Introduction
It is estimated that each year 3 to 5 million migrant farmworkers leave their home area to travel the USA to secure employment in agriculture. This is a diverse population and its composition varies from region to region. However, it is estimated that 85% of all migrant farmworkers are minorities with the largest group being Hispanic, which encompasses subgroups of Mexican Americans, Mexicans, Puerto Ricans, Cubans, and individuals from Central and South America1.
Farmworkers continue to be one of the most impoverished and underserved populations in the USA. They suffer from mortality and morbidity rates greater than those of the majority of the American population because of the combination of poverty, limited access to health care, and hazardous working conditions2.
In this highly mobile population, access to quality health care continues to be a pressing problem. Due to the migrant farmworkers' low annual wages, they are frequently unable to pay for needed health care, and many farmers do not provide employer-based health insurance coverage1. Other barriers to the much needed health-care services for this population include lack of transportation to clinics, loss of wages due to medical appointments, and fear of losing their jobs if time is taken off during the day for medical appointments1. Limited access to health-care services can be especially problematic when farmworkers are diagnosed with conditions such as tuberculosis, diabetes, cancer, and HIV-related illness which require extensive monitoring and treatments that entail multiple visits1.
Hispanic farmworkers are especially vulnerable to diabetes. Research has shown that this chronic disease disproportionately affects Hispanic Americans1,3-4. Typically, these Americans are twice as likely to have diabetes as non-Hispanic Caucasians of similar age5.
Diabetes is a chronic disease that requires clients to schedule multiple office visits with a multidisciplinary team to learn how to successfully manage and delay the progression of complications. The scheduling of these visits is problematic for many populations but especially for those who migrate across the USA for employment and already have limited access to health care1.
In response to the health needs of Hispanic migrant farmworkers who travel to Minnesota and North Dakota, the Migrant Health Service Inc (MHSI) diabetes program coordinator, a doctoral-level registered nurse, implemented evening cluster clinics. These clinics provided health care, education and counseling to clients diagnosed with diabetes. Through their attendance at a single cluster clinic, clients were able to accomplish 11 office visits in 3-4 hours. The theoretical model on which these cluster clinics are based is described in Heuer, Hess, and Klug6.
Purpose
The purpose of this study was to describe the Hispanic migrant farmworkers' perceptions of services provided at the multidiscipline cluster clinics from May 1998 to October 2003. During this period, there were 37 cluster clinics that served a rural population that spanned an area of 447 linear miles from northeastern North Dakota through southern Minnesota.
Methods
Context of this study
Migrant Health Services Inc provided the leadership, management, administration, and financial support for cluster clinics as part of a more comprehensive diabetes program implemented in rural Minnesota and North Dakota since 1998. The mission of the MHSI Diabetes Program is the reduction of the elevated mortality rate and high medical costs associated with diabetes in the Hispanic population through quality, culturally-sensitive health-care services accompanied by effective client self-management.
Starting in 1998, there were seven 'mini-clinics' or 'stations' within each cluster clinic as well as a registration station and an exit interview station. A laboratory station was used to obtain blood specimens for analysis of hemoglobin AlC, microalbumin, cholesterol, and blood sugar. Measurements of blood pressure, height and weight were obtained at the physical assessment station. Screening of sight with a Snelling eye chart and the administration of pupil dilation eye drops occurred at the eye examination station. At the next station, an ophthalmologist conducted a retinopathy examination. Podiatry care was provided within a foot examination station. At two additional stations, a dietician and a diabetes educator consulted, advised and educated clients. At the exit interview, clinical findings were reviewed and clarified with the client, recommendations and follow-up procedures were reinforced, and medical referrals were made as needed. Over time three stations were added to address additional client health and educational needs. In 2000, a dental hygienist began client education and distribution of dental products. A foot care station was added in 2002, so that feet were soaked, toenails were clipped, calluses were filed, and then the feet were massaged. Electrocardiogram baseline measurement was added as an eleventh station in 2003.
Health care, education, and counseling were provided at these MHSI cluster clinics in accordance with the American Diabetes Association Clinical Practice Recommendations7. Education and counseling addressed such issues as nutrition, diet, exercise, tobacco use, foot care, and access to recommended services and referrals6. To reinforce the educational component taught at each particular station, clients were given incentives such as white socks at the foot care station, a bottle of glucose strips at the diabetes educator station, and fruit or healthy snacks at the nutritionist station.
