Introduction
The many benefits of breastfeeding continue to be reinforced by new research1-3. Breastfeeding is a major public health issue, with rates of breastfeeding being a well accepted indicator of wellbeing for mothers and babies2.
In general, living in a rural or remote area translates to limited access to supportive facilities. For childbearing women in rural Australia the provision of maternity services continues to be hampered by shortages of GP obstetricians and midwives4 and closures of smaller maternity units (120 units having closed in the past 10 years)5.
Australian breastfeeding data collections do not always differentiate between rural and urban place of residence. Recently the New South Wales Health Survey of 2001 found combined exclusive or partial breastfeeding rates among rural women of 58% at 4 months and 49% at 6 months6. Rates of 'any breastfeeding' from national and state surveys in 1995 at 3 months were 63% nationally and 62% for South Australia. At 6 months both were 46%7. In 2001, national data only were available and showed little variation for Australia-wide rates (65% at 3 months and 48% at 6 months)8.
It is during the first weeks while lactation is being established that most women stop breastfeeding3. Studies world-wide confirm that insufficient milk and its associated supply concerns is the most commonly highlighted reason for stopping breastfeeding3,8 although most women who stop early do so because of perceived problems rather than by choice9. Other reasons are associated with an unsettled baby; finding breastfeeding more demanding than expected; painful or cracked nipples and mastitis9-11. Family and partner support for breastfeeding also plays an important role9. In an Australian study of 1559 women from mixed city and rural locations, breastfeeding at discharge was significantly associated with partner support for breastfeeding and breastfeeding intention10. The benefit of peer support in increasing uptake and duration of breastfeeding is now well established from randomised trials in both developing12 and developed countries13.
This study formed the breastfeeding component of a larger 44 question postnatal needs assessment that utilised a sample of birthing women who reside in the Lower Eyre Peninsula of South Australia, undertaken at a time when primary healthcare models were being promoted and introduced14. The study did not differentiate between partial or exclusive breastfeeding. The study objectives were to:
- collect rates of any breastfeeding at 6 weeks, 3 months and 6 months postpartum
- seek women's postnatal breastfeeding needs and how they were met.
Study site and population
Two community hospitals serve this coastal and agricultural area that is approximately 7-9 hours' drive from Adelaide, the capital city. Sixteen towns in the area have populations that range from 40 to 2500 (total population 4219)15. Most study participants had planned to give birth in one of the two local hospitals staffed by nurses, midwives and GP obstetricians. Both hospitals had fewer than 50 births during 2002 (hospital A, n = 27; hospital B, n = 14) while the nearest regional hospital had 240 births16. A small proportion of the women had either booked or been transferred to the regional hospital, usually for an emergency Caesarean section, although Caesareans could also be performed on site by a visiting general surgeon. Others had transferred to the capital city hospitals during pregnancy.
Since this survey was conducted, hospital B no longer provides maternity services because they are without a practising GP obstetrician.
Method
A structured questionnaire with provision for additional open-ended responses to the main questions was developed to ascertain whether women had needed support or information on common issues related to breastfeeding and whether, how well and by whom that need was met in hospital and at home. For example, a woman may have approached a healthcare professional (midwife, nurse or doctor), a self-help group such as the Australian Breastfeeding Association (formerly Nursing Mothers Association of Australia) or a family member such as partner, mother or mother-in-law, sister or friend. In the first instance, the 22 question breastfeeding component of the questionnaire was piloted with four recent mothers and an experienced lactation consultant; minor modifications were made. Breastfeeding domains included the need for support to establish and maintain breastfeeding, attachment, engorgement, mastitis and whether breastfeeding in public had been an issue. The final interview questionnaire, which took approximately 10 min to complete, was introduced to 10 women (n = 5 face-to-face and n = 5 by telephone) and found to be clearly understood and acceptable to them with no further adjustments required.
Epi-Info (CDC, Atlanta, GA, USA), a public domain database and statistics system for epidemiology, was used to develop a database. Double data entry was undertaken to reduce the risk of transcription errors. The sample was described using frequency tables and means, as required. For the open-ended questions, themes were established by discussion and consensus with two midwife colleagues. Occasionally direct quotes have been used.
