Introduction
Mental illness is a common medical condition. The World Health Organisation predicts that depression will rank as the second highest burden of disease by 20201. In the National Survey of Mental Health and Wellbeing, almost one in five Australians had experienced an anxiety, affective or substance abuse disorder in the last 12 months; however, less than half of these sought professional help2.
In Australia, approximately one-third of the population live in rural and remote areas, but only 8% of psychiatrists practise in such locations3. Thus, the majority (or all) of the medical care for mental illness resides in the primary care environment, with the GP often being the first port of call4. Rural GPs already have a substantial workload and the statistics of mental illness will only serve to increase this workload. The GP's ability to provide effective care is limited due to time and varying capacities to assess, diagnose and treat psychological disorders5.
Federal government policy encouraged a shift in mental health care from the hospital to the community6,7. This movement has seen the establishment of mental health services throughout metropolitan, as well as rural and remote locations. However, the integration of these services with primary care has presented a challenge. Consequently, numerous service models have been proposed along the lines of a similar process that has already occurred in the UK8.
The models which have been implemented in Australia include:
- community mental health team
- shifted outpatient clinic
- attached mental health professional
- consultant liaison model.
The community mental health team model was a step outside the hospital environs; however, there appeared to be little collaboration with primary care. In Townsville, Queensland, GPs reported difficulty accessing the mental health service due to the differing views on the role of the service9. A St George study in New South Wales revealed that mental health professionals thought the GPs were not interested in the treatment of mental illness and lacked specific skills10. The difficulties with communication and continuity of care were raised as issues that needed to be addressed.
The shifted outpatient clinic model saw a psychiatrist consult patients in a non-hospital setting; however, this did little to promote linkages to primary care. Tobin and Norris stated that if continuous care of patients with chronic mental illness was going to be successful, then linkages at all levels of service delivery needed to be established10.
An example of the attached mental health professional model was reported from rural Tasmania, where a mental health professional was attached to a medical practice on a salaried basis, a process successful in decreasing the suicide rate in this area11. However, the funding for this type of care was an issue preventing the widespread adoption of this model.
The consultant liaison attachment model saw increased liaison between the mental health workers, psychiatrist and the GP. This program type has proved to be successful in Canada, where it involved a large population and a health service organisation12. It brought the psychiatrists and mental health services into the family practice. In Victoria, Australia, a travelling mental health service provided education and training to GPs and mental health providers on the assessment and treatment of patients with anxiety and depression13. The CLIPP (Consultation Liaison in Primary Care Psychiatry) project in Melbourne linked the consultant liaison model with shared care, and proved to be successful14. Interestingly, it also saw the mental health service referring patients to GPs. Sixty percent of these patients reported that they felt their physical health had improved with the involvement of the GP in their care.
Models 1 and 2 did not particularly enhance the integration of mental health services with primary care GP services, while models 3 and 4 brought mental health services into the settings occupied by primary care providers. Nevertheless, all of these four models reinforced the role of the GP as a provider of mental health care and supported the up-skilling of the GP in mental health care. Some have proved effective in improving the health care of those with mental illness. However, these projects have involved small geographical areas and have focussed on integrating the mental health services with the GP.
Another possible model for improving mental health care in rural and remote areas is to relocate the GP to within the mental health service. There are a number of mental health units throughout rural and remote Queensland which have infrequent access to visiting specialists and rely on the advice and skills of a GP for the treatment of their patients with mental illness. The incorporation of the GP into the mental health unit may serve to improve communication between mental health providers and the GP, as well as up-skilling the GP in mental health care. An extensive review of the medical literature on MEDLINE by the principal investigator failed to find any mention of this particular model of service delivery in rural and remote areas.
The aim of this study was to determine the attitude of GPs in rural and remote Queensland to the concept of locating a GP within rural mental health units, and especially:
- whether they believed there is a need and a role for this GP position
- aspects of how this could assist health care for those with mental illness
- whether they personally would be interested in such a role
- whether they feel professionally competent to manage mental illness
- what form of remuneration they would prefer.
