Introduction
Videoconferencing is now a firmly established feature of rural health care in Australia. There are numerous examples of programs that use videoconference to slash the barriers of distance, small population sizes and workforce shortages by offering specialist consultations, supervision of remote staff, routine meetings of disperse team members and the delivery of continuing professional education1,2. However, videoconferencing has not been used as extensively outside the provision or support of traditional health care3.
Rural communities have, on average, a higher proportion of older people than is found in major cities4. Caring for older residents who cannot live independently is becoming an increasing priority for health services, local governments and, most importantly, family members. There is compelling evidence that support programs for carers of family members with disabling conditions increase carers' health and wellbeing and their capacity to continue in the caring role5-9.
Description of program
The Carers Support and Education Project was the first project of its kind in Australia to offer education, practical advice and opportunities for networking to rural carers using the technology of videoconferencing10. The project encompassed the Midwest, Murchison and Gascoyne regions of Western Australia, an area approximately the size of the state of Victoria, located 400-900 km from the capital city Perth. Approximately 70 000 people live in this region, with 30 000 in the regional centre Geraldton.
The basic program consisted of a two-hour session facilitated by an educational psychologist based in Perth, an expert in supporting carers and other volunteers. Sessions started with icebreakers, which engaged all the participants. Each carer then spoke individually, describing for whom they were caring, and identifying their main areas of concern while other participants listened. Some sessions also included small group discussions of how to solve particular problems.
The facilitator delivered the sessions from the videoconference facility managed by the Western Australian Country Health Service. Videoconferencing is the transmission of images (video) and speech (audio), between two or more locations. Some of the videoconference units could only transmit the video and audio over digital phone lines known as ISDN (integrated services digital network); whereas, other sites were also able to use a local area network using IP (internet protocol). Up to three sites (towns) participated in any one session, with a median attendance of six (range 1-18). The videoconferencing facilities for each rural site were in the health service or at a local telecentre.
The regional Telehealth Coordinator (first author) and the Midwest Commonwealth Carer Respite Centre Coordinator coordinated the program. Local Home and Community Care (HACC) coordinators promoted the sessions to carers in the rural towns. From the program's inception in June 2004 to the end of 2005, there were 21 videoconference sessions involving 12 towns and 146 carers. All participating towns are mapped (Fig 1). Towns have had between one and four sessions and many carers have participated in two or more sessions.
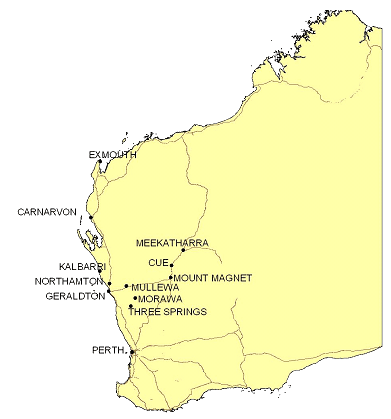
Figure 1: Locations of Western Australian rural sites participating in the carers program.
Evaluation data and methods
In mid-2005 the first author was awarded a primary health care research fellowship to evaluate the carers program. The research protocol was approved by the Human Research Ethics Committee of The University of Western Australia.
Because the program was a pilot, this evaluation used semi-structured interviews to explore participants' and service providers' perceptions. Semi-structured interviews are an efficient way to gain information on topics relevant for the evaluation, while still giving respondents the opportunity to express their thoughts in their own words11. To ensure reliable and comparable data, formal question lines were developed that were similar for carers and service providers. Respondents were asked to describe their previous experience with videoconferencing, and discuss the relevance and value of sessions, raise practical issues related to the use of technology, and describe any changes in behaviour.
To maximise the diversity of experiences while retaining representativeness, the first author conducted interviews with carers and HACC coordinators. The eight carers who were interviewed were randomly selected from attendance lists from four of the 12 participating towns. The four towns were selected purposively to achieve diversity in population size, number of sessions held and average number of participants. Seven of the initially selected carers agreed to participate; one carer was unavailable during the study period and was replaced by another carer identified in the same way. Of the eight carers, seven were caring for a spouse and one was caring for her mother. Two carers were male. Four of the eight carers were providing care to someone with dementia, while the other care recipients had a range of medical conditions resulting in them requiring care.
