Introduction
Australia, like many countries around the world, has a significant maldistribution of medical practitioners in favour of metropolitan areas, with significant shortages in non-metropolitan areas. Studies have demonstrated that the decision to enter rural practice is associated with both rural background and rural practice exposure during undergraduate training1-3. During the 1990s, successive Australian governments introduced a variety of policies and incentives aimed at increasing the non-metropolitan medical workforce4. One of these was a requirement that all existing medical schools incorporate dedicated teaching about rural health into their curricula. Another was to fund rural clinical schools attached to existing medical schools; all of which at that time were in capital cities with one exception. More recently, there has been a trend in the early years of this century towards the establishment of regional medical schools (eg, in Australia, Canada and the UK).
In Australia, this has been in response to the Federal Government increasing the number of medical school places. This provided an opportunity for some universities to seek funding to establish new medical schools. The School of Medicine at James Cook University (JCU) in north Queensland was the first new medical school to be opened in Australia in over a quarter of a century and enrolled its first cohort of students in 2000. It was also the only Australian medical school located in a truly regional setting (Townsville's population is 160 000 and it is more than 1000 km north of Brisbane, the capital of Queensland). The school was established with the aim of increasing the number of medical graduates who understand rural, remote, Indigenous and tropical health issues. A number of strategies underpin the aim, including: training local rural background students; utilizing suitable curriculum design; providing career opportunities locally; and providing postgraduate training locally5. The course involves a 6 year integrated curriculum which exposes students early and regularly to rural practice. Additionally, issues related to rural, Indigenous and tropical health are integrated into all elements of the curriculum, as well as being the focus of a dedicated subject in the second year5.
Sixty-four students entered the course in 2000. One of the authors (AU) was in that first cohort and was impressed by the diversity of life experiences and expectations of her colleagues. In 2001, AU undertook a survey to record an anthology of the life experiences of this first cohort as a research elective subject supervised by the principal author6. Towards the end of 2005, just before this cohort graduated, the authors conducted a short follow-up survey of students regarding location of their internship and their career intentions. Fifty-eight students graduated in December 2005. This article compares key findings from the two surveys.
Method
In each instance (August 2001 and October 2005), students were sent questionnaires seeking information on various issues. No identifying information, such as names and student numbers, was requested or recorded. The 2001 questionnaire sought basic demographic information (age, sex) as well as information on education history (location, previous university study), previous career, occupation of both parents, geographical background (place of birth, 'home' in 5 years prior to entering medicine), reasons for choosing medicine and JCU's course, and career aspirations (discipline, location of practice)6. The 2001 study also included an interview component which focused primarily on participants' life and work experiences prior to entering medical school. The 2005 questionnaire used the same questions as in 2001 about career aspirations and reflection on career intentions at entry and at exit, plus location of internship. The same demographic information was also sought (sex; age at time of entry) in order to assess representativeness of each respondent group compared with the entire cohort at each time, and also between the two surveys.
Between 2001 and 2005, some students left the cohort (left the course, or repeated an earlier year of the course), while some joined as accelerated entries (4 in 2001 and 1 in 2002). No attempt was made to identify and exclude the responses from these students. Ethical clearance was obtained from the James Cook University Human Ethics Committee for each study (H1235 and H2175).
Results
The slight change in gender composition of the group over time is demonstrated (Table 1). More males have left the cohort - generally through repeating earlier years - whereas females have left the course entirely. Similar numbers of males (3) and females (2) have entered under accelerated entry.
Table 1: Characteristics of first cohort - 2001 and 2005
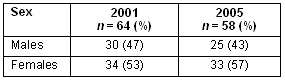
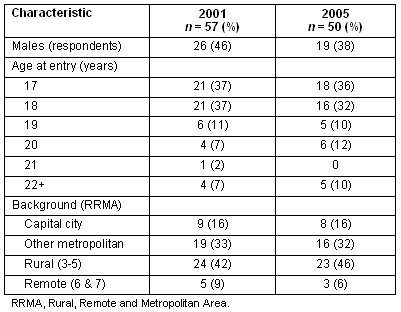
In 2001, 57 (89%) of the 64 students returned completed questionnaires while, in 2005, 50 of 58 (86%) responded. A slightly lower proportion of males responded in 2005 than in 2001 (Table 2). The slight change in the group's composition is also demonstrated in terms of reported age at entry and self-reported 'background'. Those who entered the course in years two and three were older at entry, because they had undertaken other tertiary courses.
