Introduction
Australian remote area nurses (RANs) are a group of specialist advanced-practice nurses who provide and coordinate a diverse range of healthcare services for remote communities, which are predominantly Aboriginal1-3. They work in unique, challenging and at times dangerous environments, yet their problems have been largely ignored2,4-8. This may partly explain why there is a high turnover of RANs. Little research has been performed to explore the reasons for this turnover, or the impact that health service management may have on the retention of RANs. For many RANs, their line managers are located away from the workplace, possibly hundreds of kilometres away, an experience defined in this article as 'distance management'. In this context, 'management' refers to nursing line managers above the level of health centre manager (or equivalent), who are responsible for the management of a group or region of remote health centres. Effective management under these circumstances is challenging, but potentially has a great impact on job satisfaction and hence retention of RANs. For this reason it was the focus of this study.
There is an emerging skill gap in the remote health workforce, as qualified and experienced RANs are leaving the workforce, practice is more becoming more demanding, and new graduates are either choosing not to work in remote settings or are leaving soon after entering remote practice3,9. Furthermore, there is a major national nursing workforce shortage emerging, with predictions that approximately one-third of nurses with advanced and specialist skills (such as RANs) will retire within the next 15 years10. There has been no nationally coordinated approach to ensure that these nurses can be replaced1,3,11. This has made recruitment and retention of nurses an important issue for health managers, especially in specialist groups such as RANs12,13.
The quality of nursing management has a significant impact on retention of RANs, as in the profession generally3,13,14. High staff turnover rates can be profoundly negative to health outcomes because remote health services and programs are interrupted15. Furthermore, health services spend large amounts of money on recruiting, relocating, and orientating new RANs, who may then remain only for a short time.
To date there have been no Australian studies, or any directly relevant overseas studies, exploring the effects of distance management on nurses. Hegney et al.15 reported a number of retention factors which fell within the management realm, but distance management was not specifically explored.
Charoenngam et al.16 found that in the industrial sector, distance is not necessarily a barrier to effective management, and that appropriate use of communication technology is a critical factor in the success of distance management. Two studies found that geographical distance was a barrier to effective leadership17,18, but others found that this depends on the leadership style expressed in communications with remote team members19.
This study arose from a growing perception among students in a Master of Remote Health Practice program that many of their friends and colleagues were leaving remote practice, citing problems with distance management as part of the reason. The purpose of this study was to identify the effects of distance management on RANs, from the perspective of the RANs themselves, and to generate insights into how these effects might affect their retention.
Methods
The study design employed mixed methods to identify factors relating to distance management that may impact of the retention of RANs. Statistical data were collected through anonymous surveys. Telephone and face-to-face interviews were used to collect qualitative data.
The data collection instruments were developed by the researchers as a Master of Remote Health Practice student project during a study retreat in Alice Springs, Northern Territory (NT), Australia. They were refined through email discussions, and then piloted by an independent steering group at the Council of Remote Area Nurses of Australia (CRANA) and the Centre for Remote Health in Alice Springs. The instruments were amended following feedback from the steering group, most of whom were RANs or ex-RANs.
Ethical approval
Ethical approval was gained from the Human Research Ethics Committee of Flinders University, South Australia.
Data collection
The surveys were distributed by fax to all non-Aboriginal-controlled remote health services in NT, Western Australia (WA) and South Australia (SA), as identified by CRANA. A follow-up phone call was made by one of the researchers to verify reception of the documents, and they were re-faxed if necessary. The intention was to include all RANs in these remote health services in the sample.
Data collection occurred in three ways. First, an anonymous survey consisting of 12 demographic questions, 29 four-point Likert scale questions and six open-ended questions was sent to 110 RANs currently employed in government and other non-Aboriginal-controlled remote health services in NT, WA and SA. Comments were invited with the Likert scale questions to elicit qualitative responses. After 2-4 weeks, one of the researchers made another follow-up phone call to remind potential participants of the survey. The survey is included as a weblink.
