Introduction
Rural and remote Australia is characterised by a diversity of environmental, demographic and economic variables. These factors impact the health status of rural Australians along a number of dimensions so that individual communities assume a distinct character of their own1. Indigenous and non-Indigenous communities, mining sites, tourist and portside towns, small inland townships, grain and pastoral holdings form unique socio-demographic amalgams. In addition, a number of rural communities have been subject to the withdrawal of services related to banking, transport and government activity, such as health and education2.
Meeting such diverse health needs involves particular challenges for mental health service providers3. Three-quarters of people in the general community seeking mental health care do so through consultation with a GP, and the majority of detection, treatment and referral of mental health disorders falls to GPs4. Furthermore, due to the shortage of allied health services in rural and remote Australia, rural GPs do not have the capacity to work collaboratively in a shared care framework. The more remote the community, the higher the likelihood that GPs provide complex care. Rural reliance on GPs as a singular resource adds weight to concerns that the extent of under-treatment in the community has a non-metropolitan component5.
The Australian Government has responded to some of these issues through using the More Allied Health Services (MAHS) and the Better Outcomes in Mental Health (BOMH) programs. The MAHS program was specifically funded to provide allied health resources to rural primary care settings although not specifically targeting mental health care6. The BOMHC was the more recent initiative and was funded to provide mental health resources to primary care practices, although not specifically to rural areas7. A major problem with both initiatives for rural settings was that both were project based and that funding has not been established or recurrent. There was a clear expectation that communities and existing services would be expected to establish funding streams to make such projects ongoing services. It has been noted that, in rural communities in particular, this has led to difficulties attracting and sustaining qualified professionals in the identified positions8.
The prevalence of mental health disorders in rural populations has not been well researched or documented9. The few studies that have attempted to differentiate the mental health status of rural and urban populations have presented mixed findings. Some studies have demonstrated higher prevalence rates in urban populations, whereas other research has identified elevated indicators of mental health problems as evidence of poorer mental wellbeing in rural sectors. Incidence and prevalence rates are somewhat difficult to interpret considering the use of disparate research methods and the use of differential access to mental health services as an indicator of prevalence, which may be related to prevalence but is nonetheless a distinctly different issue. Small populations in rural and remote regions can make comparative attempts unreliable and further obstruct a clear representation10.
This is further complicated by a lack of agreed definition of rurality11. While the range of diverse variables inherent in rural communities has been resistant to straightforward classification, several indexes using largely geographical indicators have been developed to provide input into health-care planning and funding12. The most commonly utilised standards are the RRMA (Rural Remote Metropolitan Areas) the ARIA (Accessibility/Remoteness Index) and, more recently, the ARIA+. The RRMA has been utilised in interpreting a range of health information, such as mortality statistics, cancer incidence, medical labour force data, Medicare data and risk factors11. This schema acknowledges that the generic issues encountered in rural health per se are implicit in mental health, and that factors that impact physical health also have the potential to influence mental health13.
In acknowledgement that a large portion of rural disadvantage is due to service accessibility, ARIA was developed to facilitate distinctions between social and locational barriers. Use of ARIA in research has confirmed an association between the size of service centres and the availability of services, and is useful in studies using accessibility as the premise of disadvantage in rural areas10. ARIA has important implications for mental health service evaluation in that a major inhibitory factor in accessing mental health care is the long distances between centres and fewer GPs and even fewer specialists per capita12.
It has also been argued that mental health status is dependant on more subtle and intricate factors that are not considered in national systems such as RRMA or ARIA10,14. The aggregation of mental health indicators masks regional differences, such as community relationships, population size and growth, and aesthetic variables, which are significant contributing factors to mental health status12. Consequently, Judd et al.15-17 have argued that more effort should be put in to developing a model of 'place' that integrates geographical location with cultural, social and economic aspects of the environment to better inform policy and funding initiatives in health service delivery.
