Introduction
Cambodia (population 13 million) has been on a steady path of reconstruction following the end of civil war and the signing of peace accords in 1993. Although the country has registered comparatively low levels of social and economic development (Gross National Income [GNI] US$350 per capita)1 and associated high rates of child and maternal mortality, there are promising signs that the country is gradually developing institutional, economic, and civil societal frameworks. One example of this development is occurring within the health sector. Although human resources and health infrastructure were almost completely destroyed during the Pol Pot regime between 1975 and 1979, the health system now consists of a network of 935 health centers, 76 operational health districts, 24 provincial health departments, and more than 20 national health programs, including the National Immunization Program (NIP)2. Established in 1986 with the technical assistance of UNICEF, the NIP has expanded nationally and coordinates the immunization of children under the age of one year (cohort of 372 000 in 2006) against seven diseases, as well as immunization against tetanus among women of child-bearing age.
The NIP has achieved impressive public health outcomes between 2000 and 2005. Demographic health surveys conducted in 2000 and 2005 have seen a significant rise in the immunization coverage rate of diphtheria, pertussis and tetanus vaccine (DPT3) in children aged 12 months of age from 43% in 2000 to 76% in 20053. There has been a related decline in the reporting of vaccine-preventable diseases. Neonatal tetanus cases have reduced from 169 in 2002 to 68 in 2005 (decline in incidence from .05 to .02 per 1000 births). Suspected measles cases have been reduced from 3640 in 2001 to 264 in 2005 (decline in incidence from 289 to 19 per million population), and measles immunization coverage has increased from 41% (2000) to 70% (2005)4, p.55 (Fig1).
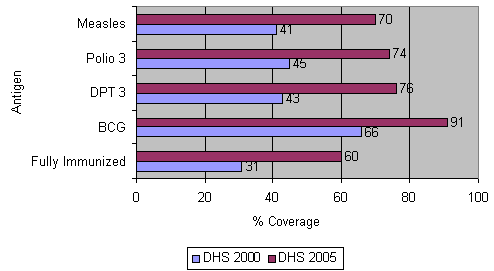
Figure 1: Trends in vaccination among children aged 12-23 months Cambodia Demographic Health Surveys (DHS) 2000 and 2005. Data source3. DPT, Diphtheria, pertussis and tetanus.
Additionally, the latest evidence from the demographic health survey in 2005 indicates no significant difference between rural and urban immunization coverage rates, despite that fact that 80% of the population of Cambodia is rurally based3. In this period, the national program also responded to the logistical challenges of introducing auto-disable syringes, a new vaccine (hepatitis B), and a new vaccine cold chain and waste management system.
Background on the health planning system in Cambodia
The health sector has developed in tandem with the extension of national programs addressing tuberculosis, malaria, HIV/AIDS, and immunization. In 1996, health sector reform was undertaken by the Ministry of Health (MOH), and included definitions of packages of essential services and minimum population catchments for secondary level (referral hospital) and primary care level (health center)4.
Subsequent to health sector reform, the MOH developed a new planning system in 2002 and drafted the National Health Sector Strategic Plan5,6. Under the new planning system, health systems at all levels, including national health programs, share common strategic areas, planning formats, and planning tools and follow the same annual and three-year planning cycle. An important feature of the new planning system is that objective setting and activity development are undertaken prior to budgeting, to ensure that there is a match between identified activities and resources required to implement them. All plans are integrated at provincial, district, and health facility levels. There is no specific requirement below the national level with regard to planning for the national program. A five-year strategic plan (for both the health sector and the national program) is developed only at the national level.
Objectives and sources of information
The objectives of this article are to:
- describe the process of national program planning in Cambodia.
- outline the impact of new immunization planning approaches, specifically those of the Cambodian National Immunization Program, on the quality of national program management and public health outcomes.
- identify future challenges and opportunities for immunization health planning and national program planning more generally in Cambodia.
The processes of sub-national and financial planning have been described previously in the literature7,8. This review, in contrast, will primarily focus on the process and development of national health planning.
