Context and issues
The rollout of individualised funding in Australia under the National Disability Insurance Scheme (NDIS) will enable increased funding for disability services Australia-wide, including regional and remote areas. The provision of allied health and community support services seeks to increase participation and improve daily living of all individuals living with a disability. Geographical distance, however, is a known barrier in the equitable access of disability and health services in more remote locations. A recent rural carer survey by Gallego et al found that issues of long waiting lists, extensive travel times and lack of choice of specialist disability services were frequently reported1. Many of these barriers stem from staff recruitment and retention issues in the remote area health sector, which have been highlighted in the literature2,3.
The 2017 State of the disability sector report, delivered by National Disability Services, indicates that 73% of service providers under the NDIS reported increased demand for their services over the previous year4. Less than half (43%) expected to be able to satisfy future demand. In the latest report in 2018, it was reported that allied health, and more specifically psychologists, were the most difficult staff to attract and retain to the sector5. NDIS reported that these difficulties are exacerbated in regional and remote areas of Australia5.
Autism spectrum disorder is currently the most prevalent primary diagnosis of children aged 0–14 years entering the scheme6 and intervention often requires specialised programs of support delivered by experienced staff7. Technology has the potential to provide a timely, low-cost alternative that extends access to autism-specialist services for people in remote locations. Technology-delivered intervention, also known as tele-health or tele-practice, is a growing field with eight studies recorded prior to 20108, and an additional 14 studies conducted up until 20189. Studies in the Australian disability sector, including the delivery of speech pathology10,11 and adult autism assessment12, have reported positive outcomes. However, barriers exist with technology difficulties10,11, building rapport11 and limitations based on clients’ severity of disorder10. Parmanto et al reported lower scores for general acceptability of telehealth as a replacement for in-person services12. Sutherland et al have suggested a need to further 'investigate facilitators and barriers to the use of telehealth with clinicians, parents and individuals on the autism spectrum’ (p. 334)9. When designing tele-practice services, Abimbola et al recommended that organisations consider using a multi-stakeholder approach in its evaluation13.
Aims of the evaluation
The project was funded by the National Disability Services under Innovative Workforce Funding and aimed to identify feasibility, essential requirements and potential barriers in delivering therapy support to regional and remote participants on the autism spectrum via video-conferencing technology. The evaluation areas of the current project included:
- development of a competent tele-therapy support team to deliver high quality collaborative tele-therapy service for participants in regional and remote areas
- understanding the role of collaboration and capacity building within a tele-therapy service
- examining the need for autism-specific services in regional and remote areas
- examining the need for in-person contact as part of a tele-therapy program
- identifying barriers in the success of a tele-therapy model of disability support.
Participants
A multidisciplinary team including a speech pathologist, occupational therapist, psychologist and a special educator were recruited via an expression of interest from the project lead within an autism-specific, not-for-profit organisation. All successful therapists had a minimum of 2 years experience in delivering autism support, and no prior experience in delivering autism support via tele-therapy. Tele-therapists were trained by the project lead via group webinar and individual online consultation to deliver tele-therapy services. Child participants were recruited via an expression of interest email sent to the service waitlist of the not-for-profit organisation. Parents gave written consent for themselves and their child(ren) to participate. A total of 16 children on the autism spectrum (median age 8 years, range 2–12 years) and their families participated in the program. Participants and their families resided in 13 separate regional communities across northern, western and southern New South Wales (NSW). Local support teams including educators and allied health staff were recruited via an information statement emailed to them by children’s parents. Consent forms were returned to the project lead. Local support team members (educators and allied health professionals) were recruited in all three regional areas of NSW. Figure 1 shows the geographical spread of tele-therapists and participants in NSW.
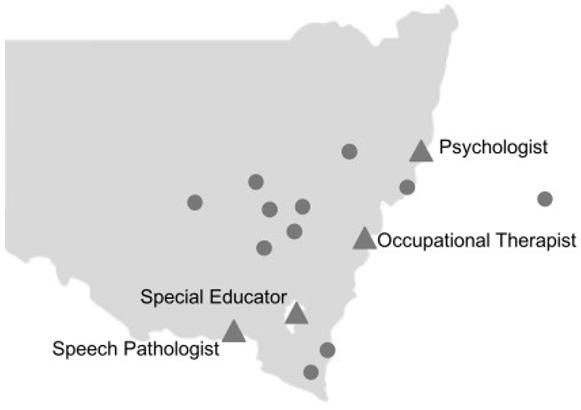 Figure 1: Regional location of tele-therapists (triangles) and participants (circles).
Figure 1: Regional location of tele-therapists (triangles) and participants (circles).
