Introduction
Diabetes and the Navajo
The Navajo nation, with over 250 000 members1, is the largest federally recognized tribe within the USA, encompassing nearly 70 000 km2 within parts of three states: Arizona, New Mexico, and Utah (Fig 1). The reservation is larger than 10 of 50 of the United States1. Most of the Navajo nation is extremely remote and rural, and many Navajo live in isolated family clusters. The region is semi-arid although there are significant rangelands, forests and irrigated farmlands. The median age of inhabitants is 22.5 years2.
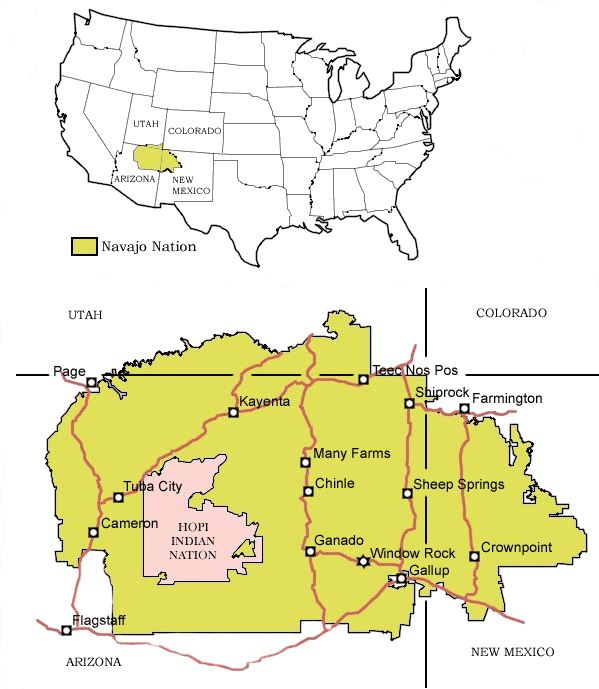
Figure 1: Map of the Navajo nation (not to scale).
Type-2 (non-insulin dependent) diabetes and the associated cardiovascular disease (CVD) risk are on the increase in the USA. Indigenous American people, including the Navajo, have been particularly hard hit by this trend. In an 8 year period alone, from 1990-1997 the prevalence of diabetes rose 29%3. Diabetes is not in the Navajo tradition. Called 'the sugar illness', the historical progression of diabetes is correlated with colonization by westward expansion of the USA in the 1800's, and often poor federal policy toward Indigenous people that resulted. Gradual shifts away from traditional diets, active lifestyles including hunting, farming, and herding, and adoption of a more Anglo-American diet began to occur4. Past federal nutrition guidelines advocating meaty, cheesy foods, criticized for not taking into account traditional diets, exacerbated the dietary transitions of the Navajo4,5. Further, the contemporary rise in consumption of nutrient poor, sugary, processed, and 'fast foods' of convenience (foods often containing large amounts of trans- and saturated fats), in combination with low intakes of fruits/vegetables and sedentary lifestyles have produced disastrous health consequences4,6-10. For example, the number of reported cases of type-2 diabetes in the Navajo increased from one person out of 6000 in 1937 to 21-23% of the population aged 20 years and older in 1997, or more than 4 times the rate found in the general US population11,12. More than 40% of Navajo adults over 45 years are diabetic, yet one-third of this group is unaware of their diabetic condition13. Navajo with diabetes are 2.8 times more likely to be overweight, 2 times more likely to be sedentary and are more likely to suffer premature death related to CVD than their non diabetic counterparts6,11,14-17. A huge concern among this group is the number of children, adolescents, and young adults (<15-24 years) who are receiving diagnoses of diabetes. The prevalence of diabetes in this population increased by 46%, from 6.4 per 1000 to 9.3 per 1000 between 1990 and 199818 - more specifically, adolescents aged 15-19 years saw an increase in diabetes rates of 106% between 1990 and 200120.