Both Hispanic bilingual health outreach workers (BHOs) and diabetes lay educators (DLEs) served in the cluster clinics as 'insiders' providing intra-cultural perspectives and language interpretation. The BHOs were staff members at the sponsoring migrant health nurse-managed health centers. The DLEs were natural leaders from the migrant farmworker communities in Minnesota and North Dakota recruited to provide language translation, client advocacy, and cultural information during seasonal health-related activities of this migrant population6.
For cultural and physical reasons, healthy food choices such as sandwiches, vegetables, chips, salsa, fruit and a non-sugar lemonade drink were provided at each clinic. Because food is inherent to social gatherings of this population, it was served to promote a welcoming environment. Further, many of the farmworkers had not eaten an evening meal; they had come to these clinics from their fieldwork. Therefore, the food was also used for glycemic control.
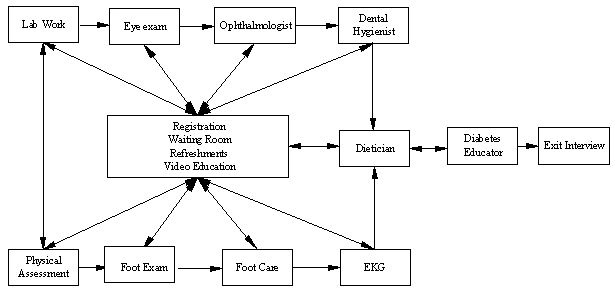
Figure 1: Physical arrangement of mini-clinics within a cluster clinic.
Research design, data, and data analysis
This study involved both quantitative and qualitative descriptive research methodologies8. Two sources of data were used: (i) a written survey of 566 clients; and (ii) in-depth individual interviews conducted with12 clients.
Subjects
Two samples of subjects provided data for this study. The first sample consisted of the 566 clients (85% of the 666 clients served in the 37 cluster clinics between 1998-2003) who had returned a 15-item English/Spanish questionnaire administered at the end of each clinic. This instrument elicited client perceptions of the quality of the cluster clinic services. Twelve of these clients (seven females and five males) constituted a convenience sample based on their willingness to participate in individual interviews, and the availability of two researchers and an assisting DLE interpreter. The purpose of the interviews was to expand on and verify written comments provided on the questionnaire.
All of the 566 clients were Hispanic, and 91% had type-2 diabetes. Spanish was the primary language of more than 40% of these clients, who ranged in age from 23 to 77 years (M = 51 years; SD = 11 years) with 14% being 65 years and older. Females constituted 53% of the sample. The subjects' annual household income ranged from none to US$32,000 (M = $9988; SD = 5751). The most common sources of non-personal funding for medical costs were MHSI vouchers and state programs, used by 83% of the subjects. Only 1% had private health insurance; 8% had Medicare; and 4% had Medicaid coverage.
Instruments
The 15-item client questionnaire was available in both English and Spanish. The instrument elicited both quantitative and qualitative responses. A four-point anchored scale (excellent, good, fair, and poor) allowed clients to rate 11 cluster clinic services. Two yes/no items and two open-ended questions elicited the remainder of the client feedback. The specific questionnaire items are presented with the results below.
A protocol used for the individual interviews included three open-ended questions. Question 1: What are the benefits of these clinics for you? Question 2: What have you learned about diabetes at these clinics? Question 3: What other needs do you have that are not being addressed? These questions elicited information about cluster clinic benefits, barriers, and suggestions for improvement.
Procedures
At the end of each Cluster Clinic, clients were provided with the opportunity to complete the questionnaire. Due to the literacy level and/or dilation of the clients' eyes, a BHO read and completed the questionnaire for the majority of the clients. To guard against introducing bias into the data, the BHO received specific instruction in data collection procedures and the importance of valid and reliable data collection. Further, no item on the questionnaire referred specially to the BHO.
The 12 interviews were conducted at two of the 37 cluster clinics. One researcher asked the questions while the second researcher typed the responses into a computer. On completion of the interviews, the qualitative data were analyzed through systematic reduction, unitizing, coding, categorizing, and identification of themes9. This study was approved by the University of North Dakota Institutional Review Board.