Second, a snowball sample of 26 ex-RANs were interviewed using a semi-structured questionnaire similar to the survey but more open-ended, to elicit data about their perceptions of remote practice and distance management. The initial six interviewees were identified by the researchers, and participants were then asked to refer people they knew who had left the RAN workforce within the previous 2 years. This continued until no new themes emerged from the interviews. Participants were made aware of the services of the Bush Crisis Line (a free confidential counselling service provided by CRANA for remote health personnel) before and after the interview, for potential use if they experienced difficulty following the recounting of traumatic experiences.
Third, nine nursing executives with experience in the distance management of remote health services were identified by the researchers from publicly available data about remote health organisations. The selection of these participants was based on their length of service in remote health and, in particular, their length of service in remote nursing management roles. They were interviewed using a semi-structured open-question interview format to obtain their perceptions of distance management of RANs.
Interviews and analysis
Interviews were recorded using handwritten notes, which were subsequently typed; the transcriptions were de-identified and shared among the whole group. A sub-group analysed the themes and issues emerging from the data, which were documented and sent to the whole group for further discussion and interpretation. The surveys were returned to CRANA, de-identified and a sub-group entered the quantifiable data into Microsoft Excel 2003 and SPSS v 13 (student version; SPSS Inc; Chicago, IL, USA) software and analysed using descriptive statistics. Determining significant associations between variables was not part of this study. The whole analysis and interpretation was discussed via several teleconferences over a period of months. Presentations of preliminary results were made to a national conference of RANs in Hobart, Tasmania, and to executive managers in the NT Department of Health and Community Services which provided further confirmation and rigour of interpretations.
The findings were presented predominantly by their frequency and importance, as rated by the RANs. This emerged numerically and by repetition of key points. The results are both a RAN perspective of the most important factors that influence their enjoyment of work, and also their perceptions of the difficulties and challenges faced in relating to management by distance.
Limitations
Logistical and time constraints restricted sampling to WA, SA and NT. It was difficult to effectively sample SA and WA due to problems in obtaining current, comprehensive contact details for the remote clinics in those states. Therefore, as most of the respondents were from NT (90%), the results should be carefully evaluated for their relevance in other jurisdictions. The RANs who worked in Aboriginal-controlled remote health services were also excluded from the study for logistical reasons, so no conclusions can be drawn about their perceptions of management or their working and living conditions.
There may be self-selection bias in the results due to respondents being those who felt most strongly about the issues being researched. On the other hand, it is possible that the most highly-stressed, overworked RANs may not have had the time or energy to complete the survey and, hence, were not represented. It was not possible to determine if there were demographic differences between respondents and non-respondents.
The use of snowball sampling to select ex-RANs for telephone interview may have introduced bias to the data. It is possible that only ex-RANs with exceptional or particularly negative experiences were referred by their peers for interview. For this reason, information from ex-RANs was used only to add depth to the themes expressed by current RANs. The sample was not intended to be representative of ex-RANs.
Results
The sample
Sixty-one surveys were returned, giving a 55% response rate. There were no significant demographic differences among current RANs (n = 61) and the ex-RANs (n = 26) who participated. The average age of participants was greater than 40 years with 81% of respondents being female, and the average years spent in remote work being 5.5 years. Of the participants, 78% were initially educated in hospital-based training programs and 48% had not undertaken post-graduate education.
The setting
Survey respondents were located in areas with an Accessibility and Remoteness Index of Australia (ARIA+) grade of 4 or 5: remote or very remote (Fig 1).
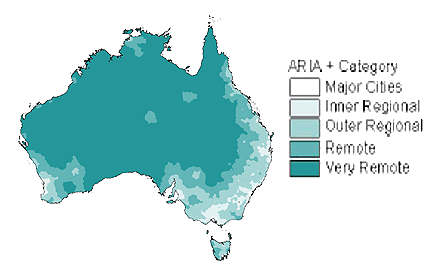
Figure 1: Accessibility/Remoteness Index of Australia (ARIA) and category map20.
These areas encompass 86% of Australia's landmass, but only 6% of its population20. In describing the characteristics of the communities in which they worked, participants used the following descriptors: alcohol abuse, marijuana use, dry community, petrol sniffing, population less than 500, Indigenous population, violence, domestic violence, and high unemployment.