In the absence of a local research and ethics committee, the research proposal was submitted to the Queen Elizabeth Hospital Research and Ethics committee in Adelaide and approval obtained to proceed as follows. In early 2003, consent was obtained by the chief executive officer and directors of nursing (DONs) of hospitals A and B for the health service employed researcher (GS) to conduct the research to obtain names, addresses and telephone numbers of women who had given birth there or who had been transferred elsewhere during 2002. These women were then sent a letter by the DON explaining the study and providing an opportunity to decline a follow-up phone call from the researcher. The letter acted as a written information sheet for the study. As no refusals had been received after 3 weeks, the researcher telephoned each woman to discuss the study and offer a further opportunity to decline, and finally to invite her to participate. Oral consent was obtained during the telephone call and a time arranged for either a telephone interview (n = 41) or a face-to-face interview in the woman's home (n = 17). There were no refusals.
The flow chart demonstrates the recruitment process (Fig 1). Women were recruited who had given birth at either hospital A (n = 25) or B (n = 13), or who had been transferred to the regional hospital or a city hospital (n = 15). Three had moved without forwarding addresses. Others who had booked at the regional hospital were referred by their GP to the study (n = 6). Approximately 15 eligible women who resided within the Lower Eyre Health Service area who had given birth at the regional hospital were unable to be contacted within the study time frame (Fig 1). The final sample of 59 women resulted in 76.6% of an estimated 77 eligible women resident in the Lower Eyre Health Service area who gave birth during 2002.
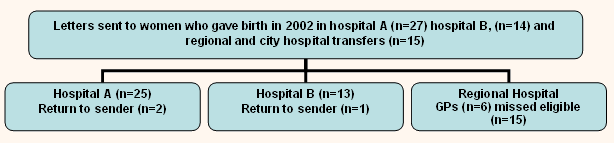
Figure 1: Flow chart of recruitment process: total sample n = 59.
Results
All but one of the participants initiated breastfeeding (98%) and these 58 women constitute the study sample. Age and parity are presented (Table 1). Ages ranged from 20-41 years (mean 32.3, mode 32) and for 18 women (31.5%) this was their first baby. The highest concentration was among multiparous women in the 30-34 year age group (n = 20, 34.5%). The mean age of babies at the time of survey was 8 months. Mode of birth is shown (Table 2). There were 24 (41%) women who had shared care with their GP and a midwife and 33 (56%) who had GP-only care. Others had combined GP and specialist care.
Table 1: Age and parity of women who commenced breastfeeding
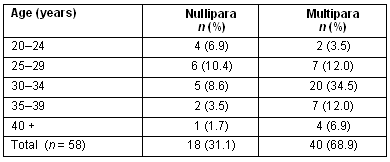
Table 2: Mode of birth whole sample

Breastfeeding rates are highlighted and where available, state and national figures are included for comparison (Table 3). At 6 weeks, 43 women (74%) were still breastfeeding. State and national figures are not available at 6 weeks but the study rate was comparable with 73% from an earlier South Australian study11. At 3 months the study breastfeeding rates compared poorly with state and national figures (55% vs 62% and 63%, respectively). At 6 months the figures were comparable (50% vs 46%, Table 3).
Table 3: Partially and exclusively breastfeeding at 2 weeks, 6 weeks, 3 months and 6 months local, state and national figures
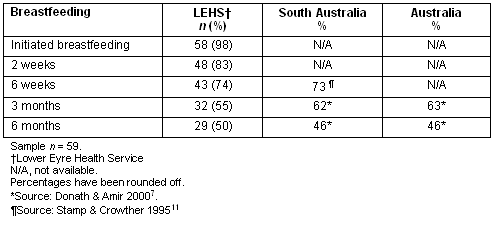
Table 4 shows reasons given for stopping breastfeeding. Individual responses indicate the attempts by many women to initiate and maintain breastfeeding. Further elucidation of reasons, under the heading 'too hard', are found in the direct quotes below:
The baby was not gaining weight and I felt pressure
Too frequent feeding was exhausting along with problems with supply
I tried for a week then put him on the bottle
The baby got sick and refused the breast, it was very stressful
I tried - it was too hard, the baby wouldn't attach
It's easier on the bottle
I'd had enough
Table 4: Reasons for stopping breastfeeding

Four out of the 9 women who had mastitis were among those who abandoned breastfeeding, giving mastitis as a reason.