Handwritten notes were taken during the interviews and expanded immediately afterwards. Audiotapes were used to check the accuracy of the notes. Interviews lasted 30 to 45 min.
Because this was an evaluation of a pilot, we coded the data into evaluation domains: process (quality of the sessions and the videoconference), impact (attendance, knowledge gains), and outcomes (changes in behaviour by carers and service providers). Next, within each domain, we used inductive coding to identify and refine themes by comparing and contrasting the text within the groups of carers and service providers and between carers, providers and the facilitators11,12. Both authors were involved in the analysis. The results presented in this article emerged from themes that appeared in virtually all interviews and had consistent or reinforcing meanings within and across carers, service providers and the facilitator.
Results
In this article we report our findings in relation to the acceptability of the videoconferencing technology, and perceived impact of the program on carers and the health service.
Acceptability of technology
Even though the facilitator and carers had no experience of videoconferencing prior to the program, all but one carer expressed great satisfaction with the quality of interaction. Several carers commented it was like having the presenter in the room, and even those with hearing or vision impairments were able to participate fully. One carer suggested that carers actually 'seemed to share more with someone being distant'. The theme that videoconferencing was an improvement over face-to-face interactions was echoed by the facilitator, who said:
In fact in a lot of ways it was like being in the room and even better not being in the room as people did not feel threatened by you physically being there, but as long as you could see people to pick up the non-verbals it was an excellent medium to do an interaction group discussion type process.
Claims that the technology inhibited related to circumstances when multiple sites were involved. A local HACC coordinator thought that some carers were not able to participate fully when there were two or more towns involved; however, she was the only rural respondent who mentioned this as a problem. The facilitator's dissatisfaction with multipoint videoconferencing was overcome by switching to a system that enable her to simultaneously view all sites.
Impact and outcomes on carers
The program was initially conceived and promoted as an educational intervention, in which carers would learn coping skills from an expert. All carers stated that the desire to 'learn' how to give better care to their family member was their major reason for attending session. The facilitator used learning aids such as a 'stress tips' handout to provide this information. Therefore, during the interviews carers were asked if they had displayed the 'stress tips' and probed for what content they remembered. Of the six carers who received the laminated tips, five were very positive about their value. They had displayed their sheet on the refrigerator and found the tips to be helpful, and recall of the messages was good.
'Sharing' was a key theme to emerge relating to perceived value of the program. According to the carers, sharing occurred when they related the problems they were experiencing to the facilitator and when they listened to other carers describing their emotions. Experiences such as guilt and its associated anger and frustration, and stress in having to be available to respond to the care recipient's every need were common themes. Even carers who were reticent about sharing their experiences explained in the interviews that they had gained from the sharing that occurred in the sessions. A typical comment was, 'Sharing with others was a good thing even though I said I'm a bit uncomfortable with that...it was a good thing being able to share'. The facilitator had intentionally reinforced the value of learning from others by stressing that the coping strategies she recommended had originally been suggested by other carers with whom she had worked; they were 'by carers and for carers.'
Through sharing, that is by hearing others express the same concerns and by observing or participating in finding some practical solutions, participants gained the skills or confidence they need to make changes. Five carers described small behaviour changes. For example, one man had been considering selling his tools; he explained that his shed was where he went to relax. Encouraged by the facilitator and other participants, he said he decided not to sell his tools and still enjoys using his shed. A woman stated she had learned to live more for the moment and following the session asked for respite care for her husband when she needs a break. Another had started to have some time for herself and enjoyed an outing with a friend. A fourth stated that she had the courage to say no to her mother and not feel guilty. The final change reported was from a woman who stated she now gets out into the garden a bit more and that she had been more relaxed since the sessions. Even the carer who had been very definite during the interview that she had done nothing different eagerly reported at the next session she attended the numerous changes that she had made as a result of the first session.