Sources of information for this review included international literature, strategic and operational plans of the Cambodian MOH (sector, national program, and sub-national health plans), routine health information, recently published studies on health planning in Cambodia, and information generated through development of a financial sustainability plan for immunization. Three of the authors of this review have led or facilitated national and sub-national program planning processes in Cambodia between 2002 and 2006, and others have provided input in to the development of multi-year planning processes on a regional and global level. Planning forums conducted by the NIP in 2005 included annual program reviews, provincial health planning, health facility micro-planning, and communication workshops with local authorities in each of the country's 24 provinces (for more detail on communication activity and sub national planning methodology see9,10, respectively).
Developments in National Immunization Program planning 2002-2006
In recent years, key adaptations to the NIP process successfully addressed health sector and civil society developments. These important reforms included:
- Strengthening links among immunization and health sector and international planning.
- Developing a multiyear plan (MYP) and financial sustainability plan (FSP).
- Strengthening national decision-making structures and processes.
- Widening stakeholder participation in planning.
- Strengthening service micro-planning.
Each of these reforms is outlined in detail below.
REFORM 1: Strengthening links among immunization planning, health sector and international health planning
Planners for the NIP (national level program managers) actively consult with the Planning Department of the MOH to identify and measure progress toward Millennium Development Goals using immunization indicators. The WHO has set regional goals for measles and hepatitis B elimination, and UNICEF likewise has developed global goals and targets for neonatal tetanus elimination11,12. These regional and global targets and strategies provide points of reference for national planners to measure performance and pinpoint technical assistance and resource needs.
A key feature of the new national health planning system is the development of a revised national planning cycle. The new planning system was developed by the MOH in 2002 in response to the need to develop a more decentralized planning framework following health sector reform in 199613. All management and facility levels (including national programs) follow this cycle. An annual review of the national program is conducted in February, with goals and activities subsequently developed. In line with the budget cycle of the Ministry of Finance, the first budget submission is undertaken in June. The plan and budget are reviewed at the end of the year, in preparation for implementation the following January. Frequently, revisions are required to the plan in December based on the revised budget envelope of the Ministry of Finance, updated information on international funding from donors, and shifts in national priorities and strategies with regard to the most recent health information.
REFORM 2: Developing multiyear and financial sustainability planning
One of the main challenges for national program planners is to coordinate this range of national and international funding sources. To this end, NIP planners have coordinated central-level donor plans, so that each of these forms a sub-component of the overall MYP for immunization. There is no separate disease elimination or control plan from an international source that is not integrated within the framework of the overall national program plan. Working toward a comprehensive NIP plan and a shared monitoring framework is a key element of success in resource coordination, particularly in terms of reducing overlap of donor commitments.
In 2002, with technical assistance supported through the GAVI Alliance, Cambodia was one of the first countries to develop an FSP for immunization services. The financial projections of this plan indicated a rise in costs from US$4.7 million in 2002 to US$7.15 million in 200414. This is largely attributable to the introduction of new vaccines (100% of districts having introduced combined hepatitis B-diphtheria-pertussis-tetanus vaccine) and new technologies within the cold chain, syringes, and waste management systems. Specific technology innovations have included: (i) introduction of auto-disposable syringes for all immunizations; (ii) installation of gas-powered refrigerators at all health centers across the country; and (iii) installation of waste incineration systems at most health districts.
The contribution of government funding to the NIP as a proportion of overall funding has kept pace with the overall growth in immunization program costs. Equally importantly, the program is mobilizing additional international resources to support the attainment of program objectives.
REFORM 3: Strengthening national decision-making structures and processes
In general, the key elements for enhancing the quality of program management include strong skills in leadership, organization, resource allocation, and human resource management. Improvements in resource coordination and mobilization require application of these functions and skills by senior program planners. Figure 2 provides a summary of some of the complex and varied program initiatives undertaken by the NIP to improve program management in recent years, some of which have been documented in the international literature.

Figure 2: Reorganization of decision-making structures and processes in Cambodia. NIP, National Immunization Program.
Organization: Among the most important factors for undertaking this set of complex management tasks is the development and function of effective planning forums. The NIP established three main planning forums to support management policy making, resource coordination, and planning development.