Methods
Setting
This survey was conducted in rural and remote Queensland in locations classified as rural, remote and metropolitan area classification (RRMA) 5-715. Within this classification system, RRMA 1 are capital cities, RRMA 2 are other densely populated urban areas, RRMA 3 are regional cities, with RRMA 4-7 being increasingly isolated rural/remote locations, RRMA 7 being the most remote.
Participants
The participants were all general practitioners listed on the databases of the Rural Divisions of General Practice covering RRMA 5-7 in Queensland. These GPs were entitled to refer patients with mental illness to the mental health units located in RRMA 5-7. However, to eliminate a potential conflict of interest, the GPs who could potentially refer patients to the Central Highlands Mental Health Service, due to their geographical proximity, were excluded because the principal investigator was providing services at that location.
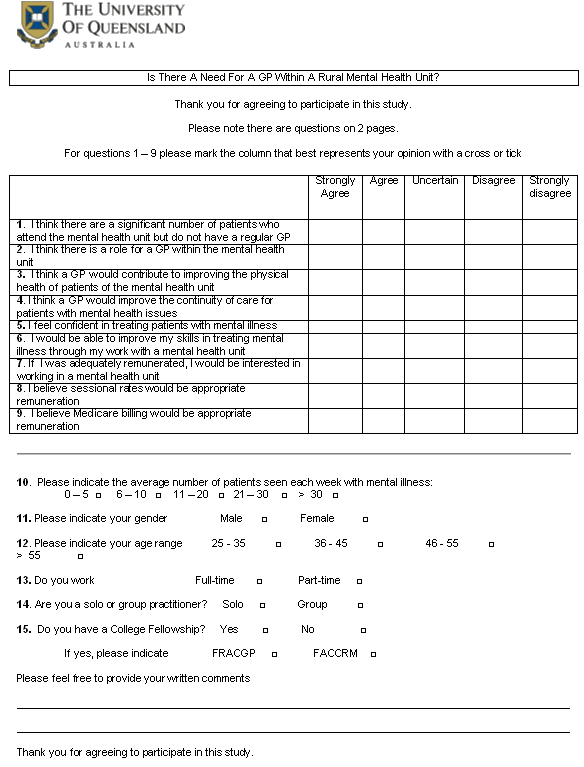
Questionnaire
The questionnaire was designed to gather the opinions of the rural and remote GPs regarding the need for a GP within a rural mental health unit. The first nine questions used a 5 point Likert scale (strongly disagree = -2, disagree = -1, uncertain = 0, agree = 1, and strongly agree = 2) to ascertain opinions about each of the following:
- the prevalence of mental health patients without a GP
- the GP's contribution to the health of the patients with mental illness
- the GP's confidence in treating mental illness
- the GP's willingness to provide services to the mental health unit
- the GP's chosen method of remuneration for work at a mental health unit.
The last six questions gathered demographic data: number of patients seen, age, gender, practice work structure and professional college fellowship. Participants were invited to provide free-text comments. The questionnaire is included (Appendix I).
Methodology
The participants were identified through the databases of the four rural Divisions of General Practice in Queensland. The Central Queensland Rural Division of General Practice liaised with the other three rural divisions of GP in Queensland to obtain assistance in distributing the surveys to GPs meeting the inclusion criteria. An information sheet and questionnaire were then forwarded to 210 GPs who met the inclusion criteria. The questionnaire was anonymous and voluntary. To increase the response rate, two follow-up mailings were performed at 1 and 2 months following the initial mailing.
Ethics
Ethical approval was gained from the University of Queensland Medical Research Ethics Committee.
Analysis
Data were analysed using SPSS software vers. 13 (SPSS Inc; Chicago, IL, USA). The demographic data was described using simple frequency analysis. Analysis of co-variance using the general linear model was used to calculate the significance of each opinion item with the demographic factors as covariants. The level of statistical significance was defined as p<0.05.
Results
In total 145 surveys were returned by participating GPs, a 69% response rate. The demographics of the participants are detailed (Table 1).
