Introduction
Rural Australia is experiencing an increase in individual and family distress and long-term needs arising from mental health issues in rural and remote communities1. The Healthy Horizons report and the Australian National Survey of Mental Health and Wellbeing, both of which were published in 1999, provided information about the nature and extent of mental health problems Australia-wide1,2. Almost one in five Australians over 18 years of age had experienced an anxiety, affective or substance use disorder in the 12 months prior to the survey.
In 1995, the Mental Health Council of Australia stated that there was the 'likelihood that every family in Australia will be affected by mental health problems at some stage' 3. The same report identified that in Queensland, although depression and suicide were nominated by government as two of the six target areas for major health gains, access to services for people with mental illness or mental problems were extremely limited.
People living in rural and remote areas in Queensland are disadvantaged, and many health issues and their determinants are likely to be exacerbated4. Past studies suggest that although there are some rural satellite facilities and outreach programs, there are limited psychological services in Australian rural communities3,5,6. Additionally, living in a remote area is associated with less use of psychological services7.
The researchers were commissioned to evaluate the extent of counselling and psychological services in five rural and remote communities located in South-west Queensland. Within those communities it was known that many of the current services were dependant upon 'soft' funding. Current providers of support offered their opinions on the need for additional services and the perceived impact of withdrawal of services should funding cease.
Methods
Definition of terms
Providers: Psychological service providers were not limited to psychologists but were defined as qualified and/or experienced persons who offered any form of counselling. People who met these criteria included psychologists, counsellors, mental health nurses, social workers, other health professionals who possessed a qualification in psychology, social science, nursing or behavioural science, and persons such as clergy with experience in counselling.
Psychological support: For the purposes of this study, psychological support was defined as being assessment and/or intervention on an individual or small-group basis by a recognised provider. Referrals and promotional or education activities by providers was not considered to be support. Support was divided into what was offered by 'mental health services' and 'general support' to differentiate what was offered to people who had a serious enough mental illness to be seen by the mental health service of Queensland Health and all other provision.
Ethical approval
The study received ethical approval from the University of Southern Queensland Human Research Ethics Committee.
Identification of participants
The towns: The five towns in South-west Queensland were chosen because they were rural centres and provided many services, including psychological services, to people in both towns and outlying areas. The towns were classified by the Australian Standard Geographical Classification system of remoteness classification8, as remote (Town A), outer regional (C and E) and inner regional (B and D). Town populations ranged between 4000 (A) and 10 000 (B), and total serviced population when outlying areas are included, was between 8000 (A) and 15 000 (E) (Table 1).
Table 1: Provision of services to communities from telephone directory listings of counselling and psychological services
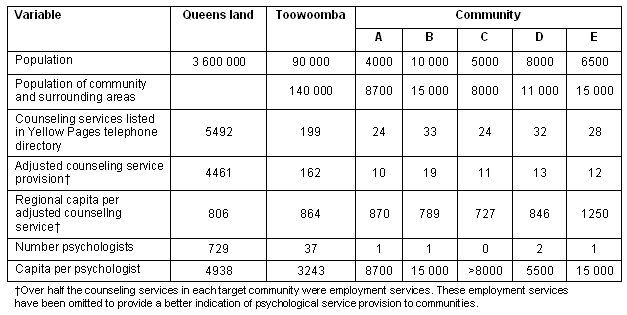
Service providers: Three primary sources were used to gather the initial information about psychological service providers in the targeted communities:
- Telstra Yellow Pages internet directory (http://www.yellowpages.com.au/) using all 18 categories of counselling services in the directory search engine
- Commonwealth Carelink directory of service providers searched by post code
- Internet search used first the Google? search engine and then expanded into an examination of national, state, and local directories for government and non-government organisations (NGO; eg Queensland Health health service district profiles).
Further information on providers in these communities was gained using a snowballing technique9 during initial contact with the providers identified through the primary sources. An already identified participant was asked to provide the names of other psychological service providers in the community. This continued until no new service providers were identified.
A total of 73 potential organisations or individuals providing services were identified. This was reduced to 30 after 43 organisations or individuals were eliminated as they either did not provide psychological services to the target communities or referred people requiring services to other organisations.
Services/organisations for which there was a physical presence in the town on a permanent or part-time basis were defined as primary service providers. Secondary service providers were also identified. These predominately offered telephone support, although some offered face-to-face contact in exceptional circumstances. Some secondary providers were large and either state- or commonwealth-funded.
Psychological support services that were specific to a very small proportion of the community population such as those associated with a specific disease or infirmity (eg Cerebral Palsy League) were also considered secondary.
