Introduction
Primary percutaneous coronary intervention (PCI) is the main treatment strategy for ST-elevation myocardial infarction (STEMI) patients in Taiwan1. Several studies have demonstrated that earlier primary PCI leads to better clinical outcomes2-6. For emergency medical services (EMSs) transporting STEMI patients directly to a PCI-capable hospital, the primary goal is to limit the time from the first medical contact to the PCI procedure to less than 90 min7. For those who initially arrive at or are being transported to a non–PCI-capable hospital, the ideal first medical contact-to-PCI procedure time is within 120 min7. Therefore, identifying a STEMI case and confirming the indication for PCI as early as possible are crucial for non-PCI-capable hospitals located in rural or non-urban counties, often without a prehospital electrocardiogram (ECG) in their EMS transportation network.
Timely referral for a PCI procedure is important. The American Heart Association STEMI Systems Accelerator Project indicated that shorter first medical contact-to-device times could be improved in 16 US metropolitan regions by key care process implementation, including prehospital catheterisation laboratory (cath lab) activation (88 min for implementers v 98 min for non-implementers; p<0.001), single call transfer protocols at non-PCI-capable hospitals (112 min v 152 min; p<0.001), emergency department (ED) bypass for direct presenters via EMS to a PCI-capable hospital (84 min v 94 min; p<0.001), ED bypass patients transferred from a non-PCI-capable hospital to a PCI-capable hospital (123 min v 167 min; p<0.001)8. However, the study rarely mentioned the referral modality in detail between a PCI-capable hospital and a non-PCI-capable hospital or EMS.
Conventionally, in this study, an emergency patient referral can be described as follows. A referral is communicated through an electronic interhospital ED medical records platform. For example, before transferring an eligible STEMI patient, physicians in a local emergency department (LED) without a PCI device have to notify and get approval from the ED in a PCI-capable tertiary university hospital (TUH-ED). However, TUH-ED physicians usually cannot provide an immediate approval to the LED for the transfer until they are sure that their cardiac cath lab facility and personnel are currently available to perform the PCI procedure. The TUH-ED member of staff makes a phone call to the cardiologist of their cath lab to find out whether they can accept a critical LED referral patient. Therefore, to improve PCI time efficiency, the LED tries to obtain permission to connect directly with the cardiologist of the TUH-cath lab even before the TUH-ED physicians are notified.
This study demonstrated that the ED delay can be reduced by creating a direct connection between the LED and the TUH cath lab personnel compared with the conventional referral model.
Methods
Study hospital characteristics
The LED belongs to a non-PCI regional hospital located in one of the rural counties in central Taiwan. The hospital has 387 beds and on average it has 2500 to 3000 emergency cases per month. The TUH is a university hospital and medical centre with a comprehensive PCI centre. It is located in a metropolitan area in the centre of Taiwan and has about 1000 beds. The TUH has 4000 to 4500 emergency cases per month and performed between 818 and 863 PCI cases per year from 2014 to 2017.
Definition of STEMI
STEMI patients were diagnosed by cardiologists based on the ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation9. In the LED, STEMI patients were diagnosed by both the LED and the TUH cardiologists due to the need for transfer, whereas the TUH STEMI patients were confirmed by the TUH cardiologists.
Group classification and data collection
All data were retrospectively collected, from the medical records in the LED and the TUH, for STEMI patients who underwent primary PCI at the TUH from 1 January 2014 to 30 June 2017.
Patients were classified into two groups according to the first emergency department they visited: group A, comprising patients referred to the TUH through TUH-ED by the LED; and group B, comprising the TUH non-referral patients.
Conventionally, in group A, the flow of communication involved five steps involving the LED physician, the TUH-ED physician and the TUH cath lab cardiologist. To achieve faster access to primary PCI, the LED implemented a direct connection termed the ‘3 + 1’ transfer step flow of communication (Fig1). In the conventional transfer, before the ambulance departure from the LED, an LED physician is required to contact the TUH-ED physician, who then receives approval from the TUH cath lab cardiologist. The TUH-ED physician then notifies the LED physician who dispatches the ambulance. In the direct connection flow, the LED physician contacts the TUH cath lab cardiologist directly, receives approval for the transfer after confirmation of the indication for the primary PCI procedure and immediately dispatches the ambulance. The TUH-ED physician receives referral information from the TUH cath lab cardiologist as the patient is en route to the TUH-ED.
This study hypothesised that this approach would lead to a shorter delay for patients in the LED and result in an earlier PCI procedure. Moreover, the LED medical team can focus on other critical patients and avoid being distracted by waiting for an approval phone call from the TUH-ED.