The responses to the nine opinion questions are detailed (Table 2). The respondents who stated that they were more confident in treating mental illness were more likely to have a college fellowship (p=0.01) or to see a higher number of mental health problems each week (p=0.004). Female practitioners were more likely to accept a sessional arrangement (p=0.04), while older practitioners were more likely to accept payment for services through Medicare, the national compulsory government insurance scheme (p=0.02).
Table 1: Demographics of general practitioner respondents
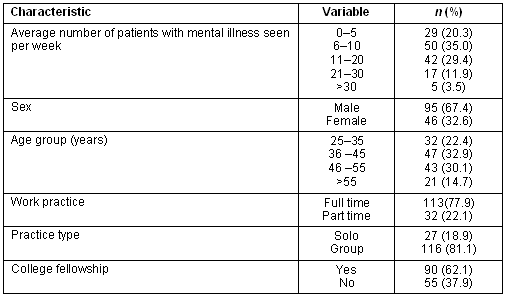
Table 2: Perceptions of general practitioner respondents

A variety of free-text responses were reported by participants which primarily focussed around the theme of the GPs as the major provider of primary care in the community. Comments considered the importance of continuity of care and looking after families, rather than simply individuals. As such, some respondents viewed the role of mental health professionals to be as secondary providers supporting the GP, rather than the reverse. However, the importance of providing mental health care and the need for GPs to further improve their skills in this area were frequently reported.
An important second theme was the working relationship between GPs and mental health providers. Although many respondents stated that they have an effective working relationship with their mental health providers, others expressed concern about the mechanics of a future closer relationship. The issues noted by respondents were:
- time
- finances
- staff
- communication
Mental health care consumes a considerable amount of time and in a busy, often already over-booked general practice, it may be very difficult to allocate sufficient time to provide the appropriate care.
Many felt they were not adequately remunerated for the time they did allocate to providing mental health care.
Chronic shortages of medical practitioners in rural and remote areas meant that the counselling and therapy often required by these patients may not be able to be provided.
Poor communication between the local mental health service and the GP has been noted previously to be a problem9,10, and in this study comments were once again made. These GPs felt that an improvement in communication between these services would definitely assist in the care of their patients. Some services do have regular meetings between the GPs and the mental health service and, in their opinion, provide a well-functioning system of care.
Discussion
The majority of GPs in this study believed that there is a role for a GP in a rural mental health unit and that this may improve the continuity of care of patients and also promote a more holistic approach to their care. With GPs providing care across the family and beyond, outcomes could be enhanced because mental illness management often extends beyond the individual. GPs provide important opportunities for continuity of care with their relative location stability, when compared with the often considerable turnover of mental health professionals and visiting psychiatrists.
If GPs are to be the primary provider of mental health care, they need to feel confident in providing such a service. It is interesting that the majority of GPs in this study indicated confidence in treating patients with mental illness, when earlier studies in New South Wales (2001) had demonstrated that GPs were largely providing non-specific, non-pharmacological interventions for patients with mental health problems16. This discrepancy may reflect the substantial increase in continuing education programs concerning mental health that have since become available, such as the 'Better Outcomes in Mental Health Care' program17. This is further suggested by a recent finding from New Zealand (2006), which showed GPs were managing mental health problems more in line with evidence-based practice than previously18. The other possibility is that these rural/remote based GPs have, by necessity due to distance, isolation and limited support services, been required to obtain higher levels of skills than their metropolitan counterparts who formed the majority of participants in the studies mentioned above.
Rural and remote GPs expressed some reservations about working within the mental health unit, related in part to uncertainty of expectations, remuneration, possible fragmentation of care and time management. This may pertain to the different organisational structure of general practice, compared with the mental health unit. GPs are centred on a predominantly private, small-business model where income is mostly from fees raised from individual patients, although much, if not all of these fees, are reimbursed through Medicare, the compulsory government insurance scheme. In contrast, mental health units are government-run and publicly funded, with the local staff and administration supported by large centralised bureaucratic processes located (at times) in geographically distant regional centres or the state capital city.