Data collection
Data were collected by telephone interview during June and July 2004. Information was provided by a person within an organisation who was directly involved with the provision of psychological support. A total of 44 interviews were held. Organisations were represented more than once in the interview process if they offered services from different locations, unless necessary information for the whole region was collected from one source.
Interviews only took place after receipt of consent given by the interviewee and, when necessary, the person within the organisation with authority to permit staff involvement in the survey.
The same research team member conducted all interviews. All interviews were undertaken by the same interviewer, an experienced researcher with extensive experience in interviewing. Each interview took between 15 and 30 min.
Instrument
Interviews were conducted using a semi-structured interview tool that collected the required quantitative data. The use of this tool guaranteed uniformity of topics across the entire sample, permitting collation and quantification of data from questions asked. The tool also provided the opportunity to explore topics further if it was believed appropriate or clarification was required.
For each service provider questions determined the:
- type of psychological services provided
- number and qualifications of people in the organisation providing psychological services
- hours of business during which time psychological service was available
- number of clients per month provided psychological services
- length of waiting lists.
In addition, the participants were asked their opinions on:
- hours of extra service that would be required to fulfil demand
- psychological service needs in their community
- the effect that withdrawal of a psychological service would have on their community.
Data analysis
Data were entered into a database for the production of basic descriptive statistical data. Qualitative data were used to assist in interpretability of findings.
Results
Service provision by telephone directory listings
A crude comparison of provision of psychological services in target communities with the regional centre of Toowoomba and with Queensland overall was obtained from telephone directory listings. Table 1 provides populations for each community and its surrounding area, the number of listings for 'counselling' and 'psychologists' provided in the Telstra Yellow Pages, and the number of residents per counselling service and psychological service.
The ratio of persons per counselling service (approximately 800 residents per service) in four of the target communities was comparable with that for Toowoomba (the largest regional town in Southern Queensland) and the rest of Queensland. However the population per psychologist appears far in excess of that for Queensland and Toowoomba. In fact, only five psychologists were listed for all target communities combined.
Service provision by interview of providers
All providers with a physical presence in the target communities of more than one day per month are listed (Table 2). Data are provided for staff numbers in terms of both full-time equivalents (FTE) and adjusted FTE for time specifically devoted to psychological service provision, including counselling activities, for each target community.
Table 2: Psychological support services for targeted communities and their outlying areas
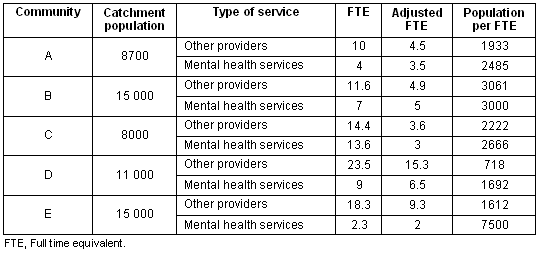
The 24 primary service providers included services within Queensland Health (eg community mental health, allied health), other government agencies, neighbourhood centres, the private sector, GPs and 11 NGOs. Six secondary providers either offered mainly a telephone service from Brisbane (the state capital) or Toowoomba or serviced only a very disease-specific and small sector of the population.
For service providers for whom psychological support was a part of their other services, information on time spent providing psychological services was not always available. In these cases, the time spent providing psychological services was estimated at 75% of work time and then adjusted according to other information provided. Overall estimate given for psychological service provision is likely, if anything, to be generous.
In Table 2 psychological services provided by the Community Mental Health Service in each community are included in a separate row. While these services represent a major source of psychological support for these communities, strict criteria for admission exist. Of the 57.6 FTE over all five communities, 20 FTE were specific to Community Mental Health. This warranted separation of these services from the more accessible 'general' services provided by other providers.
Results demonstrate a wide variation in general provision, from one provider per 718 people in Community D to one per 3061 persons in Community B. Similarly, provision through the mental health service ranged from one per 1692 persons (D) to one per 7500 in E.
Outside of the Community Mental Health services offered by Queensland Health, most support in all but one community was from NGOs. Support in communities A, B, C and E totalled 22.3 FTE, of which only 4.95 was provided by Queensland Health and 12.35 by a combination in each community of three of the five major NGOs. Only in community D was the majority support provided by Queensland Health with 12.5 FTE of the total 15.3 FTE provided by social workers, nurses and Aboriginal health workers.
Professions of those offering support
Psychological support was offered by a wide range of health professionals, including psychologists, social workers, nurses, occupational therapists, counsellors and medical officers. In general, psychologists with Queensland Health operated in Community Mental Health; outside this service support was offered by nurses or social workers. The five major primary NGOs all offered support by psychologists.