The facilitator, who had the advantage of seeing at least half of the carers for two or more sessions, reported that she observed many significant small behavioural changes and this was also confirmed by HACC coordinators.
Impact and outcomes on services
A theme that emerged from the interviews with HACC coordinators was the contrast in the services that the coordinator and other local health staff provided to carers, and what was offered by the sessions. Local staff explained that they performed a problem-solving role; they had a set of services, such as respite care, that they could offer and they rarely explored carers' wider family context or carers' own health and wellbeing. In the interviews, all HACC coordinators volunteered that they lacked the skills to elicit that information from carers. As one coordinator expressed it, 'Judy used skills that I do not have and I was able to tap into her resources and gain insight into my clients' lives'.
HACC coordinators recognized the importance that they 'observe and participate instead of being in my work role' during the sessions. This enabled them to gain more understanding about carers' needs and be on-hand to assist carers afterwards if a need was identified during the session. All the coordinators indicated that the sessions were very helpful in making it possible for them to offer more appropriate services to carers and care recipients, and to increase the likelihood that services such as respite would be utilized. However, the facilitator and a couple of the carers noted that some staff found it difficult to remain an observer, compromising the quality of the sessions. The facilitator mentioned one staff member who:
...spent more time trying to speak rather than listen ...to want to give solutions to situations where sometimes there isn't a solution ...that could shut down things ... and you work hard on overcoming that. It is more difficult when you cannot physically be in the room when this occurs.
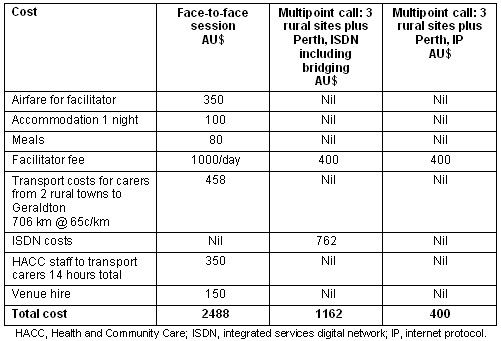
The videoconferenced sessions compared favorably to the costs of face-to-face sessions, which are typically held in the regional centre. Table 1 contrasts three scenarios. The first is a face-to-face session in which the facilitator is flown to the regional centre, and carers from two outlying towns are transported into the centre. The second and third scenarios are videoconferenced sessions to three rural sites with the facilitator in the capital city. These scenarios are only 16 to 47% of the cost of offering face-to-face sessions to the groups with the same facilitator. The difference between scenarios two and three is whether videoconferencing over IP is available. There is no charge per session for the use of videoconferencing over the internet, whereas videoconferencing over ISDN entails telephone charges.
Table 1: Comparison of the costs to deliver a face-to-face session to carers from three towns by a Perth based facilitator compared to video conference
Discussion and Conclusions
The difficult role of a carer providing care 24 hours per day, seven days per week, is increased with the challenge of living in a small rural community. Carers can access adequate support for the physical needs of their care recipient through the local health services, but there is a gap in the provision of psychosocial education and support.
In the course of this evaluation we came to understand the truth of the conclusion of a recent Cochrane review on the effectiveness of telehealth care: telehealth services are not merely the replication of services as they are given face-to-face, but rather offer care which is fundamentally different13. Videoconferencing offered facilitated interaction between carers at substantially less cost than face-to-face sessions. The small behaviour changes reported to have been made by carers suggests that this intervention was comparable to other programs reported in the literature that improved carers' quality of life and psychological functioning through 'sharing' with peers and a facilitator in face-to-face sessions6,8,9. However, all respondents also indicated advantages of videoconferencing beyond those of cost and convenience. The facilitator found that the technology enhanced her ability to monitor group and individual non-verbal cues. Local service providers said that videoconferenced sessions improved the quality of local services by raising support needs that they did not have the skills to identify. Finally, participants shared with peers in the same and neighbouring towns in ways that they had never done before, partly because the videoconferencing provided intimacy at a safe distance. Dissatisfaction with the program was associated with times that the technology impeded smooth interaction between multiple sites, and when local staff tried to assert their service-oriented solutions during the sessions.