The importance of physical activity and healthful eating habits need to be encouraged by families and communities when children are young, allowing them to carry positive health behaviors into their adult lives13. Poor dietary habits developed in childhood including unfamiliarity with fruit and vegetables in the diet increase the risk of diabetes in adulthood15,20. This was reinforced in the most comprehensive survey of Navajo health and nutrition where fruit and vegetable consumption were noted as low: consumed less than once, per person, per day7.
The rise in diabetes among the Navajo is also correlated with socio-economic status and the lack of services in remote areas of the reservation. Major limitations affecting dietary choices have been cited as: cost, availability, shelf life, and remoteness6,7. Lack of purchasing power is associated with the fact that over half of the Navajos live on a yearly per capita income of $621721 compared to the US per capita income greater than $30 00022.
A reality on the reservation is that access to quality foods, to include fresh fruits and vegetables, is often limited by the extreme remoteness of areas where Navajos reside19. Availability of fruits and vegetables on the reservation decreases with distance away from fringe cities such as Farmington and Gallup, NM. Unimproved roads predominate and large distances between communities on Navajo land mean long drives for food shopping. Isolated trading posts bridge the gap between modern grocery stores but often stock limited selections of produce provide minimal nutrition. Many Navajo homes are still without electricity. In 2000 the Energy Information Administration estimated that 36.8% of the 29 375 occupied housing units on the Navajo nation lacked electricity23. Due to this lack of electricity, home refrigeration is scarce, as are purchases of perishable foods that include some fruits and vegetables.
Why gardening in a diabetes prevention and care program?
It makes perfect sense to promote a return to gardening as a tradition among the Navajo to alleviate diabetes. The Navajo have a longstanding heritage of farming dating back to contact with Pueblo Indian communities and later the Spanish4. Consuming fruits and vegetables, exercise, and weight loss are all prescribed for diabetes management11,16,24-26. Gardening, whether in a community or home environment, is gaining popularity for inclusion in diabetes management (and prevention) for a number of reasons27-29.
First, gardeners are more likely to adopt healthier dietary habits by consuming what they produce. Indeed, a review of the scientific literature shows that consuming fruits and vegetables in modest portions provides protection against a number of diseases including diabetes30-32. The US National Cancer Institute recommends 5-9 servings of fruits and vegetables per day in their 'Eat 5 to 9 a Day for Better Health' campaign33,34 and the Native American Food Pyramid advocates 3-5 servings of vegetables and 2-4 servings of fruits per person per day35 (Appendix 1). Parents who garden are more likely to pass this knowledge onto their children36 and thus can begin to break cycles of diabetes.
Second, following the above consumption guidelines, a garden can locally produce a wider variety of nutritious food than what may be purchased at trading posts and smaller grocery stores. Traditional cultivation of several types of corn, beans, squash, watermelons, vegetables such as wild spinach or beeweed (Cleome serrulata), chili, berries from wild sumac (Rhus sp.), yucca 'bananas' (from Yucca baccata) and prickly pear cactus fruit (Opuntia sp.) among many others have been described in historical manuscripts and by tribal elders4,37. Cultivating leafy greens (such as leaf lettuce and Swiss chard), orange colored sweet potatoes, melons, and butternut squash all provide a mixture of nutritious produce. Many, if not all of these could be introduced, or reintroduced, to Navajos for incorporation into home or community garden. Although electricity is lacking in some parts of the reservation, many vegetables could be properly stored without refrigeration or canned for future consumption.
Third, gardening does not immediately come to mind as a form of physical activity. The mere mention of the word 'exercise' may elicit negative connotations that gardening does not invoke. Gardening ranked highest in exercise preference among diabetic adults and individuals who engaged in more than one physical leisure activity (including gardening) for 30 min per day, 5 days a week, improved insulin sensitivity and glycemic control and decreased the need for oral medications or insulin11,24,38. Daily activities of gardening include weeding, cultivating, irrigating, pruning, staking - activities that, for the most part, provide 'exercise'. Anywhere from 100-120 calories can be burned off in 30 min of light gardening activities, such as hand weeding; more calories burned in digging and raking39. In terms of cardiovascular health, Native Americans who engaged in gardening, among other physical activities, had increased levels of high density lipids ('good' cholesterol) over their sedentary counterparts40.
