Shortage of the health workforce has remained an important concern for health systems in many countries1-3. An adequate supply of doctors is needed to ensure access to affordable and quality health care as well as favourable health outcomes4. Although making some progress, Thailand has still encountered critical shortage and maldistribution of doctors5.
In addition to strategies to increase the production of doctors for rural areas, efforts and measures to improve retention of medical doctors in most needed and underserved areas are necessary6. This may be done through various educational strategies, ranging from rural recruitment policy to early exposure to rural healthcare services6-9. Furthermore, factors that address living and working environment as well as opportunities for personal and professional development are among key successful postgraduation factors for enhanced doctor retention3,6, particularly in remote areas where doctors are less likely to continue working in the long run. Although these interrelated strategies have been implemented in a number of developing countries such as Ecuador, Indonesia and South Africa10-13, they are usually not comprehensive and often limited to addressing a single or limited number of underlying factors3. Further, few studies have systematically evaluated short- and long-term impacts of these strategies on rural retention in developing countries.
Since 1994, two government-funded initiatives, the Collaborative Project to Increase Production of Rural Doctors (CPIRD) and the One District One Doctor (ODOD) program, have been launched with a primary aim to increase the production of doctors for rural and remote areas14,15. These special recruitment initiatives are operated through collaboration between medical schools and hospitals in the Ministry of Public Health (MOPH)14. Different from Thailand's conventional medical training, the two projects use various strategies, including special recruitment of students with rural background and utilising existing health services outside major cities as medical schools and training facilities, and early rural service exposure, followed by regulated rural placement and mandatory service with non-adherence penalty obligation. However, little evidence exists to describe the retention of graduates under the CPIRD and ODOD projects in comparison with the conventional medical training. A recent study addressed the retention of medical students under the two training tracks who entered the MOPH between 2001 and 2007, which represent an early period of the special rural recruitment project and includes only 18% of total CPIRD and ODOD students16. The present study aimed to examine the retention in MOPH hospitals of medical doctors graduated from the special recruitment and normal tracks between 2001 and 2015, and identify factors associated with rural retention over the period.
Methods
This is a retrospective study using data on newly graduated medical doctors linked with the MOPH health personnel database, which allows tracking of medical graduates from the dates of entering to leaving the MOPH health services. The present study is limited to medical graduates who commenced work for MOPH hospitals between 2001 and 2015. The MOPH hospitals represent the hospitals that serve the large majority of the Thai population. Data on age, sex, training track, years of graduation, dates of entering and leaving the MOPH services (if applicable) for each medical graduate were obtained. Data were tracked up to 1 June 2016.
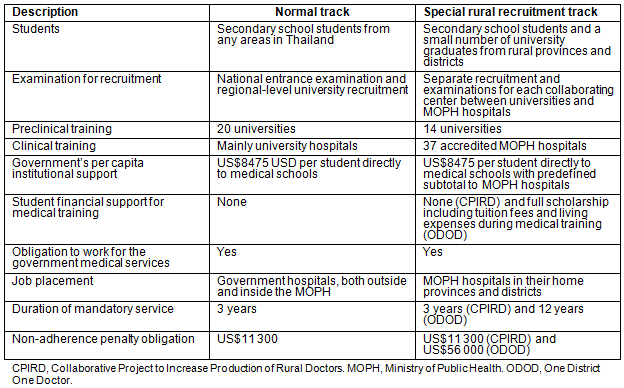
There are two main schemes of medical training in Thailand: a conventional track and special rural recruitment tracks17. Table 1 describes the two training tracks concerning student recruitment, preclinical and clinical training and postgraduation regulations. Briefly, a conventional recruitment and training of medical students, hereafter referred to as a 'normal track', has solely been operated by the Ministry of Education. Secondary school students are recruited to one of 20 medical schools based on their academic merits from the national entrance examination or regional-level university recruitment. Medical students under the normal track take a conventional 6-year course: three preclinical followed by three clinical years. Normal-track graduates are subjected to 3-year compulsory service, with a US$11,300 fine imposed for non-compliance. Their workplace is based on individuals' choice provided each year's vacancy availability.