Results
Client Perceptions of the Cluster Clinics
In the written survey, two 'yes' and 'no' items were designed to elicit clients' general perceptions of the cluster clinic staff's performance. The data were intended as one type of formative evaluation for use in administrative monitoring of the general atmosphere of client intake procedures. The clients were asked, 'Were you greeted by a receptionist when you entered?' Over the six-year period, 96% of the clients answered affirmatively. The clients were also asked, 'Were you satisfied by the way staff members treated you?' More than 99%, all except three clients, responded 'yes.'
Clients attending the 37 cluster clinics were asked on the questionnaire, 'Overall, how would you rate the services provided at this clinic?' Differing numbers of the 566 clients who responded to at least part of the questionnaire rated each of the 11 services. Client ratings were aggregated (Table 1). From 75-88% of the clients rated the 11 services as 'excellent'; an additional 21-25% rated them as 'good.' Only seven (1.2%) respondents rated some aspects of the services as fair, while one (0.2%) provided a rating of poor for one service.
Table 1: Number and percentage of client ratings of cluster clinic services 1998-2003
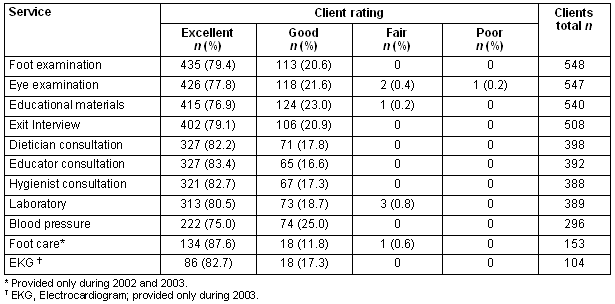
Clients were also asked, 'Do you have any other comments for MHSI to help us improve services provided at evening clinics?' The data are reported (Tables 2 and 3). A large majority of the clients' feedback consisted of the positive comments identified in Table 2. More than 85% of the clients indicated either that nothing should be changed (59%) or that everything was fine (26%). Twelve other types of comments were provided with the frequencies indicated.
Table 2: Clients' (n = 566) positive comments '...to help us improve services provided at evening clinics' 1998-2003
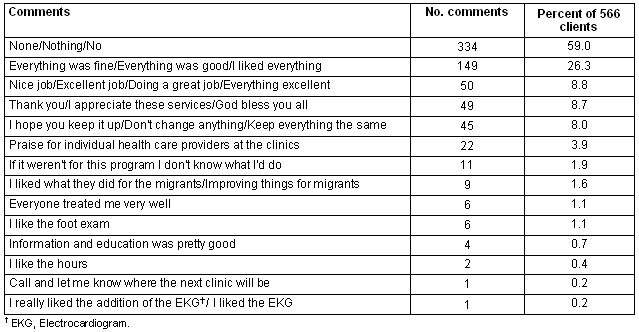
Table 3: Clients' (n = 566) suggestions '...to help us improve services provided at evening clinics' 1998-2003
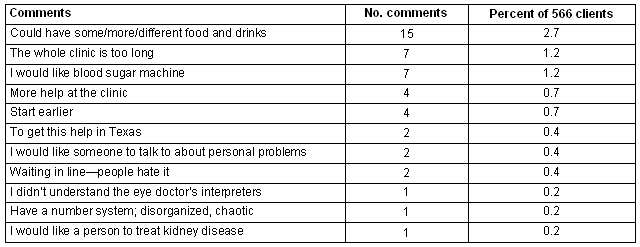
As shown (Table 3), over the 6 years only 46 comments of the 566 clients identified 11 aspects that they perceived would improve services. Nearly one-third (n = 15) of the written comments addressed food. Some clients perceived that the healthy snacks and sugar-free beverages were insufficient because those clients came directly from the fields to the clinics. Other respondents requested food during a trial period when only beverages were available. Still others requested a greater variety of food because they were often accompanied by their family members. Other comments addressed time and clinic organization, as well as requests for equipment and additional services. Within the limits of the available resources, changes were made based on this client feedback.
During the individual client interviews, responses to three guided questions yielded the 11 major themes identified (Table 4). Sample comments are quoted to illustrate those themes. Only data that did not duplicate results obtained on the written questionnaire are included in Table 4. Overall, clients perceived that they greatly benefited from their attendance at the cluster clinics.