Lastly, growing food locally at home or with a group offers the potential to raise rural household income through savings on grocery requirements. Dollars are kept with the Navajo rather than leaked out through off-reservation purchases. Participants of rural home garden projects in South and East Africa acknowledged positive economic savings in not having to purchase vegetables and some actually became interested in selling produce41,42. Small gardens contribute to positive income with every $1 invested in a garden plot yielding $6 worth of vegetables (L Sime, pers. comm. 2003). Another example is a one-third hectare 0.3 ha (0.67 acre) community supported agriculture project which produced 9350 kg of vegetables and herbs at an estimated value of over US $ 20 000 in one growing season (P Pao, pers. comm. 2006). Selling excess produce to farmers markets or even to trading posts could supplement income for progressive individuals or groups.
Gardening programs: cases and components of a diabetes prevention program
A few garden/diabetes programs have been described targeting Native Americans. A 0.4 ha (1 acre) community garden addressing diabetes care in a Northwest tribe was established near the Indian Health Service (IHS) clinic, tribal government offices, and a housing complex serving tribal elders43. Forty home gardens were also established with technical assistance provided by the program. Workshops gave advice on diet, nutrition, and health care and vans transporting the elderly detoured to the garden to allow persons to pick vegetables.
Another project started on the Standing Rock Sioux Nation in North Dakota utilized elementary students to raise vegetable transplants for dozens of gardens located around the reservation44. The project first started with a demonstration plot near a high school to catch the attention of students and emphasizes the use of heirloom and native herbs and vegetables. Some of the seed was donated as part of the Native Seeds/SEARCH program45.
Miller12 describes a Navajo diabetes care program, administered by Sage Memorial Hospital in Arizona, taking a similar holistic approach: utilizing a model garden, dietician on staff, and providing information on diabetes care. The garden, which was begun in 2004, is now in its second year with expansions to the town of Burnside, Arizona (Navajo Housing Authority site and Ganado High School) (D Preckshot, pers. comm, 2006). Cooking classes are held twice per month at the hospital to give lessons on diabetes-friendly diets.
A multidisciplinary approach
A Gardens for Health project among the Navajo fosters a culturally sensitive approach in a unique semi-arid growing climate which should promote multi-disciplinary cooperation between health care givers, nutritionists, and horticultural research and extension agents working in tandem with the community, government and individuals. Healthcare workers in the region have focused on: (1) testing for diabetes; (2) treatment in the form of insulin or oral medication; (3) counseling and education on lifestyle changes; (4) promotion of exercise; (5) promotion of diabetes friendly diets; and (6) promotion of healthy food production in the form of small-scale gardens. Agricultural workers in the region have knowledge about: (1) producing crops in a difficult growing environment of low annual rainfall; and (2) crops that garner the greatest return on investment. Traditionally, these parties may not have considered cooperation, each bound to issues relevant to individual disciplines, but by working together many similarities are exposed and faster progression against diabetes can be achieved. Utilizing elements of successful cases discussed above, a Garden for Health project could be devised from specific components.
Public Health
A Gardening for Health Project presented here is based on the Health Belief Model46,47. The six constructs of the Health Belief Model, as they relate to designing a diabetes prevention and care project are identified in Table 1. Even brief individual counseling sessions of 15 min on the health benefits of fruits and vegetables can induce increased sustained consumption48. The same approach of advice given to participants by garden staff on topics such as crop selection, horticultural techniques, harvest information and explained in lay terms can sustain the garden.