The special rural recruitment scheme is a government-funded initiative aimed to increase the production of doctors who are to work for MOPH hospitals in rural areas. This scheme includes two distinctive tracks called the CPIRD (established in 1994) and the ODOD program (established in 2005). The CPIRD/ODOD is a collaboration between the Ministry of Education and the MOPH and includes 14 universities responsible for teaching preclinical subjects in partnership with 37 accredited MOPH hospitals nationwide teaching clinical subjects. Clinical teaching is operated by the medical education centre of each hospital with close collaboration and support from its affiliated university. Medical students under the CPIRD are recruited from their rural domiciles, mainly in mixed rural-urban provinces. The ODOD program extends student recruitment to those from more targeted rural and remote areas, with full government scholarship given to pursue 6-year medical training14. To further address maldistribution, regulations on job placement, duration of mandatory service and non-adherence penalty obligation are applied. CPIRD medical graduates are subjected to 3-year mandatory service in MOPH hospitals, with a penalty of US$11,300 imposed for non-adherence. Medical graduates under the ODOD program are liable to a 12-year mandatory service in the MOPH service hospitals in their rural home districts, with a fine of US$56,000 imposed for those who do not adhere to the mandatory service.
Data analyses
The numbers of medical graduates under the normal-track and special rural recruitment track commencing work in the MOPH hospitals between 2001 and 2015 were described. Overall and year-by-year retentions in the MOPH hospitals were compared across the two training tracks using the χ2 test. Retention was defined as the percentages of medical doctors who, up to 1 June 2016, remained working in the MOPH hospitals and health services. To emphasise the impact of the special rural recruitment track on retention in the rural areas where they are needed the most, the authors examined the percentages of CPIRD/ODOD graduates who remained working in the province to which they were primarily assigned, across four geographic regions of Thailand. In a subgroup of 11 736 medical graduates entering the MOPH between 2001 and 2012, the authors examined factors associated with retention in the MOPH health services for a minimum period of 3 years, using multiple logistic regression.
Ethics approval
As part of the CPIRD program evaluation, using administrative data on its graduates without access to sensitive and identifiable information was considered low risk, so this work was exempt from ethical approval.
Results
Between the employment years 2001 to 2015, a total of 19 338 medical graduates commenced work in the MOPH health services, 5909 (30.6%) of whom were from the special rural recruitment track. The number of doctors produced under the special recruitment track increased from eight in 2001 to 883 graduates in 2015. Of note, 63% of all medical graduates under this special track were produced in the last 5 years of the project (2011-2015), while the remaining 37% were produced in the first 10 years of the project (2001-1010).
Up to 1 June 2016, 7053 of 13 431 medical graduates under the normal track and 4621 from 5909 graduates from the special recruitment track remained working in the MOPH hospitals (overall retentions of 52.5% and 78.2% respectively). The doctor retention by training tracks and years of entering the MOPH is shown in Figure 1. The retention of medical graduates under the normal track ranged from 27.3% to 88.9%, with lower retention for those entering the MOPH earlier. The retention of those under the special rural recruitment track varied from 53.9% to 94.2%, with 62.5% of those first employed in 2001 remained working in the MOPH. For each entering year, doctor retention was higher in those under the special recruitment than the normal tracks (p<0.05).
Among 4869 medical graduates under the special recruitment track who remained working for the MOPH and whose workplace could be tracked, 4425 (90.9%) still worked in the provinces to which they were primarily assigned. The percentages of CPIRD/ODOD graduates who remained working in the province to which they were primarily assigned varied across four geographic regions, with the lowest percentage of 87.0 observed in the northern region of Thailand (Fig2).
In a subgroup analysis in 11 736 medical graduates, factors that were independently associated with 3-year retention in MOPH health services included training track, sex and geographic region (Fig3). Compared to their normal-track counterparts, medical graduates under the special rural recruitment scheme were about 2.4-fold more likely to remain working in the MOPH health services for a minimum period of 3 years (odds ratio (OR) 2.44, 95% confidence interval (CI) 2.19-2.72). Female doctors were 15% less likely to remain working in the MOPH than male doctors. Compared to medical graduates working in the central region, those in the northern region were 16% more likely to remain in the MOPH (OR 1.16, 95%CI 1.01-1.33), while those in the north-eastern region were 16% less likely to be retained in the MOPH (OR 0.84, 95%CI 0.74-0.95).