Table 2: Characteristics of survey respondents - 2001 and 2005
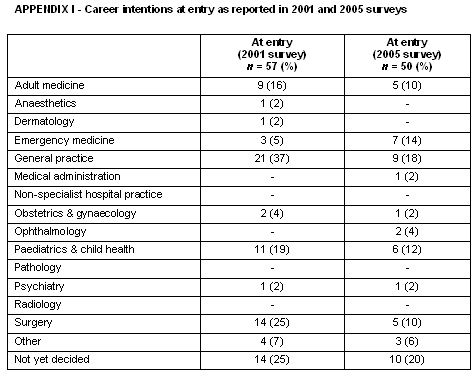
In 2001, students were asked to nominate their career aspirations (at 2001). In 2005, students were asked to nominate their career aspirations both at entry to the program (2000) and at exit (2005). Table 3 sets out the frequency of responses at entry (2001) and exit (2005).
Table 3: Career intentions at entry (2001) and exit (2005)
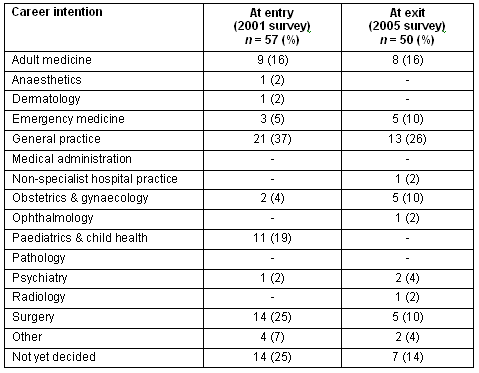
Of particular note is that the number of undecided students had halved, the numbers interested in general practice had reduced by one-third, the numbers still keen on surgery had reduced to one-third, and none were considering paediatrics at exit. Conversely, the number considering emergency medicine had almost doubled and more than doubled for obstetrics and gynaecology (O&G) since 2001.
In 2001, 66% of respondents indicated that they intended to work in rural areas, nearly the same as in 2005 (64%). In neither instance were participants asked to nominate whether they intended to work in regional, rural or remote practice. In 2001, 15 (23%) indicated that their intentions had changed since entry (2000). In 2005, 7 (14%) respondents indicated that their intentions had changed since entering the course: 6 (12%) to rural and 1 (2%) to urban - a student with a remote background who indicated that they were 'more inclined to work in a larger centre, because I want to be a specialist [O&G]'. The five now intending to 'go rural' came from regional cities and towns. One of these indicated that they had established a relationship with a rural partner.
Table 4 sets out students 'state of origin' when entering the course and the state in which students will be undertaking their internships in 2006. Forty-nine (98%) respondents indicated that they had received their first choice location for their internship.
Table 4: Home state (at entry) compared with state for internship
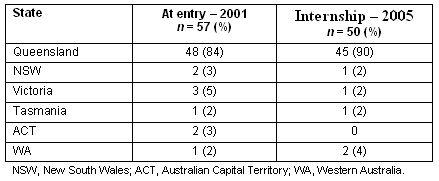
Of the 45 doing their internship in Queensland, 36% were moving to the metropolitan south-east (Brisbane, Gold Coast, Logan), while 56% were remaining in north Queensland (Townsville, Cairns, Mackay) with the remaining 8% in other rural towns (Rockhampton and Nambour).
Discussion
The original student-initiated survey was undertaken as part of a research elective and was not planned to be repeated. However, the authors recently decided that a brief follow-up survey of career intentions immediately prior to graduation presented a good opportunity to assess changes across time in this first cohort. Ideally, a follow-up survey should only include members of the original cohort, but this was not practicable in this instance because of the anonymous nature of both surveys. While some change in the demographic composition of the two respondent groups was evident (eg, age, gender and background), this was relatively minor. Thus, although there is some 'error' in the comparison of the two surveys' results, its impact is likely to be relatively minor and perhaps little different from that which might be expected in a follow-up survey of a well-defined cohort in which some members only participate in one survey or the other.
The comparison of the two studies highlights a number of interesting findings. First, given that the majority of intern positions in Queensland are in the metropolitan south-east of the state, it is pleasing to note that two-thirds of students have sought and taken posts elsewhere, predominantly in northern Queensland. It needs to be emphasized that 98% of respondents indicated that they had received their first choice intern location. In other words, they were not forced to take posts in north Queensland or other rural locations, they did so willingly. Indeed, there were many more intern places across Queensland than could be filled, so graduates could have conceivably applied to go wherever they most wanted. It also appears that there has been little if any leakage to other states, other than by those students who are returning to their home state. In both instances, these are heartening results.