Table 1: Health Belief Model Constructs as they could be used in a diabetes prevention and care program

Agronomic considerations
The principle agro-climatic barrier to growing fruits and vegetables on the Navajo nation is limited water resources. For example, mean annual rain fall in the northeastern portion of the reservation is low (208 mm)49. Crop irrigation is almost exclusively achieved using river, reservoir, or ground water and, in some cases, must be trucked in containers to homesteads50. Drip irrigation systems utilize water efficiently by precision placement of water near the plant. As such, less water is wasted, increased land area can be irrigated, and there is less weed pressure because only the crop is receiving water50.
The major limitations to adoption of drip irrigation are cost and technological inappropriateness. Home-owner drip systems are widely available at 'do-it-yourself' and hardware stores but are often cost prohibitive to lower income families while commercial systems utilize specialized equipment that may require higher water pressures than those available to typical resource-poor Navajo farmers.
Successful deployment of low cost, simple drip technology has been demonstrated in developing countries with similar agronomic and socio-economic climates found in the Navajo nation51. Manufactured in India, the KB-Drip system (for Krishak Bandhu - Bengali for 'farmer's friend') is globally advocated by International Development Enterprises52 but has had limited exposure in the USA. The principle operation of these systems is simple: an elevated water holding tank provides enough gravity pressure to drive the system. Fifty-five gallon (208 L) drums are used to store water (Fig 2) and laterals (lines of tubing that deliver water down individual crop rows) are constructed from plastic tubing (Fig 3). Punctures are made into the tubing into which microtubes are inserted to direct irrigation to individual plants (Figs 3,4). The main advantages of this system are cost, simplicity, and weed control. The cost of the system components, excluding tank, are less than US$50. However, shipping costs from India may double this cost when imported in small quantities. Bulk imports would lower total costs.

Figure 2: Typical layout of the low cost, low-tech drip system.

Figure 3: Plastic tubing used for laterals. The tubing is punctured with the hole punch. The microtube emitter is inserted into the hole.

Figure 4: Microtube emitter supplying irrigation directly to the plant.
Another agronomic barrier on the Navajo nation is frost protection during winter months which prevents year-round production of vegetable crops. Fruit trees adapted to the area are dormant during this period and out of production until spring; however, cold weather limitations for vegetable crops may be partly overcome by selecting cool-season crops tolerant of light freezes such as lettuce and members of the Brassicaceae family including broccoli, kale, and cauliflower (Appendix II,III). Other adaptations to extend the growing season of the garden into the cold season are passively heated, low-technology greenhouses or row covers that permit cultivation of a wider variety of crops out of season (Figs 5-7). Low technology greenhouses have been described for both commercial and home applications53 and designs vary as does expense54-56. Most designs utilize the basic 'hoop construction' over which UV resistant plastic is laid and secured. Unlike traditional hobby or commercial greenhouses that use natural gas, coal or electricity to provide supplemental heat during cold periods (which is cost prohibitive), heat is captured in thermal mass within the greenhouse (using black plastic mulching, water bottles painted black, or brick masonry walls among others) and released slowly at night. When outside temperatures are slightly below freezing (32°F or 0°C) inside temperatures remain slightly above freezing depending on the amount of thermal mass present within the greenhouse. Other modifications include a second layer of plastic or spun-fiber row covering placed over crops within the greenhouse to boost insulation in below freezing weather57. The 'doors' are rolled up during the day when outside temperatures are above 60°F (15°C) to vent excessive heat and closed in the late afternoon to preserve heat. The total cost for a 4 x 9 m structure was less than US$200, which is affordable in the scheme of greenhouses but may be more suitable for community gardens with pooled monetary resources.

Figure 5: Exterior of the low-tech, low-cost plastic tunnel for growing vegetables year round.

Figure 6: Interior of low-tech greenhouse; lettuce and broccoli crop pictured. The total cost for this system is less than US$200 to cover an area 4.3 x 9 m.

Figure 7: Tomato production out of season under plastic.