Respondents' concerns related to management practices, including recruitment and orientation, management responsiveness to issues raised by staff, occupational health and safety, staff leave and replacement, professional development and performance review, and exit interviews. In addition, RANs' professional role, RANs' perceived feelings of being valued by the community and their managers, and the quality of infrastructure were also over-arching issues for respondents.
Rewards of remote area practice
The RANs were asked what they enjoyed about their work. Despite their frustration at sometimes feeling inadequately supported, many respondents expressed an overwhelming sense of joy and pleasure in the nature of their work. For example:
Working remote is why I did nursing. I feel incredibly enriched from the experience; it has added another dimension to my life, almost indescribable and certainly unmeasurable.
Aspects of remote practice that respondents found attractive were:
- the type of work performed
- autonomy of practice
- opportunities to implement a case management approach
- working as a member of a small team, allowing development of strong friendships with work colleagues
- providing continuity of care across the lifespan in the context of the family and community
- skills and knowledge obtained through remote area practice were highly transferable to other settings
- good remuneration
- cross-cultural practice
- being able to work in the client's own environment and to develop the trust of the community
- the beauty and isolation of the environment.
Respondents felt well supported by technical guidelines and spontaneously commented on and praised the Standard Treatment Manual devised by the Central Australian Rural Practitioners Association (CARPA)21, which is widely used as a remote health policy manual. Comments included: 'Me and my CARPA became very good friends', and '...using the CARPA and CRANA22 manuals gave me confidence in delivering high quality, best-practice, evidence-based services'.
Management practices and responsiveness
The enthusiasm for their work expressed by respondents was overshadowed by their perception of lack of support from some managers. Many respondents said that ineffective dealings with distance management increased their frustration and stress levels, and were the reason for leaving or contemplating leaving remote practice. A RAN explained:
The only time we have contact with the manager is when you're in trouble for not filling out the right form. They only care about dollars. We care about service and people.
Managers were perceived by many respondents as being inaccessible, not being lateral thinkers, or not engaging with health teams and community members. Respondents' comments on lack of flexibility, innovation, accessibility, respect and vision underlined a perceived general lack of leadership among remote area health distance managers.
Recruitment and orientation: The importance of appropriate recruitment and orientation was recognised by all groups. Forty-seven percent of the survey respondents (n = 26) felt recruitment was generally conducted poorly. Orientation of RANs occurs in two ways: (i) central orientation in a regional centre to induct the recruit into the organisation; and (ii) community-based orientation at the workplace in remote communities. Central orientation was perceived as adequate or good by 77% (n = 40) and excellent by 10% (n = 5). Community-based orientation was also rated adequate or good by two-thirds of the respondents (n = 34) and rated poor by the other one-third (n = 19).
Management responsiveness: Half of the survey respondents said management's responsiveness to issues raised by them was poor, with comments that it was apparently dependent on the priorities of the distance management team and the individual manager. Respondents also reported frequent change in manager and in organisational structure. Lack of stability in the management team contributed a lack of effective support. Comments indicated that respondents felt that they were not listened to, valued or respected:
When I think of leaving it is usually related to frustration over dealing with management in town.
And from an interview with an ex-RAN:
I don't feel I have too many negative experiences being a RAN, but dealing with management is always a never-ending battle which can become very tiring.
Occupational health and safety
Occupational health and safety (OH&S) was regarded as an important issue with half the respondents stating this was not handled well, and none rating it as excellent. An ex-RAN interviewee said that she had experienced an 'appalling lack of assistance' and 'double standards' applied to her reporting of OH&S problems. Occupational health and safety issues were also raised during comments on the levels of violence in communities.
Leave access and replacement
Difficulty in taking leave due to lack of staff replacement was most frequently mentioned in survey and interview comments as a reason to dislike remote practice. One ex-RAN commented:
To survive in some communities, you do need regular long breaks away to restore your strength and sanity, but the system does not allow for that. If it did, people could probably stay longer.
Access to leave was reported as difficult due to travel problems, inability to plan leave because approval was tardy or not forthcoming, and inability to access replacement staff. When respondents were able to take leave, they commented that they were often not replaced or were replaced by inexperienced staff. This meant that work accumulated in their absence, and that the on-call and clinical workload of the remaining staff was sometimes increased to unsafe levels, to the detriment of any primary healthcare programs.