Conclusion
Rural and remote GPs in Queensland, Australia, believe there is a case for locating a GP within established mental health units, subject to addressing logistic and remuneration issues, because they believe this would enhance continuity of care and improve overall health for those with mental illness.
Acknowledgements
The authors would like to acknowledge the Central Queensland Rural Division of General Practice for assistance in distributing questionnaires to GPs; GPs in rural and remote Queensland for completing the questionnaires; Rural and Regional Queensland Consortium and General Practice Education and Training for providing funding for the academic position; and the Royal Australian College of General Practice for provision of funding.
References
1. Malcolm H. A Primary mental health-care model for rural Australia: outcomes for doctors and the community. Australian Journal of Rural Health 2000; 8: 167-172.
2. Andrews G, Hill W, Teeson M, Henderson S. The mental health of Australians. Canberra: Mental Health Branch, Commonwealth Department of Health & Aged Care, 1999.
3. Australian Institute of Health and Welfare. Mental health services in Australia 2000-2001. Canberra: Australian Institute of Health and Welfare, 2003.
4. Caldwell TM, Jorm AF, Knox S, Braddock D, Dear KBG, Britt H. General practice encounters for psychological problems in rural, remote and metropolitan areas in Australia. Australian and New Zealand Journal of Psychiatry 2004; 38: 774-780.
5. Vines RF, Richards JC, Thomson DM, Brechman-Toussaint M, Kluin M, Vesely L. Clinical psychology in general practice: a cohort study. Medical Journal of Australia 2004; 181: 74-77.
6. Commonwealth Department of Health and Aged Care. National action plan for promotion, prevention and early intervention for mental health. Canberra: Mental Health and Special Programs Branch, Commonwealth Department of Health and Aged Care, 2000.
7. Australian Health Ministers. National mental health plan 2003-2008. Canberra: Australian Government, 2003.
8. Gask L, Sibbald B, Creed F. Evaluating models of working at the interface between mental health services and primary care. British Journal of Psychiatry 1997; 170: 6-11.
9. Alsop M, Battye K. Integration of general practitioners and mental health services: the northern Queensland integrated mental health program. Australian Journal of Primary Health - Interchange 1999; 5: 20-26.
10. Tobin M, Norris G. Mental health and general practice: improving linkages using a total quality management approach. Australian Health Review 1998; 21: 100-110.
11. Malcolm H. Primary mental health-care model in rural Tasmania: outcomes for patients. Australian Journal of Rural Health 2002; 10: 20-25.
12. Kates N, Craven M, Crustolo A M, Nikolaou L, Allen C. Integrating mental health services within primary care. A Canadian program. General Hospital Psychiatry 1997; 19: 324-332.
13. Judd K, Davis J, Hodgins G, Scopelliti J, Agin B, Hulbert C. Rural integrated primary care psychiatry programme: a systems approach to education, training and service integration. Australasian Psychiatry 2004; 12: 42-47.
14. Meadows GN. Establishing a collaborative service model for primary mental health care. Medical Journal of Australia 1998; 168: 162-165.
15. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. AIHW cat. no. PHE 53. Canberra: AIHW, 2004.
16. Hickie IB, Davenport TA, Naismith SL, Scott EM, Hadzi-Pavlovic D, Koschera A. Treatment of common mental disorders in Australian general practice. Medical Journal of Australia 2001; 175(Suppl): S25-S30.
17. Department of Health and Ageing, Australian Government. Better outcomes in mental health care program. (Online) 2006. Available: http://www.health.gov.au/internet/wcms/publishing.nsf/content/mental-boimhc (Accessed: 13 December 2006).
18. Bushnell J, McLeod D, Dowell A, Salmond C, Ramage S, Collings S et al., MaGPIe Research Group. The treatment of common mental health problems in general practice. Family Practice 2006; 23: 53-59.
_________________
Appendix I
Questionnaire on the opinions of Queensland rural and remote GPs regarding the need for a GP within a rural mental health unit