Demonstration
Above all, the main emphasis on any Gardens for Health diabetes program among the Navajo should be community based in order to build grass roots momentum and sustained behavior change. The success of a Garden for Health project depends first on high visibility demonstration plots near IHS clinics, tribal government offices, chapter houses, schools, churches, trading posts, spiritual gathering places, and progressive family clusters. Without the relevant parties participating, this will not become reality. To demonstrate low cost, low tech drip irrigation systems in the Navajo nation, the University of Arizona and New Mexico State University are collaborating with gardening projects at the Hubble Trading Post in Ganado, AZ and in various chapters in northwest New Mexico.
Summary
Diabetes is a serious health problem in the Navajo nation. The scientific evidence is clear: that diabetes in the Navajo Nation is largely a result of an introduced diet and shifting lifestyle. Poverty and remoteness of communities on the reservation contribute to the problem. Gardening can help. Nutritious fruits and vegetables are produced closer to home in an individual or community setting. This would increase consumption, enable physical activity in daily gardening practices, and raise rural household income by eliminating some grocery purchases while providing the potential to sell excess produce in a market garden approach. The promotion of simple low-cost drip irrigation and frost protection for year-round vegetable production should be encouraged in the semi-arid Southwestern USA as they would be important components of a comprehensive diabetes prevention and care program. Gardening is a component of diabetes care but a multi-sectored approach involving agriculture, nutrition, health, policy-makers, community leaders, schools, and individuals is required to make faster progress on curbing diabetes in the Navajo nation.
References
1. Navajo Nation. Welcome to the Navajo Nation, History. Window Rock, AZ: Navajo Nation. (Online) 2005. Available: http://www.navajo.org/history.htm (Accessed 10 October 2006).
2. Joe G. Health care in the Navajo Nation: Fact Sheet 2004. Window Rock, AZ: Navajo Nation, 2004.
3. Burrows NR, Geiss LS, Engelgau MM, Acton KJ. Prevalence of diabetes among Native Americans and Alaska Natives, 1990-1997: an increasing burden. Diabetes Care 2000; 23: 1786-1790.
4. Kopp J. Crosscultural contacts: Changes in the diet and nutrition of the Navajo Indians. American Indian Culture and Research Journal 1986; 10(4): 1-30.
5. Mihesuah D. Decolonizing our diets by recovering our ancestors' gardens. American Indian Quarterly 2003; 27: 807-839.
6. Aiello MO, Fahs PS. A secondary analysis cardiovascular mortality among rural Native American women. Journal of Multicultural Nursing and Health 2001; 7: 42-47.
7. Ballew C, White LL, Strauss KF, Benson LJ, Mendlein JM, Mokdad AH. Intake of nutrients and food sources of nutrients among the Navajo: findings from the Navajo health and nutrition survey. The Journal of Nutrition 1997; 127: 2085S-2093S.
8. Mihesuah DA. Recovering our ancestors' gardens: Indigenous recipes and guide to diet and fitness. Lincoln, NB: University of Nebraska Press, 2005.
9. Nelson KM, Reiber G, Boyko EJ. Diet and exercise among adults with type 2 diabetes: findings from the Third National Health and Nutrition Examination Survey (NHANES III). Diabetes Care 2002; 25: 1722-1728.
10. Gilbert TJ, Percy CA, Sugarman JR, Benson L, Percy C. Obesity among Navajo adolescents. Relationship to dietary intake and blood pressure. American Journal of Diseases of Children 1992; 146: 289-295.
11. Will JC, Strauss KF, Mendlein JM, Ballew C, White LL, Peter DG. Diabetes mellitus among Navajo Indians: findings from the Navajo health and nutrition survey. The Journal of Nutrition 1997; 127: 2106S-2113S.
12. Miller T. Diabetes; in Navajo country, horses and gardens to treat a scourge. The New York Times June 6, 2004; Section 15, p. 9.
13. Story M, Evans M, Fabsitz RR, Clay TE, Rock BH, Broussard B. The epidemic of obesity in American Indian communities and the need for childhood obesity-prevention programs. The American Journal of Clinical Nutrition 1999; 69: 747-754.