The first of these forums is a national-level technical working group, which serves to strategically identify, implement, and monitor key national priorities in immunization management. It also enables effective mapping of national and international resources to ensure that there is no overlap of resourcing and that resources are targeted for maximum impact. The technical working group forum is supported by a higher level Immunization Coordination Committee, which is composed of representatives from the major investors in the immunization program (Ministries of Finance and Health and international donors). This group monitors the strategic direction of the NIP, but is not directly involved in operations. Sub-nationally, the central-level NIP engages provincial and district health directors (with civil society participation) in annual and mid-term reviews, so that regular two-way communication occurs between central-level policy direction and sub-national priority setting.
REFORM 4: Widening stakeholder participation in planning
Private sector and civil society: The development of the private and civil society sectors is now complementary and, in some cases, overtaking the role of the public sector in healthcare provision. Cambodia has the highest per capita out-of-pocket expenditures for healthcare provision (over 10% of GNI). Clients in two-thirds of cases turn first to private providers in the event of illness16. In a research study of 123 private providers in four Cambodian cities, 63% of facilities surveyed provide immunization services17. The current database of Medicam, Cambodia's umbrella health organization for nongovernmental organizations (NGOs), lists 111 organizations in the health sector18. This high prevalence of private-sector provision and civil society support for immunization provides significant opportunities and challenges for NIP planners in terms of quality control, resource coordination, and stakeholder participation in planning.
Immunization planning and health system strengthening: One of the major lessons of the first phase of the GAVI Alliance (2000-2005) was that some constraints to improved immunization performance are not immunization program-specific-they are mostly health system-wide19. That is, limitations in financing and human resources, obstacles to management and organization of health services, poor community demand for services, and weak infrastructure (transport, facilities, logistics) are weaknesses within the broader health system that contribute to limited immunization performance in rural areas.
Other health system-wide constraints include very low remuneration for health workers at the primary level of care and a high dependence on outreach health services (80% of all vaccinations given) in order to reach program coverage goals. The hard-to-reach characteristics of the population are exacerbated by the fact that 80% of infants are born in village homes, most often without the care of a skilled health provider. This remains a significant system barrier in terms of access to births and deaths information, which is critical for both neonatal tetanus elimination and the postnatal provision of a birth dose vaccine to newborn infants (administered within 24 hours of birth).
An additional constraint is the irregular financing of health services at the primary level of care. A recent international immunization review indicated an average of 5.5 months' delay in provision of basic operational costs to facilities20. Although financial sustainability planning has demonstrated to the government the resource needs and gaps of the immunization program, an advocacy or analytic strategy has not been applied at the country level to demonstrate to investors the economic and social benefits of immunization programs.
REFORM 5: Strengthening service micro-planning
The coverage improvement planning (CIP) strategy is another example of the use of a micro-planning process to support improved service delivery performance. (Micro-planning refers development of an operational map of the health district or health centre catchments, in order to determine unreached populations, and which population will be reached by fixed facility and which populations will be accessed by outreach services or other kind of mobile service)21.
Based on the strategy employed by WHO's Reaching Every District program, managers and advisers a central level review national data at the end of the third quarter each year and then target distribution of funds from NGOs and GAVI Alliance operational funds to the areas of greatest needs (eg the highest numbers of unimmunized) in the country. Following the introduction of CIP in 2003, immunization coverage rose in 8 out of 10 pilot districts in one year. The mean increase in DPT3 coverage across pilot districts on an annual basis was 16%. Similar strategies have been applied in immunization campaigns in recent years, with 95% coverage targets achieved through a combination of district and health center level micro-planning, local authority stakeholder engagement, and strengthened monitoring of performance (National Immunization Multiyear Planning Workshop, Cambodia National Immunization Program, unpublished data, 2006).
However, the practice of micro-planning is not widespread. Our observational analysis of sub-national integrated health plans demonstrates that the plans are not often driven by the evidence of public health data (such as births, deaths, and immunization coverage data). Most plans are descriptive of activities and costs. Information on births, deaths, reportable diseases, and drop-out rates are not very visible in plans below the national level. The analysis of this data is essential for program managers to design effective interventions to reduce maternal and infant deaths, identify locations of high risk, and identify areas of low service access.