Because this novel model of communication was implemented gradually, both communication models were in use during the initial phase. This complicated a direct comparison of delays before and after implementation. Therefore, the comparison between current LED delay time for referral patients in the LED and the TUH-ED delay time for non-referral patients in the TUH-ED were applied in this study, to determine whether the direct connection improved the transfer time for STEMI patients. The authors assumed that the ED delay time for TUH non-referral patients in the TUH was equal to that of the LED referral patients in the LED, or even shorter. Thus, from another perspective, the ED delay time in the TUH for non-referral patients can be considered equivalent to the LED delay time of the conventional model.
Data on age, sex, first ECG time difference, LED delay time (group A only), ambulance travel time (group A only) and TUH-ED delay time (both groups) were collected. All emergency medical durations were presented as medians because immediate resuscitation and emergency management or treatment required a prolonged ED delay in some critical patients, which produced a non-normal distribution in the study, although most acute coronary syndrome patients exhibited stable vital signs.
The statistical software used was the Statistical Package for the Social Sciences v20.0 (IBM; http://www.spss.com). The χ2 and student t-test were used to describe the characteristics including sex and age of the two groups. The Mann–Whitney U-test was used to compare ED delay time between referral patients in the LED and non-referral patients in the TUH-ED. The definitions of time efficiency are as follows:
- First ECG time difference (either LED or TUH-ED): time elapsed between a patient’s ED registration and performing the first ECG. The time difference of the first ECG was recorded by the authors as 1 min if a patient’s ED registration was done after performing the first ECG.
- LED delay time (group A only): time elapsed between a patient’s LED registration and ambulance departure for the TUH-ED. The LED registration time was recorded by the authors as the first ECG time if a patient’s LED registration was done after the first ECG.
- Ambulance travel time (group A only): time elapsed between ambulance departure from the LED and the TUH-ED registration completion.
- TUH-ED delay time (groups A and B): time elapsed between completion of the TUH-ED registration and performing PCI and balloon inflation in the cath lab. TUH-ED registration completion time was recorded by the authors as the first ECG time if a patient’s TUH-ED registration was completed after performing the first ECG.
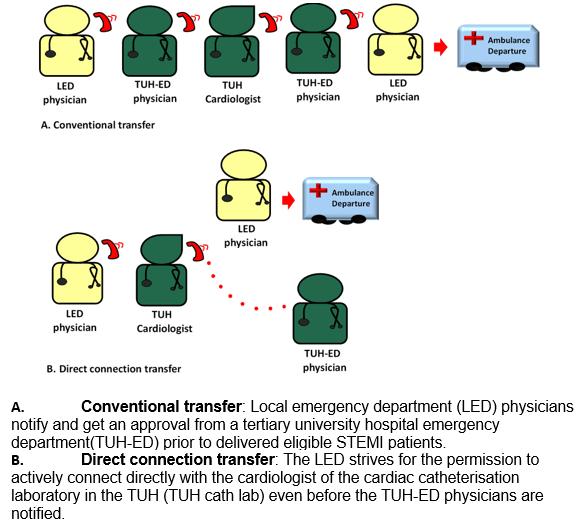 Figure 1: Flow chart of conventional transfer and direct connection in the local emergency department of a rural county in central Taiwan.
Figure 1: Flow chart of conventional transfer and direct connection in the local emergency department of a rural county in central Taiwan.
Ethics approval
This study was approved by the Institutional Review Board of Chung Shan Medical University Hospital (CSMUH No: CS2-17034).
Results
A total of 299 STEMI patients underwent primary PCI in the TUH during the 42-month study period. Of them, 73 were referred by the LED (group A) and 153 were TUH non-referral patients (group B). Twelve patients with missing or unconfirmed data (11 in group A and 1 in group B) were excluded from further analysis. Another 73 patients, from other non-urban hospitals, were excluded because their medical records were not accessible. Data for 62 patients in group A and 152 in group B underwent further analysis.
Group A patients were older than group B patients (65.6 ± 15.6 v 61.3 ± 12.5 years, p=0.06). Patients were predominantly male, with no between-group differences (80.6% v 79.6%, p=0.86; Table 1).
In group A, the medians of first ECG time difference in the LED, the LED delay time, ambulance travel time and the TUH-ED delay time were 1.0, 45.0, 21.0 and 35.0 min, respectively. In group B, the medians of first ECG time in the TUH and the TUH-ED delay time were 2.0 and 66.0 min, respectively (Table 2). Of all patients in group A, 83.8% (52/62) had the first ECG in less than 10 min compared with 88.8% (135/152) patients in group B (p=0.27); furthermore, in group A, 19.4% (12/62) of patients had an LED delay time of less than 30 min and 59.7% (37/62) had a delay time of less than60 min. Overall median time from the first hospital contact to PCI balloon inflation time (not including prehospital EMS contact) was 109.5 min in group A and 66.0 min in group B. Moreover, the calculated prehospital EMS contact to PCI balloon inflation time was 112.0 for group A, a total of 15 cases that were delivered to the LED by the EMS. However, ED delay time for referral patients in the LED was shorter than non-referral patients in the TUH-ED (45.0 v 66.0 min, p<0.01). Figure 2 shows the emergency medical durations for each phase in groups A and B.
