, are seen as a key ingredient in functioning well. 'No-one can run a hospital alone and different people from different sections are needed to make the hospital run better.'
Specific examples of useful types of meetings were cited at different hospitals. One example is a monthly supervisors' meetings, where supervisors of all sections, from medical to maintenance meet to share information, and to discuss problems that cannot be solved at unit level. 'Decisions are taken jointly.' Another is a meeting of all the staff who report to the clinical head under the title 'how to be happy at work', focussing on helping each other in the team to find new motivations in order to be happy at work.
In the context of these meetings, two warnings are sounded. Firstly, problems do not need to wait for a meeting to be dealt with. There is continuous decision-making. Secondly, issues are often more easily resolved in an informal, unstructured way rather than in meetings.
Relationships
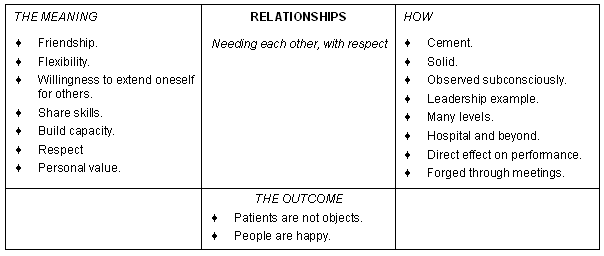
Figure 4: Relationships.
Relationships were continually emphasised as being vital to effective functioning and the basis of teamwork (Fig 4). The relationships are at many levels: 'peers, colleagues, ... medical personnel, ... the management team, ...the hospital community ... and the extended community around the hospital.' 'In a small hospital, one needs each other more and more ... so you rely on each other heavily, so relationships run deep.'
It is that relationship side of things that is the cement that holds the management together and the model for the rest of the hospital - the relationships between us were right and were solid and we liked each other.... I think perhaps that is observed subconsciously by the rest of the hospital.
Relationships also allow for openness to share skills in order to develop capacity. They are based on respect. 'We kind of know each other and respect each other.' An explanation given for this, at all sites, is the fact that hospital staff are part of the community they serve. This has two implications. Firstly the patients are not objects. Secondly, the staff have relationships and 'a strong sense of personal value' outside of their hospital roles and functions, that is, 'people are not labelled by their job. ... People socialise across professions and thus listen respectfully to the general assistant or cleaner's opinion on some issue.'
As a result of this 'people are happy', 'because when you have a nice team and a nice atmosphere you feel like doing always something better.'
Unity
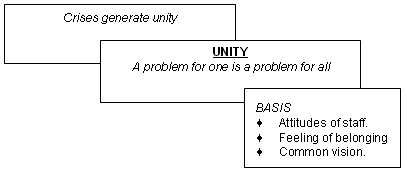
Figure 5: Unity.
Unity is another expression of relationships and of working together (Fig 5). It was specifically mentioned at each hospital site. 'If there's a problem, it's not a problem for one person, but is the problem for the whole management.' This goes beyond management to include all staff.
Crises are described as being important in generating unity. Being needed in a crisis generates a 'feeling of belonging'.
A key to this is a common vision. 'The first thing that makes the hospital function well is the people have a common vision ... to deliver health care in the whole district and not just an institutional hospital service... it helps people to feel united in their tasks and so from management down it helps.'
Commitment

Figure 6: Commitment.
Commitment, motivation and dedication of staff arise directly out of this unity and common vision (Fig 6). It was striking how often this was raised as being important in effective functioning.
There is an understanding from the team that you're working together for the good of the patient and improving patient care and because of that people are willing to be flexible and to get out of their roles and willing to work together in new ways.
The commitment must, above all, be evident at the top. There is 'the need for good leadership, .... You need people who are prepared to stand up and be accountable, take responsibility, manage times of crisis, also think strategically and plan ahead.'
This commitment arises from 'motivation to actually do the work, as opposed to earn a salary... they see the care of their patient as being something they're really proud of.' The basis for this is 'often a Christian commitment'.