Plans for surveillance activities are highly disease-specific and emphasize early detection and response for neonatal tetanus, polio, and measles outbreaks. Coverage data is aggregated at the levels of the health center (population 10 000 to 15 000), district (population 100 000), and province (population 30 000 to 300 000), but no surveillance or monitoring data is analyzed or available at the microlevel to detect pockets of unimmunized populations. High immunization drop out rates between 20% and 30% (from BCG vaccine in the first month to measles vaccine in the ninth month) were detected in remote provinces in 2004, but this information is not being analyzed routinely at subdistrict or health-center levels. This limits opportunities for managers to plan a strategic response. Under the current system, managers often only become aware of the existence of these populations when coverage surveys are conducted or when a disease outbreak occurs.
What the above reforms have demonstrated is that there is an association between improved planning performance and enhanced management performance, particularly in terms of improved resource coordination and mobilization, alignment of immunization with national and international health goals, and increased stakeholder participation in planning. On this basis, it is reasonable to conclude that enhanced management performance has been a contributing factor to recent rapidly improved immunization coverage in Cambodia.
Next steps in the development of National Health Program planning capacity
Despite significant gains in recent years (as demonstrated by the demographic health survey results alluded to earlier), Cambodia will still need to make significant progress in order to achieve regional disease elimination goals for such vaccine preventable diseases as hepatitis B, measles and neonatal tetanus. Figure 3 demonstrates Cambodia coverage of measles vaccine in relation to other countries in the region.
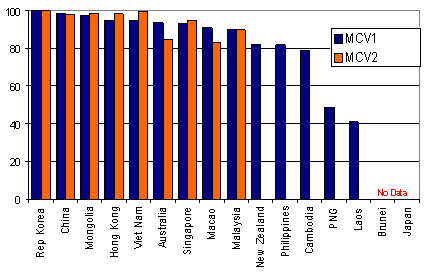
Figure 3: Measles coverage western Pacific region. MCV 1, measles 1st dose; MCV 2, measles 2nd dose. Data source: WHO Manila Technical Advisory Panel Meeting, Manila, The Philippines; 2006.
The following discussion will focus on how planning can be further strengthened through health system and civil society coordination and engagement. We will then conclude with a discussion of the implications of these developments for the future of health planning in Cambodia.
Strengthening sub-national health planning and epidemiological skills
Routine disease surveillance systems have demonstrated the capacity in countries such as Cambodia to rapidly detect disease events that then enable a planning response from national to local levels. The sharp declines in measles and tetanus incidence alluded to earlier is good evidence for this. These surveillance systems may also provide a platform for developing a routine micro-planning strategy to detect and develop responses at the facility level. Capitalizing on this opportunity will require the development of analytic, local-area epidemiological skills among district and health center managers.
Local-area planning also provides the opportunity for provincial and district planners to undertake more coordinated maternal and child health approaches. GAVI Alliance support for facility-level microplanning toward improved immunization performance, for example, may miss a significant opportunity by not embracing a wider public health agenda. Microplanners identify unimmunized children in data sets and record these numbers on catchment maps. They then can determine causes and develop solutions to reach the unreached. But equally important, for example, is the identification of mothers who have failed to access services for safe delivery or antenatal care, low acceptor rates for birth spacing, rates of tuberculosis treatment completion, or areas with low consultation rates for childhood respiratory conditions and diarrhea. An integrated, local-area planning approach would help address the collection of such data and support routine responses.
Developing a benefits analysis for health planning
The role of financial sustainability planning in costing, resource gap analysis, policy review, and advocacy in Cambodia has been outlined in detail elsewhere. An advocacy strategy that demonstrates resource gaps does not sufficiently highlight the benefits of interventions. In other words, the FSP process demonstrates resource cost (for example cost per vaccinated child), but what are the broader public health benefits associated with this investment?