Table 1: Distribution of groups A and B patients by sex and age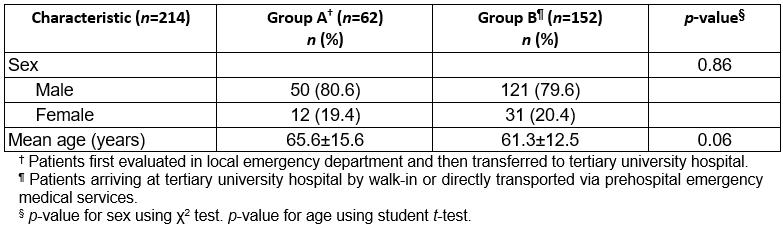
Table 2: Description of time efficiency in groups A and B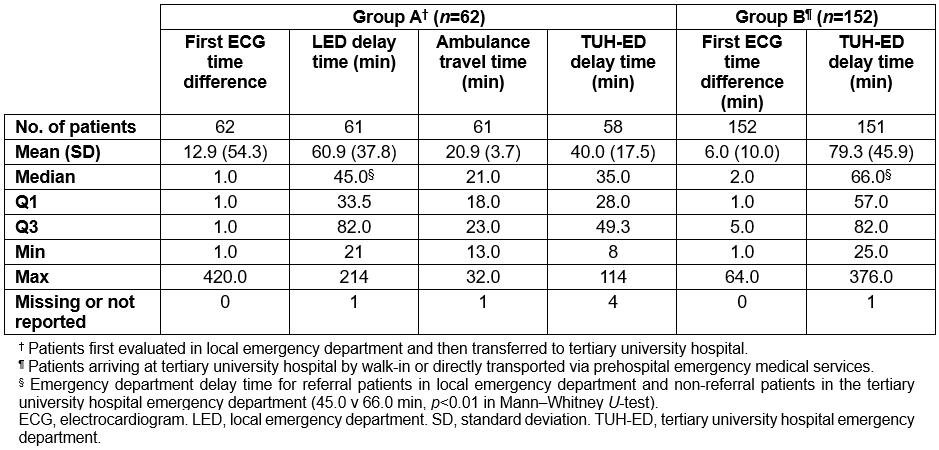
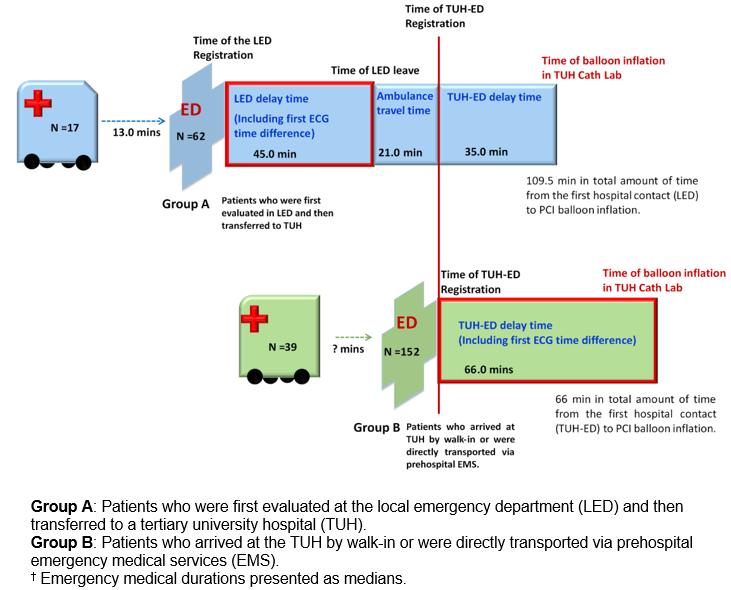 Figure 2: Emergency medical durations† for each phase in groups A and B.
Figure 2: Emergency medical durations† for each phase in groups A and B.