Communication
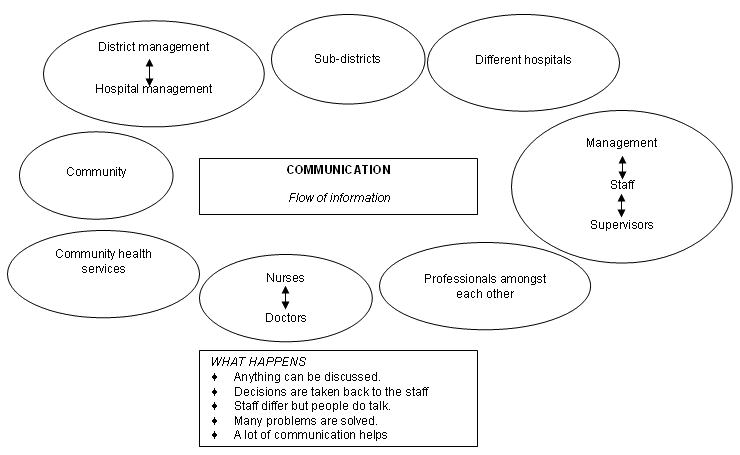
Figure 7: Communication.
The basis for teamwork, relationships and unity is communication (Fig 7). It was summarised as 'sharing of information generally ... between different people and professions, ... within the different programmes and services including community health services ... [and] between different hospitals.'
A clinical manager described working with doctors from eleven different countries. There is team work, he said, partly because 'we discuss about anything. We are here for the patients and we say we are here for the patient, but for us to be able to be for the patient we have to be able to be for each other.'
Foundational Framework and Values
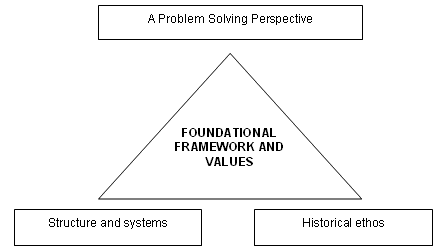
Figure 8: Foundational framework and values.
Another cluster of themes is best described under the heading of the FOUNDATIONAL FRAMEWORK AND VALUES of the team (Fig 8). The framework in which teams operate is an historical tradition which provides an ethos for staff and an approach to problem solving which is pro-active and determined, undergirded by a structure and systems which facilitate this.
Historical ethos
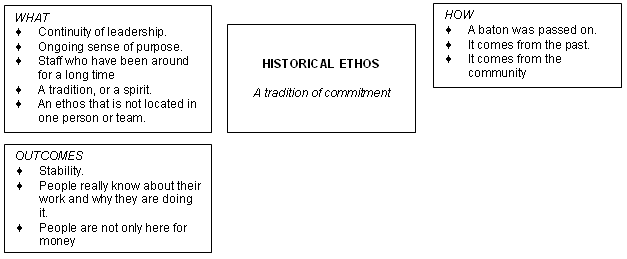
Figure 9: Historical ethos.
What is the origin of the commitment and motivation described? A concept we have labelled historical ethos comes through clearly in many different ways, described in terms such as continuity, tradition, heritage, and an ongoing sense of purpose (Fig 9).
There's often a tradition, or a spirit, that comes in my experience from the mission times, that has been carried through. There's the tradition of hard work, of dedication, of commitment, and excellence in the way that people do things, and of accountability, that might have been started by a few pioneers many years ago.
People really know about their work and why. ... They do remember that they are not only here for money, but also the main reason is to help the sick people.
One manager describes this ethos as not being located in one person or team but as a baton that is passed on through the years.
I would say that one of the important things is the history of the hospital - it has a history of being well managed and a history of excellence and a caring attitude, which stems from the mission ethos of the '70s. And the concept that in each change of, especially, management the baton was passed on to the next person and it was done prayerfully in the old days and in the new days with lots of thought so, in a way that the history was a process of building the hospital that was continued... If you're looking at it from the management perspective, certainly with superintendents you see the pictures on the wall, the galleries of those who have actually been there before you ... you realise that you are actually just another stepping stone... personally it gives you the incentive to do your best and to continue in the same line as your forefathers had done.
This ethos related to leadership is not limited to any rank or position. 'Good people get attracted to good leadership, and an ethos is built up over time. I'm not just talking about top leadership, ... I'm talking about all the managers ... the heads of each unit, ward, section.'
A problem solving perspective

Figure 10: A problem solving perspective.
Part of the culture in the various hospitals appears to be a particular perspective on and way of dealing with problems (Fig 10). Although difficult to define specifically, it was mentioned repeatedly, and can be described as the process of finding 'solutions within the team.' There appears to be an underlying understanding amongst respondents that problems can be solved, by the teams themselves, so that staff do have a sense of 'working to try and make things better in different ways.'