Thus, it may more effective to identify the inherent factors specific to a community in order to understand how 'place' contributes to the development of mental health disorders in rural populations. The National Survey of Mental Health and Wellbeing indicated that people living in rural areas found only slightly lower mean scores on the General Health Questionnaire (GHQ) than their urban counterparts18. As noted, such findings should be interpreted with caution because the broad categories of 'metropolitan' and 'non-metropolitan' can average out significant contributing community specific factors. However, other factors combined with rural living may be more powerful than just location of residence alone. Poverty, unemployment, being female, being unmarried, lower socio-economic status, alcohol abuse, history of childhood sexual abuse, poor social networks, and size of primary support group, to name only a few, are factors that have been found to be strongly associated with prevalence19.
While a review of the question of what constitutes 'place' is outside the scope of this paper, there is an excellent discussion of these issues in a recent review of the rural mental health literature20. For our purposes, though, 'place' was considered to be a multidimensional concept encompassing psychological, emotional, socio-economic and geographical factors. Consequently we operationalised how respondents might think about their 'place' of living by asking about how they felt about where they lived, as well as about where they lived.
The purpose of the study described in this article was to begin an exploration of some of these issues. In particular, we took advantage of the location to compare the impact of different types of rurality (a regional centre versus surrounding rural towns) on mental health status. In addition, we included some initial measures of the construct of 'place' including length of residency, satisfaction and perceived quality of life in place of residence.
Methodology
Participants
The area of study was Townsville, Queensland, Australia, and the outlying rural areas of Cardwell, Charters Towers, Ingham and Ayr in north Queensland. General practitioners were identified by the Townsville Division of General Practice and the North-West Primary Care Division, which are the peak primary care bodies for the geographical area. Interested GPs gave permission for the surveys to be completed in their practices and agreed to provide additional data.
Townsville is located some 1500 km North of Brisbane and is the second largest metropolitan centre in Queensland. It is one of the fastest growing regional centres in Australia and the population of Townsville and surrounding regions is approximately 170 000 and growing rapidly. Townsville is a relatively isolated centre and the nearest town is 2-3 hours by car. All of the towns where GPs agreed to participate in this study were located between two and four hours away from Townsville.
This article is concerned with the second phase of a two stage research project21. During the first phase 304 patients in general practice settings participated, and in the second phase 130 agreed to further participation. Participants were then randomly selected for interview so as to provide proportionate numbers of rural and non-rural subjects.
In all, 118 subjects completed a telephone diagnostic interview, with 66% from the rural areas and 34% from the metropolitan centre. There were 79 women (69%) in the sample and 39 men (31%). The age range was 18-90 years, with a mean age of 54 (SD = l5 years).
Measures
The Composite International Diagnostic Interview (CIDI) was developed by WHO to specifically align with the Diagnostic and Statistical Manual Fourth Edition DSM-IV and the 10th edition of the International Classification of Diseases ICD-10. The diagnostic categories are established by symptom threshold cut-offs that are representative of underlying disorder constructs. It consists of a series of probe questions for depression, anxiety and substance use disorders. If respondents indicate positively to the probe, more detailed symptom specific questions follow22.
The Composite International Diagnostic Interview - Short Form (CIDI-SF) was developed to provide a quicker process of screening for psychological disorder in epidemiological studies. The scale takes an average of 7 min to administer compared with an hour or more for the CIDI and can be conveniently administered over the phone. Although the CIDI-SF has a number of limitations, including a lack of validation studies, the developers see it as being of use in general epidemiological research where a time-consuming psychiatric interview may not be feasible23. In the past several years there have been an increasing number of publications describing the use of the CIDI-SF24-30 for a variety of purposes using a number of different approaches to administration.
The computer program used in this study ensures the logic of the interview and contains skips whenever it is impossible for the particular criteria to be met31. The CIDI-SF identifies potential symptoms of mental health problems and explores these symptoms to identify the level of clinical significance. The diagnoses made by the CIDI-SF can only be seen as an approximation of what an experienced practitioner would generate in the same setting. The CIDI-SF is able to provide a diagnosis of depression, generalised anxiety disorder, specific phobia, social phobia, agoraphobia, panic disorder, obsessive-compulsive disorder, alcohol use disorder, drug use disorder. It does not allow for diagnoses of major psychotic disorders23.