Changes in career aspirations reflect two issues. First, a methodological one; respondents in both the 2001 and 2005 surveys were asked what their aspirations were at entry, so it was possible to compare these (Appendix I). Respondents' 2005 recollections of what their aspirations were in 2001 varied, which reinforces the value of the longitudinal process when assessing career aspiration change. The JCU School of Medicine intends to follow graduates at regular intervals throughout their careers and has recently undertaken the first (course exit) survey of this cohort. The school will also be participating in the Australia-wide tracking survey of all medical graduates being conducted by the Committee of Deans of Australian Medical Schools (CDAMS). The second issue relating to changes in career aspirations from entry to exit possibly reflects exposure to the various disciplines and perhaps also positive/negative experiences during clinical rotations in the final years of the course. For example, The Townsville Hospital (TTH) has dynamic, highly skilled emergency medicine physicians, many of whom have strong links with the defence forces as reservists, so that students not only learn and experience emergency medicine at the local level, but 'rub shoulders' with experienced emergency medicine physicians who have worked (either in the military or as volunteers) in recent disaster and war zones. Additionally, JCU's medical course incorporates greater exposure to emergency medicine than any other medical course in Australia or New Zealand, in order to better prepare graduates for rural practice. As a result, a number of the TTH emergency physicians are adjunct faculty within the school and have regular contact with the students throughout their course, including a very popular year 2 activity, hosted by the army, and centred on a fully moulaged, multiple vehicle crash and involving multiple casualties. It is probably also not surprising that students' intentions change across the duration of the course as their contact with and experience of specific disciplines increases. Whether graduates subsequently pursue their exit intentions, or their intentions again change as a result of their intern and residency experiences, will only be known in 5-10 years.
The consistency across time with respect to intention to practice in rural (more correctly non-metropolitan, as participants were not asked to nominate regional, rural or remote practice) areas reflects that most respondents had eyes on rural practice from early in the course. Indeed, in the 2001 survey, which sought qualitative information on why people chose the JCU course, 26 (40%) indicated that they had applied to JCU because it was 'close to home', while another 12 (19%) 'did not want to leave Townsville' and nine (14%) indicated that they were attracted by the rural focus of the course. These findings are in line with those in other studies that have demonstrated that two important factors in clinicians' decisions to take up non-metropolitan practice are: (i) non-metropolitan background and (ii) substantial and meaningful exposure to non-metropolitan practice during the course. The large number of this cohort who wanted to be in a regional course (with a stated emphasis on rural, Indigenous and tropical practice) is strong evidence in favour of the former. The consistency in intentions across time is equally strong evidence that exposure to non-metropolitan practice throughout the course has supported those students with intentions to practice outside metropolitan areas to realize their ambitions. Even those who have headed to south-east Queensland and other state capital cities will have a sound understanding of rural, Indigenous and tropical health issues which, in itself, means that rural and Indigenous people who have to attend major urban medical facilities will possibly receive care and attention which is considerate of the context from which they come7.
Conclusion
The much-awaited graduation of JCU's first cohort of medical students has provided a unique opportunity to monitor students' career aspirations and intentions across time. Clearly, the JCU School of Medicine program attracted a significant number of entrants from non-metropolitan areas and who had a commitment to non-metropolitan medical practice. The fact that the majority of graduates are undertaking their internships in non-metropolitan areas by choice, is evidence that students not only know what non-metropolitan practice entails, but that they feel prepared to face its challenges and rewards. That graduating students remain committed to non-metropolitan practice supports the school's contention and that of others around the world, that medical education undertaken in non-metropolitan settings, with a broad-based curriculum, is the best vehicle for increasing the rural medical workforce. It will be interesting to see where these graduates are in 5 and 10 years' time. This study provides support for the development of regional medical schools that focus on local recruitment and health-care need issues.
Acknowledgements
We wish to thank the students who participated in the two surveys. We also wish to acknowledge and thank Ms Tamara McCloskey who entered the data from the 2005 study. AU input the data from the 2001 study. Funding: This student-initiated project was funded internally using resources held by the Rural Health Research Unit and School of Medicine, James Cook University. No financial gain or loss to either entity is associated with the outcomes of the research. Contributors: Author 1 undertook analysis of the 2005 survey data, the comparative analysis of data from the two studies, sought ethics approval and wrote the substantial first draft this paper. Author 1 mentored author 2 during the 2001 survey. Author 2 undertook data collection, analysis and wrote the report of the 2001 study, which has been drawn upon in this paper. Author 3 provided financial and in-kind support for both surveys (postage, printing etc). Authors 2 and 3 contributed to additions and revisions of the original draft of this paper.
References
1. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
2. Laven GA, Beilby JJ, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
3. Worley PS, Prideaux DJ, Strasser RP, Silagy CA, Magarey JA. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000: 172: 615-617.
4. Humphreys JS, Hegney D, Lipscombe J, Gregory G, Chater B. Whither rural health? Reviewing a decade of progress in rural health. Australian Journal of Rural Health 2002; 10: 2-14.
5. Hays R. Rural initiatives at the James Cook University School of Medicine: a vertically integrated regional/rural/remote medical education provider. Australian Journal of Rural Health 2001; 9(suppl): S2-S5.
6. Underhill A. In the beginning: an anthology of the life experiences of the first intake of James Cook University School of Medicine students. Townsville: School of Medicine, James Cook University, 2001.
7. Veitch PC, Sheehan MC, Holmes JH, Doolan T, Wallace A. Barriers to the use of urban medical services by rural and remote area households. Australian Journal of Rural Health 1996; 4: 104-110.