Table 5 summarises women's breastfeeding support needs on the eight domains; how well these needs were met; and the sources of support. Midwives were the main source of support, particularly in hospital for the establishment of breastfeeding and attachment of the baby to the breast.
Table 5: Breastfeeding support needs in hospital and at home
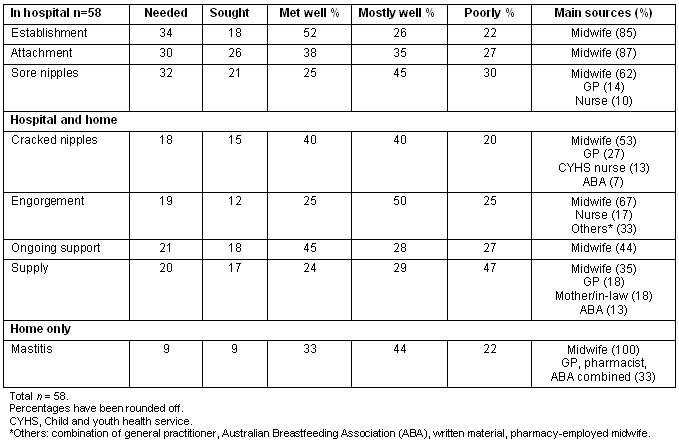
At home, the hospital midwives and GPs were the main sources of support, while the practice of bringing the baby to the hospital to see the midwife was quite common. Smaller numbers contacted the Australian Breastfeeding Association, the child and youth health service nurse; a midwife and breastfeeding counsellor employed by a local pharmacist and family members such as mothers and mothers-in-law or, very occasionally, sisters and sisters-in-law.
The following are examples of comments from women who had supply issues:
My supply went at 2 months - he was refusing a lot
My mum said the baby was similar to me. I lost confidence in the supply and put him on the bottle at 2 months
Each time I let down I tensed up, the baby lost weight - she gained on the bottle [a woman who stopped breastfeeding at 2 weeks].
In all areas except mastitis, fewer women with an identified need actually sought support (total 136 of 183, 74%). When women did seek support, their needs overall were met well (35%), mostly well (37%), or poorly (28%).
Thirty-eight (66%) of the breastfeeding women had a need to breastfeed in public, of whom 35 (92%) believed this need was not well supported within the community. The regional town (used for shopping regularly for items unavailable locally) was consistently nominated as having either poor or no facilities for breastfeeding or changing babies' nappies. Fourteen made additional comments such as:
We travel a long way to shop in [regional town] and have to feed and change the baby in a hot car
It's very poor, I need to shop there twice a week. There are no facilities and a total lack of understanding of the needs of breastfeeding mothers
There are excellent places available in Adelaide [capital city] but all my breastfeeding friends agree, it's impossible, facilities in [regional town] are practically non-existent.
A high level of conflicting advice from health professionals was experienced by 22 women (38%) and a moderate level by 13 women (22%).
After discharge, 52 (90%) would have welcomed a visit from a community midwife had it been available.
In response to questions about the level of partner and extended family support, 45 women (76%) had a very supportive and helpful partner; 37 women (64%) had a very supportive and helpful extended family, and a further 19 women (33%) had poor or unavailable family support. Only two women did not have a partner.
Comments were made that related to the importance of older women, particularly grandmothers and others, in postnatal support, and a need for such input.