You can access your leave most of time when you want, but that does not mean you can take it. RANs have a conscience and often you put off taking leave because no replacements are available and you don't want to leave your work-mates high and dry.
In some two-nurse posts, when one RAN was on leave, it became a single-nurse post. Several respondents stated they hated being in the community by themselves, which meant being on-call for extended periods with no help. A RAN elaborated:
Leave replacement is not handled well; it is one of the biggest negative factors in a RANs life. ... I have been reduced to begging not to be left in the community alone... Most of us do not do this work because it's easy, but we want to be safe practitioners and we are definitely not supported to do that.
Figure 2 shows the respondents' perceptions of access to leave, and the handling of leave replacement. Most respondents (77%, n = 44) considered that access to leave was adequate, good or excellent; while 23% (n = 13) rated it as poor. This contrasted with perceptions of leave replacement, which was rated poor by 68% (n = 37) of respondents.
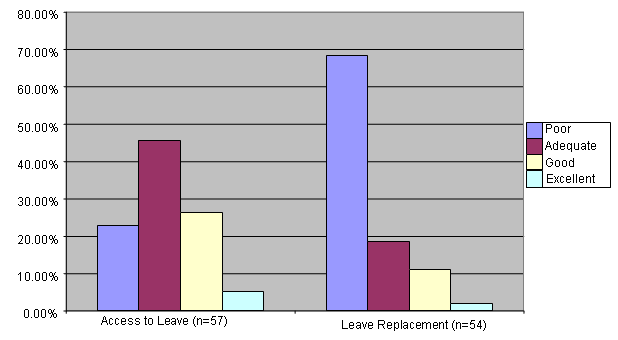
Figure 2: Access to leave and replacement.
Professional development and performance reviews
Forty-four percent of survey respondents (n = 26) rated access to professional development as poor. Respondents commented that they were often unable to attend available professional development courses and seminars because they could not access relief staff. Only one respondent had experienced a performance review.
Exit interviews
Only three out of 26 ex-RANs (12%) interviewed had an exit interview on leaving remote practice, and only one of these was formal. An ex-RAN commented:
Many people leave thinking they are failures when the truth is they were set up to fail.
Twenty ex-RAN interviewees (77%) said an exit interview would be a good idea, especially if it was conducted by an independent person and if the information was then used to inform workplace change.
Workload
Half of the RANs commented on the long working days, characterised by 24 hour, 7 days a week on call. They identified an underestimation of the workload and unrealistic expectations of them made by distance management and the community. One RAN commented:
With an unrealistic workload, we are truly set up to fail if they think we can do all they ask.
An ex-RAN explained:
Constant on call and insufficient breaks; I have been really pushed to the edge by the fatigue of never-ending calls and the ridiculous workload. You lose your perspective and how can you be professional in those circumstances?
Even those who left remote nursing and thought they were not stressed at the time described, in hindsight, similar stories of how it impacted on them:
You are not the person you once were. Not the nicest person to work with, you know its happening but you can't do anything about it, it takes over... you never feel rested or relaxed.
Infrastructure issues
Infrastructure was defined in the survey as including items such as communication, information technology, buildings, essential equipment, repairs and replacement of equipment.
Thirty-nine percent (n = 24) referred to problems accessing the internet, with 42% (n = 26) having set up and paid for their own access. A respondent made the following comment regarding internet access:
We are in the IT age, why does remote health keep throwing out anchors to slow us down?
One RAN equated the poor infrastructure and support as a lack of respect:
I feel really strongly that respect is a very important factor in any organisation and I don't feel that the health department displays this at upper levels, especially to remote health staff. If they did, the infrastructure and support would be better. I think this lack of respect leads to lack of pride in what you do because it's all too hard.
Buildings and accommodation: Thirty-nine percent of respondents (n = 20) considered clinic building quality as poor, and only 8% (n = 4) as excellent. Many respondents identified poor clinic design as an issue, as one RAN said:
By far one of the most soul destroying things is the appalling design and condition of health centres, having no option at times but to conduct consults in hallways. It is an attack on our professionalism....