14. O'Connor P, Crabtree BF, Nakamura RM. Mortality experience of Navajos with type 2 diabetes mellitus. Ethnicity and Health 1997; 2: 155-162.
15. Gahagan S, Silverstein J. Prevention and treatment of type 2 diabetes mellitus in children, with special emphasis on American Indian and Alaska Native Children. Pediatrics 2003; 112: 328-348.
16. Harwell TS, Moore K, McDowall JM, Helgerson SD, Gohdes D. Cardiovascular risk factors in Montana American Indians with and without diabetes. American Journal of Preventative Medicine 2003; 24: 265-269.
17. Archer SL, Greenlund KJ, Valdez R, Casper ML, Rith-Najarian S, Croft JB. Differences in food habits and cardiovascular disease risk factors among Native Americans with and without diabetes: the Inter-Tribal Heart Project. Public Health Nutrition 2004; 7: 1025-1032.
18. Acton KJ, Burrows NR, Moore K, Querec L, Geiss LS, Engelgau MM. Trends in diabetes prevalence among Native Americans and Alaska Native children, adolescents, and young adults. American Journal of Public Health 2002; 92: 1485-1490.
19. IHS National Diabetes Program. Special diabetes Program for Indians. In: Indian Health Services. Washington, DC: US Dept Health and Human Services, Indian Health Service, Division of Diabetes Treatment and Prevention, 2004.
20. Cunningham-Sabo LD, Davis SM, Koehler KM, Fugate ML, Di Tucci JA, Skipper BJ. Food preferences, practices, and cancer-related food and nutrition knowledge of Southwestern American Indian youth. Cancer 1996; 78: 1617-1622.
21. Navajo Nation. Navajo Nation Washington Office. Navajo Nation Profile. (Online) 2005. Available: Website address http://www.nnwo.org/nnprofile.htm (Accessed 10 October 2006).
22. US Census Bureau. Personal income per capita in constant (2000) dollars\1 2004. Washington DC: United States Census Bureau, 2006.
23. Bain G, Ballentine C, DeSouzza A, Majure L, Smith DH, Turek J. Economic and social development stemming from the electrification of the housing stock on the Navajo Nation. Flagstaff, AZ: College of Business Administration, Northern Arizona University, 2002.
24. Wood FG. Ethnic differences in exercise among adults with diabetes. Western Journal of Nursing Research 2002; 24: 502-515.
25. American Diabetes Association. Diabetes learning center for the recently diagnosed. (Online) no date. Available: http://www.diabetes.org/all-about-diabetes/diabetes-learning-center.jsp (Accessed 10 October 2006).
26. Lindstrom J, Eriksson JG, Valle TT, Aunola S, Cepaitis Z, Hakumaki M et al. Prevention of diabetes mellitus in subjects with impaired glucose tolerance in the Finnish diabetes prevention study: Results from a randomized clinical trial. Journal of the American Society of Nephrology 2003; 14: S108-S113.
27. Swank A. Sowing - and reaping the rewards: Diabetes Health Magazine. (Online) 2005. Available: http://www.diabeteshealth.com/read,7,4074.html (Accessed: 10 October 2006).
28. Owen M. How gardening can weed out diabetes: PlanTea, Inc. (Online) 2006. Available: http://www.plantea.com/gardening-diabetes.htm (Accessed 10 October, 2006).
29. Diabetes Health Connection. Gardening: Diabetes Health Connection. (Online) 2005. Available: http://www.diabeteshealthconnection.com (Accessed 10 October, 2006).
30. Lombard K. Investigation of the Flavonol Quercetin in Onion (Allium cepa L.). Texas Tech University, 2000.
31. Harvard School of Public Health. Fruits and Vegetables. (Online) 2006. Available: http://www.hsph.harvard.edu/nutritionsource/fruits.html (Accessed 10 October, 2006).
32. Knekt P, Kumpulainen J, Jarvinen R, Rissanen H, Heliovaara M, Reunanen A et al. Flavonoid intake and risk of chronic diseases. The American Journal of Clinical Nutrition 2002; 76: 560-568.