The use of videoconferencing technology has enhanced the existing services across the Midwest, Murchison and Gascoyne region of Western Australia, by providing support and networking opportunities for carers at a modest cost. Partly as a result of this evaluation the program is continuing. Future evaluations of the mature program should be designed to provide more objective data on changes in psychosocial functioning and use of health services, drawing on statistically representative samples to provide evidence on the individual and program features associated with greater enrolment and retention of carers and indicators of carers' and care recipients' wellbeing.
Telehealth represents enormous promise for rural and remote populations. Videoconferencing, in particular, offers a mechanism to enable healthcare providers and patients to interact with each other without the costs of travel or the constraints of small numbers of potential clients in each locality. Studies have shown consistently that healthcare providers and rural patients are very satisfied with videoconference consultations, with clinical outcomes equal to face-to-face consultations at a lower total cost10. The rural carers' support program shows that expanding the use of videoconferencing for health promotion and preventative health care has great potential.
Acknowledgements
The authors would like to acknowledge the support from many people both during the project and the research.
- HACC coordinators and telehealth champions across the Midwest Murchison and Gascoyne area of Western Australia together with WACHS head office who embraced the idea and provided technical assistance and support.
- Midwest Commonwealth Carer Respite Centre who provided funding for the project.
- Dr Judy Esmond, facilitator of the carer sessions, for her energy, compassion and enthusiastic support of the concept.
- The carers, who so openly shared their lives with both Dr Esmond and all attending the videoconference sessions and gave permission to be interviewed for this research.
- Combined Universities Centre for Rural Health who awarded a research fellowship that enabled this evaluation to be conducted, through funding from the Primary Health Care Research and Evaluation Development initiative of the Australian Department of Health and Ageing.
References
1. Dillon E, Loermans J, Davis D, Xu C. Evaluation of the Western Australian Department of Health telehealth project. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): 19-21.
2. Ellis I. Is telehealth the right tool for remote communities? Improving health status in rural Australia. Contemporary Nurse 2004; 16: 163-168 (Editorial).
3. Scott RE. Expanding the sphere of influence of e-health to determinants of health. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): 111-112.
4. Larson A. Rural health's demographic destiny. Rural and Remote Health 6: 551. (Online) 2006. Available: http://rrh.org.au (Accessed 29 January 2007).
5. Millan-Calenti JC, Gandoy-Crego M, Antelo-Martelo M, Lopez-Martinez M, Riveiro-Lopez MP, Mayan-Santos JM. Helping the family carers of Alzheimer's patients: from theory...to practice. A preliminary study. Archives of Gerontology and Geriatrics 2000; 30: 131-138.
6. Toseland RW, Rossiter CM, Labrecque MS. The effectiveness of peer-led and professionally led groups to support family caregivers. The Gerontologist 1989; 29: 465-471.
7. Gitlin LN, Belle SH, Burgio LD, Czaja SJ, Mahoney D, Gallagher-Thompson D et al. Effect of multicomponent interventions on caregiver burden and depression: The REACH multisite initiative at 6-month follow-up. Psychology and Aging 2003; 18: 361-374.
8. Belle SH, Czaja SJ, Schulz R, Zhang S, Burgio LD, Gitlin LN et al. Using a new taxonomy to combine the uncombinable: integrating results across diverse interventions. Psychology and Aging 2003; 18: 396-405.
9. Stoltz P, Uden G, Willman A. Support for family carers who care for an elderly person at home - a systematic literature review. Scandinavian Journal of Caring Sciences 2004; 18: 111-119.
10. Van Ast P. Supporting community carers via videoconferencing. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): 96-97.
11. Bernard HR. Social research methods: qualitative and quantitative approaches. Thousand Oaks, CA: Sage, 2000.
12. Miles M, Huberman A. Qualitative data analysis. Thousand Oaks, CA: Sage, 1994.
13. Currell R, Urquhart C, Wainwright P, Lewis R. Telemedicine versus face to face patient care: effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews 2000, Issue 2. Art no: CD002098. DOI: 10.1002/14651858.CD002098.