Intervention
The tele-therapy service was conducted using off-the-shelf video-conferencing software (Zoom) and started with an initial online session to gather information to inform an individual support plan and identify therapy goals. Six tele-therapy sessions were then conducted at a time and place (home, preschool, or school) that suited both the tele-therapist and the family and/or school and the participant.
A total of 30 goals were identified in the participant cohort from a broad range of areas, including self-care, early play skills, positive behaviour support, emotion and sensory regulation skills, independence in daily routines, and social skills training. Other goals were focused on increasing parent and teacher understanding of autism and confidence in supporting the child/participant. Tele-therapists worked under a comprehensive approach to therapeutic intervention and strategies of support were individualised to each participant, with a focus on evidence-based practice.
Data collection
Researchers used semi-structured telephone interviews to gain insight into the program from key stakeholder groups including parents, education staff, allied health professionals and the multidisciplinary team of tele-therapists. The duration of each interview was 10–25 minutes and questions covered experiences when using the video-conferencing software, reported differences between tele-therapy and in-person services (if applicable), collaboration with the child’s local support team, and general comments and feedback on the tele-therapy service. Interviews were conducted by the first author, who was independent from project delivery.
Data analysis
A total of 21 interviews were conducted in the current study, which consisted of eleven parents, six local support team members (three educators, two learning support coordinators, and one speech pathologist) and four tele-therapists. Data saturation was met when there were no new data emerging under each of the project areas14. Interviews were recorded and transcribed verbatim and entered into qualitative data analysis software NVivo v11. Researchers used a general inductive approach to analyse the data15 as this method is useful when analysing data under specific research objectives. This process involved initial line-by-line reading of text data to identify segments related to the five project evaluation areas. Next, the authors coded segments of text under each area into categories, then reduced overlap and redundancy amongst the categories. Finally, the authors created a model of the most important categories. These are presented as key findings under each project area in the next section.
Ethics approval
The study was approved by the Aspect Research Approvals Committee on 14 July 2017.
Lessons learned
The project focused on five different areas: development of the tele-health delivery team, understanding the role of collaboration, examining the need for autism-specific support, establishing the need for in-person contact and identifying barriers to success.
Development of a competent tele-health support team to deliver high quality collaborative tele-health services for participants in regional and remote areas
Need for training and practice changed: At the beginning of the project, it was observed that a significant number of hours were needed in administration, training and collaboration time between tele-therapists and the project lead. These hours were not included in the service delivery hours of the tele-therapy project. This was of major concern at the time due to the lack of billable hours and sustainability of the program. At the time this had significant implications on the design of the role and the risk of job dissatisfaction.
Towards the end of the project it was observed that administration hours significantly reduced as tele-therapists became more confident in using the technology and finding ways to work smarter with families. By the end of the project, administration hours were within the typical amount for an in-person service. This was reflected in the data, with three of the tele-therapists reporting that training, preparation and practice were vital in building confidence in delivering the tele-therapy service.
So, you need to give yourself enough time at the beginning to be really comfortable with the logging on … But if you just presume that it’s going to be easy, you let yourself down and then you let the clients [participants] down. (Tele-therapist)
Understanding the role of collaboration and capacity building within a tele-therapy service
Collaboration was valued by stakeholders: An important category of data to emerge was that families and local support team members valued being included in the tele-therapy sessions as they could learn more about supporting their child/the participant and had access to autism specialists.
Everyone sort of could get on the same page and understand why things were happening and we didn’t feel like we were banging our heads against a brick wall. (Primary school teacher)
It’s helped me to know where school’s up to and what they’re doing, it’s helped school to know where we’re at with therapy … [the tele-therapist] was able to contribute and make suggestions and put some strategies in place to help with different issues. (Parent)
Examining the need for autism-specific services in regional and remote areas
Filling the gap: A category of the data emerged which established a need for autism-specific services in regional and remote regions of New South Wales. Local support team members reported that having access to autism-specialists was a major benefit of the program – especially in regional, and remote areas, where this specialist knowledge and experience was limited.
The main difference is that we had someone who was an expert … Because we’re so isolated, to get someone with that expertise to come out here is quite rare, … so we’ve never really had someone with that expertise come into the classroom. (Primary teacher)
We’re reaching out to families that don’t have many other services and haven’t worked with someone who’s worked with autism in as much detail before … the families just being like, ‘Oh, wow. You get it!’ Because these families haven’t received autism services before. (Tele-therapist)
Establishing the need for in-person contact as part of a tele-therapy program
Similarity to in-person sessions: Mixed responses emerged from the data on the differences between in-person support and tele-therapy. Several respondents indicated that seeing the tele-therapist over the internet was similar to being in the room with them. Some responses indicated it was even better than being in-person as their child could engage on a deeper level.