33. National Cancer Institute. NCI Health Information Tip Sheet for Writers: Diet and Diseases. (Online) no date. Available: http://www.cancer.gov/newscenter/tip-sheet-diet-related-diseases (Accessed 10 October, 2006).
34. NCI. Eat 5 to 9 a Day for Better Health. (Online) no date. Available: http://www.5aday.gov/ (Accessed 10 October, 2006).
35. Hinkle A. Native American Food Pyramid. (Online) no date. Website address http://www.nal.usda.gov/fnic/Fpyr/NAmFGP.html (Accessed 10 October, 2006).
36. Faber M, Venter SL, Benade AJS. Increased vitamin A intake in children aged 2-5 years through targeted home-gardens in a rural South African community. Public Health Nutrition 2002; 5: 11-16.
37. Norrell B. Traditional Navajo foods and lifestyle bring health and strength. Seattle. WA: Tribal Connections. (Online) 2003. Available: http://www.tribalconnections.org/health_news/secondary_features/traditional.html (Accessed 10 October, 2006).
38. Wood FG. Leisure time activity of Mexican Americans with diabetes. Issues and innovations in nursing practice 2003; 45: 190-196.
39. Diabetic-lifestyle.com. Gardening for Health and Satisfaction: Diabetes-lifestyle.com. (Online) 2003. Available: http://www.diabetic-lifestyle.com/articles/apr03_burni_1.htm (Accessed 10 October, 2006).
40. Yurgalevitch SM, Kriska AM, Welty TK, Go O, Robbins DC, Howard BV. Physical activity and lipids and lipoproteins in American Indians ages 45-74. Medicine and Science in Sports and Exercise 1998; 30: 543-549.
41. Faber M, Phunngula MA, Venter SL, Dhansay MA, Benade AJS. Home gardens focusing on the production of yellow and dark-green leafy vegetables increase the serum retinol concentrations of 2-5-y-old children in South Africa. The American Journal of Clinical Nutrition 2002; 76: 1048-1054.
42. Bellows AC, Brown K. Health benefits of urban agriculture: Community Food Security Coalition. Venice, CA: Community Food Security Coalition, 2003.
43. Armstrong DL. A community diabetes education and gardening project to improve diabetes care in a northwest American Indian tribe. The Diabetes Educator 2000; 26: 113-120.
44. Woodard S. Indian Country Today: Plant a traditional-foods garden. (Online) 2005. Available: http://www.indiancountry.com/content.cfm?id=1096410865 (Accessed 11 October 2006).
45. Native Seeds/SEARCH. Ancient seeds for modern needs. (Online) no date. Available: http://www.nativeseeds.org/v2/default.php (Accessed 10 October, 2006).
46. National Institutes of Health. Theory at a glance: A guide to health promotion practice. Bethesda, MD: United States Department of Health and Human Services, 1997.
47. Janz NK, Champion VL, Stecher VJ. The health belief model. In: K Glanz, BK Rimer, FM Lewis (Eds). Health behavior and health education theory, research and practice, 3rd edn. San Francisco, CA: Jossey Bass, 2002.
48. Steptoe A, Perkins-Porras L, McKay C, Rink E, Hilton S, Cappuccio FP. Behavioural counseling to increase consumption of fruit and vegetables in low income adults: randomized trial. BMJ 2003; 326(7394): 1-6.
49. O'Neill MK, Arnold RN, Smeal D, Jim T, Owen CK, Kohler KD et al. Thirty-eighth annual progress report for 2004: NMSU Agricultural Science Center at Farmington. Las Cruces, NM: NMSU Agricultural Experiment Station and Cooperative Service, 2004.
50. Smeal D, Williams Z. Low-tech, low-cost drip irrigation system for small plots. Farmington, NM: New Mexico State University Agricultural Science Center at Farmington, 2005; 127-133.