For the five communities the personnel offering support by primary providers are summarised (Table 3). About one-quarter of the psychological support workers fall into each of the professional categories.
Table 3: Profession of persons offering psychological support from primary sources

Identified unmet areas of need
Participants were asked if they believed there was a need for additional psychological services and in what area was the need greatest. There was a general reluctance of interviewees to state which issues (eg domestic violence, alcohol) were most important. This was primarily because they considered them inter-related. However, a number of areas were identified. The results are presented (Table 4).
The issue of need identified most frequently across communities was support for alcohol and drug abuse. Counselling for women subjected to sexual abuse issues, and lack of crisis support were identified in four of the five communities. It was believed that counselling for people with minor disabilities was lacking. Education as to what psychological support services may offer was identified as an unmet need in Community A. Respondents stressed, however, that this need must not be met at the expense of face-to-face support.
Table 4: Identified unmet areas of need for psychological support
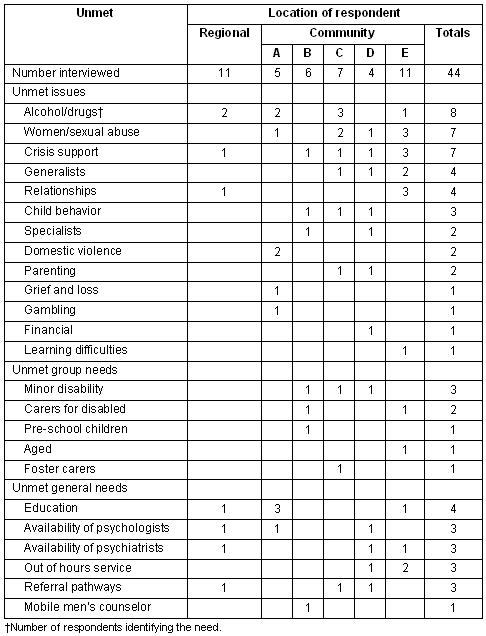
Effect of withdrawal of psychological services
When asked what the effect of removal of the major providers would be, two of the 44 respondents suggested that loss of a major provider would have little effect, because there was virtually no provision of psychological services in the first place. The other providers offered the opinion that the effect would be major. Terms used were 'overload of remaining services', 'void in provision', 'catastrophic', 'devastating'. This applied to loss of both specialised and generalised services which would generally lead to total, or at least substantial, lack of psychological service provision in that community as well as reduced access to already overworked alternative services.
When asked to comment on the overall situation one primary provider stated:
There are escalating needs that we have to meet with reduced resources in an environment of non-recurrent funding. As a result, lots of needs are not identified and this is exacerbated by the fact that rural people are reluctant to discuss issues. Furthermore, there is far too much paperwork cutting into valuable clinical time.
Two respondents noted that their community was used to loss of provision. As a result, they reported that communities were very wary of new initiatives because they did not believe the initiatives would last.
Waiting lists
The major service providers (Queensland Health and the five principal NGOs) offer some type of immediate assessment; however, waiting time for subsequent appointments was variable, ranging from one day to a month or 6 weeks.
Other important issues identified
Qualifications and experience of providers: Although most providers were qualified, there were three organisations where counsellors were trained but for whom formal qualifications were lacking. Concern was expressed by three respondents about advice being offered by such 'unqualified' people; however, these vastly experienced counsellors were generally recognised as providing a valuable service. It was also recognised that compromise had to be reached between a service being provided and there being no service at all.
Accessibility of services: A comment from an organisation involved with the labour market typifies the general feeling about psychological service support:
We do not tend to refer customers to private psychologists due to their lack of financial funds to pay for these services. In our rural communities, we regularly refer customers to social workers employed through Queensland Health, as it seems to be easier for these customers to access this type of support than to be offered psychological assistance through the mental health service. However, it is our experience that many customers referred for psychological assistance at the Mental Health Service are denied support through this service on the grounds that they do not fit in with their criteria ... Furthermore, for anything other than crisis situations, appointments within the health service are very difficult to obtain.
Reluctance to access services: Several providers talked of rural culture and reluctance to access psychological services. This was primarily because of the stigma associated with accessing psychological services and concern regarding confidentiality in a rural/remote environment. The situation, therefore, arises that on the one hand, there are insufficient numbers of providers, and on the other, people are reluctant to seek support because they associate psychology with mental illness.