The lack of an economics or public health benefits analysis exposes program plans to the high risk of being viewed as a public liability rather than a public investment opportunity with demonstrated impacts on economic growth. In the case of immunization planning, recent economic analysis demonstrates that the annual financial return on immunization is 18% - equivalent to investment in basic education22. A more thorough analysis of death and disability averted, hospitalizations prevented, and the role of immunization in economic development is likely to become a critical requirement for sustained public investment in immunization. This is especially the case given the increasing role of Departments and Ministries of Planning and Finance in making assessments of social sector priorities.
Figure 4 illustrates an example of a benefits analysis of the impact of an immunization program at the country level. This approach can strengthen advocacy efforts by contrasting the investment information (resource and costs analysis) with the outcomes information (public health, social, and economic impacts of investment), in order to give decision-makers a more balanced assessment of the costs and benefits of interventions.

Figure 4: Examples of a benefits analysis of immunization programs in Cambodia Sources: Royal Government of Cambodia National Immunization Program, Ministry of Health. Hepatitis B sero survey. Unpublished report, 2004; also23,24.
Country-level assessments could be combined into a powerful public health, social, and economic rationale for investment in immunization at a country level. This should be an integral component of the situation analysis in multiyear planning.
Rethinking the culture and organization of national program planning
As discussed, Cambodia has been undergoing a process of political, social, and economic reform in recent years15,25. Chief among the political reforms is the process of decentralization, whereby elected commune councils are taking on increasing roles of public service management in areas such as rural development. Administrative decentralization is also underway, with provincial health departments assuming additional roles in areas of planning and financing for health programs. The country's shift from a state-controlled to a private-sector economy has been ongoing for the last 15 years. There is now a thriving but unregulated private health sector, which is rapidly developing in urban areas in particular.
The NIP has responded to the challenges resulting from such development and has undertaken a range of responses to harmonize the implementation of national program planning with social change (Fig 2). Through these activities, it has become clear that keeping pace with social change involves reshaping the organization and culture of national program planning.
The culture of planning
National program planning is vertical by tradition - and this has arguably been one of its great strengths. The ability to centrally direct and manage resources toward targeted objectives has produced some significant public health achievements, including the certification of Cambodia as polio-free by WHO and, as described earlier, sharp reductions in the incidence of measles.
However, current trends involving health systems and social development have begun to impact on the character of national program planning. These include an increase in international partnerships, political and administrative decentralization, the expansion of the private sector, the decline of socialist health systems, and the associated development of civil society. Such social and system changes are exposing national programs to external societal and political pressures as never before.
Previously, a secure international financing environment and centrally-directed program management structure provided some protection for national programs from these external pressures. But in the current era of governance and health sector reform, this is no longer the case. When financial, human resources, and logistical systems are increasingly influenced by partners outside the control of national program managers, the national program is at higher risk of plan failure. These outside constituents include departments of finance and planning, private sector interests, civil society organizations, and sub-national planners, each of whom would not prioritize immunization objectives in the same manner as a national technical manager.
Given the growth of outside participation in planning, maintaining immunization as a country priority will require effective communication with these stakeholders regarding public health evidence on the epidemiology of preventable disease and the health benefits of related interventions. The same approach applies to planning for other health programs.
Civil society development does, however, present significant opportunities to program planners for resource mobilization and health advocacy. Mass media and religious leaders are increasingly influencing public attitudes toward health-seeking behaviors. Additionally, the participation of NGOs in health and social service delivery provides significant opportunities for national and sector program managers to mobilize additional resources for health, particularly at service delivery points in rural areas. Figure 5 illustrates the integration of these sectors in the overall provision of health care26,27.
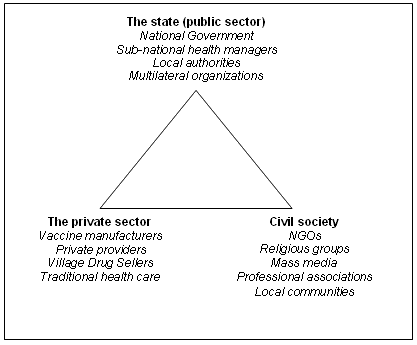
Figure 5: A framework of the health care system incorporating three sectors.