Discussion
The study sample provided good representation of women who planned to give birth locally by age, mode of birth and parity (Tables 1,2). However, because this study consisted of a small sample within a limited geographical location, care must be taken in generalising these results to other rural regions with a different structure for maternity care. A further study limitation was the lack of distinction between exclusive and partial breastfeeding, particularly because exclusive breastfeeding until 6 months is now recommended by the NHMRC17. Any follow-up studies should make this distinction clear and investigate the extent to which the NHMRC guideline is being implemented17. Other possible limitations were that private health cover, often used as a surrogate for socio-economic status was not collected, and that the study size precluded comparisons between the experience of primiparous and multiparous women.
The top five reasons for stopping breastfeeding in this study (loss of supply; too hard; mastitis; lack of confidence in supply; and sore or cracked nipples) are consistent with findings from Australian and reviews of international studies3,9,11. Indeed, perceived insufficient milk is so commonly cited throughout the literature that it has been suggested that this may be a universal way of expressing lack of confidence in breastfeeding by mothers18. Individual quotes from mothers in this study indicate some of the difficulties and stresses involved in their breastfeeding experiences.
In hospital, the midwife provided most of the support for components that contribute to breastfeeding success. Although the breastfeeding support given was mostly well regarded, when the eight breastfeeding domains were combined, one in four women with needs did not seek support. Larger surveys in a range of settings have shown that women often do not seek help when needed for issues related to their postnatal recovery18. In addition, this study confirmed what is already known: that inconsistent or conflicting advice from health professionals is common9. It was clear that many women worked hard to maintain their lactation but there were gaps in the availability of support for breastfeeding and associated problems after discharge from hospital. Access to accurate non-judgemental support is an important element of breastfeeding success, and is much desired by women19.
Implications of this research
In Western society, public environments such as shops and restaurants can be unsupportive of breastfeeding. A South Australian telephone survey suggested there was little support for breastfeeding outside the home20. Discomfort and embarrassment about breast exposure can contribute to reasons why women choose not to breastfeed or abandon it early3. This study highlighted the lack of facilities for changing the nappies of babies and support for breastfeeding, particular in the regional town, and is a possible area for community action.
The one third of women with poor or unavailable extended family support may benefit from supportive interventions. Low breastfeeding rates and an interest in the role of senior women in providing breastfeeding support highlighted by this study led to the introduction of the Elderberries program. The Elderberries model draws on the wisdom and experience of senior community women who volunteer to work in partnership with the community midwife and local hospital midwives21.
At the time of the study, the two rural hospitals did not have a breastfeeding policy. Appropriate practice standards such as the 10 steps to successful breastfeeding highlighted in the Baby Friendly Hospital Initiative exist22, with six of the steps having a high level of implementation Australia-wide23. The hospitals now have a breastfeeding policy and it has become mandatory that all nursing staff attend training sessions, as well as the Elderberries24. If the Elderberry model is successfully integrated into the community and acceptable to new mothers and their families, the essential components could form the basis of a cluster randomised trial to test its effectiveness in increasing breastfeeding rates for a wider population of Australian rural women.
Acknowledgements
The authors acknowledge and thank all the women who shared their experiences of breastfeeding, the mothers who helped pilot the questionnaire and the directors of nursing for their support for the study. Special thanks also to Deb Sykes who discussed ideas and provided support during the study, Karen Tiller who helped develop and pilot the questionnaire and Christine Franks and Flick Wright who provided comments on the manuscript. Finally, thanks to the anonymous reviewers who provided insights and comments that have led to clarification, additions and changes of emphasis that have strengthened the article.
References
1. Howie PW, Forsyth JS, Ogston SA, Clarke A, Florey CD. Protective effect of breast feeding against infection. British Medical Journal 1990; 300: 11-16.
2. McVeigh P. Is breastfeeding best practice? Medical Journal of Australia 2002; 177: 128-129.
3. Fairbank L, O'Meara S, Renfrew MJ, Woolridge M, Sowden AJ, Lister-Sharp D. A systematic review to evaluate the effectiveness of interventions to promote the initiation of breastfeeding. Health Technology Assessment 2000; 4(25): 1-171.