Method
In the first stage of the study, participants completed the General Health Questionnaire (GHQ12) and provided demographic information. Respondents were also asked to report any pre-existing physical or psychological conditions from a checklist. They then provided a self rating (3-point scale) on their current physical and psychological wellbeing. Finally, the respondents provided information about their current living circumstances, including length of residence, satisfaction with location, quality of life, and whether they were caring for an aged or disabled relative. On completion of the questionnaires, the respondents placed the forms inside an envelope and handed this to the GP during their consultation.
The GP then completed a patient assessment section indicating if the patient had been previously diagnosed with a physical or psychological condition or complaint, rating the patient's physical wellbeing on a scale of 1 (very poor) to 8 (very good), their psychological wellbeing on a scale of 1 (very poor) to 8 (very good), and whether they had conducted any psychological interventions, prescribed medication or referred the patient to a mental health specialist during the consultation. The GP completed a patient assessment section indicating if the patient had a current illness or complaint, rating of the patient's physical health and psychological health and whether the GP provided any psychological interventions, prescribed medication or referred the patient to a mental health specialist during the consultation. Patient permission was sought to authorize further contact from the researchers for stage two of the study.
In the second stage, the CIDI-SF, a brief structured interview, was administered over the telephone using a computer-aided interview version developed by Campbell31.
Results
There were no significant differences between the rural and regional groups on gender, age, level of education, relationship status, number of dependants, employment, or income. The distributions across these variables can be seen (Table 1).
In the overall sample, 41 (34.7%) of the respondents were identified as meeting the criteria for a diagnosable mental illness on the CIDI-SF. This is somewhat higher than the rate found in the WHO study of psychological problems in primary care (25%)32, but similar to that found in the most recent Australian SPHERE primary care study33-35. There was a significant difference between rural and regional participants in the numbers diagnosed with a mental illness. Some 34 (83%) of those diagnosed with a disorder were located in a rural area compared with 7 (17%) being located in a regional urban centre (c2=6.83, df=1. p<0.009). This gives a relative risk of 2.49 (1.21, 5.11 95% CI) for a diagnosis of psychological disorder for the rural participants.
Table 1: Frequencies of sociodemographic variables in each sample
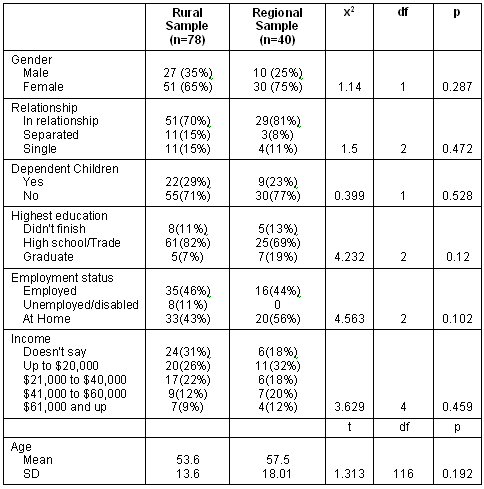
This difference was not accounted for by differential sampling from the different locations, because the same proportion of participants sourced from rural and regional GP practices in study 1 was randomly selected for follow-up interview. Participants from a rural setting were 2.5 times more likely to be diagnosed with a mental illness than participants from the regional centre.
The relationship between diagnosis and other variables was explored using logistic regression. The dependent variable of whether or not a participant received a CIDI-SF diagnosis was evaluated in relation to a range of sociodemographic variables (age, sex, relationships status, education, income, employment) and variables related to residence (rurality, caring for sick or disabled relative, length of residence, satisfaction with place of residence, perceived quality of life). The results of this analysis are reported (Table 2).
