Introduction
The international rural medical workforce shortage is well recognized1,2 and as a consequence it is important to understand factors influencing medical students to become interested in working in rural areas. There is strong evidence that the geographical background of a doctor is a predictor of practice locality3-18. Rural doctors are two to four times more likely than urban doctors to have a rural background5,11,12,16,19. Nevertheless, studies have identified that 34% to 67% of rural doctors have an urban background5,11,12,16,19.
Rural practice is also associated with undergraduate and postgraduate experience in rural areas8,11,20,21 and rural background of spouse/partner22. Factors attracting and deterring students from rural practice relate to work, community and family issues23,24.
Research has investigated specialty and general practice career choice as a socially constructed process25, and how 'sense of place' can be used to understand retention of rural doctors26. However, research on rural medical recruitment is lacking in qualitative rich data, and questions relating to how urban background students develop an interest in rural practice remain unanswered. This article presents findings from a broader project and outlines the first qualitative data focusing on rural career interest among urban background students.
Methods
Sample
Between March and August 2002, ten focus groups of 6-10 medical students were conducted at three Australian universities and a national student rural health conference. All focus groups were homogeneous for stage of training (either first or final year) and at least one other factor (gender, medical school admissions process or rural interest). These factors were chosen because it was thought that they may contribute to the students' attitudes to rural practice. Between July and December 2003 semi-structured interviews with 49 first and final year medical students from three New South Wales (NSW) universities were undertaken. These universities were chosen because of their geographical locations (including two capital city and one regional city medical schools) and differing entry criteria (including graduate entry, undergraduate entry and mixed entry schools). Characteristics of interview students are shown (Table 1). Maximum variation sampling was used, with researchers attempting to include students from different demographic backgrounds.
Table 1: Universities, years of study background and sex of interview participants
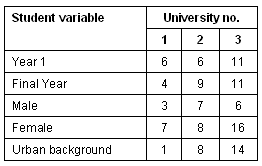
The students
Eighty-two students, 36 male and 46 female, participated in the focus groups. Forty-eight students, 18 male and 38 female, were interviewed. The age range of the students was from 17 to 40 years. A variety of participants were included: single and married; those with children and those without; undergraduate and graduate students; those with many years work experience (in a variety of occupations) and those who entered university immediately after completing their secondary education; and others from Aboriginal and non-English speaking backgrounds.
Recruitment of participants
Invitations to participate in the focus groups and semi-structured interviews were by electronic notices on the three medical faculty web sites. Recruitment for the interviews was also via a paper notice distributed to faculty tutorial groups and by announcement at a student rural health conference. All recruitment notices and announcements explained that participation was not restricted to students interested in rural practice - in line with the aim of the broader project.
Focus group and interview questions
The focus groups lasted between 60 and 90 min. The interviews, lasting 20 to 40 min, were conducted face to face except for five conducted via telephone. The same questions were used for the focus groups and interviews; and were developed, on the basis of the literature review, specifically for the purposes of this project. Questioning focused on the students' attitudes and intentions in relation to: discipline of medicine, geographical location, practice environments in which they wished to work; and influences on their career intentions and the decision-making process. While a theme list was used to structure the interviews, the project incorporated an informant-led approach and data collection was sensitive to the issues raised by subjects.
Data analysis
The focus group sessions and interviews were recorded on audiotapes and later transcribed. The transcriptions were analysed for content and emergent themes using the N6 computer package (QSR International; Melbourne, VIC, Australia)22 to organize data. Data were coded and checked independently by two researchers who discussed the data to come to a consensus on its meaning, ensuring researcher triangulation. Data from the two methods were compared to ensure methodological triangulation.
Geographical background of students
Data were analysed to identify urban background students with an interest in rural practice. In line with previous studies, geographical background is here defined as the area where a student has spent the greater part of his or her childhood11,27.
Employing this definition, 47 focus group participants were identified as being of urban background with 25 of these indicating an interest in rural practice. Forty-seven interviews provided sufficient data for analysis of participants' background. Of the 23 urban background participants identified from the interviews 18 indicated an interest in rural practice.
Ethics
Ethical issues for this project related to informed consent of participants in the focus groups, and the maintenance of confidentiality. Ethics approval was given by the Human Research Ethics Committees of the Universities of Newcastle, Sydney, and NSW prior to commencement of the project.
Results
Analysis shows the students' level of interest in rural practice depends on a complex interaction of factors relating to student characteristics, the locations they consider for practice and other external influences. Student factors and related location factors associated with an interest in rural practice are listed (Table 2).