4. National Health and Medical Research Council. Options for Effective Care in Childbirth. Canberra: AGPS, 1996.
5. Rural Doctors Association of Australia. Rural birthing services discussed with senior policy makers. RDAA News 2005; 4(2): 5. (Editorial)
6. Hector D, Webb K, Lymer S. Describing breastfeeding practices in New South Wales using data from the NSW Child Health Survey, 2001. NSW Public Health Bulletin 2002; 16(3-4): 47-51.
7. Donath S, Amir L. Rates of breastfeeding in Australia by state and socio-economic status: evidence from the 1995 National Health Survey. Journal of Paediatric and Child Health 2000; 36: 164-168.
8. Australian Bureau of Statistics 2001. Breastfeeding in Australia, 2001. (Online) 2003. Available: http://www.abs.gov.au/Ausstats/abs@.nsf/525a1b9402141235ca25682000146abc/8e65d6253e10f802ca256da40003a07c!OpenDocument#2.%20BREASTFEEDING%20PRACTICES%20IN%20AUS (Accessed 4 May 2006).
9. Dennis C-L. Breastfeeding initiation and duration: A 1990-2000 literature review. Journal of Obstetric Gynecologic and Neonatal Nursing 2002; 31: 12-32.
10. Scott JA, Landers MCG, Hughes RM, Binns CW. Factors associated with breastfeeding at discharge and duration of breastfeeding. Journal of Paediatric and Child Health 2001; 37: 254-261.
11. Stamp GE, Crowther CA. Breastfeeding, Why start? Why stop? A prospective survey of South Australian women. Breastfeeding Review 1995; 3: 15-19.
12. Haider R, Ashworth A, Kabir I, Huttly SR. Effect of community-based peer counsellors on exclusive breastfeeding practices in Dhaka, Bangladesh: a randomised controlled trial. Lancet 2000; 356(9242): 1643-1647.
13. Dennis CL. Hodnett E, Gallop, Chalmers B. The effect of peer support on breast-feeding duration among primiparous women: a randomised controlled trial. Canadian Medical Association Journal 2002; 166: 42-43.
14. Government of South Australia. Better choices, better health. Final Report of the South Australian Generational Health Review. Adelaide: Government of South Australia, 2003.
15. Australian Bureau of Statistics. Census of Population and Housing 2001, Usual Residence Profile. Canberra: AGPS, 2002.
16. Chan A, Scott J, Anh-Minh N, Kean R. Pregnancy Outcome in South Australia. Adelaide, SA: Pregnancy Outcome Unit, Department of Human Services, 2003.
17. National Health and Medical Research Council. Dietary guidelines for children and adolescents in Australia - incorporating the infant feeding guidelines for health workers. Canberra: AGPS, 2003.
18. Amir LH, Cwikel J. Why do women stop breastfeeding? A closer look at 'not enough milk' among Israeli women in the Negev Region. Breastfeeding Review 2005; 13(3): 7-13.
19. Graffy G, Taylor J. What information, advice and support do women want with breastfeeding? Birth 2005, 32: 179-174.
20. McIntyre E, Hiller JE, Turnbull D. Community attitudes to infant feeding. Breastfeeding Review 2001; 9: 27-33.
21. Lower Eyre Health Services. Elderberries: Supporting Mothers to strengthen each other and enhance families' parenting capacity in our community. Adelaide SA: Lower Eyre Health Services, Australian Government Department of Health and Ageing, 2005.
22. BFHI. Baby friendly hospital initiative, protecting, promoting and supporting breastfeeding in Australia. (Online) 2005. Available: http://www.bfhi.org.au (Accessed 10 March 2006).
23. Walsh AD, Pincombe J, Stamp GE. The ten steps to successful breastfeeding in Australian hospitals. Breastfeeding Review 2006; 14: 25-31.
24. McIntyre E, Byrne J. Breastfeeding management in a baby friendly hospital: an 8 hour structured course for health professionals working with mothers and babies in maternity units, 3rd edition. Australian Lactation Courses.