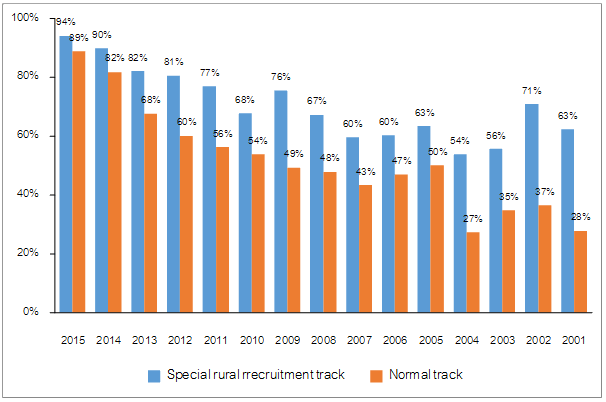
Figure 1: Retention of medical graduates under the normal and special rural recruitment tracks by year of work commencement in a Ministry of Public Health hospital.
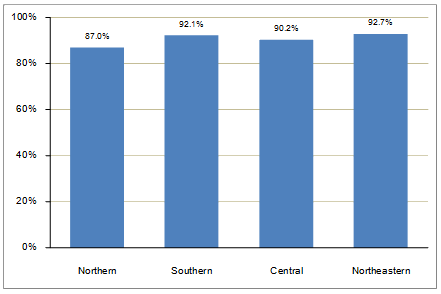
Figure 2: Percentages of medical graduates under the special rural recruitment scheme who remained working in the provinces to which they were primarily assigned, by geographic region.
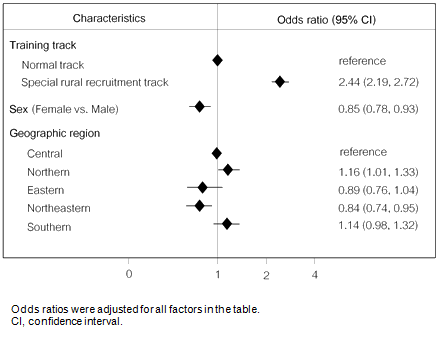
Figure 3: Association between training tracks and 3-year retention of 11 736 medical graduates in health services in the Ministry of Public Health, using multiple logistic regression.
Discussion
This article describes the retention of medical graduates who commenced work for the MOPH hospitals between 2001 and 2015 and compares the retention between the normal-track and special rural recruitment tracks. Medical graduates under the special recruitment track were more likely to remain in the MOPH health services than their normal-track counterparts. A considerable proportion of those under the special recruitment track who remained in the MOPH still worked in the provinces to which they were primarily allocated.
The beneficial effect of a collaborative approach used in Thailand's special rural recruitment scheme on doctor retention might be explained by a number of strategies, including educational measures, such as recruitment policy and utilising existing health services outside major cities as medical schools and training facilities and early exposure to rural services, followed by postgraduation regulations and policy interventions, such as regulated rural placement and mandatory service.
Educational strategies such as targeted recruitment policy to enrol students with rural background, early exposure to rural healthcare services and locating medical schools and training facilities outside the capital and major cities might help increase the likelihood of medical graduates choosing to work and remain in rural areas6-9,18,19. Students' rural background has been reported to be an independent predictor of rural primary care practice and retention9,20. It has been emphasised that doctors should be produced in real health service systems with enhancing community-oriented competencies such as teamwork skills and being a change agent20,21. The present study shows that special recruitment of medical students with rural backgrounds followed by clinical teaching in MOPH hospitals in provincial cities of Thailand, seen as early exposure to rural health services, probably has beneficial effects on the number of doctors who started and remained working in rural health services. Previous studies suggest that medical graduates under the special recruitment scheme are more likely than those recruited through a normal track to continue working in rural areas for a longer period after mandatory service22,23. As the large majority of graduates under the special rural recruitment track remained working in the provinces to which they were primarily assigned, this approach might also help improve Thailand's doctor maldistribution.
Various regulatory measures implemented under Thailand's special rural recruitment track may also positively affect doctors' decisions to work and remain in the MOPH health services. Compulsory service requirements in rural and remote areas are regulated to help increase recruitment and subsequent retention of doctors in the MOPH hospitals. The ODOD project may have had a greater contribution to addressing critical shortage of doctors than the CPIRD project as the former enrols students from the districts that evidently suffered from chronic shortage and the project requires a longer compulsory period of practice in the targeted MOPH hospitals.
Strategies to enhance friendly working environments may also have a significant impact on the adequacy of skilled and motivated health professionals to deliver effective health services3,6,8, which in turn may help improve retention in remote and rural areas. Medical graduates under the special recruitment track are required to undertake a 1-year internship in MOPH provincial hospitals in the area of their primary placement. This might help strengthen professional support and networks, which is believed to enhance the probability that they would continue working in remote and rural areas1,6. A systematic review by Lehmann and colleagues suggests that bundles of interventions including attention to living environments, working conditions and environments, and professional development opportunities are linked to attraction and retention of doctors in rural areas in low-middle income countries3.