Look, I found it very personable, it wasn’t like it was any different really than being in the same room with someone. (Parent)
When he started to swing around on his chair, he realised that I couldn’t see him, so he centred himself and just concentrated face to face [in-person] on what we were talking about. (Tele-therapist)
Additional in-person sessions may increase rapport: Some parents, however, as well as some tele-therapists and educators, advised that the addition of in-person services would help in establishing and developing rapport with the participant.
I did feel the difference. I think the quality of the face to face [in-person] dimension, there is a noticeable difference in information gathering. And the rapport was a lot easier to establish face to face. (Tele-therapist)
I would prefer to sit down with a person one on one and face to face [in-person] in a room. I think people really get a lot of benefit from that. (Learning support coordinator)
This was consistent with the findings of Fairweather et al11; however, participants in the current study were also realistic about the accessibility of in-person services in regional and remote regions. The implications of this finding suggest a need to investigate a blended model of online and in-person services and the optimal ratios for success.
But in saying that, when you’re in remote areas, you just don’t have access to these specialists. So, if we can do it by our technology, and that is our only option, then it is better than nothing. (Learning support coordinator)
Identifying barriers to the success of a tele-therapy model of disability support
Limitation on goals requiring physical interaction: Parmanto et al12 reported low acceptability of tele-health as a replacement for in-person services; however, it may be necessary when no other comparable local service option is available. A series of limitations for tele-therapy were anticipated and outlined as part of the intake process to families and service providers. They include medical intervention, including prescription of medications and management of chronic disease; psychiatric treatment; and assistive equipment, including fitting of wheelchairs, scooters, walkers, canes, crutches, prosthetic devices and orthotic devices, to enhance mobility. In addition, the study found that fine and gross motor goals, where physical interaction was required by a trained occupational therapist, were also reported to be limited by the online platform. Therapists felt more restricted and less successful in being able to address these goals, which they would normally be able to do at in-person therapy. The implications of such a finding is that there will be limitations on delivery of the full breadth of occupational therapy supports via tele-therapy.
Obviously, you’re not there, so there’s not the same sort of physical interactions. So if you were doing something like speech or OT [occupational therapy] or something like that and you really needed to help position something or do something like that. Obviously, that is not possible via the same platform. (Parent)
I was using more of a building capacity type model … as my work as an OT [occupational therapist], a lot of it is a lot more hands on, and looking at things like handwriting, or play skills, you do need that physical contact with the client [participant]. (Tele-therapist)
Scheduling and local staff changes as barriers: While collaboration was a key target of the current program, several barriers were cited by parents, such as scheduling and local support staffing changes, that impacted on the ability of the tele-therapist to collaborate with the child’s team. These results are consistent with findings on the retention difficulties experienced in regional and remote areas2,3. These barriers, however, may have been experienced regardless of the mode of delivery.
I was telling them [educators] about some of the programs that we’ve been working on, and they pretty much just said, ‘Well, we’ve got our own, and that’s what we do’. (Parent)
I think we tried to involve his school, but I think that his teacher also signed up for two other things at the same time. (Parent)
Interestingly, and unlike previous studies10,11, difficulties with technology was not reported as a barrier in the delivery of tele-therapy services. As technology continues to improve, and the use of high quality, off-the-shelf platforms such as Zoom become more consistent, it is hoped that technology will no longer serve as a barrier in the effective delivery of tele-health services in regional and remote areas.
Although the sample size was adequate in meeting data saturation, a limitation of this study is that the authors may not have captured adequate data from regional and remote allied health professionals to understand the impact of tele-therapy in their local community and job role. Also, the small sample is restricted to regional and remote areas of NSW, and therefore may limit generalisation to other areas of Australia.
Conclusions
This research adds to the growing body of information supporting the use of tele-practice for geographically isolated regions. Interviews with all involved in the tele-therapy pilot indicated that online services are filling a gap in regional and remote autism-specific service provision. The service was reported to increase collaboration and access to specialists. Larger scale research is needed to investigate a blended model of service delivery so that an optimal ratio of online and in-person support can be established. There is a need for further research to investigate innovative ways in which allied health services that require physical interaction can be effectively delivered via tele-therapy. Overall, the project indicates that the delivery of allied health disability services to individuals on the spectrum is a feasible and acceptable platform for autism-related support.
Acknowledgements
The authors acknowledge all participants in the project, including individuals on the autism spectrum, their families and local support networks, as well as the tele-therapists. They also acknowledge the support provided in the form of an Innovative Workforce Fund grant, administered by National Disability Services with funding from the Australian Government Department of Social Services.
References
You might also be interested in:
2006 - Home medication reviews: what do people in the Australian Riverland think of them?