Table 2: Related student and location factors

Similarities and differences in first and final year cohorts
Because the sample included young students who were school leavers and older graduate and mature age students, the differences between individual students related more to their age and life experiences rather than to their year of study. Some mature age first year students had lived and worked in rural areas for prolonged periods prior to studying medicine and these experiences had a major influence on their location intention. In contrast younger students (both first and final year), who did not have commitments to partners and children, tended to be more uncertain about their future location and were more likely to want to 'go everywhere'.
Social and geographical familiarity
Most students expressed a preference for places with which they were familiar or which were similar to places where they had had past experience, for example saying their location choice would depend on 'what you know' (Fig 1).

Figure 1: Student and location factors: words of the students.
Some had had very little experience of rural life but were open to learning more about it and changing their preferred location as a result of experience, for example a first year female student said:
I haven't been inland very much so I don't know what it is like there...but hopefully if I do a placement there I might be able to find out what it's like.
Most who were interested in rural practice indicated they preferred such features as 'the people and mainly the pace, and your closeness to the environment without the traffic'.
Values
Most students were motivated by altruism, indicating that a desire 'to make a difference in people's lives' was a major reason for considering rural practice. They were aware of the ' real unmet need in the country', because of what they had heard in the media and at the university, their own experience during rural placements or in previous work they had done, or the experience of family and friends living in rural areas.
Some expressed a preference for working in the public health system or in salaried positions rather than private practice, seeing this as more consistent with their philosophy.
Work interests
Another theme emerging from the data was a preference to work as either rural GPs or rural general specialists, because of 'the variety' and 'the diversity of medicine'. Many indicated that 'knowing patients and knowing them in greater context than say you would in a Sydney hospital or whatever' appealed to them.
Many expressed a preference for group practices with shared on call work, with several indicating they would not be interested in solo practice. Those interested in specialties realised that 'you've got to be in a large enough place to have a patient base really' so they would need work in a large rural town.
Life experience interests
A theme relating to 'short-term adventure' also emerged, with younger students expressing interest in working in a rural area in the short term, being attracted by 'the foreignness and the opportunity of it' . These students tended not to see rural practice as a long-term option but were seeking short-term adventure lasting a year or two, although some were open to the influence of short-term experience on their long-term career choices.
Lifestyle preferences and leisure interests
A theme relating to lifestyle preferences was also identified. Most saw the rural environment as a 'much nicer and healthier place to live' and preferred 'being able to be outdoors, instead of being in the city where there's lots of travel'.
Unlike students interested only in urban careers, they felt they would enjoy rural social life and leisure pursuits. Many indicated that they were attracted to rural areas by 'the beach and the mountains and all that sort of nice stuff' and 'fabulous wineries and stuff like that'.
Close social relationships
Close social relationships were discussed by most students. Almost all who had partners were concerned about their partner's ability to find suitable work in a rural area. Some had partners working in occupations for which work would be readily available in rural areas, with others indicating their partners were seeking a career change or break and would be willing to work differently, for example from home using electronic communications, if they moved to a rural area.
When asked about possible future changes to career plans many, especially female students, indicated that a 'job for your partner... would be extremely important' and their intentions would change if their partner was 'somebody that needs to work in the city'.
Some felt that rural areas provided a better lifestyle for young children but had concerns about 'schooling opportunities for older children' and stated that they 'wouldn't want to send my children to boarding school'.
Some were concerned about their parents' attitudes to their moving to a rural area, wanting to be 'within driving distance' of 'older parents' so that they could support them, while others anticipated a need for 'grandparental support' in the future.
Influences
The students identified a number of factors influencing them to develop an interest in rural practice.
Previous rural experience: Some students had some rural experience during previous undergraduate training, previous work or because of visits to friends or extended family. Some students' rural experience had been in developing countries or remote areas and they had a commitment to working in communities with high levels of health-care need.
Rural undergraduate experience: placements rural and urban: Many indicated that undergraduate experience was a major influence in their developing an interest in rural practice. For some, who had initially had no interest in rural practice, their rural placements were their first rural experiences and had influenced them to consider working somewhere 'that I just never would have thought of before'. Some students had been interested in rural practice prior to the rural placements and their interest was reinforced by the rural placement. Students who had undertaken longer-term placements felt that 'actually making friends and really getting to know what living in that community was like you know played a major part in that decision'. Some, especially those interested in general practice, had been influenced by the contrast between negative experiences during urban placements and positive rural experiences.