If we were to take resources as we have them, human and material, we would not make a move in any way. But on a daily basis we look to put that aside and perhaps see what do we do with what we have. ...There are problems. ....because we want to get the service accessible to most people we actually force our way to say we may do this here and there. ...It's actually something that keeps us going... we turn our problems to challenges ... We just keep going to say we want to achieve something.
One manager provided an interesting perspective on the issue of dealing with problems. He detailed many of the problems experienced in an isolated, rural hospital, for example 'landslides and floods and trees over the road, gangsters at night', 'electricity ... very unreliable and water', 'shortage of vehicles', 'telephone ... hardly reliable,' etc. In the right context and with the right people, these can provoke a determination to succeed, to overcome the problem:
...that's fine, let's just do it our own way, let's see if we can do it, just to prove to people it can be done without electricity, telephones, water, anything. We can work. It's almost a challenge against the managers in far off white cities or far off ivory towers of administration, of learning.
He goes on to make a point many health workers will identify with:
The isolation ... is almost a challenge ... you try to solve your problems alone as a challenge, I suppose. We didn't see eye to eye on many issues with the head office, especially related to community health issues, and it was nice to know that you are not observed. You could do what you felt in your heart to do and there weren't going to be many problems coming from it. So there was kind of a cheeky side: let's just do it regardless of what the administrators would say at head office.
This isolation is a very important issue in rural hospitals; these hospital managers were apparently able to let the isolation work for them, making them more determined, bolder and more innovative.
Structure and systems
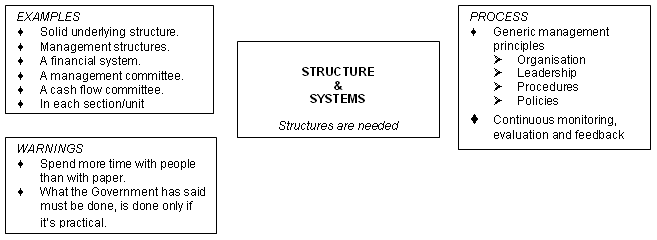
Figure 11: Structure and systems.
It became clear through the interviews that a solid underlying structure is needed, to allow for this kind of problem solving to happen. It is the framework on which everything else hangs. 'You need management structures' and to apply 'generic management principles.' However, this structure cannot just be a management structure. 'Each section, each unit of the hospital needs to have some degree of organisation, some leadership, some ways of doing things, procedures, policies.' Attention is thus given to establishing functional structures and systems within each unit of the hospital and to maintaining these structures and systems (Fig 11).
Systems require good administration. At the same time, however, the structures cannot be separated from people.
You can put all the other bits of paper together, but if you don't have the spirit of it, then you don't end up with the health care system. Whereas you can have a health care system without all this paper work, while people are in the right attitude. So it's better if you've got to choose where you're going to invest your time, it's certainly better if you have more time with the people than time with the paper.
An important function of the structures is to ensure that there is continuous monitoring, evaluation and feedback.
This infrastructure also serves as a monitoring body to make sure that things are developing and that needs are being met, by services, and by evaluating structures as well.
Head office documents are applied only when relevant and practical.
[The hospital] needs to sift information, take what is practical from their side... what the Government has said must be done is done only if it's practical and relevant to us down here at the hospital.
This provides a picture of an orderly, logical, structured process underlying decision making.
The Health Service and the Community
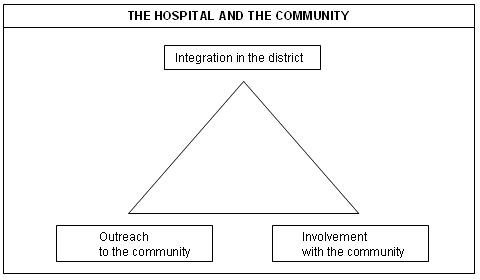
Figure 12: The health service and the community.
A last cluster of themes focus on the relationship between the hospital, different aspects of the health service and the community (Fig 12).
Integration in the district
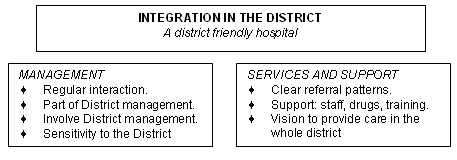
Figure 13: Integration in the district.