Table 2: Logistic regression of sociodemographic and residence variables against diagnostic category
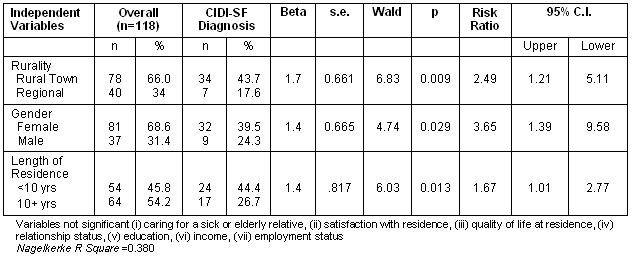
The only variables that had a significant relationship with the likelihood of receiving a diagnosis were rurality, sex, and length of time resident in an area. The regression was quite meaningful and the identified predictors accounted for approximately 38% of the variance in diagnostic category (it is, however, acknowledged that the interpretation of r-square with logistic regression is problematic and that this figure should be interpreted quite conservatively). Rural residence continued to be a major predictor of diagnosis with participants from a rural setting being five times more likely to receive a diagnosis. Interestingly, the length of time that a participant had been resident in an area was also predictive of a diagnosis. Participants who had been resident in an area for less than 10 years were four times more likely than participants who had been resident for 10 years or more to receive a diagnosis. Gender was also significant with women four times more likely than men to receive a diagnosis.
Discussion
This study found that there was a significant difference in the number of people receiving a diagnosis between the rural and regional groups. Those living in the rural setting were at a greatly increased risk of being diagnosed with mental health disorder than those who lived in the regional centre. The difference in rates of diagnosis between the rural and regional settings was quite marked, and this should be considered cautiously given the sample size and other methodological limitations to the study. Our findings were limited by the size of the sample, which was quite small, and by the fact that all of the participants were strongly selected. Not only had they volunteered to complete the initial survey in their GP surgery, but also the final number were only those who were further willing to volunteer for a detailed phone interview. There is no doubt that some level of bias may have been introduced through this methodology.
However such a finding certainly points to rurality as a factor in the development of psychological disorders. This finding is, to some degree, supported by our finding that another measure of 'place' (less time in an area) was significantly associated with likelihood of a psychological problem. Length of residence is likely to be a compound factor with many other issues linked to it such as more established social networks, more stability, and so on. Thus, the association that we found here may reflect the influence of a number of underlying variables that we did not measure. It must be acknowledged, however, that there are alternative explanations for these results that cannot be ruled out. It may be that rural residents are more likely to receive mental health care from their GP due to lack of access to mental health specialists. In addition, there is the possibility that people with psychological problems may migrate to rural settings for reduced housing costs, which would lead to them being over-represented in this study.
Conclusion
Mental health care in rural Australia is characterised by distinct issues due to geographical isolation compounded by a range of situational dynamics. Availability, location, affordability, appropriateness, accessibility, and heterogeneity of exposure to health risks all mediate effective mental health care36. Yet there is little or no research available that specifically addresses the impact of 'rurality' and 'place' on the psychological wellbeing of people. Most studies to date have utilised broad and inadequate markers of the 'rurality' issues. The current study suggests that there may indeed be value in further developing these concepts and directly assessing the role of these factors in both rural and non-rural settings. Indeed it may now be time for a major evaluation of mental health in Australia that takes account of the heterogenous nature of the population and allows for a better understanding of the impact of quality of life, location in a community, and access to services on our population's psychological wellbeing.
The key to providing good quality psychological services in rural Australia will require getting three critical issues right. Further research needs to focus on developing understanding of the level of need in rural setting, understanding of the rural cultural attitudes to mental health and how to address these, and a proper evaluation of how to provide universal/primary care mental health services in the uniqueness of a rural setting without merely settling for 'off-the-shelf' models of service delivery that have little or no relevance to the cultural context of rural people.
References
1. Fraser C, Judd F, Jackson H, Murray G, Humphreys J, Hodgins G. Does one size really fit all? Why the mental health of rural Australians requires further research. Australian Journal of Rural Health 2002; 10: 288-295.
2. Fuller J, Edwards J, Procter N, Moss J. How definition of mental health problems can influence help seeking in rural and remote communities. Australian Journal of Rural Health 2000; 8: 148-153.