Most participants did not regard all rural and remote areas as being the same. Those who had had rural experience, either prior to entry to medicine or during their undergraduate training, were aware of issues relating to the remoteness and size of the town. They distinguished between living and working in a rural and remote area, and between working in a small or large rural town. For example, a final year student said:
I've been to...about half a dozen small towns during the past 2 years, ranging from larger size (30-40 000) all the way down to somewhere like [small town} which is about a population of a few thousands, about 5000. So ... not so much in a small town ...but I would be happy to work in just the larger towns.
Another contrasted the remoteness of two towns where she had undertaken placements:
I don't think [remote town]'s a place to live long term 'cause it's quite cliquey and, also just very very isolated like, whereas here less remote rural town] you can travel to a town like within an hour.
Role models: A number had been inspired to consider rural practice by doctors whom they had met and worked with. Sometimes this had happened prior to their entry to medical training and had also inspired them to consider a career as a doctor.
Bonded scholarships: Eleven students held scholarships which obliged them to spend a period of time working in a rural area after graduation. Final year students had state government funded scholarships which obliged them to work in rural areas during their junior doctor years, while first year students had federal government funded scholarships which obliged them to work in rural areas after completion of postgraduate training. All scholarship holders indicated that they had been interested in rural practice prior to taking up the scholarship, with the scholarship reinforcing their preexisting interest in rural practice. However all of the first year students indicated that 'a big part of the reason' for taking the scholarship 'was the money'.
University: location, student mix and faculty attitudes: Some students attending regional universities commented that moving from a capital city to regional city had broadened their outlook so they realized:
that there are all these other places, and that there are other places outside of [capital city] and that it's not the be all and end all, which is the mind set of a lot of [capital city] people.
Some commented on the influence of meeting students from rural backgrounds, the proximity to rural areas and positive attitudes of faculty to rural practice.
Conclusions
The sampling method for this study involved self-selection of students so it is possible that some participants may have had strong views on aspects of the topic being discussed, and generalization of the results should be undertaken with care. However, the study provides new insights into why and how urban background students develop an interest in rural practice, which could be used to develop larger quantitative studies.
Previous researchers have identified a number of factors underlying rural career choice by medical students, usually considering associations between factors or groups of factors quantitatively4,11,20-22,24,28-30. However this study used qualitative methods to investigate the process of the development of an interest in rural practice by urban background students.
In discussing his research on general practice and specialty career choice, Burack suggested 'the process of specialty choice can be described as a socially constructed process of "trying on possible selves"'25. Participants in this study seemed to go through a similar process, seeking to find locations that would match their interests and needs, and where they would have some 'sense of personal fit'25, as well as being able to maintain significant social relationships.
The students could be described as being 'predisposed' to developing an interest in rural practice because of their openness to changing their geographical preferences, their high level of altruism, their interest in generalist work, and interest in leisure activities which could be accommodated in a rural area. When exposed to rural locations, which provided them with knowledge of how their interests and needs could be met in a rural area, and which matched their values and interests, or to rural role models with whom they could identify, they became interested in rural practice. Most became interested in moving away from an urban area in response to rural experience, with some being influenced by relocating from a capital city to a regional city. The rural interest of some students was reinforced by rural scholarships. For some students, existing social relationships were an enabling factor for taking up a career in rural practice, while for others they were a limiting factor because their partners or close families were unable or unwilling to relocate to a rural area.
These findings are consistent with previous research on rural doctor recruitment4,11,20-22,24,28-30. Some predisposing student factors have been identified in previous studies, for example Somers found that rural intent medical students scored 'a sense of being needed' more highly than urban intent students24, and Rabinowitz found that doctors who practised in underserved areas were more likely to have had a strong interest in practising in an underserved area prior to attending medical school31.
The preference of students for areas with which they were familiar provides an understanding of how rural background and rural experience contribute to a doctor's interest in rural practice.
The importance of close social relationships has also been identified in previous studies. For example some studies have found an association between rural practice and rural background of the doctor's spouse22, and others found students see opportunities for spouse/partner as important in relation to rural practice24,29.
The findings reported in this article could be used for further research and rural recruitment strategies. Increasing the numbers of rural background medical students has been used as a strategy to increase rural recruitment4,8,14. It may also be possible to increase rural recruitment by increasing the numbers of 'predisposed' urban background students studying medicine.
This study provides further evidence on the role of rural undergraduate experience5, attendance at regional universities, and rural role models in influencing medical students to become interested in rural practice. While previous research has tended to treat rural experience as a homogeneous entity5,11,21, this study showed the students' interest in rural practice differed according to the remoteness of the community and the size of the town; and they responded differently to experience in different locations. Although some students who had had rural and remote experience felt mismatched with remote communities and small towns, they still saw a larger town as an option for the future. Exposure of students to rural experience in a range of locations may increase the number of students who develop an interest in rural practice by maximizing their opportunities to find a location that matches their values and interests. Further research investigating the effects of providing students with a variety of rural and remote experiences is needed to confirm this finding.