It was noted by one psychologist that 'cold-calling' is effective for offering psychological services in rural communities. The perception was that, although people in rural communities often need support, they are reluctant to take the initiative themselves. If support is offered at their place of residence, however, they are happy to engage.
Nature of service provision: Another concern spoken about was the lack of crisis support. This was exacerbated by the general lack of out-of-hours service support and 'fragmented' services, with counsellors only operating in a location for limited periods each week or month. It may be that consolidation is required. One provider noted that sporadic visits led to a complex and confusing situation for both clients and practitioners.
Funding issues: NGOs are very concerned about their funding status. Five NGOs provide the bulk of general services to the communities; all five are dependant on 'soft' funding which is never guaranteed. Managers noted that a lack of continuity is of great concern to clients. The lack of job security is concerning to employers and employees alike. They reported that unless funds are sustainable and have continuity it is difficult to attract qualified and experienced people. Interruption of service was reported as very damaging, because client confidence was lost and was difficult to regain.
Discussion
Psychological services audit
The audit of telephone listings suggested that counselling services are fairly consistent with the state average. This contrasted with very limited numbers of psychologists available in any target communities. Indeed, only five psychologists appeared in the telephone directory when searches by town were undertaken. More detailed audit, however, identified 34 psychologists working in the region. Consumers have been shown to use telephone directories as a major source of information about health services (Eley, Hossain, Khatri; unpub. obs) and our results, therefore, would indicate that this form of information is not reliable for determining available services.
In fact the audit of actual services presented a very different picture. At first glance, the number of services appear counter to the assertion made by others that there is a paucity of psychological services in rural communities4-6. However, many services investigated are quite restrictive in the clients they see. The largest provider of psychological services to target communities, Community Mental Health, only supports patients with moderate to severe mental illness. The majority of people who would benefit from support do not fall into these categories and, as such, are dependant on other sources of support
The large service gap between those not meeting the criteria for the largest provider was mentioned repeatedly. This means that regular, reliable and accessible general psychological support is limited to the NGOs who receive some funding through state and federal government departments. Unfortunately NGOs are not guaranteed able to provide continuous services to communities because of funding situations. Additionally, figures suggest that the majority of psychologists in target communities are primarily employed by these NGOs, thus creating an unsure supply of a very limited resource.
Support is not confined to that given by psychologists and counsellors but to a whole array of individuals who address, and are recognised by their peers to address, the mental health of rural and remote population in South-west Queensland. In these environments the reality of who offers support often differs from the strict definitions of the allied health professions.
In addition to the primary and secondary providers there are other providers who offer services in target communities. However, they provide services to clients with specific illnesses or disabilities, and thus reach only a small proportion of the community. Additionally, most rarely have a physical presence in the community and frequency of visits is extremely variable.
The results, therefore, provide clarification of the initial findings presented by Dobson et a6. Specifically, while there is fairly good provision to communities for moderate and severe psychiatric illnesses, there is a paucity of services that provide general psychological support to target communities.
Indeed, the results indicate also the paucity of private psychologists providing services to communities. It will be interesting to observe the affect that recent government initiatives, such as the Better Outcomes in Mental Health Initiative10, have on the provision of psychological support in these communities. The data for this study was collected prior to this initiative having any impact upon psychological support to the communities targeted in this study.
Needs analysis of psychological services
Alcohol, drugs, women's issues, sexual abuse, and crisis support were the most commonly identified needs across target communities. Providers considered that these issues were often intertwined. Indeed, alcohol and drug abuse has been recognised as a national issue where up to one in ten adult Australians are likely to have a substance-use disorder2.
Impact on communities of withdrawal of services
There was, without exception, grave concern regarding the impact on communities of withdrawal of services. The loss of specialist and/or generalist services would lead to a substantial loss of psychological service provision in any target community. Losses would lead to increased demand on other already overworked services unlikely to be able to meet any extra demand. The already fragile situation of lack of continuity of services and client confidence would be damaged further.
Other issues
It is encouraging that providers in target communities appear to be working well together, despite minimal funding and resources. Nevertheless, a number of challenges exist regarding accessibility and provision of psychological services that need to be overcome. Access to free services for clients in target communities is minimal11 because there are strict criteria for admission or long waiting times. The majority of rural people are unable to afford paid psychological services. There are also other barriers to accessing psychological services present in these communities. From our experience and the findings of this study, there appears a stigma associated with accessing psychological support because it is associated with mental illness12,13. Coupled with this are concerns about whether confidentiality can be maintained in a small rural community13.