An important aspect of structure is the hospital's place within the district (Fig 13). All respondents felt that their hospitals were well integrated into the districts. The hospital management team was 'involved in planning, implementation, evaluation of the entire district.' What does this mean in practice?
I have a concept ... of a district friendly hospital, in other words, the facts that make a hospital friendly as it were, to the district that it serves, the population, that its placed within, so for example that there are clear referral patterns and the clinics are visited regularly and supported with staff or drugs or training or whatever.
The integration described above arises out of a broader understanding on the part of hospital management, a vision to provide 'health care in the whole district.' 'The focus for the district hospital is not concentrating on the boundaries of your vicinity, of your hospital, you go beyond the gate, you need to go beyond the gate.'
Outreach to the Community
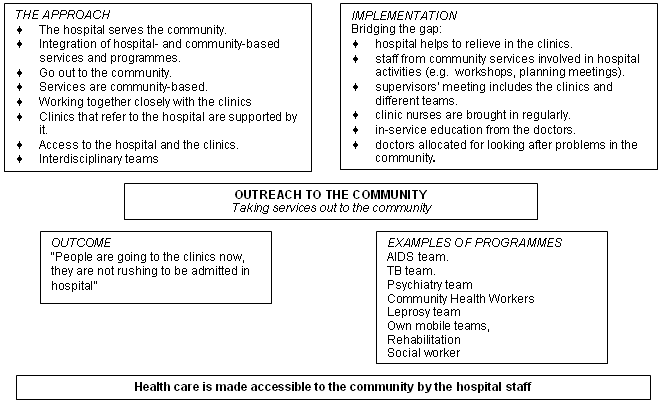
Figure 14: Outreach to the community.
The underlying principle here is clearly that 'the hospital serves the community. The hospital came into being because the community is there.' This understanding is manifested in integration of hospital and community programmes (Fig 14). The hospital has a commitment to 'the process of making sure that its health care is made accessible to the community by the hospital staff.'
Furthermore the staff from community services are involved in activities in the hospital such as workshops, planning meetings and in-service education. 'On the clinic side, ... support ... is given by regular visits to clinics and ... there are doctors who are specifically allocated for looking after problems in the community.'
Involvement with the community
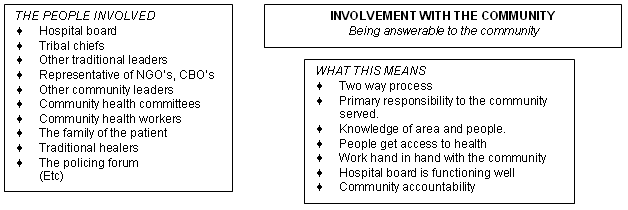
Figure 15: Involvement with the community.
Access to health care by the community can only happen if the hospital is working together with the community (Fig 15). This is a 'two way process of the community making their needs known' and the hospital knowing the community it serves.
There is a sense of being answerable to the community. The hospital feels 'a primary responsibility to the community it serves. What I see happening is a lot of hospitals giving their accountability to provincial head office, rather than to that local community.'
The structure that makes much of this happen is the hospital board, which includes traditional leaders, representatives of NGOs, CBOs (community bases organisations) and other community leaders. However, involvement of the community goes beyond the Board to many other levels in the hospital.
Now we are involving the family in the rehabilitation [of psychiatric patients] and the same with HIV patients and the same with TB. We are getting traditional healers involved. ... There is quite a number of them who work at TB care ... we work hand in hand with them.
Capacity building
The last of the major themes raised was staff development, i.e. the importance of training and building capacity (Fig 16).
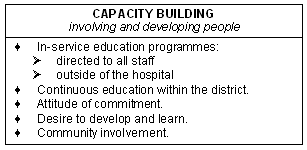
Figure 16: Capacity building.
This staff development is not just for certain types of staff, but for everyone working in the hospital, 'all members of staff, right from the lower categories ... the cleaners, the groundsmen, the professional nurses.'
Discussion
The interviews provided a wealth of wisdom and insight, not only concerning the ingredients for successful management of these hospitals, but also other components of their overall functioning. They provide a framework for what is possible in a rural hospital context. Any district hospital leadership would do well to consider these ideas. They provide a useful basis for training, as envisaged at the outset.
A number of core concepts from management literature were highlighted in the themes raised by these managers. Central to these concepts are leadership development, establishing a functional team and ensuring accountability to the community, representing users of the service.