3. Humphreys JS, Jones JA, Jones MP, Mildenhall D, Mara PR, Chater B et al. The influence of geographical location on the complexity of rural general practice activities. Medical Journal of Australia 2003; 179: 416-420.
4. Whiteford H, Buckingham B, Manderscheid R. Australia's National Mental Health Strategy. British Journal of Psychiatry 2002; 180: 210-215.
5. Sanderson K, Andrews G. Mental disorders and burden of disease: how was disability estimated and was it valid? Australian and New Zealand Journal of Psychiatry 2001; 35: 668-676.
6. Commonwealth Department of Health and Ageing. Guidelines for the More Allied Health Services program. Canberra, ACT: Commonwealth Government; 2002.
7. Mental Health Branch. Better outcomes in mental health care initiative. (Online) 2002. Available from: http://www.health.gov.au/mentalhealth (Accessed 28 August 2006).
8. Bowers E, Holmwood C, McCabe CJ. Models of primary health care psychotherapy and counselling. Adelaide, SA: Flinders University, Department of General Practice, 2002.
9. Judd F, Murray G, Fraser C, Humphreys J, Hodgins G, Jackson H. The mental health of rural Australians: Developing a framework for strategic research. Australian Journal of Rural Health 2002; 10: 296-301.
10. Fuller J, Edwards J, Proctor N, Moss J. Mental health in rural and remote Australia. In: D Wilkinson, I Blue (Eds). The new rural health. Melbourne: Oxford University Press, 2002; 171-185.
11. Humphreys J. Rural health status: what do statistics show that we don't already know? Australian Journal of Rural Health 1999; 7: 60-63.
12. Murray G, Judd F, Jackson H, Fraser C, Komiti A, Hodgins G et al. Rurality and mental health: the role of accessibility. Australian and New Zealand Journal of Psychiatry 2004; 38: 629-934.
13. Aoun S, Underwood R, Rouse I. Primary mental health care in a rural community: patient and illness profiles, treatment and referral. Australian Journal of Rural Health 1997; 5: 37-42.
14. Bramston P, Rogers-Clarke C, Hegney D, Bishop J. Gender roles and geographic location as predictors of emotional distress in Australian women. Australian Journal of Rural Health 2000; 8: 154-160.
15. Judd F, Fraser C, Grigg M, Scopelliti J, Hodgins G, Donoghue A et al. Rural psychiatry: special issues and models of service delivery. Disease Management and Health Outcomes 2002; 10: 771-781.
16. Judd F, Humphreys J. Mental health issues for rural and remote Australia. Australian Journal of Rural Health 2001; 9: 254.
17. Judd F, Jackson H, Komiti A, Murray G, Hodgins G, Fraser C. High prevalence disorders in urban and rural communities. Australian and New Zealand Journal of Psychiatry 2002; 36: 104-113.
18. Korten A, Henderson S. The Australian National Survey of Mental Health and Well-Being. Common psychological symptoms and disablement. British Journal of Psychiatry 2000; 177: 325-330.
19. Judd F, Davis J, Hodgins G, Scopelliti J, Agin B, Hulbert C. Rural Integrated Primary Care Psychiatry Program: a systems approach to education, training, and service integration. Australasian Psychiatry 2004; 12: 42-47.
20. Philo C, Parr H, Burns N. Rural madness: a geographical reading and critique of the rural mental health literature. Journal of Rural Studies 2003; 19: 259-281.
21. Campbell A, Caffrey J, Manoff T. Does rurality effect mental health? A primary care study. Townsville: James Cook University, 2005; 27.
22. Nelson CB, Rc K, D M. Scoring the WHO's Composite International Diagnostic Interview Short Form (CIDI-SF; v1.1 Dec2002). (Online) 1998. Available from: http://www3.who.int/cidi/cidisf.htm (Accessed 28 August 2006).
23. Kessler RC, Andrews G, Mroczek D, Ustun B, Wittchen H. The World Health Organization composite international diagnostic interview short-form (CIDI-SF). International Journal of Methods in Psychiatric Research 1998; 7: 171-185.