Staff accommodation was mostly rated in positive terms, with 83% of respondents (n = 45) giving their accommodation an adequate, good or excellent rating (Fig3). Visitor accommodation was less positive, however, with 52% of respondents (n = 27) rating it as poor, and only 8% (n = 4) as excellent. The implications of poor visitors' accommodation is either an imposition on the RAN's own home or a reduction in visiting specialist, professional support and management services.
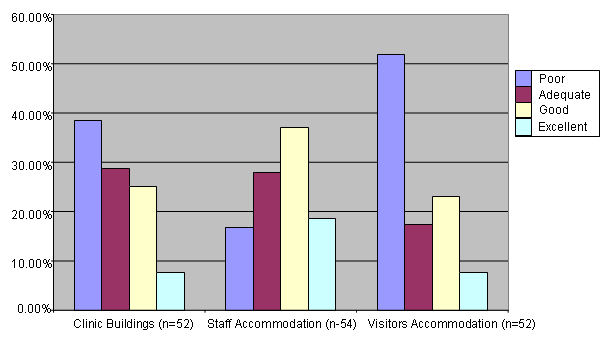
Figure 3: Clinic buildings and staff and visitor accommodation.
Equipment and general repairs: While most respondents felt that replacement of essential clinical equipment was handled adequately or well (n = 39, 64%), one-fifth (n = 13) rated it as poor. Likewise, the great majority (n = 50, 88%) gave the level of existing equipment a positive rating, but some (n = 7, 12%) said it was poor. However, getting repairs carried out was a less positive experience for many respondents. Forty-one percent (n = 22) rated the repair of essential clinical equipment as poor, and 50% (n = 28) rated the handling of general repairs as poor.
A RAN summed up the frustrations of getting repairs done and keeping equipment running:
The saying, 'if it ain't broke don't fix it' would not even come close in communities. Things can be so broken, out of date and beyond repair and still not rate in the 'fix it' plan.
Some of the respondents commented that they did not always receive training on how to use new equipment and 18% (n = 11) suggested that standardisation of the inventory and supply of clinic equipment would be beneficial.
Critical incidents
A 'critical incident' to respondents meant dealing with a range of incidents from a serious car accident or violence-related trauma, to social disruption in the community. The RANs were asked about the support they received after critical incidents. One-third of respondents (n = 20) reported that the support given by remote management teams was poor and, if given, was 'too little too late'. There was a perception that management was more concerned with paperwork than staff. For example, an ex-RAN said:
Management did not listen to my plea. In the end you just lose it and quit so you can save yourself. Management should not let people get to that stage. I actually asked for help but got none... you feel like you have to carry on, until you can't do it anymore....
One of the support mechanisms used by RANs was the Bush Crisis Line which was highly regarded and frequently mentioned as a means of gaining psychological support. Some RANs commented that the best support was from their peers, because they understood the situation.
Violence
The survey did not contain a direct question on violence. Despite this, 17 respondents (28%) mentioned violence as a feature of their work environment. When ex-RANs were specifically asked about safety, 100% said it was an issue that impacted on physical, emotional, spiritual, social and cultural wellbeing. Both ex-RANs and RANs commented about the inadequacy of basic safety issues, such as effective duress alarms that would trigger a local response, rather than one many hundreds of kilometres away. Some RANs noted accommodation was not always secure, lacking adequate locks, lighting, safety spaces such as secure verandas, and security doors.
Respondents commented about being on call alone at night, being ill-prepared for working without support, and having no local police. A RAN said:
It is unbelievable that anyone expects you to leave home in the middle of the night to deliver a service. It's just dangerous. Some places had systems in place so you have some back up. But there is always the situation where they fall down and you have to make a choice, and often women and children are involved, and you just to have to go. Imagine being a nurse in the city and being asked to go and attend to someone in the night by yourself?
Equity of employment conditions between remote area nurses and other remote professionals
In total, 64% of respondents (n = 39) identified a lack of incentives to remain in remote practice, and serious inequalities between themselves and other remote professionals in relation to incentives and support. For example, personal and family support for doctors is well funded by an Australian Government scheme, with workforce agencies established in every state and territory. Financial supports for travel, accommodation and continuing professional development are all features of this support.