Many of the issues identified by managers in this research are similar to the constituent parts of the 7S Model, of Waterman, Peters and Phillips15. According to this model, there are seven aspects of an organisation that are needed to harmonise with each other, viz. strategy, structure, system, staff, style, shared values, and skills. The resonance of these, which were tested extensively in surveys of successful American businesses, with the themes identified is clear and serves to validate the usefulness of the themes for managers.
It is obvious that communication was not simply a theme, but central to much of what was happening in these hospitals. It has been said that if the problems in communication can be solved, most of the problems in any organisation, if not the world, will be solved16. Communication is central to building communities17, which is essentially how these managers view their hospitals. Communication clearly underpins the problem solving processes described, as well as the sense of unity, what happens in meetings, and outreach to the wider community.
There is also the understanding that all supervisors must play a role as leaders18. In terms of the theory of learning organisations, leaders model the openness, risk taking and reflection necessary for learning; they also communicate a compelling vision of the organisation (institution) and provide the empathy, support and personal advocacy needed to lead others towards this vision15. In other words, they do not simply manage staff, but play a role in developing vision, motivating staff and achieving goals to which they themselves ascribe. This is based on the example of the management teams who themselves function critically as leaders, defined inter alia by their ability to identify future problems and set in place problem-solving mechanisms for these19, thus shaping the culture of their hospitals' functioning20.
It is apparent from the interviews that these managers have been able to achieve some of what colleagues in Tanzania felt were needed to improve the functioning of their health service, such as greater health manager control over resources; stronger employment, disciplinary and reward systems; and more responsibility for communities in relation to districts13.
The issue of the ethos of the hospital, difficult to define and even more difficult to develop, is perhaps fundamental in ensuring leadership at so many levels. Values are a critical factor in determining motivation, because those involved in management become excited about what they care about19. These values frequently arise out of the cultural context of the staff members, who are often steeped in the traditional African philosophy of ubuntu (compassion, caring, sharing, humaneness, empathy21). Common values arise out of a sense of community and cannot be thrust upon an organisation21; values depend on relationships22. Thus teamwork itself fosters shared values and purpose, just as it is dependent on them.
Many of these themes relate to so-called 'soft' issues such as relationships, unity, commitment, and communication - the process aspects of management rather than the structural and organisational ones - while emphasizing that the latter are also essential. A picture emerges of structures and systems developing around purposes and people23, in a classical 'form follows function' approach. Despite being the subject of much attention in management literature17,20-25, these aspects are difficult to legislate or systematise; however, they may be the critical factors which distinguish successful hospitals. There is certainly a need for further research around these, in the context of hospital management, especially to determine quantifiably which of these make the biggest impact. Nevertheless they already provide an important framework for training of managers.
It is thus important not only that district hospital managers themselves look at these issues - and it is clear from the results that a feature of those interviewed was their leadership in taking initiative and implementing processes without waiting for direction or blessing from higher authorities - but also that political authorities wishing to ensure implementation of healthcare reforms need to take seriously process issues in management and to find ways to train managers to be leaders who can implement the reforms in a motivated way, as conceptualised in the Health Workers for Change programme26. This is often threatening to authorities because of the independence that must be offered to these managers, but must surely reap rewards in terms of successful outcomes.
Conclusion
A question raised is how a manager begins the process of developing a successful hospital. There is a vast literature around this, as evidenced by a recent systematic review on the subject27. However, most hospital managers are seeking something down-to-earth that they can understand and apply easily within their contexts. Spontaneously, interviewees suggested ways to do this. One respondent explained,
You have to start by identifying core groups of people you can work with, and understand why they're struggling ... and to try to help them to see ways in which they can be a positive influence on daily basis.
Another said,
I want to emphasise the role of leadership and the role of the community above the others... I think in terms of what we can do to stimulate district hospitals, I would put my money into those areas, developing leadership and developing community accountability. Some kind of leadership development programme is absolutely crucial.
The Health Workers for Change process, which has been found to be applicable in a range of different settings and countries26, offers one method which can assist the development of a positive relationship between health workers and patients, create teamwork within a facility, and develop a supportive environment for facility staff to take more initiative28.
The key issue is obviously the development of a team in the hospital, a team with a unified vision of giving patients priority, respecting each other as well as patients, and working in and with the community to achieve optimal health care.
Acknowledgements
The project on which this article is based was funded by the Health Systems Trust of South Africa. The authors are grateful to all those who consented to being interviewed; keep up the good work!