Table 4: Themes and sample comments extracted from 12 client Interviews addressing three guide questions (Q1-Q3)

Discussion
The data provided by the cluster clinic clients suggest that these clinics provide valued and needed services. As a result, the authors have identified six characteristics that have contributed to the success of these clinics. The first characteristic is the provision of both direct and referral services to this underserved population who has low income, limited access to private insurance, minimal access to Medicare and Medicaid coverage, and migrant lifestyle.
The second characteristic is comprehensive delivery of services by a single source, at one time, in one place. The services consist of: (i) screening, identifying, monitoring, serving, and referring clients relative to the American Diabetes Association's clinical practice recommendations; and (ii) providing education, psychosocial support and advocacy to enable ultimate self-management in such areas as nutrition, exercise, weight control, dental hygiene, foot care and eye health.
The third characteristic is the collaborative delivery of these services. Collaborative participation involves the coordination of schedules for numerous health-care providers and support staff who offered their services, for pay, during evenings at some non-clinical, non-medical facility, in settings in which these professionals do not typically work, for example, a church, school or social service agency. Further, cluster clinic services require the collaborative sharing of project information and client records to assure continuity and appropriateness of care for this mobile population while maintaining high standards of confidentiality and informed consent. Successful collaboration also involves: (i) healthcare providers' recognition of the need and acceptance of the challenge to provide services under the cluster clinic conditions; and (ii) clients' development of sufficient trust to motivate their participation.
The fourth characteristic is access-driven delivery of services. The healthcare and diabetes education of cluster clinics is provided to the migrant Hispanic farmworkers in places where they can access it during the time they have away from fieldwork in the evenings.
The fifth characteristic is delivery of culturally-sensitive and linguistically-appropriate services. Such services are achieved through: (i) support and advocacy for the clients; (ii) language interpretation services; and (iii) education for the healthcare providers about cultural issues such as traditional, alternative medicinal practices and culturally-sensitive approaches and responses to Hispanic farmworker clients.
The sixth characteristic is the revision of service delivery based on client feedback from the cluster clinics. Data collection, analysis, and translation are on-going procedures in the research and program evaluation agendas set for the cluster clinics. The diabetes program coordinator, the MHSI Executive Advisory Board, and the health-care providers also use the client demographics, client health-care information, and cluster clinic participants' (ie, clients and providers') perceptions to guide decision-making and service provision.
Conclusions
Providing quality services in a location that is accessible and sufficiently adaptable to meet the needs of both the health-care providers and the clients requires on-going evaluation and creative ingenuity. Four of the primary challenges include: (i) locating and preparing facilities; (ii) recruiting health care providers for the clinics; (iii) achieving effective, appropriate communication with clients; and (iv) securing funding.
Finding, leasing, scheduling, and preparing facilities in which to operate the cluster in a church, school, health facility, or agency site. These seemingly 'make-shift' arrangements are the only feasible way to provide accessible services in highly rural areas where the migrant farmworkers are employed.
Staffing for each cluster clinic consists of hiring 25-30 providers. This multidisciplinary team consists of migrant health nurses, BHOs, DLEs, and numerous community providers. At times, recruitment of providers is challenging because their participation in the evening cluster clinics is in addition to their 'day jobs' clinics is a consistent challenge. Because no physical facilities are dedicated only to cluster clinics, every individual clinic has to be physically set up before and taken down after each evening
Overcoming the linguistic and cultural barriers to provide health care to Hispanic clients increases the challenges for the provision of culturally-sensitive care. Clients' linguistic needs and literacy levels require continuous assessment and intentional problem solving.
The most troubling challenge remains, even now, securing need-based permanency of funding for cluster clinics. Initiated with Rural Health Outreach grant monies, the present project was later shifted to federal funds with which it continues to be supported. The unpredictable, erratic availability of funding from federal and foundational health or migrant health sources leaves this project in annual jeopardy.