The issue of supporting families was important for some respondents, with comments such as:
The sole reason I left is for my children. There is no support for part-time remote nurses, they lose their housing and have no help with childcare. If I could have been supported in my role as a mother I would still be there. It is a great waste of experienced nurses on the ground.
Experts' views
The views of experts interviewed aligned quite closely with those of the RANs. The characteristics of good distance management expressed by the experts included knowing the context in which clinical care is provided and understanding the area being managed. This knowledge was perceived as enabling the managers to develop empathy towards remote staff.
Management skills and roles
All experts mentioned the need for good communication and interpersonal skills. They identified that the management teams' roles should be clearly delineated and communicated to remote staff. Appropriate selection processes in matching RANs to communities were also identified as important. Other management functions identified by the experts were: availability of staff development, leave, relief staff, feedback, debriefing, professional support, salary and employment conditions.
Recruitment and retention: Experts noted that where management is dysfunctional, the recruitment and retention rates of RANs fall, and the resulting staff shortage exacerbates other problems. One expert mentioned that crisis management skills and the ability to get out of crisis mode differentiated good from poor managers. Others mentioned a lack of time to build rapport with their staff.
Lack of infrastructure, high bureaucratic demands (especially a large volume of paperwork), lack of control over funding, and frequent turnover of staff also worked to decrease effective management. One expert believed some RANs have unrealistic expectations of their manager. Another expert suggested that effective problem-solving is hampered by RANs' reluctance to communicate with management about problems until they get 'out of hand'.
Leadership and vision: It was acknowledged by several experts that quality leadership at all levels enhanced team cohesion. Appointing managers with an optimal mix of personality traits, skills, experience and qualifications was seen as important. One expert compared leadership with management:
Leadership is a different thing; it's very, very difficult to lead a remote team. ... Management is not such a difficult thing, because you set the policies in place and then really it's about ensuring that people follow them. But leadership is extremely difficult. We need to employ people into management who have exceptional management and leadership skills.
When asked to articulate their vision for best practice in remote health management, the experts identified a broad range of creative suggestions. For example, future remote health managers needed to be identified from the field, then trained and mentored to achieve a high level of leadership and management skills. This could be achieved by the rotation of RANs into other positions where they can learn about and influence policy and provide regular feedback. Managers need to be appropriately educated, and adequately supported, recognising the unique and challenging complexity of the role, building on a base of clinically relevant experience in remote health.
Experts expressed the importance of mangers having clinical experience and training with regular two-way communication to ensure that policy, management and leadership reflect the reality of practice. An expert recognised the gaps:
There is too big a gap between policy makers and practice. Policy makers need to consult with practitioners and could access the professional issues through organisations like CRANA.
A way forward
The experts perceived the most urgently needed human, physical or monetary resources necessary to improve RAN recruitment and retention to be the provision of appropriate standard accommodation for staff and visitors, and budgets that allow adequate relief for staff.
Experts believed managers should make use of available and emerging technology to communicate with RANs, and work to improve RANs' understanding of the role of the management team. Remote health managers should promote integration of remote health services into the wider health service environment. Furthermore, they should encourage the establishment of remote nurse practitioners to achieve standardisation of practice, and skilled knowledge and leadership. Managers should seek adequate human resources support for their role, and for the RANs they manage. Finally, they should seek to attract and support Aboriginal people in remote health management positions.
Discussion
Remote area nursing is a rewarding career, enjoyed by most participants. With systemic support and reform in place to give more support, RANs may stay longer in remote practice, which could lead to better remote health outcomes.
Both RANs and experts identified the gaps in remote area health care, and potential improvements. Despite the criticisms of distance management and identification of challenges, the majority of RANs expressed a deep satisfaction with their work. They believed this could be improved by better management practices. The perception gained from this study is that the RANs' negative, rather than positive work experience is related to distance management.