24. Egede L, Zheng D. Independent factors associated with major depressive disorder in a national sample of individuals with diabetes. Diabetes Care 2003; 26: 104-111.
25. Goodwin R, Pine D. Respiratory disease and panic attacks among adults in the United States. Chest 2002; 122: 645-651.
26. Pollack H, Danziger S, Seefeldt K, Jayakody R. Substance use among welfare recipients: trends and policy responses. Social Service Review 2002; June: 256-274.
27. Rosen D, Spencer MS, Tolman RM, Williams DR, Jackson JS. Psychiatric disorders and substance dependence among unmarried low-income mothers. Health and Social Work 2003; 28: 157-165.
28. Sturm R, Gresenz C. Relations of income inequality and family income to chronic medical conditions and mental health disorders: national survey in USA. BMJ 2002; 324(7328): 20-24.
29. Wade T, Cairney J, Pevalin D. Emergence of gender differences in depression during adolescence: national panel results from three countries. Journal of the American Academy of Child and Adolescent Psychiatry 2002; 41: 190-198.
30. Young S, Klap R, Sherbourne C, Wells K. The quality of care for depressive and anxiety disorders in the United States. Archives of General Psychiatry 2001; 58: 55.
31. Campbell A. Psychological problems in rural primary care: evaluating a model of mental health service delivery in rural Tasmania. Launceston: University of Tasmania, 2004.
32. Sartorius N, Ustun T, Jorges-Alberto C, Goldberg D, Lecrubier Y, Ormel J et al. An international study of psychological problems in primary care: preliminary report from the WHO collaborative project on 'Psychological problems in general health care'. Archives of General Psychiatry 1993; 50: 819-824.
33. Hickie IB, Davenport TA, Hadzi-Pavlovic D, Koschera A, Naismith SL, Scott EM et al. Development of a simple screening tool for common mental disorders in general practice. Medical Journal of Australia 2001; 16(175): S10-S7.
34. Hickie IB, Davenport TA, Naismith SL, Scott EM. SPHERE: a national depression project. SPHERE National Secretariat. Medical Journal of Australia 2001; 16(175): S4-S5.
35. Hickie IB, Davenport TA, Naismith SL, Scott EM. Conclusions about the assessment and management of common mental disorders in Australian general practice. Medical Journal of Australia 2001; 16(175): S52-S55.
36. Patterson C. The emergence of rural health research in Australia. Australian Journal of Rural Health 2000; 8: 280-285.
37. Campbell A. The evaluation of a model of primary mental health care in rural Tasmania. Australian Journal Rural Health 2005; 13: 142-148.
Abstract
Introduction:
Until recently, there has been a significant gap in the literature exploring the issues of the mental health needs for rural communities in Australia. In this study we investigated the prevalence of diagnosable psychological disorders in both a rural and a non-rural primary care sample in far north Queensland, Australia.Method: In a previous study we had screened some 300 GP attendees, on a number of sociodemographic variables and measures of psychological wellbeing, from four rural GP practices and one regional GP practice. Of these, 130 participants agreed to further follow up. In this study, 118 of the participants were selected and contacted by phone to complete the Composite International Diagnostic Interview-Short Form (CIDI-SF). The CIDI-SF diagnosis was then analysed in relation to the sociodemographic indicators that had previously been collected.
Results: The prevalence of diagnosable mental health disorders in the rural sample was found to be higher in comparison with the regional urban sample. The sociodemographic factors of rural residence, gender, and length of residence were associated with having a CIDI-SF diagnosis.
Conclusion: Although there were a number of methodological limitations to this study, there did appear to be a significant relationship between rural location and the likelihood of receiving a CIDI-SF diagnosis. Why this might be the case is not clear, and we consider a number of explanations, but our finding suggests that further research in mental health should consider the issue of rurality as a key feature to be explored.
Key words: mental health disorders, prevalence, rurality.
You might also be interested in:
2011 - Nature and nurture in the family physician's choice of practice location
2006 - Comparison of stroke among Christians and Muslims in Thrace, Greece