Cluster clinics are designed to meet the health care, educational, and counseling needs of the Hispanic migrant farmworkers diagnosed with diabetes. These clinics are a feasible and effective way of improving health-care services to a mobile population. Through the use of multi-disciplinary providers, culturally-sensitive health care is provided for Hispanic migrant farmworkers in the rural settings of Minnesota and North Dakota. Although there are continual challenges to implementing these cluster clinics, the services increase access to health care and self-management skills for a vulnerable, underserved population. Quality health care and education can be provided through clusters clinics in ways that will, over time, reduce health-care disparities for this population.
Acknowledgements
This study was supported in part by a grant from the US Department of Rural Health, grant no. DO4RH 00251-03. Gratitude is expressed for the research and technical assistance of Andrea Smith, Chronic Disease Manager, and Kristi Jacobson, Research and Enrollment Facilitator.
References
1. National Center for Farmworker Health. Overview of American farmworkers. (Online) 2005. Available: http://www.ncfh.org/aaf_01.php (Accessed 14 January 2005).
2. Migrant Clinicians Network. The Migrant/Seasonal Farmworker. (Online) 2005. Available: http://www.migrantclinician.org/migrant_info/migrant.php (Accessed 14 January 2005).
3. Center for Disease Control. Health disparities experienced by Hispanics - United States. Morbidity and Mortality Weekly Report 2004; 53: 935-937.
4. Center for Disease Control. Self-reported prevalence of diabetes among Hispanics - United States, 1994-1997. Morbidity and Mortality Weekly Report 1999; 48: 8-12.
5. National Diabetes Information Clearinghouse. Hispanics/Latinos diabetes. (Online) 2002. Available: http://diabetes.niddk.nih.gov/dm/pubs/hispanicamerican/ (Accessed 14 January 2005).
6. Heuer L, Hess CW, Klug MG. Meeting the health care needs of a rural Hispanic migrant population with diabetes. The Journal of Rural Health 2004; 20: 265-270.
7. American Diabetes Association. American Diabetes Association: Clinical Practice Recommendations. Diabetes Care 2004; 3: S15-S35.
8. Gall JP, Gall MD, Borg WR. Applying educational research: A practical guide, 5th edn. Boston: Pearson, Allyn, and Bacon, 2004; 3-4, 179-185.
9. Lincoln YS, Guba EG. Naturalistic inquiry. Beverly Hills, CA: Sage, 1985; 339-356.
Abstract
Introduction: Diabetes is a chronic disease that requires individuals to schedule multiple office visits with a multidisciplinary team to learn how to successfully manage and delay the progression of complications. To respond to the health-care and educational needs of Hispanic migrant farmworkers who travel to Minnesota and North Dakota, the Migrant Health Service Inc diabetes program coordinator implemented evening cluster clinics. The purpose of this research project was to describe Hispanic migrant farmworkers' perceptions of the services provided to them at 37 multidisciplinary cluster clinics designed to serve this rural population diagnosed with diabetes.
Methods: This descriptive research employed a questionnaire and individual interviews. Both quantitative and qualitative data were obtained from cluster clinic clients. Quantitative data consisted of the numbers and percentages of clients providing various responses to questionnaire items. The qualitative data consisted of the verbal responses of clients to two open-ended questionnaire items and to an interview protocol.
Results: The main findings of the project indicated that 75-88% of the clients rated the services provided at the 37 cluster clinics as 'excellent'; an additional 21-25% rated them as 'good.' More than 85% of the clients indicated either that 'nothing should be changed' (59%) or that 'everything was fine' (26%). These ratings and content analysis of the interview data revealed that the clients perceived they had received quality services at these cluster clinics. The authors also discuss six characteristics that they believed contributed to the successful delivery of health care and education through cluster clinics. These characteristics include: (1) provision of both direct and referral services for this underserved population; (2) comprehensive delivery of services in a single setting; (3) collaborative delivery of services; (4) access-driven delivery of services; (5) delivery of culturally-sensitive and linguistically-appropriate services; and (6) evidence-based service delivery.
Conclusions: Cluster clinics are an effective way to improve health-care services, education, and counseling for the under-served or unserved Hispanic migrant population diagnosed with diabetes. The authors conclude with four primary challenges to the implementation of these cluster clinics which include: (1) locating and preparing facilities; (2) recruiting health-care providers for the clinics; (3) achieving effective, appropriate communication with clients; and (4) securing funding.
Key words: cluster clinics, diabetes, Hispanic, migrant farmworkers