The recruitment and orientation of RANs was recognised by all three groups of participants as an issue in the retention of RANs. Managers should select appropriate people to perform the role and also attempt to match the nurse to the particular community. It is important to acquire the correct mix of skills and gender balance in communities where this is a cultural issue and where it helps to provide a culturally appropriate service. The lack of local cultural and community orientation, in many cases, was an issue. A suggestion was made that local cultural and community orientation be formalised, and the local people involved be acknowledged and paid for their role. This would assist new RANs to be more culturally safe practitioners.
The theme of a second-class health system appeared throughout the data. This may reflect the fact that remote area health serves only 6% of the Australian population (except when some of the other 94% visit remote areas as tourists) and is chronically under-funded. Remote area nurses mainly serve Aboriginal communities, many of which are disenfranchised and disrupted. There is an apparent lack of structure to build capacity for local Indigenous staff. Further, there is a perception that the remote health system is suboptimal and would not be acceptable in urban Australia. Additionally, RANs felt that they were treated as 'second-class' in relation to other remote professional staff, such as doctors, teachers and police officers.
The establishment of the Remote Health Practice program by CRANA and Flinders University, SA, has contributed to meeting the educational needs of RANs. However, there is often little recognition by management of the need for on-going education for RANs, as seen in the difficulty of accessing relief staff when RANs attend courses. There is a substantial gap between undergraduate nursing education and the advanced and extended role of RANs, so professional development is a necessity, not a luxury.
The lack or inadequacy of infrastructure and support adds to the RANs' sense of isolation. Not all infrastructure and support factors can be influenced by management, but many can. However, some managers are perceived by respondents to be doing little to improve the things that can be improved.
Almost 40% of respondents thought that the current clinics are inadequate, and a number described long waits for repairs or requisitions of essential clinical equipment needed by RANs to carry out their work effectively. Inadequate infrastructure and a poor work environment creates the perception among RANs that they are not considered important enough or valued enough for adequate services to be provided.
Some RANs expressed the feeling of not being listened to, or that their concerns were not taken seriously. This perception compounds the feeling of being 'second class citizens'. Such feelings, combined with poor infrastructure and inadequate communication with distant managers, can render RANs less resilient to the challenges of remote practice, and may ultimately cause them to leave the remote workforce. These are issues that managers can address. While budget limitations are acknowledged, improved communication between managers and RANs can keep RANs informed, expedite the repair of equipment and buildings, and deal effectively with OH&S issues. RANs may then have a sense of being heard, and that someone cares about their practice.
Distant managers need to acknowledge and respond to feedback, complaints and ideas raised by RANs. The perceived lack of responsiveness was one of the major frustrations with both current and former RANs. There needs to be a common understanding of practice priorities, essential supplies, and workload capacity - and this should be reflected in policy. Despite distance management being recognised in management literature as a specialist field, none of the experts mentioned specific distance management training for remote health managers in their vision for the future. This may be because they feel it is not required, or perhaps it is assumed that recruits to management positions will be appropriately skilled.
A positive note that bodes well for the future of the specialty of remote area nursing is the expressed fact that most RANs love their work and do not want to leave the field, despite the negative features. It is the hope and desire of the respondents to this research project that whatever managers can do to enhance the quality and effectiveness of distance management, they will do. A vision of remote health care shared by both RANs and their managers, backed up with practical actions on both sides, may see an end to the poor retention of RANs.
Conclusion
Some factors which impact on the retention of RANs are not dependent on management, but there are many factors which can be modified by astute managers. Distance management is arguably more difficult than on-site management, but distance is not an insurmountable barrier. However, distance management needs to be recognized as requiring particular skills and attributes when recruiting managers, so that the challenges of the role can be met. Effective communication and leadership, and prompt attention to infrastructure issues, are the keys to ensuring that RANs feel valued and supported. Valued and supported RANs are more likely to be retained than those who are disillusioned and burnt out. This does not mean that all RANs will stay in the field, but any reduction in the turnover rate will benefit remote communities and the health system.