Issues have been identified regarding provider and professional-related factors that may affect the ability to provide appropriate psychological services in these communities. For health professionals providing services to these communities there is a lack of training opportunities and remuneration. Additionally, it is difficult to retain experienced, qualified professionals when there is a lack of continuity in terms of funding provided for general psychological support. The problem of lack of funding continuity has been identified by this team in the past as a barrier that needs to be addressed if communities are to retain the qualified health professionals they attract14.
There is evidence that when professionally provided psychological support is not immediately available, other support may be provided by community members without professional qualifications. While this support may fulfil an important community need, there is concern that some support sources may provide less than adequate support.
Finally, there appears to be a disturbing trend away from provision of counselling and face-to-face intervention in favour of health promotion and education programs. While health promotion and education programmes serve an important role in health outcomes for communities, it is just as important that they not replace provision of psychological support and interventions.
Cautions and limitations
We are confident that all principal providers of support have been identified, although we accept that other providers may exist. For example, other potential providers within small specialist services were identified but not contacted because of time constraints (eg support groups for Parkinson's disease, lupus, deafness and arthritis). In addition, more general provision of support through nursing homes, religious groups, shelters and so forth was not followed in detail. According to evidence, the need for psychological support within these institutions was identified and dealt with by referral to other psychological support services in or outside the community.
The audit determined people in positions and did not determine service positions that existed but were unfilled owing to lack of funding or unavailability of suitable staff. Numbers can change from week to week; although numbers of providers may rise, equally they may fall. The audit thus provided a snap-shot of the situation in mid-2004. We would suggest, however, based on more recent discussions with providers, that the situation has not changed. Indeed support for mental health was considered to be the greatest issue (after workforce) by health service providers throughout southern Queensland in 200615.
It must also be acknowledged that only providers were surveyed. Their opinion may not necessarily be representative of the wider community and this must be taken into account when interpreting the results of this research.
Acknowledgements
Funds for this project were provided by the Southern Queensland Rural Division of General Practice. We would like to thank the participants who provided their valuable time and knowledge to the project.
References
1. National Rural Health Alliance. Australian Health Ministers conference: healthy horizons 1999-2003. Canberra: National Rural Health Alliance, 1999.
2. Andrews G, Hall W, Teeson M, Henderson S. The national survey of mental health and wellbeing: the mental health of Australians. Canberra: Mental Health Branch, Commonwealth Department of Health and Aged Care, 1999.
3. Mental Health Council of Australia. Not for service: experiences of injustice and despair in mental health care in Australia. Canberra: Mental Health Council of Australia, 2005.
4. Queensland Health and Harper C, Cardona M, Bright M, Neill A, McClintock C, McCulloch B et al. Health determinants Queensland 2004 public health services. Brisbane: Queensland Health, 2004.
5. Caldwell TM, Jorm, AF, Knox S, Braddock D, Dear KBG, Britt H. General practice encounters for psychological problems in rural, remote and metropolitan areas in Australia. Australian and New Zealand Journal of Psychiatry 2004; 38: 774-780.
6. Dobson M, Fogarty G, Machin T. Survey of provision of allied health services for the Southern Queensland Rural Division of General Practice - final report. Toowoomba, QLD: University of Southern Queensland, 2003.
7. Parslow RA, Jorm AF. Who uses mental health services in Australia? An analysis of data from the National Survey of Mental Health and Wellbeing. Australian and New Zealand Journal of Psychiatry 2000; 34: 997-1008.
8. Australian Bureau of Statistics. Australian standard geographical classification system. Canberra: ABS, 2001.
9. Oppenheim AN. Questionnaire design, interviewing and attitude measurement. London: Pinter, 1992.
10. Commonwealth Department of Health and Ageing. Better outcomes in mental health care initiative: information sheet - update November 2002. Canberra: Commonwealth Department of Health and Ageing, 2002.
11. Judd F, Humphreys J. Mental health issues for rural and remote Australia. Australian Journal of Rural Health 2001; 9: 254-258.
12. Roberts L, Battaglia J, Epstein R. Frontier ethics: mental health care needs and ethical dilemmas in rural communities. Psychiatric services 1999; 50: 497-503.
13. Bishop B, Pellegrini S, Syme G, Shepherdson V. Rural women's health networks. Canberra: Department of Community Services and Health/AGPS, 1993.
14. Fallon T, Buikstra E, Rees S. A process and outcome evaluation of the South-West healthy communities program. Toowoomba, QLD: University of Southern Queensland, 2004.
15. Eley RM, Fahey P, Fallon A, Hegney D, Gorman D, Rogers-Clark C. Key issues in rural health: perspectives of health service providers in Queensland. Toowoomba, QLD: University of Southern Queensland, 2006.