References
1. African National Congress. A National Health Plan for South Africa. Johannesburg: African National Congress, 1994.
2. National Department of Health. White Paper on the Transformation of the Health Sector. Pretoria: National Department of Health, 1997.
3. National Health Act, 2004. (Act No. 61 of 2003) Cape Town: Government Gazette 2004; 469: 26595.
4. National Department of Health. A District Hospital Service Package for South Africa: A set of norms and standards. Pretoria: Department of Health, 2003.
5. McIntyre D, Gilson L. Putting equity in health back onto the social policy agenda: experience from South Africa. Social Science & Medicine 2002; 54: 1637-1656.
6. Berwick DM. A primer on leading the improvement of systems. BMJ 1996; 312: 619-622.
7. Blas E, Limbambala ME. The challenge of hospitals in health sector reform: the case of Zambia. Health Policy Plan 2001; 16(Suppl 2): 29-43.
8. Collins C, Green A. Public sector hospitals and organizational change: an agenda for policy analysis. International Journal of Health Services 1999; 24: 459-475.
9. Mills A, Hongoro C, Broomberg J. Improving the efficiency of district hospitals: is contracting an option? Tropical Medicine and Internal Health 1997; 2: 116-126.
10. McPake BI. Public autonomous hospitals in sub-Saharan Africa: trends and issues. Health Policy 1996; 35: 155-177.
11. Bukonda N, Tavrow P, Abdallah H, Hoffner K, Tembo J. Implementing a national hospital accreditation program: the Zambian experience. International Journal of Quality Health Care 2002; 14(Suppl 1): 7-16.
12. Oyaya CO, Rifkin SB. Health sector reforms in Kenya: an examination of district level planning. Health Policy 2003; 64: 113-127.
13. Gilson L. Management and Health Care Reform in Sub-Saharan Africa. Social Science Medicine 1995; 40(5): 695-710.
14. Couper I, Hugo J. Management of District Hospitals: Suggested Elements for Improvement. Durban: Health Systems Trust, 2002. (Online) 2005. Available from www.hst.org.za (Accessed 13 September 2005)
15. Iles V, Sutherland K. Managing change in the NHS: Organisational change. A review for health care managers, professionals and researchers. London: School of Hygiene & Tropical Medicine: National Coordinating Centre for NHS Service Delivery and Organisation, 2001; 65. Available from www.sdo.lshtm.ac.uk. Accessed on 20th March 2005
16. Schulz R, Johnson AC. Management of hospitals. 2nd edn. New York: McGraw-Hill, 1983.
17. Peck MS. The different drum. London: Arrow Books, 1987.
18. Sloane RM, Sloane BLW. A guide to health facilities: personnel and management. St Louis: CV Mosby, 1977.
19. Sheldon A. Organizational issues in health care management. New York: Spectrum, 1975.
20. Katzenbach JR, Smith DK. The wisdom of teams: creating the high-performance organization. New York: HarperBusiness, 1994.
21. Boon M. The African way: the power of interactive leadership. Sandton: Zebra Press, 1996.
22. Hanson DS. A place to shine: emerging from the shadows at work. Boston: Butterworth-Heinemann, 1996.
23. Senge P. The fifth discipline. New York: Doubleday, 1994.
24. Greenleaf RK. Servant leadership. New York: Paulist Press, 1977.
25. Jaworski J. Synchronicity: the inner path of leadership. San Francisco: Berrett-Koehler, 1998.
26. Fonn S, Mtonga AS, Nkoloma HC et al. Health providers' opinions on provider-client relations: results of a multi-country study to test Health Workers for Change. Health Policy Plan 2001; 16(Suppl. 1): 19-23
27. Greenhalgh T, Robert G, Bate P, Kyriakidou O, Macfarlane F, Peacock R. How to Spread Good Ideas: A systematic review of the literature on diffusion, dissemination and sustainability of innovations in health service delivery and organisation. Report for the National Coordinating Centre for NHS Service Delivery and Organisation (NCCSDO), April 2004. (Online) 2004. Available: www.sdo.lshtm.ac.uk (Accessed 20 March 2005).
28. Onyango-Ouma W, Laisser R, Mbilima M et al. An evaluation of health workers for change in seven settings: a useful management and health system development tool. Health Policy Plan 2001; 16(Suppl.1): 24-32.