Within this broader definition of the health-care system, it is critical for national program planners to thoroughly analyze and engage stakeholders in program planning to ensure that resources are coordinated and targeted to areas of greatest need. Unlike vertical program management under socialist health systems, these stakeholders cannot be controlled solely by a national program. The challenge for national program planners, therefore, is to shift from a culture of control to a culture of influence. This will require developing partnerships with these outside stakeholders in order to achieve shared goals.
The organization of planning
Making a shift in planning methods will necessitate alterations in the organization of planning. A vertical or nationally-controlled approach to planning concentrates decision-making in the hands of technical experts (such as immunization technicians). The shift to an influence-driven and less directive culture would mean that planning is organized along the lines of partnership and collaboration (with international agencies, government departments, and local authorities), delegation (provincial health departments) and, in some cases, regulation (private sector).
Economic and social trends toward decentralization and privatization indicate that immunization is already becoming less subject to direct national control. Given these changes in the external environment, the challenge for NIP planners is to negotiate effectively with sector planners (eg in the Department of Planning), financiers (Department of Finance and provincial health departments), and civil society constituents to ensure there is a match between immunization objectives and operational resource requirements and standards.
NIP planners have approached this organizational challenge in a number of ways. Firstly, the NIP established national and sub-national planning forums to engage international, political, and sub-national stakeholders in planning development and review. The dialogue that has been initiated and/or strengthened between the NIP and sub-national political leaders, NGOs, and private-sector stakeholders illustrates that planners are now becoming increasingly aware of the new organizational and cultural environment in which public health programs are being managed and implemented.
Other analysts have noted that the elements of a strong policy and planning approach combine application of technical skills with recognition of planning as a political process28,29. Feasibility of implementation, particularly in countries developing more pluralistic social models, is dependent on both the rationality of technical objectives and the capacity to coordinate, regulate, and influence a range of investors and providers from public, private, and civil society sectors.
In the final analysis, the success of planning is reflected in the plan's implementation and in achieving a match between community health needs and public health investment, and in this case in improved immunization coverage and declines in vaccine preventable disease incidence. The ways in which planners influence and coordinate investors and providers toward shared technical and organizational goals based on sound epidemiological evidence is the key to planning success, and reflects the emerging roles of the state in developing countries as financiers and regulators - and not just providers - of public health care.
Conclusion
Recent social and health sector reforms, accompanied by the development of civil society, have changed the character of national health program planning in Cambodia. National program planning is now linked to health sector planning systems. Decentralization has resulted in the necessity for national program planning to involve sub-national political leaders in program advocacy and sub-national health managers in planning and financing. Non-governmental organizations are increasingly becoming a central component of planning strategy. The expansion of the private health sector has resulted in the initiation of a dialogue between private practitioners and the public sector in support of improved quality of care. Increasing program costs are also being successfully managed by the NIP through the mobilization of national and international resources for immunization, and this may encourage or support similar approaches for other national health programs. Improved health outcomes have been recorded, illustrated by sharp declines in disease incidence and a sharp increase in immunization coverage. The NIP has adapted the organization and culture of planning to the new social and institutional context. In doing so, the program has positioned itself well to take on additional challenges in coming years associated with expanding international partnerships, the continued development of civil society, further health system decentralization, and the requirement to further improve coverage in support of disease elimination goals. However, as costs continue to rise, planners in the future will need to emphasize the economic and public health benefits of immunization programs in order to sustain increasing levels of national and international investment.
References
1. Royal Government of Cambodia. Royal Government of Cambodia national strategic development plan 2006-2010. Phnom Penh, Cambodia: Royal Government of Cambodia, 2006.
2. Ministry of Health. National health sector strategic plan 2003-2007. Phnom Penh: MOH Phnom Penh, 2003.
3. National Institute of Public Health, Ministry of Health Cambodia. Demographic health survey 2005. Phnom Penh, Cambodia: MOH, 2006.
4. Royal Government of Cambodia Ministry of Health. Ministry of Health guidelines for operational districts. Phnom Penh, Cambodia: MOH, 1997.
5. Royal Government of Cambodia Ministry of Health and Ministry of Planning. Ministry of Health planning guidelines. Phnom Penh, Cambodia: MOH, 2002.