Acknowledgements
The authors would like to acknowledge the generous support of the following: for logistical support, Centre for Remote Health, Charles Darwin University, Flinders University and the Council for Remote Area Nurses of Australia; for psychological support for respondents: the Bush Crisis Line; for the distribution of surveys: Mr Ian Davey; for statistical support: Professor Neil Piller (Flinders University); for typing and data entry: Ms Sally Weymouth; for student support: Ms Sue Lenthall and Ms Sabina Knight. Susan Jannese RN, is acknowledged for her contribution to the design of the research study, the literature review, and the data collection and collation. Also thanked are the RANs who helped spread the word, and all those who participated in the study through the survey, by being interviewed, or in refining the instruments.
References
1. Johnstone MJ, Stewart M. Ethical issues in the recruitment and retention of graduate nurses: A national concern. Contemporary Nurse 2003; 14: 240-241.
2. Hanna L. Continued neglect of rural and remote nursing in Australia: The link with poor health outcomes. Australian Journal of Advanced Nursing 2001; 19: 36-45.
3. National Rural Health Alliance. Action on nursing in rural and remote areas: A discussion paper. (Online) 2002. Available: http://nrha.ruralhealth.org.au/cms/uploads/publications/7_nursing.pdf (Accessed 3 May 2003).
4. Colditz GA, Elliott GC. Queensland's rural practitioners: background and motivations. Medical Journal of Australia 1978; 2: 63-66.
5. Ormiston T. Nurses at work: the whole truth about remote area nursing. Australian Nurses Journal 1983; 12: 22-23.
6. Koltz J. Isolated nursing update: few luxuries for outback nurses. Queensland Nurse 1984; 3: 33-35.
7. Cramer J. Management issues in remote area health services. In: Proceedings, Australian Rural Health Conference; 12-15 August 1992; Toowoomba, QLD. Toowoomba: National Rural Health Alliance, 1992.
8. New South Wales Department of Health. Final report: Nursing Recruitment and Retention Taskforce. Sydney, NSW: NSW Government, 1995.
9. Duffield C, O'Brien-Pallas L. The causes and consequences of nursing shortages: a helicopter view of the research. Australian Health Review 2003; 26: 186-193.
10. Australian Institute of Health and Welfare. Nursing and midwifery labour force 2003. Canberra, ACT: AIHW, 2003.
11. Aboriginal Medical Services Alliance Northern Territory. Submission to the Senate Community Affairs Reference Committee inquiry into nursing. Canberra, ACT: AMSANT, 2001.
12. Bartram T, Joiner T, Stanton P. Factors affecting job stress and job satisfaction of Australian nurses: implications for recruitment and retention. Contemporary Nurse: Health Care Across the Lifespan 2004; 17: 10.
13. Hogan P. Human resource management strategies for the retention of nurses. Contemporary Nurse 2001; 10: 251-257.
14. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Why nurses are resigning from rural and remote Queensland health facilities. Collegian 2002; 9: 33-39.
15. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Retaining rural and remote area nurses: the Queensland, Australia experience. Journal of Nursing Administration 2002; 32: 128-135.
16. Charoenngam C, Ogulana SO, Ning-Fu K, Dey PK. Re-engineering construction communication in distance management framework. Business Process Management Journal 2004; 10: 645-672.
17. Howell JM, Hall-Merenda KE. The ties that bind: the impact of leader-member exchange, transformational and transactional leadership, and distance on predicting follower performance. Journal of Applied Psychology 1999; 84: 680-694.
18. Podsakoff PM, Todor WD, Grover RA, Huber VL. Situational moderators of leader reward and punishment behaviours on subordinate performance and satisfaction. Academy of Management Journal 1984; 25: 810-821.
19. Kelloway K, Barling J, Kelley E, Comtois J, Gatien B. Remote transformational leadership. Leadership & Organization Development Journal 2003; 24: 163-171.
20. Department of Health and Aged Care. Measuring remoteness: Accessibility/Remoteness Index of Australia (ARIA) revised edn. Canberra, ACT: Information and Research Branch, Department of Health and Aged Care, 2001.
21. Central Australian Rural Practitioners Association. CARPA Standard Treatment Manual, 4th edn. Alice Springs, NT: CARPA, 2003.
22. Council of Remote Area Nurses of Australia. Clinical procedures manual for remote and rural practice. Alice Springs, NT: CRANA, 2001.