Thailand is among a number of countries that have implemented a collaborative approach to increasing production and retention of doctors in rural areas. Collaboration in most countries was initiated by one medical school and mainly limited to the partnership between a single medical school and a small cluster of rural medical practices, involving a relatively short period of exposure to rural medical practices and healthcare services ranging from weeks to less than one year in Canada, Australia and the USA24,25. In contrast, Thailand's special rural recruitment project was initiated by the MOPH, traditionally a main user, seeking partnership with medical schools in producing doctors to serve the country's underserved areas. It involves 3-year preclinical teaching in 14 collaborating medical schools, followed by a 3-year clinical teaching in 37 mixed urban-rural MOPH hospitals of varying sizes nationwide.
Over the past few decades, Thailand's health system and healthcare services have evolved, for example, changes in national health insurance policy, more complex care teams and the introduction of systemic health service planning26. Such changes may shape the way health professionals, particularly newly graduated ones, see the country's health system and services and may have led to their decision to start and continue working in public hospitals. This is beyond the scope of this article, and hence further research is needed to understand the complex and multi-facet interaction between strategies used in this special recruitment initiative, postgraduation living and working environment and changing healthcare systems.
Financial incentive programs have been reported to possibly have benefits on helping raise the number of health professionals working in underserved areas. A systematic review of 43 studies including five different types of financial incentive program suggests that participants under the financial incentive programs are more likely than non-participants to work in underserved areas in the long run, although they are less likely to remain at the site of original placement27. However, most included studies are from Western countries and only few studies from developing countries. Consequently, it remains uncertain whether such benefits could be generalised to less well-resourced countries. In Thailand, there have been successive changes in strategies and interventions to address financial incentives in doctors working in the MOPH hospitals. One important financial intervention began in 2009, when doctors were given special incentives in return for providing services in rural district areas depending on rurality index and the duration they served in the area. However, it is unclear how and to what extent such intervention has influenced the retention of doctors under the normal and special recruitment tracks reported in the present study. To date, there is no evidence to systematically describe the impact of Thailand's financial incentive program for return of service and retention of doctors in rural areas, in relation to other interventions addressing working environment.
Due to a complex interplay of factors influencing the retention of doctors, a bundle of contextually relevant interventions and multi-sectoral collaboration within and beyond government are needed and these should be implemented in harmony3,6. No single intervention is likely to solve the complex aetiology of doctor shortage and maldistribution. Hence choices of interventions should be informed by a clear picture of health workforce and related policy context3. This requires a comprehensive situation analysis, a labour market analysis and an analysis of the factors influencing doctors' decisions to relocate to, remain in or leave rural and remote areas6. Engagement of stakeholders across several sectors is an essential element for the success of rural medical education, recruitment and retention policies6,21. As public and private health sectors have competitive recruitment, and bidirectional intersectoral movement is prevalent, a clear and comprehensive picture of the health workforce in both sectors is needed. Accordingly, effective health workforce planning should be done in collaboration between both the public and private sectors3,6.
Although the present study illustrates some aspects of the impact of Thailand's national collaborative approach to enhancing production and retention of medical doctors, it does not describe other dimensions of program evaluation. Further studies are needed to describe the relevance, acceptability and affordability of the programs6,28. Sound evaluation of policy interventions and programs has generally been lacking and this should be accomplished in order to inform ways to improve ongoing projects and to develop new ones. As data presented in the present article are based on MOPH health workforce database, it exclusively depicts recruitment and retention of doctors in the MOPH. Due to lack of data on workplace of the normal-track graduates, it could not be determined if graduates under the special rural recruitment track were more likely than their normal-track counterparts to remain working in the provinces to which they were primarily assigned. However, this embraces critical processes of the special rural recruitment initiative and outputs at which it was specifically aimed.
Conclusions
A special rural recruitment initiative based on collaboration between the Ministry of Education and MOPH had significant impact on enhancing retention of doctors who worked in the MOPH health services, which serve most of the Thai population. However, progress on comprehensive health workforce information, multisectoral health workforce planning, strategies to generate friendly working environments and specific financial incentive programs is needed to further improve Thailand's doctor shortage and maldistribution.
Acknowledgements
The authors thank Mr Nawapat Umthong for research data management.
References