6. Royal Government of Cambodia Ministry of Health. Health sector strategic plan 2003-2007. Phnom Penh, Cambodia: MOH, 2003.
7. Soeung S, Grundy J, Ly CK et al. Improving immunization coverage through budgeted micro-plans and sub-national performance agreements: early experiences from Cambodia. Asia Pacific Journal of Public Health 2006; 18: 29-38.
8. Soeung S, Grundy J, Biggs BA, Boreland M, Cane J, Samnang C et al. A management systems response to improving immunization coverage in developing countries: a case study from Cambodia. Rural Remote Health 4: 263. (Online) 2004. Available: Rural and Remote Health (Accessed 3 May 2007).
9. Men B, Grundy J, Cane J et al. Key issues relating to decentralization at the provincial level of health management in Cambodia. International Journal of Health Management and Planning 2005; 20: 3-19.
10. Soeung S, Grundy J, Ly CK et al. Improving immunization coverage through budgeted micro-plans and sub-national performance agreements: early experiences from Cambodia. Asia Pacific Journal of Public Health 2006; 18: 29-38.
11. WHO Office of the Western Pacific Region. Fifteenth Meeting of the Technical Advisory Group on the EPI and Polio Eradication in the Western Pacific Region. (Online), 2005. Available: WHO Office of the Western Pacific Region (Accessed 3 May 2007).
12. UNICEF, WHO, UNFPA. Maternal and neonatal tetanus elimination by 2005: strategies for achieving and maintaining elimination. (Online) 2000. Available: UNICEF, WHO, UNFPA (Accessed 3 May 2007).
13. Ministry of Health. Health Planning Guidelines 2002. Phnom Penh; MOH, 2002.
14. Soeung S, Grundy J, Maynard J et al. Financial sustainability planning for immunization services in Cambodia. Health Policy and Planning 2006; 21: 302-309.
15. Men B, Grundy J, Cane J, Rasmey LC, An NS, Soeung SC et al. Key issues relating to decentralization at the provincial level of health management in Cambodia. International Journal of Health Management and Planning 2005; 20: 3-19.
16. Royal Government of Cambodia Ministry of Planning. Ministry of Planning Demographic and Health Survey Cambodia. Phnom Penh, Cambodia: MOP, 2000.
17. Royal Government of Cambodia National Immunization Program. Research study private sector immunization practice. Phnom Penh, Cambodia: NIP, 2006.
18. Medicam. Medicam: The membership organisation for NGOs active in the health sector in Cambodia. (Online) 2006. Available: Medicam (Accessed 26 July 2006).
19. GAVI Alliance. Achieving our immunization goal 2003, final report. Geneva, Switzerland: GAVI Alliance; 2003. Available: Achieving our immunization goal (Accessed 3 May 2007).
20. National Immunization Program, WHO, UNICEF, PATH. Expanded programme review. Phnom Penh, Cambodia: Ministry of Health, 2005.
21. WHO. Immunization in practice. A practical guide for health staff Geneva: WHO, 2004.
22. Bloom D, Canning D, Weston M. The value of vaccination. World Economics 2005; 6: 15-39.
23. Touch, S. Japanese encephalitis in Cambodia: disease surveillance. In: Proceedings, Biregional Japanese Encephalitis Meeting. 30-31 March 2005; Bangkok, Thailand, 2005.
24. Bresee JS, Hummelman E, Nelson EA, Glass RI. Rotavirus in Asia. Journal of Infectious Diseases 2005; 192(Suppl 1): S1-S5.
5. Royal Government of Cambodia Council for Administrative Reform. Governance action plan. Phnom Penh, Cambodia: CAR, 2000.
26. Jareg P, Kaseje D. Growth of civil society in developing countries: implications for health. Lancet 1998; 351(9105): 819-822.
27. WHO. Why health systems matter. (Online) 2000. Available: World Health Report 2000. (Accessed 3 May 2007).
28. Green A. An introduction to health planning in developing countries, 2nd edn. Oxford, UK: Oxford University Press, 2002.
29. Walt G, Gilson L. The central role of policy analysis. Health Policy and Planning 2002; 9: 353-370.