Discussion
Even though it seems more reasonable, in terms of patient safety and administration, to send approved patients directly to the cath lab from the rural LED, in the current inter-hospital transfer system in Taiwan these patients are usually first re-evaluated by an emergency physician in the TUH-ED before being transferred to the TUH cath lab. However, each person-to-person communication adds time delays, especially between two busy EDs. The present study demonstrated that the delay in the time to urgent primary PCI for STEMI patients can be shortened by creating a direct connection between the LED and the TUH cath lab. To the best of the authors’ knowledge, this might be the first report focused on this ‘3 + 1’ transfer step for acute coronary syndrome patients in Taiwan.
The demographic characteristics of the study population are comparable to those of a nationwide study. Yin et al. conducted a 15-year epidemiology study in Taiwan and showed that STEMI patients were more likely to be male, accounting for 77% of the patients; the age distribution was 64 ± 14 years10. Despite being of similar age, this study compared only two hospitals in Taiwan, and selection bias may exist.
There are various performance indicators to track the quality and efficiency of care for STEMI patients7. Prehospital ECG using an EMS bypass strategy has been frequently discussed11-13. In Taiwan, the local county government manages the local EMS system. In this study, the TUH prehospital timeline is unavailable because the author located at the LED cannot access the EMS database system in the TUH from another county. The LED data showed that only 27.4% (17/62) of patients were brought to the LED via EMS, with a median prehospital transportation time of 13.0 min. For these 17 EMS-delivered patients (excluding two patients for whom the PCI balloon inflation time was not reported), after including the prehospital EMS transport to the LED time, the calculated first medical contact to the balloon inflation time was 112.0 min. This study’s access to the prehospital EMS transportation time in group B was limited, although it was expected to be shorter in urban areas where the TUH is located. Due to Taiwan’s highly accessible medical system, people can visit either public or private medical facilities without referral14. Some ambulatory STEMI patients choose to seek medical treatment themselves instead of calling the EMS. Given the large number of STEMI patients who walk into the ED directly and are not brought via EMS, the earlier identification of STEMI patients in LEDs is of crucial importance. Public education strategies for the rescue of critical STEMI patients might also be necessary.
As seen in Table 2, STEMI patients received their first ECG quite early in both the LED and TUH-ED. However, some STEMI patients were still identified late. These patients may present in such a critical condition that they need to be resuscitated first, or they may present with atypical symptoms15. In rural or non-urban LEDs without cath labs, the choice between admitting such STEMI patients for thrombolysis medication versus transferring them to PCI-capable hospitals is difficult. Lassen et al indicated PCI should be the preferred reperfusion strategy if the extra time needed to perform PCI is less than 120 min, even if the first medical contact-to-PCI delay is greater than 120 min16. Therefore, strategies to improve the efficiency and safety of treatment are of crucial importance.
Reducing the communication steps, even by just one or two phone calls, can help to reduce the ED delay time for referred STEMI patients in the LED. However, this study found that there was still a 35 min delay from the TUH-ED registration time to the cath lab balloon inflation. It is not known whether this delay was due to the time required for decision-making by the patients or their families, overcrowding of the TUH-ED or managerial or administrative problems related to workflow. Future work is needed to examine the causes of the delays17-19.
The shortcut approach described in this study not only expedites the management of STEMI cases but also offers an informal telemedicine consulting window. It helps the rural or non-urban hospitals lacking specialists by providing them access to cardiologists’ timely interpretations of ECGs20. However, using electronic platforms for telemedicine functions may raise concerns regarding patient privacy. A direct connection to the cardiologist avoids second-hand information being passed to the cath lab members from the TUH-ED, reducing waiting times for STEMI patients in the LED. The novel direct connection described here presents the opportunity to replace the conventional transfer protocol in rural non-PCI-capable hospitals.
There are some limitations to this study. First, it was limited in its comparison of the effectiveness of a direct connection because the protocol had been evolving progressively before it was fully implemented on 1 January 2014. Second, the authors were not able to compare the prehospital EMS transportation times between the groups as the prehospital EMS transportation time in group B patients was not available. Third, conducting a long-term follow-up of the morbidity and mortality of the STEMI patients from different hospitals was not easy; therefore, the related data could not be presented in this study. Fourth, because this study focused on the efficiency of process change, the variables that might affect prognosis, such as medical history and Killip classification, were not included.
Conclusion
The direct connection between the LED and the TUH cath lab significantly shortened the delay time in the LED, allowing the primary PCI procedure for transferred STEMI patients to be conducted earlier.
Acknowledgements
The authors thank the co-workers at Chung Shan Medical University Hospital and Nantou Hospital, Ministry of Health and Welfare, for their assistance with data collection. This study was supported by Ministry of Health and Welfare, Taiwan (NANT-10603). The funding agencies did not influence the study design, data collection and analysis, decision to publish or preparation of the manuscript.
References
You might also be interested in:
2019 - Analysis of a decade of skin cancer prevention using a mobile unit