51. Okwach GE. Soil and water management: solution for dryland agriculture? The Prunus Tribune 2005; 3: 9.
52. International Development Enterprises. International Development Enterprises Website. (Online) 2006. Available: http://www.ideorg.org/ (Accessed 11 October 2006).
53. Rice RP, Tindall HD. Fruit and vegetable production in warm climates. London: Macmillan, 1990.
54. ATTRA. Solar greenhouses: Horticulture Resource List. (Online) Available: http://attra.ncat.org/attra-pub/solar-gh.html (Accessed 10 October, 2006).
55. Jimenez D, Walser R, Torres R. Hoop house construction for New Mexico: 12-ft. x 40-ft. hoop house. Las Cruces, NM: New Mexico State University Cooperative Extension Service, 2005.
56. Dickerson GW. Row cover vegetable production techniques. Las Cruces, NM: New Mexico State University Cooperative Extension Service, 2004.
57. Emmert EM. Low-cost plastic greenhouses. Lexington, KY: Kentucky Agricultural Experiment Station, 1955; 7.
58. Maynard DN, Hochmuth GJ. Knott's handbook for vegetable growers, 4th edn. New York: John Wiley and Sons, 1997.
59. The George Mateljan Foundation. The world's healthiest foods. (Online) 2006. Available: http://www.whfoods.com (Accessed 10 October, 2006).
_________________
Appendix I
The Native American food pyramid
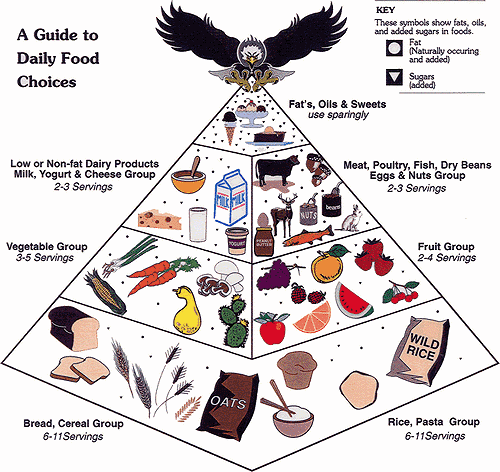

Appendix II
Some vegetable crops and their contribution to the diet, categorized according to season appropriate for a Navajo Gardens for Health45,58,59
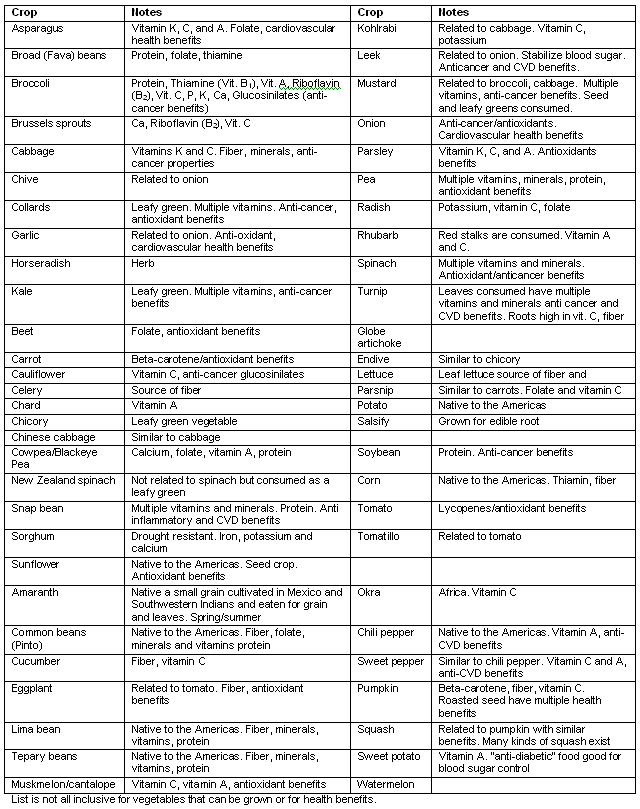
Appendix III
Sources of seed or garden program information