Acknowledgement
The authors wish to acknowledge the National Health and Medical Research Council who provided funding for this research project.
References
1. Hicks LL. Social policy implications of physician shortage areas in Missouri. American Journal of Public Health 1984; 74: 1316-1321.
2. Wilkinson D. Inequitable distribution of general practitioners in Australia: analysis by state and territory using census data. Australian Journal of Rural Health 2000; 8: 87-93.
3. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93: 789-793.
4. Kamien M, Buttfield IH. Some solutions to the shortage of general practitioners in rural Australia. Part 1. Medical school selection. Medical Journal of Australia 1990; 153: 105-107. [Comment].
5. Rolfe IE, Pearson SA, O'Connell DL, Dickinson J. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian and New Zealand Journal of Medicine 1995; 25: 512-517.
6. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
7. Kassebaum DG, Szenas PL. Rural sources of medical students, and graduates' choice of rural practice. Academic Medicine 1993; 68: 232-236.
8. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. JAMA 2001; 286: 1041-1048.
9. Becker P, Hartz A, Cutler J. Time trends in the association of a rural or urban background with physician location. Journal of Medical Education 1979; 54: 544-550.
10. Colditz GA, Elliott CJ. Queensland's rural practitioners: background and motivations. Medical Journal of Australia 1978; 2: 636-636.
11. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location Canadian Medical Association Journal 1999; 160: 1159-1163.
12. Wilkinson D, Beilby JJ, Thompson DJ, Laven GA, Chamberlain NL, Laurence CO. Associations between rural background and where South Australian general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
13. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. Which medical schools produce rural physicians? JAMA 1992; 268: 1559-1565.
14. Rabinowitz H. Recruitment and retention of rural physicians: how much progress have we made? Journal of the American Board of Family Practice 1995; 8: 496-499.
15. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
16. Strasser RP. Attitudes of Victorian rural GPs to country practice and training. Australian Family Physician 1992; 21: 808-812.
17. Kamien M. Report to the Ministerial Enquiry into the recruitment and retention of country doctors in Western Australia. Perth: University of Western Australia, 1987.
18. Alexander C. The shortage of rural general practitioners in north western NSW. Australian Journal of Rural Health 1997; 5: 31-36.
19. Cooper JK, Heald K, Samuels M. Affecting the supply of rural physicians. American Journal of Public Health 1977; 67: 756-759.
20. Hays, RB, Nicholls, Wise A, Craig M, Adkins P, Mahoney M. Choosing a career in rural practice in Queensland. Australian Journal of Rural Health 1995; 3: 171-174.
21. Kamien M, Buttfield IH. Some solutions to the shortage of general practitioners in rural Australia. Part 2. Undergraduate education. Medical Journal of Australia 1990; 153: 107-108, 112.
22. Laven GA, Beilby JJ, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
23. Silagy CA, Piterman L. Attitudes of senior medical students from two Australian schools towards rural training and practice. Academic Medicine 1991; 66: 417-419.
24. Somers GT, Young AE, Strasser R. Rural career choice issues as reported by first year medical students and rural general practitioners. Australian Journal of Rural Health 2001; 9(Suppl1): S6-S13.
25. Burack JH, Irby DM, Carline JD, Ambrozy DM, Ellsbury KE, Stritter FT. A study of medical students' specialty-choice pathways: trying on possible selves. Academic Medicine 1997; 72: 534-541.
26. Cutchin MP. Physician retention in rural communities: the perspective of experiential place integration. Health and Place 1997; 3: 25-41.
27. Cullison S, Reid JC, Colwill JM. The rural-urban distribution of medical school applicants. Journal of Medical Education 1976; 51: 47-49.
28. Cullison S, Reid C, Colwill JM. Medical school admissions, specialty selection, and distribution of physicians. JAMA 1976; 235: 502-505.
29. Piterman L, Silagy C. Hospital interns' and residents' perceptions of rural training and practice in Victoria. Medical Journal of Australia 1991; 155: 630-633.
30. Rabinowitz HK, Diamond JJ, Veloski JJ, Gayle JA. The impact of multiple predictors on generalist physicians' care of underserved populations. American Journal of Public Health 2000; 90: 1225-1228.
31. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. Journal of American Medical Association 1999; 281: 255-260.

